Introduction
In Australia there is a current medical workforce shortage1, a 'crisis' more acute in rural areas and, particularly, in general practice2. There have been several strategies aimed at improving recruitment and retention of GPs in rural areas, generally directed at smaller and more remote rural communities categorized as RRMA 4-73. The Rural Remote and Metropolitan Area (RRMA) classification simply denotes population size and remoteness, and is graded from RRMA 1 (capital city) to RRMA 7 (remote area). The RRMA classification system has been used to determine Commonwealth Government funding and location incentives. However, shortages of GPs continue to be identified in the larger RRMA 3 rural communities, with a population of over 25 000, including Tamworth, a regional centre of approximately 42 000 in the northwest of New South Wales (NSW). In recent years this region has had very poor GP access, with an average of over 2000 patients per full time GP, compared with the NSW state average of 11334,5. Furthermore, a decline in GP numbers had been evident for a decade, with anecdotal evidence of no new GPs joining the workforce in the 4 years prior to 2005. It was not unusual for all Tamworth GPs to 'close their books' to new patients, and for existing patients to wait for periods of up to 6 weeks for a standard GP appointment (NSW Rural Doctor's Network, Pers. comm., February 2005).
Key to the understanding of rural workforce is the perceptions of the GPs themselves. While much has been written about barriers and enablers to rural practice, there is less literature on GP perceptions of changing workforce needs. The timing of this study relates to the development of a number of workforce initiatives in Tamworth following a period of workforce decline. This provided an opportunity to track GP perceptions before and after some of these workforce changes were implemented. This article compares GP perceptions of workforce shortage in Tamworth with concurrent levels of workforce participation in the period 2005-2006.
In 2004 the University of Newcastle's University Department of Rural Health (UDRH) Northern NSW6 received additional capacity building funding through the Primary Health Care Research, and Evaluation Development (PHCRED)7 program enabling the appointment of a GP academic. Through a strategic partnership with the local North West Slopes Division of General Practice, the PHCRED team undertook a process evaluation of a newly established managed practice (Peel Health Care) and conducted surveys of local GPs prior to the practice opening and 12 months later.
Method
General practitioners practising in the Tamworth post code of 2340 were identified through the North West Slopes Division of General Practice database and invited to participate in a survey. The survey utilized semi-structured closed- and open-ended questions to obtain information about each GP's work location, the number of sessions he or she was working, their perceptions of the local workforce situation, and if they were taking on new patients or, if not, why not? Survey questions were delivered in face-to-face interviews by the chief investigator. Interviews lasted up to 30 min and were all conducted in GPs' surgeries. The rationale for an interview approach was to increase the participation rate from that likely to have been achieved by a postal survey. Initial interviews were conducted in June 2005 with follow-up interviews in May 2006. Interviews were taped and later transcribed for analysis. This study only reports the quantitative data related to local workforce issues.
The GP workforce participation was calculated from the number of 'sessions' spent consulting. A session was defined as 2.5 to 4 hours of clinical time with a maximum of 10 sessions each week with the full time equivalent (FTE) defined as 8 or more sessions each week8. Participating GPs were asked to estimate local GP workforce shortage as being either nil, less than 4 FTE, between 4 and 9 FTE or greater than 10 FTE GPs.
The difference across time between the two sets of data was tested by means of a two-tailed Fisher's exact test9. Only data from the GPs interviewed in the 2005 cohort was used for comparative analysis. Additional data on numbers of consulting sessions and acceptance of new patients was independently obtained for GPs who had commenced work in Tamworth during the 12 month study period. The study had ethics approval from the University of Newcastle Human Research Ethics Committee, with all participating subjects giving informed consent.
Results
Ninety-four percent (31 of 33) of Tamworth GPs participated in the initial survey in May 2005. By the time of the follow-up survey in June 2006, two GPs had left the area but the remaining cohort of 29 GPs all participated.
The GPs worked in 12 group or solo practices in Tamworth, none of which were accepting new patients in May 2005. Reasons given for this were long waiting times for existing patients and overworked staff. The GPs reported that practice reception staff at the front desk often bore the brunt of patient anger over lack of access. General practitioners' estimates of the local GP workforce shortage are shown (Table 1). All practitioners initially interviewed believed there was a workforce shortage. This shortage was perceived to be greater than 10 FTE GPs by 6.5% of surveyed GPs, while 64.5% perceived the shortage was between 5-9 FTE GPs and 29% as 1-4 FTE GPs.
