full article:
Geography, demography and maternity services in the Barkly region, Northern Territory, Australia
Australia's Barkly region in the Northern Territory (NT) has an area of 320 000 km2 and a population of 5700, 64% of whom are Aboriginal. The regional centre Tennant Creek has a population of 3100, of whom 52% are Aboriginal1,2. The nearest health service that provides birthing is in Alice Springs Hospital (ASH), 500 km to the south. There are strong historical and cultural links to the town of Mt Isa, 660 km east in the neighbouring state Queensland, and some women travel there and to other locations to have their babies.
Aboriginal and Torres Strait Islander mothers throughout Australia are characterised by younger age, higher parity, and higher rates of preterm birth and low birthweight than non-Indigenous women3. Approximately 74% of Barkly mothers are Aboriginal4-6.
In Tennant Creek there is a 20 bed public hospital, a general practice clinic, and an Aboriginal community controlled health service. Outside Tennant Creek, the Barkly region has 4 health centres in remote townships with largely Aboriginal populations7-10. These services provide antenatal and postnatal care by midwives, nurses, Aboriginal Health Practitioners and non-specialist doctors of varying levels of experience, but no planned birthing11. Specialist advice is available by telephone, and several times per year an obstetrician from Alice Springs conducts out-patient clinics12. Ultrasound is available in Tennant Creek one week per month, and in Alice Springs at all times. Since 2006 there has been no service for planned births in the Barkly region; prior to that women with low risk pregnancies could give birth at Tennant Creek Hospital (TCH)13. However, every year a small number of women give birth at TCH and in health centres despite the lack of planned birthing services4-6.
It is current NT Department of Health (DoH) protocol that women who live in remote townships should give birth in their regional hospital14. However, since the provision of planned birthing services at Tennant Creek ceased in 2006, all Barkly women must leave the region to give birth in a hospital with facilities for operative delivery. To support their travel, usually to Alice Springs, women are offered limited financial assistance including bus fares or equivalent, and accommodation subsidies from 38 weeks gestation or earlier15. There is provision for one escort for women aged 16 years or younger and for nulliparous women14,15. Additional escorts may be approved at the discretion of the delegated officer. In practice, most non-Aboriginal women drive to Alice Springs alone or with their partner or another family member and stay in commercial accommodation while they await the birth; most Aboriginal women travel by bus, often with a family member, and stay in an Aboriginal hostel.
Northern Territory maternity services review
The 2007 review of NT Maternity Services recommended improved integration of maternity care services to provide high quality woman-centred services throughout the NT16. The review noted the dissatisfaction of women and families in the Barkly region, who have no option of birthing within their region. A subsequent report on maternity services in the Barkly region noted that the number of births in TCH had been declining for many years before the birthing service officially closed in 2006 with the departure of the Director of Medical Services (Fig1). The maternity services review recommended a pilot study of birthing at TCH13,16.
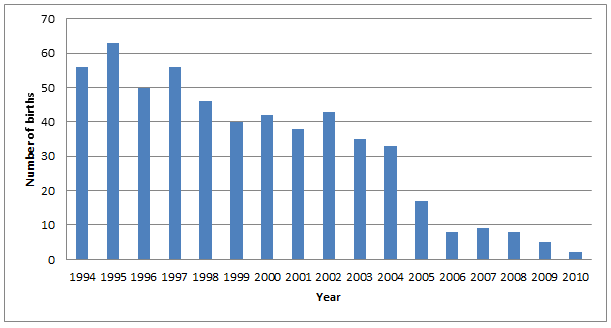
Figure 1: Births at Tennant Creek Hospital, Northern Territory, 1994 to 2010. Data sources:
Mothers and Babies reports4-6 (for 1994 to 2007); NT Department of Health Perinatal Data Analyst,
pers. comm., 18 July 2012 (for 2008 & 2009); Midwives Data Collection, NT Department of Health;
unpubl. data, 2010 (for 2010).4-6.
The closure of rural and remote maternity services in Australia is well documented17. Some clinicians express concern about the safety of re-commencing low risk birthing services in TCH due to the difficulty in maintaining an adequately skilled workforce to provide operative delivery13. At the same time, both Aboriginal and non-Aboriginal community members express concern about the need to travel to Alice Springs or elsewhere for birthing services, which means being separated from home and community for a number of weeks. This concern is shared by some clinicians. The vast distances separating Barkly townships and Tennant Creek from the nearest birthing services in Alice Springs increases the call for local birthing services. Assertions about the psychological, social and cultural risks of translocation to Alice Springs are met with counter claims about the perceived high levels of clinical risk13,18.
