Inequity in the geographic distribution of physicians, that is, a concentration of physicians in urban areas and shortage in rural areas, is a globally recognised social problem1. In Japan, redressing the maldistribution is considered an issue of high political priority, and various policies have been enacted by the national and local governments2. The diffusion of medical schools to rural areas and an expansion of medical school intakes have been facilitated by the government-led 'one-prefecture-one-medical-school' policy since the 1950s3. The national and local governments have built and managed public clinics and hospitals in rural areas2. These governments also founded a medical school solely for producing rural doctors (Jichi Medical University)4-6, and have expanded the 'rural sub-quota' among medical schools since 20062,6. In spite of the apparent successes of some of these policies2, the geographic distribution of physicians has not become more equitable7-9. Rather, it appears to have been exacerbated since 200410,11.
Some factors related to physicians are known to increase the probability of their rural recruitment1,12, including: rural upbringing13-15, graduation from a rural medical education programs5,16, having a specialty related to primary care17,18 and early-career rural exposure19,20. These findings are based largely on studies that investigated the characteristics of rural physicians compared with those of urban physicians. Studies focussing on the migration of physicians and analysing the flow pattern, however, are quite limited21-24. Studies that incorporate the concept of 'distance' in the analysis of flow are especially scarce.
Distance is presumably an important determinant in physicians' choice of location. To a physician who lives in a city, for example, the psychological barrier to moving to a rural area would be different between a rural town in the vicinity of the city, and a town which is similarly rural but is in a remote place. Thus, for the purpose of recruiting physicians to underserved areas, taking distance into account may be essential.
In addition, associations between the characteristics of physicians and their migration patterns are not well known. Past studies have agreed that younger physicians are more likely to move than older physicians21,22,24, but these studies are inconsistent regarding whether male physicians are more mobile than female physicians24, or vice versa21,22. Moreover, which characteristics of physicians increase the probability of long-distance migration, a necessary condition for recruiting in remote areas, are unknown.
These important pieces of evidence may be the basis for effective planning of workforce policies for medically underserved areas. When attracting physicians to rural and remote areas, policy-makers need to know which types of physicians are most likely to migrate to such areas. These high-mobility physicians should be a target of political intervention. Identification of physicians who are potentially mobile to rural and remote areas requires analysis of physician migration incorporating data on distance, and this has rarely, if ever, been done.
In this study, therefore, the flow of all the clinical physicians in Hiroshima Prefecture, Japan, was analysed with particular attention to migration to rural and distant places. Effective workforce policies for rural and remote areas will then be discussed.
Physician data derived from the Physician Census in 2002 and 2008 was used, provided by the Ministry of Health, Labour and Welfare with permission to use the data for research purposes. All those who hold a physician license in Japan are obliged to register in the Census. Among registered license holders, only those whose main jobs were 'practice' and affiliations were 'clinics' or 'hospitals' (91.1% of all the license holders) were recognised as 'physicians' in this study. A cohort of physicians (n=4268) who worked in Hiroshima in both 2002 and 2008 was extracted from the whole physician data.
Population data were derived from the Population and Population Dynamics Based on the National Basic Resident Register 2002-200825. Japan has three levels of government: municipal, prefectural and national. Municipality- (ward of large city, city, town and village) level population in Hiroshima Prefecture was extracted from the whole data25. Because many of the municipalities were merged during the period under consideration, the geographic border of municipalities in 2008 was applied to municipalities in earlier years so that the 2008 border was fixed throughout the period, both in population and physician data.
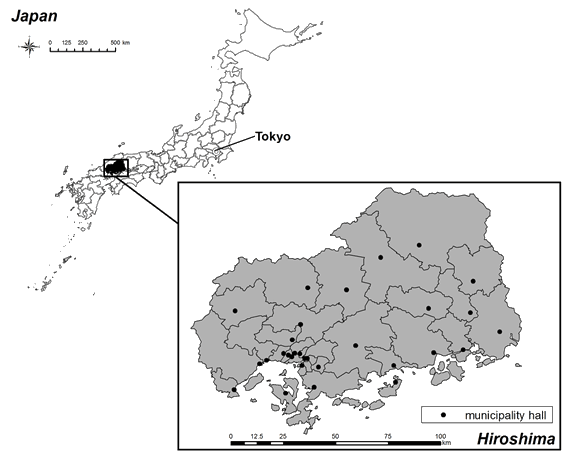
Figure 1: Hiroshima prefecture and its municipalities.
