In Australia, residents of rural-remote areas experience significantly poorer health outcomes than residents of major cities1. Life expectancy is decreased by as much as 7 years, with excess deaths mainly attributed to cardiovascular disease, chronic obstructive pulmonary disease and cancers1. Tobacco smoking is a major risk factor for these diseases and smoking prevalence is between 1.2 and 1.7 times greater in rural-remote areas than major cities2. Therefore, reducing smoking prevalence among rural-remote residents has the potential to dramatically improve health outcomes.
In rural-remote Australia, government-controlled primary healthcare (PHC) services, such as hospital outpatient and primary health services, are well placed to deliver clinic-based anti-smoking programs because they provide multidisciplinary care, target whole communities and are located in the communities they serve3. While clinic-based anti-smoking programs are effective tobacco treatments4,5, little is known of the challenges encountered and strategies employed when implementing such programs through rural-remote PHC services.
The current understanding of these challenges and strategies is limited to that of rural England6, rural Appalachian Kentucky7 and rural-remote Indigenous populations of Australia8-15. Challenges cited include limited access to healthcare services due to insufficient resources, long travel distances and poor transport options, as well as high levels of community stress, mental illness and smoking. These studies focus on the challenges encountered when implementing programs for Indigenous or non-Indigenous groups rather than for communities where both populations co-exist. Australian rural-remote communities are demographically complex, consisting of a mix of Indigenous and non-Indigenous residents, as well as advantaged and disadvantaged people all accessing the same services. Other nations, such as Canada, the USA and New Zealand, have similar mixed communities in rural-remote areas. Therefore, there is a need for a broader understanding of the challenges encountered and the strategies employed when implementing anti-smoking programs in whole rural-remote communities.
The aim of this article is to explore the lived experiences of PHC staff involved in implementing a whole-of-community anti-smoking program in rural-remote Australia, specifically identifying the challenges encountered and strategies employed. The findings are beneficial for informing the design and delivery of this and other anti-smoking programs to improve their effectiveness and cost-benefit, thereby improving whole-of-community health outcomes in rural-remote areas.
Background to the anti-smoking program
In 2005, locally based government and Aboriginal community-controlled health organisations (ACCHOs) commenced implementing an anti-smoking program for seven remote communities of far western New South Wales (NSW), Australia. The program consisted of an individualised management plan, subsidised nicotine replacement therapy (NRT) and weekly one-on-one counselling and support sessions with a designated case manager over 12 weeks, in addition to Quitline telephone support. Clients unable to or failing to attend weekly appointments were followed up by their case manager by phone or in their home, community or workplace. Clients were also referred to a general practitioner (GP) for the NRTs varenicline or bupropion. Mental health and/or drug and alcohol issues were also assessed.
Case managers included nursing staff, Indigenous health workers and other PHC workers from government-controlled PHC and multipurpose facilities, and one ACCHO. Case manager training consisted of general smoking cessation education and training specific to program delivery. GP services were provided by local, independently operated clinics or the Royal Flying Doctor Service (RFDS).
Between 2008 and 2010, the program was evaluated by a six-member research team drawn from the organisations involved in implementing the program. The findings presented here are from a sub-study of that evaluation.
Study design and methodology
The purpose of this sub-study was to explore the lived experiences of health staff implementing an anti-smoking program; therefore a qualitative research design was adopted, guided by a phenomenological perspective. Phenomenology is used to describe the meaning of the lived experiences of those engaged with the phenomenon of interest16,17.
Study setting
The study was conducted in rural-remote communities of far-western NSW, a region occupying nearly 25% of NSW but supporting less than 0.5% of the population18,19. Ten per cent of the population identifies as Indigenous compared to 2.5% for all NSW, with four of the smaller participating towns reporting 37-58% of residents as Indigenous18. The region is classified as 'remote' overall20 and the average state suburb index of socioeconomic disadvantage is 1.9 where '1' is most disadvantaged and '10' is most advantaged21. At the time of the evaluation, smoking rates were 23-25%, compared to 17-18% for NSW overall22.
Participants and sampling
Study participants were purposively selected based on their involvement in implementing the program and their experience providing services to the participating communities. Because the pool of participants to draw from was limited to the constraints of the rural-remote setting, the aim of the selection process was to ensure that a range of views was represented rather than to achieve thematic saturation. Participants included case managers (primary healthcare staff such as nurses and Aboriginal healthcare workers) and health service managers (HSMs) employed by the government health department or ACCHO, and GPs employed by the RFDS (see Table 1). RFDS GPs were qualified to comment because they were intimately engaged in the delivery of the program, compared to non-RFDS GPs who did not have the same level of involvement.
