Rural and remote communities, especially Aboriginal communities, continue to face significant health disparity compared to their urban counterparts1-4. However, there is evidence reporting a correlation between effective and appropriate primary healthcare (PHC) delivery and closing health gaps5-7.
Current literature on essential structural PHC requirements includes measurable mainstream elements such as funding, workforce supply, supportive policy, infrastructure and linkages8,9. Recent literature provides a range of essential factors that need to be taken into account when redesigning PHC services: accessibility to services and workforce requirements10, evidence of effectiveness11, local priorities and the socioeconomic determinants of health12.
The importance of community readiness13 and involvement to develop local solutions to the challenges of providing services in rural and remote areas using a population health approach is becoming increasingly recognised14,15.
In Australia, strengthening PHC delivery is a key priority under national health reform, and provides an opportunity to consider service delivery with a holistic perspective16. The key question is: 'What facilitates and enables health system change at the local level, especially for rural and remote Aboriginal communities?'
This study examines the experience of one remote community towards a holistic delivery of PHC in a remote region of Western Australia. The Fitzroy Valley is situated in remote north-western Western Australia, servicing a population of approximately 3500 people with Aboriginal peoples from four main language groups17. The township of Fitzroy Crossing is centrally located and serves as a regional hub. The township population is approximately 1600, 60% of whom are Aboriginal, with Aboriginality increasing to 100% in the valley subregional hubs and satellite outstations17. Typical of regional WA, the local hospital emergency department is a key point of access to health care, including primary care services.
The Fitzroy Valley began its PHC journey in 2000. The principal 'change champion', leading the Aboriginal community controlled health service (ACCHS), had a vision to create a unique model for Aboriginal health. This vision integrated cultural, clinical and PHC services through a health services partnership. This vision received the encouragement and endorsement of the WA Minister of Health. After extensive community consultations, the ACCHS approached the local hospital to take on all clinical services, while the ACCHS maintained responsibility for environmental health, health education and health promotion. In delineating roles, duplication of services and competition for funding was avoided, leading to improved service delivery. The partnership was formalised in 2004 with government endorsement of a partnership agreement. The partnership included the local community health centre, which also provided remote health services. In 2007 all three services were co-located.
In 2009, the hospital was successful in its application as one of two WA sites to implement the Council of Australian Governments (COAG) section 19(2) exemption from the Health Insurance Act 197318,19. This initiative enables small rural and remote hospitals serving populations with catchments of fewer than 7000 people and an identified general practitioner (GP) workforce shortage to claim for non-admitted primary care. Under the exemptions, rebates are reinvested back into PHC services at the claiming site to enhance further expansion of PHC20.
This qualitative study describes the perspectives of key leaders involved in the health service change during the 19(2) implementation. The objective was to identify the key enablers that supported PHC re-orientation of the acute care model.
What is already known
- Poor access to PHC is a significant contributor to poorer health outcomes for rural and remote Australians compared to urban populations.
- The health of Aboriginal peoples remains unacceptably poorer, with a high chronic disease burden compared to non-Aboriginal people.
- Evidence suggests robust PHC systems can delay or prevent chronic disease.
- Rigorous evaluation of effective rural and remote PHC models is limited in Australia, with little known about appropriate models of remote Aboriginal PHC delivery.
What this study adds
- evidence that community participation in PHC service design for remote Aboriginal communities is crucial for sustainability
- evidence of the importance of health service partnerships supporting community self determination to improve health service delivery
- a description of the key enablers for reorienting services in remote Aboriginal communities to a PHC model
Key informants from the partnership operational group employed between 2004 and 2009 were interviewed between October 2012 and March 2013. Individual, in-depth interviews were completed with five of six senior leaders involved in the development of the Fitzroy Valley Health Partnership. Participants' backgrounds included medicine, health promotion, drug and alcohol management, and Aboriginal cultural health and policy. Because the study was exploratory in design, questions were open-ended and related to the barriers and enablers experienced in the health service redesign. Interviews were recorded and transcripts were thematically analysed. To provide research rigour, the transcripts were independently analysed by two investigators (VC, CR). Any differences were discussed and resolved. Four of five informants were interviewed face-to-face and one by teleconference.