A network analysis was performed (ie the shortest travel-path between two locations on a road network, including highways, was established) to find the travel distance (in min) by car from the location of each municipal hall. Among the 30 municipalities in Hiroshima, the distances of all the combinations (435 patterns) in two municipalities were measured. The travel time was calculated using geographic information system software ArcGIS v10.0 (ESRI; Japan) and ArcGIS Data Collection Road Network 2011 (ESRI; Japan). In the Road Network, driving speeds of all the segments of the roads are classified into 42 categories depending on the following four variables: (i) road type (highway, national etc); (ii) road width; (iii) road density in the surrounding area; and (iv) legal upper limit velocity of the segment.
Two data sets were created. One was the physician cohort discussed, where the physician data were connected to distance and demographics of municipalities. The other was the list of combinations (870 patterns) of the two municipalities which include data on the number of physicians in both municipalities, the number of moved physicians in the period, the demographics of both places and the distance. Based on this municipal dataset, the numbers of moved physicians were classified into five categories of distance (<20, 20-40, 40-60, 60-80, >80 min). Because the number of moved physicians changes in proportion to the population size of the original municipality and that of the destination, the population-adjusted number of moved physicians was calculated as (number of moved physicians * 1010) / (original population * destination population).
Migration patterns were classified into three categories: to rural areas, to urban areas, and internal. Migration to rural areas was defined as the movement to a municipality where population density is more than 300 persons/km2 lower than the original municipality. Migration to urban areas was the movement to municipality with population density more than 300 persons/km2 higher than the original place. Internal migration was the movement between areas whose difference in population densities is less than 300 persons/km2. These definitions were based on the assumption that the gap in rurality between two places is more important in a physician's decision-making of migration than whether the destination is categorised 'rural' or 'urban', by a certain fixed criteria made for the purposes of the research. That is, physicians in a metropolitan city may have a psychological barrier to moving to middle-sized cities to a similar extent that physicians in the middle-sized cities feel a barrier to going to small towns.
Based on the cohort dataset, cross-table analysis was conducted comparing the migration rate between male and female physicians. Similar cross-table analysis was conducted in terms of a physician's age (≤40 or >40 years) and affiliation (clinic or hospital). With regard to physicians who migrated, the difference of the moved distance was compared with the median test between the two categories of sex, age, and institution. The median test was used because of the non-parametric distribution of distance data among the subjects. Finally, a logistic regression analysis was conducted to evaluate the predictive power of each characteristic of physicians (sex, age, or institution) for migration to rural areas or migration to distant areas, adjusted for other characteristics. The distant area in this analysis was defined as a municipality which is 70 min or more distant from the original municipality. The population density of the original municipality was also incorporated in the regression model as a covariate. This was in order to avoid confounding the results because, by definition in this study, physicians in the most urban municipality cannot move to urban areas and those in the most rural municipality cannot move to rural areas.
Statistical analyses were carried out using SPSS for Windows v18.0 (www.spss.com) and p-values < 0.05 were considered statistically significant.
The study was approved by the Ethics Committee of Epidemiological Studies, Hiroshima University (#Epidemiology-332).
The total population in Hiroshima Prefecture was 2.86 million, the area was 8479 km2, the number of physicians was 6074, and the number of physicians per 100 000 population was 211.7. Basic statistics for the 30 municipalities in Hiroshima Prefecture are shown (Table 1). In addition, the statistics of the 4268 physicians in the cohort are shown (Table 2). Between 2002 and 2008, 24.8% of physicians crossed municipal borders, and among the movers, 82.7% moved either to urban or to rural areas. Of the movers, 66.6% moved distances that were less than a 60 min drive.
Association between distance and the number of movers is shown (Fig2). Adjusted for populations of both original and destination municipalities, the number of migrated physicians decreased as the distance increased. This holds true in both directions: migration to urban areas, and migration to rural areas.
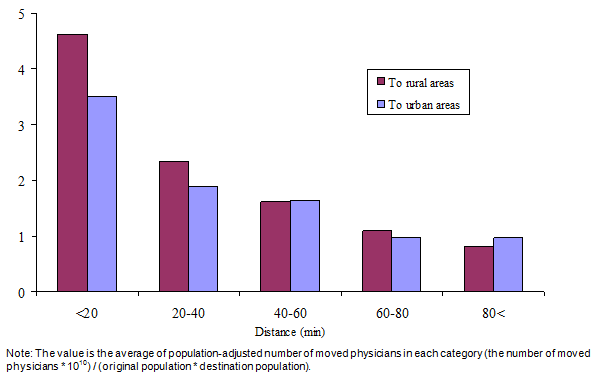
Figure 2: Average number of moved physicians according to distance.
