Introduction
Consumer-driven services play an important role in mental health service delivery in rural and remote Australia. Their origins often lie in the need for creative options and innovative solutions for those with mental illness in contexts where there are inadequate on-the-ground supports. It is known that the 'culture of self reliance' operating in some small rural and remote Australian communities mitigates against help seeking for mental illness1,2 but there may be a positive outcome of this self reliance. The attitude that 'if we don't do it no-one will' is the precursor to numbers of consumer-driven services responding to the needs expressed locally by people with a lived experience of mental illness and their carers. Services take into account the rural cultural expectations of self-sufficiency and the problems associated with the stigma of identifying as having a mental illness3. The solutions are locally devised, flexible, and locally owned. However, because they are not driven by a funding program or necessarily aligned with a state or national level mental health strategic direction, they may lack legitimacy, struggle for funding, and become unsustainable. Certainly, they are rarely comprehensively evaluated and there is little Australian published work about their strengths and limitations.
Internationally the situation is different. Consumer-based organisations operated by and for people with serious mental health problems have expanded greatly in the USA and Canada in the past 20 years and the literature is now well represented with evaluations of their programs. Some widely recognised organisations are 'The Welcome Basket'4 and the 'Independent Living Movement'5 These services have come to offer not only mutual support, but they have also adopted agendas for broader social change6. For example, Davidson et al identified that peer support can assist in recovery as peers serve as community role models and help to de-stigmatise mental illness in both the community and the mental health system7. In the UK, Truman and Raine identified that the social elements of participation in activities provided opportunities to mix with others, including mental health service providers, on an even footing and this was thought to be a starting point for reintegration into the community8. Mead identified four components of mutual support group programs that are related to positive outcomes: the peer principle, the helper principle, empowerment, and advocacy5. The peer principle is finding affiliation with someone with similar life experience and having an equal relationship and the helper principle is that the notion that being helpful to someone else is also self-healing. Empowerment is about finding hope and believing that recovery is possible and taking personal responsibility for making it happen. Finally, advocacy (self and system advocacy skills), involves choice and decision-making opportunities and skill development.
This article adds to the Australian literature about consumer-driven mental health services and in particular the contextual factors and program mechanisms that produce positive outcomes. The Station in rural South Australia is a consumer-driven mental health community centre located in a unique heritage-listed old police station. It provides people recovering from a mental illness and their carers, as well as community members, with a safe and supportive environment in which to meet and conduct activities. People can access information and peer support, engage in a range of activities, both informal and structured, and increase knowledge and skills for living. The objectives of The Station are to:
- facilitate a range of activities to meet the members' needs, interests, and abilities
- foster a safe and supportive environment where autonomy and self-determination is encouraged
- help members regain self-worth, self-esteem, purpose, and confidence
- demystify and de-stigmatise mental illness by promoting community awareness and involvement.
The Station has a total membership of approximately 50 from the region (upper Yorke Peninsula and lower Mid-North) and is open 3 days each week. Gender is balanced but there are greater numbers of older people attending than younger. A partnership with the local community mental health team and the regional health service provides resources and expertise, while the government Country Health SA funds two part-time coordinator salaries. There is considerable in-kind support from local government. The organisation is incorporated and it is managed by a committee composed of three to four people with a mental illness, up to four community people with an interest in mental health issues, and one mental health professional.
A non-medical, recovery orientated, and a holistic primary health care approach are used to achieve health and wellbeing. There is a high degree of consumer involvement in all aspects of service delivery. Participation in activities enables people to develop their confidence and skills and take advantage of new opportunities and friendships. Outings encourage social connectedness. Activities include massage, painting, art and craft, creative writing, gardening, Tai Chi, and health promotional programs. The provision of a healthy lunch is a core program which is self-funded. Members, staff, students, and volunteers organise all aspects of the lunch program.
Method
After 10 years operation, The Station thought it was timely to evaluate the service and was successful in obtaining a Capacity Building Development Grant from the Mental Health Council of Australia. Because of the complexity of The Station's processes and outcomes and its embedded nature within the community, a realist evaluation framework9 was chosen. Realist evaluation has an explanatory rather than judgemental focus. It seeks to 'unpack' the mechanisms of how complex programs work (or why they fail) in particular settings using qualitative or quantitative methods. Consistent with the realist approach the objectives of the evaluation were to:
- describe, analyse, and promote the service and governance model at The Station and determine how the model works and for whom and its sustainability
- identify gaps in The Station's services
- analyse The Station's partnerships at a local, regional, and national level in order to determine how they might be strengthened and extended
- develop and implement a plan-action-review cycle for the organisation to continually monitor its progress against its aims and objectives.
