Introduction
As the workforce in rural general practice in New Zealand changes, with fewer and older GPs serving more patients1,2, more female and part-time GPs making up the workforce3, after hours services, seen as a burden for many years, are under pressure to change4. This is an international problem and many solutions have been sought5.
In urban New Zealand communities there has been a development of after hours clinics run by either a co-operative of GPs or by doctors with a special interest in out of hours care. Increasingly rural communities close to urban centres have joined these out of hours co-operatives to the extent that many patients have to travel for up to an hour to access services in the evening or weekends. The cost of accessing out of hours care has proved prohibitive for some patients with charges of up to NZ$100 not being uncommon6. Consequently in urban communities many patients chose to attend a hospital emergency department for conditions which could be managed in the community. In other countries the concept of nurse run walk-in-centres have been developed and have provided a useful adjunct to general practice and emergency department care6.
In rural areas of New Zealand a variety of solutions are emerging. In communities where the health board has a small rural hospital the GPs may hand over care at nights to the hospital - which is staffed by nurses and medical officers employed by the District Health Board. In other communities the GPs continue to provide a traditional 24 hours a day, 7 days a week service using a roster of local GPs, sometimes merging with other regional centres. Where there are insufficient GPs willing to provide this care, patients may be directed to a larger regional centre or, in some towns, a nurse triage system has been set up incorporating either practice nurses or community nurses employed by a health board.
Setting
Opotiki is a rural town serving a district of 9200 people in the Eastern Bay of Plenty in the North Island of New Zealand. The nearest accident and emergency clinic is 55 km distant in Whakatane. The district is geographically distinct from surrounding areas and has a high Maori population and high levels of deprivation7. Patients seeking after hours care call for an ambulance, call or attend the Community Health Centre staffed by members of the Opotiki Independent Nursing Service (OPINS) (funded by the Bay of Plenty District Health Board), or present to a private GP clinic held each morning and evening during weekends and public holidays. Telephone enquiries to the on-call GP are directed to the Opotiki Community Health Centre and are triaged by OPINS. The community health centre has 4 GP beds and 2 maternity beds and an assessment room. The service described developed when one GP clinic closed leaving three full time GPs to share the after hours workload. The town is also served by a St John's Ambulance Service that has a single paid officer working from 0900 to 1700 Monday to Friday. After hours calls are covered by volunteers.
The aim of this study is to report on the initiative in a rural New Zealand community to meet the needs for after hours care with a mixture of nurse triage/treatment, general practice clinics and a volunteer ambulance service. The study also aimed to identify the amount of after hours care generated over a period of 4 weeks by a well defined rural community.
Methods
During the month of May 2007 all patient encounters were recorded by the ambulance and nursing services and GPs who supplied after hours care, defined as care provided between 1700 and 0830 Monday to Friday and between 1700 Friday and 0830 Monday, over weekends and public holidays. To avoid duplication, ambulance services excluded patients who were referred after GP or nurse assessment. Data collected included details of patient demographics, time of encounter, reason for encounter and outcome in terms of referral or treatment. These were recorded on specifically designed data sheets that had been developed by the lead author and piloted in the out-of-hours nursing service and one GP clinic prior to the study. Staff also recorded whether the patient had self-referred or if they had been referred by other professionals.
Forms detailing the results were collected weekly and collated into an Excel spreadsheet by a research worker. The results were analysed using standard Microsoft Excel tools.
Results
Two hundred and four patients were seen after hours in the month: 90/204 (44%) by the GPs, 92/204 (45%) by the nurses and 22 (11%) by the ambulance staff. Fifty-six per cent were male. In total, 137/204 (67%) of patients seen were Maori, 28% were New Zealand European, 3% were from other ethnic groups and 2% had no ethnicity recorded.
Table 1: Outcome of encounter
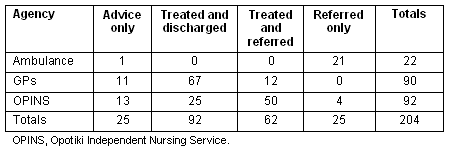
Table 1 shows how many patients were seen and the outcome of that encounter by each service. It is interesting to note that although the GP after hours clinic is available for only four sessions each weekend as opposed to the 24 hour availability of the nurse, the services saw approximately the same number of patients face to face during the month.