All HSMs and GPs, personally invited to participate by the project officer, accepted the invitation. Approximately 80% of case managers, invited and encouraged to participate through their HSM, accepted. All study participants lived and/or worked in the study area. Two HSMs and all GPs were qualified to comment on all communities because they provided services to all seven. Case managers and the remaining HSMs were qualified to comment on five communities for the same reason.
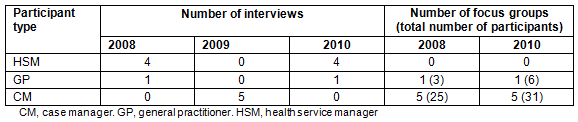
Table 1: Interview and focus group schedule and participant number for the anti-smoking program evaluation
Data collection
Data were collected using semi-structured in-depth interviews and focus groups in three phases over a 3-year period (Table 1) by three members of the research team. HSMs were interviewed to capture their experiences in implementing the program as a manager. Since HSMs work in isolation from other managers, individual interviews were appropriate for these participants. Case managers participated in focus groups to capture the team environment in which they work. The 2008 focus groups provided an overview of issues for investigators to explore in more depth during case manager interviews in 2009. Focus groups in 2010 enabled investigators to validate 2008 findings and identify any changes over time. GPs participated in interviews and focus groups to explore their perspectives in both the independent and team environment. Using both methods provided a more complete understanding of participants' experiences. Open-ended questions were designed and agreed upon by the research team. Questions differed slightly between participant types to reflect differing roles in the program, but largely addressed the following: smoking in the community, recruitment and referral of smokers to the program, implementation of the program and its impact on the workplace, staff support and training and program improvements.
Two research team members facilitated interviews and focus groups, probing participants when issues of particular interest were raised. Prompts were used when issues of interest did not spontaneously arise.
Because year 1 focus groups and interviews were repeated in year 3, some participants were involved in more than one data collection period. Case managers were not interviewed a second time because year 3 case manager focus groups did not reveal any new concepts.
Most discussions were conducted face-to-face and in the workplace. One GP interview took place in a public venue and case manager interviews were conducted by telephone. In 2010, one case manager focus group and one GP interview were conducted by telephone because participants could not keep the original face-to-face appointments. Interviews took 30-55 minutes and focus groups 55-75 minutes. All discussions were audio-recorded and supplemented with field notes.
Data preparation and management
Audio-recordings were transcribed verbatim by a professional service. Transcripts were cleaned of identifying data, corrected against audio-recordings and clarified using field notes. Only one case manager was asked, post-interview, to clarify a discussion point. Transcript data were managed using word processing software. Transcripts were labelled to identify participant quotes according to study location, method, study year and participant role in the program (see footnotes of Tables 2,3). Data analysis
Data analysis was based on the method described by Bradley et al23. The first round of analysis involved one investigator reviewing transcripts line-by-line and inductively assigning codes to emergent concepts. To faithfully report on emergent phenomena, data was not interpreted according to a pre-existing theoretical framework16. Through constant comparison, codes were refined until a hierarchy of conceptual codes and sub-codes was developed. This coding framework was finalised once no new concepts emerged.
The second round of analysis involved another investigator using the same coding framework to apply codes independently to transcripts. Coding discrepancies arising from the two investigators were discussed by the research team and resolved by consensus to optimise inter-coder reliability. The 'find' function in Microsoft Word was used to collate identically coded concepts, in place of NVivo. This manual approach to data analysis assisted familiarisation with the data and themes. Concepts of similar meaning were clustered to form themes and compared to the transcribed text in an iterative manner, improving the accuracy of synthesis and interpretation of meaning. Linkages between themes were also developed at this stage.
Ethics approval
The study was approved by the Greater Western Human Research Ethics Committee, NSW (project number GW2006/29) and the Board of Maari Ma Health Aboriginal Corporation.
This study found that implementing a smoking cessation intervention in rural-remote communities is challenged by the following: limited health service resources, collaboration and accessibility, high levels of community distress, mental illness and disadvantage, normalisation of smoking, and low staff morale. The study also identified strategies used by health staff to manage some of those challenges and improve program delivery. A summary of the findings and supporting quotes are presented in Tables 2 (challenges) and 3 (strategies). These findings highlight the issues that need to be considered when designing and delivering smoking interventions in rural-remote settings.
Table 2: Challenges of implementing an anti-smoking program in rural-remote communities: participant quotes
 Table 3: Strategies for implementing an anti-smoking program in rural-remote communities: participant quotes
Table 3: Strategies for implementing an anti-smoking program in rural-remote communities: participant quotes

Limited health service resources and access to training
Case managers participating in the study expressed feeling overwhelmed by their existing workloads, the diversity of their roles and the lack of staff, training and other resources to cope. A strategy used to minimise the impact of the program on existing workloads was to identify a target audience 'so that we can work within our capacity' (HSM-IVb1 - see footnotes of Tables 2 and 3 for code explanations). Those targeted were Indigenous, had chronic disease or were pregnant. Despite this attempt to work within capacity, case managers still felt overwhelmed and reported that often they did not have sufficient time to commit to client follow-up.
