full article:
Rates of childhood and adolescent obesity have tripled over the past three decades, with a third of all children and adolescents in the USA currently overweight or obese1,2. Identifying those children most at risk and the environmental and geographic factors that contribute to this risk is critical to focussing prevention efforts.
Studies have identified geographic variation in overweight and obesity rates among children3-8. Many studies have found that children living in rural areas are more likely to be overweight or obese than their urban peers5,9-11. Based on an analysis of the 2003 National Survey of Children's Health for 47 757 children aged 10-17 years, and using the 2003 Urban Influence Codes to define rurality, Liu et al12found that overweight status was more prevalent among rural (16.5%) than urban children (14.3%) after adjusting for potential confounders. However, several studies have found no significant differences in weight status based on rural residence13-16.
Reasons for different rates of overweight and obesity among children based on geography are unclear. Prior research has not identified consistent patterns regarding factors such as diet quality or physical activity, which are often associated with place of residence and the built environment. Based on data from the 2007 National Survey of Children's Health, for youth aged 10-17 years (n=45 392) and adjusting for known confounders, Kasehagen et al17 found no association between neighborhood characteristics and youth physical activity within seven levels of Rural-Urban Commuting Areas (RUCAs) representing a continuum from isolated rural to dense urban communities. Joens-Matre et al6 and Moore et al18 found higher levels of physical activity among youth in rural, as compared with urban or suburban areas. In contrast, Shearer et al19 found higher rates of moderate to vigorous physical activity among low-income youth in urban settings, as compared to those in suburban or rural areas.
Access to healthy food may also differ between geographic regions. Based on a review of 54 studies published between 1985 and 2008, Larson et al20 found that residents of rural neighborhoods (as well as neighborhoods characterized by a high prevalence of low-income or minority residents) were most often affected by poor access to supermarkets and healthful food. Further, the authors found that neighborhood residents who had better access to supermarkets and limited access to convenience stores tended to have healthier diets.
The objective of the present study was to identify differences in body mass index (BMI), and overweight and obesity prevalence by urban-rural school location within small counties (total population less than 500 000), in order to identify types of communities that could most benefit from future interventions. Given inconsistent findings in the literature, an additional objective was to go beyond a dichotomous urban-rural analysis and identify differences in overweight and obesity rates among a more nuanced range of geographic subregions along the urban-rural continuum.
An observational study was conducted using FITNESSGRAM21 data collected from 5th, 7th and 9th grade students in public schools in California during 2010-2011, available through the California Department of Education. FITNESSGRAM data included height and weight as measured by school staff, date of birth, gender, ethnicity, and individual level eligibility for free or reduced price meals from the National School Lunch Program22,23 for all schools in the 42 counties. The sample included 204 597 5th, 7th and 9th grade students in 1976 schools in 42 Californian counties with total populations less than 500 000.
The FITNESSGRAM dataset was merged with the 2011 Public Elementary/Secondary School Universe Survey Data from the National Center for Educational Statistics Common Core of Data to include an urban-rural indicator24. The National Center for Educational Statistics dataset included an 'urban-centric locale' code (ULOCAL)25 for each school, consisting of four broad classifications and three subcategories within each classification, as follows:
- City: Territory inside an urbanized area and inside a principal city with a population of 250 000 or more ('large'); territory inside an urbanized area and inside a principal city with a population less than 250 000 and greater than or equal to 100 000 ('midsize'); territory inside an urbanized area and inside a principal city with population less than 100 000 ('small').
- Suburb: Territory outside a principal city and inside an urbanized area with population of 250 000 or more ('large'); territory outside a principal city and inside an urbanized area with population less than 250 000 and greater than or equal to 100 000 ('midsize'); territory outside a principal city and inside an urbanized area with population less than 100 000 ('small').
- Town: Territory inside an urban cluster that is less than or equal to 10 miles (16 km) from an urbanized area ('remote'), territory inside an urban cluster that is more than 10 miles and less than or equal to 35 miles (56 km) from an urbanized area ('distant'), territory inside an urban cluster that is more than 35 miles from an urbanized area ('fringe').