This article concentrates on the first objective of the evaluation.
Participatory action research
The evaluation was conducted as participatory action research (PAR). The Station members, (past and present) volunteers, management committee members, and staff were involved in all phases of the research process. An enthusiastic team of 14 volunteered for the advisory working group but often there were more people in attendance sitting around the table at the fortnightly workshops. The team decided the research questions, the information needed to answer the questions, and how it should be collected. Ethics approval was obtained from the Human Research Ethics Committee (HREC) of the University of South Australia in October 2008.
Data collection
Three sets of information were used: in-depth interviews, a document review, and a stakeholder analysis. Twenty-three in-depth interviews were conducted with those who indicated willingness to participate and made their contact details available to the university researchers. The university researchers randomly selected interviewees from within five groups: those with a lived experience of mental illness, volunteers, management committee, staff, and people who did not attend The Station but who had a lived experience of mental illness. It was found that often volunteers and management committee members also had a lived experience of mental illness and interviewees responded from both these perspectives. Interviews focused on The Station's role in assisting recovery from mental illness, limitations and strengths of The Station's program, and contextual influences.
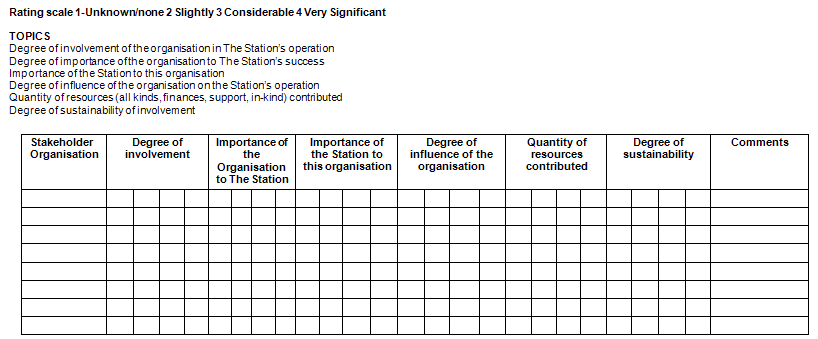
The document review involved an analysis of constitution, goal statements, annual reports, newspaper clippings, membership/volunteer application form, and guidelines for members. Stakeholders were identified by the advisory working group and then rated, through group discussion, on the following topics:
- degree of involvement of the stakeholder in The Station's operation
- degree of importance of the stakeholder to The Station's success
- importance of The Station to the stakeholder
- degree of the stakeholder influence on The Station's operation
- quantity of resources (all kinds, finances, support, in-kind) contributed
- degree of sustainability of involvement.
The following rating scale was used: 1 = unknown or none, 2 = slightly, 3 = considerable, 4 = very significant.
The framework for stakeholder analysis is included (Appendix I).
Data analysis
In-depth interviews and focus groups were transcribed, de-identified, sent back to participants for verification. The information was entered into descriptive categories in N6 (QSR; www.qsr.international.com). Categories were evaluated and themes developed guided by the realist evaluation approach9 to identify the important contextual influences, program mechanisms, outcomes, and sustainability. Data from the stakeholder analysis were entered into Microsoft Excel and charts produced and all relevant documents were reviewed. This provided further information about outcomes, program mechanisms, contextual influences and sustainability. Finally the three data sets were triangulated to check for corroboration or lack of corroboration.
Limitations of the evaluation design
There are several design limitations. The most important one is that it was difficult to interview people for whom The Station's program did not work and therefore very little information was collected about this topic. As is the case in a realist evaluation9, establishing the relationship between contextual factors, program mechanisms, and outcomes was complex. However, because of the high degree of consensus about the important factors operating at The Station the researchers are confident of the findings. One of the most challenging aspects of a PAR evaluation is balancing inclusivity with the need to protect the anonymity and confidentiality of participants and their views. This was achieved by presenting summary findings to participants as themes and only using quotations to illustrate themes where participants could not identify the source.
