Introduction
While the number of specialist emergency physicians in Australia is increasing, most of these doctors practise in large tertiary hospitals. Australian Medical Workforce Advisory Committee (AMWAC) figures indicate that only 2.5% of emergency specialists practise in rural and regional areas where 28.7% of the population live - a lower proportion than for most other specialties1.
Most of the presentations to emergency departments (EDs) in rural and regional Australia are dealt with by doctors other than emergency specialists. The number of these 'non-specialist' practitioners in the emergency medicine (EM) workforce is largely unknown. Many are overseas trained doctors (OTDs) or short term locums recruited to 'areas of need'. The knowledge, skills, qualifications and experience of these doctors vary enormously. The loss of older, highly skilled procedural doctors from rural areas is a matter of concern in all disciplines2.
Dealing with medical emergencies is frequently identified by rural doctors as an area of concern due to low caseloads, lack of resources, lack of familiarity with current practices and lack of close support from referral hospitals3-5. Lack of confidence in dealing with emergencies is also a deterrent to young doctors taking up salaried positions in rural practices and hospitals6. A recent study into training prevocational doctors across Australia found only a minority felt adequately prepared for dealing with clinical emergencies7.
The challenge is to ensure those medical practitioners in rural and regional areas have the necessary knowledge, skills and support services to safely deliver an acceptable standard of care to the population they serve.
The aim of this study was to undertake a more detailed investigation of the non-specialist EM doctors, as well as to examine ideas and strategies to secure a more highly trained workforce.
Methods
Ethics approval
Ethics approval for this research was sought and obtained from the Human Research Ethics Committee (Tasmania) Network.
Methodology process
Postal survey of doctors: Convenience sampling was used to survey ED doctors working in hospitals in RRMA classification 3 and 4 areas of Australia8. These EDs had 10 000 to 30 000 presentations per annum. Survey forms were distributed to any doctor working in an ED - irrespective of seniority, employment status or level of training. A total of 18 questions were asked covering educational background, level of training, relevant experience, positive and negative aspects of the job, as well as plans for the future. All responses were anonymous.
Interviews with stakeholders: Semi-structured interviews were conducted with individuals and representatives of organisations identified as key persons, stake holders, or participants in the education, training and service delivery of EM in Australia, New Zealand and Canada. All interview transcripts were de-identified. Persons interviewed were specifically asked to comment on perceived difficulties in recruitment and retention, educational standards and possible solutions to workforce shortages.
Results
Postal survey of emergency department doctors
A total of 340 survey forms were distributed to 57 rural and regional hospitals, and 230 surveys were returned: a response rate of 68%.
Training and qualifications: Just over half (55%) of the respondents had received their basic training in Australia or New Zealand (Fig 1). While most of those trained overseas had completed the Australian Medical Council examination and were eligible for full registration, a significant proportion had not, and were practising with some form of limited or conditional registration.
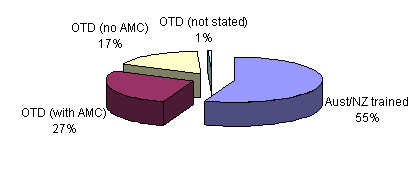
Figure 1: Respondents by eligibility for registration. OTD, overseas trained doctors; AMC, Australian Medical Council.
Just over one-third (35%) of the respondents held a 'relevant' fellowship diploma for the position occupied (Fig 2). In all, 58 doctors were Fellows of the Royal Australian College of General Practitioners (RACGP), 34 were Fellows of the Australian College of Rural and Remote Medicine (ACRRM) and only 13 were Fellows of the Australasian College for Emergency Medicine (FACEM); 21 respondents were dual or triple fellowship holders.
A slightly greater percentage of respondents (38%) were non-fellowship holders but held one or more relevant 'short course' certificates in early management of severe trauma, emergency life support, advanced paediatric life support or other similar emergency courses.
Of concern is the 27% of respondents who held no relevant fellowship nor any relevant certificate in EM. While the relevance of any particular qualification is debatable, and it can be argued that knowledge and skills can be acquired by 'on-the-job' training, the successful completion of such qualifications demonstrates a commitment to maintaining and advancing knowledge.
Of similar concern was the finding that less than half the respondents participated in any formal continuing medical education (CME) or maintenance of professional standards (MOPS) program.
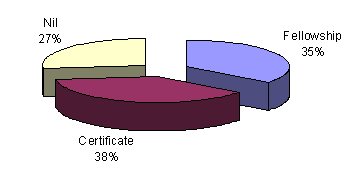
Figure 2: Respondents by postgraduate qualifications.
Previous rural experience: 23% of those surveyed had no prior rural experience before coming to their existing job (Fig 3). The figure was slightly higher for OTDs (29%) coming to work in the relatively unsupervised rural environment.