Similar concerns are felt by families in communities throughout rural and remote NT and Australia as a whole17-19. In recognition of these issues and the disadvantage experienced by rural and remote families due to lack of services, Australia's National Maternity Services Plan has a strong focus on both rural and remote maternity care and Aboriginal and Torres Strait Islander populations. This includes a commitment to expand choices near women's homes and a focus on culturally competent maternity care17.
This project was a collaboration between the local Aboriginal community controlled health service, Anyinginyi Health Aboriginal Corporation and the NT DoH. It aimed to provide clinical data to inform a discussion about birthing in TCH by reviewing the indications for specialist referral of Barkly women who gave birth in 2010. The Australian College of Midwives National Guidelines for Consultation and Referral (ACM Guidelines)20 were used as a standard to determine if, hypothetically, specialist referral for birthing in ASH would have been indicated for the woman or baby. By the same standard, women with no indication for specialist referral based on the ACM Guidelines could have been offered the option of giving birth at TCH if planned low-risk birthing services were established.
The project was a retrospective cross-sectional study of women resident in the Barkly who gave birth in 2010. Women were identified from the NT Midwives Data Collection (NT Department of Health, unpubl. data, 2010). Those who gave birth outside Central Australia were excluded because the focus was on regional service provision rather than the birthing population.
Two midwives examined each woman's maternity records. All who gave birth in the Barkly, either at TCH or in a township health centre, were transferred to ASH with their baby. Therefore records were available at ASH for every birth. Demographic, medical, obstetric and neonatal information was extracted from the ASH records. Review of primary care records was found unnecessary as relevant antenatal information was provided from health centres to ASH.
The ACM Guidelines provide evidence based guidance to midwives to optimise maternity care by promoting collaboration with other midwives, doctors and other professionals as required. They were developed by a multidisciplinary expert working group of midwives, obstetricians, neonatologists and consumers20. In this project the ACM Guidelines' recommendations were used for indications for referral to medical specialists. The ACM Guidelines provide a published standard referral guideline regarding who would require referral to ASH for birthing care.
Ethics approval
The project was approved by the Central Australian Human Research Ethics Committee (CAHREC): #2011:10:02.
Barkly women who gave birth in 2010 and their babies
The NT Midwives Data Collection recorded 99 women resident in Barkly who gave birth in 2010. Sixteen delivered outside Central Australia and were excluded from further analysis. All 83 women who gave birth in Central Australia either gave birth at ASH or were transferred to ASH soon after birthing, and these women are the population of this study. Of the women, 69 (83%) were Aboriginal, and five women were born outside Australia (2 in the Philippines and one each in England, Fiji, and India).
Over half the women (n=42) were resident in Tennant Creek, while the others were resident in 10 smaller townships in the Barkly region. Of the identified women, 35% were nulliparous; 20 (29%) were aged under 20 years and one was under 16 years. The women's ages are shown (Fig2).
All infants were liveborn and there were three sets of twins. Sixteen percent (13/83) of all births and 12% (10/80) of singleton births occurred before 37 weeks gestation (preterm). Mean birthweight was 3154 g (standard deviation [SD] 744.3 g); mean singleton birthweight was 3176 g, (SD 677 g). In 21% (18/86) of all births and 15% (12/80) of singleton births, the baby weighed less than 2500g. Nine (10%) of the babies weighed more than 4000g, including five (6%) who weighed more than 4500g.
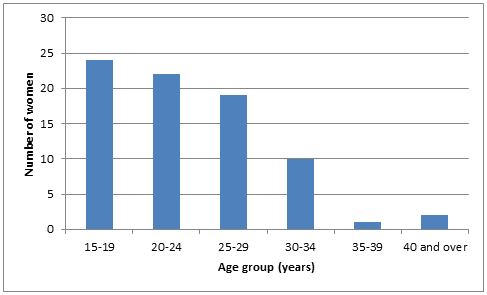
Figure 2: Age groups of Barkly women who gave birth at or were referred to Alice Springs Hospital in 2010.
Indications for referral
Based on the ACM Guidelines20, 24 women had 29 indications for obstetric referral identified on presentation in pregnancy or during antenatal care (Table 1). Indications for referral to specialist care were identified in a further 14 women during the pregnancy, and 13 during labour and delivery. Ten infants in total had indications for specialist referral. This includes two infants born to mothers who did not require referral themselves. Maternal and fetal/ infant indications for referral identified during labour, delivery and postpartum periods are shown (Table 2). A flowchart is provided which shows the progress and outcomes of Barkly women and births in 2010 (Fig3).
