Introduction
Attending to the critical shortage and sustainability of health care professionals and resources in rural areas in Australia is a continuing challenge. In response, there is a heightened focus on new models of healthcare delivery and collaboration that optimise the quality of patient care, respond to complex health needs and increase professional job satisfaction. The incorporation of interprofessional rural health education within universities has been proposed as a key way of addressing these challenges both internationally and within Australia1-8.
Interprofessional education (IPE) is currently defined as occurring 'when two or more professions learn with, from and about each other to improve collaboration and the quality of care'9. It is argued that 'there is a strong theoretical base to support the implementation of IPE'6 in the training and educational pathways of all health professionals. Exposing students to effective IPE programs throughout their curriculum has been shown to have a number of positive outcomes5,7,10,11. These outcomes include an increase in mutual understanding of the roles and values of other health professionals, raised awareness of the importance of collaborative and team working skills, enhanced communication and improved patient care and outcomes5,7,10,11. The development and implementation of IPE strategies has been claimed to prepare future health professionals for 'real' practice and collaboration. However there is as yet 'only limited evidence of success'6,12 in measuring the long term effects of IPE on professional practice and collaboration.
The tertiary education of health professionals provides a key opportunity for universities to develop and promote consistent opportunities for IPE that prepare health science students for future practice. Effective IPE programs must therefore reflect the changing nature of healthcare provision and collaboration by using, for example, interactive and problem-based authentic learning environments2 that promote group work, reflection and mentorship1. These strategies facilitate one of the key aims of IPE by providing students with the opportunity to 'learn with, from and about one another'2, whereby students are able to 'investigate their professional roles and determine the boundaries between them'13-14.
The contextual setting of interprofessional health education has also been identified as a critical component of its effectiveness5-6,15-18. The implementation of interprofessional health education in rural areas has been argued to be beneficial for two key reasons. First, rural communities are argued to provide 'an ideal context in which learners can observe and participate in sound interprofessional clinical practices'6 by exposing students to the necessity of collaborative practice and expertise4,8. Facilitating students to experience the opportunities and challenges of rural healthcare is thus an effective context for interprofessional education, where disciplines 'must learn to collaborate with others to solve problems beyond their immediate scopes of practice and expertise'7. Second, there is acknowledgement that educating health professionals within a rural environment is an effective strategy for increasing health professional knowledge and experience of working or living in a rural environment7. The ultimate outcome of this strategy is potentially the recruitment and retention of health professionals in rural and remote areas internationally and also within Australia. Within the state of Tasmania, the provision of rural education opportunities is particularly critical to health workforce strategies, given the geographical classification of much of the state as rural or remote.
Method and Implementation
If health care workers are expected to work together and share expertise in a team environment, it makes sense that their education and training should prepare them for this type of working environment19.
An interprofessional development team within the University of Tasmania's Faculty of Health Science, led by the University Department of Rural Health, collaborated in designing the RIPPER (Rural Interprofessional Program Education Retreat) project. The initial objective of RIPPER was to develop a rural interprofessional learning module for final year undergraduate health science students at the University of Tasmania. The aims of the RIPPER project were:
- To foster and facilitate positive and productive inter-professional learning experiences for final year undergraduate health science students.
- To allow students to gain an understanding of the importance of an inter-professional and team approach to delivering health care to people living in both urban and rural areas.
- To encourage students to consider rural practice as a future career.
A rural community in North East Tasmania was chosen to be the one in which the RIPPER project would be implemented. Approximately 60 undergraduate students from the disciplines of medicine, nursing and pharmacy volunteered to participate in the program over two weekends in 2006 and 2007.
The format and educational design of the RIPPER initiative was focussed on a multi-station circuit that consisted of three learning stations. Each learning station was based on an interprofessional rural case-based scenario that employed experiential and interactive educational strategies. One station utilised high fidelity simulation using a resuscitation manikin, while the others focussed on low fidelity simulation and role play. Each learning station required students to work collaboratively in small clinically relevant6 interprofessional teams that engaged the skills and knowledge of each profession. Each team was required to attend to and interact with the immediate management of the emergency health scenario, to consider strategies for prevention and patient aftercare, and ultimately to develop best practice management algorithms. Table 1 provides an overview of the three scenarios and their key learning outcomes.
