Introduction
In response to concerns about the rural health workforce shortage, the Australian Government funded clinical schools in rural locations across Australia in 2000. One of the aims of this initiative is that, in training students in a rural community, they will be more likely to return to practice in a rural community after graduation. This major effort focuses on long-term placements in rural areas during students' clinical training1. There is significant evidence that graduates who have had long placements in rural areas are likely to return to a rural location to practice2-7. The University of Melbourne (UoM) established a rural clinical school (RCS) in Shepparton, 175 km north of Melbourne, Victoria in 2001, with other major Victorian sites at Ballarat 110 m west, and Wangaratta 240 km north-east of Melbourne.
The first students commenced their clinical training at the RCS in 2002. The first two intakes were small and limited to students who chose the RCS as their first preference (n = 10 and 14). From 2004, the RCS has met the Commonwealth requirement of 25% of the Australian Commonwealth supported students spending at least 50% of their clinical training at the RCS (48 students per year for three semesters, or 18 months).
This requirement created anxiety among the students, and the majority of medical students placed the RCS as their least preferred option. In 2004 and 2005, only 17 and seven students, respectively, ranked the RCS as their first option. Consequently, 31 and 41 students respectively, who had metropolitan preferences, were allocated to the RCS in 2004-2005. This 'conscription' resulted in the student body expressing significant discontent. This study explores students' reasons for clinical school preferences and their concerns regarding allocation to the RCS.
Methods
Previously published survey questions were refined by the authors through discussion and common agreement8. The study design and questionnaire were approved by UoM Human Research Ethics Committee. All medical students at UoM were invited by email to participate in an internet-based survey in late 2005. A reminder invitation was sent to the students, then in years 2 to 6 of the medical course, in early 2006. A total of 1599 students were contacted. Participants voluntarily accessed the internet-based questionnaire (Catalyst Tools; University of Washington, Seattle, WA, USA). Of 1599 students surveyed, 785 responses were received. Forty-four emails were returned as either 'address unknown' or the student was unable to be contacted, and these students were excluded from the analysis. The adjusted response rate was 51% (785 of 1555).
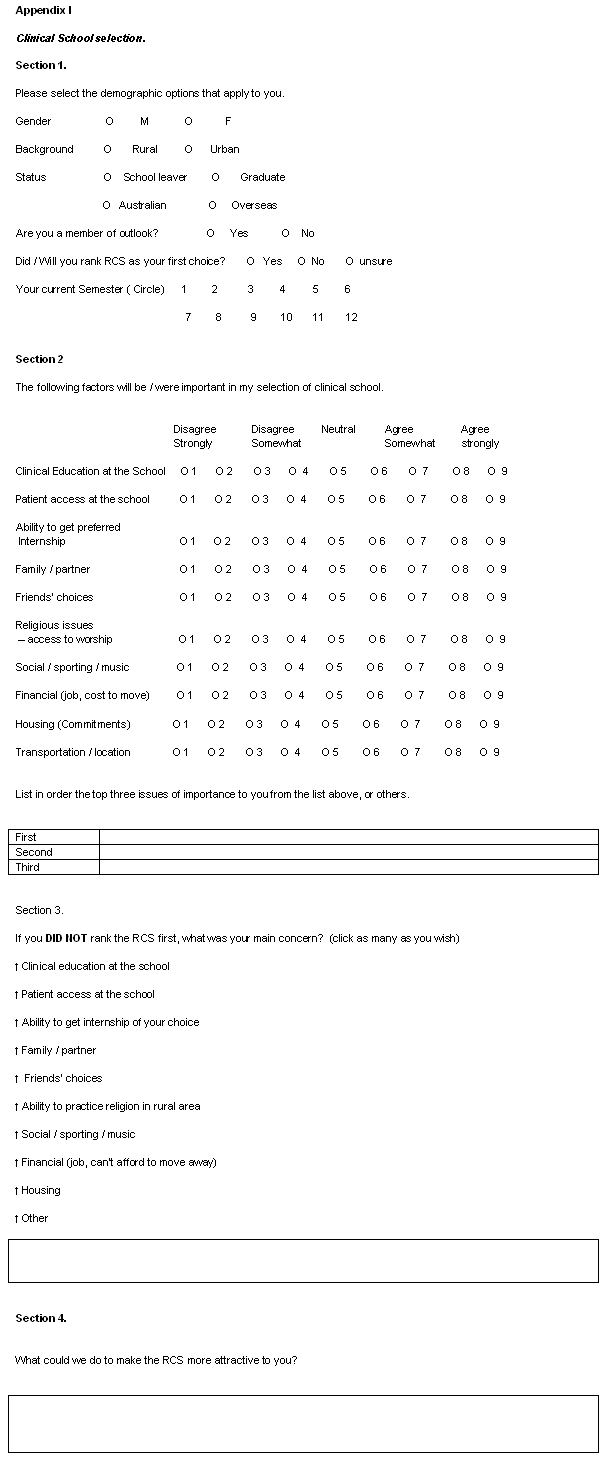
The response rate of 51% appears low, but not unusually so for an internet-based survey. Leece et al.9 and Balter et al.10 both reported response rates of 13-14% lower for internet surveys, compared with written surveys. The survey (Appendix I) focused on four areas: (i) demographic information; (ii) the factors important in the student's selection of a clinical school (Likert scale 1 [strongly disagree] to 9 [strongly agree] and ranking of the three items of greatest importance to the individual); (iii) factors important to students who did not rank the RCS as their first preference; (iv) suggested ways to make the RCS more attractive.
