Context
Setting
The Northern Territory (NT) of Australia is a unique environment for training medical students. It occupies approximately one-sixth of the land area of Australia, but comprises only 1% of the population (approximately 200 000)1. Approximately 30% of the population are Indigenous, compared with 2% nationally2. The capital city Darwin has approximately 100 000 people. Although small compared with other state capitals, Darwin is the major business and health centre for the NT and is regarded as the 'big smoke' by most Territorians.
Since 1998, the Northern Territory Clinical School (NTCS) has been teaching graduate entry students in their final 2 years of medicine at its main campus in Darwin. The NTCS, a clinical school of Flinders University, originally focused almost exclusively on hospital-based learning, with third year students undertaking sequential rotations at Royal Darwin Hospital (RDH) in the core clinical disciplines. The community-based component of clinical training was comparatively small: students undertook only 8 half-day placements in urban general practice and spent 2 weeks in a rural general practice setting.
Community based medical education
In recent years, the focus of international medical student education has shifted from traditional hospital-based training to learning in the community3. This reflects a move away from long-stay hospital care towards day cases and community-oriented care. In Australia, another factor driving this change is the projected massive increase in medical student numbers over the next few years4. This increase will require the development of multiple new training locations, including general practice settings, both rural and urban.
Community based medical education (CBME) has a sound educational basis, with a particular focus on patient centredness, whole-person care, social determinants of health, multidisciplinary care and continuity of care5. Community based medical education in the rural setting has been shown to deliver effective and high quality training6, and has been implemented as a strategy to help address medical workforce shortages in many rural and regional areas7.
At a local level, reviews of the Flinders University third year curriculum revealed a relative lack of exposure to community medicine and public health8. This was incongruous in the learning environment of the NT, one characterised by Aboriginal health and an emphasis on rural and remote primary care practice. Addressing this imbalance was a major driving force towards moving to a community-based curriculum. In addition, RDH had reached saturation of teaching capacity and was faced with increasing numbers of students applying for training.
In 2006, a program of the NTCS known as the Northern Territory Rural Clinical School (NTRCS) commenced in the small outback town of Katherine. Students in this program undertook half their third year training in a variety of rural settings, including the local hospital and community clinics. This model was expanded into the Central Australian town of Alice Springs in 2007.
Issue
In 2008, the NTCS enrolled its first cohort of students in a new 'hybrid' CBME program, based in urban Darwin. The program involved placing four third year students in general practice and other community health settings throughout urban Darwin for one semester of their clinical training, and in traditional hospital-based training for the other. Students swapped at the mid-point of the year, so all were exposed to both training settings. In this article, we discuss the process and challenges involved in establishing this hybrid CBME program, particularly the adaptation of an existing successful rural model to an urban setting.
Program design and development
The key steps in the development of the urban CBME program are summarised in Figure 1 and elaborated below. These steps were not discrete activities, nor was program development a simple linear process - steps occurred in parallel and were often interconnected.

Figure 1: Key steps in the development of the urban community based medical education program.
Engagement with key partners and stakeholders: Community engagement is the foundation stone of successful community-based programs9. A community consultation process was conducted with key partners and stakeholders at the conception of the new program. Participants included GPs and community health providers, NTCS hospital teachers and academics, general practice and other community organisations, Aboriginal health groups, NT and Federal governments, consumer representatives, and organisations responsible for health professional training and medical workforce planning.
The consultation process highlighted the potential strengths and weaknesses of the program, and emphasised the importance of vertically integrated learning. The consultation process also helped fashion the overall aims of the new CBME program by better defining the 'end product', namely 'a world class doctor with an affinity to live and work in the NT'. Key attributes were identified as clinical competence, cultural sensitivity and safety10, professionalism, and the ability to work in a team.
From this consultation process, a stakeholder forum was established to inform and guide the development and implementation of the new program. This was equivalent to the community advisory committees in the NTRCS model.
