Introduction
Thrombolysis for patients with an ST elevation myocardial infarction (STEMI) is most effective if given promptly1,2. Pre-hospital thrombolysis may offer the best opportunity for rapid delivery of lytic therapy. In remote areas, pre-hospital thrombolysis has been shown to be effective and to reduce mortality3. In urban areas there is less certainty about the benefits of pre-hospital thrombolysis and patients are often taken directly to hospital. In the study area, which covers the Highlands of Scotland, patients at more than 30 min travel distance from the local hospital were deemed suitable for pre-hospital thrombolysis, while those closer were brought straight to hospital.
A recent local review of current practice demonstrated relatively poor use of pre-hospital thrombolysis (13%). Furthermore, there were considerable delays in the delivery of in-hospital thrombolysis (average call-to-needle time approximately 70 min). In patients close to hospital, pre-hospital thrombolysis may have offered a potential advantage in terms of earlier thrombolysis. While protocol redesign to encourage a greater use of pre-hospital thrombolysis would seem advantageous, it was felt important to examine more closely the reasons for the current low uptake. Although pre-hospital thrombolysis will often be given by paramedics, there remains an important role for the GP as either a provider, or at least local champion, of this service.
General practitioners' attitudes to pre-hospital thrombolysis are thought to be crucial in the delivery of this service4; however, even in the area where the GREAT study was undertaken, the uptake of pre-hospital thrombolysis greatly fell after the study was completed5. Differences in perceptions between rural or remote and urban GPs have not previously been examined.
The aim of this study was to investigate the attitudes and beliefs of GPs with a view to pre-empting potential barriers to service redesign.
Methods
This was a questionnaire based survey of GPs in the North of Scotland (Highland Region). The rational for the study and the final questionnaire was reviewed and approved for distribution to local GPs by the members of the coronary artery disease managed clinical network.
Questionnaire design
The questionnaire was designed by a multidisciplinary group within the local managed clinical network. This process involved several phases. First, members of the group were asked to independently create a list of potential questionnaire queries. These were collated and duplication removed. The questionnaire was then reviewed by several clinical staff members including GPs to form a sense check. The final design was a pragmatic compromise between 'sufficient detail' for the results to be useful and 'brevity' to encourage completion. The final version was trialled on a further small group of staff (doctors and nurses) before being sent to GPs. The questionnaire was simultaneously sent by email and conventional post to all GPs (n = 261) located in the study area.
Definition of rurality
Defining rurality and remote medical practice is complex6,7. This current study took a pragmatic approach to this issue and individual doctors were asked to report if they worked in a mainly 'remote or rural' (rural) or 'urban' practice. The questionnaire was anonymous so there was no formal method for confirming rurality other than the perception of the individual doctor.
Data handling and analysis
Data were entered into an Excel spreadsheet for statistical analysis. For the purposes of further analysis the data were divided into three groups 'urban', 'rural' and 'undefined'. Data were analysed by either unpaired Student's t-test or χ2 statistic as appropriate with significance taken at the 5% level. Qualitative responses were grouped following thematic analysis8.
Results
There was a 49% (n = 127) response. More questionnaires were returned by conventional post than email (106 vs 21, p <0.0001). Ninety-one (72%) GPs described themselves as either rural or urban. The remainder did not specify, suggesting both a both a rural and urban component to their practice (Table 1).
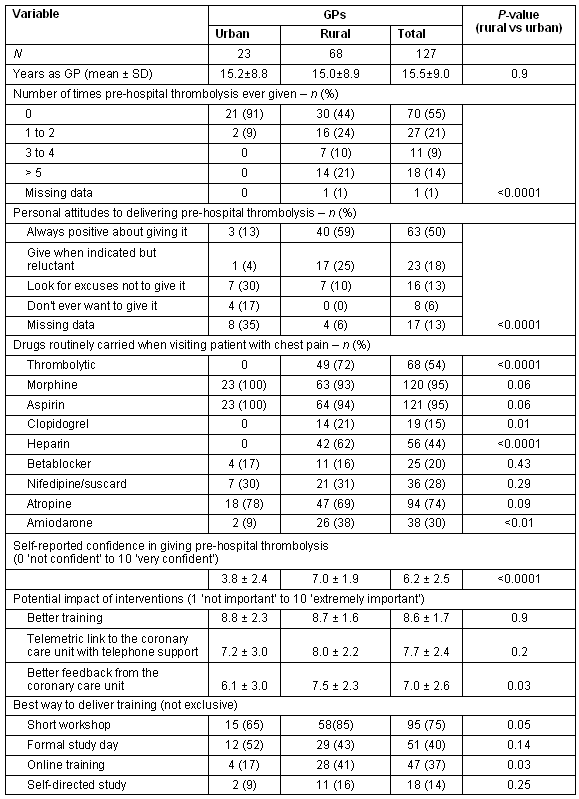
Table 1: Differences between urban and rural GPs attitudes regarding ECG skills and pre-hospital thrombolysis
Effect of previous experience and years in practice on confidence at administering pre-hospital thrombolysis
There did not appear to be a relationship between confidence in giving pre-hospital thrombolysis and number of years worked as a GP. Irrespective of experience rural GPs who had previously administered pre-hospital thrombolysis reported higher confidence compared with GPs who had never given pre-hospital thrombolysis (7.5 ± 1.7 vs 6.3 ± 2.0, p = 0.01; Fig1). Only two urban GPs had previously given pre-hospital thrombolysis and therefore no analysis was possible on the experience of urban GPs.
