full article:
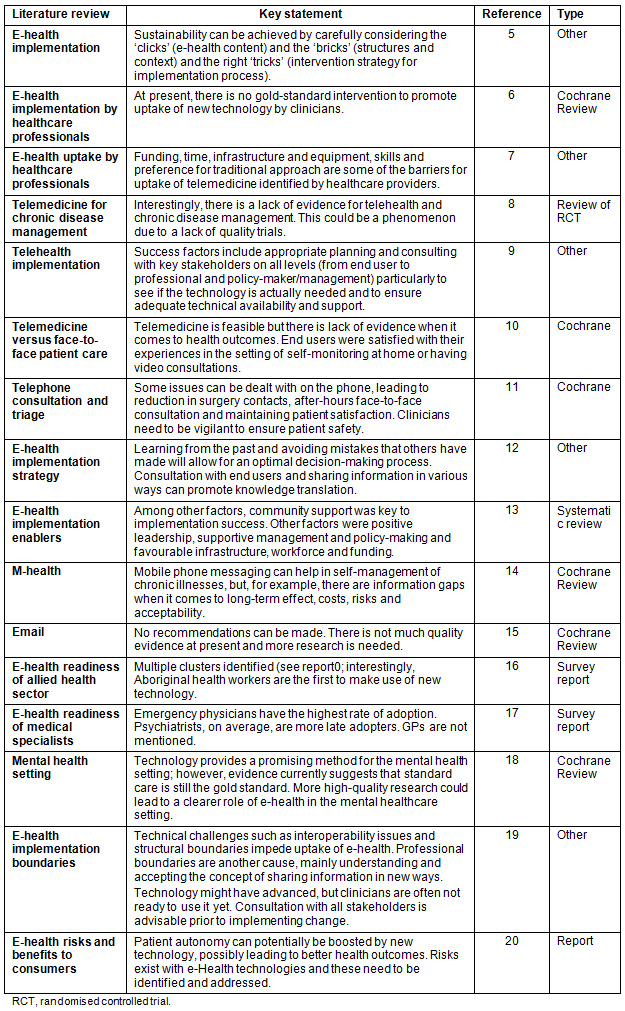
In the 1920s, John Flynn and Alf Traeger started a long-standing Royal Flying Doctor Service tradition of using telecommunications to facilitate healthcare delivery in remote Australia, telehealth in its prime1.Today the term 'e-health' is used to describe the transfer of health resources and provision of health care by electronic means2. E-health has been a recurrent topic in health reform, yet its implementation is complex3. A recent consumer survey about rural telehealth indicated a need for e-health technology but identified significant barriers4. It is currently not known what patients in rural and remote Australia want and need from e-health, nor what their concerns are. Similarly, as shown in Table 1, innovation in e-health requires an exploration of the views and needs of healthcare providers serving patients who might potentially benefit from e-health. The background and rationale for the three components of this study derive from these issues, and are outlined below.
Table 1: Key issues in e-health implementation5-20
Royal Flying Doctor Service setting
The Royal Flying Doctor Service South East Section (RFDS SE) provides traditional outreach visits to remote communities. In addition, it offers telehealth consultations to those in its geographic region 24 hours a day. As a result, the RFDS 'on call' medical officer (MO) consults with remote clinic nurses and patients from isolated properties in far-west New South Wales and surrounds by telephone. Over 5000 telehealth consultations typically are provided in any year21. Newer forms of electronic communication, such as video consultations, are under active consideration by RFDS SE in line with recent health reform22. Australia's national government has introduced the national broadband network (NBN) and personally controlled electronic health records (PCEHR) as ways to assist healthcare provision (see http://health.gov.au/ehealth-nbntelehealth). However, it is not clear how patients, healthcare providers and organisations in outback communities perceive these initiatives.
Readiness assessment and implementation theory
Roger's diffusion of innovations theory states that the pre-existing stage of readiness is important for implementation of new policies, practices or technologies23. To inform the selection of interventions targeting professionals or their patients to promote the uptake of technologies, the Cochrane Collaboration Effective Practice and Organisation of Care Group (EPOC) recommends a needs assessment for each unique context of innovation or reform24. Implementation strategies can then be designed in response to unique barriers and maximise opportunities for change25.