Table 2: Referral outcome
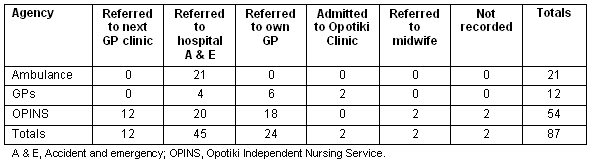
Table 2 shows the number of patients referred on by each service. Nurses referred 20 patients to the Accident and Emergency Department in Whakatane Hospital while the GPs only referred four patients during the month; 78% of patients were treated within the community without need for the hospital assessment. Excluding patients collected by ambulance, 87% of patients seen by the nurse or doctor were dealt with by local services alone. Most patients referred by OPINS and the GPs to Whakatane were transported by ambulance.
Table 3: Percentage of conditions dealt with according to agency
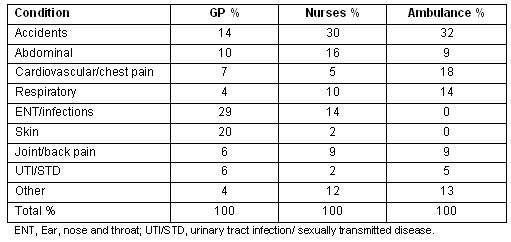
Table 3 is a comparison of the type of conditions seen by each of the services expressed as a percentage. Unsurprisingly more acute conditions are dealt with by ambulance services and nurses. Although not designated as such, the nurse assessment room acts as an accident and emergency service, dealing with all patients who present to the door at any time. The variation in conditions seen results from the difference in availability of the two services, in that patients seeking treatment for chest pain, fractures or lacerations are unlikely to wait until the next available GP clinic but will be treated and referred on to the Whakatane Hospital.
Telephone triage
During the assessment period doctors dealt with five patients and nurses 36 patients by phone after hours. Previously collected data regarding nurse telephone triage reported an average of 35 calls per month after hours to the nursing service.
Contact rates
The estimated population of the Opotiki district is 9200. Using this figure as the denominator, the total rate of after hours contact is 320 per 1000 persons per year. Excluding telephone-only consultations, for direct face-to-face contact the rate was 245/1000 per year: for Maori the rate was 425/1000 per year, while for non-Maori the rate was 151/1000 per year. Ambulance services provide an urgent call service at a rate of 29/1000 persons per year.
Limitations
These data have been collected from a single community in a small town in New Zealand which has cultural, socioeconomic and demographic differences from the general population. There needs to be caution in transferring these results to communities outside of the Opotiki district.
The month of May was chosen because there is no public holiday in that month, the aim was to collect information relating to normal out of hours activity as a baseline, and public holiday activity is likely to add to the demand for services. It was also a consideration that there are no expected excessive demands on the out of hours services from seasonal illness. The involvement of the whole service in collecting detailed information was necessary and a prolonged period of data collection was deemed to be inappropriate, a single calendar month was seen as an achievable target. Utilization rates will vary from month to month and the validity and reliability of the data collection tool was not checked in this study, patients may have been seen by providers and data not recorded.
It was felt that these limitations would bias the results towards providing a minimum expected utilization rate.
The data collected were aimed at determining the after hours workload of each individual provider group. Ambulance data excluded patients who were referred by the nurse or GP to the ambulance service after hours, and this would have the effect of lowering the number of patient contacts assessed with regard to ambulance services. Patients who were seen by the nurse and later also seen by the GP were recorded as having been seen by each provider. This will tend to increase the number of total patient contacts, but this reflects the reality of workload in after hours clinics were nurses work in collaboration with doctors. Only 12 patients were referred by the nurses to the doctor and we do not know that they all attended after hours.
Discussion
Murdoch reported 1233 out-of-hours contacts for a GP practice in Winton, New Zealand in one year8, a rate of 195/1000 persons per year. The rate of consultation we found at 245/1000 per year is similar and because the Opotiki population is geographically well defined and 55 km distant from an accident and emergency service this is likely to reflect closely the total utilization by this population.
Although comparisons of after hours care utilization internationally need to be made with caution because of differences in definition, an assessment across the whole of the UK found an overall after hours call rate of 159/1000 persons per year9, with a higher demand of 270/1000 persons per year in areas of poorer socioeconomic status. In Ireland a similar rate of contact to that found in our study was reported with a rate between 220 and 300/1000 persons per year in rural settings; a lower rate of contact in urban settings at 70-90/100 persons per year was noted, possibly due to the presence of locally available accident and emergency services10.
It is known that demand for after hours care varies among areas, doctors, and services11, with age12, deprivation13, illness levels in a community and higher levels of young children in a population9 increasing utilization, but with much variation unexplained.
