Introduction
Depression is the fourth leading cause of the global disease burden1. By 2020, depression will be second only to heart disease in its contribution to the global burden of disease in relation to disability-adjusted life years2. Several studies have shown that up to 23% of elderly patients suffer from depression or depressive symptoms3,4. Although major depression is relatively rare in the population of older adults, minor depressive symptoms are particularly common in later life. Importantly, the consequences of these minor depressive disorders for the well-being and functioning of older adults seem to be similar when compared with major depressive disorders, contributing to adverse effects on quality of life5,6.
Depression in later life is generally regarded to be highly treatable, but under-treatment is still common in this population7-13. Up to 20% of people attending primary healthcare providers in developing countries suffer from the often-linked disorders of anxiety and depression, but symptoms of these conditions often go unrecognized, with under-reporting of depression being a major problem worldwide1. Additionally, past research has shown that only 35% of those with depression receive treatment14. Based on a convenience sample of 482 primary care visits by patients 65 years and older, Adelman and colleagues found that depression was discussed in only 7% of medical visits15. The researchers note that this low figure could be related to the cross-sectional design of their study; nonetheless, they express surprise at the low rate of depression discussion in a population where depression is prevalent. Given that the majority of depressed elderly people are treated in the primary care sector8,16-19, and that depressed older patients are more than twice as likely as non-elderly patients to visit their primary care physician at least once a month, even after controlling for co-morbidities20, it is critical to better understand how primary care physicians approach and treat depression in their older adult patients21.
The treatment of depression in older adults by primary care physicians may be especially important in rural regions, where ready access to healthcare providers is an issue. For instance, in the USA, while more than 20% of the population lives in places defined as rural, only 9% of all physicians practice in these communities22,23. However, the greatest need may be in rural America, where patients have rates of suicide and major depression equal to or slightly higher than their urban counterparts24-26. The disparity in mental health services between rural and urban areas is a major concern27,28. To improve mental health care in rural areas, it is important to examine and understand the barriers and needs that primary care physicians experience in their care of depressed elderly people.
Methods
Study population
The present study focused on rural Illinois primary care physicians: family physicians and general internists. Surveys were sent to a convenience sample of 68 primary care physicians affiliated with 6 different hospitals in rural Illinois, and to all 94 graduates and preceptors of the Rural Medical Education (RMED) Program of the University of Illinois College of Medicine at Rockford. This represents a sample of approximately 25% of rural family and general practice physicians in Illinois.
Instrument
The data collection instrument consisted of a four-page survey composed of 5 parts, based on an earlier survey of primary care physicians29 and updated to reflect the recent literature on the treatment of depression, especially that related to older adults (Appendix I).
Part 1: Current practices: Data collected on current practices was in regard to recognizing and managing depression in older adults, including questions about routine screening methods, use of screening tests and guidelines, laboratory examinations, gaps between preference of treatment and the availability of that treatment and the use of patient education materials.
Part 2: Information on attitudes and perceptions: Data on attitudes and perceptions included responses to statements on the diagnosis and treatment of geriatric depression in primary care, where physicians were asked to specify the extent of agreement or disagreement using a 5 point Likert scale.
Part 3: Identification of barriers: Barriers to adequate diagnosis and treatment of geriatric depression were identified, including the stigma of psychiatric treatment, access to mental healthcare in the community, inadequate insurance coverage for mental health care and not enough time for discussion.
Part 4: Physicians' reports of needs and directions: Physicians' reports of needs and directions to improve care for depressed geriatric patients was collected by asking the respondents to rate 15 items, including increased time with each patient, better availability of psychologists, increased reimbursement for counseling and mental health services located in primary care practice.
Part 5: Background and demographics: Background and demographics data included physicians' sex, age, specialty, percentage of depressed patients in practice, percentage of depressed elderly patients and involvement in teaching medical students and residents.
The survey was a self-report, self-administered instrument, taking approximately 10-15 min to complete. It was tested and piloted in relation to content and completion time. The survey instrument and study methods were approved by the university Institutional Review Board.
