This article reports the development, implementation and evaluation of a professional development program for international medical graduates (IMGs) working in Gippsland. In Australia, IMGs constitute more than one-quarter of the medical workforce1. IMGs make a major contribution to the delivery of patient care in Gippsland, Victoria. Although the wealth of professional experience that IMGs bring is recognised and valued, there has been considerable discussion about their competence and need for educational support, especially at the beginning of their placement in Australia, and particularly when located in rural settings. In this project, clinicians across Gippsland worked with faculty from the Gippsland Medical School (GMS) to develop, implement and evaluate a program designed to support IMGs. The program was called Gippsland Inspiring Professional Standards among International Experts (GIPSIE).
An underpinning philosophy of the GIPSIE program was the desire to provide a learning environment that was flexible, supportive and motivating. It aimed to adopt the best evidence for education and health service and, wherever possible, this was contextualised for local practice. Generic program aims were to:
- Provide IMGs with an opportunity to further develop knowledge, attitudes and skills for safe and effective clinical practice in Gippsland.
- Develop individual IMG's self-awareness of strengths and areas for development.
- Promote Gippsland as a region regarded as supportive of IMG education and training.
Literature on international medical graduates
There are several recent literature reviews in Australia and abroad documenting IMG experiences and the content of orientation programs2-5. Here the focus is on the Australian literature. Most areas of medical practice are experiencing workforce shortages6,7. These shortages have been attributed to the increasing demands of an ageing population and a reduction in the hours worked by medical doctors and have led to the growing dependence on IMGs7. IMG recruitment has been a strategy of workforce planning to overcome shortages. Designated areas of need are heavily dependent on IMGs to maintain workforce8. However, there are unanswered questions regarding the appropriateness of IMG training, orientation and support8,9 for working in rural contexts. Emergency departments outside major cities rely on IMGs. However, there are no training or education standards for these departments, with most doctors feeling the need for further training10. IMGs usually come from cultures markedly different to that in rural Australia, and English is not their first language. IMGs are often poorly orientated to the local healthcare system and there is a paucity of resources to support their ongoing training and educational needs. Moreover, there is limited funding to support existing doctors in their efforts to teach and nurture this large and important group working in rural Australia.
Needs of international medical graduates: A survey of GPs in rural practice, both IMGs and Australian graduates, revealed similar perceptions regarding professional development needs, training opportunities, professional support, networking and financial support6,11. Another survey found that English language communication and understanding the Australian healthcare system were common areas of need12. A qualitative study of IMGs in general practice training found that language and communication, cultural issues, understanding the Australian healthcare system, clinical knowledge, consulting styles and registrar support were areas of challenge during transition to a new position13.
McGrath described IMGs' needs as including the need for information, orientation to healthcare systems and workplaces, improved communication skills with both patients and co-workers, emphasising the requirement for standardised assessment of knowledge and skills, and education and training support14. IMGs have been found to have gaps in medical knowledge, clinical reasoning skills and communication skills15.
Orientation/support/education programs for international medical graduates: Effective orientation can assist IMGs in the transition to practice in a new country, reduce isolation and enhance integration into new community16. In Australia there is no national approach to support the integration of IMGs into the workforce14. A small study examined orientation of IMGs to a rural community and found that the median orientation length was one week, with preference among IMGs being for 2 weeks; 25% of the sample had no formal orientation, with only just over half being satisfied with their orientation17. Orientation topics given the highest importance by IMGs were clinical and financial issues, and the lowest importance was assigned to social topics, with confidence ratings matching these preferences17. Suggested improvements included a paid orientation, visits to several practices, more question time and more emergency medicine updates. The study also found that problems settling in could have been reduced with more information about the community, job information for spouses and the availability of a car17.
An evaluation of a pre-employment program was undertaken with 66 IMG participants5. This 4 week, full-time program included communication, health and workplace skills; sessions on culture shock and the role of the junior doctor, with confidence and attitudes towards general duties and workplace skills measured5. Results included reports of greater understanding of staff and communication issues, familiarisation with the hospital environment, a more realistic understanding of their role and future professional development needs and the establishment of a peer network5.
A systematic review of the literature about communication issues faced by IMGs was undertaken to provide training organisations with the background needed to understand the issues18. The findings of the literature review included the need for: IMGs to adjust to a change in status; clinicians to understand the high level of language proficiency required of IMGs; the development of IMGs' communication skills; clinicians to understand IMGs' expectations about teaching and learning; and IMGS to be able to interact with a variety of people18.
The GIPSIE program
Educational theory and methods: The GIPSIE program draws on theories of expertise, contextualised learning, reflective practice and principles of adult learning. Expertise develops when individuals are given the opportunity for deliberate practice and feedback19. That is, learners are given the opportunity to actively seek to improve their performance together with expert judgments on their strengths and areas for development. Contextualisation of learning refers to the process in which learners are taught in the setting in which they are expected to practice20,21. This is sometimes referred to as situated learning. It was proposed to recreate settings in simulation-based education through environments that reflected the physical, psychological and social fidelity of clinical practice. Reflective practice encourages learners to understand their actions by 'reflecting' on their strengths and areas for development in specific scenarios, followed by developing strategies to maintain their strengths and improve less effective practices22-24. Adult learning principles ensured that the program was interactive and experiential, aligned with participants' current working practice and addressing their individual needs25.