Of great interest was the finding that 39% of respondents had moved to their current position from a similar rural EM position. The high numbers suggest a significant degree of instability or dissatisfaction with many in the workforce on the move seeking a greater degree of personal and professional satisfaction.
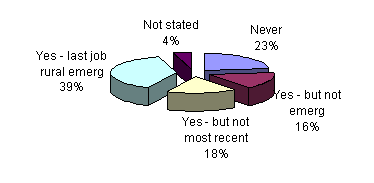
Figure 3: Respondents by previous rural experience.
Positive and negative aspects of current position: Overwhelmingly, the casemix that reflected the huge variety of clinical material seen in the ED was the most frequently rated positive feature (74%). The second most positive feature was the camaraderie of the medical and nursing colleagues in the ED (58%) - a feature perhaps more likely to be found in the close knit environment of smaller EDs.
Other issues such as pay and conditions, work environment, administrative support and hospital resources were variably rated as positive or negative features. These issues appeared to reflect more the individual hospital rather than the overall profession.
Compatibility with family life also featured as both a positive and negative factor. On the one hand, many doctors (33%) found it attractive to be able to work a predictable shift and leave the 'office' without any responsibilities until the next shift. On the other hand, 26% cited this as a negative factor due to the effect on their family of having to work unsociable hours.
There were numerous other negative factors but no one outstanding issue. Most respondents listed multiple negative aspects of the job. These included:
- medical staffing levels
- demanding work load
- excessive working hours
- difficulty accessing educational activities
- fear of litigation
- access block
- lack of peer support
Future employment and training: While one-third of respondents reported no intention to change their current situation, the majority indicated they were likely to substantially change their situation (Fig 4). For many, this included moving to another hospital or clinical area, reducing their hours of work, reducing involvement in emergency medicine, or leaving the workforce altogether. Only 6% had an intention to increase their involvement in EM. This adds further to the impression that the current workforce has a significant degree of instability and uncertainty for the future.
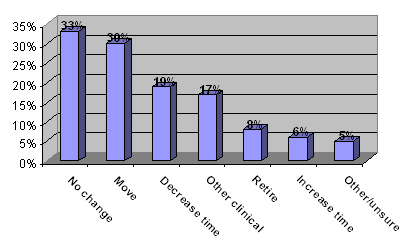
Figure 4: Respondents by future plans.
Most respondents identified a need to undertake further training in EM. Weekend 'short courses' and similar educational activities were by far the most popular intended training plans (59%). Almost certainly, this popularity reflected the small time commitment and relatively easy access to these programs. Some 20% of respondents indicated a desire to undertake a specific postgraduate diploma or certificate in EM; while 12% of respondents planned to pursue the FACEM.
Interviews and consultations
Interviews were conducted with 53 educators, administrators and employers. The majority (67%) were from Australia and the remainder from Canada and New Zealand. While 73% were clinicians, all interviewees had significant involvement in EM recruitment or education. More than half of those interviewed had worked in another country during some part of their professional career.
There were several consistent themes on workforce issues identified in these interviews:
- There is a major shortage of suitably trained and experienced doctors to meet the current needs of rural and regional EM.
- This shortage is expected to worsen in the near future.
- The heavy reliance on doctors educated in other countries creates additional problems relating to standard of training, communication, cultural issues, and resources required to support their professional development.
- There is more to recruiting and retaining than simply offering larger remuneration which may only create a more volatile workforce.
Not surprisingly, there was considerable divergence of opinion on what could or should be done to improve the situation. There were four broad, but somewhat contradictory, views expressed on future directions for the EM workforce (Fig 5):
- The more specialists view (22% of interviewees): By providing funding and expanding the number of specialist trainees, as well as making conditions more attractive for rural specialists, this will ultimately translate into a highly skilled medical workforce in the rural and regional hospitals of the same standard as major urban hospitals.
- The more general practitioners view (30%): The rural and regional workforce is the domain of generalists and there needs to be more funded GP training posts. Existing training schemes encompass EM and this is quite appropriate for most rural and regional areas together with existing short courses and locally based training.
- The imported workforce view (10%): As there will be insufficient locally trained staff for the foreseeable future, there should be aggressive recruiting from other countries with a 'fast tracking' process to expedite visas and registration for these doctors. This should be linked to an education system to bring them up to the required standard as soon as possible.
- The radical view (38%): Traditional specialist college-based education systems have failed to meet the EM workforce needs of rural and regional communities. The flow-on effect from additional undergraduate and specialist training positions is uncertain. Alternative and innovative ways of addressing the problem are a matter of urgency.
