Introduction
Priority setting entails making decisions about the allocation of resources to identify and address important health issues. Prioritisation can operate at the micro-level (such as for individual programs), the meso-level (local communities and service catchments or regional health authorities), or the macro-level (eg governmental)1. With tighter health budgets, an increasing demand for health services, and more stringent accountability requirements, formal approaches to priority setting are being developed. However, there is no consensus about which tool, methodology, framework or approach should be used to set priorities and, in addition, decision-makers are often unfamiliar with what is available2-5.
This article presents a model of 13 factors that influenced priority setting for a community health plan prepared by decision-makers in a primary healthcare alliance in a regional area in Victoria, Australia. The model offers an insight into the 'real world' experience of meso-level planning. The article opens with an overview of the policy and service context, and then examines the international literature tracing the development of approaches and tools for setting priorities in primary health care. The 13 factors are then presented, revealing the complexity and multidimensionality of influences on priority setting.
The policy and service context
A recent report on Australia's national primary health care strategy6 has identified that in future the system must be broad based (involving health and relevant non-health services) and must engage with local communities to plan and deliver population-based approaches to addressing local priorities. Within Victoria, Australia, Primary Care Partnerships (PCPs) are a state government initiative that has been operating for a decade. Primary care partnerships aim to improve the overall health and wellbeing outcomes of the Victorian population when using primary care services, as well as helping to reduce service usage (hospital, medical, residential) through early intervention and health promotion7. There are 31 PCPs in Victoria comprising over 800 member agencies8. As such, the actual nature of PCPs - their structure, the organisational partnerships they form and the problems they address - is complex9. Each PCP is required to develop a 3 year strategic plan focusing on 2 or 3 health and wellbeing priorities. The 3 key health promotion priorities adopted by PCPs across Victoria between 2006 were 2009 were to promote:
- Mental health and wellbeing
- Physical activity and healthy communities
- Accessible and nutritious food.
The Central Highlands PCP was established in 2000 and facilitates collaboration with both its member agencies (totalling 34 and comprising local health, education and human service sector agencies) and other organisations to improve the health and wellbeing outcomes of the community within the region by facilitating collaborative health promotion, consumer participation and improving service access10.
The framework for priority setting presented in this article summarises the real-world experiences from a research project undertaken in 2009 by the University of Ballarat for the Central Highlands PCP (CHPCP), located in regional Victoria. The project entailed a comprehensive health and wellbeing needs analysis for the 4 local government areas comprising the CHPCP catchment region (City of Ballarat, Golden Plains Shire, Hepburn Shire and Moorabool Shire), with a total population of approximately 147 000. The key stages of the project were:
- Collation and analysis of extant health data
- Identification of health needs and priorities within the catchment.
The report was submitted to the CHPCP to inform the development of a three-year community health plan.
Review of the literature on priority setting
The research literature reveals that priority setting 'is complex, difficult, contentious and often controversial' (p.8)1, that the public's views about important priorities are highly contingent upon the technique of data collection11,12, that priority setting entails trade-offs, choices and sacrifices13 in hierarchical, politicised environments14, and that approaches can be 'so technical in nature that their relevance is lost ... [or] ...too general ... so as to prevent real decisions being made' (p.1662)4. In the face of this complexity, there are increasing demands from governments and healthcare funders for more formalised, workable and transparent approaches to priority setting.
In the last decade there have been at least 4 major advances in working towards a mature, agreed approach to priority setting in health care. The first major advance was signalled by the shift from the idea that priority setting could be achieved by the application of a rational, linear set of rules (eg analyses of cost effectiveness, or program budgeting and marginal analysis) to an appreciation that the process was inherently complex, contingent and contentious15. Related to this, the second major advance involved the emergence of multidimensional approaches. Strictly economic appraisals were softened by the embrace of ethical, sociological and political considerations, accompanied by the adoption of methodologies such as participatory action research. These approaches acknowledge that setting priorities involves value choices, for example the 'Accountability for Reasonableness' framework assesses the fairness of priority setting according to the criteria of relevance, publicity, revisions/appeal, and enforcement3. Theories of distributive justice can also help us to make judgements about how scarce health resources should be distributed16.