Development of content
This research focused on commonly occurring clinical events to support participants in their everyday practice. Issues known to be challenging for IMGs were identified and explored. Content was developed in conjunction with local physicians, surgeons, emergency physicians and paediatricians. Additionally, the program drew on the Australian Curriculum Framework for Junior Doctors26 and was aligned with material offered by the Postgraduate Medical Council of Victoria (PMCV)27. A summarised version of content is listed (Fig1); while participants' ratings of the learning objectives are given (Table 1), as are their ratings of the educational methods (Table 2). Further information is available on the GIPSIE website.
The key stages of GIPSIE are provided (Fig2). After multi-source feedback (MSF), the program began with a questionnaire-based learning needs analysis designed to ensure that program content was individualised, an important step in promoting receptiveness to learning. An immersion weekend workshop preceded 4 fortnightly evening meetings. There were 24 contact hours and an additional 3 hours of observed clinical practice. A combination of massed and distributed learning was adopted, supported by web-based, self-directed and interactive learning methods between sessions to ensure continuity and application of learning.
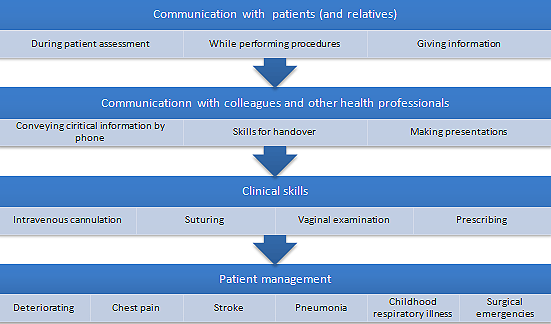
Figure 1: Summary of content of the GIPSIE program.
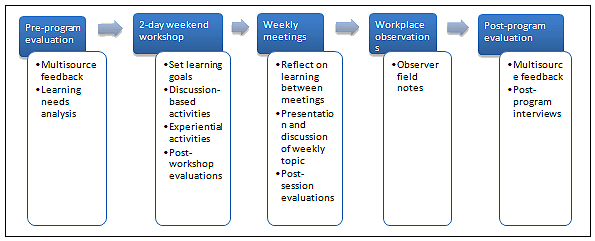
Figure 2: Key stages of the GIPSIE program.
Table 1: Participants' (n=17) ratings of the degree to which they met learning objectives
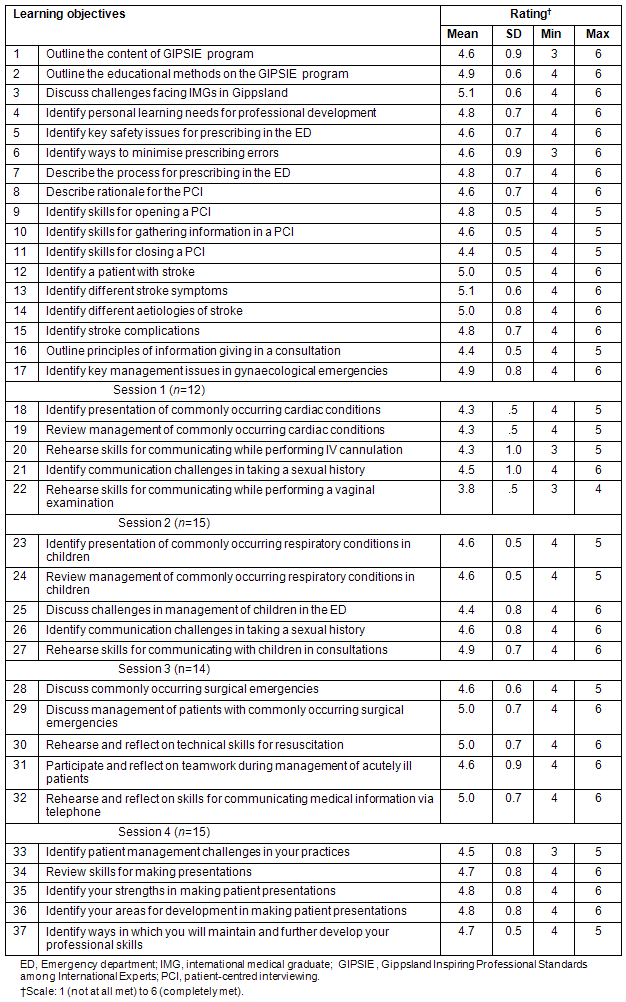
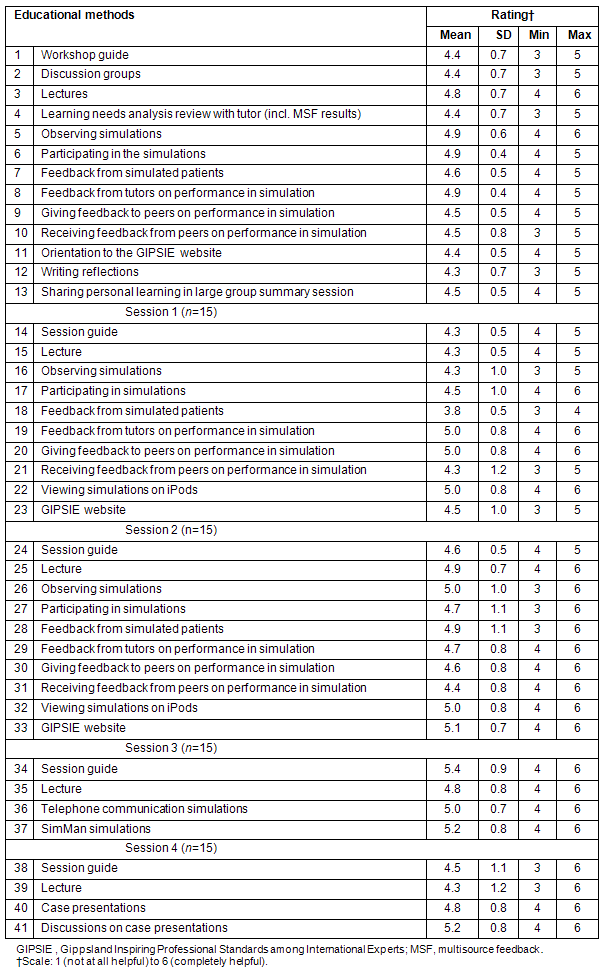
Table 2: Participants' (n=17) ratings of the value of the educational methods
Simulated consultations
Participants were given an opportunity to participate in simulated patient (SP) encounters based on commonly occurring scenarios from local practice. Orientation to simulation was a feature of the program. While the SPs provided feedback from a patient perspective, clinical experts provided feedback on medical elements28. Simulated consultations enabled a wide range of topics to be addressed through realistic patient encounters. Interactions were videotaped using digital recording facilities and played back to participants for review. This approach is widely acknowledged as a powerful learning approach29,30. The iPod nano devices enabled participants to have later audiovisual access to their simulated encounters. This was considered particularly important given that English was not their first language and the opportunity to review performance was likely to be helpful. IMGs were provided with the chance to practise a range of communication skills relevant in patient and clinician interactions: reflective listening, empathic skills, and use of open-ended questions, as well as rapport building skills and dealing with difficult situations. The communication content of the program drew heavily on a previously published curriculum31.
