Introduction
All registrars in GP (general practice) training are obliged to train for a minimum of 6 months in a rural GP. It has been documented that rural training experiences can impact on the likelihood of doctors practising in that environment in the future1,2. In particular, it has been suggested that career choice is mediated by post-medical-school placement experience3. Therefore, in order to maximise the potential for registrars to consider a rural GP career, it is essential that positive rural placement experiences are provided during registrar training.
In order to positively influence registrars' rural experience before and during their placement it is important to understand the registrars' positive and negative pre-placement expectations. Previous research has found that doctors' rural training placements have the potential to raise both professional and psychosocial concerns4,5.
While there is existing research exploring concerns of registrars leading up to their rural placement, it is not well documented whether these concerns are actualised during the rural placement experience. The current study addressed this issue by exploring GP registrar pre-placement expectations and comparing them with GP registrar post-placement experiences. A qualitative approach has been used in this research to identify themes and extract rich data. This approach is not designed to produce generalisable results.
Method
Ethics approval for the research was granted through the University of Adelaide Human Research Ethics Committee. Participants were recruited through the Adelaide to Outback GP Training Program (AOGP) by advertising at workshops and through their newsletter during 2007. Of the 30 GP registrars who volunteered to participate, 19 had also completed a rural placement. This group represented one-third of the AOGP registrar population.
An independent research assistant (TB), not associated with the AOGP training program, was employed to arrange and conduct the interviews in order to avoid interviewer bias.
A semi-structured interview schedule was developed focusing on previous rural experience (eg schooling, university), expectations before the rural placement, and experiences during the rural placement. Open-ended questions were used throughout and a number of prompts were available. Where possible, registrars were asked to provide specific examples of experience.
Interviews were conducted in a location convenient for the participant and generally lasted 30 min. All interviews were audio recorded and transcribed. Interviews were continued until saturation was reached for both the pre-placement and post-placement groups and no new information emerged. Participant demographics were collected using a questionnaire.
Thematic analysis of the interviews was conducted using NVIVO 7 (QSR International; Melbourne, VIC, Australia; www.qsrinternational.com). The analysis compared the pre-placement expectation themes with the post-placement experience themes. Each interview in which a specific theme was coded was recorded as one reference to that theme. This coding criteria was used to gauge how frequently among interviews a theme was discussed, indicating its importance. This information showed which themes were common among participants, but does not represent an absolute quantity that could be used for statistical analysis.
Many themes were coded as both positive and negative, according to the different views of the interviewees. Therefore, a coding criterion was used to judge whether overall a theme was viewed as positive or negative. If a theme was discussed as positive 75% of the time or more, it was labelled as positive overall (+), and vice versa for negative themes (-). If less than 75% had indicated either positive or negative then it was coded as mixed evidence (-/+). Researchers coded interviews independently and agreed on the positive and negative themes.
Results
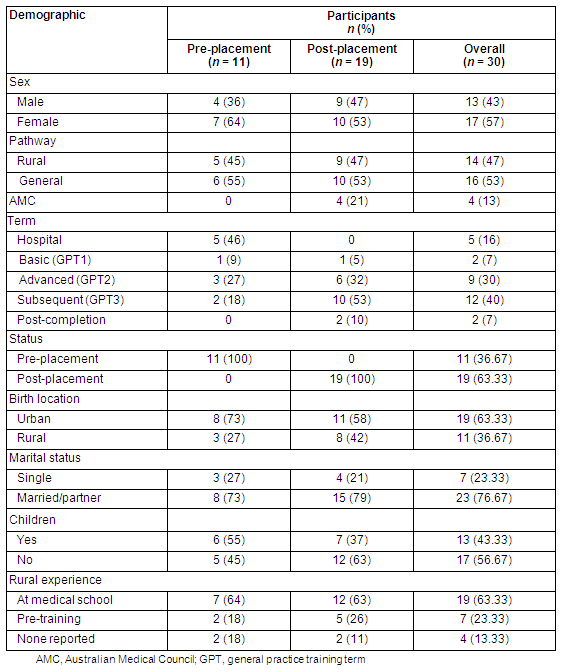
A summary of participant demographics is provided (Table 1). One-third of participants were pre-rural placement and two-thirds were post-rural placement. Gender and training pathway distribution was balanced across both pre- and post-placement groups. The majority of registrars in both groups had a partner. Approximately half of the pre-placement registrars had children but only 37% of post-placement registrars had children. The demographic spread from the sample of volunteers was similar to the demographic spread of the AOGP registrar population.