A key part of building students' skills and knowledge was the running of each scenario in two iterations. At the commencement of each scenario, each interprofessional student group was divided into two smaller teams. The first team were provided with minimal briefing and were then required to interact with the scenario while the second team observed. Students and facilitators then reflected on and evaluated the performance of this first iteration of the scenario. The scenario was then re-run with the second student group, who were expected to draw on their discussion, reflection and evaluation from the first iteration. At the conclusion of both iterations, the larger group were bought back together to reflect on best-practice management for the particular health scenario, including consideration of prevention and aftercare. Table 2 provides an overview of the structure of the RIPPER program.
Table 1: Overview of RIPPER learning objectives, learning outcomes and scenarios
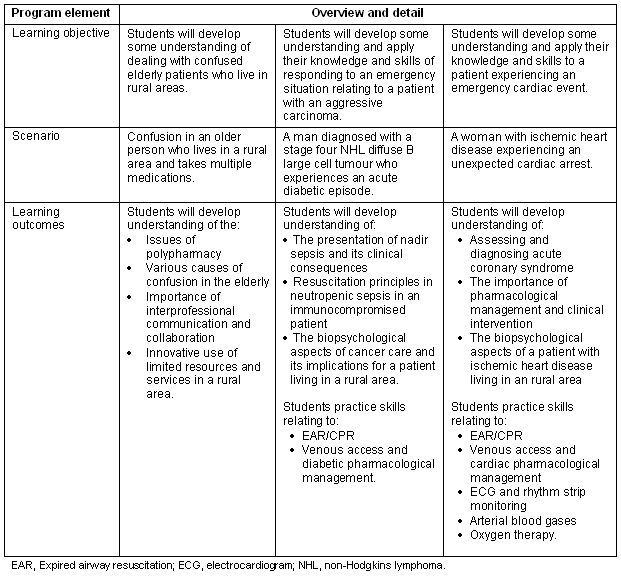
Table 2: Structure of the RIPPER pilot

The use of clinically focussed learning scenarios within a rural community setting aimed to promote not only an engaging approach to collaborative practice, but also the opportunity to profile the capabilities of rural health care providers. The program involved University of Tasmania health academics, and health professionals from the regional hospital and the local community and hospital. Their backgrounds included expertise in the areas of rural health, clinical education, emergency medicine, nursing and midwifery, aged care, pharmacy and community practice. These health professionals and educators provided mentorship for students and facilitation of the learning sessions. This enabled the sharing of skills and knowledge between students and health professionals.
Evaluation
In evaluating the RIPPER project a pre and post quasi-experimental design method was utilised. Two questionnaires were distributed before and after the event. This evaluative approach is argued to assist in detecting 'changes resulting from an interprofessional course more accurately as there is data collection at two points in time: before and after the course'20. The questionnaire was designed using open- and closed-ended questions to gather both quantitative and qualitative data. These data were used to measure students' perceptions of interprofessional learning and practice, and the degree to which the aims and learning outcomes of the program were met.
Quantitative data were collected from a 13 item questionnaire using a 5 point Likert scale ranging from 'strongly agree' to 'strongly disagree'. The questions aimed to measure students' attitudes to shared learning and teamwork; perceptions of other healthcare professionals including roles and responsibilities; understandings of collaboration and teamwork; and intention and likelihood of practising in a rural community.
Qualitative data were also collected on 8 items. Students were asked to define their understanding of interprofessional practice and the roles and responsibilities of respective health professionals before and after the program. Students were also asked to detail their learning expectations before the program; in the post-evaluation they were asked if these expectations were met.
Focus group interviews were used as an additional qualitative method for evaluating students' perceptions of the design and relevance of the program. The sessions were led by an independent facilitator, with full consent granted for interviews with each student. Informal group discussions with local health professionals and academics involved in facilitating the program were also undertaken immediately after the completion of the program. All qualitative data were recorded using notes and audio-recordings and transcribed. A thematic analysis was undertaken to interpret the qualitative data.
Thematic analysis is part of an interpretive method that examines and seeks to explain the meanings that emerge from qualitative data, such as the transcripts of focus groups, interviews and surveys21-23. The process of thematic analysis includes identifying emerging issues and categorising them into themes. For example, the analysis of the RIPPER focus groups and surveys focussed on what was said by students in the surveys and focus groups, similarities and differences between perceptions and statements, and the professional context in which the students spoke.
