full article:
Introduction
Research efforts investigating the mental health of Australians living in rural areas, in particular rural adolescents, have been scant1-5. An overview of rural health research in Australia in the period 1990-1999 revealed only a small number of published articles on adolescent mental health6 despite the fact that, as Kilkkinen et al7 highlighted, children and adolescents represent a higher proportion of the population in rural and remote areas compared with urban areas, and research needs to target these priority groups. The Australian National Health Policy also supported the need for greater research attention on the mental health of rural and remote Australians8, and the rural health policy framework, 'Healthy Horizons', recognises 'mental health, suicide and attempted suicide as among the highest priorities for action in rural health'9.
This paucity of research investigating rural adolescent mental health in Australia in particular, is of concern for a number of reasons:
- It has been empirically established that, in contrast to the overall health gains of world populations in recent decades, the burden of mental illness is mounting.
- Mental and behavioural health disorders are common, being present at any point in time in approximately 10% of the population, and affecting more than 25% of all people at some time during their lives10.
- In 2002, depression accounted for 4.5% of the worldwide total burden of disease. It is also responsible for the greatest proportion of burden attributable to non-fatal health outcomes, accounting for almost 12% of total years lived with disability worldwide10.
- It is estimated that by 2030, depression will be one of the leading causes of disease along with HIV/AIDS and heart disease11.
Moreover, it has been reported that adolescents living in rural areas appear to be at a heightened risk for developing a mental health problem, compared with their urban counterparts. This is apparently due to a number of psychosocial factors:
- stressful life events, perceived control of life events12
- lack of access to mental health services
- the effect of the economic downturn on rural areas, and severe drought in a number of geographical regions.
In addition, the suicide rates are consistently higher in rural towns than in metropolitan areas; for example, the suicide rate of males aged 15-24 years in rural towns has been reported as approximately twice that of their city counterparts13. For young Indigenous males, the suicide rate is up to 40% higher than the national Australian average14.
In response to such issues, The Australian Rural Mental Health Study15 embarked on building an evidence base for the adult rural population. 'Proxy' (ie alternative) measures of child health and wellbeing have also been included in this study. The establishment of headspace16, a federally funded youth mental health foundation service, in a number of rural areas of Australia has included two centres in South Australia. However, Boyd1 suggests that while we are facing a period of mental health reform with such strategies:
...although assurances have been made that the needs of rural youth will be considered as part of a national strategy to transform youth mental health services, rural communities remain without vision or direction as to how this might be achieved.
One possible way to achieve direction in order to address the needs of adolescents from rural communities may be to enhance the evidence base of this population. This may be achieved by investigating not only prevalence rates of adolescent mental health problems, but also by examining the individual, family7 and community factors, or the determinants17, of such problems. For it has been suggested that many large population-based studies have failed to include an assessment of such important factors associated with mental health problems18.
A number of studies have reported that family processes, in particular the nature and quality of adolescents' relationships with their parents, contribute to the onset and maintenance of a range of negative developmental outcomes19,20. The nature of the interpersonal interactions children experience with their parents may influence the level of perceived acceptance from their parents, for instance, which may impact on a young person's developing sense of self and identity. If responses during interactions from significant others are disregarded and/or not recognised as important, a negative self-view is more likely, which may increase the risk for developing an internalising problem, such as depression or anxiety.
However, the challenge is to integrate variables of interest from multiple domains (ie individual, family, and community) into a theoretical framework capable of structuring and exploring the possible processes that influence specific developmental outcomes. Employing a theoretically derived framework for the basis of empirical research is essential, as the data generated is evidence-based and so more likely to effectively inform policy and, hence, interventions and/or preventative efforts.
The framework that formed the basis of this study is a Process Model21 which consists of a number of theoretically-derived variables. A multidimensional blueprint such as this enables a dynamic investigation of Individual Processes (eg self-esteem; emotional security), Family Processes (eg parenting practices and styles); and inherent predispositions, such as gender. The potential value of such a framework is that it can address negative or positive outcomes, and examine risk or protective factors, at the child/adolescent and family levels. Each variable of interest may be assessed independently, or the interaction of numerous factors, moderators and/or mediators, may be examined.