Ethics approval
The study was approved by the WA Country Health Services Research Ethics Committee, WA Aboriginal Health Information and Ethics Committee, and the Kimberley Aboriginal Health Planning Forum Research Subcommittee; approval 2011:26.
A number of consistent themes emerged from the interviews (Fig1). The themes are described in order of the frequency with which they were mentioned by different participants. Three key enablers emerged as crucial in driving the changes towards a more PHC-orientated approach: community readiness, participation and desire for self-determination; health service relationships provided through a formal health service partnership; and strong local leadership.
The changes to healthcare services in the Fitzroy Valley were initiated and led by strong local community leaders. Community readiness for change in response to high mortality rates and the burden of disease became apparent when key individuals courageously expressed their concerns in public forums and described their vision for the future. Over a 2-year consultation period with Fitzroy Valley community groups led by local leaders and community elders, a consensus was reached regarding the type of health services the community wanted. 'In our culture we don't speak for somebody else' (community leader). The extensive and exhaustive consultation resulted in a unified position. The shared vision of a culturally secure health partnership promoting community self-determination resulted in a unique model of care for this Aboriginal community. This commitment from the community was also crucial for sustainability in an environment with high government staff turnover.
The formal partnership provided the necessary governance structure and formalised the relationship between the government health providers and the community. 'The partnership was really quite visionary' (senior Western Australian health manager). The partnership was both the vehicle for change and key to sustainability, but wouldn't have been possible without strong local leadership both in the community and the health service. These leaders persisted in the face of resistance to change from staff and the bureaucratic hurdles required and displayed determination to persevere when faced with challenges and barriers to change. 'Whatever the barrier is, you have to find a way through' (senior Western Australian health manager). One of the many barriers that need to be worked through was the Commonwealth funding requirement for the ACCHS to provide medical care.
The co-location of the ACCHS and government health service partners was important in terms of community perceptions, as well as facilitating communication and co-ordination. 'Co-locating our services really cemented the model in the community eye' (senior community leader). Co-location of the three services facilitated both formal and informal contact for staff and patients, and embedded the vision of the health service for both community and workforce.
Re-alignment of the hospital to a stronger PHC approach attracted a workforce excited by the prospect of making a real difference in remote Aboriginal health. 'This was so exciting, we had no problem with getting people to come here' (senior health department manager).
Funding generated through the Medicare 19(2) exemption policy was the final critical enabler identified. 'Hospitals don't need re-orienting. Governments do!' (senior health department manager). A separate Commonwealth funding stream establishing a GP-style clinic was very novel for the state-funded hospital. 'Everybody was totally risk averse rather than looking at how to make it work' (senior health department manager). An executive decision was made to employ a dedicated 19(2) project officer to address bureaucratic barriers. This decision gave direction to the 19(2) implementation, and by mid-2009 funding commenced. The successful implementation of 19(2) was an opportunity to expand access to PHC services and more specifically to improve chronic disease care.
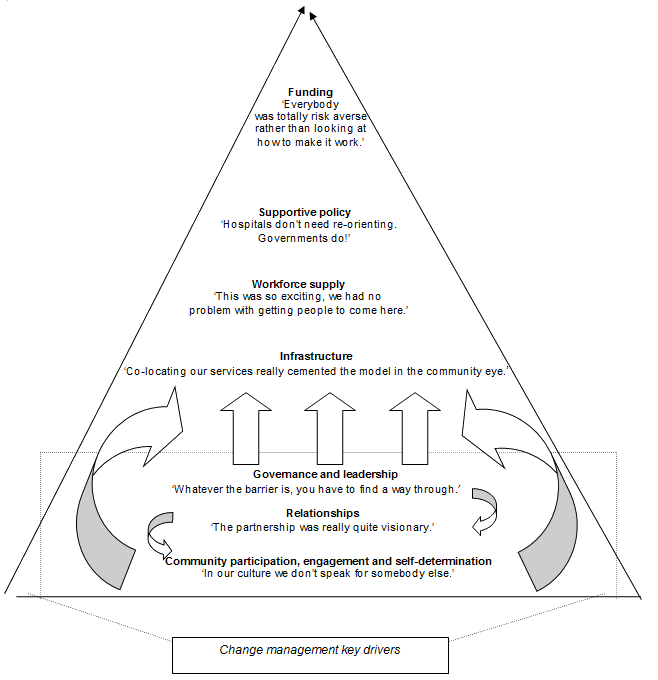
Figure 1: Summary of informant interview findings: hierarchy of major themes and the interactions between them. Quotes have been taken from the interview transcripts.