Results and Discussion
In total, 59 students from the disciplines of medicine, nursing and pharmacy participated in RIPPER over the first and second iterations of the project. In evaluating the program, 58 pre- (98% response rate) and 57 post-surveys (96% response rate) were completed by participating students. The collection of qualitative and quantitative evaluation data allowed an integrated analysis of the themes and issues that were raised by students and staff who participated in the program24. The following section provides a brief synopsis of the key themes and results of this evaluation.
Understandings of 'interprofessional practice'
A key aim of the RIPPER program was to increase students' understanding of interprofessional practice and the importance of a team approach to rural healthcare.
In both iterations of the program, the pre-questionnaires indicated that students' interpretations of interprofessional practice most commonly included themes of 'using professional skills and knowledge' and 'collaboration'. The post-evaluations in both program iterations showed significant shifts in how students' conceptualised and defined interprofessional practice. As Table 3 demonstrates, one of the most significant examples from the 2006 program was the students' increased recognition of 'patient outcomes' as a key focus of interprofessional practice.
Table 3: Summary of understanding of 'interprofessional practice' pre- and post-workshop 2006 (multiple categorisations using χ-squared tests where p <.05)
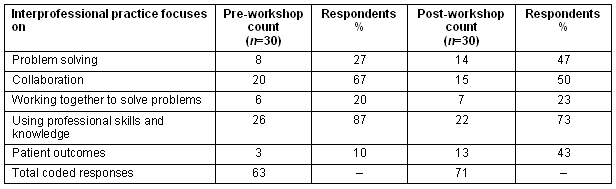
This increased focus indicates that students ascribed greater value to interprofessional teamwork and collaboration as a way of optimising the quality of patient care. The following comments by three students highlight this view:
Utilising the strengths of each team to achieve best patient results.
Better appreciation of how a team can effectively work together for a patient even they aren't familiar with each other.
[Have learnt] we all have significant roles that are interconnected for optimum patient outcomes.
In respect to students' understanding of rural interprofessional practice, the post-surveys showed that students recognised the importance of 'working together' and 'problem solving' as a key component of interprofessional practice in a rural setting. The following quotes demonstrate the ways in which RIPPER helped students to increase their understanding of this team approach to rural healthcare.
Fantastic weekend, very important to work as a team and see how that works in rural health.
Better understanding of rural health care and issues.
I've got more of an idea what it's like to work in rural.
Professional roles and responsibilities
Another key component of how students understood and valued interprofessional practice was associated with their perceptions of professional roles and responsibilities. Students were asked to describe their perceptions about the professional role of doctors, nurses and pharmacists before and after the workshop. In both survey evaluations the majority of respondents identified more traditional, preconceived aspects of other health professionals. For example, students described pharmacists as providers of 'medication advice', nurses as providers of 'patient care' and 'assessment and diagnostics' as the focus of the role of doctors.
In the post-workshop questionnaire, a number of comments illustrated a broader understanding among students of their own professional role in their own discipline, as well as the respective roles of other disciplines. This shift can be viewed as indicative of students positively learning together1,25. The evaluation revealed that RIPPER provided students with an opportunity to challenge and redefine their professional boundaries (including skills) in a setting that mirrored an authentic practice environment. The following quotes exemplify how the program facilitated students to 'learn with, from and about one another'2.
I enjoyed the opportunity to learn and work with nursing and pharmacy students; we've never really done this in our six years of uni before.
I now see that we all have significant roles in patient care, doctors aren't the only ones treating diagnosing...
I now know more about what the other professionals do, helpful for next year when I'm 'out there' doing this stuff in practice.
Will feel more comfortable working alongside doctors and nurses in the future.
Program design
The evaluation gathered information concerning the design and content of the program. Approximately 70% of students (n = 41) specifically identified the interactive and authentic case-based learning environment of RIPPER as one of the most positive aspects. Students most commonly commented on the 'real' and 'authentic' nature of the learning environment. The use of role play and high fidelity simulation as a way of utilising and improving students' skills and knowledge was identified as one of the most liked parts of the program. The following quotes demonstrate this.
It simulated real life.
It was confronting but the role plays were a great way of learning...
Having practical experience to work collaboratively...the CPR session was particularly useful.
I didn't expect to be challenged, it was a useful experience.