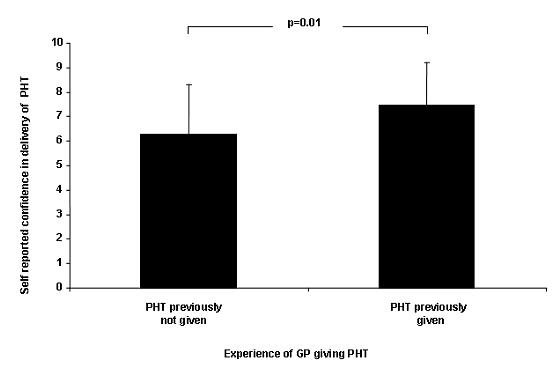
Figure 1: Effect of previous experience of administering pre-hospital thrombolysis (PHT) on confidence in administering pre-hospital thrombolysis
Qualitative responses
In the questionnaire, GPs were asked two open questions:
- What do you think are the main factors preventing delivery of pre-hospital thrombolysis? (Q6)
- What more could be done to increase your own willingness to administer pre-hospital thrombolysis? (Q8)
Responses were classified into four areas: training, experience, organisational and equipment issues (Fig2).
Training: A major and recurring theme with GPs was the perception that there is poor training in the delivery of thrombolysis: 'lack of skills in ECG interpretation', 'I have never been trained to give thrombolysis - just given the kit and assumed I would get on with it', 'I feel I am not up to date'.
Experience: Lack of experience was identified as an issue: 'not enough exposure', 'the last MI I saw was 10 years ago', 'lack or experience so fear making the wrong decision', 'fear of adverse events', 'uncertainty with ECG interpretation'.
Organisational: There was a variety of responses from GPs regarding the role of the ambulance service and the GP in providing emergency care: 'I expect the ambulance service to give it', 'training GPs is a waste of resource - we are not an emergency service', 'I don't think training is relevant to me', 'integration of GPs and ambulance service is important'.
Equipment: Many GPs felt that current equipment carried to chest pain patient calls was a barrier to delivery of thrombolysis: 'difficult with lone working to carry all the gear', 'lack of portable ECG equipment', 'not every GP has an ECG machine to take on a home visit'.

Figure 2: General practitioners' perceived potential barriers to the delivery of pre-hospital thrombolysis. A&E, Accident and emergency department; CCU, coronary care unit; MI, myocardial infarction.
Discussion
This questionnaire-based survey has highlighted several potential barriers to improving the uptake of pre-hospital thrombolysis with important differences between urban and rural GPs. These have been classified according to training, experience, equipment and organisational factors.
Early reperfusion therapy in patients with STEMI decreases mortality and morbidity1,2,9-11. Despite the advantages of primary percutaneous coronary intervention (PPCI) in the acute management of STEMI, there remains an important role for thrombolysis when early PPCI is not possible. Access to PPCI in some areas may be limited by cost, lack of local expertise and services or considerable transfer times in sparsely populated regions. Thus, while PPCI has mortality advantages over thrombolysis12-15, there remains a important role for thrombolysis10,11. Pre-hospital diagnosis and delivery of thrombolysis potentially offers the best opportunity of early reperfusion therapy, more so in areas remote from hospital3. Pre-hospital thrombolysis will not be an appropriate reperfusion strategy for all patients. Nevertheless, up to 20% of the Scottish population are defined as remote or rural and therefore pre-hospital thrombolysis will remain an appropriate therapy even if there is considerable expansion of cardiac catheterisation facilities. Due to the distance and subsequent transport times, PPCI is not currently available to our population, thus thrombolyis is the primary reperfusion strategy for all our patients with 'rescue' PPCI for those patients in whom thrombolysis is unsuccessful.
In this study, rural GPs were more likely to be confident to give thrombolysis and their self-reported confidence in ECG interpretation was higher than in urban GPs. This is not surprising because rural GPs are more likely to have given pre-hospital thrombolysis. Implementation of pre-hospital thrombolysis in areas closer to hospitals may require greater support and training of urban GPs, who reported lower confidence in ECG analysis.