Several studies report that rural-remote and Indigenous health services are under-resourced, and insufficient to meet community needs, particularly in the context of delivering smoking interventions5,9,13,15,24. In addition, access to information and training opportunities is limited because staff training is not usually available locally15. Training improves knowledge and confidence in tobacco treatment but its impact diminishes over time8,12. The current study's participants reported that it was often impractical for staff to attend training sessions because their absence for days at a time would diminish local staff capacity. Some facilities tried to manage this problem by having one or two staff specialise in a clinical field who would attend training updates. While this approach meant training was affordable and the health facility could continue with business as usual, the 'specialist' staff member did not necessarily feel expert enough to train other staff on their return.
...for me to try and remember everything from then is a little bit difficult, but also ... a lot of people just went 'I don't believe you' ... 'well, here's the evidence' 'well, yeah I still don't believe you' ... trying to justify what the information I had was sometimes difficult ... (CM-IV2iv)
Consequently, participants expressed an intense need for a dedicated smoking cessation officer that could 'take away the pressure from the local case managers', give clients 'the level of attention that's required' (HSM-IVb1) and be a clinical consultant or 'central person to go to' (CM-FGb3). Other studies9,15,24 have found that appointing tobacco-dedicated staff is an important strategy for smoking interventions because they facilitate tobacco discussion, promote client recruitment and overcome time constraints13,25,26. The present findings suggest that such staff may also be important for providing the necessary expertise and training in the local setting.
Limited GP service access and involvement
Participants agreed that access to GP services for the program was essential for prescribing pharmacotherapies and for convincing clients of the merits of anti-smoking therapies. The use of pharmacotherapies has been shown to be more efficacious than placebo27 and GP advice can significantly increase a smoker's chances of quitting28. Case managers reported that GP appointments were difficult to access because of long waiting times or because services were impermanent or non-existent. Clients could wait a month to see a GP, resulting in the client losing interest. Consequently, case managers felt limited in their ability to deliver the program to clients.
In Australia, the number of GPs per head of population decreases with increasing remoteness29, while GP turnover increases30. Frequent turnover of health staff is a common problem in health facilities servicing rural-remote, Indigenous and disadvantaged communities6,15,31,32 and a barrier to the delivery of smoking interventions33,34. Staff turnover results in loss of knowledge, skills, continuity, momentum and relationships with partner organisations and the community, hindering the implementation of anti-smoking programs and diminishing their impact31-33. In the present study, case managers believed that some local GPs did not refer clients to the program because they did not value the support that programs provided. Consequently, a client's chance of success was limited by not having a case manager and GP who could, together, encourage further quit attempts. However, the lack of referral to the program by GPs may have arisen because GP turnover was high or because GPs had not been adequately informed about the program. Indeed, one GP expressed frustration at not being included in the development phase of the program and said that if GPs had been involved earlier, they may have referred more clients.
Lack of collaboration between organisations is a barrier in the implementation of anti-smoking programs9,15,34. Best practice occurs when physicians, nurses and other health professionals work in concert35 and partner organisations contribute resources34. Therefore, the early involvement of GPs and other health professionals in the development and implementation of anti-smoking programs is likely to enhance their success.
Stress, mental illness and limited access to mental health services
Although there is no definitive evidence to indicate that stress and mental illness are more prevalent in rural-remote than metropolitan areas2,36-40, the present study's participants perceived these issues to be significant for their clients, many of whom were Indigenous and disadvantaged. Stress is purported to be high among these populations and since smoking is used as a coping mechanism41,42, stress is a major cause of the failure of quit attempts9,10,41-44. The present study's participants voiced similar concerns when case managing clients.
... it's really difficult to have any conversations about quitting smoking ... until you've actually worked with someone to address some of their mental health issues ... (HSM-IVb1)
However, case managers reported often not being able to access mental health services for their clients. In rural-remote Australia, mental health services are reported to be poor and inadequate45-48, less available than in metropolitan areas49 and under-utilised because of cost, travel distance and confidentiality issues50. Case managers reported significant delays in mental health treatment because the client's mental health status was not severe enough for referral, or because the mental health team was only accessible through a GP, with whom appointments were difficult to secure. Case managers attempted to overcome the inaccessibility of these services by providing mental health support to the client themselves during weekly program appointments. The benefit of this approach was that clients had already developed a good rapport with their case manager and were able to talk about their mental health issues within the context of the program without feeling as if they were being mentally assessed. The disadvantage was that case managers felt they 'were not competent to (provide) that in an ongoing fashion' (CM-FGd3).
