In Australia more than 290 000 women give birth annually1. Approximately one-third of these women live outside major cities, and 3% (approximately 8000 women) live in areas considered remote or very remote. The availability of maternity services in rural and remote areas of Australia is declining with the closure of over 130 small rural maternity units since 19952. As a result, increasing numbers of pregnant women living in rural and remote areas relocate to give birth in hospitals in major cities or regional centres, often staying in hostels or self-care units for up to a month prior to birthing. The support available for these women is often inadequate3. In addition, some women have expressed concerns about the safety of their accommodation and the welfare of other children left behind4,5.
For these women, accurately predicting the timing of birth would be desirable, because excluding the onset of labour in the near future, may provide an opportunity to delay relocation. However, predicting the onset of term labour and birth remains imprecise. Currently, determination of the Bishop score, an assessment of cervical status, is commonly used to assess suitability for induction of labour or the onset of imminent labour (ie within 48 hours)6. However, this is a subjective assessment with interobserver variability.
In the context of preterm birth, tests for the detection of fetal fibronectin (fFN) in the cervico-vaginal secretions of women with symptoms of preterm labour have been recommended internationally for clinical practice7-9, in order to inform decision-making regarding the administration of antenatal steroids and transfer to tertiary-level units. Fetal fibronectin is a glyco-protein and a key component of the extracellular matrix of the membranes of the amniotic sac10. Disruption of the maternal-fetal membrane interface causes the release of fibronectin into cervico-vaginal secretions. The presence of fFN in cervico-vaginal fluid between 24 and 34 weeks of pregnancy is associated with impending preterm birth among women with symptoms of preterm labour11 and asymptomatic pregnant women12; however, the tests are most accurate in women who have symptoms.
Although there is a substantial body of research about the assessment of fFN in the preterm setting13, there is limited evidence about the accuracy of fFN testing to predict the onset of labour at term. Eight studies were identified that assessed fFN to predict term birth, and of these, three reported a significantly longer time-to-birth interval for women who tested negative for fFN compared with those in whom fFN was detected6,14,15. In other studies the presence of fFN was associated with a 91% and 96% sensitivity for predicting birth within 2 or 7 days of testing, respectively16,17, or there was no association found with the onset of term birth18-20.
Although the literature suggests that fFN testing may be useful in predicting imminent term birth, it is unclear whether this may be a useful test to inform decisions about relocating rural women at term to major cities for birthing. Of the available studies, the majority tested women either on their estimated date of birth or beyond term6,14,15,19,21. However, this has limited relevance to the use of the test in rural settings with no birthing services, because it is unlikely that maternity providers would support women to stay at home after 40 weeks gestation. Here we report the results of a study designed to assess the accuracy of using the fFN test, from 37 weeks gestation, for predicting term birth among women living in rural and remote areas in Central and northern Australia. The study was designed to inform the possible development of a larger study evaluating the use of the test to determine when to transfer women into major cities for birthing.
Setting and subjects
The study was undertaken in two small maternity units (with approximately 200 and 750 births per annum), in areas classified as remote districts (Australian Standard Geographic Classification) within the Northern Territory of Australia. Eligible women included those: planning to give birth at one of the units, aged 18 years or older, a singleton pregnancy, between 37+0 and 40+3 weeks (37 weeks to 40 weeks and 3 days) gestation, and with no medical or social indication for induction of labour or caesarean section in the 7 days following recruitment. Women were not eligible to participate if they had any of the following: ruptured membranes, current vaginal bleeding or bleeding in the last two weeks (moderate/gross bleeding), were in active or the early stages of labour, cervical cerclage suture in place, placenta praevia or placental abruption.
All eligible women birthing in the hospital, either from the local area of the maternity unit or those transferred in from very remote areas, were approached about the study. To assist with gaining informed consent, a DVD recording was developed by one of the researchers (S Kruske), and a registered interpreter, that included information about the study in the local Aboriginal language.
Procedure
At the antenatal visit at 37 weeks gestation (or as close as possible to) consenting women were invited to have a speculum examination and a high vaginal swab for fibronectin assessment. Specimen collection occurred prior to any digital examination or manipulation of the cervix. The fFN assessment was undertaken using the Quikcheck fFN test (Adeza Biomedical Corporation, Sunnyvale, California, USA). During the sterile speculum examination, a sterile polyester applicator tip was rotated across the posterior fornix of the vagina for 10 secs to absorb cervico-vaginal secretions. The applicator was then removed and the tip inserted into the Quikcheck test tube containing buffer and mixed vigorously for 10-15 secs. After removing as much liquid as possible from the applicator it was then discarded. The lower end of the test trip was then inserted into the buffer for 10 min, after which time the test strip was removed and the result read.