The characteristics of physicians and their relationship with the migration rate are shown (Table 3). In this cross-table analysis, female physicians were found to be more likely to move than male physicians. Physicians whose ages were less than 40 years were 3.8 times (66.9/17.4%) more likely to move than those who were 40 years old or older. Hospital physicians had a 10.8 times (42.1/3.9%) higher migration rate than clinic physicians. Even when focusing on migration to rural areas, similar results were obtained (Table 4). Female, younger, and hospital physicians were more mobile than male, older, and clinic physicians.
Characteristics of physicians and their relationship with moved distance are shown (Table 5). Male and younger physicians moved a longer distance than female and older physicians. There was no difference observed in the distance between hospital and clinic physicians.
Results of multivariate analysis on factors that associate with migration to rural areas are shown (Table 6). Adjusted for age and affiliation of physicians, the statistical significance of females' higher mobility to rural areas disappeared. Similar to the results of the univariate analysis, younger age was a significantly positive predictor of migration to rural areas. Affiliation with hospital was also a strong positive predictor of rural migration.
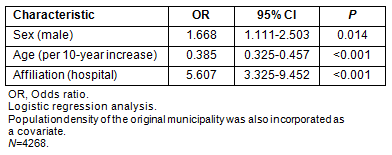
The results of the multivariate analysis with regard to moving a long distance (>70 min) are shown (Table 7). Male physicians were more likely to move a long distance. Both younger age and affiliation with hospital were positively associated with moving a long distance.
Table 1: Characteristics of municipalities
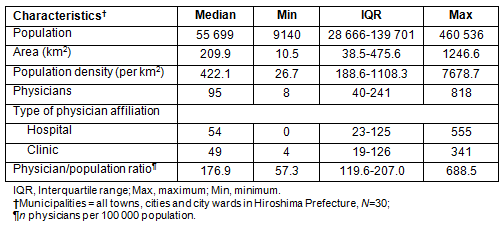
Table 2: Characteristics of physicians
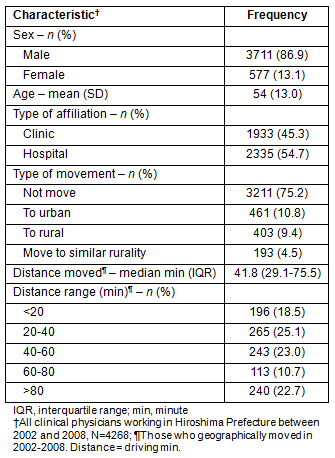
Table 3: Characteristics of physicians and movement
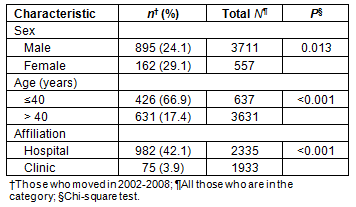
Table 4: Characteristics of physicians and movement to rural areas
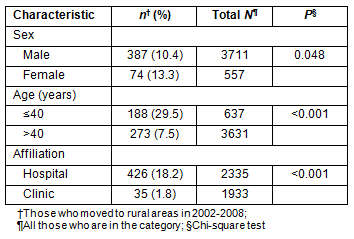
Table 5: Physician characteristics and distances moved
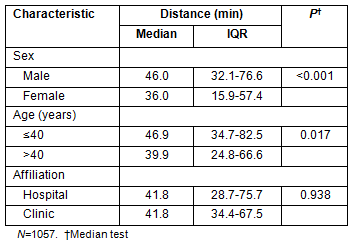
Table 6: Physician characteristics associated with moving to rural areas (multivariate analysis)
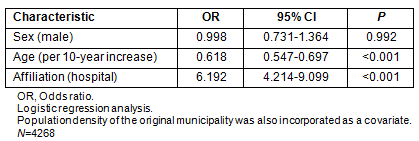
Table 7: Physician characteristics associated with a travel distance of 70 min or more (multivariate analysis)
Discussion
In Hiroshima Prefecture, a quarter of all physicians experienced migration by crossing municipal borders in the six-year period. The migration occurs more frequently as the distance between municipalities becomes shorter. Younger and hospital physicians were more likely to move than older and clinic physicians, and these types of physicians also are more mobile to rural areas than the others. In addition to young, and hospital physicians, male physicians moved a greater distance than their female counterparts.
Whether physicians or not, people are naturally attached to a place that is familiar. It is thus reasonable to expect that the movement of physicians takes place more often between places in close proximity. Even when physicians move to rural places, they would be more likely to move to near-by rural areas. The results of this study support this assumption. The number of movements decreased in proportion to the distance between the two areas.