While the Australian Government has improved access to mental health services in rural-remote areas through GPs, Aboriginal medical services and the RFDS, gaps still exist because of travel distance, unstable work-life circumstances among clients and the potential for compromising confidentiality in small communities47. Participants reported that it was best for clients to access services on the same day of referral because of long travel distances. Unfortunately, however, same-day access was often not available. Furthermore, Indigenous clients were reported to be uncomfortable accessing services outside their local health facility. Given these constraints, the most effective mental health services in rural-remote areas may be those that are accessed 'in-house' through locally based PHC services and available on the day of referral.
Participants also suggested that stress and mental illness contributed to high cannabis use among clients. Clients using cannabis during quit attempts were particularly challenging to manage because it was often smoked in conjunction with tobacco, a practice also reported among remote Indigenous communities in the Northern Territory15. The present study's findings, and that of Robertson et al15. , suggest that concomitant cannabis and tobacco smoking needs to be addressed in smoking cessation training programs.
Barriers for clients engaging with health services
Participants reported that clients engaged in rural-specific occupations often had difficulty accessing health services for their appointments, either because they worked the same business hours or were required to work out of town, often at short notice. Similarly, the ongoing change in domestic circumstances for many Indigenous clients made it particularly difficult for them to commit to weekly appointments and access the support they needed. Similar challenges were raised in other studies of rural-remote, Indigenous and disadvantaged communities in both Australia and abroad6,9,33,43,44,51. Participants reported addressing these challenges by arranging transport for clients, providing after-hours services or by visiting clients in their homes and workplaces. For those clients who were unexpectedly transferred out of town for work, staff organised pharmacotherapies at short notice, to ensure clients had sufficient supplies. In addition, the main structure of the program was changed. Instead of offering the program as a set 12-week course, commencing on a predetermined date, staff commenced offering it on a continuing basis so that clients could 'tap in and tap out as they needed' (CM-IV2v). This approach also allowed relapsing clients to recommence the program at will. Flexibility was therefore perceived as essential for the program, as has been reported for other smoking interventions9,51-54.
Regular contact between the case manager and client was seen as critical for a successful quit attempt. Case managers were expected to follow up clients each week and make contact with 'no-show' clients. Case managers, however, were concerned that persistent follow-up could place 'extra pressure on [clients] ... [and] hinder that relationship' (CM-IV2v), deterring some clients from attending the service altogether. While no other studies were found to indicate that persistent follow-up could be perceived as harassing behaviour, the current case managers reported it was important to know the client well enough so that they knew when to provide support and when to back off. Participants also reported that Indigenous clients were best case-managed by community-based Indigenous health workers to overcome similar barriers to engaging with health services and the program. Other Indigenous-focused studies have drawn the same conclusion13,15,24,54. One caveat is that it may not be culturally acceptable for Indigenous health workers to advise elders8. This issue was not raised by the current participants.
Normalisation of smoking in the community
Participants reported that smoking was normalised in their communities, making clients particularly vulnerable to relapse when significant others continued to smoke around them. Similar results have been found for disadvantaged and Indigenous communities9,10,42,43,55. Case managers attempted to address this challenge by encouraging clients to set aside smoke-free rooms or to make the entire house a smoke-free zone. Case managers also suggested that a more effective approach for the rural-remote setting might be to deliver the program to groups of clients rather than to individuals to overcome the problem of an unsupportive social environment. Participants suggested that group-based interventions might be particularly pertinent for Indigenous people because they live in extended family groups and family members can support and motivate one another. Additionally, Indigenous culture is community focused; if all members of the group are attempting to quit then there may be fewer triggers for relapse. Studies demonstrate that group-based programs can achieve better quit rates than one-on-one programs, particularly for disadvantaged, Indigenous and mentally ill people12,53,56. However, scheduled group-based programs can be problematic for clients in rural-remote locations where travel distances are long, public transport is poor and day-to-day circumstances are unpredictable6,9. One study suggested that both individual and group support were needed9.
Socioeconomically disadvantaged communities
Rural-remote areas have a higher proportion of people living in low income households than major cities (25-27% compared to 17%) and the average rural-remote weekly household income is 4-16% less than the national average57. NRT cost is a significant barrier for smoking cessation among Indigenous and disadvantaged communities10,12,14,42 while subsidised or free NRT is an enabler35,53,58. Participants reported that the program provided subsidised NRT for two reasons: full-cost NRT would be unaffordable for the many disadvantaged clients, and charging a small fee encouraged clients to be more committed to their quit attempt. Case managers noted that subsidised NRT not only motivated clients to make a quit attempt but also kept them engaged with the program. Some clients were reported to continue accessing subsidised NRT even after program completion, helping them feel more confident to remain abstinent.