The investigation into the influence of community-related factors, teacher and peer relationships on individual and family processes, and developmental outcomes are also essential. Hence, for the purposes of the current study, a Community Processes dimension consisting of a number of core elements of social capital was added to the Process Model. Social capital consists of a small set of central features, including reciprocity, trust, and cooperation among members of a social network that aims to achieve common goals22. The concept can also be broken down into 'structural' and 'cognitive' social capital. Structural components or 'what we do' refer to roles, rules, behaviours, networks and institutions. Cognitive social capital or 'what we feel' describes the values, attitudes and beliefs that produce cooperative behaviour23. Although reviews investigating potential links between a range of social capital dimensions and mental health outcomes have revealed somewhat inconsistent findings24-26, social capital has been shown to play a role in the incidence and prevalence of mental health outcomes27,28.
The following variables from the Process Model were selected for use in this study (Fig1):
- Individual Process: self-esteem.
- Family Process: parental acceptance.
- Community Process: the elements of social capital at an individual level of participation in the local community and proactivity in a social context represented structural social capital; whereas, feelings of trust and safety, and neighbourhood connections represented cognitive social capital.
The outcome focus was internalising problems, specifically, anxiety and depressive symptoms. Internalising problems were selected as the focus of the study primarily because by 2030, depression is estimated to be one of the leading causes of disease10 and Australia's most recent National Survey of Mental Health and Wellbeing (2007)29 revealed that anxiety disorders were the most common mental health problem reported in adults, considerably more prevalent that affective disorders, such as depression, affecting 14% (1/7) and 6% (1/16) of adults, respectively; however, current rates for adolescent populations are unknown. Moreover, important groups in the Australian population (ie rural, remote, and Indigenous) were not included the 1997 National Survey1,30,31. Consequently, current prevalence rates of adolescent mental health problems from rural Australia, in particular internalising disorders such as anxiety disorders, are not known.
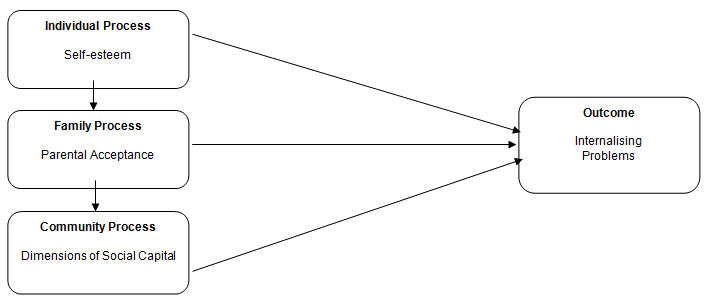
Figure 1: Selected variables to be investigated in the present study (self-esteem, parental acceptance, dimensions of social capital, and internalising problems).
Methods
In order to conduct research in government high schools, ethics approval was obtained from the South Australian Department of Education and Children's Services (DECS). A total of 28 non-government and government high schools were randomly selected within the Country Health South Australian area by each of the 7 existing health regions (Eyre Hills Mallee Southern, Mid North, Northern & Far Western, Riverland, South East, and Wakefield).
Each school was individually contacted and letters explaining the study were sent to the Heads (Principals) of each school. Eleven high schools agreed to participate, and from these a total of 560 Year 9 (2nd year of secondary school) students were invited to participate in the study. A total of 388 adolescents (208 females, 180 males) aged 13-15 years (mean age = 14.2 years) participated, a 69.3% response rate.
Information sheets and consent forms were provided to students and their parents and distributed by teachers. A list of South Australian organisations were also included to assist any parents who had possible concerns regarding their adolescent's behaviour, health, emotional wellbeing or issues regarding parenting. Students were also provided with a similar list. All participants were invited to enter a raffle for one of two $25 department store shopping vouchers. Once consent had been granted, students completed an online questionnaire at school under the supervision of a teacher, which took approximately 50 min to complete.