- Rural: Census-defined rural territory that is less than or equal to 5 miles (8 km) from an urbanized area, as well as rural territory that is less than or equal to 2.5 miles (4 km) from an urban cluster ('fringe'), more than 5 miles but less than or equal to 25 miles (40 km) from an urbanized area, as well as rural territory that is more than 2.5 miles but less than or equal to 10 miles from an urban cluster ('distant') or more than 25 miles from an urbanized area and also more than 10 miles from an urban cluster ('remote').
Centers for Disease Control and Prevention (CDC) growth charts were used to classify students as having a BMI at ³85th to <95th percentile (overweight) and ≥95th percentile (obese) for age and gender. The BMI data were cleaned using software developed by the CDC for detecting biologically implausible values, which resulted in the removal of 5224 cases based on biologically implausible values. An additional 59 cases were removed based on implausible age for grade values, and an additional 1474 cases were removed due to missing values for the ULOCAL variable. Multivariate analyses using a general linear model were conducted to compare differences in BMI between the geographic regions of the schools (city, suburb, town and rural) as well as the 11 ULOCAL subcategories; none of the schools were located in large cities. The percentage of students who were overweight and/or obese was compared by grade level, gender, and race/ethnicity across geographical regions using multivariate logistic regression models. Analyses were adjusted for student age, grade, gender, race/ethnicity (African-American, Asian, Hispanic, Indian/Alaskan, White, two or more races, or unknown), eligibility for free or reduced price meals, and clustering of students by school. When a stratified analysis was done, the variable of stratification (ie grade, gender, race/ethnicity) was not included among the covariates. When significant differences in BMI or prevalence of overweight or obesity were found between geographic regions, Tukey's method was applied to adjust for multiple comparisons at a 5% procedure-wise error rate. To evaluate whether the relationship of urban-rural status with the three dependent variables was different by grade, gender and race/ethnicity, the interaction of urban-rural status by each of the three predictors on each of the three dependent variables was examined (results not shown). Significant interactions were found for gender by urban-rural status with overweight as the outcome (p=0.03), and race/ethnicity by urban-rural status with obesity as the outcome (p=0.03). Although the remaining tests for interactions were not significant, results by grade, gender, and race/ethnicity are presented separately. The data were analyzed using Statistical Analytical Software v9.4 (SAS Institute; http://www.sas.com). A p-value at or below 0.05 was used to indicate statistical significance.
Ethics approval
The Institutional Review Board at the Public Health Institute evaluated the study and determined that it was not subject to review under the regulations found at 45 CFR part 46.
Nearly one-third of the sample of 204 597 students (31.8%) attended schools in cities; the remainder of the sample was distributed fairly equally among schools located in suburbs, towns and rural locations (Table 1). Nearly half (45.8%) of the students were Hispanic, while 50.6% were eligible for free/reduced price meals through the National School Lunch Program. There were differences in the proportion of students across geographic areas by grade level (p<0.0001), race/ethnicity (p<0.0001), and eligibility for free and reduced price meals (p<0.0001).
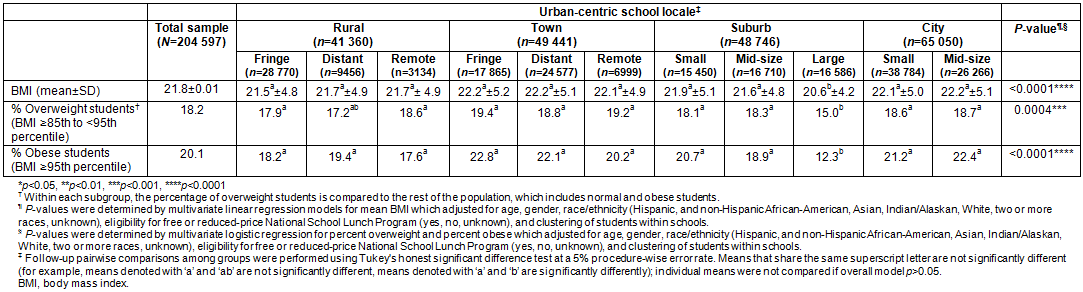
When all students were examined together, there was a significantly lower mean BMI among those in suburban schools compared with other areas, with no significant differences between students in schools located in cities, towns and rural areas (Table 2). For all students combined the prevalence of overweight status varied (p=0.01), with significantly lower prevalence for students in schools in suburbs compared to students in towns. Combined data for all students revealed that the prevalence of obesity also varied by urban-rural status (p<0.0001), with significantly lower prevalence for students in suburbs compared to cities, towns and rural areas (Table 2).