Varenicline has been shown to be more efficacious than placebo for smoking cessation27 but study participants viewed its cost as a significant barrier for clients engaging with the program. At the time of this study, the pharmaceutical benefit scheme (PBS) subsidised the cost of varenicline only once in a 12-month period59. Since most people make several quit attempts before achieving success, this regulation was perceived as a hindrance to smoking cessation because subsequent quit attempts in the same year were unaffordable. Participants suggested that the legislation be reviewed so that clients could access a second subsequent course of PBS-subsidised varenicline in a 12-month period. Indeed, in 2009, a second subsidised course was recommended to assist successfully quit program-enrolled clients to maintain abstinence59. The present findings suggest that a second subsidised course may also be beneficial for clients unable to quit first time, provided they too are enrolled in a support program.
Low staff morale
Participants commented that working in rural-remote and Indigenous health could be very discouraging because staff were 'expecting to see improvement on a daily basis' (HSM-IVb2). Case managers admitted to high expectations for the program and becoming despondent when the quit rate was much lower than anticipated. Similar findings were noted in other smoking cessation studies where staff morale waned and a sense of helplessness took over8,31.
Even for metropolitan communities where smoking has been de-normalised, 6- and 12-month quit rates are no higher than 14% and 17%60,61. For rural-remote communities where smoking is still very much the norm, it would be realistic to expect quit rates to be much lower, but it is difficult to ascertain rural-remote quit rates from the literature because program-completion rates are often low62-65. For programs where completion rates are high, quit rates are 6-19%41,63,66,67. Consequently, participants suggested that case managers be educated on the expected level of success for any anti-smoking program, and be prepared for an even lower quit rate for 'tough' target populations such as rural-remote communities.
Participants also suggested that it was important to boost case manager confidence and morale, as well as reward them for their efforts. HSMs stressed that case managers needed to be reminded that even one success was a significant achievement because of the flow-on effect to the client's family. Case managers were encouraged to think about 'every effort being a success rather than just the quitting' and to 'count your successes in ones' (HSM-IVb2).
... if you have one person change ... one thing about one aspect of their health, one time then that's a success ... (HSM-IVb2)
The present study indicates that health staff implementing whole-of-community anti-smoking programs in rural-remote Australia encounter a number of challenges including limited primary and mental healthcare resources, collaboration and accessibility; high levels of community distress, smoking and disadvantage; and low staff morale. Participants were able to recommend strategies to manage some of these challenges, including identifying a target audience for the intervention and appointing tobacco-dedicated staff; collaborating with GP and mental health services from the inception of the program to improve their involvement and accessibility; providing client transport, home visits and out-of-hours appointment times; providing group-based smoking programs to manage the influence of a smoking environment; providing ongoing subsidised pharmacotherapies; localising staff training and updates; and regularly boosting staff morale and tempering expectations.
A strength of the present study was that health staff employed in differing roles in various locations voiced similar views over the 3-year study period. Therefore, it is expected that the themes presented here are trustworthy and credible for this rural-remote population. In addition, while thematic saturation was not necessarily achieved, a wide cross-section of views was represented within the constraints of a limited pool of participants.
Although the program was delivered to rural-remote communities with significant proportions of Indigenous people, the views of Indigenous health staff may have been underrepresented. Only four interviews were conducted with Indigenous participants, and non-Indigenous outnumbered Indigenous participants in focus groups. Furthermore, the non-Indigenous investigators may have been insufficiently skilled to canvass the opinions of Indigenous participants, or may have misinterpreted comments during coding and thematic analysis. Thus, the findings of this study may have a non-Indigenous bias. However, since the present results and those of Indigenous studies9,10,12,13,15 are similar, the findings are likely to reflect both Indigenous and non-Indigenous issues.
Existing Australian studies have focused on smoking interventions delivered to rural-remote Indigenous communities. It is believed that this is the first Australian study to focus on the implementation of a whole-of-community anti-smoking program in rural-remote areas. Understanding the challenges encountered and the strategies employed when implementing such programs can assist rural-remote PHC services to design and deliver more effective anti-smoking programs. The present findings have the potential to improve the effectiveness and cost-benefit of anti-smoking programs, thereby improving whole-of-community health outcomes in rural-remote areas.
Acknowledgements
This project was funded by a NSW Health Promotion Demonstration Grant, NSW Ministry of Health, Australia. The views expressed are those of the authors and do not necessarily represent those of the NSW Ministry of Health.
References
1. Australian Institute of Health and Welfare. Rural, regional and remote health: indicators of health status and determinants of health. Rural Health Series no. 9. Cat. No. PHE 97. Canberra, ACT: AIHW, 2008.
2. Australian Institute of Health and Welfare. 2010 National Drug Strategy Household Survey report. Drug statistics series no. 25. Cat. No. PHE 145. Canberra, ACT: AIHW, 2011.