Procedural and examination skills: An approach was adopted to simulation-based education that integrates SPs with a simulator (eg suture pad) or medical equipment (eg ECG machine) within a simulated clinical setting. These hybrid simulations enable participants to integrate the complex range of psychomotor, interpersonal, professional, clinical decision-making and patient safety skills in an environment safe for learners and without harm to patients28,32-35. Two skills the PMCV lists as relevant for IMGs entering practice in Victoria were selected: suturing and ECG interpretation.
Management of deteriorating and acutely ill patients: Participants had the opportunity to participate in a simulation scenario focusing on the management of an acutely ill patient. Scenarios required participants to have sufficient clinical knowledge and judgment to recognize a deteriorating patient, to explore principles of effective teamwork and to reinforce principles of patient safety. Again, audiovisual capture enabled later review. Opportunities were provided for simulation-based training for handover and telephone communication skills including conveying urgent information clearly and concisely.
GIPSIE website: An important goal was to develop a learning community within Gippsland. The website aimed to provide flexible learning before, during and after sessions that was accessible anytime and anywhere. Website content included a communication board, learning paths, case of the week, image of the week, quizzes, newsletters, web links and more.
Research questions
The research questions were:
- To what extent is it possible to support professional development of IMGs in a regional setting?
- What aspects of the GIPSIE program were effective?
- What aspects need improvement?
Recruitment of participants
Directors of medical services in Gippsland were asked to identify potential participants. GIPSIE was introduced to participants locally and then by letter of invitation. Positions were allocated sequentially, with an ability to commit to the entire program and representation across several institutions being the criteria for inclusion.
There were 4 main instruments in the evaluation:
- Demographics and experience of Gippsland (pre-program)
- Baseline learning needs forms (pre-program)
- Multisource feedback (pre- and post-program)
- Participants' response to program (workshop and end-of-session evaluations, and telephone interviews).
Demographics and experience of Gippsland (pre-program): A questionnaire was developed to record age, sex, experience of living and working in Gippsland, career goals and experience of a range of educational methods. Responses included ratings of satisfaction and free text responses.
Baseline learning needs forms (pre-program): Participants identified their expectations and learning goals for the GIPSIE program in a questionnaire. Responses were in free-text format.
Multisource feedback (pre- and post-program): Based on an MSF form used in the UK for junior doctors, the IMG nominated colleagues to make judgments on facets of clinical practice. A six-point scale recorded level of competence. Participants were also asked to self-assess using this form, so they could start to construct a picture of how they see themselves compared with the perceptions of others.