Data collection
All physicians in the study sample were initially contacted by mail, which included the survey instrument, a personalized cover letter stating the purpose of the study, a pre-addressed, stamped return envelope and a postcard. The physicians were requested to either fill out the written survey or were given the option to complete the survey online at a designated website location, as an option to the written questionnaire. A second wave of surveys, accompanied by a reminder letter, was sent after 3 weeks. Additionally, 1 week after the second mailing, randomly selected non-respondents received an email or telephone call to request the physician to complete the survey.
Analysis
Data were analyzed using SPSS statistical software (SPSS; Chicago, IL, USA; www.spps.com). Univariate analysis described physicians' current practices, attitudes toward geriatric depression, experienced barriers and needs to improve the diagnosis and treatment of depression in the geriatric population. Chi-square tests, independent t-tests and F-tests, as appropriate, were used to assess possible differences in physicians' responses related to the demographic variables of age and sex, and the practice characteristic of proportion of elderly patients in the physicians' patient panels.
Results
A total of 76 rural primary care physicians (47%) responded to the survey. Demographic and practice characteristics of the responding physicians are presented (Table 1). More than 90% of responding physicians were family doctors. Most were male (59.2%) and the mean age was 40 years (SD = 10.2).
Table 1: Demographic and practice characteristics of responding rural primary care physicians
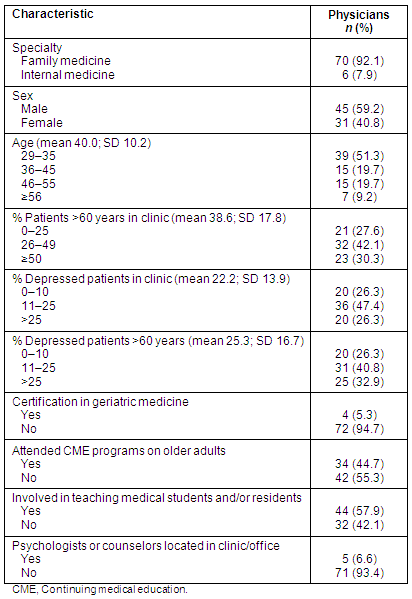
Thirty percent of the doctors reported practices where over 50% of their patients were older adults (over the age of 60). In response to the question 'About what percent of your patients do you estimate to be depressed?' most physicians (47.4%) estimated the percentage of depressed patients in their practices as 25% or less, but over one-quarter reported greater than 25% depressed patients. The figure increased to approximately one-third for depressed patients over the age of 60. There was a strong correlation between overall estimate of depressed patients in the physicians' practices and percentage of older adults with depression (r = .80; p <.001).
Nearly 45% of the physicians indicated having attended continuing medical education programs relating to older adult healthcare within the past year. And almost three-fifths of the physicians were involved in teaching medical students and/or residents. In terms of building mental health capacity within their own practices, five physicians (6.6%) indicated that psychologists or counselors were on-site in their clinics, and four physicians (5.3%) were certified in geriatric medicine.
Physician practices in depression screening and treatment: All responding physicians indicated they routinely screened for depression in their older patients. Information is presented on the symptoms these rural primary care physicians used in conducting screenings, as well as tests or interviews in the diagnosis of depression in older adults (Table 2). Six symptoms were identified by 90-100% of the physicians as used in screening for depression in their patients: sad mood; loss of interest/pleasure; decreased energy; anxiety/irritability; sleep disturbance; and multiple worries/distress. The symptom least often mentioned in relation to depression screening was pain (45%). On average, the physicians indicated approximately 9 symptoms considered in the screening and diagnosis of depression in older patients.
Table 2: Rural physicians' reported practices in the screening and diagnosis of depression in older adults
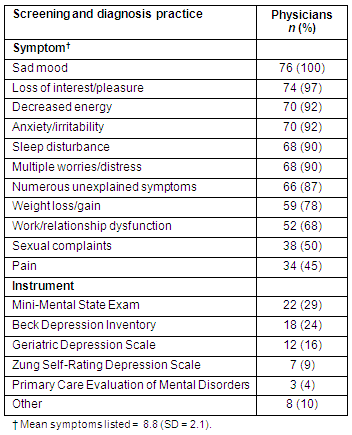
Sixty-one percent of the primary care physicians reported that they did not use a standard test or screening instrument for depression diagnosis. When a depression assessment instrument was used, most often mentioned was the Beck Depression Inventory (24%), followed by the Geriatric Depression Scale. The Mini-Mental State Exam (29%) was also commonly used to evaluate geriatric patients.