3. Department of Health and Ageing. National strategic framework for rural and remote health. Canberra, ACT: Commonwealth of Australia, 2012.
4. Miller M, Wood L. Effectiveness of smoking cessation interventions: review of evidence and implications for best practice in Australian health care settings. Australian and New Zealand Journal of Public Health 2003; 27(3): 300-309.
5. Carson KV, Brinn MP, Peters M, Veale A, Esterman AJ, Smith BJ. Interventions for smoking cessation in Indigenous populations. Cochrane Database of Systematic Reviews 2012; 1. Art.No.: CD009046. DOI: 10.1002/14651858.CD009046.pub2.
6. Bauld L, Coleman T, Adams C, Pound E, Ferguson J. Delivering the English smoking treatment services. Addiction 2005; 100 (Suppl. 2): 19-27.
7. Kruger TM, Howell BM, Haney A, Davis RE, Fields N, Schoenberg NE. Perceptions of smoking cessation programs in rural Appalachia. American Journal of Health Behavior 2012; 36(3): 373-384.
8. Harvey D, Tsey K, Cadet-James Y, Minniecon DL, Ivers R, McCalman J, et al. An evaluation of tobacco brief intervention training in three Indigenous health care settings in North Queensland. Australian and New Zealand Journal of Public Health 2002; 26(5): 426-431.
9. Lindorff K. Tobacco - time for action. Canberra, ACT: National Aboriginal Community Controlled Health Organisation. (Online) 2002. Available: http://trove.nla.gov.au/work/26537245?selectedversion=NBD41306181 (Accessed 30 October 2015).
10. Mark A, McLeod I, Booker J, Ardler C. Aboriginal health worker smoking: a barrier to lower community smoking rates? Aboriginal and Islander Health Worker Journal 2005; 29(5): 22-26.
11. Pilkington AAG, Carter OBJ, Cameron AS, Thompson SC. Tobacco control practices among Aboriginal health professionals in Western Australia. Australian Journal of Primary Health 2009; 15(2): 152-158.
12. Johnston V, Thomas DP. What works in Indigenous tobacco control? The perceptions of remote Indigenous community members and health staff. Health Promotion Journal of Australia 2010; 21(1): 45-50.
13. Thomas D, Johnston V, Fitz J. Lessons for Aboriginal tobacco control in remote communities: an evaluation of the Northern Territory 'Tobacco Project'. Australian and New Zealand Journal of Public Health 2010; 34(1): 45-49.
14. Dawson AP, Cargo M, Stewart H, Chong A, Daniel M. Aboriginal Health Workers experience multilevel barriers to quitting smoking: a qualitative study. International Journal for Equity in Health 2012; 11: 27.
15. Robertson JA, Conigrave KM, Ivers R, Usher K, Clough AR. Translation of tobacco policy into practice in disadvantaged and marginalized subpopulations: a study of challenges and opportunities in remote Australian Indigenous communities. Health Research Policy and Systems 2012; 10: 23
16. Hycner RH. Some guidelines for the phenomenological analysis of interview data. Human Studies 1985; 8(3): 279-303.
17. Starks H, Trinidad SB. Choose Your Method: A comparison of phenomenology, discourse analysis, and grounded theory. Qualitative Health Research 2007; 17(10): 1372-1380.
18. Australian Bureau of Statistics. 2011 census. (Online). Available: http://www.abs.gov.au/websitedbs/censushome.nsf/home/census?opendocument&navpos=10 (Accessed 14 February 2014).
19. Australian Bureau of Statistics. National regional profile, 2007-2011. (Online). Available: http://www.ausstats.abs.gov.au/ausstats/nrpmaps.nsf/NEW+GmapPages/national+regional+profile (Accessed 19 February 2014).
20. National Centre for Social Applications of GIS. National Centre for Social Applications of Geographic Information Systems. (Online). Available: http://www.spatialonline.com.au (Accessed 4 February 2015).
21. Australian Bureau of Statistics. Census of population and housing: socio-economic indexes for areas (SEIFA), Australia. (Online) 2011. Available: http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/2033.0.55.0012011?OpenDocument (Accessed 12 February 2014).
22. Centre for Epidemiology and Evidence. Health Statistics New South Wales. (Online) 2015. Available: http://www.healthstats.nsw.gov.au (Accessed 23 January 2015).
23. Bradley EH, Curry LA, Devers KJ. Qualitative data analysis for health services research: developing taxonomy, themes and theory. Health Services Research 2007; 42(4): 1758-1772.
24. Marley JV, Kitaura T, Atkinson D, Metcalfe S, Maguire GP, Gray D. Clinical trials in a remote Aboriginal setting: lessons from the BOABS smoking cessation study. BMC Public Health 2014; 14: 579.