Aim of the current study
This study was designed to explore readiness for e-health in outback Australia by surveying RFDS SE health staff, managers and patients.
There is a number of existing instruments designed to measure readiness for telehealth26,27. One Canadian instrument28 has been especially recommended for its versatility across diverse projects to support implementation of telemedicine. This tool was adapted as described below.
Provider and organisational surveys
A nine-page instrument for healthcare providers containing 48 quantitative questions assessing core, engagement and structural readiness was customised. Satisfaction with status quo of healthcare delivery and options for change were key components. A qualitative section gave participants the opportunity to express their thoughts on e-health technologies in more detail. In December 2012, paper-based copies of this instrument were distributed to each member of the RFDS SE Health Services Department (HSD) to ensure all nursing, mental health, medical and dental staff could complete their survey anonymously.
A parallel version of the HSD instrument was developed for simultaneous administration to managers in RFDS SE to identify their perceptions, awareness and ideas about e-health technology. Forty-eight questions assessed core, engagement and workplace readiness and awareness of existing and future technology needs, internal planning, communication and administrative, human, and physical structures. All senior managerial RFDS SE Broken Hill staff were also invited to complete a paper-based survey anonymously in December 2012.
Client survey
This instrument was designed for RFDS SE clinic patients as a structured telephone interview with qualitative and quantitative items. It comprised basic demographic questions and three further parts (A, B and C). During development, it was pilot-tested with staff and volunteers not included in the main study to fine-tune the instrument in terms of readability and user-friendliness. Part A examined the patient's current healthcare situation and how it met their needs. Part B addressed e-health technology and how it might be useful. Part C further explored technology currently available to patients.
A convenience sample of patients sequentially attending 15 remote RFDS SE fly-in clinics during a two-week period in April and May 2013 was invited to participate. Sufficient copies of the study consent form were given to the attending MO every day for distribution in conjunction with local clinic staff. An information sheet was given to each patient with a consent form attached. The completed consent forms were returned in a sealed envelope to the RFDS SE base and processed by the research team. The telephone survey was then conducted at the patient's convenience. Data from very small, potentially identifiable communities have been collated before publication to further protect their identity.
Copies of the survey instruments can be obtained by contacting the corresponding author.
Sample sizes and statistical analysis
Provider and organisational surveys: Sample sizes for these surveys were determined by organisational size. Specifically, all eligible staff were surveyed. As both HSD and manager surveys were anonymous, response aiding strategies were not deployed at the level of the individual. Non-responders were never identifiable, precluding any assessment of response bias. Participation was encouraged through email notices and announcements at staff meetings.
Client survey: The patient sample size was pragmatically determined: resources restricted patient recruitment to a four-week period, divided into two blocks. RFDS SE provides on average about 600 remote clinic consultations per month across all clinics from its base in Broken Hill. The required target population size was estimated to be 200, assuming a worst-case scenario of a 25% response rate, which would result in a final sample size of 50. If 30% of patients are ready for e-health at baseline, this sample size would be sufficient to detect this with a 95% confidence interval of 0.1215.
Analysis: Information from returned surveys and telephone interviews was coded and entered into an Excel database. Frequencies were determined for basic demographic information and item responses. Calculation of scores per individual answer and subsection was undertaken as follows: each quantitative question in parts A-C was coded with a score of zero to five as per original design28.
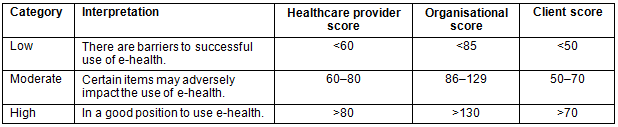
E-health readiness scores were calculated by adding all three core components, resulting in three different readiness categories: 'low', 'medium' and 'high' (Table 2). Low signifies that there are barriers for successful uptake of e-health. Medium signifies that certain items may adversely impact on implementation of e-health. High signifies a good position for e-health implementation. Qualitative responses were also entered into the same database.
Table 2: E-health readiness score interpretation (adapted from Jennett et al28)
Ethics approval
Ethics approval was obtained from the University of Sydney Human Research Ethics Committee (approval number 2012/2823).
