Introduction
The need to understand health human resources has become increasingly evident at the international and Canadian national and provincial levels. Every province has acknowledged the importance of research that focuses on rural health workforce issues in Canada1. Vacancies in health occupations increase wait times, modify delivery approaches, change the roles of personnel, decrease frequency of service, influence service cancellations, and change service eligibility criteria2. The quality and frequency of health services are dependent on the size, skill, commitment and availability of the health workforce3.
New health education programs with the goal of attracting students more likely to stay and practice in rural and northern areas of Canada are opening up across the country4. Educators and health administrators are increasingly interested in identifying factors associated with the selection and maintenance of rural and northern practice. Most studies about factors that contribute to professionals choosing rural practice have concerned physicians5-6, a few have concerned nurses7-8, and even fewer have addressed allied health professionals9-10. Much of the literature has focused on students or new graduates and their perceptions of rural practice4,8-21. Little research has considered the perspective of professionals who have stayed in rural practice11.
The study reported here examined the factors and experiences that health professionals who have practiced in northern BC long term identify as influential in their choice to pursue rural training, initiate rural practice, and remain in rural practice. The primary objective was to identify the personal characteristics and experiences shared by health professionals across disciplines who have worked long term in northern BC. The following questions were addressed:
- What factors were important when choosing rural training?
- What factors influenced decisions to choose a rural or northern community as a work destination and stay long term?
- What personal characteristics and experiences are shared by these healthcare professionals?
Background
The recruitment and retention of healthcare professionals in northern BC has been and continues to be a struggle22. Consumers in northern BC's health region claim the vacancies and turnover of healthcare professionals in their region have negative effects on the care they receive in their communities23. In response to staffing issues, several recruitment incentive programs, including scholarships and signing bonuses, have been used to attract healthcare professionals.
The University of Northern British Columbia (UNBC) has introduced training programs such as the Northern Medical, Nursing, and Social Work Programs in response to research that repeatedly suggested rurally-trained students are more likely to practice in a rural area4,8,14-20. The application process for the Northern Medical Program includes an assessment of rural suitability in an attempt to admit students likely to practice in the region after graduation15. Little is known about the allied health workforce in BC and it would be helpful to understand if their assessable rural suitability factors are similar to those of medical applicants.
There has been significant research into the contributing influences for physicians taking up rural practice. For example a systematic review of the influence of 'rural exposure' on medical students' uptake of rural practice in Australia21 found that training environments, including curriculum and residency, influenced new graduates' rural practice decisions. However, inconsistencies throughout the literature have been highlighted pertaining to how specific characteristics of rural training, such as length, frequency, timing, and level (undergraduate or graduate) affect the uptake of a rural career21. The Australian study emphasized the need to examine specific aspects of the rural experience within education programs21, because the role of rural exposure inconclusive. Similar research related to factors contributing to other rural healthcare providers taking up rural practice is scarce24-26.
A high turnover of health professionals in the rural and northern Canadian health sectors emphasizes the need to identify factors associated with professionals staying in rural and northern practice. In addition, many health education programs have limited places and competitive application processes. An assessment of the factors associated with choosing rural training, rural practice and the reasons for staying in rural or northern practice would assist screening for entrance to allied health professional education programs. Exploring the personal characteristics of a variety of allied health professionals who have practiced in rural and northern communities long term would inform recruitment and education program selection for health professions such as clinical psychology, physiotherapy, occupational therapy, speech language pathology and social work.
Context of the study
The geographic region targeted in this study was the northern two-thirds of BC, for which there is one regional health authority, Northern Health, and a northern university, UNBC. Northern BC covers approximately 650 000 km2 and contains approximately 300 000 people, with only one community of greater than 50 00027. Some allied health professionals such as social workers, physiotherapists, occupational therapists and speech language pathologists work in each of the three sub-regional areas (Northwest, Northern Interior, and Northeast). Other allied health professionals, such as psychologists, work in the regional centre Prince George and provide services across the region.
The literature pertaining to health human resources uses various definitions of 'northern' and 'rural' at different levels of analysis28,29. The longstanding debate regarding what constitutes 'rural', 'northern' or both, concerns the fact that some definitions are based solely on geographical boundaries, while others use social representation, and others a mixture of both28. The term 'rural' is usually related to population size, density, level of isolation, economic/industrial base of the community, as well as access to healthcare professionals, resources, and services30. The term 'northern' usually encompasses a combination of characteristics including remoteness, lack of healthcare services, and hardship31, which can include a sense of place created 'culturally, economically, and geographically' (p. 376)29. No standard definition of 'rural' or 'northern' was used in the present research. Rather, the definitions and terms of cited sources and participants were retained.