Data analysis
Responses were downloaded from the internet, de-identified, coded and analysed. Open-ended questions were coded and themed using standard qualitative methods 11. Statistical analysis was done using parametric statistics in SPSS (SPSS Inc; Chicago, IL, USA). Responses were cross-tabulated by gender; rural versus urban background; Australian versus international residency; school leaver or graduate entry to medical school.
Results
Of the total student cohort studied, 48% were of school-leaver entry and 20% graduate entry into the course. In addition, 32% of the cohort was of international origin. Rural-origin students, defined as those coming from towns of RRMA classification 3-7 accounted for 7% of the total cohort. This equated to 10% of the Australian students.
Of the total number of respondents, 12% (n = 785) had either chosen the RCS or indicated an intention to do so for their clinical placement. Of respondents, 28% indicated they were international students, and because the RCS is required to take only Commonwealth Supported Place (CSP) students to meet the requirement of funding, these respondents were removed from the sample, giving a percentage of CSP students preferring the RCS as 16% (n = 90 of 567 CSP students).
Table 1 shows the factors rated most important by all UoM medical students in their selection of clinical school. They were asked: 'The following factors will be/were important in my selection of clinical school'. Clearly, student perceptions relating to clinical education, transport/location and patient access had a significant influence on the students' clinical school selection.
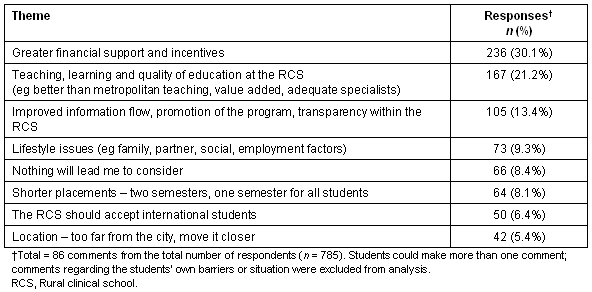
Students were asked to list the three main issues most important to students in clinical school selection. The most frequently reported issues fell into two categories, education and social (largely family/relationship), as shown (Table 2). Students who did not rank the RCS as their first choice of clinical school were asked to rank their three main concerns about the RCS. The five most common concerns are shown (Table 3). Finally, students were asked to comment on possible changes that would make the rural clinical school more attractive to the individual student (Table 4).
Table 1: Factors rated most important by all University of Melbourne medical students in their selection of clinical school
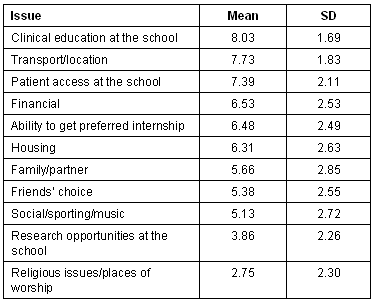
Table 2: University of Melbourne medical students' three main issues most important in clinical school selection
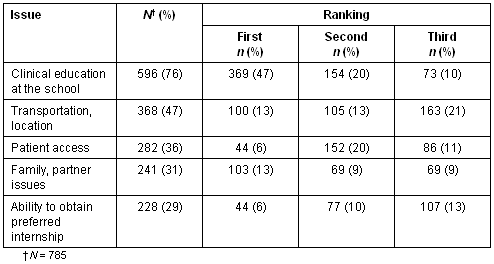
Table 3: Five most common concerns of University of Melbourne medical students' three main concerns about the rural clinical school
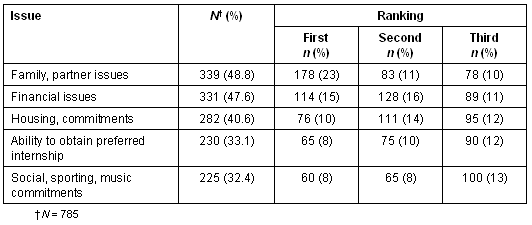
Table 4: Possible changes that would make the rural clinical school more attractive to the individual student
Discussion
In 2004 we studied the barriers reported by students who were allocated to train at UoM RCS in that year8. Although the major concern expressed by the students was a preference for training at a metropolitan clinical school, the major barriers identified were social rather than educational, in particular related to family and partner commitments, transport, and financial concerns. A significant concern was that training in a rural location would negatively impact on the student's future career, including the chance of attaining a preferred location for internship, and hence entry to their preferred specialist training program. To broaden our understanding of barriers, we designed this study to explore the concerns of the whole medical student cohort.