Participants' responses to the program: Immediately after sessions and at the end of the workshop, participants were asked to rate the degree to which they met learning objectives and the educational methods used. Six-point rating scales were used (from 1 = 'not at all met or not at all helpful' to 6 = 'completely met or helpful') and free text, where participants were asked to identify what worked well and what needed to be improved. Three months after GIPSIE, a telephone interview explored participants' experiences of the program emphasising the transfer of learning.
Data analysis
Quantitative data were entered into SPSS v17.0 (www.spss.com) for analysis. Descriptive statistics summarised data. Individual differences pre- and post-program were identified using the Wilcoxon signed-rank test. Statistical significance was established at p<0.05. Qualitative data (free-text comments and interview data) were thematically analysed independently and then agreement negotiated by the researchers (DN, AW, CH). An external evaluator (CS) reviewed de-identified data to ensure rigorous evaluation.
Human Research Ethics approval
Human Research Ethics Committee approval was obtained from Standing Committee on Ethics in Research involving Humans (SCERH) following the project (# CF08/2794 - 2008001457).
Participant baseline information
Seventeen participants registered for the program (10 male and 7 female), aged 27 to 51 years (mean=35). Participants came from 12 countries (Sri Lanka, the Philippines, Colombia, India, Bulgaria, Bangladesh, Iran, Afghanistan, Vietnam, China, Egypt and Bosnia) and spoke 14 languages (other than English). Participants had been in Australia between 2 and 120 months (mean=46) and in Gippsland for 2 to 42 months (mean=13). Thirteen had previously attended educational programs designed for IMGs. Four had prior experience with part-task trainers, eight with manikins and 11 with SPs. Participants reported their experience as minimal. Two participants had prior experience of MSF and three of analysis of learning needs. Seven had experience of using video review. On a six-point scale, their mean rating of enjoyment of workplace was 4.7 (range=2; SD=0.6) and perceived support in their workplace was 4.3 (range=3; SD=0.9).
Challenges of being an international medical graduate in Gippsland
Participants identified several challenges that can be broadly classified into overlapping categories: professional issues including education, assessment and communication; and cultural issues, specifically including working in Gippsland.
Professional issues: All of the challenges identified had a professional component. Those who were previously consultants encountered challenges in having to prove themselves in their new, more junior capacity. Relearning skills was confronting and not without difficulty. Similarly, working under supervision was sometimes threatening, although almost always appreciated. Constructive and positive supervision was highly valued.
Participants were confused by the selective use of protocols in Australian healthcare settings. They reported a need for greater support at work especially after hours, and suggested that more could be done to encourage doctors who have completed the rotation to support incoming IMGs.
Participants highlighted the value of the opportunity to share their experiences of their new roles and communities. They raised issues on dealing with administration, mentoring, study support and racism. Major terrorist activities had heightened local sensitivities. There was overwhelming support for improved orientation or induction to the workplace.
Participants wanted more education and assessment that acknowledged their prior experience and full registration as 'Australian' doctors. They described a need to 'refresh' their knowledge because, as 'senior' doctors elsewhere they had not performed many procedures that were now part of their daily work. Although confident in identifying many of their patients' presenting conditions, they were unfamiliar with local treatment regimens.
Communication with patients, their relatives, peers and consultants (in person, by telephone or in writing) was a critical issue for each participant. Jargon and colloquialisms were problematic. Communicating with consultants was a particular problem and telephone communication was also difficult.
Cultural issues: Several aspects of culture were identified as challenging including the workings of the local hospital unit/emergency department, its relationship with the rest of the hospital, participants' own roles and responsibilities and those of others in the healthcare team and the broader Australian healthcare system. The process of patient referral was also different from the systems participants were familiar with. Although largely viewed positively, living in a rural environment was identified as new. Most participants had come to Gippsland from an urban area. Participants wanted orientation to the local community.
Reasons for working in Gippsland related almost always to job opportunities and, for some, a preference for living and working in a regional and rural setting. Participants reported they enjoyed Gippsland for the people, its geography and recreational opportunities while they disliked the lack of public transport, winter weather, limited multiculturalism and educational opportunities for children, and some of the heavy industry. Just over half the participants intended to stay in Gippsland and gave reasons such as opportunities for work and training. For those who did not want to stay, their reasons included no opportunities for their partner to work, restricted training opportunities and a limited social network.
Baseline learning needs
Pre-program each IMG recorded their personal program goals. These were adjusted after they had received their summarised MSF, and in discussion with a faculty member. Dominant themes within the participants' goals included development of general management of patients and specific clinical skills (eg lumbar puncture, central line insertion, chest drains). Communication was consistently identified as a goal, including communicating with patients and their relatives and with colleagues, in person and in writing; and specifically, insight into the use of colloquialisms and acronyms. Additionally, participants aimed to improve their understanding of hospital operations and the broader Australian healthcare system. Thus, the IMGs could clearly articulate specific skills and knowledge that would assist them to work more effectively in their current clinical contexts.