After the specimen collection for fFN testing was undertaken, a second high vaginal swab was collected for micro culture and sensitivity testing. Repeat fFN testing at 7 day intervals was undertaken until the woman was 40+3 weeks. At the time of testing neither participating women nor health staff other than the individual involved in performing the test were informed of the fFN test result.
Information about women's demographic characteristics, medical history and health during the current pregnancy was collected from medical records. The primary outcome of the study was the time-to-birth interval in days from the fFN test date. Time-to-birth was first calculated from the date of the first fFN test, and then separately, from the date of the last fFN test. In addition, the time-to-birth interval was categorized as either ≤ 7 days or >7 days, to assess birth occurring within 7 days of testing, separately for the first fFN test and last fFN test. Finally, also examined was the effect of a fFN test on time-to-birth and birth ≤ 7 days of testing for those women who had a test between 38+0 and 38+6 weeks, because this is the usual gestation at which women are transferred into major centres for birthing.
Statistical analysis
Results are expressed as mean (standard deviation [SD]), or number and percentage, as appropriate. Time-to-birth was modelled using linear regression, and separate models considered the effects of the results of the first fFN test, the last fFN test and the test undertaken at 38 weeks gestation. Logistic regression was used to examine the effect of the fFN test result on birth within 7 days of testing, separately for the first fFN test, last fFN test, and among tests undertaken at 38 weeks gestation.
In 52 of the fFN tests performed, lubricant was used when undertaking the speculum examination to collect the fFN swab, which can affect the accuracy of the test10. Accordingly, all linear and logistic regression models were adjusted for the use of lubricant. Similarly, all models were adjusted for gestational age at the time of the test (with the exception of the models examining the effects of tests undertaken at 38 weeks gestation). In addition, in the analyses of the last test results, the models were adjusted for the conduct of a previous fFN test.
Four tests were found to have been undertaken outside the gestational age criteria (n=3 at 36+6 weeks gestation, and n=1 at 41+0 weeks gestation). Sensitivity analyses excluding these tests from the models were undertaken. All analyses were undertaken in Stata v10.1 (StataCorp; College Station, TX; USA ). A p-value <0.05 was considered statistically significant.
Ethics approval
Approval to conduct this study was obtained from the Human Research Ethics Committee of the Northern Territory Department of Health and Families and the Menzies School of Health Research (#HREC-07/71), and the Central Australian Human Research Ethics committee, and their relevant Aboriginal subcommittees.
In total, 76 women were enrolled, however one woman was excluded from further analyses as she went into spontaneous labour prior to any testing being performed. Of the remaining 75 women participating in the study, the average age was 29.9 years (SD 6.2) and just over one-quarter of women (n=20, 27%) were nulliparous (Table 1). The majority of women (n=62, 83%) went into labour spontaneously and had a normal vaginal birth (n=65, 87%). The mean gestation at birth was 39+3 weeks (SD 4.6) and the mean birth weight of infants was 3515 g (SD 426).
The number of fFN tests performed, the mean gestational age at each test and the result at each fFN test are described (Table 2). A total of 156 tests were performed. Most women (n=49, 65%) had more than one test performed (average tests 1.8, range 1-4). The mean interval from testing to birth according to the results of the first, last and 38 week fFN test is presented (Table 3).
Table 1: Demographic characteristics and birth outcomes,
N=75 (n & % unless otherwise indicated)
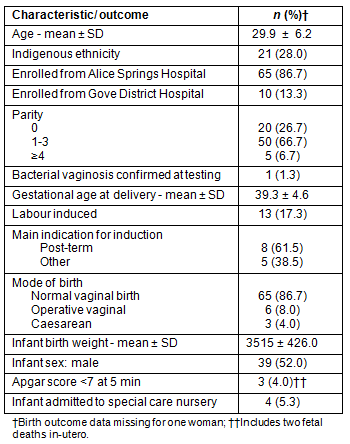
Table 2: Number of fFN tests undertaken, gestational age at testing and proportion of positive results
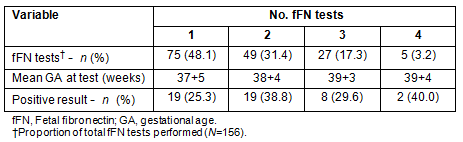
Table 3: Mean interval from testing to birth (days)
for the results of the first, last and 38 week fFN test
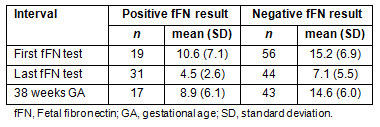
Mean difference (days) in time-to-birth
When the analyses considered the effects of the first fFN test result, the unadjusted mean difference in the time-to-birth between women with a negative fFN test and those with a positive test was 4.6 days (95% confidence interval [CI] 0.9-8.3). Adjustment for gestational age at the time of the test and the use of lubricant increased the mean difference estimate to 5.4 days (95% CI 2.0-8.8). The results were unchanged after the exclusion of the three tests undertaken at 36+6 weeks.