Table 1: Indications for referral for obstetric consultation identified during
antenatal period of Barkly women who delivered in Central Australia in 2010 (n=83)
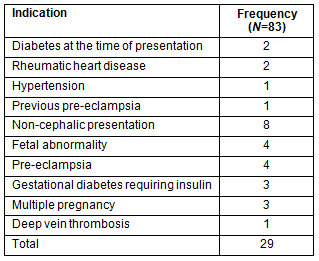
Table 2: Indications for referral to specialist care of Barkly women
who gave birth in 2010 and their infants: indications
arising during labour, delivery and post partum (n=83)
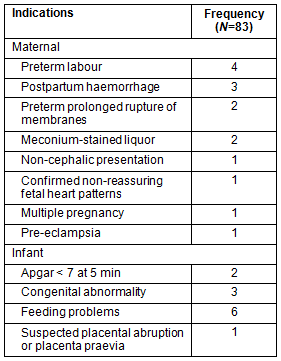
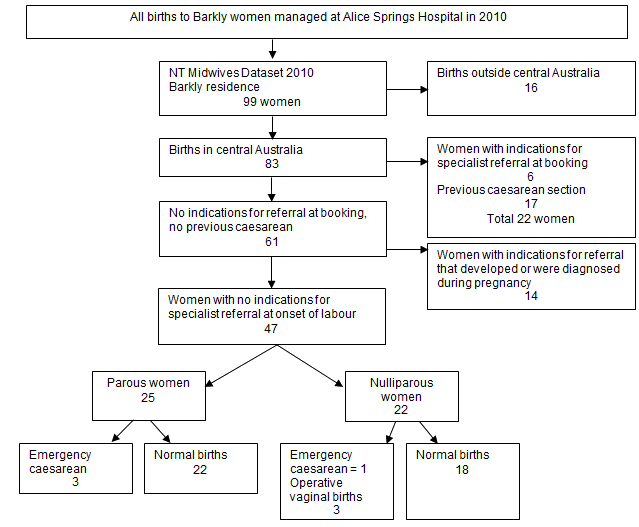
Figure 3: Flowchart of Barkly women and births in 2010. Data source:
Midwives Data Collection, NT Department of Health; unpubl. data, 2010.
Identification of women for birthing in Tennant Creek
If a low-risk birthing service were available at TCH without capacity for caesarean section, then 40 women could have been managed at TCH (22 multiparous & 18 nulliparous). If TCH was caesarean-section capable, 47 women could have been offered the option of birthing there (Fig3).
Women delivering in Barkly region or transferred in labour to Alice Springs Hospital
Six women gave birth in the Barkly region, in health centres or at TCH. All six women and their babies were transferred immediately by air to ASH. None of these women had indications for referral to specialist care prior to the onset of labour. Two women had three indications for referral during labour, birth and immediately postpartum. These were failure to progress followed by postpartum haemorrhage; and preterm labour at 35 weeks. No women gave birth in Alice Springs outside the hospital.
Eleven women were transferred to ASH in labour, either from TCH or a township health centre. None of these women gave birth en-route. Four had already reached 38 weeks gestation, at which time, if policy was strictly followed, the women would have been in Alice Springs. Indications for referral for the women transferred in labour were one each rheumatic heart disease, gestational diabetes, breech presentation and four with preterm labour, including one with breech presentation. Five had no indications for referral at the time the transfer was arranged.
Discussion
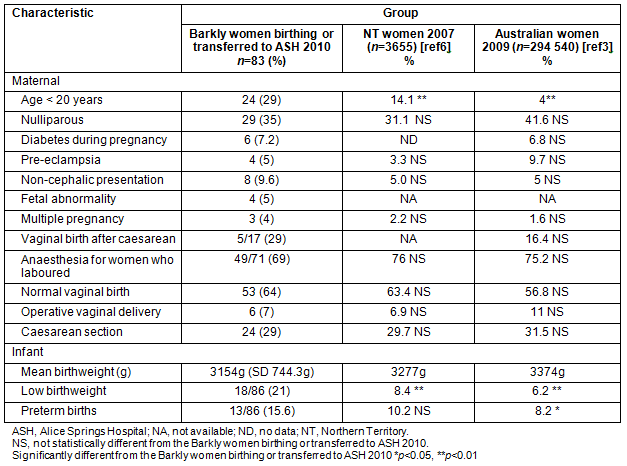
Demographic and obstetric characteristics of the Barkly women and their babies are shown (Table 3) compared with NT (2007)6 and Australian (2009)3 groups. Statistically significant differences were the younger age of the Barkly women, and the rates of low birthweight and preterm birth. These outcome differences reflect the younger age of the Barkly women and the much higher proportion of Aboriginal women.