Establishment of the community based medical education team: A key preliminary step was to appoint an academic to develop and lead the new program. This academic also had responsibility for the NTRCS, allowing very close alignment and cross-fertilisation of the two programs. The multidisciplinary nature of the new CBME program was reflected by the establishment of an interprofessional academic team, which consisted of two GPs, a speech pathologist, a dietician, an Aboriginal cultural awareness consultant, and the NTCS research and evaluation officer.
Development of aims and action plan: The aims of the CBME program were then developed through amalgamation of the relevant aspects of the NTCS strategic aims, the Flinders University third year curriculum, the consultation findings, and review of the literature on CBME (Fig 2).

Figure 2: Aims of the urban community based medical education program.
Following the formulation of aims, a plan for the development and implementation of the new program was written, consisting of key objectives, actions and targets.
Development of a curriculum framework: The third year core curriculum is dictated by Flinders University at all training sites, rural and urban. However, local adaptation is necessary to reflect the particular characteristics of the different locations and programs. Implementation of the new urban CBME program therefore required the development of a new framework for curriculum delivery, attempting to best match the required learning objectives with available learning opportunities in each setting.
This process was informed by a series of meetings with key groups, including GPs, students, hospital clinicians and other providers. Hospital teachers identified the content and nature of current student teaching, including their perception of coverage of prescribed curriculum objectives. Community-based providers were invited to nominate learning objectives for their particular discipline or setting e.g. family planning. Of note, these meetings revealed that the specific content of existing student teaching in both hospital and community settings was not well defined.
In order to identify potential learning opportunities and predict clinical exposure within the Darwin community setting, we analysed local data from the nationwide study of general practice clinical activity (the Bettering the Evaluation and Care of Health (BEACH) study)11. This included patient demographics, reasons for encounter and problems managed, and provided a summary profile of the general practice clinical activity (i.e. the potential teaching and learning opportunities) in urban Darwin. We believe this is the first time general practice clinical activity data has been used for evidence-based curriculum development.
A curriculum mapping exercise was then performed, based on the Flinders University third year curriculum objectives; prescribed lists of conditions, presentations and procedural skills; the Australian National Health Priority areas12; the Darwin BEACH data; and additional NT relevant objectives. Gaps and redundancies were identified and the information was used to inform GP preceptors, hospital clinicians and community supervisors.
Multidisciplinary teaching: Like its rural counterpart, the core of the new CBME program is based on patient exposure in the general practice setting. Students were to spend 1.5 to 2 days (roughly one-third of the week, each week) in general practice, attending patients under the supervision of GP preceptors.
However, one of the strengths of CBME is to provide an opportunity for students to see the patient care pathway span a range of services13, and especially to experience teaching by non-medical teachers. Consequently, we incorporated a range of non-medical, community healthcare providers into the curriculum through the formation of our so-called 'C4 program' (Continuing Comprehensive Care in the Community). This represented a significant change from the NTRCS and many other rural programs, where access to hospital specialists is the major complement to general practice teaching. A considerable fraction (approximately one-third) of the CBME week is based in non-GP healthcare settings, with the remainder spent in formal tutorials.
Recruitment of training placements: A practice recruitment process was undertaken, including individual and group meetings with GPs and other health providers. Recruitment of early adopters led to further visits and written agreements for placements. As a result, four general practices were enlisted and 'champions' of the program identified as GP and community preceptors.
Nearly 120 community providers and organisations in Darwin were recognised as having particular relevance to the CBME program. From this list, the CBME team selected a core group to provide compulsory placements for all students in the program, for example family planning, community midwives program, day surgery. For the 'optional' placements, students are encouraged to follow patients from the general practice setting to the other community providers, according to their own learning goals, or their patients' health needs.
A model of vertically integrated teaching was facilitated by interdisciplinary teacher training. The GP preceptors and community based providers were invited to a series of orientation and teacher training workshops, covering teaching skills, curricula and assessment requirements.