Response rates and e-health scores
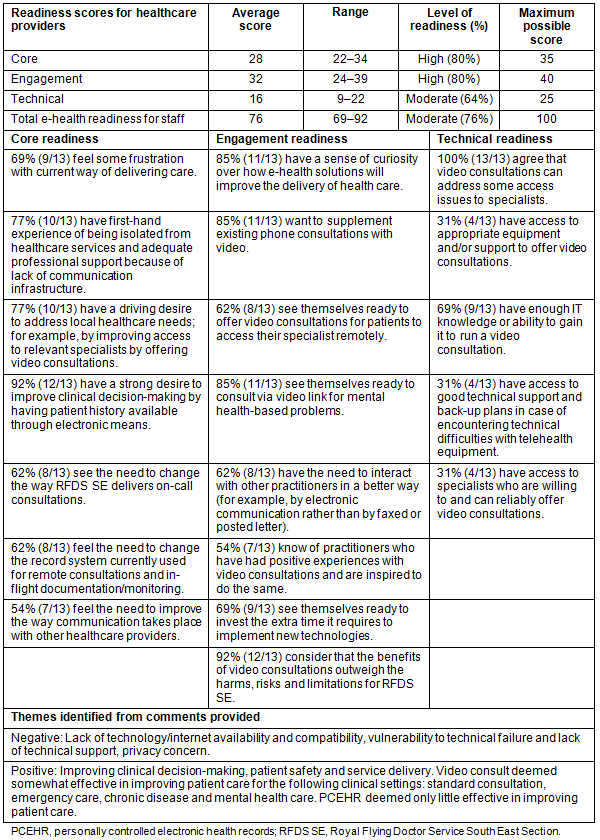
Healthcare provider (HSD) survey: Of 30 health service providers in RFDS SE, 13 staff members completed and returned surveys (43% response rate). Service providers had a high-moderate readiness score of 76 (Table 3). The technical readiness score was the lowest, suggesting major impediments ahead in implementation.
Healthcare providers were particularly concerned about privacy issues, technical support and vulnerability to technical failures, but could see benefits of e-health technology for clinical decision-making, patient safety and service delivery (Table 3, identified themes).
Healthcare providers deemed the PCEHR to be only slightly effective in improving patient care. By contrast, video consults were deemed somewhat effective in improving patient care for the following clinical settings: standard consultation, emergency care, chronic disease and mental health care (Table 3, additional comments).
Table 3: Healthcare provider survey readiness scores (n=13)
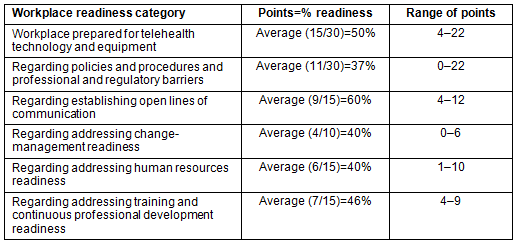
Organisational (managers) survey: Of six managers, five completed and returned surveys (83% response rate). Their average e-health readiness score was 123 out of 245 (range 80-157), equating to a moderate level of readiness for e-health. Table 4 shows that core need for e-health and planning readiness were high among managers; however, workplace readiness scores were moderate. Managers were overall confident of having adequate technical support. Table 5 displays workplace readiness in subsections, revealing key challenges ahead, such as policies and procedures and professional and regulatory barriers.
Table 4: Organisational survey readiness scores (n=5)

Table 5: Workplace readiness (n=5)
Client survey: Of 172 patients attending clinics during the survey period, 62 consented to participate (response rate 36%). However, only 45 participants could be reached to complete the phone interview. As shown in Table 6, overall core-readiness in the community was calculated as moderate. More than two-thirds of the population interviewed did not feel isolated and considered that their health needs were met. However, nearly all patients had a desire for change, particularly with respect to the model of healthcare delivery (Table 6). More than two-thirds had heard about telehealth. Ninety-one percent found video links helpful to overcoming cultural barriers, 88% found them useful for accessing specialists and 84% found them acceptable for mental health consultations. The majority found video links an addition to - rather than a replacement for - existing services (Table 6). Further, 95% indicated they felt in control of patient and community well-being. In their comments, several participants expressed concerns about losing face-to-face local health services as technology was introduced.