25. Miller NH. Translating smoking cessation research findings into clinical practice: The 'Staying Free' Program. Nursing Research 2006; 55(4S): S38-S43.
26. McDaniel AM, Stratton RM, Britain M. Systems approaches to tobacco dependence treatment. Annual Review of Nursing Research 2009; 27(1): 345-363.
27. Eisenberg MJ, Filion KB, Yavin D, Bélisle P, Mottillo S, Joseph L, et al. Pharmacotherapies for smoking cessation: a meta-analysis of randomized controlled trials. Canadian Medical Association Journal 2008; 179(2): 135-144.
28. Zwar NA, Richmond RL. Role of the general practitioner in smoking cessation. Drug and Alcohol Review 2006; 25(1): 21-26.
29. Department of Health and Ageing. Report on the Audit of Health Workforce in Rural and Regional Australia. Canberra, ACT: Commonwealth of Australia, 2008.
30. Russell DJ, Humphreys JS, McGrail MR, Cameron WI, Williams PJ. The value of survival analyses for evidence-based rural medical workforce planning. Human Resources for Health 2013; 11: 65.
31. Zapka J, Goins KV, Pbert L, Ockene JK. Translating efficacy research to effectiveness studies in practice: lessons from research to promote smoking cessation in community health centers. Health Promotion Practice 2004; 5(3): 245-255.
32. Ritchie D, Gnich W, Parry O, Platt S. 'People pull the rug from under your feet': barriers to successful public health programmes. BMC Public Health 2008; 8: 173.
33. Panaretto K, Coutts J, Johnson L, Morgan A, Leon D, Hayman N. Evaluating performance of and organisational capacity to deliver brief interventions in Aboriginal and Torres Strait Islander medical services. Australian and New Zealand Journal of Public Health 2010; 34(1): 38-44.
34. MacLean S, Berends L, Hunter B, Roberts B, Mugavin J. Factors that enable and hinder the implementation of projects in the alcohol and other drug fields. Australian and New Zealand Journal of Public Health 2012; 36(1): 61-68.
35. McIvor A, Kayser J, Assaad J-M, Brosky G, Demarest P, Desmarais P, et al. Best practices for smoking cessation interventions in primary care. Canadian Respiratory Journal 2009; 16(4): 129-134.
36. Judd FK, Jackson HJ, Komiti A, Murray G, Hodgins G, Fraser C. High prevalence disorders in urban and rural communities. Australian and New Zealand Journal of Psychiatry 2002; 36(1): 104-113.
37. Murray G, Judd F, Jackson H, Fraser C, Komiti A, Hodgins G, et al. Rurality and mental health: the role of accessibility. Australian and New Zealand Journal of Psychiatry 2004; 38(8): 629-634.
38. Australian Institute of Health and Welfare. Australia's health, 2014. Australia's Health Series no. 14. Cat. no. AUS 178. Canberra, ACT: AIHW, 2014.
39. Kelly BJ, Stain HJ, Coleman C, Perkins D, Fragar L, Fuller J, et al. Mental health and well-being within rural communities: the Australian rural mental health study. Australian Journal of Rural Health 2010; 18(1): 16-24.
40. Kelly BJ, Lewin TJ, Stain HJ, Coleman C, Fitzgerald M, Perkins D, et al. Determinants of mental health and well-being within rural and remote communities. Social Psychiatry and Psychiatric Epidemiology 2011; 46(12): 1331-1342.
41. DiGiacomo M, Davidson PM, Davison J, Moore L, Abbott P. Stressful life events, resources, and access: key considerations in quitting smoking at an Aboriginal Medical Service. Australian and New Zealand Journal of Public Health 2007; 31(2): 174-176.
42. Bryant J, Bonevski B, Paul C, O'Brien J, Oakes W. Developing cessation interventions for the social and community service setting: a qualitative study of barriers to quitting among disadvantaged Australian smokers. BMC Public Health 2011; 11: 493.
43. Stead M, MacAskill S, MacKintosh A-M, Reece J, Eadie D. 'It's as if you're locked in': qualitative explanations for area effects on smoking in disadvantaged communities. Health & Place 2001; 7(4): 333-343.
44. Smith KB, Humphreys JS, Wilson MGA. Addressing the health disadvantage of rural populations: how does epidemiological evidence inform rural health policies and research? Australian Journal of Rural Health 2007; 16(1): 56-66.
45. Parslow RA, Jorm AF. Who uses mental health services in Australia? An analysis of data from the National Survey of Mental Health and Wellbeing. Australian and New Zealand Journal of Psychiatry 2000; 34(6): 997-1008.
46. Murray G, Hodgins G, Judd F, Jackson H, Davis J. Introduction of a clinical psychology intern program to a rural mental health service. Australian Psychologist 2002; 37(2): 129-134.
