full article:
Diabetes is one of the eight National Health Priority Areas in Australia due to its associated morbidity and mortality rates, which contribute greatly to national health costs1,2. The direct healthcare expenditure on diabetes in the year 2004-2005 was A$989 million1. Diabetes affects more than one million Australians3 and is predicted to increase in the future4,5. The rates of diabetes consultations1,6, hospitalisation for diabetes complications1,7, and diabetes-related deaths are higher in rural and remote areas of Australia than in major cities and regional areas1. Diabetes as a reason for consultation constituted 1.9/100 encounters in metropolitan areas whereas the rate in rural and remote areas was 4/100 encounters6. In 2004-2005, diabetes hospitalisation in major city and inner regional areas was 68.9 persons/10 000 population compared to 197.9 persons/10 000 population in rural and remote areas1. In 2003-2005, death where diabetes was an underlying cause was found in 33 persons/100 000 population in the major city and inner regional areas whereas the rate in rural and remote areas was 119.5 persons/100 000 population1.
General practitioners (GPs) have a major role in diabetes management, with over 2.9 million diabetes consultations nationally per year in general practice8. This GP role is particularly critical in rural and remote locations, given the limited access to specialist services, allied health professionals and other treatment facilities. Despite the ready availability of local evidence-based diabetes guidelines such as Diabetes management in general practice: Guideline for type 2 diabetes 2011/129 and continuing professional development programs, the gap between evidence-based best practice and actual GP practice is widely recognised10-15. There is, therefore, a strong need to examine effective strategies16-20 to promote the adoption of the evidence-based practice guidelines in management of diabetes in rural and remote general practice.
The use of online continuing medical education (CME) is increasing21-23. A US study reported an increase in physician participation in internet-based learning activities from 305 410 to 4 365 014 during the 2002-200824.The online medium holds several potential benefits to rural and remote GPs including convenience and ready availability, reductions in travelling cost and time, and flexibility to complete at one's own place and time25-27. Research indicates that web-based CME can be effective in imparting knowledge20,25,26,28,29; however there is limited research examining the effects of online CME on practice behaviour20,25,27,30 and patient outcomes20, with mixed results in improving practice/patient outcomes20.
Organisations such as the Australian College of Rural and Remote Medicine (ACRRM), the Royal Australian College of General Practitioners (RACGP), and the Rural Health Education Foundation (RHEF) provide many distance education programs, including online programs. However, these programs have not been rigorously evaluated to determine their effectiveness in producing lasting improvement in GP knowledge, practices and patient outcomes.
This national survey was conducted as part of a PhD research program, forming one arm of a National Health and Medical Research Council (NHMRC)-funded project entitled 'The effectiveness of continuing medical education and feedback in altering diabetes outcomes at a population level'. This main project is examining whether a rural GP-focused intervention involving online CME, GP reminders and feedback can improve patients' outcomes as measured by HbA1c (glycosylated haemoglobin), blood lipids and urinary microalbumin.
A study using a quasi-experimental design is also being conducted as a part of the PhD research to examine the effect of the online CME program on GPs' knowledge, attitudes and practices, examine the barriers in adopting and completing the program, and explore other barriers to online learning.
This national survey was conducted with a comparable population sample to the population in the quasi-experimental study aiming to estimate current knowledge, attitudes and practices in type 2 diabetes management of Australian rural and remote GPs in order to provide focused learning initiatives.
A 35-item questionnaire was developed (Appendix 1). The knowledge questions in the questionnaire were multiple choice questions which were drawn from the online CME program developed by the main NHMRC study. These questions were generated in the broader NHMRC project with input from the Baker IDI team, including GPs and an endocrinologist. Validity of the questions was tested among GPs in focus groups as part of the NHMRC study and an expert reference panel involved in question development and selection. The questions related to screening, prevalence of type 2 diabetes, risk factors for type 2 diabetes, initial assessment, oral medication, monitoring of complications of type 2 diabetes, managing complications and and insulin administration. Case study format was used for some questions. The answers were scored by assigning marks. Each correct answer was given one mark and a wrong answer was given a zero mark.
The questionnaire was piloted in 2011 with 12 GPs (a 14.8% response rate) practising in rural and remote towns meeting the selection criteria for the final survey.
After analysing the responses, the questionnaire was modified, which resulted in elimination of questions with universally correct answers, universally incorrect answers or where ambiguity was present. The final version of the questionnaire included 24 knowledge questions, two sets of attitudinal questions, two open-ended questions regarding learning needs and practice problems regarding type 2 diabetes management; the remaining seven were questions about sources of type 2 diabetes education, prevalence of type 2 diabetes in their own practice and demographic details.
The final questionnaire was mailed to all identifiable GPs (n=854) who:
- were currently practising in a town with a population between 10 000 and 30 000 and classified by the 'Australian Remoteness Index for Areas Plus' (ARIA+) classification system31 as having an index value 2.4 and greater; therefore involving outer regional, remote, and very remote locations within Australia
- were listed in the Medical Directory of Australia, a comprehensive public-domain listing of GPs practising within Australia
- had not participated in the pilot survey.
GPs located in towns selected for the quasi-experimental study were excluded from this survey.
GPs were offered the choice of completing the questionnaire online or on paper. To increase response rates, GPs were informed that the first 10 GPs to complete and return their survey would receive an AU$50 gift voucher and all GPs returning their completed survey by a set deadline would be automatically entered into a draw to win an Apple iPad2. Non-respondents were posted a reminder postcard 2 weeks after the first mailout.
A second round of questionnaires were mailed to 715 GPs who did not respond to the first mailout. Two final reminders were distributed at two-weekly intervals to non-respondents.
Data collection was completed by April 2012. Data were analysed using Statistical Package for the Social Sciences (SPSS) v20 (SPSS Inc.; http://www.spss.com).