Table 3: Demographic and obstetric characteristics for Barkly mothers
and babies in 2010 compared with other Australian women6,3
The young age of the women is the most outstanding feature of the Barkly cohort. Young age reflects and amplifies other disadvantages of women in the region, and may increase their vulnerability, particularly if they are required to travel outside the region for birthing. Research in a range of settings has shown that poorer outcomes of young mothers are associated with their limited access to acceptable care. High quality, accessible maternity care may overcome the increased risks of adverse outcomes for young mothers and their babies21,22.
Policy and planning considerations
In northern Canada an Indigenous midwife-led maternity service was initiated in 1986, with the explicit goal to end the routine evacuation of pregnant women to distant hospitals. Recent analysis of outcome data showed that women giving birth in remote villages experienced low rates of intervention. Perinatal mortality and congenital anomalies were within the expected range, despite high rates of food insecurity, unemployment, alcohol and drug use, and tobacco smoking23. Like their Canadian counterparts, the Aboriginal women in the Barkly region may benefit from midwifery services provided by their own people in their own communities24.
Current NT DoH protocol requires all women in the Barkly who are in labour or who give birth in health centres to be transferred to a regional maternity service25. Although this protocol does not refer to TCH, transfer of mothers and newborns from TCH to ASH is routine. Such practice is not consistent with the ACM Guidelines, which contain specific indications for referral20. In the absence of identified indications for referral, the routine transfer of women during pregnancy, labour and after giving birth presents an additional source of disadvantage for women who may already be disadvantaged by remoteness, young age and the inequalities experienced by Aboriginal people. Implementation of such a policy to transfer all women and their babies to a specialist service may not always provide best-practice care24. Maternity care must address social, emotional and cultural health needs, and be as close to home as possible24.
Limitations and strengths
This study described births from a regional cohort of women who received birthing care at the regional hospital over one year. No information was sought about women who gave birth outside central Australia. The study presents a pragmatic approach to considering birthing services in the region. If low-risk birthing services were available at TCH, some women who previously chose to give birth outside the Barkly region, other than at Alice Springs, may choose to remain in Tennant Creek for birthing. Generalisations cannot be drawn from the data, either for other cohorts of Barkly women or for women from elsewhere. Rather, the data provide a framework to consider service development in the region, and discuss options with women and care providers.
While maternity services throughout Australia have closed in recent years17, the Barkly region is distinctive in its extreme isolation and high proportion of Aboriginal women. This presents a challenge to the attempt to reconcile a range of medical, cultural, psychological and social issues. International examples of birthing services in remote areas, such as in Canada, need to be considered in planning future services in the Barkly region.
Analysis of the births to Barkly women in 2010 has highlighted the routine transfer of all women in labour and after giving birth, even in the absence of indications for specialist referral. The ACM Guidelines should be considered when local protocols are developed. Collaboration in the care of women who give birth outside ASH may enable specialists to be involved even when mother and baby are not in ASH. This may enhance the quality of maternity care for Barkly women.
Acknowledgements
The authors acknowledge the work of midwives Rita Apelt and Suzanne Peel who collected the data from the ASH records, and the Acute Care Information Services for data on births in TCH 2008 and 2009.
References
1. Australian Bureau of Statistics. 2011 Census QuickStats: All people - usual residents. (Online) 2011. Available: http://www.abs.gov.au/websitedbs/censushome.nsf/home/quickstats? opendocument&navpos=220 (Accessed 8 May 2012).
2. Australian Bureau of Statistics. National Regional Profile: Barkly (S) (Local Government Area). (Online) 2010. Available: http://www.abs.gov.au/AUSSTATS (Accessed 23 Oct 2012).
3. Li Z, McNally L, Hilder L, Sullivan EA. Australia's mothers and babies 2009. Perinatal statistics series no 25. Cat. no PER 52. Sydney, NSW: AIHW National Perinatal Epidemiology and Statistics Unit, 2011.
4. Zhang X, Johnstone K. Northern Territory Midwives' Collection. Mothers and Babies 2005. Darwin, NT: Department of Health and Families, 2009.