Discussion
This study identifies crucial enablers underpinning an effective community partnership model delivering PHC services to a remote Aboriginal region. This Western Australian partnership model exemplifies the importance of community readiness and local leadership for creating a sustainable PHC service that meets local community needs in an acceptable way.
The key enablers of this change were the willingness of other key partners for the community leaders to take the lead and provide the dedicated time and resources that allowed the community-driven model to be developed. This was reflected in the partnership, which recognised that cultural custodianship resides with the ACCHS, which takes the lead role in cultural responsibility. However, the hospital and community health were also required to shoulder their responsibility in providing a culturally safe service. Cultural custodianship reflects a genuine desire from the government health services to support Aboriginal self-determination by working in a paradigm not under their control, and it is this cultivation of good will that cements this partnership.
The partnership was pivotal in providing strong local leadership. Leadership is an integral factor associated with the successful organisational change, with two essential components: the alignment of leaders and leader sponsorship. Alignment refers to organisational sharing of the same values. Sponsorship signifies that leaders must be observed instigating change21. Alignment was readily demonstrated in this partnership with the sharing of a vision developed by the community through grassroots participation. Sponsorship was observed where the partnership showed commitment to working through bureaucratic and infrastructural barriers. Regular formal and informal meetings between the partnership, staff and community provided effective governance.
Co-location of the services associated with new infrastructure facilitated the implementation of change and cemented the community's view of the strength of the partnership arrangement, and provided a visual reminder.
The difficulties of recruiting and retaining essential staff to remote areas is well documented22. The re-orientation of the hospital to a stronger PHC approach facilitated the recruitment of staff who wanted to participate in the delivery of PHC services that would make a difference to the lives and wellbeing of Fitzroy Valley residents. This was enhanced by the publicity about community-initiated alcohol restrictions. Health professionals were motivated to improving Aboriginal health outcomes through a shared vision for the future.
The findings of this study add to the existing limited knowledge of how to develop effective PHC services in remote Aboriginal communities. Government-provided resources - infrastructure, workforce, policy and funding - are essential prerequisites for health service delivery8. However, this study highlights the critical alignment of three key enablers: community participation, readiness and self determination; the formal health services partnership; and local leadership, which enabled implementation and drove success in re-orientating an acute care hospital towards PHC delivery in a sustainable manner.
This study highlights the importance of local leadership both in the community and the health services to redesign health services to meet the needs of the community they serve.
Local leadership is essential for the redesign of community-based health services - each community is different but this principle can be applied to other community health services, regardless of their location.
Acknowledgements
This study was made possible through funding provided by a Western Australia State Health Research Advisory Council (SHRAC) Grant.
The research reported in this article is a project of the Australian Primary Health Care Research Institute, which is supported by a grant from the Commonwealth of Australia as represented by the Department of Health and Ageing. The information and opinions contained in it do not necessarily reflect the views or policy of the Australian Primary Health Care Research Institute or the Commonwealth of Australia.
References
1. Department of Social Services. Closing the gap: Prime Minister's report 2013. (Online) 2013. Available: http://www.dpmc.gov.au/pmc-indigenous-affairs/publication/closing-gap-prime-ministers-report-2015 (Accessed 14 July 2015).
2. Department of Health and Ageing. National health reform: improving primary health care for all Australians. (Online) 2011. Available: https://www.wentwest.com.au/images/docs/ImprovingPrimaryHealthCareforallAustralians_000.pdf (Accessed 14 July 2015).