When data were examined by grade level, 5th grade students in suburban schools had a lower prevalence of obesity than those in cities and towns. Among 7th graders, students in suburban schools had a lower prevalence of obesity than students in schools in towns. Among 9th grade students, prevalence of overweight similarly varied by urban-rural status (p=0.02).
Among females, prevalence of overweight and obesity varied (p=0.006, p <0.0001, respectively), with suburbs having lower rates than towns and cities (Table 3). Among males, prevalence of obesity also varied (p<0.0001), with suburbs having lower rates than other areas.
Among whites, there were differences in prevalence of overweight and obesity by urban-rural status (p=0.01, p<0.0001, respectively), with suburbs having lower rates than towns (Table 4). Among Hispanics, the prevalence of obesity also varied by urban-rural status (p=0.001), with suburbs having lower rates than towns and cities.
In further urban-centric locale code sub-category analyses, large suburban areas showed lower rates of obesity for all grades combined compared to any other sub-category (Table 5). Variations in weight status were also seen when comparing large suburban groups to small or mid-size suburban groups.
Table 1: Descriptive characteristic of participating students included in the California FITNESSGRAM data, 2010-2011 by urban-rural status (N=204 597)?
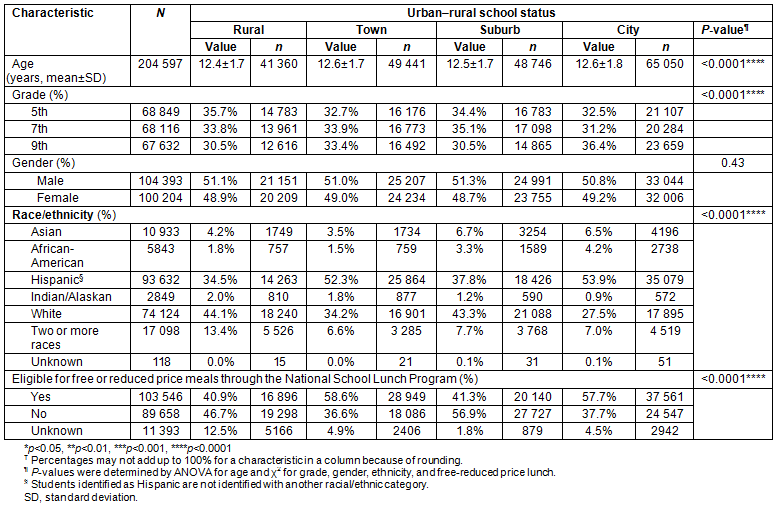
Table 2: Body mass index and overweight/obesity status by grade for students in the California FITNESSGRAM data, 2010-2011 by urban-rural status