A small group of students (n = 5) identified that they were uncomfortable with the use of experiential learning techniques such as role play. This response was most common to pharmacy students, and may have been attributable to the limited nature of interactive case-based learning in their undergraduate program. It may also reflect language barriers, for example a number of the students were international students with English as their second language. Students also identified the supportive learning environment as one of the most positive parts of their experience. Over 80% of students (n = 48) specifically noted themes associated with mentorship, guidance and support from facilitating health professionals and academic staff as beneficial to their learning experience. Comments included:
Good scenarios and great support from clinicians, teaching staff throughout.
Excellent staff resources and support.
Students were asked to provide feedback in the post-workshop survey about the most liked and disliked aspects of RIPPER. General feedback associated with the design of and suggestions for future improvement to the course included the desire by students for more learning stations and scenarios.
I felt some of the activities could have been condensed into a shorter time period which could have furthered other learning opportunities.
I think there was too much reflection, we could have done another scenario instead.
More scenarios please!
Students further relayed their desire for more rural IPE within their undergraduate training. This is a key point raised within the literature6 relating to the effectiveness of interprofessional learning and training opportunities being strengthened by the 'vertical integration'6 of these activities in the university curriculum. Examples of students' comments included:
Invaluable, we need more scenarios and interdisciplinary training throughout our degree.
Good to have before making the transition to a health profession.
Should be more things like this in our course.
It was too short; we needed more time to learn together.
Table 4 shows the positive aspects of RIPPER most frequently described by students. These included the value of working and learning together, the opportunity of meeting people and networking professionally, and learning in a mentored environment.
Table 4: Aspects of RIPPER most liked by students (n=59)

Students also commented on their learning expectations before and after participating in RIPPER. The most common response before the program indicated an expectation of increased skills and knowledge. At the conclusion of the program, students noted that the greatest learning outcome was related to the theme of collaboration and development of team working skills, rather than the acquisition of new skills. These results were supported by comments which demonstrated a shift in students' perceptions about the value of the experience of learning together. Students identified that learning together is important in its own right; is important for team work; and will better prepare them for professional practice.
Conclusion
Interprofessional health education is a well recognised key to more effective interprofessional practice. However, discipline-specific health education has been the standard practice at undergraduate level in the Faculty of Health Science at the University of Tasmania. Evaluation data from the RIPPER initiative indicates that the program has been successful in promoting the value and need for undergraduate health science students to learn with and from one another, in a relevant and supportive environment.
The evaluation further demonstrates that RIPPER is an effective model for interprofessional learning and practice. This included the use of a number of relevant educational models including adult learning, experiential learning, simulation, reflective practice and peer evaluation. The evaluation highlighted that student exposure to rural health issues resulted in an increased awareness of the nature of rural healthcare provision and the importance of professional collaboration. In the light of an under-resourced rural workforce, these positive learning experiences relevant to rural practice could enhance the future recruitment and retention of staff.
It is important to note that the evaluation findings acknowledged that the students themselves identified the value and importance of interprofessional learning. For example, students voluntarily provided comments expressing their desire for similar and other interprofessional learning opportunities throughout their undergraduate program.
The authors believe that RIPPER should be retained as an elective rural learning module or as one component of a core interprofessional educational unit at the University of Tasmania. The authors also acknowledge that to be truly effective IPE requires a number of interprofessional learning activities incorporated as core and vertically6 integrated components of the University of Tasmania's Health Science curriculum.
There are a number of issues impacting on the sustainability of RIPPER similarly reported in other IPE courses overseas and within Australia4,7. The continued funding of the course is a particular issue. At present the project is funded by the University Department of Rural Health; however, the continued sustainability of the program is dependent on the integration of the course into the Faculty of Health Science curriculum. The resources and time constraints of the program on health professionals and academic staff should also be recognised. With the exception of the development team, the involvement and steadfast commitment of local health professionals and academics to the program is on a voluntary basis. The commitment to IPE and learning needs to be fostered and advanced at faculty level. Initiatives such as staff development for all academics involved in the education and training of health science undergraduate students is one strategy to encourage this commitment to interprofessional education.
Acknowledgements
The authors would like to acknowledge University of Tasmania academics and health professionals for their commitment to and involvement in various aspects of the design, development and implementation of the RIPPER project.
References
1. Parsell G, Bligh J. The Development of a questionnaire to assess the readiness of health care students for interprofessional learning (RIPLS). Medical Education 1999; 22: 95-100.
2. Humphris D, Hean S. Educating the future workforce: building the evidence about interprofessional learning. Journal of Health Services Research and Policy 2004; 9 (1): 24-27.