When the results were based on the last fFN test result, the mean difference in time-to-birth between women with a positive versus negative fFn test was reduced. The unadjusted mean difference was 2.6 days (95% CI 0.5-4.7 days), and adjustment for gestational age, lubricant and a previous fFN test increased the mean difference slightly to 2.7 days (95% CI 0.6-4.8). Exclusion of the test undertaken at 41+0 weeks did not substantially alter the results (adjusted mean different 2.9 days, 95% CI 0.8-5.1).
Birth within 7 days of testing
From the time of the first fFn test, 17 women gave birth within 7 days, and 9 (53.0%) of these women had a positive result. For the 58 women who did not give birth within 7 days, 10 women (17.2%) returned a positive result. Having a positive fFN test was associated with a significant increase in the odds of giving birth within 7 days of testing (unadjusted odds ratio (OR) 5.4, 95% CI 1.7-17.4). With adjustment for gestational age at test and lubricant use the OR increased to 11.0 (95% CI 2.5-48.7). Exclusion of the three tests undertaken at 36+6 weeks did not substantially alter the findings (adjusted OR (AOR) 10.7, 95% CI 2.5-46.4).
From the time of the last fFN test, 58 women gave birth within 7 days, and 29 (50.0%) of these women had a positive result. For the 17 women who did not birth within 7 days, 2 (11.8%) returned a positive fFN test. Therefore, having a positive last fFN test was associated with significantly increased odds of giving birth within 7 days (unadjusted OR 7.5, 95% CI 1.5-35.8). After adjustment for the effect of gestational age, lubricant use and conduct of a previous fFN test, the AOR associated with a positive fFN test was 8.1 (95% CI 1.6-39.8). Exclusion of the test undertaken at 41.0 weeks did not substantially alter the findings (AOR 8.3, 95% CI 1.7-41.1).
Effects of tests undertaken at 38 weeks
There were 60 women who had a fFN test undertaken at 38 weeks gestation, the typical gestational age at which women are relocated for birthing. When the analysis set was restricted to these tests, the unadjusted estimated mean difference in time-to-birth was 5.7 days (95% CI 2.2-9.2 days), and this was unchanged when the analyses was adjusted for the effect of lubricant. Among these women, 14 birthed within 7 days of testing, and of these 10 (71.4%) had a positive fFN test. In contrast, 7 (15.2%) of the 46 women who did not give birth within 7 days had a positive fFN test. Therefore, having a positive fFN test result at 38 weeks was associated with a significant increase in odds of birth within 7 days (unadjusted OR 13.9, 95% CI 3.4 -57.1). After adjustment for the effect of lubricant use, the odds ratio increased slightly to 14.4 (95% CI 3.4-60.2).
Discussion
In this study, a positive fFN result was associated with a significantly shorter time-to-birth interval, and increased odds of giving birth within 7 days of testing when compared with a negative fFN result. When testing occurred at 37 or 38 weeks gestation, women with a positive result gave birth approximately 5.5 days earlier than women with a negative test result. The results were similar when the last fFN test was considered, however the mean difference in time-to-birth was diminished. These findings indicate that the presence of fFN in cervico-vaginal secretions at term can predict impending birth.
Although there is a paucity of research assessing the use of this test at term, our findings are consistent with the majority of available studies22. Of the four identified studies assessing fFN at term that report time-to-birth interval, three found a significantly different interval between women with a positive compared with a negative test result, with the mean difference ranging from 2.2 to 5.4 days6,14,15.