Measures
Self-esteem: The Rosenberg Self-Esteem Scale (RSES) was used to assess self-esteem32. The RSES is a 10-item self-report uni-dimensional measure of global self-esteem, consisting of statements related to overall feelings of self-worth or self-acceptance. Scores range from 0 to 30, with higher scores indicating higher self-esteem. Scores between 15 and 25 are considered to be within normal range; scores below 15 suggest low self-esteem. Example questions include: 'I feel that I am a person of worth' and 'I feel at least on an equal plane with others'. In this study the internal consistency alpha (α) = 0.86.
Parental Acceptance: Parental acceptance was assessed using the Acceptance subscale from the revised Child Report of Parent Behaviour Inventory (CRPBI)33. This revised measure contains ten items designed to assess the adolescents' perceptions of the extent to which they feel accepted by their parent/s. Adolescents responded on a 3 point Likert-type scale from 1 (= not like her/him) to 3 (= a lot like her/him) as to how well items described their parent/s. Example questions include: 'My Mother/Father is a person who ...makes me feel better after talking over my worries with her/him' and '...tells me how much s/he loves me'. Higher scores indicated greater levels of parental acceptance as perceived by the adolescent. In this study α = .89.
Social Capital: A total of four measurable components of social capital were assessed via 12 questions selected from the Social Capital Questionnaire34. A total of 6 questions each representing structural and cognitive social capital were included.
Structural Social Capital
Participation in the local community - Example questions included: 'Have you attended a local community event in the past 6 months (church fete, school concert)?' and 'Are you an active member of a local organisation or club (sport, craft, social club)?'.
Proactivity in a social context - Example questions included: 'Have you ever picked up other people's rubbish in a public place?' and 'If you need information to make a life decision, do you know where to find that information?'
Cognitive Social Capital
Feelings of trust and safety - Example questions included: 'If someone's car breaks down outside your home, do you invite them into your home to use your phone?' and 'Does your local community feel like home?'
Neighbourhood connection - Example questions included: 'If you were caring for a child and needed to go out for a while, would you ask a neighbour for help?' and 'When you go shopping in your local area are you likely to run into friends and acquaintances?'
Responses ranged from: 'Not at all/Not much' (=1) to 'Yes, definitely/Frequently' (=4). Total structural, cognitive and combined scores were calculated. Possible combined total scores ranged from 12 to 48. Both structural and cognitive total scores each ranged from 6 to 24. Higher scores indicated greater social capital as reported by the adolescents.
Internalising Symptoms: Internalising symptoms were measured with the Revised Child Anxiety & Depression Scales (RCADS)35. The RCADS is a 47 item self-report questionnaire, with 5 scales corresponding to separation anxiety disorder (SAD), social phobia (SP), generalized anxiety disorder (GAD), panic disorder (PD), obsessive compulsive disorder (OCD), and 10 items for major depressive disorder (MDD). The RCADS has been shown to have clinical and research utility for young Australians up to the age of 19 years36. Items were scored on a scale from 0 to 3 and a total internalising score was calculated based on the total score of the RCADS. Total possible scores ranged from 0 to 141 with higher scores indicating more severe levels of anxiety and depressive symptoms. Respondents were also categorised into one of 3 symptom severity categories based on their total RCADS score: mild: 0-46; moderate: 47-94; and severe: 95-141. Adolescents scoring within the moderate symptom category indicate symptoms above the clinical threshold35. In this study α = 0.87.
Results
Prior to analyses, variables were examined for accuracy of data entry, missing values and fit between the distributions and the evaluation of assumptions of multivariate analysis. All assumptions were considered to be met. Statistical analyses were completed using PASW Statistics 17.0 (SPSS Corp; Chicago, IL, USA: http://www.spss.com/). Relationships between all measures were investigated using Pearson product-moment correlations coefficients and associations between self-esteem, parental acceptance, social capital, and internalising problems were assessed using multivariate linear regressions.