Social responsiveness: Another factor influencing curriculum development was the obligation for greater social responsiveness14. Using the Committee of Deans of Australian Medical Schools (CDAMS) document15 as a framework, Aboriginal health teaching was substantially reinforced in the new CBME program. This included the development of an ongoing program of cultural safety training for both students and staff. In addition, a remote Aboriginal health immersion (a 2 week placement with an Aboriginal homelands service in East Arnhem Land in the remote north-east of the NT) was created. This learning experience was developed to provide complementary clinical and cultural experience to urban practice, and help address the most pressing health issue for the Northern Territory, the health of its Indigenous people. The process required the engagement of Aboriginal faculty and Aboriginal networks, community consultation and negotiation, as well as development of specific orientation and training material.
Additionally, the CBME curriculum aims to cover other priority community health concerns, including those for refugees, prisoners and other marginalised groups.
Patient encounter log: In order to assess clinical exposure in the urban setting, a patient encounter log book was developed to capture student encounters with patients. For each encounter, students are required to document a basic demographic profile, presenting symptoms, working diagnosis, and management, using the International Classification of Primary Care (ICPC)-216 codes for easy comparison to BEACH data. The level of student involvement (observed, supervised or performed independently) is recorded. Students are also requested to identify up to three learning objectives from each encounter.
Log books have been used for decades in the undergraduate setting to record the clinical and educational experiences of medical students. They come in a wide variety of formats, including handheld (eg pocket-sized encounter cards17), optically scanned18, electronic (Personal Digital Assistant19 and web-based20). After consideration of the experience of other centres, we decided to use an online system linked to a centralised, secure database.
It is proposed to use the patient log to record encounter details in all teaching sites in the new program, namely urban community general practices and other health centres, remote Aboriginal communities, and the teaching hospital. Incorporation of the logbook into the NTRCS program is planned.
Data will to be used to support student learning, as a tool for reflection and feedback21, and to measure achievement of educational objectives22. Aggregated data from the whole year will be compared among training environments and against the BEACH study data to identify gaps and redundancies, support curriculum development and evaluate the program. It is also intended that the data for academic staff and GP preceptor teacher training be used to encourage greater engagement in the program.
Development of an evaluation framework
The CBME evaluation framework was developed as part of the NTCS quality assurance reporting requirements, in order to provide objective data about the program's efficacy and to identify potential areas for development. Specific evaluation methods and outcome measures were developed for each of the core domains of the framework; namely students, clinical preceptors, administrative staff and the curriculum.
Lessons learnt
Similarities with rural CBME
In translating a successful rural CBME model to an urban setting, we predicted that a majority of the reported educational advantages would persist (Table 1). From analysis of the international literature, local BEACH data and consultation findings, we were confident that the new urban program would offer students equivalent high quality learning experiences. These include exposure to core clinical presentations, continuity of care23, integrated learning23, one-to-one supervision and mentoring, and pastoral care24. In addition we expected the urban program to offer exposure to a range of models of healthcare delivery, for example private general practice, Aboriginal community control and public health clinics.
Table 1: Key issues in community based medical education program development and responses to translating a rural to an urban model
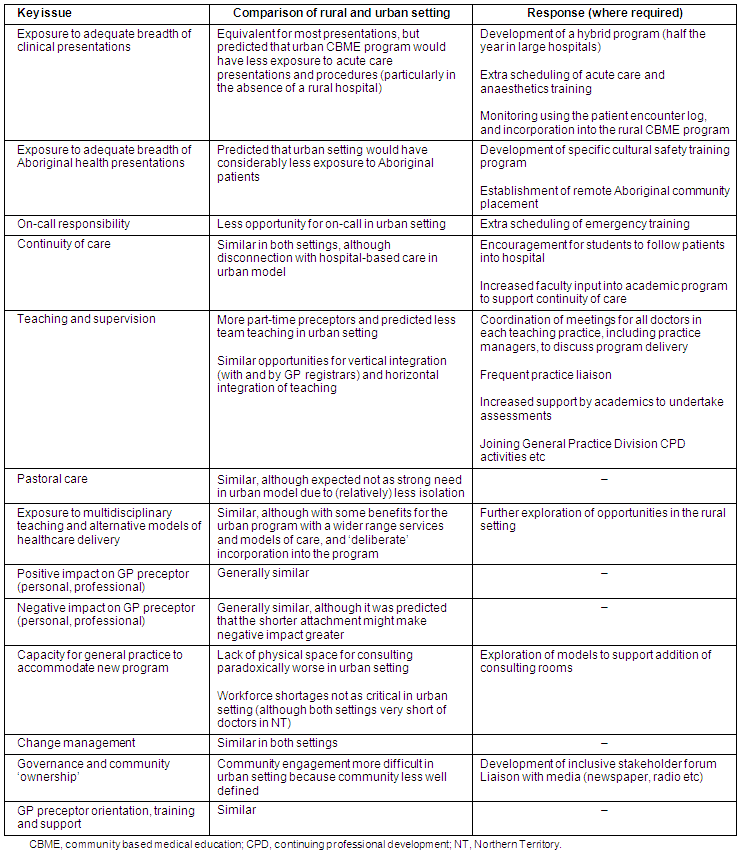
We also expected that the impacts of the program on the new urban GP preceptors would be equivalent to those experienced by their rural counterparts. These included both positive aspects (increased satisfaction and enjoyment, professional development, improved teamwork, enhanced patient care) and negative aspects (stress, discomfort with the training role, conflicting time pressures, reduced productivity and lost income)25.
