Serious health workforce shortages and maldistribution of most health practitioners in rural areas is well documented and a real challenge to healthcare systems. The rural medical workforce shortage has been the subject of extensive research and expenditure for several decades, including significant investment in medical schools through rural education and training interventions such as Rural Undergraduate Support and Coordination (RUSC) and Rural Clinical Schools (RCS) programs, along with bonded rural medical school places and scholarships.
These initiatives have been influenced by the metaphor of the 'rural pipeline' which includes:
- recruiting students from rural backgrounds
- delivering training in rural regions
- rural curriculum providing repeated rural exposures
- building regionally based postgraduate training pathways1.
Subsequent studies from the USA and increasingly from Australia have provided more support for the pipeline approach with prolonged rural placements thought to increase opportunities for rural connectedness2,3 and to be particularly effective in the clinical years of medical training when early rural intentions can be reinforced4,5.
However, recent reviews of the evidence relating to the effect of rural exposure have adopted more conservative and cautionary positions. Ranmuthugala et al noted that 'in examining the specific contribution of rural exposure towards increasing uptake of rural practice, the evidence is inconclusive, largely due to the failure to adjust for those critical independent predictors of rural practice'6. They also emphasize that most of the Australian evidence about rural training programs is limited and 'few studies attempt to identify the influence of specific aspects of rural training programs (in terms of nature, timing, frequency and duration) on uptake of rural practice'. Inconsistencies and imprecision in identifying factors affecting preference for future rural practice have been highlighted7 and attention has been drawn to the urgent need for rigour in evaluating untested interventions8.
A recent study described the development and evaluation of a predictive model and index of rural medical practice intention, which provides important insights into individual factors associated with rural practice preference and illustrates the power and potential of 'a robust, consistent, systematic longitudinal tracking project'9.
The aim of the present study was to identify and assess factors influencing medical students' preferences for future rural practice through analysis of quantitative and qualitative baseline data from a longitudinal tracking study of medical students at Australian RCSs. This rurally-developed Federation of Rural Australian Medical Educators (FRAME) questionnaire has now been coordinated with the Medical Schools Outcome Database (MSOD)10.
Questionnaires were distributed to 166 medical students who had completed their RCS term at one of 6 Australian universities in 2006. Ethics approval was obtained for the study from each of the participating universities.
Questionnaire
The survey instrument 'Rural Clinical School Evaluation 2006' was developed as an evaluation tool to determine baseline data about students studying in RCSs10. Background characteristics assessed included rural background and education. Students were asked to identify their preferred location for future practice, the specialty they wished to pursue, and to rate their agreement or disagreement with 13 items assessing their beliefs about rural work and life. Further questions explored the impact of the RCS experience on future preferences.
Data analyses
All data were pooled. The software SPSS v15 (www.spss.com) was used to generate descriptive analyses and to identify factors used in the decision about future practice location. Open-ended responses were coded and themed using qualitative methods.
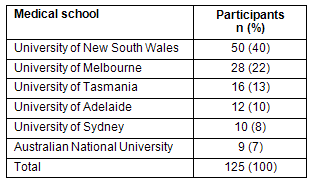
Responses were received from 75.3% (n=125) of the 166 medical students surveyed, who had completed an RCS term in 2006 (Table 1).
Table 1: Participants according to their medical school (2006)
Preferred location for future medical practice
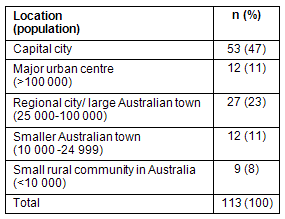
Students were asked to nominate the town/city size of their preferred location for future medical practice (Table 2). Almost half the students (42%; n=48) nominated regional or rural practice, with the balance (majority) of the students preferring a capital city (47%; n=53) or major urban centre (11%; n=12).