Table 6: Client survey readiness scores (n=45)
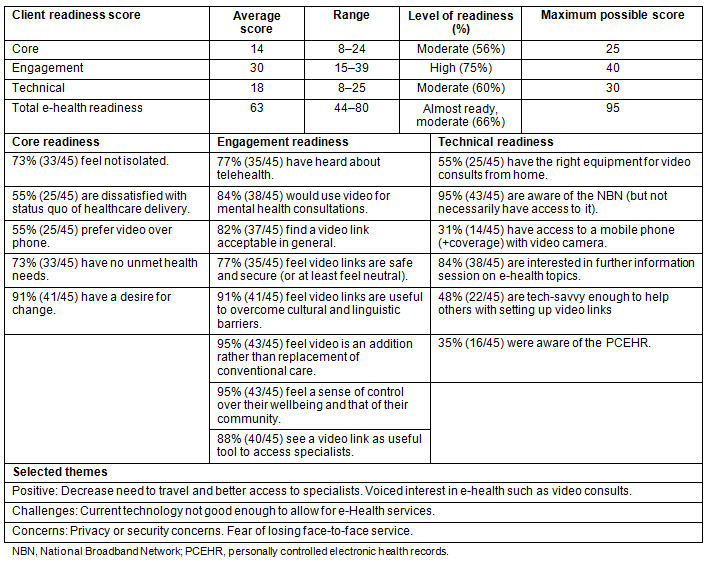
Almost all, 95%, were aware of the NBN but only 35% were aware of the PCEHR. Bandwidth issues and/or lack of NBN availability were mentioned as key issues by several participants in their qualitative comments.
Interest in further information sessions on e-health topics was high (Table 6). However, only 31% of the participants had access to mobile phone coverage with integrated video technology and only 55% had access to the necessary equipment for video consults from home. Finally, more than half (52%) were not tech-savvy enough to assist a neighbour with setting up a video link. Table 6 presents a selection of comments.
Discussion
Patient readiness is a key factor for the successful implementation of any given primary healthcare delivery model, including e-health29.
RFDS SE patients and providers were willing to engage in e-health as it is perceived as an overall benefit to the community. These results are supported by a previous survey published in January 2013 by the Consumer Health Forum4. Current literature suggests that e-health benefits rural communities and has a potential to decrease the 'urban-rural health disparities' and even improve 'rural medical workforces recruitment and retention'30.
The patients and healthcare providers who participated in this exploratory study perceived technological barriers as one major hurdle, in line with current literature7. This reflects the need for adequate funding to allow for quality infrastructure, equipment and on-demand technology support for end users as pointed out by clinicians and patients alike. In contrast, 60% of managers felt that current information support was adequate. All stakeholders were willing to engage with new technology to extend the traditional approach to include e-health for appropriate settings.
Implications for implementation
Results from the patient survey can assist organisations such as RFDS SE with the introduction of e-health with a particular focus on video consultations in remote emergency rooms and for access to medical specialists.
An implementation approach could include educational components based on Roger's work on innovation31, EPOC resources25 and the Ottawa model23, which can serve as relevant frameworks for adoption of innovations such as e-health technology32.The theory of diffusion of innovation focuses on the way in which new ideas or technologies (innovations) spread through groups or communities. Diffusion of innovation theory places important emphasis on innovators as 'change agents' who identify with the concerns of the community and influence decisions about the adoption of an innovation33.
For example, one focus of the implementation project is on the knowledge stage, where individuals learn about e-health innovations. Subsequently, individuals are in the persuasion stage, where opinions are formed, positive or negative. This can serve as a guide for the subsequent roll-out of e-health innovations. The focus of EPOC is on interventions designed to improve professional practice with or without patient-mediated strategies and the delivery of effective health service; for example, in this case, to influence e-health delivery through patients' needs. The Ottawa model may be particularly useful for RFDS SE as it is a method developed within continuity-of-care innovations involving multiple settings and keeping a focus on patients' needs in the knowledge translation process.
The barriers and enablers identified in this study are significant in demonstrating that a tailor-made, needs-based intervention strategy could assist organisations such as RFDS SE to adopt new technologies appropriately.