As is shown, the mean level of self-esteem (M = 19.89) was considered in the 'normal' range (Table 1). A mean 'moderate' level of perceived acceptance (M = 22.56) by their parents was reported, and the total mean level of social capital (M = 21.47) was considered 'low' (a score of 22 and over was considered in the 'moderate' range). Based on the total mean score of the RCADS, the adolescents experienced a moderat' level of internalising symptoms (M = 47.09). No significant differences were found for males (M = 46.02, SD = 9.0) and females (M = 48.17. SD =11.2, t [386] = -.74, p = .42), two-tailed.
Based on the total mean score of the RCADS, 25% of adolescents experienced anxious and/or depressive symptoms ranging in severity from mild to severe (Table 2). Approximately 4% of adolescents reported experiencing severe symptoms.
The relationship between parental acceptance and self-esteem was moderate and positive (Table 3), indicating that adolescents who reported a higher level of parental acceptance also reported a greater level of self-esteem.
Table 1: Means (standard deviations) of all measures for adolescents
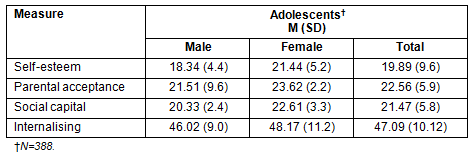
Table 2: Total prevalence rates (%) of severity of internalising symptoms
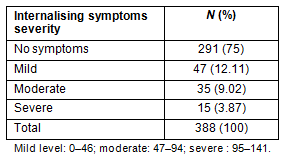
Table 3: Correlations of measures for adolescents

A moderate, negative relationship was found between parental acceptance and internalising symptoms, indicating that adolescents who reported that they felt accepted by their parents experienced lower symptoms of anxiety and depression. A moderate and negative relationship was found between self-esteem and the total internalising score, signifying that the greater level of self-esteem, the less internalising difficulties experienced by the adolescents.
The relationship between social capital and self-esteem were smaller, yet still significant and positive, indicating that adolescents who reported a greater sense of social capital within their communities, experienced higher self esteem.
The relationship between parental acceptance and social capital was very small and negative, yet significant, indicating that adolescents who perceived their parents to accept them reported higher social capital. The relationship between social capital and internalising problems was not significant.
Results from a linear regression demonstrated that parental acceptance was significantly related to greater self esteem, F (1, 386), = 70.47, β = .393, p = .000. Approximately 15% of the variance in self-esteem was explained by its relationship with parental acceptance (R2 = .15). Parental acceptance also predicted social capital, F (1, 386), = 11.68, β = .17, p = .001. Approximately 4% of the variance in self-esteem was explained by its relationship with social capital (R2 = .04).
Results from a linear regression demonstrated that social capital was significantly related to greater self esteem, F (1, 386), = 16.80, β = .22, p = .000. Approximately 4.2% of the variance in self-esteem was explained by its relationship with social capital (R2 = .04).
A simultaneous regression analysis was conducted to evaluate how much of the variance in internalising problems could be explained by the level self-esteem, parental acceptance and social capital. The linear contribution of the three predictors was significantly related to internalising problems F (3, 384) = 58.33, p = .000. Approximately 33% of the variance in internalising problems could be accounted for by the combination of predictors, R2 = .33.
Self-esteem and parental acceptance were the significant contributors to the prediction of internalising problems in the adolescent sample (β = .52, p = .000). Social capital was not a significant predictor of internalising problems.
Discussion
The present study contributes a small step towards building an evidence-base for the prevalence rates and determinants of internalising problems of adolescents from rural South Australia. Moreover, employing a multidimensional theoretical framework enables an investigation of the various determinants of mental health problems from individual, family and community domains.
Implications
Although the results from the present study represent adolescents from South Australia only, a number of implications are worth noting. For instance, based on the total mean score of the RCADS, the adolescents experienced a 'moderate' level of internalising symptoms. Further, approximately 13% of adolescents were considered to be above the clinical threshold, with 4% reporting experiencing severe symptoms. Although it is difficult to compare these findings with national figures (because young people were not included in the 2007 National Study, and anxiety disorders and young people from rural areas were not included in the 1997 National Study) such results must be of concern.