47. Department of Health and Ageing. Mental Health Service in Rural and Remote Areas program evaluation. Final evaluation report, version 1.3. Canberra, ACT: Commonwealth of Australia, 2011.
48. Perkins D, Fuller J, Kelly BJ, Lewin TJ, Fitzgerald M, Coleman C, et al. Factors associated with reported service use for mental health problems by residents of rural and remote communities: cross-sectional findings from a baseline survey. BMC Health Services Research 2013; 13: 157.
49. Betts VT, Thornicroft G. International mid-term review of the second National Mental Health Plan for Australia. National Mental Health Strategy. Canberra, ACT: Department of Health and Ageing, 2002.
50. Handley T, Kay-Lambkin F, Inder K, Lewin T, Attia J, Fuller J, et al. Self-reported contacts for mental health problems by rural residents: predicted service needs, facilitators and barriers. BMC Psychiatry 2014; 14: 249.
51. Kwong K, Ferketich AK, Wewers ME, Shek A, Tsang T, Tso A. Development and evaluation of a physician-led smoking cessation intervention for low-income Chinese Americans. Journal of Smoking Cessation 2009; 4(2): 92-98.
52. Ritchie D, Schulz S, Bryce A. One size fits all? A process evaluation - the turn of the 'story' in smoking cessation. Public Health 2007; 121(5): 341-348.
53. Mikhailovich K, Morrison P. An evaluation of a smoking cessation program for special populations in Australia. Journal of Smoking Cessation 2008; 3(1): 50-56.
54. DiGiacomo M, Davidson PM, Abbott PA, Davison J, Moore L, Thompson SC. Smoking cessation in Indigenous populations of Australia, New Zealand, Canada, and the United States: elements of effective interventions. International Journal of Environmental Research and Public Health 2011; 8: 388-410.
55. Johnston V, Thomas D. Smoking behaviours in a remote Australian Indigenous community: the influence of family and other factors. Social Science & Medicine 2008; 67(11): 1708-1716.
56. Mardle T, Merrett S, Wright J, Percival F, Lockhart I. Real world evaluation of three models of NHS smoking cessation service in England. BMC Research Notes 2012; 5: 9.
57. Australian Bureau of Statistics. Australian social trends. Catalogue no. 4102.0. Canberra, ACT: ABS, 2003.
58. Bryant J, Bonevski B, Paul C, O'Brien J, Oakes W. Delivering smoking cessation support to disadvantaged groups: a qualitative study of the potential of community welfare organizations. Health Education Research 2010; 25(6): 979-990.
59. Department of Health and Ageing. Public summary documents by product: varenicline tartrate, tablet, 1mg, Champix®, November 2009. (Online) 2009. Available: http://www.pbs.gov.au/info/industry/listing/elements/pbac-meetings/psd/2009-11/pbac-psd-Varenicline-nov09 (Accessed 30 October 2015).
60. Zhu S-H, Melcer T, Sun J, Rosbrook B, Pierce JP. Smoking cessation with and without assistance: a population-based analysis. American Journal of Preventive Medicine 2000; 18(4): 305-311.
61. Fiore MC, McCarthy DE, Jackson TC, Zehner ME, Jorenby DE, Mielke M, et al. Integrating smoking cessation treatment into primary care: an effectiveness study. Preventive Medicine 2004: 38(4): 412-420.
62. Hancock L, Sanson-Fisher R, Perkins J, McClintock A, Howley P, Gibberd R. Effect of a community action program on adult quit smoking rates in rural Australian towns: the CART project. Preventive Medicine 2001; 32(2): 118-127.
63. Mark A, McLeod I, Booker J, Ardler C. The Koori Tobacco Cessation Project. Health Promotion Journal of Australia 2004; 15(3): 200-204.
64. Queensland Health. SmokeCheck Evaluation Report 2006. Brisbane, Qld: Queensland Government, 2007.
65. Gould G, McChecan A, van der Zwan R. Give up the smokes: a smoking cessation program for Indigenous Australians. In: Proceedings, 10th National Rural Health Conference; May, Cairns, Qld. (Online) 2009. Available: http://nrha.org.au/10thNRHC/10thnrhc.ruralhealth.org.au/papers/docs/Gould_Gillian_D9.pdf (Accessed 11 July 2013).
66. Adams K, Rumbiolo S, Charles S. Evaluation of Rumbalara's 'No More Dhonga' short course in giving up smokes. Aboriginal and Islander Health Worker Journal 2006; 30 (5): 20-21.
67. Ivers R, Farrington M, Burns C, Bailie R, D'Abbs P, Richmond R, Tipiloura E. A study of the use of free nicotine patches by Indigenous people. Australian and New Zealand Journal of Public Health 2003; 27(5): 486-490.