Statistical analysis
Descriptive statistics were performed on demographic data and frequency distributions were calculated for all questionnaire items. Knowledge scores were calculated for three sub-categories: (1) screening, assessment and prevalence; (2) medical management; and (3) complication assessment and management. A mean knowledge score of 80% in each sub-category was established by consensus of the investigators as sufficient knowledge for the purpose of this study.
GPs' confidence in managing type 2 diabetes was calculated based on a tally of GP responses to six questionnaire items. GP ratings on a three-point Likert scale ranging from 1 ('not at all confident') to 3 ('very confident') were tallied, creating a confidence score range of 6 to 18. Textual responses to two open-ended questions regarding GP learning needs and practice problems were read multiple times to reveal emergent themes, then classified and coded accordingly. Frequencies were calculated for each.
Pearson product-moment correlation coefficients were performed to examine associations between GP knowledge, confidence, age and number of years working in general practice. Independent sample t-tests were conducted to compare differences in knowledge and confidence between GPs who did or did not use Diabetes management in general practice: Guideline for type 2 diabetes 2011/12, GPs who did or did not have other health professionals working in the practice who assist with diabetes patient care, and age groups. A one-way between-groups analysis of variance (one-way ANOVA) was used to compare the mean difference of knowledge and confidence between years in general practice and numbers of type 2 diabetes patients seen per month. The χ2 test for independence was used to explore the relationship between age groups and the future utilisation of type 2 diabetes education.
Ethics approval
The study was approved by the Monash University Human Research Ethics Committee (MUHREC): Project Number CF10/2616 - 2010001454.
Sample
A total of 854 GPs were distributed the questionnaires, with 209 returned questionnaires giving a response rate of 24.5%.
The majority of responses were received following the first round of mailouts: 132 (15.5%). The additional responses received from the second round of recruitment was 77 (9.0%). GPs showed a strong preference for completion of survey by post: 161 (18.9%) compared to 48 (5.6%) online.
Demographic data
As displayed in Table 1, participating GPs were predominately male, aged ≥45, and with more than 11 years of practice as a GP. The majority of GPs reported having at least one practice nurse on staff at their clinic. However, only 117 GPs (57.4%) indicated having other health professionals working at their practice who assist with diabetes patient care. The majority of GPs had seen fewer than 600 patients per month and fewer than 80 patients with type 2 diabetes per month.
One hundred and thirty-six GPs (66.7%) had used the Diabetes management in general practice: Guideline for type 2 diabetes 2011/129 in their day-to-day practices whereas 59 GPs (28.9%) had not used it and 9 GPs (4.4%) had not heard of these guidelines. Only three GPs (1.5%) were currently enrolled in other specialised training or education for diabetes management.
The gender and age of GPs who participated in this survey were consistent with the Australian GPs workforce population data32 (Table 2); however these did vary in terms of participation by state/territory.
The demographic characteristics of this GP sample were comparable to that of the Bettering the Evaluation And Care of Health (BEACH) study of general practice activity 2009-201033, with the exception of participation rates for GPs from the Northern Territory, Tasmania and Western Australia. However, there were differences in relation to gender, age and participation by state/territory between this sample of GPs and that of the BEACH study 2010-201134. This study focused only on rural and remote locations whereas the BEACH study involved both metropolitan and rural GPs (Table 2). The rural focus of this study could account for the over-representation of Tasmanian and Northern Territory GPs, as there are so few areas classified as metropolitan in those two states (even Hobart does not strictly meet the metropolitan definition).
Table 1: Characteristics of participating GPs and their practices
 Table 2: Comparison of survey demographic data: Bettering the Evaluation And Care of Health
Table 2: Comparison of survey demographic data: Bettering the Evaluation And Care of Health
(BEACH) studies 2009-10, 2010-11 and general practitioner national workforce
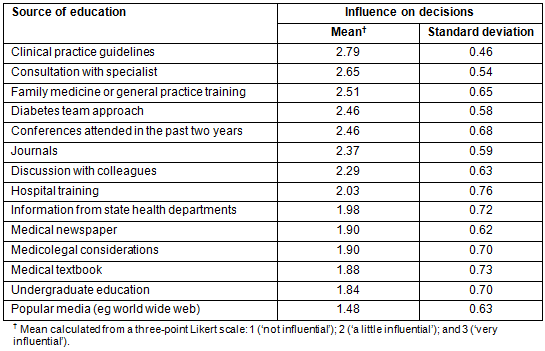
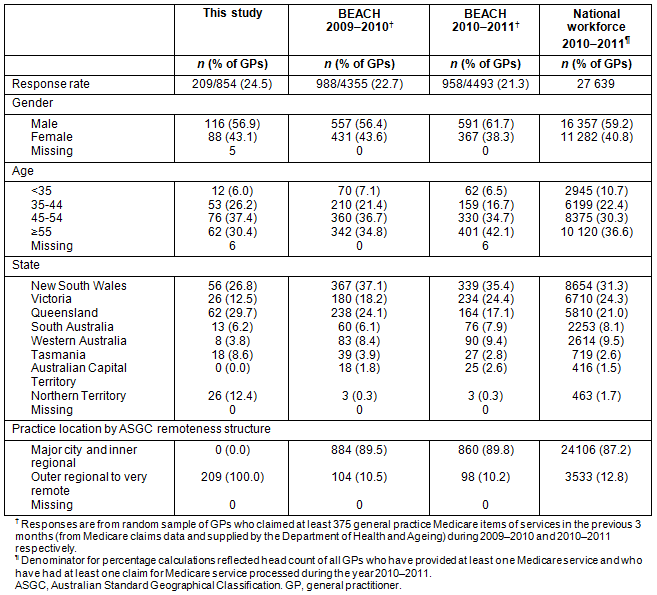 Table 3: Factors influencing daily decision-making in type 2 diabetes management
Table 3: Factors influencing daily decision-making in type 2 diabetes management
Sources of education
Influencing factors on GPs' decision making about type 2 diabetes management: GPs reported that the three most influential factors on their decisions regarding diabetes management in day-to-day practice were clinical practice guidelines, consultation with specialists, and family medicine or general practice training (Table 3). However, there may not be a statistical difference between these.