In establishing a new diagnosis of depression in elderly patients, laboratory tests most often used to screen for causes other than depression were for thyroid stimulating hormone (84%), a complete blood count (75%) and a comprehensive metabolic profile (41%). Specific medications most often mentioned in the treatment of depression were escitalopram (47%) and sertraline (30%). Besides medications, counseling was reported by the majority of physicians (80%) as another treatment modality. Exercise (12%), social activities (7%) and psychotherapy (7%) were mentioned considerably less frequently.
When asked 'Do you use clinical guidelines for diagnosis and treatment of geriatric depression?' 10 of the primary care physicians (13%) responded yes. Forty percent of the doctors indicated that they routinely gave patient education materials to those suspected of being depressed or diagnosed with depression. When asked about a gap between the treatment physicians preferred and availability of that treatment, 45% somewhat or strongly agreed that a gap existed. To some extent this view was related to the age of the patient panel, where primary care physicians with higher proportions of patients aged 60 years and older were more likely to agree that there were gaps between available and preferred treatment of depression in older adults (42.3% vs 35.1% of patients >60; p = .081).
Physician attitudes towards depression diagnosis and management: As presented (Table 3), all of the rural physicians agreed that helping depressed patients was important to them. Further, nearly all the physicians (99%) agreed that they felt confident in accurately diagnosing depression in the elderly. This confidence carried over into diagnosis and treatment of depression and prescription of antidepressants in the elderly, with 97% and 89% of physicians, respectively, reporting confidence in their abilities in these areas. Consistent with these perceptions, all the physicians agreed that diagnosis and treatment of depression in elderly patients was their responsibility as primary care doctors. Additionally, 92% of the physicians agreed that treating depressed patients is an aspect of practicing medicine that is rewarding, and no physician agreed with the statement that there is nothing that can be done for older patients with depression. In this regard, 96% of the physicians agreed with the view that elderly patients expect primary care physicians to deal with depression in their patients.
Table 3: Rural physicians' attitudes and perceptions regarding the diagnosis and treatment of depression in older adults
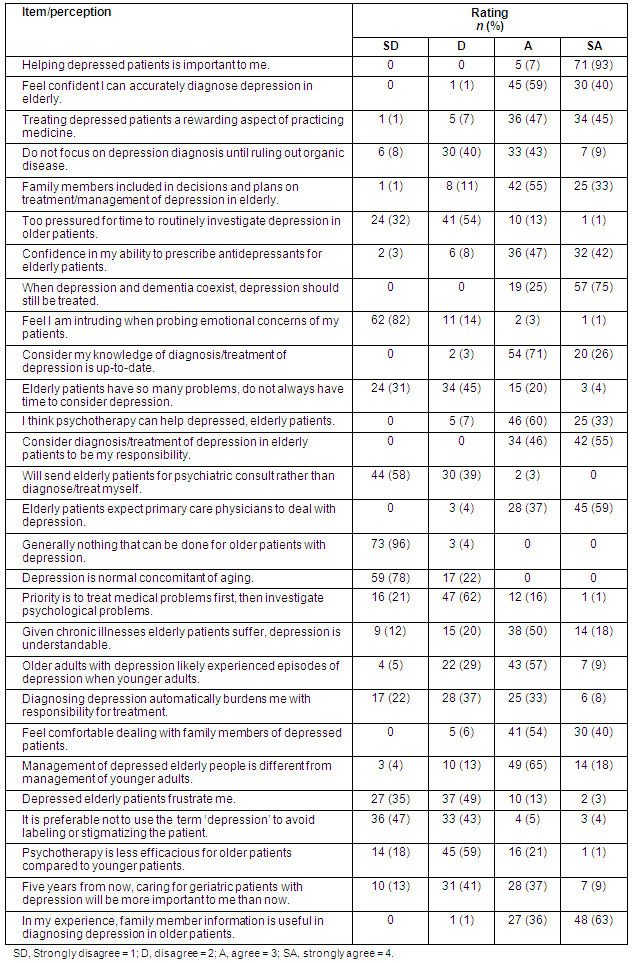
Eighty-six percent of the rural physicians disagreed that they were too pressured for time to routinely investigate depression in their older patients, including 32% who strongly disagreed. Similarly, 76% disagreed that elderly patients have so many problems that the physician does not always have time to consider depression. For the most part, the primary care physicians disagreed that depressed, older patients frustrated them (84%). Ninety percent of the physicians disagreed that it is preferable not to use the term depression because it potentially labels or stigmatizes the patient. Finally, only 3% of physicians agreed that they would send elderly patients for a psychiatric consult, rather than diagnose and treat depression themselves.