Issues of concern to students in clinical school selection
In the present study it was found that students were predominantly concerned about learning and experiential issues, the standard of clinical education, and patient access. The ability to obtain a preferred place of internship was also a common concern. Other issues were of a more personal nature with the location of the school, transportation, and family and partner issues rating highly.
Denz-Penhey et al reported significant levels of stress in a survey of the first cohort of RCS students in Western Australia, related to curriculum content, delivery and assessment, among other factors12. Our findings also revealed students' anxiety about academic standards, illustrating that access to patients and the ability to obtain a preferred internship were also major issues for UoM students. In addition, many students expressed concern about the lack of rural specialists to teach (Table 4). Areas of particular concern were the sub-specialties, particularly haematology, oncology, infectious diseases and neurology. These specialties are either not represented in the local specialist workforce or are provided by a visiting service, usually once a month or less. Visiting specialists generally have a heavy consulting workload in their sessions, making it extremely difficult for them to provide extra time to teach students.
Strategies to address the students' concerns regarding the lack of specialists to teach their sub-specialty areas can be satisfactorily addressed. Strategies include using generalist physicians and surgeons, GPs with particular areas of interest and expertise, and the use of video-conferencing of tutorials from metropolitan tertiary centres. We also found that good access to inpatients and out-patient clinics provides the opportunity to see and learn from a satisfactory number of patients if spread over the full year, rather than attempting to access these patients in the small time allocated to learning such specialties. We have also organized sessions in which selected patients with particular conditions are sourced from general practices for teaching purposes. This has been particularly successful in neurology.
These concerns are consistent with issues reported among students both in Australia and internationally. Silagy and Piterman13 reported on the attitudes of Australian final year medical students to the location of their postgraduate training. Most graduates preferred metropolitan internships, perceiving that they would have access to better training and educational opportunities. Orpin (Tasmania, Australia)14 and Crump (USA)15 reported similar concerns. However a study from the University of Newcastle, New South Wales, Australia16 revealed significant problems with patient access for medical students in a group of four large teaching hospitals. This differs from our students' repeated anecdotal comments about excellent access to patients in our RCS-affiliated hospitals.
There is a significant body of evidence to support the concept that training undergraduates in a rural location has a positive effect on the number of medical graduates who will eventually practice in a rural area. In addition, longer periods of training in a rural location also have a positive influence on the retention of rural medical practitioners2,6. There is also strong evidence that students of rural origin are more likely to practice in a rural area7,17. This evidence underpins the Australian Government's support and funding of RCSs as part of a wide-ranging strategy of rural incentives1.
Issues of concern to students who did not or plan to not chose the RCS
The common concerns among students who did not select the RCS were mainly of a non-clinical nature: family and partner, and financial and housing commitments, consistent with the findings of our previous study8. Almost 49% of respondents reported family and partner issues as their main issue. There are several significant contributing factors, including the large number of students of metropolitan background (75%), previous commitments to housing (mortgage, rental bonds) and employment commitments. In addition, selection for clinical schools occurs late in third year, by which time many students have established firm bonds and a base in the city.
These concerns were reflected in the responses to the question 'What changes would make the Rural Clinical School more attractive to you?' The major factors were financial support, and evidence that teaching, learning and experience at the RCS was at least equal to that in the metropolitan schools.
Student financial support at the RCS is significant. Quality, fully furnished accommodation is provided at all three RCS sites for a nominal rent of AU$40 per week. The compares very favorably with average rental prices for single bedroom accommodation in the vicinity of the metropolitan campus of $110-18018. Accommodation for compulsory weeks of learning in the metropolitan area is fully funded. Student bursaries are offered to students with demonstrated financial hardship. Resident Student Advisor positions are offered at each site. These students provide a range of contact and support services to the student accommodation. In return, their accommodation is provided rent free. Finally, transport to some more remote training locations is subsidized. Evidence from RCS students also suggests that costs of living in the RCS compares favorably with costs in the metropolitan area19.