Preferences for educational methods: Table 4 shows the forms of type 2 diabetes education that GPs have completed during the past 3 years (mid-2008 to mid-2011) and the forms of education that they intend to undertake in the future.
The top three preferred methods for GPs' past and future preferences remained the same. However, the rankings of these preferences varied. GPs' education preference ratings indicated that clinical guidelines will become more popular than other print-based materials whereas conference/seminar attendance will become the most preferred source of education (Table 4). There was an increase from 28.9% to 49.0% in prevalence for structured online learning in the future with associated increases also in interactive workshop, from 33.8% to 49.5%.
A χ2 test for independence indicated the younger GPs (aged ≤45 years) were significantly more likely to utilise structured online learning in the future than those aged over 46 (χ2 (1, n=196) = 8.17, p=0.017, Cramer's V = 0.20 (medium effect size)) whereas the older GPs (aged ≥55 years) were significantly more likely to utilise conferences, seminars, or lecture attendance in the future than those aged under 55 (χ2(1, n=196) = 11.14, p=0.004, Cramer's V = 0.24 (medium effect size)).
Table 4: Recent and future utilisation of type 2 diabetes education
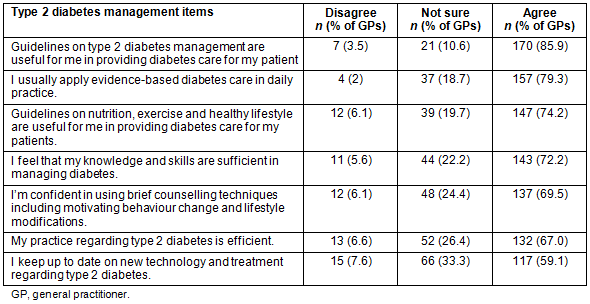
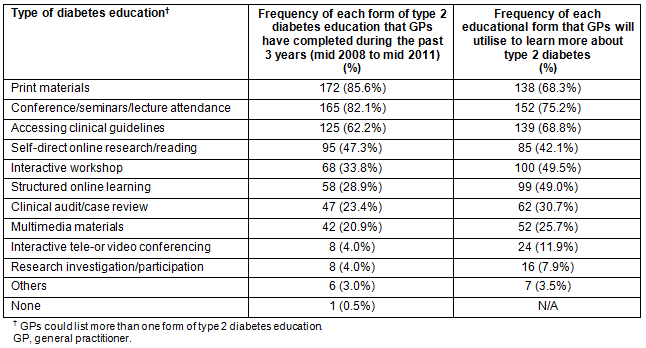 Table 5: GPs' management of type 2 diabetes
Table 5: GPs' management of type 2 diabetes
Learning needs
GPs were asked to provide their answers to the open-ended question identifying their learning needs regarding type 2 diabetes management.
Of those 209 responses, 54 participants (25.8%) declined to answer this question. A further 15 GPs (7.2%) stated that they didn't have any learning needs on type 2 diabetes. In total, 140 GPs (67.0%) reported on their learning needs, which accounted for 191 needs. Frequency of each learning topic is shown in Figure 1. Pharmacological management was the dominant learning need for this group of GPs.
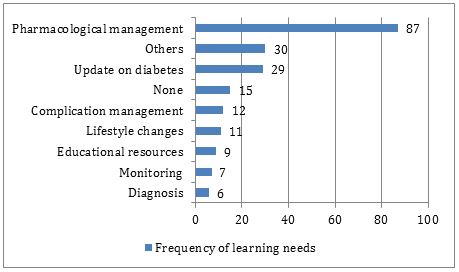 Figure 1: General practitioners' learning needs.
Figure 1: General practitioners' learning needs.
GPs' attitudes regarding type 2 diabetes management
Current type 2 diabetes management: While most GPs agreed that guidelines for type 2 diabetes management were useful in providing evidence-based diabetes care for their patients, only half of them agreed that they keep up to date with new technology and treatment regarding type 2 diabetes (Table 5).
GPs' confidence in type 2 diabetes management: The total confidence mean score for the group was 15.37 (standard deviation (SD) 1.84) out of a total possible score of 18. GPs reported feeling very confident about assessment, testing and diagnosis; assisting patients to make lifestyle changes and/or reduce risk factors; and effective use of medications. However, GPs reported feeling less confident about providing effective insulin treatment; managing complications of diabetes; and managing care plans, team care arrangements using Medicare items (Medicare is Australia's publicly funded healthcare system) (Fig2).
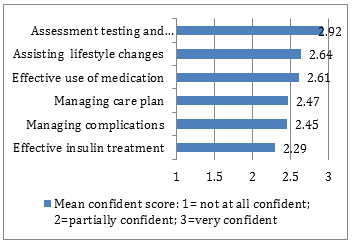 Figure 2: GPs' confidence in type 2 diabetes management
Figure 2: GPs' confidence in type 2 diabetes management
Knowledge
The mean of the total knowledge score for all respondents was 54.23 (SD 3.65) (maximum 66; range 45-62). A mean score for each of three knowledge subgroups was calculated against a perfect score of 1. The highest mean score was on complication management (mean 0.88, SD 0.07) followed by the mean score on screening, assessment and prevalence (mean 0.77, SD 0.08). The lowest mean score was on medical management (mean 0.76, SD 0.17). The knowledge on medical management group was then divided into two subgroups: knowledge of insulin and of oral medications. The mean score of oral medications was 0.75 (SD 0.23) and the mean score of insulin was 0.77 (SD 0.23).