In relation to attitudes toward treatment modality as well as involvement of family members, 93% of the physicians felt that psychotherapy can help depressed elderly patients. The physicians also tended to disagree (77%) that psychotherapy is less efficacious for older, compared with younger, patients. The majority of the physicians (94%) felt comfortable dealing with family members of depressed patients, with 99% indicating that family member information was useful in the diagnosis of depression in older adults. Consequently, 88% of the rural doctors agreed that family members should be included in decisions and plans about the treatment and management of depression in their elderly patients.
Overall, related to physicians' attitudes and perceptions, there was a mixed reaction to caring for older patients with depression currently, compared with 5 years in the future. Over half (54%) disagreed that in 5 years, caring for elderly patients with depression would be more important than at present.
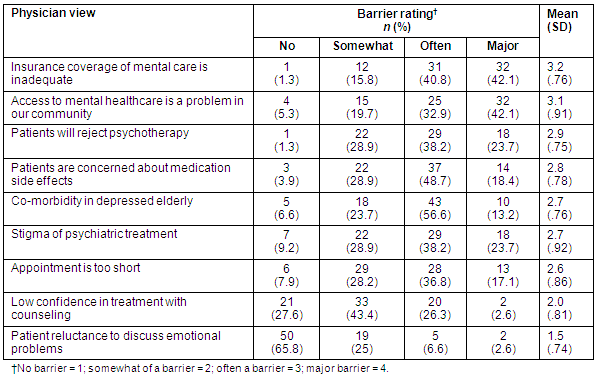
Physician reports on barriers to care and views on improving ability to care for depressed, geriatric patients: Physicians were asked to respond to a list of 9 possible barriers to the diagnosis and treatment of geriatric depression by indicating the extent to which each was perceived as a barrier. Results of the physicians' assessments are presented (Table 4). Most likely to be viewed as barriers to diagnosis and treatment of geriatric depression were inadequate insurance coverage for mental healthcare and lack of access to mental healthcare in the community (both with a mean score >3 on a 4 point scale). These two most often reported factors reflect access or system-level obstacles to care. On the individual side, approximately 62% of the physicians agreed barriers to diagnosis and treatment of geriatric depression could be patients' rejection of psychotherapy and perceptions of the stigma associated with psychiatric treatment in general. Least likely to be viewed as barriers in depression diagnosis and care were: low confidence by the patient in treatment involving counseling, and the patient's reluctance to discuss emotional problems (with mean scores of 2 and 1.5, respectively).