Location preference responses were collapsed into 'urban' (capital city and major urban centre), and 'rural' (regional, smaller town or small rural community) for further analysis. Preference for rural or urban practice did not differ by sex (χ²(1)= 0.14, p=0.71) or age (Mann-Whitney U-test; z= -0.30, p=0.76).
Almost half (47%; n=58) the students self-reported a 'rural background'. These 'rural' students had completed an average of 5 years (Mean=5.44, SD=3.76) of their secondary schooling outside urban areas and had lived an average of 9 of the last 12 years (Mean=8.89, SD=3.06) outside a capital city. The 53% (n=66) of students who did not consider themselves to be 'rural' completed virtually none of their secondary schooling outside urban areas (Mean=0.11 years, SD= 0.62) and had lived less than 1 year (Mean=0.98, SD=1.35) outside a capital city.
A logistic regression analysis found that students from rural backgrounds were 10 times more likely to prefer to work in rural areas (OR=10, 95% CI: 4.18, 23.91), χ²(1)=28, p<0.001) when compared with other students.
Table 2: Participants' preferred location for future medical practice (2006)
Intended medical speciality
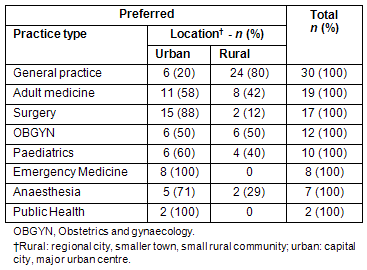
The intended medical speciality is shown for students who indicated a preference to work in an 'urban' versus a 'rural' location (Table 3). The frequencies and percentages for the top eight specialties are presented.
Of students preferring to enter general practice, 80% (n=24) wished to do so in a rural area. In comparison, only 12% (n=2) who intended to specialize in surgery indicated their preference to work in a rural setting. All eight students intending to specialise in emergency medicine indicated that they preferred an urban environment.
Table 3: Cross-tabulation of preferred future location with preferred future practice type
Impact of rural clinical school experience on self-reported interest in rural practice
Eighty-five per cent of students (n=105) agreed with the statement My RCS experience increased my interest in rural training and practice, with 62% of students (n=75) indicating that they would prefer a rural internship/basic training after their RCS experience. A substantial percentage (86%; n=108) agreed they would consider rural practice after their RCS experience.
Beliefs about rural life and rural practice
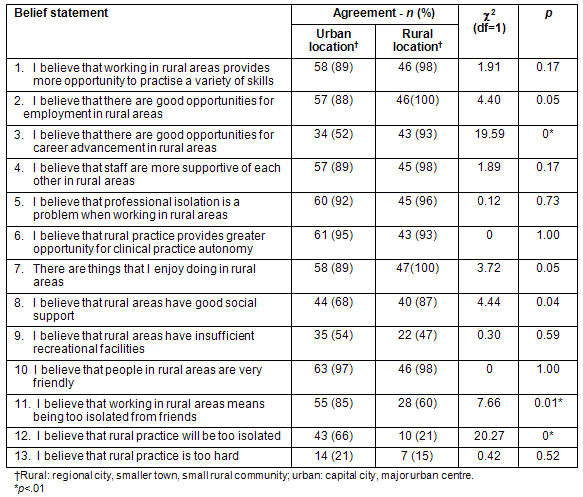
Students were asked to indicate their level of agreement with 13 statements relating to their beliefs about rural life and work. Using a χ² test for independence, the level of agreement on these items was compared for students preferring urban and rural locations (Table 4).
Students preferring to work in rural areas were more likely to believe there are good opportunities for career advancement in rural areas than those intending to work in urban areas (93% vs 52%, p<.001). On the other hand, students preferring urban versus rural locations in the future were more likely to believe that working in rural areas would be more isolated (66% vs 21%, p<.001), particularly from their friends (85% vs 60%, p=.01). There was little difference between the beliefs of those planning urban versus rural practice in relation to:
- rural work providing more opportunity to practice a variety of skills (98% vs 98%, p=0.17)
- good opportunities for employment in rural areas (88% vs 100%, p=0.05)
- rural staff more supportive of each other (89% vs 98%, p=0.17)
- professional isolation more a problem in when working rurally (92% vs 96%, p=0.73)
- rural practice providing greater opportunity for clinical practice autonomy (95% vs 93%, p=1.00).