Table 1: Demographic profile of participants
Pre-placement expectations
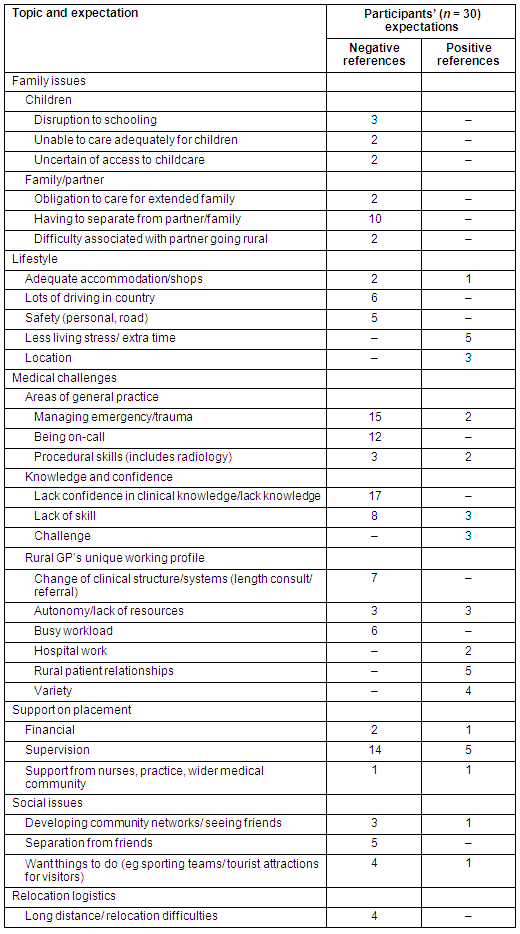
Registrars described a number of positive and negative pre-placement expectations. A summary of these is provided (Table 2). There were 16 themes describing different positive pre-placement expectations. These sorted into the following 4 categories: medical challenges, lifestyle, support on placement, and social issues. There were 42 references to these positive themes. The most commonly referenced positive expectation themes were 'establishing rural patient relationships', 'rural lifestyle (outside GP)' and 'working with specific rural supervisors'. Each of these themes was discussed in approximately 6/30 interviews.
There were 24 negative pre-placement expectation themes. These themes were referenced 138 times. As well as being sorted into one of the 4 identified categories, 2 new theme categories emerged that only contained negative pre-placement expectations: 'family issues' and 'relocation logistics'. The most commonly referenced negative expectation themes were 'dealing with emergency/trauma work' and 'lack of support from supervisor', which occurred in 15/30 interviews. There were 7 pre-placement expectation themes that did not achieve the criteria for coding as overall positive or negative themes and, therefore, were coded as 'mixed' expectations.