Table 4: Rural physicians' views of potential barriers to adequate diagnosis and treatment of geriatric depression
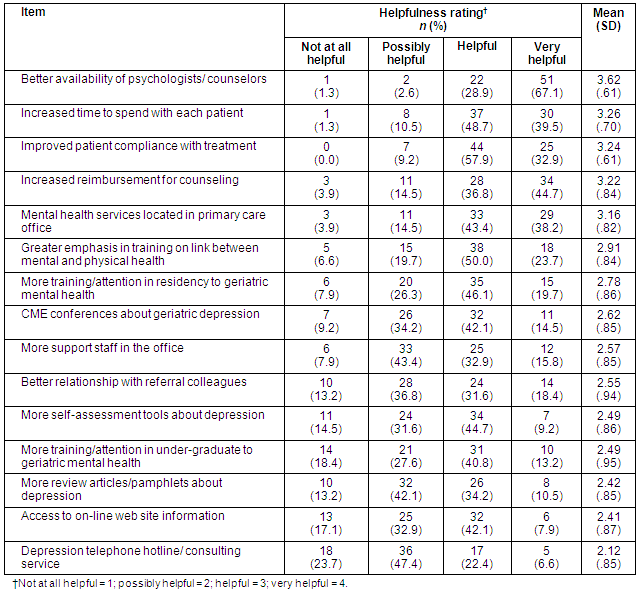
Future needs and directions in the care of older, depressed patients were assessed by physician responses to a list of 15 items that could be helpful in improving their ability to care for depressed, geriatric patients. All but three of the responding physicians agreed that it would be helpful or very helpful to have a better availability in rural areas of psychologists and counselors for improving care for older patients with depression (Table 5). This was followed most closely by increased time to spend with patients, improved patient compliance with treatment and increased reimbursement for counseling services. Also highly evaluated in terms of helpfulness for patients was location of mental health services in primary care offices. At the level of physician education, evaluated as potentially helpful were: greater emphasis in training on the link between mental and physical health; greater emphasis in residency training on geriatric mental health; and availability of continuing medical education conferences on geriatric depression. Better relationships with referral colleagues was interesting in terms of distribution of responses - 50% of the physicians, respectively, reported that better referral relationships would be not at all/possibly helpful versus helpful/very helpful. Viewed as least helpful in patient care was the availability of telephone hotline or consulting services.
These needs and directions (Table 5), were examined in relation to the earlier question of primary care physicians' views of a possible gap between available care in the rural setting and preferred treatment practices by the physicians. Physicians who responded that they agreed there was a gap between available and preferred treatments were also more likely to indicate: there should be better availability of psychologists and counselors (p = .003); there should be greater emphasis during training on the link between physical and mental health (p = .021); and there should be increased reimbursement for counseling (p = .057).
Table 5: Rural physicians' views of items potentially helpful in improving ability to care for geriatric patients with depression
Attitudes and reports of behavior by physician age, gender and proportion of patient panel 60 years and older: Also examined were physicians' reported practices and perceptions and attitudes by age (physicians less than or equal to 49 years vs greater than 50 years), sex and patient panel age (5-35% less than 60 vs 40-85% greater than or equal to 60). Younger physicians reported higher estimates of patients in their panel who were depressed: 24.4% vs 15.6% (p = .002). They were also somewhat more likely than older physicians to indicate that they could be too pressured for time to routinely investigate for depression in older adults (p = .043). However, older physicians were more likely to state that: family members are included in decisions and plans on the treatment and management of older adult depression (p = .034); inadequate insurance coverage can be a barrier to mental health care in rural areas (p = .019); and there is a need for increased time to spend with patients to improve care for older adults with depression (p = .008).
In relation to gender, female physicians, compared with males, reported higher rates of depressed patients in their practices: overall, 31% compared with 16.1% (p <.001) and with respect to geriatric depressed patients, 33.2% compared with 19.9% (p < .001). While males were more likely to report patient rejection of psychotherapy as a barrier to care (p = .016), females were more likely to view patient reluctance to discuss emotional problems as a barrier (p = .014). Finally, males were more likely to indicate that a better availability of psychologists or counselors was a need in improving care in rural areas (p = .047).
Possible variations in reports of attitudes and care delivery were, additionally, examined in relation to proportion of elderly patients in the physicians' practices. Those rural physicians with proportionately more older patients in their practices, on average, checked more needs and directions for improving their ability to care for older adult patients, 10.3 vs 8.8 (p = .056). These physicians were also more likely to: feel that more training/attention in residency to geriatric care would be helpful in improvement of care (p<.001); indicate the need for greater emphasis in and training on the link between physical and mental health (p = .041); and mention that better availability of psychologists and counselors would be important for the improvement of care for older, depressed patients (p = .020).
Discussion
This study contributes to the recent call by the American Geriatrics Society to understand how primary care physicians diagnose and treat depression in older adults, with a specific focus on rural primary care physicians21. Responding primary care doctors in Illinois reported higher averages of their older patient panels suffering from depression than is indicated in the existing literature: 33% compared with 23%3,4. By sheer numbers alone, the need is reinforced for better understanding the diagnosis and treatment of older, depressed adults.