Multi-source feedback
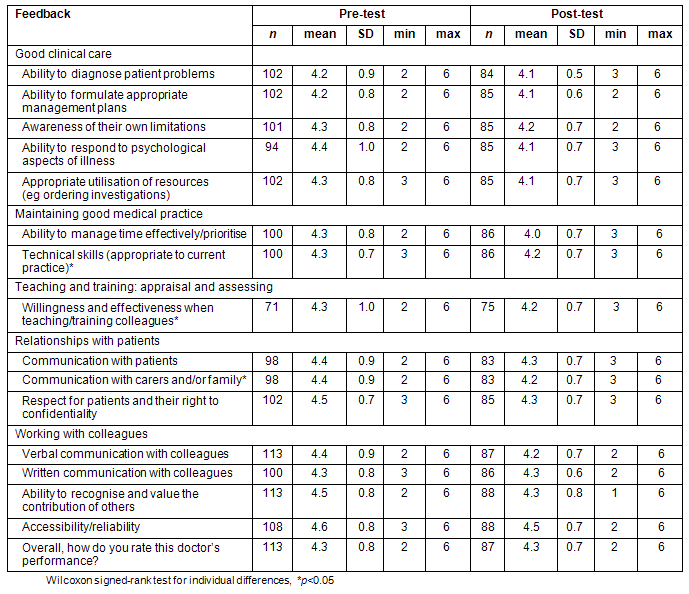
Fifteen participants completed the program and only their results are included in the MSF results. Pre-program, participants identified colleagues to complete the MSF. The same colleagues were contacted post-program to complete the MSF again. Forms were obtained from two to eight colleagues per participant at the points of testing; summary data are provided (Table 3). As a group, participants were considered to be safe and competent (mean scores exceeding 4) across all variables before and after GIPSIE. However, the range of scores suggested that some participants were less than safe and competent or borderline (mean scores at 2 or 3, respectively). Using the Wilcoxon signed-rank test to detect individual differences before and after the program, statistically significant and positive changes were identified for three variables: (i) technical skills appropriate to current practice; (ii) willingness and effectiveness when teaching/training colleagues; and (iii) communication with carers and family.
Table 3: Summary results of multisource feedback for all participants pre- and post-program (n=15)
Pre-program, MSF free text comments proved especially valuable in identifying participants' strengths. Examples include willingness and enthusiasm to learn, ability to communicate with colleagues, diligence and an ability to work hard. Specific elements of behaviours that were reported to need development included communication with patients, their families and colleagues, English language (including heavily accented English), planning and organising care, documentation, selecting appropriate tests, clinical knowledge, adherence to hospital protocols and improving confidence.
Post-program, many more strengths were identified than areas for development. These aspects also addressed items raised at the pre-test. Strengths included personal qualities, clinical ability, and communication with patients, their families and colleagues. Assessors who completed forms post-program often phrased their comments as improvements. Examples of development included time management and conflict resolution (with staff). This indicates that GIPSIE was successful in providing an infrastructure for IMGs to develop required knowledge, attitudes and skills that underpin safe and effective clinical practice in a rural setting. Examples of MSF feedback for one participant are provided (Fig3).

Figure 3: Example of free text comments for one participant in multi-source feedback.
Participant evaluations of GIPSIE sessions from weekend workshop and end of sessions
Learning objectives: Participants' ratings of the degree to which they met learning objectives are summarised (Table 1). There were 37 learning objectives. Participants rated the degree to which they met the learning objectives from 3.8 to 5.1 (SD 0.5-1.0; maximum score=6). Mean scores exceeding 5.0 were for the objectives:
Discuss challenges facing IMGs in Gippsland; Identify a patient with stroke; Identify different stroke symptoms; and Identify different aetiologies of stroke; Discuss management of patients with commonly occurring surgical emergencies; Rehearse and reflect on technical skills for resuscitation; and Rehearse and reflect on skills for communicating medical information via telephone.
The first learning objective is generic and could apply to any program designed to support IMGs. The others relate to clinical and professional skills typifying emergency situations which junior doctors and IMGs in a new clinical context are likely to experience.
Educational methods: A summary of participants' ratings of the value of educational methods in supporting them to meet learning objectives is provided (Table 2). Participants' ratings were between 4.3 and 5.3 (SD 0.4-1.1; maximum score=6). Mean ratings fell within a narrow band. Scores that equalled or exceeded 5.0 were:
Feedback from tutors on performance in simulation (session 1);giving feedback to peers on performance in simulation (session 1); observing simulations (session 2); viewing simulation on iPods (sessions 1 & 2); the GIPSIE website (session 2); session guide (session 3); SimMan simulations (session 3); telephone communication simulations (session 3); and discussion of case presentations (session 4).
Strengths of the program: Free text showed that participants enjoyed the experience enormously. They valued the variety of learning methods, focused individualised instruction and feedback, the experience of participating and observing simulated consultations (including the opportunity to integrate all elements of performance), audiovisual review of their own performance and the opportunity to explore clinical knowledge and skills in an integrated manner. Didactic sessions were also highly appreciated.