Table 2: Pre-placement expectations of rural general practice placements
Post-placement experiences
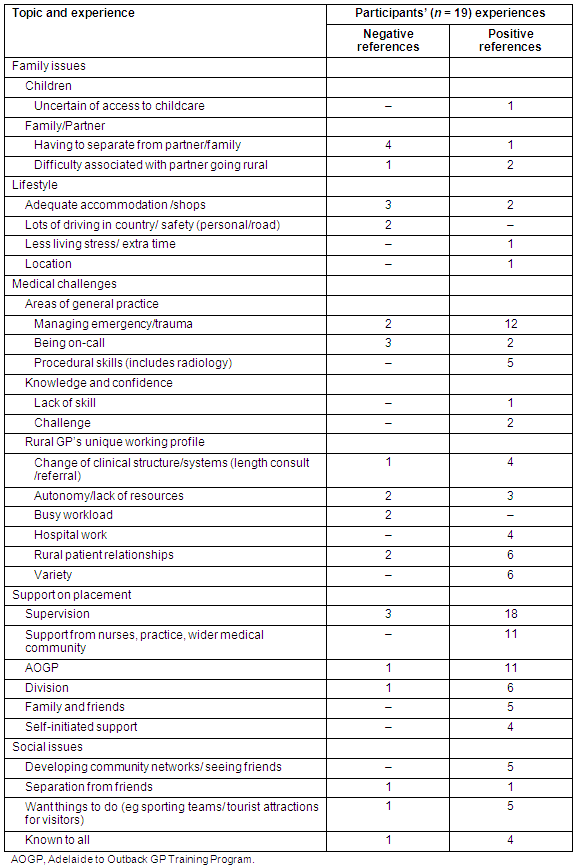
Post-placement registrars described a number of both positive and negative post-placement experiences. A summary of these is provided (Table 3). There were 26 themes describing positive post-placement experiences. These were sorted into the following categories: 'family issues', 'lifestyle', 'medical challenges', 'support on placement' and 'social issues'. There were 121 references to these positive themes. The most commonly referenced positive experiences were 'supervision' (18/19), 'managing emergency/trauma' (11/19), 'support from practice, wider medical community and AOGP' (7/9).
There were 16 negative post-placement experience themes and these were referenced 30 times. These were sorted into the same five categories. The most commonly referenced negative experience theme was 'separation from partner/family' (4/19).
Table 3: Post-placement experiences of rural general practice placements
Comparing pre-placement expectations and post-placement experiences
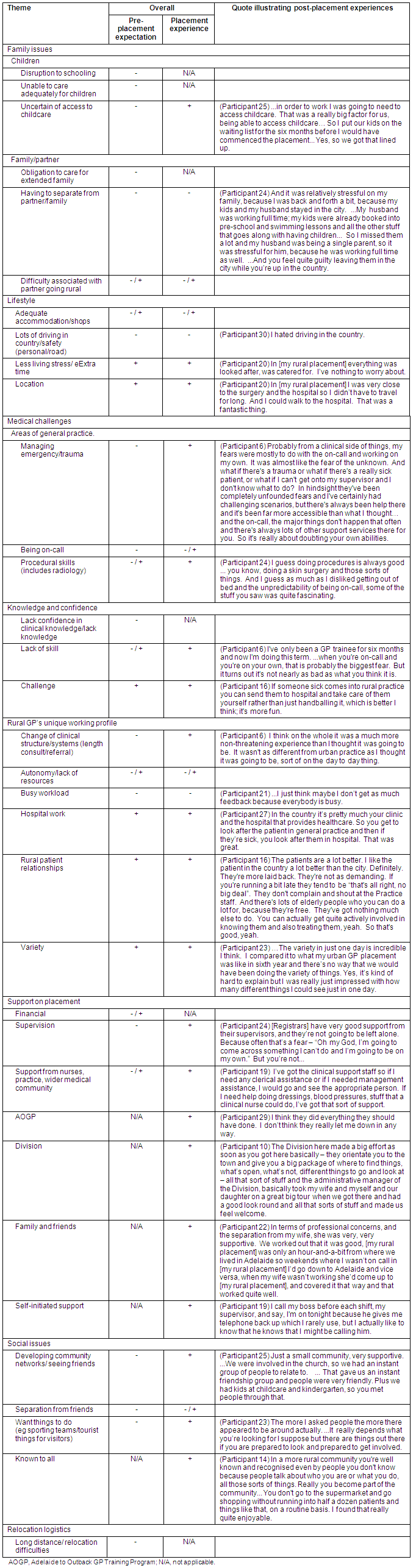
Table 4 indicates whether themes were viewed overall as being positive or negative, both pre-placement and post-placement. Thus, the table indicates how pre-placement expectations compared with post-placement experiences; whether they were the same or different. Illustrative quotes are also included to demonstrate the meaning of each of the themes.