There are many positive outcomes in this study of rural primary care physicians. All responding physicians indicated routine screening for depression in their older patients. While the majority of physicians did not indicate the use of specific instruments or inventories for depression assessment, they reported a range of symptoms addressed in depression diagnosis (average = 8.8), and two-fifths provided patients with educational materials related to depression. Approximately one-quarter of the physicians used the Beck Depression Inventory in their geriatric assessments.
Interestingly, just 13% of the rural physicians responded that they used clinical guidelines in diagnosis and management of depression. At first glance, this seems low. However, this finding is consistent with the depression clinical guidelines research of Feldman and colleagues who found that while 90.5% of primary care physicians treated depression, only 13.1% reported having a copy of depression guidelines30. Perhaps more importantly, nearly 45% of the physicians had attended continuing medical education programs focused on the health needs of older adults. Related to Feldman et al.'s analysis, the rural physicians in our study appeared to have the 'content knowledge' important for geriatric depression diagnosis and care.
Our study does indicate areas for future attention. First, while being willing to take on depression in the elderly in rural primary care (all physicians agreed that diagnosis and treatment of depression in older patients was their responsibility as primary care doctors), the physicians themselves provided ample indications that there are ongoing needs to be addressed in this area of primary care. In comparing available versus ideal treatment, nearly half the rural physicians reported a gap between their preferred treatment and the availability of treatment for their older patients. It will be important to identify what rural primary care physicians specifically refer to as gaps in care.
Second, the physicians identified a number of needs or directions in depression care, diagnosis and treatment. Most important was better availability of psychologists and counselors for attending to the needs of older depressed rural people. This was particularly emphasized by male physicians and those with higher proportions of older patients in their practice. Perhaps not surprisingly, more time to spend with patients was also mentioned as a major need in depression-related care. These are system-level factors that, if addressed, could potentially improve the mental healthcare of the rural elderly.
The challenges of time could potentially be addressed through interprofessional interventions and taking a team approach to the treatment and management of depression in older adults. Certainly, this may be more difficult in rural areas where access to healthcare professionals remains a concern. But models of care might include those similar to the primary care or patient-centered medical home, in which physicians work in a team environment to address the diverse healthcare needs of their patients31
An important message to the health education community provided by the primary care physicians in this study was the potential role of teaching in preparing physicians to address geriatric depression, as well as other mental health issues. In addition to other recommendations related to access and availability factors in geriatric mental health, the responding physicians indicated there could be greater emphasis in their training on the link between mental and physical health. One aspect of this could be more training or attention in residency on geriatric mental healthcare awareness and practices.
A possible limitation of the study is that while it had a respectable response rate for a physician survey, still less than 50% of physicians in the sampling frame responded to the study questions. It is possible that a more positive picture of physician attitudes and experiences was obtained if physicians less positive in attitude and less sure of their care opted to not respond to the survey. The responses also reflect reports of attitudes and experiences, rather than observations or chart reviews. However, our response rate is consistent with past research on physician attitudes and practices32, and we are able to provide information on an often under-examined group of physicians in the realm of mental healthcare delivery33. With respect to the latter, the study is responsive to the conclusion of a recent Lancet editorial stating 'Mental health must be one of the key priorities in any country's clinical and public health agenda'34. Overall, the study has identified the types of barriers primary care physicians experience in their diagnosis and treatment of geriatric depression, and has demonstrated a need for more attention to be directed to this important topic in rural healthcare delivery.
Acknowledgements
The authors acknowledge support for this research from a contract between the National Center for Rural Health Professions, Rockford, Illinois, and Maastricht University, The Netherlands, and funding from the National Center on Minority Health and Health Disparities, National Institutes for Health (NIH; Project EXPORT P20 MD000524). The article contents are solely the responsibility of the authors and do not necessarily represent the official views of NIH.
References
1. Worley H. Depression: a leading contributor to global burden of disease. Population Reference Bureau. (Online) 2006. Available: http://www.prb.org/Articles/2006/DepressionaLeadingContributortoGlobalBurdenofDisease.aspx (Accessed 12 November 2009).
2. Chapman DP, Perry GS. Depression as a major component of public health for older adults. Prevention and Chronic Disease 2008; 5: 1-9.