Results
After analysing each set of information separately and then comparing them (interviews, documents, and stakeholder analysis) a very high degree of 'fit' between each of the sources of information was found. For example, the policies of The Station were designed to maintain a flexibility that enabled participants to feel that this was a homely and accepting environment. The active support from the local mental health system and key stakeholders gave the service legitimacy and confidence and this was reflected in The Stations outcomes for participants. The result of this 'fit' is a coherent approach or model with clear and intended project mechanisms that consistently produce predictable positive outcomes for those who attend. All those interviewed spoke very highly of The Station in achieving its goals of creating a supportive atmosphere for all those who attend.
I have actually really achieved a lot and, how can I say it, I have accomplished things that I would never have thought in a lifetime that I could do. (Member)
I don't think I'd function without The Station in my life now. The Station became my family, an adjunct to my family, very early. It became a familiar comfortable family atmosphere, which it has always been here and I think I became a part of that. (Volunteer)
The Station benefits all those who attend, not only those who have a diagnosed mental illness. Carers, people with a lived experience of mental illness, and volunteers all reported similarly of the positive impact of The Station on their lives. People who volunteer at The Station gain a sense of community and family, 'time out' and an opportunity to learn new skills and meet new people.
My motivation for being involved initially was because, well, I needed to get involved in the community because ... You've got a choice. I could sit and mope and why me, or else I could get up and go out and meet people and stuff like that. And I also think the Station helped me a lot too. And the people I've met, different people, different ideas. (Volunteer).
Carers find that the break from caring responsibilities provides them with a useful social connection:
The Station plays a very important part of my life now because I look forward to coming. I feel isolated if I don't come because I need to have other people around me because I'm more of a people's person. They [people who attend The Station} have become like my family to me and I do enjoy it. (Carer)
The group that was selected on the basis that they might express less positive views of their Station experience in fact described very similar feelings about the personal value of their contact time and the positive effects of The Station program.
The program mechanisms that produce outcomes
Program mechanisms are those things that 'trigger', produce, or activate outcomes - how the program works. It is through the social atmosphere, relationships, and activities that occur at The Station that the program mechanisms operate. The activities themselves are not sufficient. The program mechanisms can be grouped into two distinct but overlapping themes: nurturing and empowering. The outcome of nurturing is a feeling of being accepted as one is, and the outcome of empowering is a belief in oneself. The interaction of program mechanisms and contextual factors to produce outcomes are illustrated (Fig1). It is this interaction that is all important.
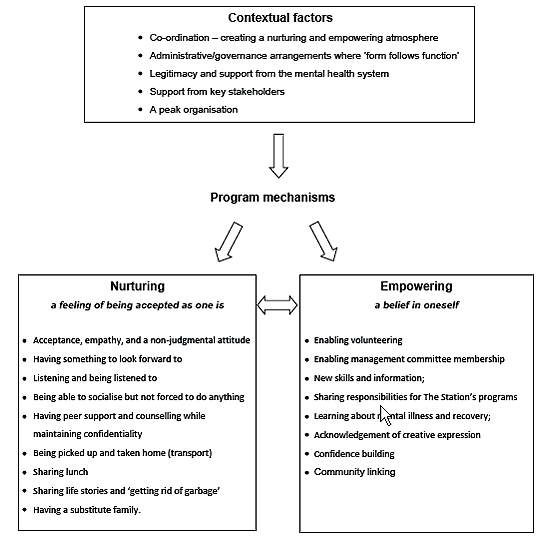
Figure 1: Contextual factors and program mechanisms producing outcomes
For those who have a mental illness recovery is a difficult process.
It's like climbing up a well. I drew a well when it was ... but in my life, I've been climbing up that well ever since. You get almost to the top brick, but you lose your grip. That's the way it's been, all my life. Now I am probably three-quarters; not quite to the top, but there's no foot hold, you just go with your fingers. If those fingers give way, you're down the bottom again. But I try to hold on very tight and try not get to the very bottom. (Member)
Overall, the first step in recovery is a feeling of being accepted as one is with or without a mental illness. A non-judgemental, warm and friendly attitude prevails at The Station and people can form trusting relationships at a level they are comfortable with even if this means just being present with other people.
It's an outreach and somewhere to go to do things and meet people, and just be me and I don't feel judged or like I have to be a certain way, or anything like that. So I've learnt to accept people as they are and not be judgmental and whatever (Member).