Areas for improvement of the program: The main area for improvement included constraints on time to complete all activities. Suggestions were made to align scenarios more closely with participants' needs to pass the Australian Medical Council (AMC) examinations. Participants wanted more of what they valued above including individual feedback, access to materials before the session, opportunities for all participants to rotate through all simulations, improved peer feedback and better quality audio in the observation rooms.
Telephone follow up
Key themes from telephone interviews conducted 3 months after completing the program revealed overwhelming satisfaction. Participants were impressed with the allocation of resources to support their learning. Some participants remained uncertain of the purpose of GIPSIE. They had come to the program for diverse reasons and expected support for passing examinations. With respect to content, participants varied in their needs. Some wanted a combination of clinical management and communication while others preferred communication only. Clinical management was reported not to necessarily target the right level or align with participants' practices. For educational methods, the most highly valued experience was role-play, real time feedback on their performance and the communication skills sessions. Participants enjoyed and reported benefits from simulation, especially SPs. They wanted more scenario-based learning. They appreciated the opportunity to work in small groups. They wanted more and longer sessions. The use of the iPod to review audiovisual clips was valued, and for some it was the first opportunity to see themselves performing. Although valued, online learning was not always accessible and connection speeds were too slow. Elements of the website were considered hard to use and not updated. However, participants proposed the website be made available to all clinicians, a move that would create a virtual network of resources and expertise relevant to medical practice in Gippsland. All participants would recommend the program. Participants enjoyed the networking during the course but this has not been sustained. Finally, participants requested more guidance on making sense of MSF results.
Discussion
The GIPSIE program is supportive of the development of professional and clinical skills for IMG participants in Gippsland. This is evidenced by the participants' responses to GIPSIE sessions and their self-reported improvements expressed during telephone interviews conducted 3 months later. The MSF results also indicate that for some variables the program was especially valuable (technical skills, teaching skills and communication with patients' relatives). These changes were also detected 3 months after the program suggesting retention of learning. Free text on MSF forms from colleagues of the participants present an overwhelmingly positive outcome. Additionally, GIPSIE appeared to provide benefits that are not easily measured but likely to have a powerful impact on retention, professional development and safety. That is, the development of a collegial culture in which clinicians feel comfortable to seek help when help is needed, rather than working beyond their competence.
The massed and distributed nature of the program enabled the development of a supportive learning community. The collaborative approach between local clinicians and GMS was a unique strength of the program. Without continued program support, this learning community is likely to fade.
The learning needs of IMG participants in the GIPSIE program reflect those identified in the literature and related to communication and all aspects of clinical practice12-14,20,21,36. The challenges of being an IMG in Gippsland related to cultural, professional and social differences are also reflective of the broader experience7,11,12,20. The content and educational methods were appropriate for the participants even though they were a disparate group of learners.
Participants consistently expressed a need for support in passing high-stakes examinations. Although this was not the goal of the program, the supportive learning community contributed to the development of effective study approaches.
GIPSIE differed to orientation programs because it was not undertaken prior to commencing employment roles. The program was also characterised by its range of educational activities, in particular the learning needs analysis, the website and simulation-based activities. A feature of the evaluation methodology is the MSF which aimed to capture data that showed change in actual practice, rather than simply participant response to the program.
Multisource feedback
The positive comments in free text cannot be confidently attributed to GIPSIE alone. The opportunity to learn in the workplace is likely to have been an important variable in developments. It had been hoped that participating in GIPSIE would instil a culture of learning, facilitating participants to seek help and guidance from peers and others in the workplace, and to recognise that it is important and acceptable to acknowledge areas that require development so others can support their learning. It was also interesting that participants became better teachers after GIPSIE, perhaps acknowledging that they too had something important to offer their peers and colleagues. An aim had been to instil a culture of learning.
Simulation-based education
Participants considered the simulation-based education a positive feature of GIPSIE. Despite minimal experience of simulation-based education, participants quickly responded positively to the range of simulation methodologies, including observing, active involvement, providing or receiving feedback. They consistently rated this type of learning as the most effective educational method of the GIPSIE program. The careful orientation to simulation-based activities is likely to have facilitated success. Although valued, feedback from simulated patients needed further development.
Web-based delivery of modules
Although participants valued the web-based delivery of educational materials, particularly during the weekly sessions, there were constraints on their subsequent uptake. Busy clinical practice and other responsibilities outside work reduced involvement. Access to materials was often not available in workplaces where they would most likely benefit from access to resources 'just in time' (ie access the the right knowledge, attitudes and skills when it is needed). The GIPSIE website has enormous potential as a regional learning resource. Development of online resources to demonstrate clinical practice is highly desirable. There is potential for much greater use of the capabilities of web-based learning. Blogs, wikis and other interactive methods have been shown to be beneficial in other educational settings37,38. Despite the challenges most participants experienced in web-based learning, participants proposed that the GIPSIE website be made available to a wider group of clinicians (and students). Promoting this culture of non-hierarchical learning was a very positive outcome.