As a consecutive National Mental Health Survey is approaching, it is timely to highlight the importance of including as many Australians as possible from rural and remote areas, and in particular young people. This will produce a more accurate evidence-based representation of Australia's adolescent population, which will more effectively inform policy and ultimately facilitate implementation of relevant strategies.
Because this study was cross-sectional, causality cannot be demonstrated. Nonetheless, the findings demonstrate the importance of parental acceptance and may have implications for preventative and intervention programs for adolescents and their families. Not only did higher levels of parental acceptance predict lower levels of internalising problems, but they also predicted higher levels of self-esteem. Such findings may be applied to educate parents regarding the benefits of parental acceptance. To begin with, it is important to inform parents that 'acceptance' does not equate to agreeing with or accepting all of their adolescent's behaviours, but more to do with recognising, validating and demonstrating understanding of their experiences, thoughts and feelings, even during times of conflict.
Such an approach shows implicit and explicit interest and concern in the adolescent's perspective (which is especially important during times of conflict or disagreement), without creating a possible impression of disappointment. Thus, an adolescent is likely to internalise this acceptance, leading to a positive inner sense of self. This is particularly necessary when faced with the challenges inherent in the developmental years when an increase in autonomous functioning requires belief in one's self-worth.
The results of this study showed that higher levels of self-esteem decreased the probability of experiencing internalising symptoms. Teaching parents relevant strategies to understand and display acceptance may not only help to strengthen the relationship with their adolescent, but further enhance their self-esteem, which may help to prevent or delay possible anxious or depressive symptoms from emerging.
Limitations and suggestions
There are a number of limitations worth noting. First and foremost, South Australia is merely one region in Australia and no rural district in Australia is homogenous3,4 Heterogeneity within rural settings must be recognised as differences do exist. For instance, different rates of suicide have been acknowledged according to the degree of geographical remoteness13. Further, the findings from this study relied on adolescent self-reports and cross-sectional data. Thus, longitudinal data are required to establish causal relationships.
In the present study, social capital did not predict lower internalising problems. Perhaps such a result reflects the low social capital scores reported by the adolescents, rather than not being beneficial to mental health. It would be of interest to examine the outcomes of studies which report higher levels of social capital to explore the effects on mental health outcomes. However, social capital is such a multifaceted concept that it is not likely to be represented by any single measure37.
Exploring potential comparisons between the prevalence rates and determinants of mental health problems of rural and urban adolescents3,38 is also important. This is especially noteworthy when considering that potential differences between rural and urban populations may have been overlooked with the omission of rural populations included in national surveys3,30,31.
Additionally, it may be useful to examine the role of other factors included in the Process Model21 in the developmental outcomes of rural adolescents. For example, emotion regulation, parental autonomy granting, and/or a range of health indicators may be explored. By adopting a strengths-based approach, the determinants of mental health may also be investigated. This may include examining protective factors that could cushion the effects of adversity specifically to conditions which rural groups are more likely to encounter (eg the impact of drought)39.
Finally, progressing from investigating what factors contribute to the onset of a particular developmental outcome, to examining how and why, or the underlying processes involved would be worthwhile. For instance, examining the interplay between various theoretically-derived individual processes as mediators of the relationships between specific family and/or community process factors. For instance, the potential role emotional security plays in the relationship between parental punitiveness and GAD; whether other aspects of social capital (eg social trust) account for the relationship between self-efficacy and PD; or the impact that self-control plays in the relationship between perceived teacher or peer support and depressive symptoms.
Conclusions
It has been suggested that in many rural and remote communities in Australia, mental health issues may be something of a 'sleeping giant'3. The challenge facing health professionals is to provide practical and evidence-based programs designed to address and/or strengthen a range of individual, family, and community factors - before the 'giant' begins to stir. Although the pathways to internalising problems are complex, it is anticipated that the knowledge gained from the current study may assist in preventing the development of mental disorders in rural youth, where local mental health services are often limited or unavailable.