Being able to accurately assess the likelihood of impending birth offers rural and remote dwelling pregnant women and their caregivers the opportunity to determine the optimal time to relocate to major cities for birthing. To be clinically useful, the fFN needs to accurately show that a negative test result indicates that women will not go into labour and birth in a rural location without access to maternity services, for a specified and meaningful period of time. In this study, a time frame of birth within 7 days of testing was chosen to assess whether weekly fFN testing would be accurate and feasible and would enable women to delay relocation for at least one week. Although it was found that women with a negative test result were significantly less likely to give birth within 7 days when compared with those with a positive result, a negative result did not reliably exclude the onset of birth. Approximately half of the women whose first or last test was negative gave birth within 7 days. Interestingly, this was less for the 38 week test (28.6%). Therefore, delaying relocation based on these test results would result in some women having unplanned or unprepared births in their communities, or an emergency evacuation back to the regional centre.
Although the majority of existing studies on this topic have involved testing women either on their estimated date of birth or beyond, two studies were identified that involved testing at earlier gestational ages, and neither demonstrated conclusively that the fFN test accurately predicted the absence of labour. Lockwood et al showed that among women with a negative fFN result at 39 weeks, 63% had not given birth within one week of testing17. Similarly, Luton et al reported that when women were assessed for fFN weekly from 38 weeks, only 29% of women whose last fFN test was negative remained undelivered at 7 days after testing, compared with 9% of women whose last fFN test was positive15.
The authors are aware of only one other study evaluating the accuracy of this test among remote dwelling women specifically for the purpose of allowing women to stay in their communities for a longer period of time23. The findings of this unpublished pilot study involving 17 women in Nunavut, Canada are consistent with the present and earlier studies, as more than half of all participants gave birth within 7 days of their last negative fFN test23. Although further research in this setting could be conducted to determine the accuracy of the test for predicting birth within a shorter time frame (eg 2 days of testing), this is not practical in a rural setting as it would increase the burden of testing on women and local healthcare providers. It is also unclear whether delaying relocation for only a couple of days would be meaningful to the women themselves. Therefore, collectively, the current evidence about the accuracy of this test for excluding term birth does not support the use of the test to inform decisions related to the timing of relocation, nor does it support further research into this topic without modification of the test itself.
This study has the limitation that lubricant was used to assist insertion of the speculum in approximately one-third of all tests undertaken. Lubricants can interfere with the absorption of the specimen onto the swab10, resulting in false negative test results. As a result, all analyses were adjusted for the use of lubricant; however, in all instances, adjustment strengthened the effect estimates.
Late pregnancy and birthing are very important times for any woman and her family. Prolonged social dislocation at this time in an unfamiliar environment can be extremely disruptive to families and carries its own risks4,5. In this study, although we found the presence of fFN in cervical secretions was associated with impending term birth, the absence of fFN did not reliably exclude the onset of birth, with up to 50% of women with a negative fFN test giving birth within 7 days of testing. This indicates that testing for fFN in rural and remote settings would not safely allow women at term to delay transferring into major centres for birthing. Until services are improved, women in these areas will continue to be transferred in late pregnancy, which is suboptimal. Re-establishment of primary maternity services in Australia's rural and remote areas would be a far more satisfactory option, and would help to address the current inequity in access to appropriate maternity care experienced by rural women and their families.
References
1. Laws PJ, Sullivan EA. Australia's mothers and babies 2008. Canberra, ACT: Australian Institute of Health and Welfare, 2010.
2. Rural Doctors Association of Australia. Governments Must Heed the Evidence: Small Maternity Units are Safer (updated 7 December 2005). Canberra, ACT: RDAA, 2005.
3. Australian Government Department of Health Ageing. Improving Maternity Services in Australia: The Report of the Maternity Services Review. Canberra, ACT. (Online) 2009. Available: http: //www.health.gov.au/internet/main/publishing.nsf/Content/maternityservicesreview-report (Accessed 8 February 2011).
4. Kildea S. And the women said... Report on birthing services for Aboriginal women from remote Top End communities. Darwin, NT: Territory Health Services, 1999.
5. Dietsch E, Davies C, Shackleton P, Alston M, McLeod M. 'Luckily we had a torch' : contemporary birthing experiences of women living in rural and remote NSW. Wagga Wagga, NSW: Charles Stuart University, 2008.
6. Ahner R, Kub-Csizi P, Heinzl H, Bikas D, Rabl M, Wagenbichler P et al. The fast-reacting fetal fibronectin test: A screening method for better prediction of the time of delivery. American Journal of Obstetrics and Gynecology 1997; 177(6): 1478-1482.