Table 4: Participants' beliefs about rural life and rural practice
Other factors affecting preference for future rural practice
Students provided 69 open-ended responses to What things would encourage you to consider further rural practice? and 74 responses to What would encourage you to choose a rural hospital for some/most of your post medical school training?
While a few statements appeared to indicate a decision to practice rurally (7 statements), most responses indicated that support and incentives (financial, technological), lifestyle considerations and partner and family opportunities and support were key factors influencing rural training and practice decisions.
Practice factors including availability of professional and collegial assistance were the most important factors in choosing rural training and practice along with out-of-hours and locum support.
The availability of more junior medical officer (JMO) and permanent rural postgraduate year (PGY) 1-3 posts (rather than rotations from city hospitals) was important. The depth and breadth of clinical experience in rural areas and academic excellence were also important.
Importantly, the availability of rural specialty and sub-specialty training positions, ability to practice in their chosen specialty and opportunities for continuing professional development were cited by many students.
Discussion
The literature suggests that experience of training in a rural area is positive for many medical students11,12 and elements of the wider RCS multi-university baseline study, reported elsewhere, strongly supported that notion. The quality of teaching, opportunities for skill development, patient access, lifestyle and a supportive environment were often recognised. These RCS experiences clearly influenced students' interest in future rural training and practice. Our study results provide evidence to support rural medical recruitment and retention through education and training, using the metaphor of the rural pipeline1, with important insights into the factors affecting preference for future rural practice.
This study reinforces the findings of multiple single-institution studies showing that rural residence prior to entry into medical school is the strongest predictor of rural practice intention2,13-15. The 47% of medical students who self-defined as rural origin reported 5 years of rural schooling. The consistency of this finding validates the Australian Government's RUSC definition of rurality as five years schooling outside a major population centre and supports the use of this definition for selection and support of rural students, because they are also more likely to practice rurally. It also validates MSOD data suggesting that rural background is one of the strongest predictors of rural practice after graduation9.
A stated intent to practice in a rural area is an independent predictor of later rural practice16, which is strongly associated with rural origin17. While the stated preference for rural practice at exit in this study was approximately 10% less than the stated preference at entry by 60% of rural origin students (MSOD data) for rural practice9, logistic regression analysis of the present data revealed that medical students from rural backgrounds, after an RCS experience, were 10 times more likely to state intent to practice in rural areas when compared with non-rural-origin students. This finding should help to justify policy and funding decisions to support rural origin students and RCSs, as well as further programs to support post-graduate rural programs.
The MSOD predictive model and index of rural medicine findings confirmed that generalist intentions were another key predictor and that, by contrast, intentions towards specialist practice were a negative indicator for rural practice intention9. In the present study, differentials by specialty suggested that medical students can foresee a career in rural general practice with training and support opportunities, but that students interested even in 'generalist specialties' do not see clear opportunities and support for quality training and supported careers in rural areas. The qualitative data show that access to, and availability of, specialist training posts in rural areas are key needs for consideration of future rural practice.
It will be interesting to compare these data with ongoing FRAME survey findings as RCSs have been breaking new ground in demonstrating that specialist curricula can be taught in rural environments. A recent Flinders University study reported that of vocational career choice for medical graduates with RCS experience 43% chose specialties other than general practice, and that these graduates may contribute to redressing specialist shortfalls in rural areas18.