Academic performance is of great importance to the students, and over the 4 years of the school's operation, results in assessment have been comparable with the metropolitan schools. Statistical analysis performed by the School of Medicine of the overall assessments of UoM medical students has shown no statistical difference among the four clinical schools, except for the graduating class of 2006. In this year, the mean final mark for RCS students was 74.3% compared with an overall mean of 71.8%
Conclusion
This study confirmed that the major issues of concern to UoM medical students in choosing RCSs are the quality of education and experience at the school, and social aspects related to re-location to a distant site. Although little can be done regarding family and financial issues, these remain important concerns for students when considering relocation to a RCS. In addition, academic results, quality of teaching, and ability to gain a preferred internship placement remain important concerns for students despite evidence that these are equal or better at the UoM RCS, compared with the metropolitan clinical schools.
Acknowledgements
The establishment and operation of rural clinical schools are funded by the Australian Government. The authors thank The University of Melbourne School of Medicine for providing student email contacts; Ms Lucia Rossi for managing the survey and collating responses; and the University of Washington, Seattle, USA for permitting the use of the 'Catalyst' internet program.
References
1. Australian Government, Department of Health and Ageing. Rural Clinical Schools program. (Online) 2005. Available: http://www.health.gov.au/clinicalschools (Accessed 22 May 2007).
2. Denz-Penhey H, Shannon S, Murdoch CJ, Newbury JW. Do benefits accrue for longer rotations for students at Rural Clinical Schools. Rural and Remote Health 5: 414. (Online) 2005. Available: www.rrh.org.au (Accessed 15 May 2007).
3. Rabinowitz H. Recruitment, retention and follow-up of graduates of a program to increase the number of family physicians in rural and underserved areas. New England Journal of Medicine 1993; 328: 961-963.
4. Rabinowitz HK, Diamond JJ, Markham FW, Hazelwood CE. A program to increase the number of family physicians in rural and underserved areas: impact after 22 years. JAMA 1999; 281: 255-260.
5. Smucny J, Beatty P, Grant W, Dennison T, Wolff LT. An evaluation of the rural Medical Education Program of the State University of New York Upstate Medical University, 1990-2003. Academic Medicine 2005; 80: 715-716.
6. Matsumoto M, Okayama M, Inoue K, Kajii E. Factors associated with rural doctors' intention to continue a rural career: a survey of 3072 doctors in Japan. Australian Journal of Rural Health 2005; 13: 219-225.
7. Rourke JT, Incitti F, Rourke LL, Kennard M. Relationship between practice location of Ontario family physicians and their rural background or amount of rural medical education experience. Canadian Journal of Rural Medicine 2005; 10: 231-240.
8. Jones GI, DeWitt DE, Elliott SL. Medical students' reported barriers to training at a rural clinical school. Australian Journal of Rural Health 2005; 13: 271-275.
9. Leece P, Bhandari M, Sprague S, Swiontowski MF, Schemitsch EH, Tornetta P et al. Internet versus mailed questionnaires: a randomized comparison (2). Journal of Medical Internet Research 2004; 6(3): e31.
10. Balter KA, Balter O, Fondell E, Lagerros YT. Web-based and mailed questionnaires: a comparison of response rates and compliance. Epidemiology 2005; 16: 577-579.
11. Pope C, Mays N. Rigour and qualitative research. BMJ 1995; 311: 109-110.
12. Denz-Penhey H, Murdoch C, Lockyer-Stevens V. 'What makes it really good, makes it really bad.' An exploration of early student experience in the first cohort of the Rural Clinical School in the University of Western Australia. Rural and Remote Health 4: 300. (Online) 2004. Available: www.rrh.org.au (Accessed 15 May 2007).
13. Silagy CA, Piterman L. Attitudes of senior medical students from two Australian schools towards rural training and practice. Academic Medicine 1991; 66: 417-419.
14. Orpin M, Gabriel M. Recruiting undergraduates to rural practice: what the students can tell us. Rural and Remote Health 5: 412. (Online) 2005. Available: www.rrh.org.au (Accessed 15 May 2007).
15. Crump WJ, Barnett D, Fricker S. A sense of place: rural training at a regional medical school campus. Journal of Rural Health 2004; 20: 80-84.
16. Olson LG, Hill SR, Newby DA. Barriers to student access to patients in a group of teaching hospitals. Medical Journal of Australia 2005; 183: 461-463.
17. de Vries E, Reid S. Do South African medical students of rural origin return to rural practice? South African Medical Journal 2003; 93:789-793.
18. The University of Melbourne. Costs of living at Melbourne University. (Online) no date. Available: University of Melbourne Student Services (Accessed 22 May 2007).
19. McNamara E. MSS Counterhandbook. Melbourne, Vic: University of Melbourne Medical Student Society, 2006; 40-50.
__________________