Introduction
Obstructed labour is a disorder of foeto-pelvic relationships characterised by failure to progress despite strong uterine contractions. Obstructed labour affects 3-6% of labouring women globally, and is a major cause of both maternal and newborn morbidity and mortality1. Obstructed labour is associated to high perinatal mortality rate (150 to 650 per 1000 births) and contributes to 8% of maternal mortality2-5. More than 80% of these maternal deaths can be prevented by improving the availability and quality of Emergency Obstetric Care (EmOC)5.
Malawi is a sub-Saharan African country in which approximately 80% of the population live in rural areas and only 57% of deliveries take place in health facilities, with the remainder taking place at home or with a Traditional Birth Attendant (TBA)6. The referral system is weak due to poor roads, lack of transport and an absence of communication between health centres and hospitals. In addition, suboptimal quality of care is a common problem in health facilities7. This implies that emergency obstetric care services are difficult to access and, where accessible, are of sub-optimal quality.
Criteria-based audit can improve the quality of professional practice8. Criteria-based audit is strongly supported by expert opinion as well as national and international organisations including the World Health Organisation (WHO) and the National Institute of Clinical Excellence (NICE) in the United Kingdom9,10. NICE defines audit as:
A quality improvement process that seeks to improve patient care and outcomes through systematic review of care against explicit criteria and implementation of change. Aspects of structure, processes, and outcomes of care are selected and systematically evaluated against explicit criteria. Where indicated, changes are implemented at individual, team, or service level and further monitoring is used to confirm improvement in healthcare delivery 10.
The criteria-based audit consists of five steps which constitute the classic audit cycle (Fig1). The first step is the development of standards. Once standards have been developed, current practice is measured and compared with standards (optimal practice). Gaps in current practice are identified, recommendations made and implemented, and progress is evaluated.
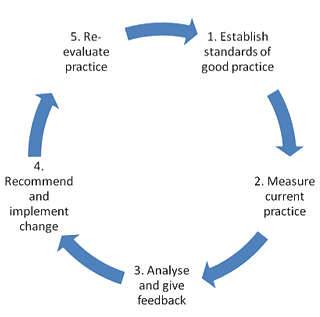
Figure 1: Criteria-based audit cycle. This figure presents the classic criterion-based audit cycle, which has five steps: (i) establishing standards of best practice; (ii) measuring the current practice; (iii) comparing the current practice with standards of best practice; (iv) making and implementing recommendations to fill the gaps between current practice and best practice; and (v) involving a re-evaluation of the recommendations implemented and where necessary refining practice.
Traditionally standards have been developed by a panel of experts and then implemented by a multidisciplinary team. As part of a collaborative program to reduce maternal and neonatal mortality in Malawi, the authors sought to introduce criteria-based audit for emergency obstetric care. The feasibility of involving all cadres of health professionals in the establishment of standards for obstructed labour in Malawi was studied. This article describes the process and presents the standards for obstructed labour developed in Malawi.
Methods
Standards for obstructed labour were developed in three districts (Salima, Kasungu, Lilongwe) in the Central region of Malawi. The three districts have a population of 2 812 183 people with 73 health facilities (9 hospitals and 64 health centres). Before the establishment of these standards a baseline survey was conducted in the three districts. All hospitals and health centres in the three districts were visited and data collected on maternal and newborn health services and outcomes for a period of 3 months (1 May to 31 July 2006). These data helped identify areas in which standards should be established.
The standards for obstructed labour were established during three workshops that brought together participants from the three districts and from the Ministry of Health.
Workshop 1: Establish standards for obstructed labour
The standards were developed using evidence from Malawi national guidelines and WHO manuals11,12. Where necessary, this was supplemented by evidence from the Cochrane database and articles from peer-reviewed journals. Local standards were established during a workshop that brought together 61 participants who included representatives from all hospitals, some health centres and the Ministry of Health. Health professionals of all grades working in maternity units (nurses, midwives, laboratory technicians, anaesthetic technicians, doctors and obstetricians) were represented. The workshop was led by healthcare providers in the three districts. Participants were divided into four groups and each group was made up of a multidisciplinary team. There was one facilitator per group and the facilitator encouraged active participation of all members in the group. The seven objectives were established during a joint session in which all groups were present. The groups established the structure, process and outcome during break-out sessions. During plenary sessions that followed the break-out sessions, the groups came together and each group presented its work. The participants discussed how standards are derived and how they are stated with clear objectives and structure, process and outcome criteria for each objective. The participants had lively discussion and debated openly on subjects such as: What is feasible in our districts? What is the reproductive policy and strategic plan? What is current evidence/best practice? Agreement on standards were reached by simple consensus. At the end of this two-day workshop, the participants agreed on seven objectives and developed the structure, process and outcome criteria for each objective.