Furthermore, stakeholder consultation identified that the capacity for Darwin urban general practice to accommodate an increased number of medical students was limited, a situation not dissimilar to the rural setting. The medical workforce of Darwin is more transient and proportionately more part-time compared with other large urban centres26. Other factors similar to rural settings include critical workforce shortages, competition with other learners (e.g. GP registrars, junior doctors) and lack of physical space for consulting (practices are located in shopping malls with limited room for expansion).
Another substantial challenge in implementing the program was change management, again a commonly reported issue in the rural CBME literature27,28. This manifested at a number of levels - within the organisation, across the hospital and GP faculty and in curriculum development. Despite the demonstrated success of the existing rural model, the change from traditional hospital teaching to an urban CBME model was particularly challenging for many NTCS academics and hospital clinicians. Similarly, new GP preceptors expressed significant concerns about the program. This required a substantial amount of consultation, discussion and support.
Differences from rural CBME
Although the commonalities between the two models were significant, there were a few key areas where the new urban program differed from the rural model (Table 1). On the positive side, the urban program was expected to provide access to a much wider range of community service providers and other (non-medical) health professionals than the small towns where the RCS was based, for example refugee health. We also identified the potential for an enhanced advocacy role for students in the urban program, in the setting of less cohesive teams and multiple providers.
One particular challenge in developing the urban program was the difficulty defining the 'community' in which it was to be based. This was in contrast to the more discrete community of the NTRCS campuses. We were aware that true community ownership was the result of partnership development with local stakeholders, and strived to be inclusive in representation of the CBME stakeholder's forum.
The hybrid model
In balancing these various factors, the so-called 'hybrid' model was developed (Fig 3), comprising half the core clinical training in the community with the balance in the traditional hospital setting. This was a pragmatic approach to providing a greater community-based experience in the context of limited capacity and opportunities (e.g. acute care), but it brought with it a number of challenges. In particular, we recognised the risk of educational disconnection between the two environments, with the potential to lead to an artificial division of the curriculum into community and hospital elements. The short duration of the CBME and hospital placements (20 weeks each) could also potentially compromise the depth and effectiveness of the student-preceptor learning relationship29.

Figure 3: Schematic representation of hybrid community based medical education program. CBME, community based medical education; Med, medical; Surg, surgical; O&G, obstetrics and gynaecology; Paeds, paediatrics; Psych, psychiatry.
Conclusion
Although it has been demonstrated that the rural community curriculum is transferable from one rural setting to another27, very few centres have implemented primary care CBME models in urban environments (the majority being longitudinal integrated clerkships in other ambulatory care settings30). The hybrid Darwin CBME model will test the assumption that the documented academic success and the learning methods used in the rural clinical schools are transferable to a small urban community setting. Conversely, our experience demonstrates that there are many lessons to be transferred back to the rural setting.