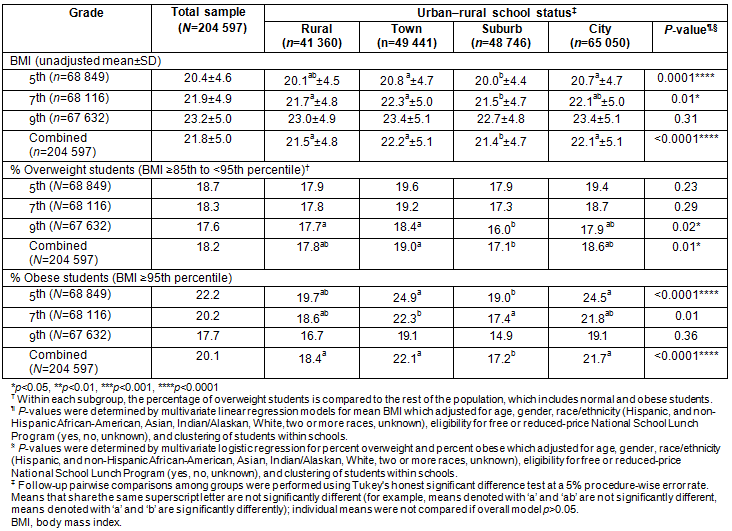
Table 3: Body mass index and overweight/obesity status by gender for students in the California FITNESSGRAM data, 2010-2011 by urban-rural status
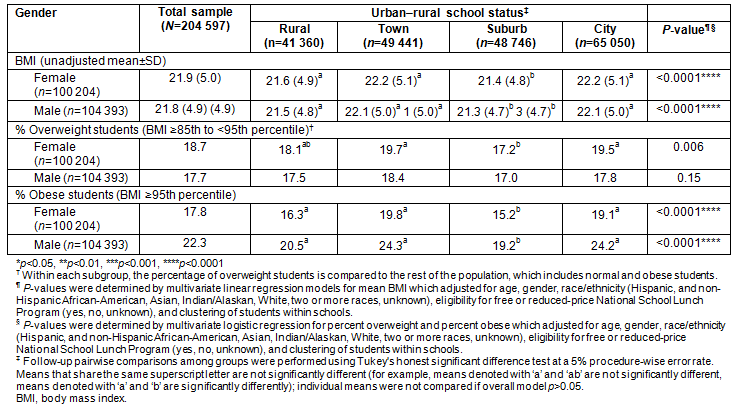
Table 4: Body mass index and overweight/obesity status by race/ethnicity for students in the California FITNESSGRAM data, 2010-2011 by urban-rural status
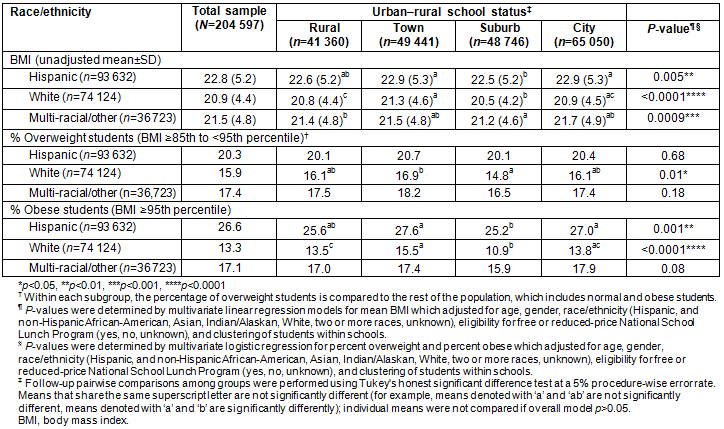
Table 5: Body mass index and overweight/obesity status for students included in the California FITNESSGRAM data, 2010-2011 by subcategories within each urban-centric status classification
Discussion
Overall, lower mean BMI and lower prevalence of overweight and obesity were found among students attending schools located in suburban areas, in particular large suburban areas. Students in rural schools had BMI and prevalence of overweight and obesity that were largely similar to students in schools located in towns and urban areas. The mean BMI differences (0.1-0.8 kg/m2) observed in this study between youth attending schools in suburbs and other areas is meaningful in light of the fact that school or community-based obesity prevention trials have been considered successful in achieving BMI decreases of similar magnitude26-29. When subgroups of students were examined, the lower prevalence of overweight and obesity appeared to be more driven by females than males, and more driven by Hispanics and non-Hispanic white students than those from other racial/ethnic backgrounds.