Workshop 2: Review and finalise the standards initially developed
The second workshop brought together 55 participants from the Ministry of Health, health centres and hospitals of the three target districts. The participants reviewed the standards developed during the first workshop and agreed on a final list of criteria. During this review process, the participants considered evidence from the WHO manuals and national guidelines11,12 and their relevance to the three districts.
Workshop 3: Select criteria to audit during the next 6 months
The third workshop brought together 58 participants from health centres and hospitals (healthcare providers and administrators). From the initial list of 137 criteria, 6 criteria were selected to be audited within the next 6 months, in order to assess and improve the management of obstructed labour in maternity units in the three districts. Current practice will be measured by a retrospective review of case notes. Gaps between current practice and standards will be identified and recommendations made for change. A re-audit will be conducted later to evaluate the recommendations and practice.
Results
Prolonged/obstructed labour in the three districts prior to the establishment of standards
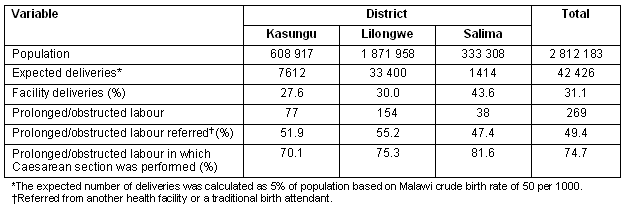
During a period of three months (1 May to 31 July 2006) there were 269 cases of prolonged labour and/or obstructed labour in the three districts. Before the establishment of standards the healthcare providers did not routinely distinguish between prolonged labour and obstructed labour. Approximately half (49.4%) the cases of obstructed labour were referred from another health facility (65.0%) or by a TBA (35.0%). However some of the cases referred by health centres had been referred to the health centre by a TBA. Approximately three-quarters (74.7%) of the cases of obstructed labour had Caesarean section. All hospitals and health centres declared that routinely monitor all cases of labour with a partograph. Table 1 presents statistics on prolonged labour/obstructed in the three districts before the establishment of standards.
Table 1: Obstructed labour in three districts in Malawi (1 May to 31 July 2006)
Agreed standards for obstructed labour
Table 2 presents the definition of obstructed labour as agreed by participants. Prolonged labour was defined as labour lasting more than 12 hours12. Prolonged labour precedes the development of obstructed labour which is a syndrome characterised by signs of failure to progress despite adequate uterine contractions.
Table 2: Working definition of obstructed labour, as agreed by participants

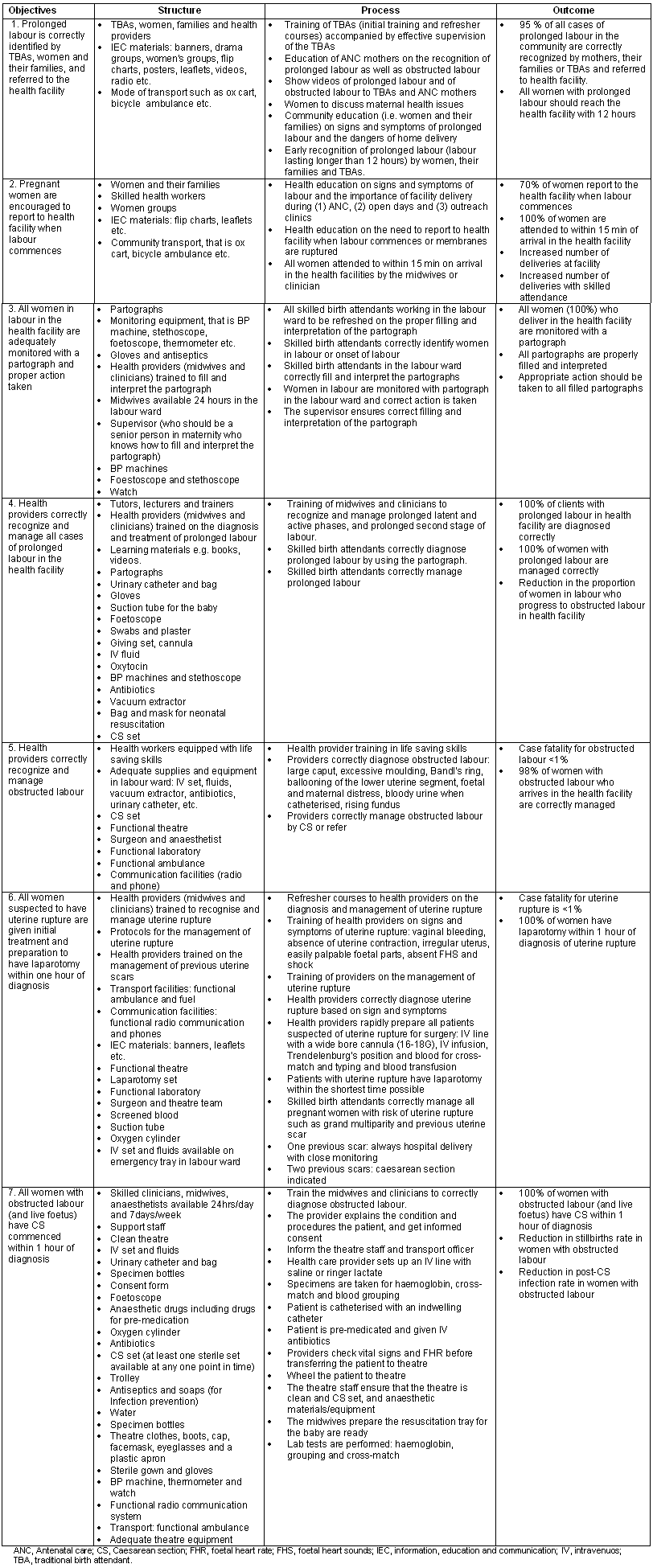
The standards developed for obstructed labour consisted of seven objectives, each with structure, process and outcome criteria. The standards addressed different aspects of the management of obstructed labour, namely: early recognition of prolonged labour by labouring women and TBAs; early arrival of women during labour at health facilities; proper use of partograph by healthcare providers; proper management of prolonged and/or obstructed labour; and proper management of uterine rupture (a common complication of obstructed labour). Table 3 presents the agreed standards for obstructed labour (each bullet point in this table represents to one criterion).
The seven objectives were:
- Prolonged labour is correctly identified by TBAs, women and their families, and referred to the health facility.