The GIPSIE website could provide access to needed just-in-time resources, but it also could sustain a virtual community of IMGs with supportive faculty. The forthcoming National Broadband Network could be exploited to revitalise this resource. The website could also be expanded to provide information about local Gippsland communities and events in order to provide direction to IMGs attempting to assimilate into areas of Gippsland. This medium could be used to track participants' attempts to apply knowledge, skills and attitudes addressed by GIPSIE within the clinical context by means of added features, for example blog posts reporting what challenges are encountered and how these might be overcome in the workplace.
Limitations
Although very comprehensive, there are limitations to the evaluation. The sample is small and highly selective and, therefore, may not reflect a broader IMG population. GIPSIE was developed and implemented by faculty committed to supporting IMG education and so may not readily transfer to other settings. Self-report was used as one measure of progress. There is evidence that such data can be unreliable when participants lack insight or may be influenced by other factors (eg social desirability)39,40. However, this was addressed by adopting other evaluation measures such as MSF.
Future directions
The sustainability of programs such as GIPSIE requires significant human and physical infrastructure. High quality 'patient-safe' training is resource-intensive. Building further capacity across the region will be a major goal given the pressures under which medical and other healthcare professionals are already working. However, this is viewed as a positive challenge and if the infrastructure is in place - web site, high quality learning materials, simulation facilities and expertise to support simulation-based education - then the task will be easier. Providing simulation scenarios that align with the AMC's Anthology of Medical Conditions41 would ensure systematic coverage of important clinical practice. Offering additional sessions would be educationally sound and provide opportunities to refresh skills and develop new ones in a 'safe learning environment' away from the pressure of clinical practice but still in a familiar place with supportive colleagues. This would also provide a forum to maintain the network. Given that some of the IMGs intend to remain in Gippsland this is a potentially critical longer term support. Future evaluation strategies could also adopt online capture of participants' responses to the program and reflections on clinical practice. Innovative work has been conducted with IMGs using this technique42.
The GIPSIE program provided a proof of concept that it is possible to support the professional development of IMGs working in a rural clinical context. This support was developed and tailored to address self and other identified learning needs. Having an educational hub at the Gippsland Medical School with attendant resources supported this endeavour. The program also facilitated the development of a network of directors of medical services in Gippsland representing a wide range of service provision challenges facing these IMGs.
Several aspects of the program should be highlighted - the content of teaching, and that learning was focussed on the learners' areas of need - as having the potential to maximise its impact. The design of the program being consistent with the principles of contemporary evidence-based medical education was likely to have contributed to its success. Participants enjoyed the experience, reported sustainable gains in learning, and wanted more of the same to enhance their development as effective and efficient practitioners.
GIPSIE required a significant investment of resources both on the part of learners and teachers. It would be useful to explore ways to sustain the returns from this initial implementation by recruiting GIPSIE graduates to provide structured support to new IMGs if the program is funded to continue. Also, because assessment clearly drives learning, some program content could address components of the AMC examination, a clearly identified concern for many participants.
Acknowledgments
The authors acknowledge the Department of Human Services (Victoria) for funding, and the following colleagues who offered their expertise: M Bishop, S Greig, D Birks, B Maydom, J Keast, C Rossetti, K Thomas, R Edwards, A Hood, L Snell and A Ng.
References
1. Medical Training Review Panel, Australian Government Department of Health and Ageing. Overseas Trained Doctor Subcommittee Report. Canberra, ACT; Medical Training Review Panel, 2004.
2. Confederation of Postgraduate Medical Education. International medical graduates. Melbourne, VIC: Confederation of Postgraduate Medical Education Councils, 2004.
3. Hawthorne L, Birrell B, Young D. The retention of overseas trained doctors in general practice in regional Victoria. Melbourne, VIC: Rural Workforce Agency Victoria, 2003.
4. Swierczynski M. Induction courses for international doctors. BMJ 2002; 325(S159): 00-00.
5. Sullivan E, Willcock S, Ardzejewska K, Slaytor E. A pre-employment programme for overseas-trained doctors entering the Australian workforce. Medical Education 2002; 36: 316-621.
6. Alexander C, Fraser JD. Education, training and support needs of Australian trained doctors and international medical graduates in rural Australia: a case of special needs? Rural and Remote Health 7(2):681. (Online) 2007. Available: www.rrh.org.au (Accessed 29 November 2011).
7. Spike NA. International medical graduates: the Australian perspective. Academic Medicine 2006; 81(9): 842-846.
8. Arkles RS, Hill PS, Jackson Pulver L. Overseas - trained doctors in Aboriginal and Torres Strait Islander health services: many unanswered questions. Medical Journal of Australia 2007; 186(10): 528-530.
9. Birrell RJ. Australian policy on overseas-trained doctors. Medical Journal of Australia 2004; 181(11-12): 635-639.
10. Arvier PT, Walker JH, McDonagh T. Training emergency medicine doctors for rural and regional Australia: can we learn from other countries? Rural and Remote Health 7(2):705. (Online) 2007. Available: www.rrh.org.au (Accessed 29 November 2011).