Relatively few other studies of children30,31 and adults32,33 have similarly found a lower prevalence of overweight and obesity in suburban areas. For example, the 2014 California Health Interview Survey for adolescents34 also found a lower prevalence of overweight and obesity in suburban areas. However, in this study, they sampled the entire state, including large urban areas, and participants self-reported their height and weight in contrast to the present study, which excluded these large urban areas and included measured height and weight. Bailey-Davis et al35 found lower rates among youth in suburban areas. Lewis et al36. found that children living in rural areas were at increased risk for overweight compared to children in urban areas. However, no difference was found between urban and suburban youth. In a study of Swedish schoolchildren, Sjöberg et al37 found that there were urban-rural differences for obesity prevalence in boys only, which is in contrast to the present study's findings of similar urban-rural differences for obesity for both genders. To the authors' knowledge, there is no research examining urban-rural differences for obesity prevalence by race/ethnicity. Further research should examine gender and racial/ethnic disparities and how these relate to urban and rural geographical differences.
It is unclear which aspects of large suburbs may be associated with lower BMI among students attending schools in those areas. Sandercock et al38 found that most studies reported no differences in physical activity among children in urban, rural and suburban environments. Lopez and Hynes39 note that research exploring associations between the built environment, physical activity, and overweight suggests that environmental factors characteristic of suburbs may be associated with decreased physical activity and an increased risk of being overweight. At the same time, however, Lopez and Hynes note that inner city populations tend to have higher rates of obesity and physical inactivity despite neighborhoods with excellent street connectivity and sidewalks. More research is needed to identify which aspects of the built environment promote physical activity40.
Access to healthy food may also differ between geographic regions; in particular, residents of suburban areas have been shown to have greater access to supermarkets and affordable healthful food compared to other areas41-43. Based on a review of 54 studies published between 1985 and 2008, Larson et al20 found that residents of low-income, minority, and rural neighborhoods are most often affected by poor access to supermarkets and healthful food.
Overall, the findings revealed lower rates of overweight and obesity among students attending schools in suburban areas and did not reveal higher rates of overweight and obesity among students attending schools in rural areas compared to towns or urban areas. In addition to refining how locations along the urban-rural spectrum are classified, further research using data collected over longer periods of time is needed to see if large suburban school or home location is associated with lower BMI and overweight and obesity in other states and geographic regions. Further research is also needed to identify the principal factors - including food access, transportation and other characteristics of the built environment - associated with differences in BMI and obesity in urban, suburban, town and rural areas.
This study has several strengths. It is based on a large sample size of over 200 000 students. The dataset contains data for virtually all 5th, 7th and 9th grade students attending public schools in California's 42 less populous counties. This study is important because it also identified differences in overweight and obesity at a more granular level than the typical binary urban-rural divide and identifies more specific geographic areas that require attention. By identifying lower rates of overweight and obesity in large suburban areas, the study also identifies a need for future research to identify what can be learned from large suburbs that may be informative for child obesity prevention.
The principal limitation of this study is the fact that urban-rural classifications are based on school location, which may not be the same classification as students' actual place of residence, as has been used in other studies1,5. This study is also limited by inability to control for other student-level factors, such as dietary intake or physical activity, that may contribute to differences in weight status. Further, although schools are provided guidance by the California Department of Education on how to conduct the weight and height measures reported as part of FITNESSGRAM, differences in the accuracy of measurements likely exist across schools. While attempts to minimize inaccurate measures were done by using the CDC algorithms for identifying implausible BMI measures, less obvious measurement errors could not be identified. This sample of 42 counties did not include any large urban areas. Further, differences in the designation of rural, urban and suburban areas present a another barrier to comparing findings from this and other studies31,44,45. However, the urban-centric locale code25 has been used in numerous studies relating to students and educational institutions46-48.
Students attending schools in suburban, especially larger suburban, areas appear to have a lower prevalence of overweight and obesity than their peers at schools in other geographic areas. Further research is needed to understand the principal factors associated with differences in weight status across urban, suburban, town and rural areas.
Acknowledgements
The authors wish to thank Virginia Gildengorin, PhD, with the Nutrition Policy Institute, University of California Division of Agriculture and Natural Resources, for her statistical contributions. This research was funded by CA4Health, a project of the Public Health Institute, with funding from the Centers for Disease Control and Prevention (#5U58DP003677-03). The findings and conclusions are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention.