A team approach
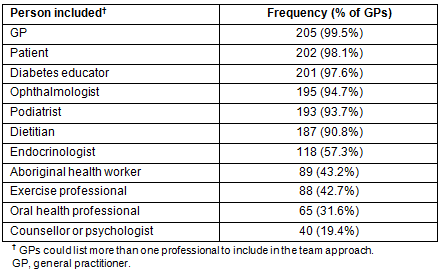
GPs were asked to indicate which of the people are most commonly included in a team approach to diabetes management in adults. More than 90% of GPs indicated that GP, patient, diabetes educator, ophthalmologist, podiatrist and dietician are the most common people included in the team approach to diabetes management (Table 6). However, only half included an endocrinologist in a team approach, which may reflect lack of endocrinologists in rural and remote areas. Few GPs regarded counsellors or psychologists as commonly being included in a team approach to diabetes management.
Table 6: People most commonly included in diabetes management teams
Accessibility to other health professional and specialist services
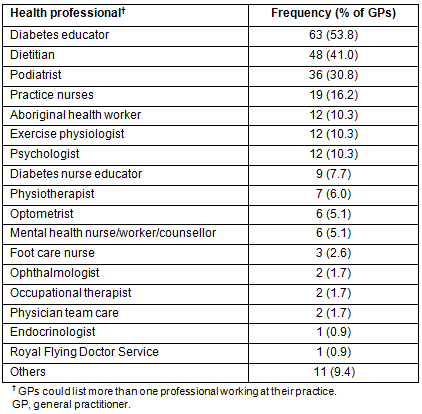
One hundred and seventeen GPs (57.4%) reported that they had one or more other health professionals at their practice who assisted with diabetes patient care. Diabetes educators and dieticians were the most frequently reported health professions (Table 7).
Table 7: Other health professionals at GP practice assisting with diabetes patient care
Practices
Current prevalence of type 2 diabetes: One hundred and ninety-four GPs (92.8%) reported seeing between 4 and 1200 patients (mean 369.7 (SD 243.6); median 400 (interquartile range (IQR) 137; 500 patients))35. (The GP who reported seeing 4000 patients per month of which 500 patients had type 2 diabetes was excluded from the analysis.)
Of those patients seen monthly, the number of patients diagnosed with type 2 diabetes ranged from 1 to 350; (mean 47.8 (SD 46); median 40 (IQR 20; 60 patients)).
One hundred and seventy GPs (85.0%) believed that number of patients they saw with type 2 diabetes had increased over the past 10 years, whereas 26 GPs (13.0%) believed that the number of diabetes patients had decreased; four GPs (2.0%) believed that the number of diabetes patients had stayed the same.
Practice problems: GPs provided written responses identifying any difficulties they encountered regarding their current type 2 diabetes management.
Of 209 participating GPs, 64 participants (30.6%) declined to answer this question. Twenty GPs (9.6%) stated that they did not have any problems regarding their current type 2 diabetes management. Therefore the diabetes management difficulties were identified by 125 GPs (59.8%), who provided 195 problems.
Difficulties were categorised into system of care-related problems (n=81), GPs' clinical management related problems (n=69), patient-related problems (n=40) and others (n=5). Accessibility to nurse and allied health professionals was a dominant part of the system of care related problem, followed by care planning, managing team based care and difficulty in getting access to specialists (Fig3). The medication treatment was the most frequently reported problem of GPs' clinical management related problems (Fig4). Patient-related problems included patients' compliance (n=26) and treating 'difficult' patients (n=14).
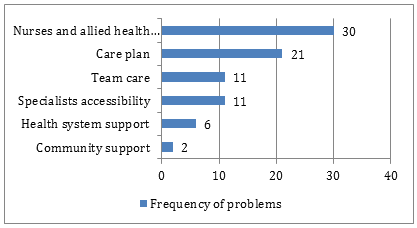 Figure 3: System of care related problems
Figure 3: System of care related problems
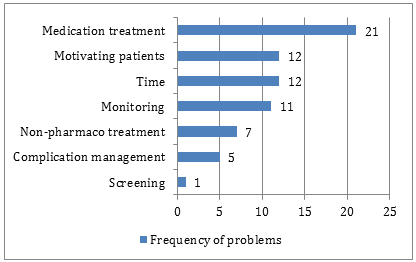 Figure 4: GPs' clinical management related problems
Figure 4: GPs' clinical management related problems
Relationship between knowledge, confidence in type 2 diabetes management, age, and number of years working in general practice
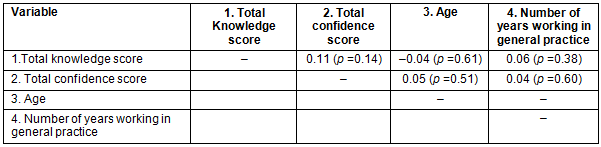
Knowledge and confidence in type 2 diabetes management were not related to age and number of years working in general practice (Table 8).