The third major advance has been driven by the consumer movement in health care, through which patients, clients and the broader community have demanded having a strong voice in decision-making. While there is now general agreement that consumers should be involved in setting priorities, debate continues about the best approach to this11, whether public input risks a 'dictatorship of the uninformed' (p1001)17, how much weight should be given to the views of the public18, and how their views should be used or mediated19. Many also question whether the involvement of service users and the public - while couched in the language of consultation and empowerment - is anything more than tokenistic20.
The fourth major advance has been a declared commitment to a collaborative approach to priority setting. Because it is now understood that priority setting is a political act, a collaborative process should minimise power imbalances and provide genuine opportunities for participation14. This has generated new approaches to priority setting, such as participatory action research4,5,21.
These 4 advances have yielded more sophisticated ways to approach priority setting in health care. For example, researchers4 have identified 10 inputs into the priority setting process. These include community input, literature reviews, practice guidelines, financial data and provincial or federal requirements. This model is useful because it lists the sources and types of data that should be considered, and so can inform the data collection phase of priority setting. Recently, a second tool has been developed using a Delphi technique with healthcare decision makers across Canada. Others have identified 10 factors (5 process and 5 outcome) essential for successful priority setting1. The 5 process elements were: (i) stakeholder engagement; (ii) use of an explicit process; (iii) careful information management; (iv) decisions based on clear value choices and context; and (v) revision or appeal mechanisms. The 5 outcome elements were: (i) improved stakeholder understanding; (ii) shifted priorities and/or reallocated resources; (iii) improved decision-making quality through institutional learning; (iv) stakeholder acceptance and satisfaction; and (v) positive externalities, ensuring information is 'transparent' and readily available to stakeholders.
These tools have been derived from research about decision-makers' views on the ideal processes or criteria. However, there has been little research or critical reflection based on the real world experiences of decision-makers actually involved in the process. Learning from actual experience may help to bridge the gap between approaches that are highly technical and those too general to be useful.
Methodology
Reflective professional practice refers to a structured, inductive approach to formalising learnings from a specific set of experiences22. The reflective process typically involves 3 phases:
- Identification and description of practices and experiences in the local context.
- Reflection on these practices and experiences - such as articulating assumptions, searching for patterns, and codifying or classifying patterns.
- Developing theory and practice by refining or amending existing theories and models23.
Reflective practice has been used extensively in health and education settings, and can be a special application for health practitioners in rural and remote areas24,25.
Each of these 3 phases of reflective practice guided the development of the framework for priority settings. First and most importantly, the authors participated in meetings with both the Project Management Group and the PCP Full Alliance for the 11 months of the project's duration. This provided the researchers an opportunity to identify the current practices and experiences of practitioners regarding priority setting in the catchment area, and to regularly present information back to the management group and the full alliance for their consideration. The process of reflection for model development was then undertaken by the authors who, as experienced researchers, reflected on and identified the themes that would later form the stages or key priorities for the model. A critical review of the relevant literature helped to further define the resulting 13 factors in the model presented here.
The model: a practice innovation
The model provides a guide for primary healthcare organisations' decision-making (Fig1). It acknowledges that priority setting is complex and dynamic, and that successful decision-making is highly dependent on local contexts and conditions.
A framework for priority setting
This framework identifies and describes a set of factors that influence the setting of priorities in primary health care. The 13 factors range from economic, political, policy, epidemiological, moral, evidentiary to evaluative domains. All of these factors were observed to come into play at various times during the project and, in particular, during discussions with the Project Management Group and the PCP Full Alliance.
In presenting the framework, 3 observations are offered. First, while the list is comprehensive, the authors do not claim that it is exhaustive. There are doubtless other factors at work which would be revealed by further systematic research. Second, the 13 factors are not presented in any particular order; the tool is offered for the use of other primary care planning teams to conceptualise their decision-making. Third, the 13 factors are interdependent; they dynamically influence each other when decisions are being made about specific priorities.
1. Data comparison (state-wide and catchment level): Data comparison refers to using comparative epidemiological data to identify priority health needs within a given catchment. Such data include demographic profiles, morbidity and mortality statistics, hospital admission data, measures of community health and wellbeing, and indicators of socio-economic disadvantage. Datasets are sometimes available to enable comparisons at a community, local government area, regional, state-wide and national level. Where it is apparent that the catchment is experiencing poorer health status or disadvantage relative to the average (or benchmark) in other catchments, or at state-wide or national levels, then this health issue becomes a priority. Such comparisons are essential to identify the differences that exist in rural areas, as well as the differences that exist between rural and metropolitan populations and where discrepancies in health data are likely to exist. In catchments where multiple disadvantages exist, other contributing factors will need to be considered.