The first time I went there, [The Station} there was just this acceptance.....there was no judgement at all... they didn't care I was shaky... or having trouble stringing a conversation together. They just said, 'Hi, how are you? Welcome here! And here have a cup of tea'. (Member)
Another member explained:
When I first went to The Station I was very scared and withdrawn ...now that people are starting to talk to me it's just fantastic. I reckon it's been a whirl wind of change for me. Just opening up and just flourishing, just being around people and having friends and giving people hugs. (Member)
The specific nurturing mechanisms of The Station program were identified as:
- acceptance, empathy, and a non-judgemental attitude
- having something to look forward to
- listening and being listened to
- being able to socialise but not forced to do anything
- having peer support and counselling while maintaining confidentiality
- being picked up and taken home (transport)
- sharing lunch
- sharing life stories and 'getting rid of garbage'
- having a substitute family.
Once a feeling of acceptance is experienced empowering mechanisms result in a belief in oneself, or that the person is able to do things that they thought they would not and become a valuable member of the community. Specifically, the mechanisms involve the following:
- enabling volunteering at The Station
- enabling membership of the management committee
- providing opportunities to learn new skills and gain information
- sharing responsibilities for running The Station including assisting in fund raising
- providing information about mental illness and recovery
- providing opportunities for creative expression and acknowledging this
- confidence building
- supporting links with the community through outings.
Some examples of what people meant by empowerment include:
Before, if anyone said are you going to get a job, I would have said 'No, I'll never be able to work', but now I'm the president and secretary of the management committee I feel I could get a job part-time. Now I know that that's not a big deal to most people, part-time work, but to me that's like walking on the moon!.
Employment was reported to be an important step in recovery. While the financial rewards are significant what is possibly more important is the feeling of contributing to society.
So my job has been tiring but I actually feel a lot better for working in my mental health, because I've got that confidence now that I can do it. I've also got a sense of worth because I feel like I'm actually contributing more to society now. So overall, it's just been fantastic. (Management member)
The contextual factors that support the program mechanisms
The contextual factors that were critical in supporting the program mechanisms at The Station were:
- coordination - creating a nurturing and empowering atmosphere
- administrative/governance arrangements where 'form follows function'
- legitimacy and support from the mental health system locally and at the state level
- support from key stakeholders
- a peak organisation to act as a conduit between government and the service.
The role of coordination involves balancing informality and relating in a genuine way to people with a variety of needs while coping with the inevitable uncertainty about 'how people are travelling'. People interviewed, were well aware of the importance of coordination in producing a positive atmosphere and most put it down to 'personalities' - the right people: 'I just love the atmosphere. It's just a really positive atmosphere and the people are really friendly'. Creating a welcoming, nurturing, and empowering social environment is the responsibility of everyone but it is the coordinators who do this on a daily basis. The skills involved are a high degree of perceptiveness about social relationships, an ability to relate to a range of people, allowing people to take responsibility, and an ability to balance group and individual needs.
The Station has an administrative system where the policies and protocols are determined by the functions and not vice versa. For example, the membership volunteer application form is brief and there is no requirement to disclose mental illness. A description of health problems is optional. The guidelines for members are clear and straightforward, for example 'give support to each other - not therapy or medical advice'. Achieving a balance between form and function is a very difficult task which The Station has managed exceptionally well:
Sometimes our management committee, they can be a bit of a rabble - but when the chips are down, when they're fighting for the survival of this place, it's the people with the mental health issues that stick it out. They stick it out and they work through these issues, they don't cut and run.
The mental health system is vital to the future of The Station and vice versa. Originally it was the one-on-one support of a mental health professional in the system that enabled The Station to 'start its journey'. Now the South Australian mental health system is the major funding source and fully supports the model of community mental health centres as an adjunct to service delivery. However, this relationship, like that of the other key stakeholders is conducted without any formal documentation of the roles and responsibilities of each of the partners. This enables a great deal of flexibility to tailor services to needs but it has its downside and there is a level of uncertainty that The Station copes with about its future.
An important finding from the stakeholder analysis was that two stakeholders who rated highly on the degree of importance to The Station's functioning (the local mental health system and local government) rated low on the sustainability of their involvement and their degree of influence on The Station's program. This suggests that that there may not be reciprocity in the relationships with these stakeholders and if there is, it is implicit rather than explicit.
Finally, The Station is part of a peak organisation the One Voice Network which advocates with the mental health system and more broadly on behalf of consumer-driven mental health initiatives in rural South Australia.