3. Australian Institute of Health and Welfare. Australia's health 2014. (Online) 2014. Cat. no. AUS 178. Available: http://www.aihw.gov.au/publication-detail/?id=60129547205 (Accessed 14 July 2015)
4. Hoy WE, Baker PR, Kelly AM, Wang Z. Reducing premature death and renal failure in Australian Aboriginals. Medical Journal of Australia 2000; 172(10): 473-478.
5. Wakerman J, Humphreys J, Wells R, Kuipers K, Jones JA, Entwistle P, et al. Features of effective primary health care models in rural and remote Australia: a case study analysis. Medical Journal of Australia 2009; 191(2): 88-91.
6. Australian Institute of Health and Welfare. Australia's health 2012. Australia's health no. 13, cat. no. AUS 156. Canberra, ACT: AIHW, 2013.
7. Rowley KG, O'Dea K, Anderson I, McDermott R, Saraswati K, Tilmouth R, et al. Lower than expected morbidity and mortality for an Australian Aboriginal population: 10-year follow-up in a decentralised community. Medical Journal of Australia 2008; 188(5): 283-287.
8. Starfield B, Shi L, MacIntosh J. Contribution of primary health care to health systems and health. Milbank Quarterly 2005; 83(3): 457-502.
9. Australian Institute of Health and Welfare. Rural, regional and remote health: indicators of health system performance. Rural health series no. 10. (Online) 2008. Available: http://www.aihw.gov.au/WorkArea/DownloadAsset.aspx?id=6442459852 (Accessed 27 November 2013).
10. McGrail M, Humphreys J. The index of rural access: an innovative integrated approach for measuring primary care access. BMC Health Services Research 2009; 9: 124.
11. Segal L, Leach M. An evidence-based health workforce model for primary and community care. Implement Science 2011; 93(6): 1-8.
12. Keleher H. Population health planning for health equity. Australian Journal of Primary Health 2011; 17(4): 327-333.
13. Laverack G. Health promotion practice: building empowered communities. Maidenhead: Open University Press, 2007; 22.
14. Katterl R, Jackson Bowers E, Hagger C, Bywood P. Regionally based needs assessment in Australian primary health care. Adelaide: Primary Health Care Research and Information Service, 2011.
15. Farmer J, Nimegeer A. Community participation to design rural primary healthcare services. BMC Health Services Research 2014; 14: 130.
16. Steering Committee for the Review of Government Service Provision. National Agreement performance information 2010-11. (Online) 2011. Available: http://www.pc.gov.au/__data/assets/pdf_file/0018/118143/healthcare-agreement-2010-11.pdf (Accessed 14 July 2015).
17. Morphy F. Population, people and place: the Fitzroy Valley Population Project. Centre for Aboriginal Economic Policy Research working paper no. 70/2010. (Online) 2010. Available: http://caepr.anu.edu.au/sites/default/files/Publications/WP/CAEPRWP70.pdf (Accessed 27 November 2013).
18. Office of Parliamentary Counsel. Health Insurance Regulations 1975. (Online) 1975. Available: http://www.comlaw.gov.au/Details/F2013C00002 (Accessed 27 November 2013).
19. Department of Health. Memorandum of Understanding between the Commonwealth of Australia and Western Australia - relevant to the COAG 19(2) Exemption initiative. (Online) 2006. Available: http://www.amawa.com.au/wp-content/uploads/2013/03/mou_exemption.pdf (Accessed 27 November 2013).
20. Department of Health and Ageing. Medicare billing for primary care in small rural hospitals. COAG Section 19(2) Exemption for non-admitted services. (Online) 2007. Available: http://www.rdaq.com.au/Portals/RDAQ/Documents/Reports/Coag19fowebsite.pdf (Accessed 14 July 2015).
21. Kotter JP. Accelerate! Harvard Business Review 2012; 90(11): 44-58.
22. Productivity Commission. Australia's health workforce, Australian productivity research report. (Online) 2005. Available: http://www.pc.gov.au/inquiries/completed/health-workforce/report/healthworkforce.pdf (Accessed 14 July 2015).