References
1. Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of childhood and adult obesity in the United States, 2011-2012. Journal of the American Medical Association 2014; 311(8): 806-814. https://doi.org/10.1001/jama.2014.732
2. National Center for Health Statistics. Health, United States, 2011: with special feature on socioeconomic status and health. Hyattsville, MD: National Center for Health Statistics, 2012.
3. Shriver LH, Harrist AW, Hubbs-Tait L, Topham G, Page M, Barrett A. Weight status, physical activity, and fitness among third-grade rural children. Journal of School Health 2011; 81(9): 536-544. https://doi.org/10.1111/j.1746-1561.2011.00624.x
4. Davis AM, Boles RE, James RL, Sullivan DK, Donnelly JE, Swirczynski DL, et al. Health behaviors and weight status among urban and rural children. Rural and Remote Health (Internet) 2008; 8(2): 810. Available: http://www.rrh.org.au (Accessed 8 October 2014).
5. Davis AM, Bennett KJ, Befort C, Nollen N. Obesity and related health behaviors among urban and rural children in the United States: data from the National Health And Nutrition Examination Survey 2003-2004 and 2005-2006. Journal of Pediatric Psychology 2011; 36(6): 669-676. https://doi.org/10.1093/jpepsy/jsq117
6. Joens-Matre RR, Welk GJ, Calabro MA, Russell DW, Nicklay E, Hensley LD. Rural-urban differences in physical activity, physical fitness, and overweight prevalence of children. Journal of Rural Health 2008; 24(1): 49-54. https://doi.org/10.1111/j.1748-0361.2008.00136.x
7. Lutfiyya MN, Lipsky MS, Wisdom-Behounek J, Inpanbutr-Martinkus M. Is rural residency a risk factor for overweight and obesity for U.S. children? Obesity (Silver Spring) 2007; 15(9): 2348-2356. https://doi.org/10.1038/oby.2007.278
8. Singh GK, Kogan MD, van Dyck PC. Changes in state-specific childhood obesity and overweight prevalence in the United States from 2003 to 2007. Archives of Pediatrics & Adolescent Medicine 2010; 164(7): 598-607. https://doi.org/10.1001/archpediatrics.2010.84
9. Johnson JA, 3rd, Johnson AM. Urban-rural differences in childhood and adolescent obesity in the United States: a systematic review and meta-analysis. Childhood Obesity 2015; 11(3): 233-241. https://doi.org/10.1089/chi.2014.0085
10. Liu JH, Jones SJ, Sun H, Probst JC, Merchant AT, Cavicchia P. Diet, physical activity, and sedentary behaviors as risk factors for childhood obesity: an urban and rural comparison. Childhood Obesity 2012; 8(5): 440-448. https://doi.org/10.1089/chi.2011.0090
11. U.S. Department of Health and Human Services, Health Resources and Services Administration, Maternal and Child Health Bureau. The health and well-being of children in rural areas: a portrait of the nation 2011-2012. Rockville, MD: U.S. Department of Health and Human Services, 2015.
12. Liu J, Bennett KJ, Harun N, Probst JC. Urban?rural differences in overweight status and physical inactivity among US children aged 10?17 years. Journal of Rural Health 2008; 24(4): 407-415. https://doi.org/10.1111/j.1748-0361.2008.00188.x
13. Sandercock GR, Ogunleye A, Voss C. Comparison of cardiorespiratory fitness and body mass index between rural and urban youth: findings from the East of England Healthy Hearts Study. Pediatrics International 2011; 53(5): 718-724. https://doi.org/10.1111/j.1442-200X.2011.03354.x
14. Czajka K, Fiszer K, Kolodziej M. The relation between selected health behaviour and body mass index amongst adolescents living in urban and rural areas in south-western Poland. Roczniki Pa?stwowego Zak?adu Higieny 2013; 64(2): 135-141.
15. Cleland V, Hume C, Crawford D, Timperio A, Hesketh K, Baur L, et al. Urban-rural comparison of weight status among women and children living in socioeconomically disadvantaged neighbourhoods. Medical Journal of Australia 2010; 192(3): 137-140.