3. Glasser M, Stearns JA, de Kemp E, van Hout J, Hott D. Dementia and depression symptomatology as assessed through screening tests of older patients in an outpatient clinic. Family Practice Research Journal 1994; 14: 261-272.
4. Licht-Strunk E, van der Kooij KG, van Schaik DJF, van Marwijk HWJ, van Hout HPJ, de Haan M et al. Prevalence of depression in older patients consulting their general practitioner in The Netherlands. International Journal of Geriatric Psychiatry 2005; 20: 1013-1019.
5. Beekman ATF, Geerlings SW, Deeg DJH, Smit JH, Schoevers RS, de Beurs E et al. The natural history of late-life depression. A 6-year prospective study in the community. Archives of General Psychiatry 2002: 59: 605-611.
6. Cuijpers P, van Straten A, Smit F. Psychological treatment of late-life depression. International Journal of Geriatric Psychiatry 2006; 12: 1139-1149.
7. Gum AM, Arean PA, Hunkeier E, Tang L Katon W, Hitchcock P, Steffens DC et al. Depression treatment preferences in older primary care patients. Gerontologist 2006; 46: 14-22.
8. Alexopoulos GS. Depression in the elderly. Lancet 2005; 365: 1961-1970.
9. Unutzer J, Katon W, Callahan CM. Collaborative care of late-life depression in the primary care setting: a randomized controlled trial. JAMA 2002; 288: 2836-2845.
10. Gilbody S, Whitty P, Grimshaw J, Thomas R. Educational and organizational interventions to improve the management of depression in primary care. JAMA 2003; 289: 3145-3151.
11. Beekman AT, Deeg DJ, Braam AW. Consequences of major and minor depression in later life: a study of disability, well-being and service utilization. Psychological Medicine 1997; 27: 1397-1409.
12. Charney DS, Reynolds CF, Lewis L. Depression and bipolar support alliance consensus statement on the unmet needs in diagnosis and treatment of mood disorders in late life. Archives of General Psychiatry 2003; 60: 664-672.
13. Burroughs H, Lovell K, Morley M, Balwin R, Burns A, Chew-Graham C. 'Justifiable depression': how primary care professionals and patients view late-life depression? Family Practice 2006; 23: 369-377.
14. Murray CJ, Lopez AD. Evidence-based health policy - lessons from the global burden of disease study. Science 1996; 274: 740-743.
15. Adelman RA, Greene MG, Friedmann E, Cook MA. Discussion of depression in follow-up medical visits with older patients. Journal of the American Geriatric Society 2008; 56: 16-22.
16. Jeste DV, Alexopoulos GS, Bartels SJ. Consensus statement on the upcoming crisis in geriatric mental health: research agenda for the next two decades. Archives of General Psychiatry 1999; 56: 848-853.
17. Rost K, Fortney J, Mingliag Z, Smith J, Smith GRS. Treatment of depression in rural Arkansas: policy implications for improving care. Journal of Rural Health 1999; 15: 308-315.
18. Harman JS, Veazie PJ, Lyness JM. Primary care physician office visits for depression by older Americans. Journal of General Internal Medicine 2006; 21: 926-930.
19. Williams JW Jr, Rost K, Dietrich AJ, Ciotti MC, Zyzanski SJ, Cornell J. Primary care physicians' approach to depressive disorders. Archives of Family Medicine 1999; 8: 58-67.
20. Menchetti M, Cevenini N, De Ronchi D, Quartesan R, Berardi D. Depression and frequent attendance in elderly primary care patients. General Hospital Psychiatry 2006; 28: 119-124.
21. Reynolds CF 3rd, Cruz M, Teh CF, Rollman BL. Improving evidence-based management of depression for older Americans in primary care: If not now, when? Journal of the American Geriatr Soc. 2007; 55: 2083-2085.
22. Petterson SM. Metropolitan-nonmetropolitan differences in amount and type of mental health treatment. Archives of Psychiatr Nursing 2003; 17: 12-19.
23. Rosenblatt RA. A view from the periphery - health care in rural America. New England Journal of Medicine 2004; 351: 1049-1051.