2. Moving upstream to target social determinants of health: One of the core principles for primary health care is addressing and targeting the social determinants of health. These are the underlying social, economic and political conditions that shape the production and distribution of health and illness26. Those who suffer disadvantages are more likely to experience poorer health outcomes and shortened life expectancy. Therefore, priority setting in primary health should be oriented towards the 'upstream' determinants such as employment, housing, education, and transport. However, achieving measurable change on the social determinants of health can be very costly and may take many years of concerted effort and commitment from agencies and stakeholders towards agreement on shared goals, for both medium and long-term future. Other political considerations are will be discussed.
3. Identifying the scale of the problem (number of people affected): The scale of a particular health problem refers to the number of people in a given catchment who are directly and indirectly affected by it. Epidemiological and demographical data can be used to identify the scale of a problem, such as the number of: (a) people with type II diabetes; or (b) child protection notifications; or (c) young people who are disengaged from employment, education and training. There are, however, limitations to relying solely on this factor to determine health priorities, for example data may be unreliable or out of date. It can also be difficult to quantify the number of people indirectly affected by a health issue (eg the number of households where both parents are unemployed, or the number of informal carers for a cancer patient). Moreover, the scale of a problem is better assessed over time, suggesting that longitudinal or trend data may be necessary. One final consideration for this priority is that the scale of a specific problem does provide information about its cost to society or the economy. For example, are the 750 people living in sub-standard housing a greater priority than 750 people living in isolated towns who do not have access to private or public transport? The scale of a health problem is only one consideration in setting health priorities.
4. Impact of problem (morbidity and mortality): This factor is concerned with the impact or consequences of a health problem, such as the social, economic, and even environmental impact of a particular problem. These impacts are identified using measures or terms such as quality of life, financial cost to the individual and the health system, and social costs such as stigma associated with particular health problems, for example obesity. Data on some issues are readily available, such as Disability Adjusted Life Years (DALYs) which provides a measure of the number of years of life lost prematurely as a result of death or the number of years of life lived with disease27. Other agencies also publish impact costings, such as the Productivity Commission28 (eg calculating the economic costs of ageing and unemployment), and the Australian Institute of Health and Welfare (quantifying the burden of particular diseases). Such information can provide a useful measure of the impact of a health problem at a catchment level but it is important to note that a measure of impact is not available for all health problems, particularly those less overt, or inherently more qualitative and therefore less able to be measured, for example the stigma of obesity or political disengagement.
5. Aligning priority with governments' priorities and targets: This factor refers to setting local catchment health priorities that are aligned with the policy priorities and goals within relevant jurisdictions. At one level, this is a relatively straightforward procedure: policy documents, strategic plans and funding agreements set by relevant local, state and federal governments are reviewed to ensure that the catchment health priorities are in accord. For example, the Victorian Department of Human Services29 had set the following priorities for PCPs preparing their three-year health plans: promoting mental health and wellbeing; promoting physical activity and healthy communities; and promoting accessible and nutritious food. At another level, policy-making and implementation is a 'messy' and contested business. The health and welfare agency members of the PCPs are themselves funded by many different organisations, programs, departments, and levels of government. Program funding cuts across geographical boundaries and time periods resulting in the potential for overlapping and competing priorities. Moreover, PCP member agencies are both collaborators and competitors for funding. Ensuring that local catchment health priorities are aligned with stated priorities and targets is an administrative procedure interwoven by political positioning and strategic decision-making.
6. Maintaining progress with existing community health plan initiatives: Achieving improvements in population health outcomes requires a staunch commitment to long-term change; often, significant improvements will not be seen for 10-15 years26. This means that to maintain progress it is essential that plans for community health maintain their focus beyond annual and even triennial cycles. The setting of health priorities must therefore demonstrate a firm resolve to undertake sustained action on the deeper structures affecting population health. However, this degree of resolve can prove difficult, especially when changes occur in government, let alone changes to priorities and targets or when a redistribution of funding occurs. New health problems demand urgent attention while others lose priority and recede from attention. However, local catchments must be responsive to rapid changes in health needs, as was demonstrated by the devastating bushfires in rural Victoria in 20098.