Discussion
Both the concepts of nurturing and empowerment have been recognised previously as important outcomes of consumer-based community mental health centre programs4,5,10,11. Brown wrote that participation in consumer-run organisations can be either 'socially supportive' or 'empowering' and finds that both types of participation are important to recovery12. Empowering activities relate to involvement in leadership or organisational functioning, while socially supportive participation (nurturing) means forming intimate and sharing social relationships with others.
Consumer-operated programs provide a caring and sharing community, where the person can find the necessary understanding and recognition that society at large is not able to give13.
There is a particular problem with the term 'empowerment' in that it has become a rather overused and imprecise term with its underlying dimensions applied to many different aspects of mental health and the mental health system14. In spite of the difficulty with the term, the empowerment outcomes of The Station were clearly that at a personal level people gained control over their lives and felt that they could contribute to society in some way.
It is clear that in rural and remote communities the community mental health centre model has both advantages and disadvantages. First, the visibility of the service in a small community may attract negative attitudes towards people who are associated with the centre and who may then be identified as mentally ill. The bulk of the international disability literature promotes the inclusion of people with a disability into ordinary social life rather than to develop separate facilities15. The relationship between social exclusion and mental ill-health is complex, with many of the elements of 'exclusion' (low income, lack of social networks, joblessness) being in different circumstances both causal factors and consequences of mental ill-health16. The Station is mindful of the stigma that many of its members have experienced because of their mental illness, and it balances the maintenance of a safe atmosphere with encouraging broader social linkages. Actively fund raising, publicising its activities, and supporting its members who are re-integrating into the community enable important community connections to be made.
An important outcome of the evaluation was the regional community forum to promote The Station's approach. This was organised by The Station and all the key community organisations and government agencies in the area were invited and most attended. The event was significant in that it enabled The Station to develop confidence in its achievements and network with some organisations that it had previously seen as 'exclusive'. Conversely, several representatives of these 'exclusive' local organisations confided that they had not known much about The Station's activities or about mental illness in the community and had been afraid to ask.
The forum strengthened the natural supports found in rural communities that Bjorklund argued are one of its greatest strengths17. This 'connectedness' is harnessed in innovative ways to form strong informal relationships to support people living with a mental illness. For example, employers are often willing to offer opportunities to those recovering from mental illness because they have a relationship with them. Local businesses promote The Station as a place to volunteer and seek social support. In order to break down the barriers those members may feel when they 'return to community' it is important that The Station actively places itself confidently 'to be part of the community'. 'Return to the community' is not an explicit objective of The Station although it was always envisioned that it would be a place where people go until they're confident to go back into the community. The vision was that 'The Station would be a bridge; that people would come here and they would use it to regain their skills and move on' (Staff person).
The Station has created a nurturing and empowering environment without replicating the 'patient-staff' relationships that members may have found unhelpful in the mental health system. The Station employs paid coordinators and yet maintains a friendly non-clinical atmosphere. Staff maintain that the degree of ownership of the policies and practices is one of the reasons that the model works.
We worked through all these, our aims, our philosophies, our vision, our objectives. We worked through it with the members... So it was really working with the members right from the word go. I think that gave them a strong sense of ownership. (Staff member)
The question of sustainability is important. Some data pointed to personalities as being central to the high level facilitation skills, identified as contextual factors that enabled program mechanisms to work. If the coordinators change it was though that The Station might not work so well. This evaluation provides further clarity about the program mechanisms and what supports them, enabling the management committee to ensure that new coordinators understand and support the approach. The Station management committee consider that achieving sustainability is an ongoing process of overcoming a myriad of issues that present themselves.
Conclusions
The contextual factors that assist recovery from mental illness and the program mechanisms that operate at The Station can be clearly identified and together form a coherent model that reliably and consistently produces outcomes for participants. The model produces beneficial outcomes not only for those who come as members but also by those who volunteer, by carers who attend, and by those who are on the management committee. This is perhaps because, unlike the formal mental health system, the distinction between those who have a lived experience of mental illness, staff, volunteers, and management is blurred.
Although potentially there could be criticism of this model from those supporting an individualised community inclusion approach to recovery from mental illness there is evidence from those who use The Station that recovery from mental illness had been significantly assisted.