Hailey et al (2003) summarised the literature on determinants of success and failure in telehealth implementation9. This current exploratory study revealed the perceived needs of healthcare providers, organisational stakeholders and patients, including their preference for an approach genuinely motivated by the promise of better patient outcomes, cooperation of stakeholders, adequate support (technical, policy, financial and staff) and reliable equipment (Fig1).

Figure 1: Determinants of success and failure in telehealth9 and recommendations
for the Royal Flying Doctor Service South East Section from this exploratory study.
This is the first Australian attempt to explore the views of staff, managers and patients simultaneously in an assessment of needs, views and barriers prior to implementation of e-health. While interpretation of the study results is limited by relatively modest sample sizes, it was found that clinic patients, healthcare providers and RFDS SE as an organisation are interested in engaging in e-health to improve the level of healthcare delivery. However, there are challenges around the technical capacity and the structural and organisational support for an e-health venture in an outback setting. Specific patient, healthcare provider and organisational needs have been identified and allow for the development of a tailor-made implementation strategy particularly to overcome technical challenges.
The approach taken in this study could be expanded using a pre-post test design to permit rigorous evaluation of e-health implementation.
Acknowledgements
This study would have been impossible without the generous help of Kerry Kelly at RFDS SE. The excellent research assistance provided by Ken De Jong, Amy De Jong and Rachel Oommen has been vital to the success of this study.
References
1. RFDS. RFDS history. (Online). Available: www.flyingdoctor.org.au/About-Us/Our-History/85-years-of-the-RFDS (Accessed 1 October 2013).
2. WHO. E-Health. (Online). Available: www.who.int/trade/glossary/story021/en (Accessed 1 October 2013).
3. Jolly R. The e health revolution - easier said than done. Social Policy Section, Research Paper 3, 2011 to 2012 (Online). Available: www.aph.gov.au/About_Parliament/Parliamentary_Departments/Parliamentary_Library/pubs/rp/rp1112/12rp03 (Accessed 1 October 2013).
4. Rural Health Education Foundation. Survey results about telehealth in rural and remote areas. (Online) 2013. Available: http://ourhealth.org.au/have-a-say/have-your-say-now/rural-and-remote/results-our-telehealth-rural-and-remote-areas-survey (Accessed 1 October 2013).
5. Hage E, Roo JP, van Offenbeek MA, Boonstra A. Implementation factors and their effect on e-Health service adoption in rural communities: a systematic literature review. BMC Health Services Research 2013; 13: 19.
6. Gagnon MP, Légaré F, Labrecque M, Frémont P, Pluye P, Gagnon J, et al. Interventions for promoting information and communication technologies adoption in healthcare professionals. Cochrane Database of Systematic Reviews 2009; 1: CD006093.
7. Moffatt JJ, Eley DS. Barriers to the up-take of telemedicine in Australia - a view from providers. Rural and Remote Health 11(2): 1581. (Online) 2011. Available: www.rrh.org.au (Accessed December 2013).
8. Wootton R. Twenty years of telemedicine in chronic disease management - an evidence synthesis. Journal of Telemedicine and Telecare 2012; 18: 211-220.
9. Hailey D, Crowe B. A profile of success and failure in telehealth-evidence and opinion from the successes and failures in telehealth conferences. Journal of Telemedicine and Telecare 2003: S22-S24.
10. Currell R, Urquhart C, Wainwright P, Lewis R. Telemedicine versus face to face patient care: effects on professional practice and health care outcomes. Cochrane Database of Systematic Reviews 2000; 2: CD002098.
11. Bunn F, Byrne G, Kendall S. Telephone consultation and triage: effects on health care use and patient satisfaction. Cochrane Database of Systematic Reviews 2004; 3: CD004180.
12. Gagnon MP, Duplantie J, Fortin JP, Lamothe L, Légaré F, Labrecque M. Integrating scientific evidence to support telehomecare development in a remote region. Telemedicine Journal of E-Health 2009; 15(2): 195-198.
13. Wakerman J, Humphreys JS, Wells R, Kuipers P, Entwistle P, Jones J. Primary health care delivery models in rural and remote Australia - a systematic review. BMC Health Services Research 2008; 8: 276.
14. De Jongh T, Gurol-Urganci I, Vodopivec-Jamsek V, Car J, Atun R. Mobile phone messaging for facilitating self-management of long-term illnesses. Cochrane Database of Systematic Reviews 2012; 12: CD007459.