Opotiki district is distinct from other areas in New Zealand with its higher levels of deprivation and a high proportion of Maori7. In our survey Maori use of the after hours service was almost three times that of non-Maori, and this was not unexpected and reflects the high health needs of the Maori population14.
The effects of rurality on demand for out-of-hours care are complex and unclear11. Rural patients may delay calling for help until normal office hours because they perceive it is easier to get an urgent appointment the next day, they value the relationship they have with the GP, and see advantage in being undemanding15,16. These attitudes may be explain some delays in diagnosis and treatment of significant illness17,18 and tend to lower use of out-of-hours care in rural settings.
We made no assessment of urgency of need in our study, but in a large cross-sectional survey of out-of-hours care in the UK, 5% of out-of-hours GP contacts were considered urgent, 55% necessary, 26% could have waited until the next day and 14% were unnecessary19. In the same study, 23% of cases seen out of hours by GPs had upper respiratory tract infections, 12% had diarrhoea and vomiting, 8% had ear infections and 7% had chest infections. It is difficult to draw comparisons when definitions and diagnostic criteria are not defined but, broadly, this is comparable with our survey findings. In all, 13% of patients seen by nurses and doctors in our study were sent to hospital, where Salisbury et al. found a 5.5% admission rate following out-of-hours calls in the UK9.
Zeitz et al20, in exploring the issues raised by providers of after hours care in rural Australia, identify many of the same issues that service providers report when discussing out-of-hours care in Opotiki.
Nurses providing triage have to negotiate the difficult interface between private practice and the public service, finding themselves dealing with doctors who sometimes respond inappropriately when disturbed in the night, but understanding the need to protect doctors who are working all day as well as providing after hours care through the night.
Community expectations of the service are that a doctor will be available at all times, and that when services are provided in the 'hospital' that they will be provided at no cost. This can lead to disappointment and aggression when a doctor's fee is requested and, alternatively, surprise when a fee is not required after nurse-led treatment.
It is not uncommon for security issues to arise when the nurse is assessing patients during the night. The threat to personal safety has been studied in the Australian setting, and is one reason female doctors are less likely to provide after hours services11. If nurses are to increasingly become the 'front line' this issue needs to be tackled.
Although it is clear nurses can substitute for doctors safely in many primary care settings21 there are challenges to the nursing scope of practice at times, particularly when patient needs are acute.
The system of care that is in place could be improved by better communication with the community about the scope of service provided. In addition, nurses providing out-of-hours triage lament the lack of standing orders to facilitate care, and medico-legal issues need to be considered in all patient contacts.
Murdoch illustrated clearly that providing after hours care is not financially viable in rural New Zealand8. The service provided to the Opotiki district is heavily reliant on the support of the Bay of Plenty District Health Board, without which the provision of out-of-hours services would be under severe threat. The structure of the system in Opotiki may be valuable for other areas to consider as they re-evaluate their provision of services. This service is similar to others developing in many small towns in New Zealand and, within limitations, it is hoped that this article will help inform primary healthcare organisations and district health boards in planning for the need to provide communities with out-of-hours medical care.
Acknowledgements
The service that has evolved in Opotiki relies on good relationships between the GPs and OPINS, and the consistent support of the St John's Ambulance service and Whakatane Hospital. The authors thank the staff involved in developing this report, and research worker Madelaine Scott-Jones.
References
1. Janes R, London M. Rural general practitioners in New Zealand: November 1999 census. New Zealand Family Physician 2001; 28: 244-249.
2. Mel Pande M, Fretter J, Stenson A, Webber C, Turner J. Royal New Zealand College of General Practitioners Workforce Survey 2005, part 3 General Practitioners in Urban and Rural New Zealand. Wellington: Royal New Zealand College of General Practitioners, 2006.
3. Raymont A, Lay-Yee R, Pearson J, Davis P. New Zealand general practitioners' characteristics and workload: the National Primary Medical Care Survey. New Zealand Medical Journal 2005; 118(1215): U1475.
4. Minogue M, Goodyear-Smith F, Fishman T. The black hole of general practice manpower. New Zealand Family Physician 2005; 32(5): 317-322.
5. Leibowitz R, Day S, Dunt D. A systematic review of the effect of different models of after-hours primary medical care services on clinical outcome, medical workload, and patient and GP satisfaction. Family Practitioner 2003; 20(3):311-317.
6. Ministry of Health. After hours service coverage and high fees, Health Report, 18 October 2007, HC-13-02-04. Wellington: Ministry of Health, 2008.