The Darwin CBME program is small, and is still in its early stages. Eight students (four each semester) completed the first year of the hybrid urban CBME program in 2008. Formal evaluation of the program will be reported separately; however, the effectiveness of the Darwin CBME will become clear over time, with respect to academic performance, cost-effectiveness and sustainability. Regardless, we believe that our program will provide novel information about medical student training in a hybrid urban CBME model, and help inform other clinical schools, both nationally and in other countries, that are considering adopting similar programs.
Acknowledgments
The authors acknowledge the great contributions of the GP preceptors and general practices, other community providers, and the CBME students in helping bring the program to fruition.
References
1. Australian Bureau of Statistics. Population for States and Territories. 3101.0 - Australian demographic statistics. (Online) 2008. Available: http://www.abs.gov.au/ausstats/abs@.nsf/mf/3101.0/ (Accessed 13 August 2008).
2. Australian Bureau of Statistics. Population distribution, Aboriginal and Torres Strait Islander Australians. (Online) 2006. Available: http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/4705.0Main+Features12006?OpenDocument (Accessed June 26 2008).
3. Thistlethwaite J, Kidd MR, Hudson JN. General practice: a leading provider of medical student education in the 21st century. Medical Journal of Australia 2007; 187: 124-128.
4. Joyce CM, Stoelwinder JU, McNeil JJ, Piterman L. Riding the wave: current and emerging trends in graduates from Australian university medical schools. Medical Journal of Australia 2007; 186: 309-312.
5. Habbick BF, Leeder SR Orienting medical education to community need: a review. Medical Education 1996; 30: 163-171.
6. Worley P, Esterman A, Prideaux D. Cohort study of examination performance of undergraduate medical students learning in community settings. BMJ 2004; 328: 207-209.
7. McDonnel Smedts A, Lowe MP. Clinical training in the top end: impact of the Northern Territory Clinical School, Australia, on the Territory's health workforce. Rural and Remote Health 7: 723. (Online) 2007. Available: www.rrh.org.au (Accessed: 12 August 2009).
8. Couper I. Evaluation of the parallel rural community curriculum at Flinders University in the context of GEMP Year 3. Parktown: University of the Witwatersrand; 2006.
9. Worley P. Relationships: a new way to analyse community-based medical education? Part 1. Education for Health 2002; 15: 117-128.
10. Nguyen H. Patient-centred care. Cultural safety in Indigenous health. Australian Family Physician 2008; 37: 990-994.
11. Britt H, Miller GC, Charles J, Pan Y, Valenti L, Henderson J et al. General practice activity in Australia 2005-06. Genneral practice series 19. AIHW cat no GEP 19. Canberra, ACT: Australian Institute of Health and Welfare, 2007.
12. Australian Institute of Health and Welfare. Health priority areas. Canberra, ACT: Australian Institute of Health and Welfare. (Online) no date. Available: http://www.aihw.gov.au/nhpa/index.cfm (Accessed 22 April 2008).
13. Lennox A, Peterson S. Development and evaluation of a community based multi-agency course for medical students: a descriptive survey. BMJ 1998; 316: 596-599.
14. Boelen C, Heck JE. Defining and measuring the social accountability of medical schools. Geneva: World Health Organisation, 1995.
15. Phillips G. CDAMS Indigenous Health Curriculum Framework. Melbourne, Vic: VicHealth, Koori Health Research and Community Development Unit on behalf of the Committee of Deans of Australian Medical Schools, The University of Melbourne, 2004.
16. International Classification Committee of WONCA. ICPC-2 International Classification of Primary care, 2nd edn. Oxford: Oxford University Press, 1998.
17. Rattner SL et al. Documenting and Comparing Medical Students' Clinical Experiences. JAMMA 2001; 286: 1035-1040.
18. Kowlowitz V, Slatt LM, Kollisch DO, Strayhorn G. Monitoring students' clinical experiences during a third year family medicine clerkship. Academic Medicine 1996; 71: 387-389.