7. Available resources to solve problems: Some health issues (such as the provision of adequate, secure housing for all members of a community) require substantial financial outlays. A primary consideration when setting priorities is to assess the existing and future resources available to address the specified health problem. Other health issues (such as developing improved levels of community respect and inclusion) will require less financial support but greater persistence and community effort to change cultural beliefs and institutional practices. In summary, the resources available to address a health problem and support a new initiative will include dedicated or allocated program/service funding, as well as financial or in-kind contributions from health and welfare agencies.
8. Considering the values of all members (ensuring all members of society have their basic needs met): When setting priorities, economic, policy and political factors are usually to the fore. However, the set of values held by agencies and community members, although rarely articulated, deeply underpins many of the debates about priorities. For example, should priorities focus on the group in greatest need, such as those who experience serious and multiple disadvantages? If so, the Socio-economic Indexes for Areas (SEIFA) Index30 enables the neediest communities to be identified down to neighbourhood, town or postcode level. Or should all members of society first have assured their basic needs for housing, food, access to affordable utilities, education, and employment before other needs are addressed? Should services be universally provided or selective or subsidised, or based on the principle of mutual obligation? What balance should be struck between the allocation of resources to health promotion and illness prevention, and to the treatment of diseases and injuries? Should those who knowingly take health risks have a lower priority for health services allocation? Values clarification is essential for focused, long-term planning.
9. Consumer voice and consumer action: Consumers and stakeholders are the actual, intended recipients of a health program. The importance of a 'consumer voice' is widely recognised as integral to the process of priority setting1,26,31, and is also seen as important by the consumers and their advocates17. Certainly, genuine participation in and 'ownership' of a program during its development increases the likelihood of uptake by consumers and improves program effectiveness. However, a number of problems can arise when implementing this principle. These include issues that range from determining the aim or intention of seeking consumer input (consultation-only or for advice or collaboration or empowerment?); the methodologies or strategies necessary to obtain appropriate consumer participation; the level of importance attributed to each consumer response; and how these are reconciled among various consumers and consumer groups. Within the current project, consumers' views were represented in at least 3 ways, through: (i) consumer representation on committees at the agency level; (ii) needs analyses that provided some project data; and a consumer representative advisory group of the CHPCP. However, there was no direct consumer involvement in the setting of priorities for the catchment healthcare plan.
10. Assessing the financial cost of not addressing the problem: Setting priorities involves making choices. As such, it is concerned with achieving positive outcomes as well as reducing the cost of negative ones, and reckoning the opportunity cost - that is, the cost of not taking action to address a particular health issue. Considering the financial cost of not addressing a problem is an important consideration; however, in many instances reliable costings of the impact of certain health problems is not available. While it can be relatively easy to calculate the costs of influenza (eg by summing the costs of vaccination programs, hospital treatments, premature death, and days off work), it is much more difficult to calculate the cost of homelessness, or of young people who are disengaged from education and employment. Within Australia, agencies including the National Centre for Social and Economic Modelling32, the Productivity Commission28 and the Australian Institute of Health and Welfare33 have performed calculations of the cost of various health problems, initiatives and reforms, which can be useful inclusions in discussions when setting priorities.
11. Leveraging off other concurrent initiatives: At any one time, a range of local, regional, state, national and global health initiatives will target specific health priorities. For example, to reduce the number and severity of traffic accidents, at least 4 organisational levels are at work: (i) the Australian Federal Government funds 'Accident Blackspot' road improvement works; (ii) the Victorian Transport Accident Commission runs television advertisements about wearing seatbelts and safe driving; (iii) regional divisions of the Victoria Police conduct alcohol breath-testing campaigns; and (iv) volunteer groups offer 'driver reviver' stops along major highways during holiday periods. Thus, catchment-level health priority initiatives can complement and effectively 'leverage off' programs that are being run by agencies operating at other levels. By having a comprehensive understanding of these programs, primary healthcare agencies in local catchments can select health priorities that have a stronger likelihood of success. Leveraging, however, also raises methodological concerns, particularly with regard to evaluating the impact and outcomes of the local initiative: how will an evaluator disentangle the effects of multiple, concurrent initiatives that have overlapping goals?