Of 16 overall negative pre-placement expectation themes, only 3 were also discussed as negative post-placement experiences ('separation from family', 'busy workload' and 'lots of driving'; Table 4). Two were discussed as mixed post-placement experiences ('separation from friends', 'being on-call'). Six were discussed as overall positive post-placement experiences ('supervision', 'managing emergency/ trauma', 'adapting to the clinic structure', 'finding childcare', 'community integration' and 'having things to do'). Five were not commented on post-placement.
Similarly, the pre-placement expectations that were coded as mixed evidence tended to be discussed as positive experiences (Table 4). The overall trend was for the experience to be discussed more positively than the pre-placement expectation.
One important area where the actual experience was more positive than the expectation was in terms of support from the supervisor for on-call emergencies. Pre- placement, the majority of registrars were concerned about dealing with emergencies when they are on-call and not having appropriate support from their supervisors.
I guess being in the middle of nowhere with a big sort of motor vehicle accident and wondering how I'll survive trying to manage that all by myself. I guess more the extreme examples, where it's more or less I guess you're sort of solo in managing the situation. (Participant 17)
However, after having experienced a rural placement registrars reported that they had actually been supported well by their supervisors.
And you do realise that even if your supervisor was a little bit far away, you could actually call the next town as well. I know that also your resources are back in Adelaide; you could always be on the phone calling someone experienced from the Royal Adelaide Hospital for example. (Participant 27)
There were also five unexpected positive post-placement experience themes. These were: 'being known to all', 'regional training providers' (RTPs) support', 'Division support', 'support from family and friends' and 'self-initiated support'. Some examples of self-initiated support were:
- approaching the clinic before their placement to develop relationships and acquire information
- making several trips before their placement to get to know the community
- ringing the supervisor every time they went on call to warn that they may be calling for help.
Table 4: Pre-placement expectations and post-placement experiences discussed for rural general practice placements
Discussion
The expectation and experience themes identified were in accordance with previous research in this area with registrars and the partners of registrars4-7, although there was no distinction between the positive and mixed pre-placement expectations, which represented a substantial proportion of expectations in the current research4,5. All positive expectations were also discussed as positive experiences. Half of the pre-placement expectations in this study, however, were negative. All of the 6 coding categories contained negative themes. Two of these categories only contained negative expectation themes ('family issues' and 'relocation logistics'). Three-quarters of negative pre-placement expectations were discussed by post-placement registrars as positive experiences (73%). In addition, a number of unexpected positive experiences were discussed. Therefore, while the pre-placement expectations discussed were mostly negative, the actual post-placement experiences discussed were mostly positive. This supports previous research, which indicates that registrars' rural placement experiences tend to be positive7.
As a result of these findings there are four possible implications. First, it is important to be aware that there are some existing positive stereotypes about rural practice that are warranted. These should be reinforced during the lead up to rural placement.
Second, for those areas that are discussed as negative experiences, there is a need to explore how support can be targeted to ensure more positive experiences. Unfortunately some aspects are controlable and others are not. For example, one of the most cited negative experiences was 'separation from family', over which there is little control. 'Lots of driving' and 'busy workload' are also difficult aspects to change. The best that can realistically be done is to discuss these areas before the registrar begins their placement, and to ensure support is in place to help the registrar manage the situation.
Third, for those negative expectations discussed as overall positive experiences, there is a need to focus on debunking unwarranted pre-placement expectations so that registrars do not have unrealistic concerns. An example of this is in providing realistic perspective regarding the fear that registrars will not have adequate support from their supervisor when managing emergency situations. This was the area of most concern for registrars before their placement but it converted to an overall positive experience.