Acknowledgements
The authors acknowledge the cooperation from the Year 9 teachers and principals and sincerely thank the students and parents for their support and participation. The authors also thank Dr Victoria Gilliland for her assistance with the technical development of the online questionnaire. A version of this paper was presented at the Australian Psychological Society (APS) conference in Darwin, Australia in November 2009.
References
1. Boyd CP, Hayes L, Wilson RL, Bearsley-Smith C. Harnessing the social capital or rural communities for youth mental health: an asset-based community development framework. Australian Journal of Rural Health 2008; 16: 189-193.
2. Aisbett DL, Boyd CP, Francis KJ, Newnham K, Newnham K. Understanding barriers to mental health service utilization for adolescents in rural Australia. Rural and Remote Health 7: 624. (Online) 2007. Available: http://www.rrh.org.au (Accessed 2 February 2008).
3. Judd FK, Humphreys JS. Mental health issues for rural and remote Australians. Australian Journal of Rural Health 2001; 9: 254-258.
4. Fraser C, Judd F, Jackson H, Murray G, Humphreys J, Hodgins GA. Does one size really fit all? Why the mental health of rural Australians requires further research. Australian Journal of Rural Health 2002; 10: 288-295.
5. Boyd CP, Aisbett DL, Francis K, Kelly M, Newnham K, Newnham K. Issues in rural adolescent mental health in Australia. Rural and Remote Health 6: 501. (Online) 2006. Available: http://www.rrh.org.au (Accessed 2 February 2008).
6. Patterson C. Systematic overview of rural health research in Australia in the serial literature. Australian Journal of Rural Health 2008; 8: 286-293.
7. Kilkkinen A, Kao-Philpot A, O'Neil A, Philpot B, Reddy P, Bunker S et al. Prevalence of psychological distress, anxiety and depression in rural communities in Australia. Australian Journal of Rural Health 2007; 15: 114-119.
8. Hourihan F, Kelly B. National health policy: what does this mean for rural mental health research? Australian Journal of Rural Health 2006; 14: 49-50.
9. Australian Health Ministers' Advisory Council National Rural Health Policy Sub-committee, National Rural Health Alliance. Healthy Horizons Outlook 2003-2007. A Framework for Improving the Health of Rural, Regional and Remote Australians. Available: http://nrha.ruralhealth.org.au/cms/uploads/publications/hh_2003_03.pdf (Accessed 21 January 2010).
10. WHO. World Health Report 2001: Mental Health: New Understanding, New Hope. Geneva: WHO, 2001.
11. Mathers CD, Loncar D. Projections of global mortality and burden of disease from 2002 to 2030. PLoS Medicine 2006; 3(11): e442.
12. Eckert KA. Wilkinson D, Taylor AW, Stewart S, Tucker GR. A population view of mental illness in South Australia: broader issues than location. Rural and Remote Health 6: 541. (Online) 2006. Available: http://www.rrh.org.au (Accessed 12 November 2010).
13. Australian Institute of Health and Welfare. Australia's Health 2000: The Seventh Biennial Health Report of the Australian Institute of Health and Welfare. Canberra: AIHW, 2000. Available: http://www.aihw.gov.au/publications/index.cfm/title/5742 (Accessed 2 September 2007).
14. The National Rural Health Alliance, Mental health in Rural Areas Australia College of Health Service Executives. National Rural Health Alliance Suicide in rural Australia, 2009. (Online) 2009. Australian Institute of Health and Welfare. Available: http://nrha.ruralhealth.org.au/cms/uploads/factsheets/fact-sheet-14-suicide.pdf (Accessed 10 February 2010).
15. Kelly BJ, Stain HJ, Coleman C, Perkins D, Fragar L, Fuller J et al. Mental health and well-being within rural communities: the Australian Rural Mental Health Study. Australian Journal of Rural Health 2010; 18: 16-24.
16. Hodges CA, O'Brien MS, McGorry PD. headspace: National Youth Mental Health foundation: making headway with rural young people and their mental health. Australian Journal of Rural Health 2007: 15: 77-80.