12. Potential to produce improvement (immediate and sustained): Health planning requires that the potential improvement of a new program can be maintained - particularly in the longer term. However, sustained improvement is compromised by 'pilotitis' (which refers to the dissatisfaction felt by stakeholders and service providers alike when one-off pilot projects which have been effective do not receive recurrent funding or are limited in their geographical catchment34). 'Pilotitis' reflects the very real pressures on service providers to demonstrate that they can achieve demonstrable results within the funding project timelines (typically from one to 3 years). The implications for setting health priorities are that agencies must strike a balance between realising immediate success and building program sustainability.
13. Strength of evidence base (degree of certainty to produce improvements): The strength of the evidence base is an increasingly important consideration in setting priorities in primary health care. Systematic reviews of the effects of a wide range of clinical interventions in medicine are now readily accessible through the Cochrane Collaboration and many agencies (ie Australia's National Health and Medical Research Council) are issuing clinical guidelines based on these systematic reviews of the evidence base. Reviews of interventions in other fields more relevant to primary health care (ie education, justice and welfare) are progressively becoming available through the Campbell Collaboration, and evaluations are also becoming a required component built into the funding budget of many new projects. This is heightening expectations that the strength of the evidence base be considered in setting health priorities. For example, WHO's Commission on the Social Determinants of Health26 has declared it a major goal to invest in generating and sharing new evidence on the social determinants of health and on the effectiveness of strategies to reduce health inequities through action on the social determinants. Research knowledge in primary health is underdeveloped compared with the medical field, and there are many complications in implementing successful interventions in primary health compared with clinical medicine35.
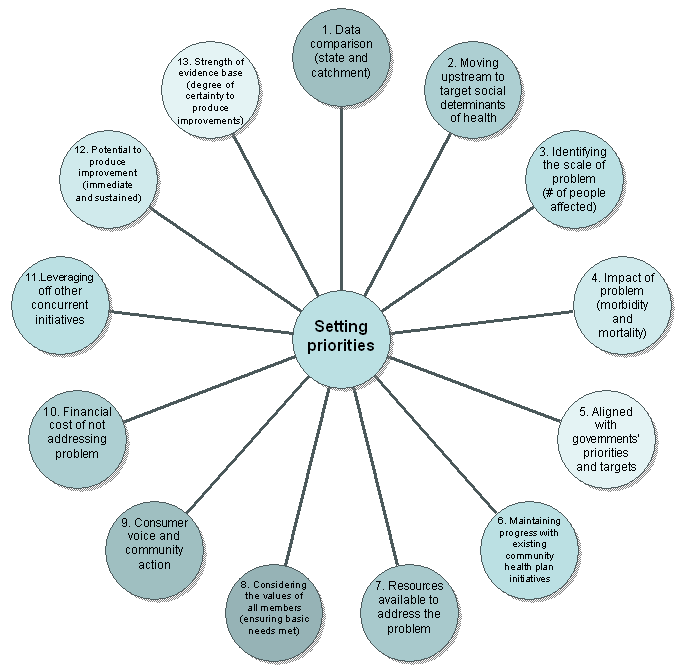
Figure 1: A model for priority-setting in primary health care.
What can be learnt from this practice innovation?
This practice innovation advances current knowledge about priority setting in four ways. First, it reveals the complex, multidimensional, interdisciplinary constellation of factors operating to shape the setting of health priorities. While economic considerations are critically important in resource allocation, it is apparent that moral, political, epidemiological and programmatic factors, as well as the demand for interventions that are evidence-based, all come into play. Second, this practice innovation reveals how priority setting resists simple quantification. All 13 individual factors do not easily lend themselves to weighting, measurement or ranking, and thus it is not feasible to derive a score that pinpoints which health need should be prioritised above others. This is an approach that invites discussion, debate, and reflection. Third, this is a heuristic model, based on the real-world experiences of a group engaged in the process of priority setting. Like many decision-makers, these participants did not utilise formal tools or methodologies1, and thus, through this model, the authors have conceptualised the 'practice wisdom' or 'the ability to base sound judgements on deep understandings in conditions of uncertainty'36 applied by experienced health practitioners and managers.