3. Russell K, Hymans D. Interprofessional education for undergraduate students. Public Health Nursing 1999; 16 (4): 254-262.
4. Albert E, Dalton L, Spencer J, Dunn M, Walker J. Doing it together: the Tasmanian Interdisciplinary Rural Placement Program. Australian Journal of Rural Health 2004; 12: 30-31.
5. McNair R, Brown R, Stone N, Sims J. Rural interprofessional education: promoting teamwork in primary health care education and practice. Australian Journal of Rural Health 2001; 9 (suppl): S19- S26.
6. Hays R. Interprofessional education in rural practice: how, when and where? Rural and Remote Health 8: 939. (Online) 2008. Available: http://www.rrh.org.au (Accessed 1 September 2008).
7. Medves J, Paterson M, Chapman C, Young J, Tata J, Bowes D, Hobbs N, McAndres B, O'Riordan A. A new interprofessional course preparing learners for life in rural communities. Rural and Remote Health 8: 836. (Online) 2008. Available: http://www.rrh.org.au (Accessed 1 September 2008).
8. Dalton L, Spencer J, Dunn M, Albert EG, Walker JH, Farrell GA. Re-thinking approaches to undergraduate health professional education: Interdisciplinary rural placement program. Collegian 2003; 10(1): 17-21.
9. Centre for the Advancement of Interprofessional Education (CAIPE). Defining IPE. (Online) 2002. Available: http://www.caipe.org.uk (Accessed 1 September 2008).
10. Roberts C, Howe A, Winterburn S, Fox N. Not so easy as it sounds: a qualitative study of a shared learning project between medical and nursing undergraduate students. Medical Teacher 2000; 22 (4): 386-391.
11. Pirrie A, Hamilton S, Wilson V. Multidisciplinary education; some issues and concerns. Educational Research 1999; 41(3): 301-314.
12. Hammick M, Freeth D, Koppel I, Reeves S, Barr H. A best evidence systematic review of interprofessional education. BEME Guide no.9. Medical Teacher 2007: 29: 735-751.
13. Faresjo T. Interprofessional education- to break boundaries and build bridges. Rural and Remote Health 6: 602. (Online) 2006. Available: http://www.rrh.org.au (Accessed 1 September 2008).
14. Cooke S, Chew-Graham C, Boggis C, Wakefield A. I never realised that doctors were into feelings too: changing student perceptions through interprofessional education. Learning in Health and Social Care 2003; 2(3): 137-146.
15. Hays R. Interprofessional education in the community: where to begin. The Clinical Teacher 2007; 4: 141-145.
16. Geller Z, Rhyne R, Hansbarger L, Borrego M, Van Leit B, Scarlett I. Interdisciplinary health professional education in rural New Mexico: a 10 year experience. Learning in Health and Social Care 2002; 1: 22-46.
17. Hayward KS, Powell LT, McRoberts J. Changes in student perception of interdisciplinary practice in rural setting. Journal of Allied Health 1996; 25: 315-327.
18. Racher FE. An interdisciplinary rural health course: opportunities and challenges. Nurse Education Today 2002; 22: 387-392.
19. Ramanow R. Building on Values: The Future of Healthcare in Canada: Final Report. Saskatoon: Commission on the Future of Health Care in Canada, 2002: 109.
20. Freeth D, Reeves S, Koppel I, Hammick M, Barr H. Evaluating Interprofessional education: a self help guide. Higher Education Academy Health Sciences and Practice Network. (Online) 2005. Available: http://www.health.heacademy.ac.uk/publications/occasionalpaper/occp5 (Accessed 10 October 2007).
21. Ezzy D. Qualitative analysis: practice and innovation. New South Wales: Allen and Unwin, 2002.
22. Rice P, Ezzy D. Qualitative research methods: a health focus. Melbourne: Oxford University Press, 1999.
23. Willis K. Analysing qualitative data. In: M Walter (Ed). Social research methods: an australian perspective. Melbourne, Vic: Oxford University Press, 2006.
24. Braithwaite J, Travaglia J. The ACT Health Inter-professional learning and clinical education project: background discussion paper #'1'. The value, governance and context of interprofessional learning and practice. Canberra: Braithwaite and Associates and the ACT Department of Health, 2005.
25. Cooke S, Chew-Graham C, Boggis C, Wakefield, A. I never realised that doctors were into feelings too: changing student perceptions through interprofessional education. Learning in Health and Social Care 2003; 2(3): 137-146.