The perceived role of GPs in delivering pre-hospital thrombolysis varied greatly. Many GPs, while lacking in confidence, reported a desire for further training to improve skills. Other GPs clearly stated that they did not consider emergency treatment of myocardial infarction in terms of thrombolysis part of their role, and that the treatment of acute STEMI in the community should be performed by the ambulance service. This was a view that was held by urban rather than rural GPs.
The poor response rate by email compared with a good postal response was unexpected. There are several reasons why this may have occurred. It is possible that not all GPs routinely use email. Furthermore, the questionnaire was primarily designed as a postal questionnaire; if it had been designed as an online survey the electronic response rate may have been higher. This was a deliberate decision based on local knowledge of primary care and the general lack of email communication between primary and secondary care in our region. Nevertheless, the use of online surveys in the future should be considered as they have many potential advantages, namely easy of administration, including data collation and ease of electronic reminders.
Implications for practice
It is clear from the study responses that there is a perception among some GPs that delivering thrombolysis to patients with STEMI is no longer the role of the GP, and that GPs should not be providing emergency care. Nevertheless, even GPs in urban areas may be first to the scene of a patient suffering a STEMI and it is important that at the very least GPs do not discourage ambulance paramedics from delivering appropriate thrombolysis. Paradoxically, in remote areas it is clear that a lack of ambulance crews and poor communication between the ambulance service and GPs leads to instances of 'scoop and run' to hospital, even when the distances are considerable and local GPs have the ability and desire to administer pre-hospital thrombolysis. Clear local clinical care pathways might help resolve some of these issues.
As a result of this survey a training program has been established for the coronary care nurses and a telemetry link to all ambulances in our area installed with a dedicated 'thrombolysis' telephone. Thus a 24 hour/7 days per week ECG analysis and support service is available to the ambulance crews which, with mandatory transmission of ECG for chest pain patients, should improve diagnostic accuracy and confidence in delivering pre-hospital thrombolysis where appropriate. However, in many remote areas there are insufficiently manned ambulances (single crew or driver only) where a dual response with the GP is necessary to deliver pre-hospital thrombolysis. Furthermore, due to ambulance shortages, GPs may be the first attenders and therefore increased training and support for GPs is an important consideration. When, as part of the questionnaire process, GPs were offered a free online ECG course there was a greater than 50% course uptake, confirming GPs' expressed need and desire for additional ECG training.
The role of secondary care
Despite best efforts, it is unlikely that pre-hospital thrombolysis will be given to all eligible patients due to clinical diagnostic uncertainty in the pre-hospital environment. ECG misinterpretation is an issue, although improved techniques for transmission of ECGs to emergency departments and coronary care units should minimise this. Where pre-hospital thrombolysis has been inappropriately withheld, prompt in-hospital recognition of STEMI and delivery of thrombolysis should remain a priority for hospital staff. Encouraging delivery of thrombolysis in emergency departments or by nurse practitioners may reduce door-to-needle times16.
Study limitations
The response rate of 49% was a reasonable response from busy GPs. The questionnaire was sent only once. While increased numbers of responders could have been achieved by repeated reminded either by post, email or telephone, a decision was taken by the managed clinical network that this approach might risk alienating local GPs. Thus, this questionnaire-based survey may have been susceptible to reporting bias; it is possible that GPs with a strong opinion about pre-hospital thrombolysis or with more experience and confidence may have been more likely to respond. Nevertheless, our survey revealed a variety of responses in terms of attitudes to pre-hospital thrombolysis, suggesting that this survey reflected the breadth of opinion of the whole GP population in our area. Some GPs reported neither 'rural' nor 'urban' location. The assumption was made that these responses signified practices with both elements; however, non-response is also a possibility. These data should be considered with caution and therefore were removed from analysis of rural vs urban issues (Table 1).
Future research
Several areas merit further research. First, strategies to improve the uptake of pre-hospital thrombolysis should be developed. Some of these (including increased education for GPs and paramedics, a coronary care 'hot line' and telemetry link) have been developed locally and the clinical effectiveness of these should be assessed. Second, the complex issue of who should deliver emergency care to patients in urban and rural areas deserves further study. The perception by some (mainly urban) GPs that this is not part of the GP's role is of interest. Third, there is anecdotal evidence of poor communication in the pre-hospital setting between GPs and the ambulance service, and this warrants more detailed investigation. Finally, engaging the public in these issues is crucial. While reducing delays for the delivery of thrombolysis by healthcare staff is important, delay is also caused by patients' reluctance to make the call for help. The reasons for this are not clear and probably multifactorial.