It was more difficult to identify those for whom the program does not work. However, it was identified that the social setting at The Station is a vital element for imparting a feeling of acceptance and gaining a belief in oneself. It is therefore surmised that people who are unable to relate to others with a mental illness in this type of social setting may not benefit. Some who were interviewed said that the social setting was very intimidating at their first contact and claimed that a degree of recovery from mental illness was needed for successful social integration into The Station community. Although it was not possible to interview people who had lost their social connections with the community it was said that these people could not benefit from The Station because they could not attend.
The sustainability of this model rests on its ongoing acceptance and support within the rural community, community mental health providers, and the mental health system. This evaluation provides a clear description of the model and justifies its efficacy in assisting client recovery from mental illness. As such, it may consolidate legitimacy in both state and national mental health systems and so contribute towards future sustainability.
Acknowledgements
The Station advisory working group greatly assisted the conduct of this evaluation, and the participants in interviews are thanked for their contribution. The evaluation was conducted with funding through the Mental Health Council Australian Department of Health and Ageing. Author Judy Taylor has a Primary Health Care research fellowship from the Australian Government Department of Health and Ageing. Full information about the steps in the evaluation and the instruments used can be obtained from the coordinator, The Station (South Australia; thestation@internode.on.net).
References
1. Fuller J, Edwards J, Proctor N, Moss J. How definitions of mental health problems can influence help seeking in rural and remote communities. Australian Journal of Rural Health 2000; 8(3): 148-153.
2. Wainer J, Chesters J. Rural mental health: Neither romanticism nor despair. Australian Journal of Rural Health 2000; 8(3): 141-147.
3. Judd F, Jackson H, Komiti A, Murray G, Fraser C, Grieve A et al. Help seeking by rural residents for mental health problems: The importance of agrarian values. Australian and New Zealand Journal of Psychiatry 2006; 40(9): 769-776.
4. Weingarten R, Chinman M, Tworkowski S, Stayner D, Davidson L. The welcome basket project: Consumers reaching out to consumers. Psychiatric Rehabilitation Journal 2000; 24(1): 65-68.
5. Mead S, MacNeil C. Peer support: What makes it unique? International Journal of Psychosocial Rehabilitation 2006; 10(2): 29-37.
6. Janzen R, Nelson G, Housfather N, Ochocka J. Capturing system level activities of mental health consumer-run mental health services. American Journal of Community Psychology 2007; 39: 287-299.
7. Davidson L, Chinman M, Sells D, Rowe M. Peers support amongst adults with a serious mental illness: A report from the field. Schizophrenia Bulletin 2006; 32(3): 443.
8. Truman C, Raine P. Experience and meaning of consumer involvement: Some explorations from a community mental health project. In: M Robb, S Barrett, C Komaromy, A Rogers (Eds.). Communication, relationships and care; A reader. New York: Routledge Taylor Francis Group, 2004; 43-54.
9. Pawson R, Tilley N. Realistic evaluation. London, UK: Sage, 1997.
10. Chinman M, Weingarten R, Stayner D, Davidson L. Chronicity revisited: Achieving a person-environment fit through a consumer-run service. Community Mental Health Journal 2001; 37(3): 215-229.
11. Nelson G, Ochocka J, Griffin K, Lord J. Nothing about me, without me: Participatory action research with self help/mutual aid organizations for psychiatric consumer/survivors. American Journal of Community Psychology 1998; 26: 881-912.
12. Brown L, Shepherd M, Merkle E, Wituk S, Meissen G. Understanding how participation in a consumer run organisation relates to recovery. American Journal of Community Psychology 2008; 42(1-20): 167-178.
13. Van Tosh L, Del Vecchio P. Consumer-operated self-help program; A technical report, US Center for Mental Health Services, 2000. In: Corrigan P, Slopen N, Gracia G, Phelan S, Keogh C, Keck L. Some recovery processes in mutual-help groups for persons with mental illness II: Qualitative analysis of participant interviews. Community Mental Health Journal 2005; 41(6): 723.
14. Rogers S, Chamberlin J, Ellison M, Crean T. A consumer-constructed scale to measure empowerment among users of mental health services. Psychiatric Services 1997; 48: 1042-1047.
15. Sayce L. Social inclusion and mental health. Psychiatric Bulletin 2001; 25(4): 121.
16. Brown G, Harris T. Social origins of depression. London: Tavistock Publications, 1978.
17. Bjorklund R, Pippard J. The mental health consumer movement: Implications for rural practice. Community Mental Health Journal 1999; 35(4): 348-359.
________________________________
Appendix 1: Stakeholder Analysis Worksheet