Suggested strategies included:
- expanded general practice/family medicine curricula
- university based courses
- distance education modules
- alternative pathways to specialist qualifications
- recognition of overseas EM qualifications
- expanded short course training
- further development of nurse practitioner programs, expanded-scope paramedics and other alternative forms of service delivery.
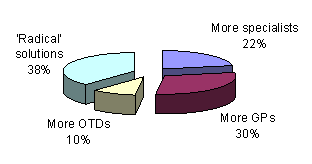
Figure 5: Suggested solutions to rural emergency medicine workforce shortages. OTDs, overseas trained doctors.
Discussion
Rural postgraduate training
Most specialist medical training takes place in tertiary hospitals that can provide the sophisticated support services as well as the necessary 'critical mass' of population to sustain professional interest. It is debatable if rural areas can provide the high standard of training that is relevant for specialist practice9,10. Eley and Barker sounded a note of caution on apparent declining interest by some rural medical graduates in taking up intern positions at their training hospitals despite very positive undergraduate experiences. Major areas of concern included 'unsupportive workplace environment' and 'inadequate professional development opportunities'. They also speculated that a relative lack of specialist training opportunities may be affecting internship choice11. Postgraduate medical education is complex with multiple organisations including specialist colleges, universities, state and national health departments, local health authorities, and postgraduate medical councils all playing variable roles in teaching, accreditation, funding and recognition.
In its report issued in December 2005, the Australian Productivity Commission noted that medical shortages remain despite a growing workforce and increasing numbers of OTDs12. The maldistribution between urban and rural areas was significant. The Commission also noted that there is limited clinical training capacity that is restricting the expansion of many professions, and a lack of coordination between education, training places and service delivery requirements. Among a number of recommendations, the Commission supported a strong focus on education and training opportunities in rural and remote areas.
The Australasian College for Emergency Medicine (ACEM) has a position paper on rural EM that acknowledges the role of non-fellows13. To date, ACEM has not become involved in the issue of training non-specialist EM doctors, although non-specialists are able to enrol in ACEM's Maintenance of Professional Standards Program. The fellowship programs of the RACGP and ACRRM are constrained by the need to encompass the entire range of generalist practice, although both allow for 'advanced skills' training in specialist areas including EM.
International practice
Rural and regional New Zealand is in a similar situation to Australia where most EM services are provided by non-specialist doctors. The University of Auckland offers a Postgraduate Diploma in Community Emergency Medicine by distance learning14. The Division of General Practice and Primary Health Care within the Auckland University, also offers an 'Accident and Medical Care' course which is aimed at non-specialist practitioners. This has been developed in conjunction with the New Zealand Accident and Medical Practitioners Association15.
In Canada, the Royal College of Physicians awards a specialist fellowship in EM. Parallel to this, the Canadian College of Family Physicians awards a Certificate of special competency in EM (CCFP-EM) requiring an additional 12 months of EM beyond the usual 2 year family medicine training. Very few specialist emergency physicians practise in rural Canada16. Many more Canadian emergency physicians have obtained their qualifications via the family medicine pathway (1555 physicians over 22 years) than the specialist track (468 physicians over 20 years)17. Most CCFP-EM graduates end up practising purely EM rather than a blend of general practice and EM18.
Role of other health professionals
The Productivity Commission report also recommended that other health professionals should have an expanded role in providing services that have traditionally been provided by the medical profession12. In Australia, emergency nurse practitioners (ENP) now exist in some major metropolitan hospitals. To date, ENPs have largely been tasked with seeing and treating patients with minor complaints, with evidence suggesting they are as good as, if not better than junior doctors19,20. In remote communities, nurses have traditionally had an expanded scope of practice that recognises the need to provide a diverse range of services without immediate medical support. Similarly, rural paramedics are seeking to extend their scope of practice beyond that of their urban colleagues21. These concepts have not been enthusiastically embraced by long-established medical organisations.
Conclusions
Emergency medicine remains a popular career choice for postgraduate training. The excitement, challenge and variety of clinical work have strong appeal. The opportunity to undertake training part time and practise part time makes EM a career more compatible with family life than many other medical pathways.
A significant difficulty appears to be maintaining enthusiasm and interest in those attracted to rural practice in the first place. The apparent instability in the workforce and the large number of negative issues raised in the workforce survey suggest that much more needs to be done as part of ensuring a viable career structure for rural EM doctors. Recurring themes of remuneration, workforce shortages, family needs, after hours and on call commitments, and access to training and professional development, are widespread in all rural health disciplines.
For many people, the short term solution of using increasing numbers of OTDs from developing countries raises moral and ethical questions as the supply from other affluent 'western' countries dries up.