Conclusions
This questionnaire-based survey has highlighted several potential barriers to improving the uptake of pre-hospital thrombolysis. These issues were classified as those regarding training, experience, equipment and organisational factors. Key differences existed between rural and urban GPs. Rural GPs were more likely to be confident to give thrombolysis. However, to implement pre-hospital thrombolysis in areas closer to hospitals may require greater support and training of urban GPs, who reported lower confidence in ECG analysis. The perceived role of GPs in delivering pre-hospital thrombolysis varied greatly. Many GPs, while under-confident, reported a desire for further training to improve skills. Other GPs clearly stated that they did not consider emergency treatment of myocardial infarction in terms of thrombolysis as part of their role, and that the treatment of acute STEMI in the community should be performed by the ambulance service. This view held by urban rather than rural GPs and should be clarified to ensure that the presence of a GP does not discourage paramedics from delivering pre-hospital thrombolysis. In remote areas it is clear that a lack of ambulance crews and poor communication between the ambulance service and GPs leads to instances of 'scoop and run' to hospital, even when the distances are considerable and local GPs have the ability and desire to administer pre-hospital thrombolysis. Clear local clinical care pathways may help resolve some of these issues.
Acknowledgments
The authors thank Mr David Fitzpatrick, Dr Elizabeth Imray and Dr Anne Scott for their assistance in the preparation of this manuscript.
References
1. The GUSTO investigators. An international randomized trial comparing four thrombolytic strategies for acute myocardial infarction. New England Journal of Medicine 1993; 329: 673-682.
2. Boersma E, Maas ACP, Deckers JW, Simoons ML. Early thrombolytic treatment in acute myocardial infarction: reappraisal of the 'golden hour'. Lancet 1996; 348: 771-775.
3. GREAT Group. Feasibility, safety and efficacy of domiciliary thrombolysis by general practitioners. BMJ 1992; 305: 548-553.
4. Rawles J. Attitudes of general practitioners to prehospital thrombolysis. BMJ 1994; 309: 379-382.
5. Rawles J, Sinclair C, Jennings K, Ritchie L, Waugh N. Audit of prehospital thrombolysis by general practitioners in peripheral practices in Grampian. Heart 1998; 80: 231-234.
6. Muula A. How do we define 'rurality' in the teaching on medical demography? Rural Remote Health 7: 653. (Online) 2007. Available: www.rrh.org.au (Accessed 26 February 2009).
7. Smith JD, Margolis SA, Ayton J, Ross V, Chalmers E, Giddings P et al. Defining remote medical practice. A consensus viewpoint of medical practitioners working and teaching in remote practice. Medical Journal of Australia 2008; 188(3): 159-161.
8. Aronson J. A pragmatic view of thematic analysis. The Qualitative Report 1994; 2(1). Online (1994). Available: http://www.nova.edu/ssss/QR/BackIssues/QR2-1/aronson.html (Accessed 26 February 2009).
9. Fibrinolytic Therapy Trialist's (FTT) Collaborative Group. Indications for fibrinolytic therapy in suspected acute myocardial infarction: collaborative overview of early mortality and major morbidity results from all randomised trials of more than 1000 patients. Lancet 1994; 343(8893): 311-322.
10. The GUSTO investigators. An international randomised trial comparing 4 thrombolytic strategies for acute myocardial infarction. New England Journal of Medicine 1993; 329: 673-682.
11. SIGN guideline 93. Acute coronary syndromes. (Online) 2007. Available: www.sign.ac.uk/guidelines/fulltext/93/index.html (Accessed 21 April 2008).
12. Nallamothu BK, Fox KAA, Kennelly BM, Van de Werf F, Gore J M, Steg P G et al. Relationship of treatment delays and mortality in patients undergoing fibrinolysis and primary percutaneous coronary intervention. The Global Registry of Acute Coronary Events. Heart 2007; 93: 1552-1555.
13. Steg PG, Bonnefoy E, Chabaud S, Lapostolle F, Dubien P-Y, Cristofini P et al. Impact of time to treatment on mortality after prehospital fibrinolysis or primary angioplasty. Data from the CAPTIM randomised clinical trial. Circulation 2003; 108: 2851-2856.
14. Widimsky P, Bilkova D, Penicka M, Novak M, Lanikova M, Porizka V et al. Long-term outcomes of patients with acute myocardial infarction presenting to hospitals without catheterisation laboratory and randomised to immediate thrombolysis or interhospital transport for primary percutaneous coronary intervention. Five-year follow-up of the PRAGUE-2 trial. European Heart Journal 2007; 28: 671-684.
15. Armstrong PW, WEST Steering Committee. A comparison of pharmalogic therapy with/without timely coronary intervention versus primary percutaneous intervention early after STEMI: the WEST (Which Early ST-elevation myocardial infarction Therapy) study. European Heart Journal 2006; 27: 1530-1538.
16. Cornfield AR, Graham CA, Adams JN, Booth I, McGuffie AC. Emergency department thrombolysis improves door-to-needle times. Emergency Medicine Journal 2004; 21: 676-680.