16. Peytremann-Bridevaux I, Faeh D, Santos-Eggimann B. Prevalence of overweight and obesity in rural and urban settings of 10 European countries. Preventive Medicine 2007; 44(5): 442-446. https://doi.org/10.1016/j.ypmed.2006.11.011
17. Kasehagen L, Busacker A, Kane D, Rohan A. Associations between neighborhood characteristics and physical activity among youth within rural-urban commuting areas in the U.S. Maternal and Child Health Journal 2012; 16(Suppl 2): 258-267. https://doi.org/10.1007/s10995-012-1188-3
18. Moore JB, Beets MW, Morris SF, Kolbe MB. Comparison of objectively measured physical activity levels of rural, suburban, and urban youth. American Journal of Preventive Medicine 2014; 46(3): 289-292. https://doi.org/10.1016/j.amepre.2013.11.001
19. Shearer C, Blanchard C, Kirk S, Lyons R, Dummer T, Pitter R, et al. Physical activity and nutrition among youth in rural, suburban and urban neighbourhood types. Canadian Journal of Public Health 2012; 103(9 Suppl 3): eS55-60.
20. Larson NI, Story MT, Nelson MC. Neighborhood environments: disparities in access to healthy foods in the U.S. American Journal of Preventive Medicine 2009; 36(1): 74-81. https://doi.org/10.1016/j.amepre.2008.09.025
21. Plowman SA, Meredith MD (Eds). Fitnessgram/Activitygram reference guide, 4th edn. Dallas, TX: The Cooper Institute, 2013.
22. Harwell MR, Maeda Y, Lee K. Replicating and extending White's (1982) meta-analysis of the relationship between SES and student achievement. In: Annual Meeting of the American Educational Research Association. San Diego, CA, 2004.
23. Sirin SR. Socioeconomic status and academic achievement: a meta-analytic review of research. Review of Educational Research 2005; 75(3): 417-453. https://doi.org/10.3102/00346543075003417
24. National Center for Education Statistics, Common Core of Data. Public elementary/secondary school universe survey data (Internet) 1986. Available: http://nces.ed.gov/ccd/pubschuniv.asp (Accessed 21 March 2017).
25. National Center for Education Statistics, Common Core of Data. Identification of rural locales. (Internet). Available: http://nces.ed.gov/ccd/rural_locales.asp (Accessed 21 March 2017).
26. Killen JD, Robinson TN, Telch MJ, Saylor KE, Maron DJ, Rich T, et al. The Stanford Adolescent Heart Health Program. Health Education Quarterly 1989; 16(2): 263-283.
27. Robinson TN. Reducing children's television viewing to prevent obesity: a randomized controlled trial. Journal of the American Medical Association 1999; 282(16): 1561-1567. https://doi.org/10.1001/jama.282.16.1561
28. Sallis JF, McKenzie TL, Conway TL, Elder JP, Prochaska JJ, Brown M, et al. Environmental interventions for eating and physical activity: a randomized controlled trial in middle schools. American Journal of Preventive Medicine 2003; 24(3): 209-217. https://doi.org/10.1016/S0749-3797(02)00646-3
29. de Silva-Sanigorski AM, Bell AC, Kremer P, Nichols M, Crellin M, Smith M, et al. Reducing obesity in early childhood: results from Romp & Chomp, an Australian community-wide intervention program. American Journal of Clinical Nutrition 2010; 91(4): 831-840. https://doi.org/10.3945/ajcn.2009.28826
30. Dunton GF, Kaplan J, Wolch J, Jerrett M, Reynolds KD. Physical environmental correlates of childhood obesity: a systematic review. Obesity Reviews 2009; 10(4): 393-402. https://doi.org/10.1111/j.1467-789X.2009.00572.x
31. Nelson MC, Gordon-Larsen P, Song Y, Popkin BM. Built and social environments associations with adolescent overweight and activity. American Journal of Preventive Medicine 2006; 31(2): 109-117. https://doi.org/10.1016/j.amepre.2006.03.026
32. Eberhardt MS, Pamuk ER. The importance of place of residence: examining health in rural and nonrural areas. American Journal of Public Health 2004; 94(10): 1682-1686. https://doi.org/10.2105/AJPH.94.10.1682
33. Ramsey PW, Glenn LL. Obesity and health status in rural, urban, and suburban southern women. Southern Medical Journal 2002; 95(7): 666-671. https://doi.org/10.1097/00007611-200295070-00002
34. UCLA Center for Health Policy Research. AskCHIS Body Mass Index - 4 level (teen only) compared by rural and urban - Claritas definition (4 levels). (Internet) 2014. Available: http://www.ask.chis.ucla.edu (Accessed 21 March 2017).