24. Singh GK, Siahpush M. Increasing rural-urban gradients in US suicide mortality, 1970-1997. American Journal Public Health 2002; 92: 1161-1167.
25. Probst JC, Laditka SB, Moore CG, Harun N, Powell P, Baxley EG. Rural-urban differences in depression prevalence: implications for family medicine. Family Medicine 2006; 38: 653-660.
26. Badger L, Robinson H, Farley T. Management of mental disorders in rural primary care: a proposal for integrated psychosocial services. Journal of Family Practice 1999; 48: 813-818.
27. Wang JL. Rural-urban differences in the prevalence of major depression and associated impairment. Social Psychiatry and Psychiatric Epidemiology 2004; 39: 19-25.
28. Fortney J, Rost K, Zhang M, Warren J. The impact of geographic accessibility on the intensity and quality of depression treatment. Medical Care 1999; 37: 884-893.
29. Glasser M, Gravdal JA. Assessment and treatment of geriatric depression in primary care settings. Archives of Family Medicine 1997; 6: 433-438.
30. Feldman EL, Jaffe A, Galambos N, Robbins A, Kelly RB et al. Clinical practice guidelines on depression: awareness, attitudes, and content knowledge among family physicians in New York. Archives of Family Medicine 1998; 7: 58-62.
31. Rosenthal TC. The medical home: growing evidence to support a new approach to primary care. Journal of American Board of Family Medicine 2008; 21: 427-440.
32. Asch DA. Response rates to mail surveys published in medical journals. Journal of Clinical Epidemiology 1997; 50: 1129-1136.
33. Steinman LE, et al. Recommendations for treating depression in community-based older adults. American Journal of Preventative Medicine 2007; 33: 175-181.
34. Anon. Movement for global mental health gains momentum. Lancet 2009. 374: 587. (Editorial)
_____________________________
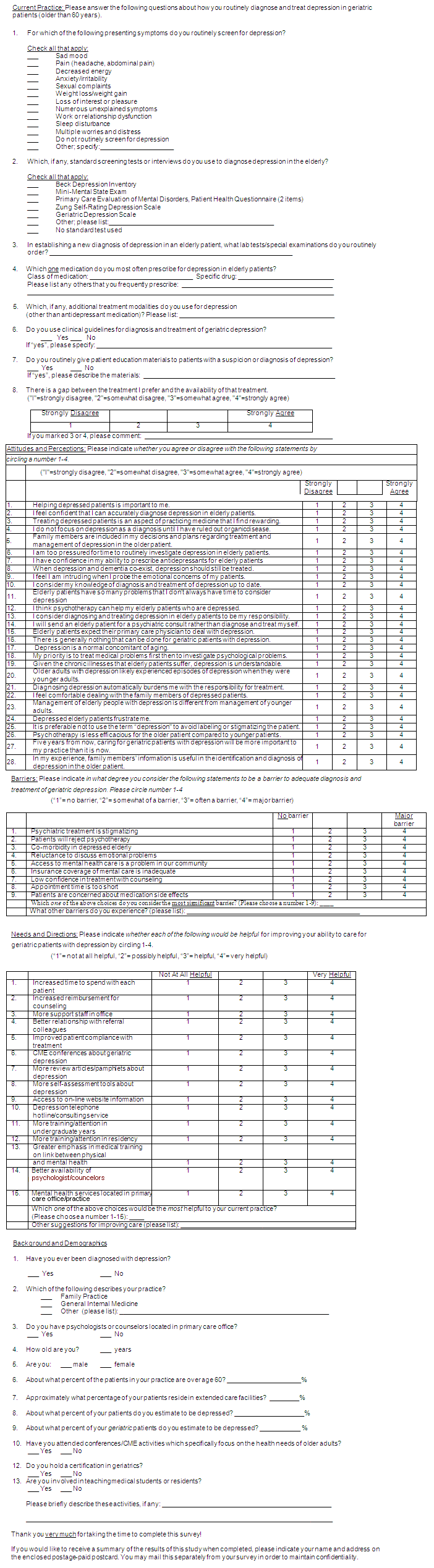
Appendix I: University of Illinois College of Medicine at Rockford physician survey: geriatric depression in primary care