Table 8: Pearson product-moment correlations between knowledge, confidence, age and number of years in general practice
Difference in knowledge and confidence between groups
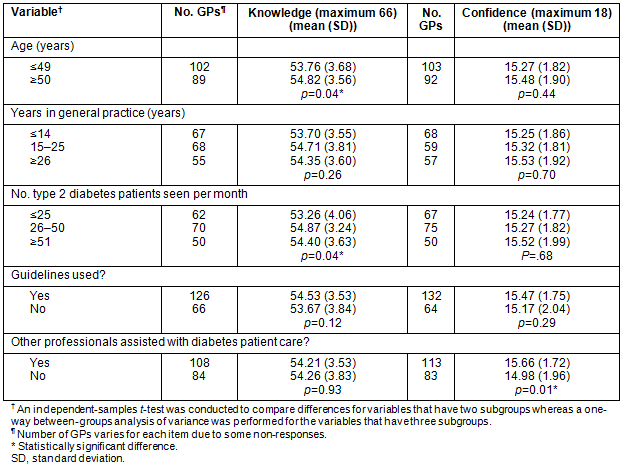
The differences in the knowledge and confidence between groups were explored using an independent-sample t-test and a one-way between-groups analysis of variance. Table 9 shows a difference in knowledge and confidence score by age, years in practice, numbers of type 2 diabetes patients seen per month, guidelines used, and assistance of other health professionals with diabetes patient care.
Younger GPs (aged ≤49 years) had significantly lower mean knowledge scores (53.76 ± 3.68, p=0.04) than GPs aged ≥ 50 years (54.82 ± 3.56, p=0.04). GPs who had seen 26-50 type 2 diabetes patients per month had significantly higher knowledge scores (54.87 ± 3.24, p=0.04) than those who had seen 25 or fewer diabetes patients per month (53.26 ± 4.06, p=0.04) but no significant difference to those who had seen 51 or more diabetes patients per month (54.40 ± 3.63, p=0.23). However, there were no significant differences in knowledge based on years worked in general practice; use or not of the Diabetes management in general practice: Guideline for type 2 diabetes 2011/12, or presence or absence of other health professionals in the practice to assist with diabetes patient care.
GPs who had other health professionals working in the practice to assist with diabetes patient care had significantly higher confidence scores (15.66 ± 1.72, p=0.01) than GPs without this extra support (14.98 ± 1.96, p=0.01). However, there were no significant differences in confidence in type 2 diabetes care between age groups, years worked in general practice or numbers of type 2 diabetes patients seen per month.
Table 9: Knowledge, confidence score for general practitioners by age, years in practice, guidelines used and type 2 diabetes caseload
Discussion
This national study provides a snapshot of current knowledge, attitudes and practices of Australian rural and remote GPs who are the major provider of diabetes care in rural and remote areas8.
Many educational programs and clinical guidelines on type 2 diabetes management are available to GPs. Despite this, GPs show deficits in knowledge and confidence when it comes to diabetes care. Confidence represents GPs' feelings of self-efficacy regarding the aspects of diabetes management. It is hard to guess the impact of confidence unless a study is conducted specifically examining relationship between confidence and behaviour or practice outcomes.
This survey demonstrated gaps in knowledge and confidence regarding diabetes management. In this study, the relationship of knowledge and confidence in some areas of diabetes management was not linear (eg knowledge and confidence in effective use of medication). It is dangerous to practise with confidence without sufficient knowledge. Therefore even though GPs feel confident there is a need to maintain current knowledge on evidence-based diabetes care. GPs reported sound levels of knowledge in regard to management of complications which did not translate into similar levels of confidence in managing these complications.
A gap between treatment targets and actual achievement in diabetes practice in Australia was found in recent literature. Jiwa et al10 explored GP management of diabetes using case scenarios and compared their management with experts in which the experts' management referred to the NHMRC guidelines. This study found that GPs were less likely to prescribe statin, to treat hypertension and refer for lifestyle modification. In addition they were more likely to underdose medication. This is similar to a study that found an evidence-based prescribing practice gap in Australian primary care11. The gap in diabetes practices was also found in Australian urbanised GPs where an initiation of oral hypoglycaemic agents was delayed despite HbA1c exceeding 7.7%, which is contrary to the recommended guidelines36.
Deficits in knowledge, confidence and gaps in practices may suggest that currently available CME resources are under-utilised and/or are not hitting the mark for GP learning needs. In addition, only half of GPs reported keeping up to date with new technology and treatment modalities for diabetes. This may be one of the possible reasons for deficits in knowledge.
Recommendations may include GPs completing required diabetes modules as part of maintenance of continuing professional development triennial requirements. ACCRM or RACGP may need to provide a mandatory online module exam on diabetes at the end of every triennium and GPs would need to pass the exam, otherwise additional diabetes training or learning activities would be required. A diabetes management hotline or email chat resource facilitated by diabetes specialist or endocrinologists could be provided and available in each GP's divisional area. However, importantly, diabetes education programs need to be firstly tested for their effectiveness in changing practice behaviour and standards.
Many studies have examined GPs' knowledge, attitudes and practices in relation to diabetes. These studies reported a variety of deficits in knowledge and competence37-41.
The present study showed no statistical difference in knowledge or attitudes between GPs who had practised 14 years or less and those who had practised more than 14 years. This result was not true in two studies38,41. Khan et al41 reported that GPs with 1-5 years of experience had significantly higher knowledge, attitudes and practice scores than those with more than 5 years experience, whereas a study of Shera et al38 showed that GPs who practised between 6 and 10 years reported significantly more correct answers in knowledge and attitudes than those with either less or more. The present study showed no difference in knowledge regarding years worked in general practice. This could be because all participants were located in rural and remote areas, which may have limited opportunities to attend educational programs.
In this study, GPs aged 50 years or more had significantly higher knowledge scores than the younger age group. The elder group may have more experience in managing more cases of type 2 diabetes than those who just completed their general practice training. This is confirmed by the results that GPs who saw more diabetes patient per month had significantly higher knowledge scores than those who reported having lighter caseloads. Even though Australian GPs need to maintain their registration by earning credit points every triennium, there is no compulsion for the education topics to include diabetes. The older group therefore may have completed diabetes programs more often than younger group. Another possible reason is response bias: more older doctors who complete diabetes education programs participated in the survey.