Methods
The study used a qualitative descriptive design32.
Participants
The participants were 26 allied health professionals who had practiced long term in northern BC. Participants belonged to health professions that have been considered or are offered as health education programs at UNBC: physiotherapy, psychology, occupational therapy, social work, and speech language pathology. The recruitment of participants commenced in November 2007 with a convenience sample drawn from the researchers' professional contacts and networks. Nine participants were recruited in this manner. Fifteen others were recruited using the snowball technique33.
Potential participants who volunteered to be interviewed were telephoned for an initial consultation to determine interview eligibility. The volunteers were asked to identify the region within northern BC in which they lived, how long they had worked as a health care professional in northern BC, and where they planned to work in the future. Only volunteers who had worked in the region for more than 4 years and who planned to continue working in northern BC were asked to participate. Efforts were made to recruit approximately five volunteers living and working in each sub-regional area to represent the geographic distribution of BC's northern population. The initial consultation ensured that a variety of types of professionals were recruited to participate in the interviews. Participants who met eligibility criteria were asked to participate in a telephone interview.
Data collection
Data were collected through semi-structured telephone interviews that lasted on average 35 min. The interviewer (first author) asked direct questions to identify demographical information, and open-ended questions (such as 'What was important in your decision to start working in northern BC?' and 'What is important in your decision to continue working here?') to explore the motivating influences for choosing rural or northern training, northern BC as a work destination, and for remaining in the area long term. The interviews were audio recorded.
Data analysis
The interviews were transcribed verbatim using Express Scribe software (NCH Software; Greenwood Village, CO, USA) and a thematic content analysis using a qualitative descriptive approach was carried out by the first author to identify common phrases or comments that pertained to personal experiences, characteristics, and the decision to begin or stay working in northern BC34. Transcribing the majority of the interviews personally as they were completed allowed the first author to review the data, begin the constant comparative method of analysis, become familiar with the core consistencies, and elaborate on those consistencies in the subsequent interviews. Interviews were used to clarify, expand, and extend themes found in the literature review and the preceding interviews. Saturation was reached with the 26 interviews.
Rigor and ethics
Rigor was addressed by extensive 'member checking', comparing findings with previous literature, and an external audit33. Member checking was undertaken via an email presentation with notes to each participant for feedback and validation. An external audit was performed by a rural clinical psychologist in the rural psychology internship rotation and rural psychology postdoctoral residency at the University of Manitoba. The auditor was asked to review the analysis process, 10 of the 26 interview transcripts, the presentation sent to participants for validation, and the final report. She validated the process using external audit questions based on Creswell (p.253)33. These measures helped to overcome the potential methodological limitations of retrospective reporting and recall bias33, the reactivity of the interviewee to the interviewer33, and selective perception of the data33.
Ethical approval for this study was sought and received from UNBC. Due to the small sample size and the limited number of people occupying the selected health care professions in northern BC, it was important to be particularly attentive to issues of confidentiality. Therefore the contexts of quotes are not provided, quotes are anonymous and potentially identifying information has been disguised.
Results
Demographics
Six speech language pathologists (27%), four clinical psychologists (15%), four occupational therapists (15%), eight social workers (31%), and four physiotherapists (15%) agreed to participate in the study. This included seven participants (27%) living in the Northwest, 13 participants (50%) living in the Northern Interior, and 6 participants (23%) living in the Northeast sub-regions. This sample was representative of the population's geographic dispersion. Eleven participants (42%) were from the regional center of northern BC, the only community with a population of over 50 000, but many of these professionals provided services to surrounding rural communities. The participants came from a variety of rural and urban backgrounds; approximately one-third came from a hometown with a population of less than 10 000 people.
Most participants were married or living with a partner at the time of the interview. Nearly every one of these participants reported their spouse was satisfied with their community and had career opportunities in a rural or northern community. Most participants had children and almost all claimed their children were satisfied with their community.
Only 11% of the participants had parents or spouse's parents living within 50 km at the time of the interview. Most of their parents lived elsewhere in BC. However, 42% of the participants had other extended family members living in northern BC. A full summary of participants' demographic characteristics is given (Table I).