17. Allan J. Determinants of mental health and well-being in rural communities: do we understand enough to influence planning and policy? Australian Journal of Rural Health 2010; 18: 3-4.
18. Australian Institute of Health and Welfare AIHW. Key national indicators of children's health, development and wellbeing: a picture of Australia's children. Cat. no. AUS 100. Canberra, ACT: AIHW, 2008.
19. Ambert A. The effect of children on parents. New York: Haworth, 1992.
20. Kerr M, Stattin H. What parents know, how they know it, and several forms of adolescent adjustment: further support for a reinterpretation of monitoring. Developmental Psychology 2000; 36: 366-380.
21. Papandrea K. Early childhood psychological resilience and family protective factors: the mediating role of self-control. Thesis. Adelaide, SA: The University of Adelaide, 2005.
22. Putnam R. Bowling alone: America's declining social capital. Journal of Democracy 1995; 6: 65-78.
23. Harpham T. Measuring the social capital of children. (Online) 2005. South Bank University. (Online) 2009. Available: http://www.dfid.gov.uk/ (Accessed 22 March 2008).
24. McKenzie K, Whitley R, Weich S. Social capital and mental health. British Journal of Psychiatry 2002; 181: 280-283.
25. Almedom AM. Social capital and mental health: an interdisciplinary review of primary evidence. Social Science & Medicine 2005; 61: 943-964.
26. De Silva MJ, McKenzie K, Harpham T, Huttly SRH. Social capital and mental illness: a systematic review. Journal of Epidemiology Community Health 2005; 59: 619-627.
27. Aneshensel CS, Sucoff CA. The neighbourhood context of adolescent mental health. Journal of Health Social Behaviour 1996; 37: 293-310.
28. Lundborg P. Social capital and substance use among Swedish adolescents - an explorative study. Social Science & Medicine 2005; 61: 1151-1158.
29. Henderson S, Andrews G, Hall W. The 2007 Australian National Survey of Mental Health and Wellbeing Survey. Australian and New Zealand Journal of Psychiatry 2009; 43: 591-593.
30. Beumont P. The mental health of young people in Australia: report by the National Mental Health Strategy. The Australian and New Zealand Journal of Psychiatry 2002; 36: 141.
31. Rajkumar S, Hoolahan B. Remoteness and issues in mental health care: experience from rural Australia. Epidemiologia e Psichiatria Sociale 13: 78-82. (Online) 2004. Available: http://www.rorrt.reachout.com.au/ (Accessed 22 March 2008).
32. Rosenberg M. Society and the adolescent self-image. Middletown, CT: Wesleyan University Press, 1989.
33. Schaefer E. Child's reports of parental behaviour: an inventory. Child Development 1965; 36: 413-424.
34. Bullen P, Onyx J. Measuring social capital in five communities. Journal of Applied Behavioral Science 2000; 36: 23-42.
35. Chorpita BF, Yim L, Moffit C, Umemoto LA, Francis SE. Assessment of symptoms of DSM-IV anxiety and depression in children: a revised child anxiety and depression scale. Behaviour Research and Therapy 2000; 38: 835-855.
36. de Ross RL, Gullone E, Chorpita BF. The Revised Child Anxiety and Depression Scale: a psychometric investigation with Australian youth. Behaviour Change 2002; 19: 90‐101.
37. Berry HL, Rickwood DJ. Measuring social capital at the individual level: personal social capital, values and psychological distress. International Journal of Mental Health Promotion 2000; 2: 35-44.
38. Quine S, Bernard D, Booth M, Kang K, Usherwood T, Alperstein G et al. Health and access issues among Australian adolescents: a rural-urban comparison. Rural and Remote Health 3: 245. (Online) 2003. Available: http://www.rrh.org.au (Accessed 22 March 2010).
39. Dean JG, Stain HJ. Mental health impact for adolescents living with prolonged drought. Australian Journal of Rural Health 2010; 18: 32-37.