Although this study showed that the clinical practice guidelines are one of the more influential factors on GPs' decisions regarding diabetes management, only two-thirds had used key clinical practice guidelines produced by RACGP and Diabetes Australia9. Notably, however, GPs who had used these guidelines did not report greater levels of knowledge on diabetes management than GPs who had not accessed the guidelines. The same result was found in one study conducted in Estonia37, where the GPs' knowledge and treatment behaviour regarding type 2 diabetes patient care was not related to use or availability of the guidelines. However, a study by Khan et al41 reported higher knowledge, attitude and practice scores regarding type 2 diabetes management in the group of GPs who had clinical practice guidelines at their clinics. The RACGP guidelines9 may not have improved GPs' knowledge, as seen in this study, because GPs may have used other local diabetes guidelines (reported by some respondents).
The guidelines on type 2 diabetes management9 include a guide on insulin treatment, when to start, choices of insulin, insulin delivery and types available, but details on the role that GPs have in practice are not described. In this study, 85.9% of respondents agreed that guidelines on type 2 diabetes management were useful. However, additional information within the guidelines that serves GPs' needs is still required. In addition, additional training or educational programs on insulin management should be provided.
Although conferences, seminars and lecture attendance are currently the most preferred option of type 2 diabetes education, the utilisation of structured online learning was predicted to increase. Given that online CME has potential benefits for rural and remote GPs, effective implementation of structured online learning to promote the adoption of the clinical practice guidelines for these GPs needs to be explored20,42-44.
GPs stated their most pressing learning needs centred around medical management, in particular effective insulin treatment. This finding corresponded with GP knowledge scores relating to medical management, highlighting the need for further educational programs addressing these topics. This has important implications for rural practice where specialists and endocrinologists are less available, thereby increasing demand for greater levels of expertise among GPs.
GPs reported an awareness of the benefit of a team approach to diabetes management, in which GP, patient, diabetes educator, ophthalmologist, podiatrist and dietician were included. However, in this study, specialists such as endocrinologists were less likely to be included in this team care approach. The possible reason may be due to the lack of endocrinologists working in these rural and remote areas, in which only 0.9% of participating GPs reported having an endocrinologist working in the practice. The importance of a team approach was also highlighted in the significantly higher confidence levels of GPs regarding type 2 diabetes management when they had other health professionals on site to assist with diabetes care. Previous studies, conducted outside Australia, showed mixed results of teamwork in diabetes care. Some studies suggested the positive impact of team care45-47 while some did not48,49. The present study did not explore whether participating GPs use team-based approaches at their practice or if this approach is effective in changing behaviour or healthcare outcomes. Future studies are needed to examine the effectiveness of a team-based care and barriers in applying this approach in diabetes care, in particular in rural and remote Australian locations.
This point is of particular importance, given the difficulties that rural and remote GPs face in gaining timely and ready access to specialists, diabetes educators, nurses and allied health professionals, and other health facilities. While most of the GPs had some access to specialists and allied health professionals, and half had other health professionals working in the practice (Table 7), many stated the difficulties in accessing assistance when needed and the burden of care this places on GPs. The Australian Government Department of Health and Ageing (DoHA) implemented Medicare rebates for GPs to have a video consultation with other specialists in a distant location in July 201150. This telehealth service provides an option for rural and remote GPs to access other medical specialists. However, there is limited evidence on the effectiveness of this delivery method in the Australian primary healthcare setting51. There is therefore a need for future studies to examine its effectiveness and also the barriers in applying this service in rural and remote GP settings.
These findings are based on a relatively representative sample of GPs when compared with GP national workforce32. The survey was conducted with GPs in clearly defined rural and remote areas using an ARIA+ classification index value of 2.4 and greater which included GPs in outer regional, remote and very remote areas of Australia with town populations of 10 000 to 30 000.
Findings from this study may be generalised with some caution to practising GPs in similar locations across Australia. Notably, this study had a moderately low response rate of 24.5%. Although this is a relatively typical response rate for general practice research, (eg BEACH study 2010-2011)34, it limits the conclusions that may be drawn from the findings.
In an effort to increase a response rate, the questionnaire was offered in both hard copy and online form, together with a variety of reminders and incentives. Methods for improving recruitment rates in the study involving GPs merit further examination in future studies.
The findings of this study provide a snapshot of current knowledge, attitudes and practices for type 2 diabetes management of Australian rural and remote GPs. GPs reported less confidence and knowledge in relation to insulin treatment and medication management. A large proportion of reported practice difficulties centred around reduced access to nurses, allied health professionals and specialists. Further research is recommended to examine the impact of CME programs on GP knowledge, attitudes and practices, including online learning and the role of telehealth in providing specialist support.
Six key points
- GPs reported deficits in knowledge regarding medical treatment and are less confident in effective management of type 2 diabetes using insulin.
- There is a disconnect between the level of knowledge of complications related to type 2 diabetes and confidence in managing these complications.
- GPs who used the RACGP guidelines reported a positive attitude about the benefit of the guidelines for type 2 diabetes management. However, the use of guidelines did not correlate with their level of knowledge.
- The majority of GP-reported challenges in managing type 2 diabetes related to the system of care, including limited access to nurses, allied health professionals and specialists. Medication treatment was the second most reported challenge that related to GPs' clinical management.
- Pharmacological management including use of injectables was identified as a significant learning need by GPs.
- Although GPs indicated a preference for face-to-face diabetes CME, they also reported a strong preference for structured online learning in the future.
Acknowledgements
The authors gratefully acknowledge funding from the National Health and Medical Research Council (546096) and support from rural and remote GPs who participated in this study.