5. Tew K, Zhang X. Northern Territory Midwives' Collection. Mothers and Babies 2006. Darwin, NT: Department of Health and Families, 2010.
6. Thompson F, Zhang X, Dempsey KE. Northern Territory Midwives' Collection. Mothers and Babies 2007. Darwin, NT: Department of Health, 2012.
7. Department of Health. Tennant Creek Hospital. (Online) no date. Available: http://www.health.nt.gov.au/Hospitals/Tennant_Creek_Hospital/index.aspx (Accessed 6 January 2013).
8. Royal Flying Doctor Service. Tennant Creek General Practice. (Online) no date. Available: http://health.nt.gov.au/Service_Locator/Remote_Health_Centres/index.aspx (Accessed 6 January 2013).
9. Anyinginyi Health Aboriginal Corporation. Parlpuru Ninji Kari (Health Centre). (Online) no date. Available: http://anyinginyi.org.au/programs-services/health-centre (Accessed 6 January 2013).
10. Department of Health. Remote Health Centres. (Online) no date. Available: http://health.nt.gov.au/Service_Locator/Remote_Health_Centres/index.aspx (Accessed 6 January 2013).
11. Malyon R, Zhao Y, Guthridge S. Health workforce modelling, Northern Territory, 2006-2022. Darwin, NT: Department of Health and Families, 2010.
12. NT Department of Health. Specialist Outreach Visit schedules. (Online) 2012. Available: http://www.health.nt.gov.au/Specialist_Outreach_NT/Visit_Schedules/index.aspx (Accessed 6 January 2013).
13. Integrated Maternity Services, Department of Health Northern Territory Government. Maternity services in the Barkly, Northern Territory. Darwin, NT: Department of Health, Northern Territory Government, 2011.
14. Department of Health. Remote Health Atlas: Births in Hospital. (Online) 2008. Available: http://remotehealthatlas.nt.gov.au/births_in_hospital.pdf (Accessed 1 January 2013).
15. NT Department of Health. Patient Assistance Travel Scheme. (Online) 2008. Available: http://www.health.nt.gov.au/Hospitals/Patient_Assistance_Travel_Scheme/ (Accessed 8 January 2013).
16. Banscott Health Consulting. Maternity Services Review in the Northern Territory Report. Department of Health and Community Services, 2007. (Online) 2007. Available: http://www.health.nt.gov.au/Publications/Corporate_Publications/Maternity_Services_Model/index.aspx#ProposalsforanIntegratedMaternityServices (Accessed 21 February 2013).
17. Government of Australia. Australian Health Ministers' Conference: National Maternity Services Plan 2010. Canberra, ACT: Government of Australia, 2011.
18. Kildea S. Risky business: contested knowledge over safe birthing services for Aboriginal women. Health Sociology Review 2006; 15(4): 387-396.
19. Kildea S. And the women said... Report on birthing services for Aboriginal women from remote Top End Communities. Darwin, NT: Territory Health Services,1999.
20. Australian College of Midwives. National Midwifery Guidelines for Consultation and Referral 2nd edition. Canberra, ACT: Australian College of Midwives, 2008.
21. Raatikainen K, Heiskanen N, Verkasalo PK, Heinonen S. Good outcome of teenage pregnancies in high-quality maternity care. European Journal of Public Health 2005; 16(2): 157-161.
22. Loto OC, Ezechi BK, Kalu E, Loto AB, Ezech LO, Ogunniyi SO. Poor obstetric performance of teenagers: is it age- or quality of care-related? Journal of Obstetrics and Gynaecology 2004; 24(4): 395-398.
23. Van Wagner V, Osepchook C, Harney E, Crosbie C, Tulugak M. Remote Midwifery in Nunavik, Quebec, Canada: Outcomes of Perinatal Care for the Inuulitsivik Health Centre, 2000-2007. Birth 2012; 39(3): 1-8.
24. Kildea S, Kruske S, Barclay L, Tracy S. 'Closing the Gap': How maternity services can contribute to reducing poor maternal infant health outcomes for Aboriginal and Torres Strait Islander women. Rural and Remote Health 10: 1383. (Online) 2010. Available: www.rrh.org.au (Accessed 10 Jan 2013).
25. Department of Health. Remote Health Atlas: Births in Community. (Online) 2008. Available: http://remotehealthatlas.nt.gov.au/births_in_community.pdf (Accessed 10 January 2013).