The finding that the migration rate and migration distance decrease as physicians become older is consistent with the results of past studies in Japan24 and the USA21,22. This is also understandable when the usual career path and life cycle of physicians are taken into account. Physicians study and train in several places before becoming full-fledged clinicians. After acquiring a substantial amount of experience, knowledge and skill, they settle in a position with high responsibility. Moreover, early-career physicians are less likely to have a family, or if do, the children would be too young for higher education. It is thus easier for these physicians to move than older physicians.
Japan's unique health economic system explains the hospital physician's higher mobility compared with clinic physicians. Japanese physicians are usually employed by hospitals for 10 to 20 years after graduating from medical school, accumulating personal capital, and then starting up their own private practice at a clinic26. According to census data, only 3% of hospital physicians are business owners, while 74% of clinic physicians are business owners27. Making the transition from a hospital employee to clinic owner, the income of the average physician doubles28. Clinic physicians who have made a substantial initial investment will aim to recover it from the income of their private practice and are, therefore, unlikely to move. It is thus quite difficult to recruit clinic physicians to rural and remote areas.
Female sex was a facilitating factor of migration in the univariate analysis, but not in the multivariate analysis. The reason for this inconsistency is probably the age distribution of female physicians, which was younger than that of the male physicians (average of 49.8 years and 54.6 years, respectively, according to the 2008 data). Migration to a distant place was associated with male rather than with female sex in the multivariate analysis. The reason for this could be that female physicians tend to move without their families, choosing places within commuting distance of their homes, while male physicians move with their families. The explanation for this difference may be the traditional practice of the working places of husbands influencing where the family lives.
Limitations
There are some limitations to this study. Because the findings of this study are embedded in Japan's unique healthcare system, they should be applied to other countries with caution. The definitions of 'movement to rural' and 'movement to distance places' are unique to Japan and cannot be applied to other countries, particularly continental countries such as Australia and Canada. The physician data in this study did not include information on clinical specialty. Specialty data was omitted when extracting Hiroshima physician data from the whole Physician Census data because of the low reliability of the specialty information. In Japan, there is no regulation on professing a specialty and any physician can be registered in the Census as any specialist. Moreover there is no specialty category that indicates primary care in the Census because Japan has no primary care discipline comparable to family medicine in the USA29-31. It is thus difficult in this study to show the difference in migration patterns between primary care and non-primary care physicians.
Another limitation is that physicians who moved in or out of Hiroshima Prefecture during the study period have not been included in the data. It is probable that such physicians were younger than those within the prefecture and thus the association between greater moved distance and younger age observed in this study may be underestimated. Future studies on physician flow are needed that include the whole of Japan. In addition, there may have been physicians who moved more than once during the study period and such plural movements were not taken into consideration.
Health workforce policies, in trying to redress geographic maldistribution of physicians, need to incorporate the known predictors of rural recruitment, such as physicians with rural background12-15, primary care17,18, rural medical education4,5,32, and early-career rural exposure19,20. Physicians who have these characteristics should be the target of political intervention to attract them work in rural areas. In addition, incorporating the migration predictors shown in this study (ie young physicians, hospital physicians, and physicians in nearby areas) would make such policies more effective in Japan. With regard to policies relating to attracting physicians to remote areas, targeting male physicians may be most effective. By combining the predictors of rural practice and those of migration, workforce policies would be able to set an appropriate target and make effective interventions to attract physicians to rural and remote areas.
Acknowledgements
The Ministry of Education, Culture, Sports, Science and Technology (Tokyo, Japan) and Satake Education and Research Fund (Hiroshima, Japan) sponsored this research. The software used in this study was supplied by the Higher Education Grant Program of ESRI Japan Corp.
References
1. World Health Organization. Increasing access to health workers in remote and rural areas through improved retention: global policy recommendations. Geneva: WHO, 2010.
2. Matsumoto M, Inoue K, Kajii E, Takeuchi K. Retention of physicians in rural Japan: concerted efforts of the government, prefectures, municipalities and medical schools. Rural and Remote Health 10(2): 1432. (Online) 2010. Available: www.rrh.org.au (Accessed 1 May 2012).
3. Asano N, Kobayashi Y, Kano K. Issues of intervention aimed at preventing prospective surplus of physicians in Japan. Medical Education 2001; 35(5): 488-494.
4. Inoue K, Hirayama Y, Igarashi M. A medical school for rural areas. Medical Education 1997; 31(6): 430-434.
5. Matsumoto M, Inoue K, Kajii E. Contract-based training system for rural physicians: follow-up of Jichi Medical University graduates (1978-2006). Journal of Rural Health 2008; 24(4): 360-368.