Fourth, this practice innovation reveals that meso-level planning (that is, at the local catchment or regional health authority level) brings additional complexities to priority setting beyond that experienced at the micro level of planning (for example, program or individual agency level). In this case, meso-level planning through the PCP requires more than 30 agencies to work together to set priorities. Outside the partnership, some of these agencies compete and, at other times, collaborate for project funding. The agencies are from different sectors, have diverse governance arrangements, and are funded from various government and non-government sources. Each agency has its own priorities and strategic goals to achieve. Therefore, setting priorities through a partnership arrangement at the meso-level can entail trade-offs between individual agency and collective priorities. Meso-level planning can challenge territorial and professional boundaries, and overturn entrenched ideas about the 'ownership' of specific client groups by agencies (eg that people with mental health issues are the sole 'responsibility' of psychiatric services).
Compared with metropolitan areas, primary health services in rural and remote locations face additional challenges: the greater geographical area, a dispersed population, lack of specialist services, and complex and often complicated health issues of the community. Priority setting therefore provides a mechanism for the sometimes competing agencies to unite and share in addressing common health problems from a more objective base. Each of the different priority factors outlined in this article provides a basis to start discussions and to consider current and future implications for setting health priorities.
Conclusions
There is growing recognition in the research literature that health priority setting approaches should be interdisciplinary and collaborative. However, there is little consensus about exactly what approach, methodology or tool should be used, and some evidence that health care professionals have limited knowledge of these approaches or even engage in explicit decision-making about priorities. The reality is that priority setting is complex and value-laden, involves trade-offs between competing objectives, must consider resource constraints, and is contorted by political cycles. The model presented here captures the full range of factors considered by participants in one PCP as they assessed health needs in the catchment and drafted a new three-year community health plan. Economic variables are but one factor among a host of political, policy, epidemiological, moral, evidentiary and evaluative considerations. The fact that the participants were not explicitly using a formal approach suggests that the model may have some heuristic value for other participants in primary health care alliances responsible for setting regional priorities.
References
1. Sibbald SL, Singer PA, Upshur R, Martin DK. Priority setting: what constitutes success? A conceptual framework for successful priority setting. BMC Health Services Research 2009; 9: 43.
2. Ham C. Priority setting in health care: learning from international experience. Health Policy 1997; 42: 49-66.
3. Kapiriri L, Norheim OF, Martin DK. Fairness and accountability for reasonableness. Do the views of priority setting decision makers differ across health systems and levels of decision making? Social Science and Medicine 2009; 68: 766-773.
4. Mitton C, Patten S, Waldner H, Donaldson C. Priority setting in health authorities: a novel approach to a historical activity. Social Science and Medicine 2003; 57: 1653-1663.
5. Patten S, Mitton C, Donaldson C. Using participatory action research to build a priority setting process in a Canadian regional health authority. Social Science and Medicine 2006; 63(5): 1121-34.
6. Department of Health and Ageing. Primary Health Care Reform in Australia. Report to Support Australia's First National Primary Health Care Strategy. (Online) 2009. Available: http://www.yourhealth.gov.au/internet/yourhealth/publishing.nsf/Content/nphc-draftreportsupp-toc/$FILE/NPHC-supp.pdf (Accessed 30 May 2010).
7. Victorian Department of Health. Primary Care Partnerships. (Online) 2009. Available: http://www.health.vic.gov.au/pcps/ (Accessed 30 May 2010).
8. Victorian Department of Health. Primary Care Partnerships. Planning and Reporting Guidelines, 2009-2012 (Online) 2009. Available: http://www.health.vic.gov.au/pcps/downloads/strategy/pcp_planningreporting_guidelines.pdf (Accessed 30 May 2010).
9. Delaney L. Primary Care Partnerships: more than just one relationship. Australian Journal of Primary Health 2009; 15: 212-217.
10. Central Highlands Primary Care Partnership. Information about the Central Highlands Primary Care Partnership. (Online) 2009. Available: http://www.chpcp.org/The%20Central%20Highlands%20Primary%20Care%20Partnership.doc (Accessed 30 May 2010).
11. Dolan P, Cookson R, Ferguson, B. Effect of discussion and deliberation on the public's views of priority setting in health care: focus group study. BMJ 1999; 318: 916-919.
12. Mullen P, Spurgeon P. Priority setting and the public. Oxfordshire: Radcliffe Medical Press, 2000.
13. Shah K. Severity of illness and priority setting in healthcare: a review of the literature. Health Policy 2009; 93(2): 77-84.