7. Statistics Zealand. Opotiki District Quarterly Review 2008; March: 13-25.
8. Murdoch JC. Making it pay and helping us stay: the viability of a rural general practice in New Zealand. New Zealand Medical Journal 2006; 119(1246): U2346.
9. Salisbury C, Trivella M, Bruster S. Demand for and supply of out of hours care from general practitioners in England and Scotland: observational study based on routinely collected data. BMJ 2000; 320(7235): 618-621. (Comment)
10. Bury G, Dowling J, Janes D. General practice out-of-hours co-operatives -population contact rates. Irish Medical Journal 2006; 99(3): 73-75.
11. Salisbury C. The demand for out-of-hours care from GPs: a review. Family Practitioner 2000; 17(4): 340-347.
12. Eastwood A, Dowell A. After hours healthcare for older patients in New Zealand. New Zealand Medical Journal 2006; 119(1234): U1979.
13. Carlisle R, Avery AJ, Marsh P. Primary care teams work harder in deprived areas. Journal of Public Health Medicine 2002; 24(1): 43-48.
14. Ministry of Health. Reducing inequalities in health. Wellington: Ministry of Health, 2008.
15. Campbell NC, Iversen L, Farmer J, Guest C, MacDonald J. A qualitative study in rural and urban areas on whether - and how - to consult during routine and out of hours. BioMed Central Family Practice 2006; 7: 26.
16. Farmer J, Iversen L, Campbell NC, Guest C, Chesson R, Deans G et al. Rural/urban differences in accounts of patients' initial decisions to consult primary care. Health and Place 2006; 12(2): 210-221.
17. Svensson L, Karlsson T, Nordlander R, Wahlin M, Zedigh C, Herlitz J. Safety and delay time in prehospital thrombolysis of acute myocardial infarction in urban and rural areas in Sweden. American Journal of Emergence Medicine 2003; 21(4): 263-270.
18. Campbell NC, Elliott AM, Sharp L, Ritchie LD, Cassidy J, Little J. Rural and urban differences in stage at diagnosis of colorectal and lung cancers. British Journal of Cancer 2001; 84(7): 910-914.
19. Brogan C, Pickard D, Gray A, Fairman S, Hill A. The use of out of hours health services: a cross sectional survey. BMJ 1998; 316(7130): 524-527.
20. Zeitz K, Malone G, Arbon P, Fleming J. Australian issues in the provision of after-hours primary medical care services in rural communities. Australian Journal of Rural Health 2006; 14(3): 99-104.
21. Laurant M, Reeves D, Hermens R, Braspenning J, Grol R, Sibbald B. Substitution of doctors by nurses in primary care. Cochrane Database of Systematic Reviews 2005, issue 2. Art. no.: CD001271. DOI: 10.1002/14651858.CD001271.pub2.
Abstract

Introduction: As the rural general practice workforce in New Zealand changes, after hours services are under pressure to change. This is an international problem. This article reports on an initiative in a rural New Zealand community to meet the need for after hours care. First contact for patients is with a community nursing team operating from the local health centre, complemented by on-call advice from GPs and GP clinics twice daily at weekends. Objective: To report on the demand for after hours services generated by a geographically defined community in New Zealand.
Methods: Design: A prospective cross-sectional survey of after hours utilization over a one month period using questionnaires was completed by the full range of healthcare professionals providing care. Setting: A single geographically defined rural community of 9200 people in the North Island of New Zealand. Participants: Rural GPs, community nurses and the ambulance service.
Results: Only 90/204 patient contacts were seen by the GPs with the remainder being managed by the nurses or ambulance staff. Nurses referred more patients to the base hospital but overall 87% of contacts handled by the doctors and nurses were managed locally. Estimated out of hours contact rate was 320/1000 persons/year (including telephone consultations). For direct face-to-face contact the rate was 245/1000 per year: for Maori the rate was 425/1000 per year while for non-Maori the rate was 151/1000 per year. Ambulance services provided an urgent call service at the rate of 29/1000 persons per year.
Conclusion: A collaborative service providing after hours care to a rural community is described and utilization rates assessed. The model of first on-call nurse with GP back up provides a sustainable service and reduces the burden on rural doctors without reducing patient access.
Key words: after hours care, general practice, New Zealand.
You might also be interested in:
2018 - Scope of Practice of Family Medicine Graduates Who Completed Rural vs Urban Program
2014 - Suicide and accidental death in Australia's rural farming communities: a review of the literature
2009 - Pandemic influenza containment and the cultural and social context of Indigenous communities