Table 1: Perceived GP workforce shortage in Tamworth during 2005-2006
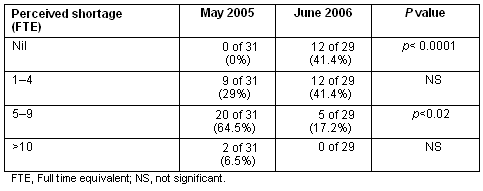
The local GP workforce increased from 27.8 to 31.5 FTE in the 12 month study period. Between surveys, six new GPs commenced practice and two left practice in Tamworth. Of the six new arrivals, three had relocated from metropolitan areas, one had relocated from a smaller rural town, one had returned to work following maternity leave and one doctor decided to move from hospital-based practice to general practice. During the study period five new practices were established in Tamworth, including the managed practice, two sole-GP practices, a group practice and an Aboriginal medical service.
In the follow-up survey 41.4% perceived the shortage as 1-4 FTE GPs (p = 0.02), 17.2% between 5-9 FTE GPs and 41.4% nil shortage. No GPs in the follow-up survey perceived the shortage as greater than 10. By June 2006, however, there was a considerable improvement in patient access with 47% (8 of 17) practices accepting new patients.
Discussion
This small localised study provides an interesting snapshot of change in a RRMA 3 rural GP workforce. The study was performed at a time when a number of new workforce initiatives were focused in the area following a period of GP workforce decline over the previous 10 years. Overall, there was a net gain in the local GP workforce of 12%. What was an interesting finding, however, was that GP perceptions of workforce shortage were sensitive to improvements in local FTE numbers and moved in line with the changed availability of services. In addition, many GPs in this rural centre seemed relatively satisfied with a GP workforce that had a higher GP : patient ratio than that in metropolitan areas. This may be because of differences in practice styles, patient expectations and practice nurse involvement.
This small increase in local workforce should, however, be discussed in the light of projections made by Joyce et al.2 for the medical workforce in the coming decade and, thus, the likely supply factors. Her work is based on assumptions that include natural attrition, shifts to non-clinical work and reduced average hours worked per practitioner. Overall it is estimated that without any new recruitment, the Australian medical workforce is expected to contract by 5-10% each year2. It remains to be seen whether government training initiatives in rural areas, such as rural clinical schools6, UDRH6, and regional GP training will adequately facilitate the necessary new recruitment.
It is difficult to predict what future medical workforce needs for a community might be due to variations in the supply of practitioners relative to population size. Thus, compared with Sydney where there are as few as 700 residents per GP, Tamworth estimates ranged between 1500 and 2000 residents per full time GP in 20054. For Tamworth to reach the NSW average of 1133 patients per practising GP, there would need to be recruitment of a further 7.7 GPs, based on 2001 census data10. Whereas, to reach comparative population : practitioner ratios as seen in metropolitan centres would require the number of GPs working in Tamworth to double. The growth of the local GP workforce in 2005/2006 was 3.7 FTE, and although short of reaching the population/practitioner state average by 4.0 FTE GPs, it was enough for 40% of GPs to perceive that the shortage had been ameliorated.
There are several factors that may have contributed to this small increase of 12% in the local GP workforce, and the subsequent improvement in access with 50% of practices ready to accept new patients in June 2006. During the study period a surprising number of new practices commenced, including several sole practices that were all actively building up their patient base. Also, in Tamworth there are a significant number of patients who are privately billed for their GP consultations. Like any commodity, consumption of medical services (as opposed to demand) is affected by cost. Private billing, which is known to be more prevalent in rural areas, may have a further reduction effect on the demand for GP services.
Furthermore, an increasing role for practice nurses in Australian general practices and their capacity to increase the scope of care and improve the efficiency of existing GPs may also be beginning to have some impact. For instance, 12 of 17 practices in Tamworth are now utilising practice nurses, with some having very substantial practice nurse to GP ratios. Practice nurses will need to be considered in future attempts to forecast the GP and primary health workforce in Australia.
There are a number of limitations of this study. The chief investigator was a local GP, which ensured a high participation rate but also introduced inherent bias. There was no measurement of concurrent changes in the practice nurse workforce in Tamworth and, finally, the study timeframe proved to be too short. Further monitoring of this local workforce is planned to better understand the perceptions of GPs and the impact of workforce changes over time.
Conclusions
In this study GP perceptions of local workforce shortage were consistent with the changes in local workforce numbers. While the reasons for these changes can only be speculated on, GPs certainly had their fingers on the pulse of change in this community. The establishment of a new managed practice and the changing practice models in rural areas are likely to have contributed positively. However, with six new GPs commencing work in the postcode area, clearly there are other factors involved. Questions remain as to whether it is possible to use GP perceptions to predict at what point the ratio of GPs to patients would lead to satisfied demand for primary healthcare services. Knowing the answer to this question would allow rural communities to better plan how many doctors would be required in the future.