15. Atherton H, Sawmynaden P, Sheikh A, Majeed A, Car J. Email for clinical communication between patients/caregivers and healthcare professionals. Cochrane Database of Systematic Reviews 2012; 11: CD007978.
16. Department of Health and Ageing. The eHealth readiness of Australia's allied health sector. (Online) 2011. Available: www.health.gov.au/internet/publications/publishing.nsf/Content/ehealth-readiness-allied-toc (Accessed 1 October 2013).
17. Department of Health and Ageing. The eHealth readiness of Australia's medical specialists. (Online) 2011. Available: www.health.gov.au/internet/publications/publishing.nsf/Content/ehealth-readiness-medical-specialists-toc (Accessed 1 October 2013).
18. Välimäki M, Hätönen H, Lahti M, Kuosmanen L, Adams CE. Information and communication technology in patient education and support for people with schizophrenia. Cochrane Database of Systematic Reviews 2012; 10: CD007198.
19. King G, O'Donnell C, Boddy D, Smith F, Heaney D, Mair FS. Boundaries and e-health implementation in health and social care. BMC Medical Informatics and Decision Making 2012; 12: 100.
20. Osbolt J, Sands DZ, Dyke P, Pratt W, Rosas AG, Walker JM. Summary report of consumer ehealth: unintended consequences work group activities. Washington, DC: Office of the National Coordinator for Health Information Technology. (Online) 2012. Available: www.healthit.gov/sites/default/files/final_report_building_better_consumer_ehealth.pdf (Accessed 1 October 2013).
21. Royal Flying Doctor Service South East Section. Annual Report 2012/13. (Online). 2013. Available: www.flyingdoctor.org.au/About-Us/Annual-Reports (Accessed December 2013).
22. Department of Health and Ageing. Connecting health services with the future: modernising Medicare by providing rebates for online consultations. Discussion paper from the Australian Government. (Online) 2010. Available: www.naccho.org.au/download/projects-activities/telehealth/Telehealth%20discussion%20paper.pdf (Accessed 1 October 2013).
23. National Collaborating Centre for Methods and Tools. Ottawa model of research use: a framework for adopting innovations. Hamilton, ON: McMaster University. (Online) 2010 (Online). Available: www.nccmt.ca/registry/view/eng/65.html (Accessed 1 October 2013).
24. Cochrane Collaboration of Effective Practice and Organisation of Care (EPOC): Taxonomy. (Online). Available: http://epoc.cochrane.org (Accessed 1 October 2013).
25. Roman R. Diffusion of innovations as a theoretical framework for telecenters. Information Technologies and International Development 2003; 1(2): 53-66.
26. Legare E, Vincent C, Lehoux P, Anderson D, Kairy D, Gagnon MP, et al. Telehealth readiness assessment tools. Journal of Telemedicine and Telecare 2010; 16(30): 107-109.
27. Legare E, Vincent C, Lehoux P, Anderson D, Kaihry D, Gagnon MP, et al. Developing and validating the French-Canadian version of the practitioner and organizational telehealth readiness assessment tools. Journal of Telemedicine and Telecare 2010; (16): 140-146.
28. Jennett PA, Gagnon MP, Brandstad HK. Preparing for success: readiness models for rural telehealth. Journal of Postgraduate Medicine 2005; 51(4): 279-285. Tools available: www.fp.ucalgary.ca/telehealth/Readiness_Tools.htm (Accessed 1 October 2013).
29. Wakerman J, Humphreys JS, Wells R, Kuipers P, Entwistle P, Jones J. Primary health care delivery models in rural and remote Australia - a systematic review. BMC Health Services Research 2008; 8: 276.
30. Moffatt JJ, Eley DS. The reported benefits of telehealth for rural Australians. Australian Health Review 2010; 34(3): 276-281.
31. Rogers E. Diffusion of innovations. New York: Free Press, 1983.
32. Sanson-Fisher R. Diffusion of innovation theory for clinical change. Medical Journal of Australia 2004; 180(6): 55.
33. Davies P, Walker A, Grimshaw M. A systematic review of the use of theory in the design of guideline dissemination and implementation strategies and interpretation of the results of rigorous evaluations. Implement Science 2010; 5: 14.