7. American College of Obstetricians and Gynecologists. ACOG Practice Bulletin: Clinical management guidelines for obstetrician-gynecologist. Number 43, May 2003. Management of preterm labor. Obstetrics and Gynecology 2003; 101(5Pt1): 1039-1047.
8. King Edward Memorial Hospital. Clinical Guidelines Section B: Obstetrics & Midwifery Guidelines 2.5.2 MFAU Quick reference guide to suspected preterm labour. Perth, WA: KEMH, 2007.
9. Royal Women's Hospital. Royal Women's Hospital Clinical Practice Guidelines. Labour: threatened preterm. Melbourne, VIC: RWH, 2007.
10. Adeza Biomedical Corporation. fFN® Adeza Biomedical Fetal Fibronectin Enzyme Immunoassay and Rapid FFN for the TLiIQ® system: Information for health care providers. California, USA: Adeza Biomedical Corporation, 2003.
11. Lockwood C, Senyei AE, Dische MR, Casal D, Shah KD, Thung SN et al. Fetal fibronectin in cervical and vaginal secretions as a predictor of preterm delivery. New England Journal of Medicine 1991; 325(10): 669-674.
12. Leeson SC, Maresh MKA, Martindale EA, Mahmood T, Muotune A, Hawkes N, et al. Detection of fetal fibronectin as a predictor of preterm delivery in high risk asymptomatic pregnancies. British Journal of Obstetrics and Gynaecology 1996; 103(1): 48-53.
13. Honest H, Bachmann L, Gupta J, Kleijnen J, Khan K. Accuracy of cervicovaginal fetal fibronectin test in predicting risk of spontaneous preterm birth: systematic review. BMJ 2002; 325(7359): 301-311.
14. Mouw RJ, Egberts J, van Roosmalen JJ, Kragt H. High cervical fetal-fibronectin concentrations and birth within 3 days in pregnancies of 41 weeks or more. New England Journal of Medicine 1995; 332(16): 1105.
15. Luton D, Guibourdenche J, Sibony O, Braig S, Benzakine Y, Oury JF et al. Fetal fibronectin in the cervical secretion predicts accurately the onset of labour at term. European Journal of Obstetrics & Gynecology and Reproductive Biology 1997; 74(2): 161-164.
16. Ahner R, Egarter C, Kiss H, Heinzl K, Zeillinger R, Schatten C et al. Fetal fibronectin as a selection criterion for induction of term labor. American Journal of Obstetrics and Gynecology 1995; 173(5): 1513-1517.
17. Lockwood C, Moscarelli RD, Wein R, Lynch L, Lapinski RH, Ghidini A. Low concentrations of vaginal fetal fibronectin as a predictor of deliveries occurring after 41 weeks. American Journal of Obstetrics and Gynecology 1994; 171(1): 1-4.
18. Nisell H, Hagskog K, Westgren M. Assessment of fetal fibronectin in cervical secretion in cases of equivocal rupture of the membranes at term. Acta Obstetricia et Gynecologia Scandinavica 1996; 75(2): 132-134.
19. Goffeng AR, Milsom I, Lindstedt G, Lundberg PA, Andersch B. Fetal fibronectin in vaginal fluid of women in prolonged pregnancy. Gynecologic and Obstetric Investigation 1997; 44(4): 224-228.
20. Rozenberg P, Goffinet F, Hessabi M. Comparison of the Bishop score, ultrasonographically measured cervical length, and fetal fibronectin assay in predicting time until delivery and type of delivery at term. American Journal of Obstetrics and Gynecology 2000; 182(1Pt 1): 108-113.
21. Ahner R, Kiss H, Egarter C, Zeillinger R, Eppel W, Karas H et al. Fetal fibronectin as a marker to predict the onset of term labor and delivery. American Journal of Obstetrics and Gynecology 1995; 172(1Part 1): 134-137.
22. Kiss H, Ahner R, Hohlagschwandtner M, Leitich H, Husslein P. Fetal fibronectin as a predictor of term labour: a literature review. Acta Obstetricia et Gynecologia Scandinavica 2000; 79(1): 3-7.
23. Healey G, MacDonald A, Kornelsen J, Grzybowski S, Hogg W. Reducing the social and economic stress for women living in rural and remote communities to give birth: A pilot study on the use of fetal fibronectin testing 'at term': community report. Qaujigiartiit Health Research Centre. (Online) 2010. Available: http: //www.qhrc.ca/apps/Docs/displayDocs.aspx (Accessed 22 November 2011).