6. Matsumoto M, Inoue K, Takeuchi K. Quality of care in Japan: an additional strategy. Lancet 2011; 378(9807): e17.
7. Kobayashi Y, Takaki H. Geographic distribution of physicians in Japan. Lancet 1992; 340(8832): 1391-1393.
8. Matsumoto M, Inoue K, Bowman R, Noguchi S, Toyokawa S, Kajii E. Geographical distributions of physicians in Japan and US: Impact of healthcare system on physician dispersal pattern. Health Policy 2010; 96: 255-261.
9. Toyokawa S, Kobayashi Y. Increasing supply of dentists induces their geographic diffusion in contrast with physicians in Japan. Social Science & Medicine 2010; 71(11): 2014-2019.
10. Toyabe S. Trend in geographic distribution of physicians in Japan. International Journal of Equity for Health 2009; 8: 5.
11. Tanihara S, Kobayashi Y, Une H, Kawachi I. Urbanization and physician maldistribution: a longitudinal study in Japan. BMC Health Services Research 2011; 11: 260.
12. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77(8): 790-798.
13. Dunbabin JS, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3(1): 212. (Online) 2003. Available: www.rrh.org.au (Accessed 1 May 2012).
14. Matsumoto M, Inoue K, Kajii E. Characteristics of medical students with rural origin: implications for selective admission policies. Health Policy 2008; 87(2): 194-202.
15. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11(6): 277-284.
16. Rabinowitz HK. Recruitment, retention, and follow-up of graduates of a program to increase the number of family physicians in rural and underserved areas. New England Journal of Medicine 1993; 328(13): 934-939.
17. Cullison S, Reid C, Colwill JM. Medical school admissions, specialty selection, and distribution of physicians. JAMA 1976; 235(5): 502-505.
18. Bowman R. The World of Rural Medical Education. (Online) no date. Available: http://www.ruralmedicaleducation.org (Accessed 1 November 2011).
19. Bowman RC, Penrod JD. Family practice residency programs and the graduation of rural family physicians. Family Medicine 1998; 30(4): 288-292.
20. Matsumoto M, Inoue K, Kajii E. Policy implications of a financial incentive programme to retain a physician workforce in underserved Japanese rural areas. Social Science & Medicine 2010; 71(4): 667-671.
21. Vanasse A, Ricketts TC, Courteau J, Orzanco MG, Randolph R, Asghari S. Long term regional migration patterns of physicians over the course of their active practice careers. Rural and Remote Health 7(4): 812. (Online) 2007. Available: www.rrh.org.au (Accessed 1 May 2012).
22. Ricketts TC, Randolph R. The diffusion of physicians. Health Affairs 2008; 27(5): 1409-1415.
23. Ricketts TC, Randolph R. Urban-rural flows of physicians. Journal of Rural Health 2007; 23(4): 277-285.
24. Inoue K, Matsumoto M, Toyokawa S, Kobayashi Y. Transition of physician distribution (1980-2002) in Japan and factors predicting future rural practice. Rural and Remote Health 9(2): 1070. (Online) 2009. Available: www.rrh.org.au (Accessed 1 May 2012).
25. Ministry of Internal Affairs and Communications. Jumin kihon daichou jinkou [Population and Population Dynamics Based on the National Basic Resident Register 2002-2008]. Tokyo: MIAC, 2002-2008.
26. Ikegami N, Campbell JC. The art of balance in health policy: maintaining Japan's low-cost, egalitarian system, Japanese edn. Tokyo: Chuko-shinsyo, 1996.
27. Ministry of Health Labour and Welfare. Ishi Shikaishi Yakuzaishi Chosa [The National Physician Census 2008]. Tokyo: MHLW, 2009 (in Japanese).
28. Ministry of Health Labour and Welfare. Iryo-keizai jittai chosa no houkoku [Report on current healthcare economics]. Tokyo: MHLW, 2007 (in Japanese).
29. Ban N, Fetters MD. Education for health professionals in Japan - time to change. Lancet 2011; 378(9798): 1206-1207.
30. Hashimoto H, Ikegami N, Shibuya K, Izumida N, Noguchi H, Yasunaga H et al. Cost containment and quality of care in Japan: is there a trade-off? The Lancet 2011; 378(9797): 1174-1182.
31. Shibuya K, Hashimoto H, Ikegami N, Nishi A, Tanimoto T, Miyata H et al. Future of Japan's system of good health at low cost with equity: beyond universal coverage. Lancet 2011; 378(9798): 1265-1273.
32. Matsumoto M, Inoue K, Kajii E. Long-term effect of the home prefecture recruiting scheme of Jichi Medical University. Rural and Remote Health 8(3): 930. (Online) 2008. Available: www.rrh.org.au (Accessed 1 May 2012).