- Pregnant women are encouraged to report to a health facility when labour commences.
- All women in labour in the health facility are adequately monitored with a partograph and proper action taken.
- Health providers correctly recognize and manage all cases of prolonged labour in a health facility.
- Health providers correctly recognize and manage obstructed labour.
- All women suspected to have uterine rupture are given initial treatment and preparation to have a laparotomy within 1 hour of diagnosis.
- All women with obstructed labour (and a live foetus) have Caesarean section commenced within 1 hour of diagnosis.
Table 3: Standards for obstructed labour, as agreed by the participants
Criteria selected to audit in the first six months
Six criteria were selected to be audited in the next 6 months, namely: (i) an intravenous (IV) line is set up and the patient hydrated by giving IV fluids; (ii) typing and cross-matching should be performed; (iii) the urinary bladder should be drained; (iv) broad spectrum antibiotics should be administered; (v) Caesarean section is commenced within 1 hour or the foetus delivered within 2 hours of diagnosis; and (vi) an observation chart (pulse, temperature, blood pressure, and urine output) is set up and maintained.
The selection was based on perceived deficiencies in the management of obstructed labour in maternity units in the three districts. The criteria addressed different aspects of care, such as treatment of dehydration, typing and cross-matching of blood, draining of the urinary bladder, administration of antibiotics, monitoring and prompt delivery by Caesarean section or vaginal delivery, as indicated.
Discussion
This article describes the development of standards for obstructed labour in a resource-limited setting by a multidisciplinary team involving all cadres of health professionals working in maternity units, as well as hospital managers and policy makers in Malawi. Criteria to be audited in the next 6 months were identified by the participants based of perceived deficiencies, level of priority and availability of resources. It was noted that important but simple principles of care for women with obstructed labour (such as hydration; typing and cross-matching; draining of the urinary bladder; and administration of broad spectrum antibiotics) were not routinely carried out for all patients with obstructed labour.
Some authors have reported the introduction of criteria-based audit in developing countries13-15. All these studies used the conventional method of establishing standards where standards are developed by a panel of experts (usually obstetricians) and then implemented by a multidisciplinary team, usually made up of nurses, midwives, doctors and specialists, including obstetricians. Following this conventional approach, the lower cadres of staff are excluded from the early stages of the audit cycle, namely the development of the standard. We involved all grades of staff in this criteria-based audit from the beginning, so they all participated in the establishment of standards. The early involvement of all staff is aimed to promote successful implementation, ownership and sustainability of the standards. We also involved hospital managers and policy-makers; their involvement was also important in promoting changes in the organisation of services. It was also hoped their involvement would encourage support from the hierarchy with regard to the provision of resources required for the implementation of the standards.