19. Kurth RJ, Silenzio V, Irigoyen MM.Use of personal digital assistants to enhance educational evaluation in a primary care clerkship. Medical Teacher 2002; 24: 488-490
20. Nierenberg DW, Eliassen MS, McAllister SB, Reid BP, Pipas CF, Young WW et al. A web-based system for students to document their experiences within six core competency domains during all clinical clerkships. Academic Medicine 2007; 82: 51-73
21. Patil NG, Lee P. Interactive logbooks for medical students: are they useful? Medical Education 2002; 36: 672-677.
2. Carney PA, Pipas CF, Eliassen MS, Donahue DA, Kollisch DO, Gephart D et al. An encounter-based analysis of the nature of teaching and learning in a 3rd-year medical school clerkship. Teaching and Learning in Medicine 2000; 12: 21-27.
23. Hirsch DA, Ogur B, Thibault G, Cox M. "Continuity" as an Organizing Principle for Clinical Education Reform. New England Journal of Medicine 2008; 356: 858-866.
24. Howe A. Twelve tips for community-based medical education. Medical Teacher 2002; 24: 9-12.
25. Walters LS, Worley PS, Prideaux D, Rolfe H, Keaney C. The impact of medical students on rural general practice preceptors. Rural and Remote Health 5: 403. (Online) 2005. Available: www.rrh.org.au (Accessed: 12 August 2009).
26. Top End Division of General Practice. Urban Darwin and Palmerston Workforce Discussion Paper. Darwin, NT: Top End Division of General Practice, 2007.
27. Walters LK, Worley PS, Mugford BV. Parallel Rural Community Curriculum: is it a transferable model? Rural and Remote Health 3: 236. (Online) 2003. Available: www.rrh.org.au (Accessed: 12 August 2009).
28. Ogur B, Hirsh D, Krupat E, Bor D. The Harvard Medical School-Cambridge integrated clerkship: an innovative model of clinical education. Academic Medicine 2007; 82: 397-404.
29. Worley P, Kitto PA. Hypothetical model of the financial impact of student attachments on rural general practices. Rural and Remote Health 1: 83. (Online) 2001. Available: www.rrh.org.au (Accessed: 12 August 2009).
30. Norris TE, Schaad DC, DeWitt D, Ogur B, Hunt DD; Consortium of Longitudinal Integrated Clerkships. Longitudinal integrated clerkships for medical students: an innovation adopted by medical schools in Australia, Canada, South Africa and the United States. Academic Medicine 2007; 84: 902-907.
Abstract
Context: The Northern Territory (NT) of Australia is a unique setting for training medical students. This learning environment is characterised by Aboriginal health and an emphasis on rural and remote primary care practice. For over a decade the NT Clinical School (NTCS) of Flinders University has been teaching undergraduate medical students in the NT. Community based medical education (CBME) has been demonstrated to be an effective method of learning medicine, particularly in rural settings. As a result, it is rapidly gaining popularity in Australia and other countries. The NTCS adopted this model some years ago with the implementation of its Rural Clinical School; however, urban models of CBME are much less well developed than those in rural areas. There is considerable pressure to better incorporate CBME into medical student teaching environment, particularly because of the projected massive increase in student numbers over the next few years. To date, the community setting of urban Darwin, the NT capital city, has not been well utilised for medical student training.
Issue: In 2008, the NTCS enrolled its first cohort of students in a new hybrid CBME program based in urban Darwin. This report describes the process and challenges involved in development of the program, including justification for a hybrid model and the adaptation of a rural model to an urban setting. Relationships were established and formalised with key partners and stakeholders, including GPs and general practices, Aboriginal medical services, community based healthcare providers and other general practice and community organisations. Other significant issues included curriculum development and review, development of learning materials and the establishment of robust evaluation methods.
Lessons learnt: Development of the CBME model in Darwin posed a number of key challenges. Although the experience of past rural programs was useful, a number of distinct differences were evident in the urban setting. Change leadership and inter-professional collaboration were key strengths in the implementation and ongoing evaluation of the program. The program will provide important information about medical student training in urban community settings, and help inform other clinical schools considering the adoption of similar models.
Key words: community based medical education, medical students, training, undergraduate.
You might also be interested in:
2012 - Rural nursing education: a photovoice perspective
2007 - GP perceptions of workforce shortage in a rural setting