11. Alexander C, Fraser J. Professional career needs of GPs and registrars working in northwestern NSW. Australian Family Physician 2005; 34(12 Suppl): 7-9.
12. Hays R. Self assessed learning needs of rurally based IMGs. Australian Family Physician 2005; 34(4): 295.
13. McDonnell L, Usherwood T. International medical graduates - challenges faced in the Australian training program. Australian Family Physician 2008; 37(6): 481-484.
14. McGrath BP. Integration of overseas-trained doctors into the Australian medical workforce. Medical Journal of Australia 2004; 181(11-12): 640-642.
15. Nasmith L. Programs for international medical graduates. Canadian Family Physician 1993; 39: 2549-2553.
16. Curran V, Hollett A, Hann S, Bradbury C. A qualitative study of the international medical graduate and the orientation process. Canadian Journal of Rural Medicine 2008; 13(4): 163-169.
17. Carlier N, Carlier M, Bisset G. Orientation of IMGs: a rural evaluation. Australian Family Physician 2005; 34(6): 485-487.
18. Pilotto LS, Duncan GF, Anderson-Wurf J. Issues for clinicians training international medical graduates: a sytematic review. Medical Journal of Australia 2007; 187(4): 225-228.
19. Ericsson K. Deliberate practice and the acquisition and maintenance of expert performance in medicine and related domains. Academic Medicine 2004; 79(10): S70-S81.
20. Lave J, Wenger E. Situated learning: legitimate peripheral participation. Cambridge: Cambridge University Press, 1991.
21. Wenger E. Communities of practice: learning, meaning and identity. Cambridge: Cambridge University Press; 1998.
22. Boud D, Keogh R, Walker D. Promoting reflection in learning. In: R Edwards, A Hanson, P Raggat (Eds). Boundaries in adult learning. New York: Routledge, 1996.
23. Schon D. The reflective practitioner: how professionals think in action. London: Temple Smith, 1983.
24. Schon D. Educating the reflective practitioner. San Francisco, CA: Jossey-Bass, 1987.
25. Knowles M. The adult learner: a negelected species. Houston, TX: Gulf, 1973.
26. Confederation of Postgraduate Medical Education Councils. Australian Curriculum Framework for Junior Doctors. Available: http://curriculum.cpmec.org.au/ (Accessed 6 December 2011).
27. Postgraduate Medical Council of Victoria. Working in Victoria's Public Hospitals: An Orientation manual for International Medical Graduates v10. (Online) 2009, updated 2011. Available: http://www.pmcv.com.au/img/orientation/orientation-manual (Accessed 6 December 2011).
28. Kneebone R, Nestel D. Learning clinical skills - the place of simulation and feedback. Clinical Teacher 2005; 2(2): 86-90.
29. Maguire P, Fairbairn S, Fletcher C. Consultation skills of young doctors: I -Benefits of feedback training in interviewing as students persist. BMJ 1986; 292: 1573-1578.
30. Maguire P, Pitceathly C. Key communication skills and how to acquire them. BMJ 2002; 325: 697-700.
31. Nestel D, Kneebone R, Barnet A. Evaluation of a clinical communication programme for perioperative and surgical care practitioners. Quality and Safety in Healthcare 2010; 19: 1-7.
32. Kneebone R, Bello F, Nestel D, Yadollahi F, Darzi A. Training and assessment of procedural skills in context using an Integrated Procedural Performance Instrument (IPPI). Studies in Health Technology and Informatics 2007; 125: 229-231.
33. Kneebone R, Kidd J, Nestel D, Asvall S, Paraskeva P, Darzi A. An innovative model for teaching and learning clinical procedures. Medical Education 2002; 36(7): 628-634.
34. Kneebone R, Nestel D, Bello F, Darzi A. An Integrated Procedural Performance Instrument (IPPI) for learning and assessing procedural skills. Clinical Teacher 2008; 5: 45-48.
35. Higham J, Nestel D, Lupton M, Kneebone R. Teaching and learning gynaecology examination with hybrid simulation. Clinical Teacher 2007; 4: 238-243.
36. Nasmith L. Programs for international medical graduates. Canadian Family Physician 1993; 39: 2549-2553.
37. Chumley-Jones HS, Dobbie A, Alford CL. Web-based learning: sound educational method or hype? A review of the evaluation literature. Academic Medicine 2002; 77(10 Suppl): S86-93.
38. Ruiz JG, Mintzer MJ, Leipzig RM. The impact of E-learning in medical education. Academic Medicine 2006; 81(3): 207-212.
39. Duffy FD, Holmboe ES. Self-assessment in lifelong learning and improving performance in practice: physician know thyself. JAMA 2006; 296(9): 1137-1139.
40. Eva KW, Regehr G. Self-assessment in the health professions: a reformulation and research agenda. Academic Medicine 2005; 80(10 Suppl): S46-54.
41. Australian Medical Council (Ed.). Anthology of medical conditions. Canberra, ACT: Australian Medical Council, 2003.
42. Crompvoets S. Using online qualitative research methods in medical education. International Journal of Multiple Research Approaches 2010; 4(3): 206-213.