References
1. Australian Institute of Health and Welfare 2008. Diabetes: Australian facts 2008. Diabetes series no. 8, cat. no. CVD 40. Canberra, ACT: Australian Institute of Health and Welfare, 2008.
2. Australian Institute of Health and Welfare. Australians' Health 2004: the ninth biennial health report of the Australian Institute of Health and Welfare. Canberra, ACT: Australian Institute of Health and Welfare, 2004.
3. National Health and Medical Research Council (NHMRC). National evidence based guidelines for the management of Type 2 diabetes mellitus. (Online) 2005. Available: http://www.nhmrc.gov.au/publications/synopses/di7todi13syn.htm (Accessed 16 December 2012).
4. Whiting DR, Guariguata L, Weil C, Shaw J. IDF Diabetes Atlas: global estimates of the prevalence of diabetes for 2011 and 2030. Diabetes Research and Clinical Practice 2011; 94(3): 311-321.
5. Davis WA, Knuiman MW, Hendrie D, Davis TME. The obesity-driven rising costs of type 2 diabetes in Australia: projections from the Fremantle Diabetes Study. Internal Medicine Journal 2006; 36(3): 155-161.
6. Knox S, Britt H, Pan Y, Miller GC, Bayram C, Valenti L, et al. Locality matters: the influence of geography on general practice activity in Australia 1998-2004. AIHW cat. no. GEP 17. Canberra, ACT: Australian Institute of Health and Welfare (General Practice Series No. 17), 2005.
7. Public Health, Rural and Regional Health and Aged Care Services Division, Victorian Government Department of Human Services. The Victorian Ambulatory Care Sensitive Conditions Study 2001-2002. Melbourne, VIC: Department of Human Services, 2004.
8. Australian Institute of Health and Welfare 2002. Diabetes: Australian facts 2002. Diabetes series no. 3, cat. no. CVD 20. Canberra, ACT: Australian Institute of Health and Welfare, 2002.
9. RACGP and Diabetes Australia. Diabetes management in general practice: Guideline for Type 2 diabetes 2011/12. (Online) 2011. Available: http://www.racgp.org.au/Content/NavigationMenu/ClinicalResources/RACGPGuidelines/Diabetesmanagement/201107diabetesmanagementingeneralpractice.pdf (Accessed 4 October 2012).
10. Jiwa M, Meng X, Sriram D, Hughes J, Colagiuri S, Twigg SM, et al. The management of Type 2 diabetes: a survey of Australian general practitioners. Diabetes Research and Clinical Practice 2012; 95(3): 326-332.
11. Krass I, Hebing R, Mitchell B, Hughes J, Peterson G, Song YJC, et al. Diabetes management in an Australian primary care population. Journal of Clinical Pharmacy and Therapeutics 2011; 36(6): 664-672.
12. Gardner K, Bailie R, Si D, O'Donoghue L, Kennedy C, Liddle H, et al. Reorienting primary health care for addressing chronic conditions in remote Australia and the South Pacific: review of evidence and lessons from an innovative quality improvement process. Australian Journal of Rural Health 2011; 19(3): 111-117.
13. Grol R, Wensing M. What drives change? Barriers to and incentives for achieving evidence-based practice. Medical Journal of Australia 2004; 180(6 SUPPL.): S57-S60.
14. Taylor J, Wilkinson D, Blue I, Dollard J. Evidence-based rural general practice: barriers and solutions in South Australia. Journal of Rural and Remote Health 2(1): 116. (Online) 2002. Available: www.rrh.org.au (Accessed 6 October 2012).
15. Young JM, Ward JE. Evidence-based medicine in general practice: beliefs and barriers among Australian GPs. Journal of Evaluation in Clinical Practice 2001; 7(2): 201-210.
16. Davis DA, Thomson MA, Oxman AD, Haynes RB. Changing physician performance: a systematic review of the effect of continuing medical education strategies. Journal of the American Medical Association 1995; 274(9): 700-705.
17. Bloom BS. Effects of continuing medical education on improving physician clinical care and patient health: a review of systematic reviews. International Journal of Technology Assessment in Health Care 2005; 21(3): 380-385.
18. Davis D, O'Brien MAT, Freemantle N, Wolf FM, Mazmanian P, Taylor-Vaisey A. Impact of formal continuing medical education: do conferences, workshops, rounds, and other traditional continuing education activities change physician behavior or health care outcomes? Journal of the American Medical Association 1999; 282(9): 867-874.
19. Davis D. Does CME work? An analysis of the effect of educational activities on physician performance or health care outcomes. International Journal of Psychiatry in Medicine 1998; 28(1): 21-39.
20. Cook DA, Levinson AJ, Garside S, Dupras DM, Erwin PJ, Montori VM. Internet-based learning in the health professions: a meta-analysis. JAMA - Journal of the American Medical Association 2008; 300(10): 1181-1196.
21. Cobb SC. Internet continuing education for health care professionals: an integrative review. Journal of Continuing Education in the Health Professions 2004; 24(3): 171-180.
22. Bennett NL, Casebeer LL, Kristofco RE, Strasser SM. Physicians' Internet information-seeking behaviors. Journal of Continuing Education in the Health Professions 2004; 24(1): 31-38.
23. Cobb SC. Comparison of oncology nurse and physician use of the Internet for continuing education. Journal of Continuing Education in Nursing 2003; 34(4): 184-188.
24. Casebeer L, Brown J, Roepke N, Grimes C, Henson B, Palmore R, et al. Evidence-based choices of physicians: a comparative analysis of physicians participating in Internet CME and non-participants. BMC Medical Education 2010; 10(1).
25. Fordis M, King JE, Ballantyne CM, Jones PH, Schneider KH, Spann SJ, et al. Comparison of the instructional efficacy of internet-based CME with live interactive CME workshops: a randomized controlled trial. Journal of the American Medical Association 2005; 294(9): 1043-1051.