Generally the literature supports the contention that students who undertake well-coordinated, longer rural placements, particularly RCS placements, are more likely to take up rural careers4,19. However, there appears to be contrasting evidence of a link between length of placements and rural internships and rural medical practice6,20. In the present study, 85% of medical students surveyed indicated that their RCS experience increased their interest in rural training and practice, with 62% indicating they would prefer rural intern training and 86% would consider rural practice. While these findings suggest that students' experiences confirm and support rural intentions, analysis of longitudinal data is required for validation. The qualitative data strongly suggest that students are interested in rural training opportunities that provide long-term prospects for permanent, rural-based junior doctor terms, more JMO positions in rural hospitals, and greater choice for postgraduate training.
This study revealed other factors that influence consideration of future rural practice and training, related to:
- availability of a range of incentives
- community, professional and family support
- long hours and availability of locums
- isolation and socialisation problems associated with living rurally.
Students' responses to open-ended questions indicate that personal issues and family are major influences on decisions about future rural practice intentions. These findings support other recent studies21,22.
Students' beliefs about rural life and rural practice after their RCS experience were influenced by their preference for urban and rural location for future practice. It is significant and positive that there was little variation in their beliefs because all relate to subsequent professional practice rather than students' perceptions of learning as a student in a rural area, and are a result of seeing their clinical lecturers practicing in a rural environment.
Students preferring urban locations believe that working in a rural area will be more isolated, particularly from their friends. The present study supports the hypothesis that perceived isolation and lifestyle opportunities are issues even among students who understand (and even prefer) rural social opportunities.
The RCS program that delivers at least one year of clinical training for 25% of government-funded medical students in rural areas was based on the assumption that longer rural placements allow the development of rural connectedness, which leads to a higher likelihood of rural practice. Analysis of the FRAME Rural Clinical School Evaluation data shows that the most significant predictor of rural practice intention is the 'winning combination' of recruiting rural-origin students and providing them with rural clinical experiences that maintain and foster their interest in rural careers. Perhaps the most important finding for policy-makers and funders is that these data foreshadow a significant increase in demand for post-graduate rural training places that are of high academic quality. The RCS program has developed a strong academic track-record in Australia; thus, its infrastructure and staff networks could serve as the basis for support of quality rural post-graduate training programs.
Given the minimum postgraduate training time in Australia of 5 years (eg to GP fellowship), it is now appropriate to collect data to demonstrate the actual practice locations, specialty choices and training pathways of these RCS graduates with the significant caveat that few, if any, rural non-GP specialty training posts have been available. The FRAME-MSOD group should be funded to facilitate this important work in conjunction with the new national registration database. With the availability of a robust longitudinal tracking tool, the FRAME investigators are in a position to undertake further research to define:
- the balance of selection versus experience in RCSs as predictors of rural practice choices
- the role of bonding versus incentives in shaping workforce outcomes
- factors that predispose urban background students to practice rurally
- variations due to approach individual RCSs and the newer regional medical schools.
Acknowledgements
This study was supported by the Department of Health and Ageing. The authors acknowledge the administrative support of Ms Anne Marmo (ethics coordination) and Ms Linda Foottit (manuscript preparation).
References
1. Dunbabin J, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce. Rural and Remote Health 3: 212. (Online) 2003. Available: www.rrh.org.au (Accessed 29 November 2011).
2. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37(9): 809-814.
3. Denz-Penhey H, Shannon, Murdoch CJ, Newbury JW. Do benefits accrue from longer rotations for students in Rural Clinical Schools? Rural and Remote Health 5(2): 414. (Online) 2005. Available: www.rrh.org.au (Accessed 29 November 2011).
4. Williamson M, Gormley A. The new rural health curriculum at Dunedin School of Medicine: how has it influenced the attitudes of medical students to a career in rural general practice? New Zealand Medical Journal 2003; 116: 1179.
5. Henry J, Edwards B, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health 9: 1083. (Online) 2009. Available: www.rrh.org.au (Accessed 29 November 2011).
6. Ranmuthugala G, Humphreys J, Solarsh B, Walters L, Worley P, Wakerman J et al. Where is the evidence that rural exposure increases uptake of rural medical practice? Australian Journal of Rural Health 2007; 15(5): 285-288.