Finally, registrars' awareness should be raised of the positive aspects of rural practice that may be unknown before undertaking a rural placement. While significant types of support from RTPs, rural workforce agencies and Divisions are already available, these findings highlight the importance of effectively communicating this to the registrars.
To achieve these aims a multi-faceted approach is required. Before the rural placement, supervisors' experiences should be drawn upon to assist in debunking unwarranted negative expectations, and to assist with discussions about putting strategies in place for coping with possible negative experiences (particularly regarding medical challenges). Early in the placement supervisors should discuss the potential negative expectations that registrars may have and clearly articulate ways that each of these can be managed.
Support organisations should work with GP supervisors to discuss the rural placement experience with registrars and debunk unwarranted expectations. In particular, a focus should be on the support available to registrars during their placement, which was found to be poorly understood in the current study. Registrars should also encouraged to be more proactive in seeking out their own support.
Limitations
The study has a number of limitations. A limitation of the research was that the qualitative methods made it difficult to determine generalisibility of the results. A follow-up survey using the information ascertained in the current research could assist with this. The current research used different groups of registrars. The pre-rural placement group could only comment on their pre-placement expectations; whereas, the post-placement group could comment on their pre-placement expectations as well as their post-placement experiences. In addition, the demographic makeup of the two groups was not identical. For example, fewer participants in the post-placement group had children than those in the pre-placement group. This may have impacted on their experience of dislocation from home. For these reasons it may have been better to interview the same group of registrars before their rural placement, and again after completion. However, the types of concerns mentioned by the group who had not undergone their rural placement were sufficiently similar to the group who had finished their rural placement to speculate that expectations had not significantly changed or been forgotten. No information was collected on whether registrars' partner/family moved to the rural placement with them. This variable may have impacted on the outcomes and should be explored in the future.
Conclusion
By understanding the expectations and experiences associated with rural placement experiences, and using this knowledge to inform the preparation for and support during rural placements, it is hoped some positive influence may be possible on registrars' decision to consider rural GP in the long term. The challenge is for supervisors, RTPs and other GP support organizations to work collaboratively and in a co-ordinated manner to communicate this important message.
Acknowledgements
The authors thank the registrars who gave their time to participate in this research. This research was funded by the Adelaide to Outback GP Training Program as a summer vacation scholarship at the University of Adelaide, which was awarded to Mr Timothy Bromley and supervised by Dr Taryn Elliott and Associate Professor Anna Chur-Hansen. Aspects of this project have been presented at the General Practice Education and Training Conference 2007 and the Australian and New Zealand Medical Education Conference in 2008.
References
1. Rolfe I, Pearson S, O'Connell D, Dickinson J. Finding solutions to the rural doctor shortage: the roles of selection vs undergraduate medical education at Newcastle. Australian New Zealand Journal of Medicine 1995; 25: 512-517.
2. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and post-graduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37: 809-814.
3. Laurence C, Elliott T. When, what and how South Australian pre-registration junior medical officers' career choices are made. Medical Education 2007; 41(5): 467-475.
4. Charles D, Ward A, Lopez D. Experiences of female general practice Registrars: Are rural attachments encouraging them to stay. Australian Journal of Rural Health 2005); 13: 331-336.
5. Larkins S, Spillman M, Vanlint J, Hays R. Stress, personal and educational problems in vocational training. Australian Family Physician 2003); 32: 473-476.
6. Bayley S, Sweatman J, Regan C, Magin P. Factors contributing to registrars' perceptions of quality of experience in rural terms: results from a qualitative study. In, Proceedings, General Practice Training and Education Conference; 27-28 August 2008; Woolongong, NSW; 2008.
7. Panozzo S, Laurence C, Black L, Poole L. Exploration of the preconceptions of living in a rural community by general practitioner registrar partners. Australian Journal of Rural Health 2009; 17: 167-170.