Acknowledgments
The authors would like to acknowledge the time and effort contributed by all the GPs involved, and the Department of Health and Aging Research Capacity Building Initiative funding through the PHCRED program.
References
1. Australian Health Workforce Advisory Committee 2003-2004. Annual Report 2003-2004. AHWAC report 2004.3. Available: http://www.health.nsw.gov.au/amwac/reports.html (Accessed 1 August 2006).
2. Joyce CM, McNeil JJ, Stoelwinder JU. More Doctors, but not enough: Australian medical workforce supply 2001-2012. Medical Journal of Australia 2006: 184: 441-446.
3. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remoteness classifications. AIHW cat. No. PHE 53. Canberra, ACT: AIHW, 2004.
4. Wilkinson D. Inequitable distribution of general practitioners in Australia: analysis by state and territory using census data. Australian Journal of Rural Health 2000; 8: 87-93.
5. May J, Morrissey M, Cooper R, Kershaw G. Supporting the rural GP workforce: impact of a managed care practice. In, Proceedings, General Practice & Primary Health Care Conference; 5-7July 2006; Perth, WA; 2006.
6. Lawson KA, Chew M, Van der Weyden MB. A revolution in rural and remote Australia: bringing health education to the bush. Medical Journal of Australia 2000; 173: 618-624.
7. Primary Health Care Research and Information Service. The PHCRED Strategy. (Online) 2006. Available: http://www.phcris.org.au/phcred/ (Accessed 1 August 2006).
8. Quality in Practice/Australian General Practice Accreditation Ltd. Rates. Available: http://www.qip.com.au/accreditation.asp?acrid=4&ratespool=1 (Accessed 1 August 2006).
9. Sprent P. Applied nonparametric statistical methods. London: Chapman and Hall, 1989; 113-122.
10. Australian Bureau of Statistics. Person Characteristics in Postal Region 2340, 2001 Census. (Online) 2007. Available: http://www.censusdata.abs.gov.au/ABSNavigation/prenav/ViewData?&action=404&documentproductno=POC2340&documenttype=Details&tabname=Details&areacode=POC2340&issue=2001&producttype=Community%20Profiles&&producttype=Community%20Profiles&javascript=true&textversion=false&navmapdisplayed=true&breadcrumb=LPD&#Usual%20Residents%20Profile (Accessed 1 September 2006).
Abstract
Introduction:
Currently Australia is experiencing a rural medical workforce shortage, especially among GPs. Strategies aimed at improving this shortage have generally been directed at small and remote rural communities (RRMA 4-7); however, longstanding GP shortages also continue in large (RRMA 3) rural communities. The key to the understanding the rural workforce is the perceptions of GPs themselves. This article compared GP perceptions of workforce shortages in Tamworth, New South Wales, Australia (an RRMA 3 town) with actual levels of workforce participation.Methods: A survey of 31/33 GPs working in the New South Wales town of Tamworth was conducted in 2005. Participating GPs were individually interviewed and were asked to estimate local GP workforce needs, calculate their weekly consulting time sessions and advise if they were accepting new patients. The survey was repeated 12 months later with the same cohort to track workforce change.
Results: In May 2005 there were 27.8 full time equivalent (FTE) GPs working in Tamworth (population 42 000). In May 2006 this had risen to 31.5 FTE practitioners. Initially, all practitioners surveyed believed there was a workforce shortage, with no practice accepting new patients. This shortage was perceived to be >10 FTE GPs (6.5%), between 5-9 GPs (64.5%) and between 1-4 GPs by 29% of surveyed GPs. In June 2006 there were 31.5 FTE GPs working in Tamworth. The follow-up survey of 29 GPs revealed a significant shift in their perceptions with only 41.4% of GPs perceiving the shortage as 1-4 FTE GPs (p = 0.2), 17.2% between 5-9 GPs and 41.4% nil. No GPs in the follow-up survey perceived the shortage as >10. At the end of the 12 month study period, 8 of 17 practices were accepting new patients.
Conclusions: GP perceptions of shortage largely reflected concurrent workforce changes that occurred during the study period where there was a 12% improvement after a prolonged period of workforce stagnation. This change drove improvements in patient access and in many GPs' minds ameliorated much of the perceived shortage. Many factors may be involved, including the increased use of practice nurses, private billing and start-up capacity. General practitioner perceptions appear to be sensitive to workforce changes, with sampled GPs working with higher patient ratios than those seen as acceptable in metropolitan areas.
Key words: general practitioner, workforce.
You might also be interested in:
2015 - Measuring organisational-level Aboriginal cultural climate to tailor cultural safety strategies