26. Wutoh R, Boren SA, Balas EA. eLearning: a review of Internet-based continuing medical education. Journal of Continuing Education in the Health Professions 2004; 24(1): 20-30.
27. Curran VR, Fleet L. A review of evaluation outcomes of web-based continuing medical education. Medical Education 2005; 39(6): 561-567.
28. Curran VR, Fleet LJ, Kirby F. A comparative evaluation of the effect of internet-based CME delivery format on satisfaction, knowledge and confidence. BMC Medical Education 2010; 10(1).
29. Curran V, Lockyer J, Sargeant J, Fleet L. Evaluation of learning outcomes in web-based continuing medical education. Academic Medicine 2006; 81(10 SUPPL.): S30-S34.
30. Short LM, Surprenant ZJ, Harris Jr JM. A community-based trial of an online intimate partner violence CME program. American Journal of Preventive Medicine 2006; 30(2): 181-185.
31. Accessibility/remoteness index of Australia (ARIA+ 2006 version). (Online) 2006. Available: http://www.adelaide.edu.au/apmrc/research/projects/category/aria.html (Accessed 16 December 2012).
32. Department of Health and Ageing. General practice statistics: GPs workforce statistics - 1984-85 to 2010-11. (Online) 2012. Available: www.health.gov.au/internet/main/publishing.nsf/Content/General+Practice+Statistics-1 (Accessed 9 December 2012).
33. Britt H, Miller G, Charles J, Henderson J, Bayram C, Pan Y, et al. General practice activity in Australia 2009-10. General practice series no. 27. Cat no. GEP 27. Canberra, ACT: Australian Institute of Health and Welfare, 2010.
34. Britt H, Miller GC, Charles J, Henderson J, Bayram C, Pan Y, et al. General practice activity in Australia 2010-11. General practice series no. 29. Sydney, NSW: Sydney University Press, 2011.
35. Billah B. Module 2: Summary statistics. Introduction to BioStat for clinical and Public Health Research, Module 1-12 manual. Melbourne, VIC: Monash University, 2012; 26.
36. Davis TME, Davis WA, Bruce DG. Glycaemic levels triggering intensification of therapy in type 2 diabetes in the community: the Fremantle Diabetes Study. Medical Journal of Australia 2006; 184(7): 325-328.
37. Rätsep A, Kalda R, Oja I, Lember M. Family doctors' knowledge and self-reported care of type 2 diabetes patients in comparison to the clinical practice guideline: cross-sectional study. BMC Family Practice 2006; 7(1): 36.
38. Shera AS, Jawad F, Basit A. Diabetes related knowledge, attitude and practices of family physicians in Pakistan. Journal of the Pakistan Medical Association 2002; 52(10): 465-470.
39. Shaikh IA, Khan AH, Khoharo HK. Knowledge, attitudes and practices of general practitioners towards diabetes mellitus in Hyderabad, Sindh. Journal of the Liaquat University of Medical and Health Sciences 2011; 10(2): 68-70.
40. Katulanda P, Constantine GR, Weerakkody MI, Perera YS, Jayawardena MG, Wijegoonawardena P, et al. Can we bridge the gap? Knowledge and practices related to Diabetes Mellitus among general practitioners in a developing country: a cross sectional study. Asia Pacific Family Medicine 2011; 10(1).
41. Khan AR, Al Abdul Lateef ZN, Khamseen MB, Al Aithan MA, Khan SA, Al Ibrahim I. Knowledge, attitude and practice of ministry of health primary health care physicians in the management of type 2 diabetes mellitus: a cross-sectional study in the Al Hasa District of Saudi Arabia, 2010. Nigerian Journal of Clinical Practice 2011; 14(1): 52-59.
42. Cook D. Where are we with web-based learning in medical education? Medical Teacher 2006; 28(7): 594-598.
43. Cook DA. The research we still are not doing: an agenda for the study of computer-based learning. Academic Medicine 2005; 80(6): 541-548.
44. Bassand JP, Priori S, Tendera M. Evidence-based vs. 'impressionist' medicine: how best to implement guidelines. European Heart Journal 2005; 26(12): 1155-1158.
45. Stevenson K, Baker R, Farooqi A, Sorrie R, Khunti K. Features of primary health care teams associated with successful quality improvement of diabetes care: a qualitative study. Family Practice 2001; 18(1): 21-26.
46. Bower P, Campbell S, Bojke C, Sibbald B. Team structure, team climate and the quality of care in primary care: an observational study. Quality and Safety in Health Care 2003; 12(4): 273-279.
47. Campbell SM, Hann M, Hacker J, Burns C, Oliver D, Thapar A, et al. Identifying predictors of high quality care in English general practice: observational study. BMJ 2001; 323(7316): 784-787.
48. Bosch M, Dijkstra R, Wensing M, van der Weijden T, Grol R. Organizational culture, team climate and diabetes care in small office-based practices. BMC Health Services Research 2008; 8(1): 180.
49. Hann M, Bower P, Campbell S, Marshall M, Reeves D. The association between culture, climate and quality of care in primary health care teams. Family Practice 2007; 24(4): 323-329.
50. The Royal Australian College of General Practitioners. Guideline for interpersonal collaboration between general practitioners and other medical specialists providing video consultations. East Melbourne, VIC: Royal Australian College of General Practitioners 2013; 1.
51. The Royal Australian College of General Practitioners. Standards for general practices offering video consultation: an addendum to the RACGP Standards for general practices (4th edn). South Melbourne, VIC: Royal Australian College of General Practitioners 2011; 93-94.
Appendix 1: Click here to access the questionnaire (pdf).