The development of standards is the first step in an audit cycle. This crucial step lays the foundation for the clinical audit cycle. If the first step is falsified, then the whole process is invalidated. However, the success of a criteria-based audit in improving the quality of care depends on the ability of the audit team to overcome constraints encountered during the entire cycle.
Conclusion
Ronsmans identified five potential constraints to the introduction of criteria-based audit in developing countries - (i) poor access to scientific literature; (ii) lack of resources to support audit activities; (iii) the hierarchical structure of the medical profession; (iv) poor quality of case notes; and (v) the scale of resource constraints16. However, our experience suggests it is feasible to develop standards of emergency obstetric care in a low-income country, using a multidisciplinary team that involves health professionals of all grades.
Acknowledgement
The authors acknowledge the Health Foundation for providing financial support for this study.
References
1. Dolea C, Abouzahr C. Global burden of obstructed labour in the year 2000. Geneva: Evidence and Information for Policy, World Health Organisation, 2003.
2. van Beekhuizen HJ, Unkels R, Mmuni NS, Kaiser M. Complications of obstructed labour: pressure necrosis of neonatal scalp and vesicovaginal fistula. Lancet 2006; 368(9542): 1210.
3. Chhabra S, Gandhi D, Jaiswal M. Obstructed labour - a preventable entity. Journal of Obstetrics and Gynaecology 2000; 20(2): 151-153.
4. Weiner R, Ronsmans C, Dorman E, Jilo H, Muhoro A, Shulman C. Labour complications remain the most important risk factors for perinatal mortality in rural Kenya. Bulletin of the World Health Organ 2003; 81(8): 561-566.
5. Melah GS, El-Nafaty AU, Massa AA, Audu BM. Obstructed labour: a public health problem in Gombe, Gombe State, Nigeria. Journal of Obstetrics and Gynaecology 2003; 23(4): 369-373.
6. National Statistical Office (Malawi), ORC Macro. 2004 Malawi Demographic and Health Survey. Calverton: ORC Macro, Maryland, 2005.
7. Seljeskog L, Sundby J, Chimango J. Factors influencing women's choice of place of delivery in rural Malawi - an explorative study. African Journal of Reproductive Health 2006; 10: 66-75.
8. Jamtvedt G, Young JM, Kristoffersen DT, O'Brien MA, Oxman AD. Audit and feedback: effects on professional practice and health care outcomes. Cochrane Database of Systematic Reviews 2006, issue 1. Art. no.: CD000259. DOI: 10.1002/14651858.CD000259.pub2.
9. World Health Organisation. Beyond the numbers: reviewing maternal deaths and complications to make pregnancy safer. Geneva: WHO, 2004.
10. National Institute for Clinical Excellence. Principles for best practice in clinical audit. Abingdon: Radcliffe Medical Press, 2002.
11. Ministry of Health and Population (Malawi), JHPIEGO. Malawi National Reproductive Health Services Delivery Guidelines. Lilongwe: Ministry of Health and Population, Malawi, 2001.
12. World Health Organisation. Integrated management of pregnancy and childbirth series (IMPAC) . Geneva: WHO, 2005. Available: http://www.euro.who.int/pregnancy/esscare/20051103_3?language=german (Accessed 20 April 2007).
13. Weeks AD, Alia G, Ononge S, Mutungi A, Otolorin EO et al. Introducing criteria based audit into Ugandan maternity units. BMJ 2003; 327: 1329-1331.
14. Graham W, Wagaarachchi P, Penney G, McCaw-Binns A, Antwi KY, Hall MH. Criteria for clinical audit of the quality of hospital-based obstetric care in developing countries. Bulletin of the World Health Organisation 2000; 78(5): 614-620.
15. Wagaarachchi PT, Graham WJ, Penney GC, McCaw-Binns A, Yeboah Antwi K, Hall MH. Holding up a mirror: changing obstetric practice through criterion-based clinical audit in developing countries. International Journal of Gynecology and Obstetrics 2001; 74: 119-130.
16. Ronsmans C. What is the evidence for the role of audits to improve the quality of obstetric care? Studies in Health Services Organisation and Policy 2001; 17: 207-228.