14. Gibson J, Martin D, Singer, P. Priority setting in hospitals: fairness, inclusiveness, and the problem of institutional power differences. Social Science and Medicine 2005; 61: 2355-2362.
15. Holm S. Goodbye to the simple solutions: the second phase of priority setting in health care. BMJ 1998; 317: 1000-1007.
16. Olsen J. Theories of distributive justice and their implications for priority setting in health care. Journal of Health Economics 1997; 16(6): 625-639.
17. Wiseman V, Mooney G, Berry G, Tang KC. Involving the general public in priority setting: experiences from Australia. Social Science and Medicine 2003; 56: 1001-1012.
18. Mitton C, Smith N, Peacock S, Evoy B, Abelson J. Public participation in health care priority setting: a scoping review. Health Policy 2009; 91: 219-228.
19. Tenbensel T. Interpreting public input into priority-setting: the role of mediating institutions. Health Policy 2002; 62: 173-194.
20. Chambers R. Involving patients and the public - is it worth the effort? Journal of the Royal Society of Medicine 2001; 94: 375-377.
21. Peacock S, Mitton C, Bate A, McCoy B, Donaldson C. Overcoming barriers to priority setting using interdisciplinary methods. Health Policy 2009; 92(2-3): 124-132.
22. Schon D. The reflective practitioner. New York: Basic Books, 1983.
23. Fook J. The reflective practitioner: developing a reflective approach to practice. In: J Fook (Ed.). The reflective practitioner. Sydney, NSW: Allen and Unwin, 1996.
24. MacLeod M, Lindsey E, Ulrich C, Fulton T, John N. The development of a practice-driven, reality-based program for rural acute care registered nurses. Journal of Continuing Education in Nursing 2008; 39(7): 298-304.
25. Pond B, Dalton L, Disher G, Cousins M. Helping medical specialists working in rural and remote Australia deal with professional isolation: the Support Scheme for Rural Specialists. Medical Journal of Australia 2009; 190(1): 24-27.
26. World Health Organisation. Commission on the Social Determinants of Health, Closing the Gap in a generation: health equity through action on the social determinants of health 2008. Final Report of the Commission on the Social Determinants of Health. Geneva: World Health Organisation, 2008.
27. Department of Human Services Public Health Branch. Burden of Disease (BoD). LGAs and Regions 2001. (Online) 2006. Available: http://www.health.vic.gov.au/healthstatus/bod/bod_reg.htm (Accessed 30 May 2010).
28. Productivity Commission. Economic implications of an ageing Australia. Canberra, ACT: Productivity Commission, 2005.
29. Department of Human Services. Primary care partnerships. Promoting healthy communities. (Online) 2008. Available: http://www.health.vic.gov.au/pcps/downloads/health_comm.pdf (Accessed 30 May 2010).
30. Australian Bureau of Statistics. Socio-economic Indexes for Areas. (Online) 2008. Available: http://www.abs.gov.au/websitedbs/D3310114.nsf/home/Seifa_entry_page (Accessed 30 May 2010).
31. Mitton C, Donaldson C. Priority setting toolkit: a guide to the use of economics in health care decision making. London: BMJ, 2004.
32. National Centre for Social and Economic Modelling, University of Canberra. Commonwealth financial planning. Women Carers in Financial Stress Report. (Online) 2009. Available: http://www.carersaustralia.com.au/uploads/CFP%20Report.pdf (Accessed 30 May 2010).
33. Australian Institute of Health and Welfare. Australia's Health. Australia's health series no 12. Cat no AUS 122. Canberra, ACT: AIHW, 2010.
34. Kuipers P, Humphreys J, Wakerman J, Wells R, Jones J, Entwistle P. Collaborative review of pilot projects to inform policy: a methodological remedy for pilotitis? Australia and New Zealand Health Policy 2008; 5(17). Available: http://www.anzhealthpolicy.com/content/5/1/17
35. Glasgow N, Marley J, Kristjanson L, Donovan J, Hall S, Harris M et al. Bringing evidence to bear on policy processes: the challenge of the Australian Primary Health Care Research Institute. Medical Journal of Australia 2008; 188(8Suppl): S46-49.
36. O'Sullivan T. Some theoretical propositions on the nature of practice wisdom. Journal of Social Work 2005; 5(2): 221-242.