7. Playford D, Larson A, Wheatland B. Going country: rural student placement factors associated with future rural employment in nursing and allied health. Australian Journal of Rural Health 2006; 14(1): 14-19.
8. Wilson N, Couper I, De Vries E, Reid S, Fish T, Marais B. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health 9: 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 29 November 2011).
9. Jones M, Humphreys J, Prideaux D. Predicting medical students' intentions to take up rural practice after graduation. Medical Education 2009; 43: 1001-1009.
10. DeWitt DE, McLean R, Newbury J, Shannon S, Critchley J. Development of a common national questionnaire to evaluate student perceptions about the Australian Rural Clinical Schools Program. Rural and Remote Health 5: 486. (Online) 2005. Available: www.rrh.org.au (Accessed 29 November 2011).
11. Lyon PM, McLean R. Students' perceptions of clinical attachments across rural and metropolitan settings. Assessment & Evaluation in Higher Education 2008; 33(1): 63-73.
12. Wilson N, Bourhuijs PAJ, Conradie HH, Reuter H, Van Heerden BB, Marais B. Perceived educational value and enjoyment of a rural clinical rotation for medical students. Rural and Remote Health 8: 999. (Online) 2009. Available: www.rrh.org.au (Accessed 29 November 2011).
13. McDonald J, Bibby L, and Carroll S. Recruiting and retaining general practitioners in rural areas: improving outcomes through evidence-based research and community capacity building. Evidence-based review: final report. University of Ballarat, VIC: Centre for Health research and Practice, 2002.
14. Curran V, Rourke J. The role of medical education in the recruitment and retention or rural physicians. Medical Teacher 2004; 26(3): 265-272.
15. Richards HM, Farmer J, Selvaraj S. Sustaining the rural primary healthcare workforce: survey of healthcare professionals in the Scottish Highlands. Rural and Remote Health 5: 365. (Online) 2005. Available: www.rrh.org.au (Accessed 29 November 2011).
16. Somers G, Strasser R, Jolly B. What does it take? The influence of rural upbringing and sense of rural background on medical students' intention to work in a rural environment. Rural and Remote Health 7: 706. (Online) 2007. Available: www.rrh.org.au (Accessed 29 November 2011).
17. Somers G, and Strasser R. Do rural mentors, rural undergraduate clubs and rural rotations increase the medical student's intention to practice in the country? In: Proceedings, ACRRM Scientific Forum; 30 April 2002; Melbourne, VIC. Available: http://www.acrrm.org.au/main.asp?NodeID=156 (Accessed 28 March 2010).
18. Worley P, Martin A, Prideaux D, Woodman R, Worley E, Lowe M. Vocational career paths of graduate entry medical students and Flinders University: a comparison of rural, remote and tertiary tracks. Medical Journal of Australia 2008; 188(3): 177-178.
19. Veitch C, Underhill A, Hays RB. The career aspirations and location intentions of James Cook University's first cohort of medical students: a longitudinal study at course entry and graduation. Rural and Remote Health 6(1): 637. (Online) 2006. Available: www.rrh.org.au (Accessed 29 November 2011).
20. McDonnel Smedts A, Lowe MP. Clinical training in the Top End: impact of the Northern Territory Clinical School, Australia on the Territory's health workforce. Rural and Remote Health 7: 723. (Online) 2007. Available: www.rrh.org.au (Accessed 29 November 2011).
21. Adams ME, Dollard J, Hollins J, Petkov J. Development of a questionnaire measuring student attitudes to working and living in rural areas. Rural and Remote Health 5(1): 327. (Online) 2003. Available: www.rrh.org.au (Accessed 29 November 2011).
22. Eley D, Young L, Shrapnel M, Wilkinson D, Baker P, Hegney D. Medical students and rural general practitioners: congruent views on the reality of recruitment into rural medicine. Australian Journal of Rural Health 2007; 15(1): 12-20.