35. Bailey-Davis L, Horst M, Hillemeier MM, Lauter A. Obesity disparities among elementary-aged children: data from school-based BMI surveillance. Pediatrics 2012; 130(6): 1102-1109. https://doi.org/10.1542/peds.2012-0192
36. Lewis RD, Meyer MC, Lehman SC, Trowbridge FL, Bason JJ, Yurman KH, et al. Prevalence and degree of childhood and adolescent overweight in rural, urban, and suburban Georgia. Journal of School Health 2006; 76(4): 126-132. https://doi.org/10.1111/j.1746-1561.2006.00080.x
37. Sjöberg A, Moraeus L, Yngve A, Poortvliet E, Al-Ansari U, Lissner L. Overweight and obesity in a representative sample of schoolchildren - exploring the urban-rural gradient in Sweden. Obesity Reviews 2011; 12(5): 305-314. https://doi.org/10.1111/j.1467-789X.2010.00838.x
38. Sandercock G, Angus C, Barton J. Physical activity levels of children living in different built environments. Preventive Medicine 2010; 50(4): 193-198. https://doi.org/10.1016/j.ypmed.2010.01.005
39. Lopez RP, Hynes HP. Obesity, physical activity, and the urban environment: public health research needs. Environmental Health 2006; 5: 25. https://doi.org/10.1186/1476-069X-5-25
40. Sallis JF, Glanz K. The role of built environments in physical activity, eating, and obesity in childhood. The Future of Children 2006; 16(1): 89-108. https://doi.org/10.1353/foc.2006.0009
41. Talukdar D. Cost of being poor: retail price and consumer price search differences across inner-city and suburban neighborhoods. Journal of Consumer Research 2008; 35(3): 457-471. https://doi.org/10.1086/589563
42. Ver Ploeg M (Ed.). Access to affordable and nutritious food: measuring and understanding food deserts and their consequences: report to Congress. Washington, DC: U.S. Department of Agriculture, 2010.
43. Walker RE, Keane CR, Burke JG. Disparities and access to healthy food in the United States: a review of food deserts literature. Health & Place 2010; 16(5): 876-884. https://doi.org/10.1016/j.healthplace.2010.04.013
44. Black JL, Macinko J. Neighborhoods and obesity. Nutrition Reviews 2008; 66(1): 2-20. https://doi.org/10.1111/j.1753-4887.2007.00001.x
45. Feng J, Glass TA, Curriero FC, Stewart WF, Schwartz BS. The built environment and obesity: a systematic review of the epidemiologic evidence. Health & Place 2010; 16(2): 175-190. https://doi.org/10.1016/j.healthplace.2009.09.008
46. Patel AI, Chandran K, Hampton KE, Hecht K, Grumbach JM, Kimura AT, et al. Observations of drinking water access in school food service areas before implementation of federal and state school water policy, California, 2011. Preventing Chronic Disease 2012; 9: E121. https://doi.org/10.5888/pcd9.110315
47. Keigher A. Teacher attrition and mobility: results from the 2008-09 Teacher Follow-Up Survey (NCES 2010-353). Washington, DC: U.S. Department of Education, National Center for Education Statistics, 2010.
48. O'Donnell K. Parents' reports of the school readiness of young children from the National Household Education Surveys Program of 2007 (NCES 2008-051). Washington, DC: U.S. Department of Education, National Center for Education Statistics, 2008.