The workforce survey revealed a high level of perceived need to undertake further training in EM. It is apparent that there is a degree of professional jealousy and disagreement between the various players in medical education and service delivery. Careful consideration must be given to the implementation of any new training program to ensure it fills a need and complements existing educational opportunities.
Nurse practitioners and other service providers are likely to play a greater role but it remains to be seen if such health professionals could fill the gap between acute primary care and specialist EM practice. The 'non-specialist' EM pathways that have been developed in New Zealand and Canada may be useful models for the needs of rural and regional Australia.
Recommendations
- A specific Australian postgraduate qualification in EM should be developed that meets the needs of doctors who wish to practise outside major city institutions.
- The delivery of teaching and clinical experience for such a qualification would, as far as possible, be located in those institutions and communities that already have a strong rural/regional focus and commitment to medical education.
- Such a qualification should be recognised as a legitimate career path of higher training within the field of EM and be rewarded with competitive remuneration and employment conditions to ensure it remains an attractive option for EM practitioners.
References
1. Australian Medical Workforce Advisory Committee. The medical workforce in rural and remote Australia, AMWAC report 1996.8. Sydney: AMWAC, 1996.
2. Australian Institute of Health and Welfare. Medical labour force 2004, National health labour force series no.38. Cat no. HWL39. Canberra: AIHW, 2006.
3. Tolhurst HM, Dickinson JM, Ireland MC. Severe emergencies in rural general practice. Australian Journal of Rural Health 1994; 3: 25-33.
4. Tolhurst HM, McMillan J, McInerney J, Bernasconi J. The emergency medicine training needs of rural general practitioners. Australian Journal of Rural Health 1999; 7: 90-96.
5. Dick M, Schluter P, Johnston C, Coulthard M. GP's perceived competence and comfort in managing medical emergencies in southeast Queensland. Australian Family Physician 2002; 31: 870-875.
6. Gillies J, Lionis C, MacDonald J, Laird C, Szabo J, Nunes B et al. Dealing with emergencies in rural areas of Europe. In: Proceedings, WONCA Europe 2000. Emergency Medicine Journal 2001; 18: 305-307.
7. Dent A, Crotty B, Cuddihy H, Duns G, Benjamin J, Jordon C et al. Learning opportunities for Australian prevocational hospital doctors: exposure, perceived quality and desired methods of learning. Medical Journal of Australia 2006; 184: 436-440.
8. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remoteness classifications, AIHW cat. no. PHE 53. Canberra: AIHW, 2004.
9. Wearne S, Wakerman J. Training our future medical workforce. Medical Journal of Australia 2004; 180: 101-102.
10. Reid S. Training our future rural medical workforce. Medical Journal of Australia 2004; 180: 651.
11. Eley D, Baker P. Does recruitment lead to retention? Rural clinical school training experiences and subsequent intern choices. Rural and Remote Health 6: 511. (Online) 2006. Available: http://rrh.org.au (Accessed 28 March 2007).
12. Productivity Commission. Australia's Health Workforce. Canberra: Productivity Commission, 2005.
13. Australasian College for Emergency Medicine. Position statement on rural emergency medicine. Melbourne: ACEM, 2002.
14. University of Auckland. Postgraduate Diploma in Community Medicine. Auckland: Faculty of Medical and Health Sciences. (Online) no date. Available: http://www.health.auckland.ac.nz/postgrad/programmes/PGDipComEmMed.pdf Accessed 28 March 2007).
15. Accident and Medical Practitioners Association. Accident and Medical Care Course. Auckland: University of Auckland/Accident and Medical Practitioners Association, 2004.
16. Canadian Association of Emergency Physicians. Recommendations for the management of rural, remote and isolated emergency health care facilities in Canada. Ottawa: CAEP, 1997.
17. Canadian Association of Emergency Physicians The supply of emergency physicians in Canada: laying the foundations for systematic study of the emergency physician workforce. Ottawa: CAEP, 2003.
18. Shepherd L, Burden J. A survey of one CCFP-EM program's graduates: their background, intended type of practice and actual practice. Canadian Journal of Emergency Medicine 2005; 7: 315-320.
19. Sakr M, Angus J, Perrin J, Nixon C, Nicholl J, Wardrope J. Care of minor injuries by emergency nurse practitioners or junior doctors: a randomised controlled trial. Lancet 1999; 354 (9187): 1321-1326.
20. Considine J, Martin R, DeVilliers S, Winter C, Jenkins J. Emergency nurse practitioner care and emergency department patient flow: case-control study. Emergency Medicine Australasia 2006; 18: 385-390.
21. O'Meara P, Kendall D, Kendall L. Working together for a sustainable urgent care system: a case study from south eastern Australia. Rural and Remote Health 4: 312. (Online) 2004. Available: http://rrh.org.au (Accessed 28 March 2007).