Table 1: Summary of participants' demographic characteristics
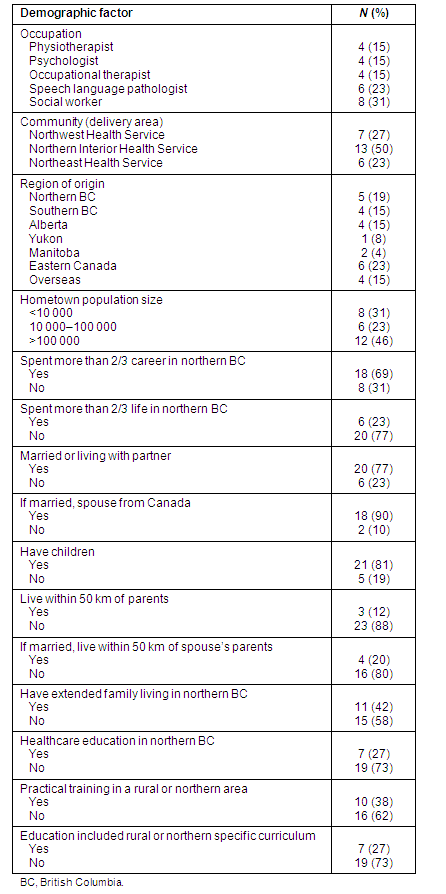
Rural or northern education
Seven participants (27%) received their healthcare education in northern BC. Some indicated they chose their profession because the program was available in the region where they lived.
I was already living in the region and basically I chose a program that I could complete in northern BC that I wouldn't have to relocate to do. So, my choice of profession is based on what was offered....
All participants who did their practical training or learned about rural health issues during their education had already decided they were probably going to work in a rural or northern setting before taking part in the rural education component. Nonetheless, the participants who completed rural or northern training suggested that the training helped to prepare them for their employment.
Practicum in rural areas gave me an idea of what I needed to be successful in rural areas. It really helped me to know what I needed to ask from my employer to be successful before I even started.
Recruitment influences
Participants identified personal background, professional, individual, and community factors that were important in their decision to choose a rural or northern area as a work destination. Many participants mentioned past positive experiences in rural or northern communities when discussing their reasons for choosing a rural or northern area as a work destination. A number suggested that growing up in a rural or northern community was significant in their decision to choose the region. A few named their spouse's rural community of origin, having family in the region, and wanting to raise children in the area as impacting on their decision to come to a rural or northern community, while others suggested getting away from their family as their reason.
I have joked and said that I have put a mountain range between me and my parents [laugh], but I wasn't escaping them. Rather, I was exerting my independence.
Financial incentives are one of BC's main recruitment techniques29. However, only a couple of the participants named financial incentives as important in their decision to work in a rural or northern area. Participants identified the need for healthcare professionals and career advancement opportunities.
I think the most important was that I would be going to a community that needed my services... So that I would have, I mean, opportunities to be of assistance to people who needed services, but that I would be able to establish a private practice that would have meaning for me.
Other major motivators included guarantees of continuing education and possibilities for interprofessional teamwork. Participants also discussed the importance of welcoming, helpful employers during the interview process and promises of peer support.
In [an urban center], there is quite a competition thing that goes on because of course, it is a larger center, people are very territorial about their clients, their contracts and stuff. Here, I mean, the response I got when I asked questions [about moving here] was that nobody was threatened. Everyone was eager for me to come and offered all kinds of information and assistance that I would have never received.
Professional preferences for variety, challenges, and trying new aspects of the job, such as teaching, also impacted on their decision.
Several individual factors and personal preferences were also influential in participants' decisions to work in a rural or northern community. The need for adventure was one of the most mentioned motivators: 'It wasn't the money that drove me. It was the adventure!' Love of the wilderness and outdoor recreation were also identified. In addition, community factors such as the friendliness of the people, low real estate prices, and the slow pace of living. Many discussed how the quality of life allowed them more money and time for vacations and recreation. Many of these factors were also identified as influential in retention.
Retention influences
A handful of participants had come to work in a rural or northern community with the idea of obtaining a few years experience and moving on. However, every participant eventually decided to stay in the region long term. Participants identified several aspects of the community, the job, and the region itself when describing why they had decided to remain. Similar to influential recruitment factors were personal background, professional factors, individual factors and community factors that all had varying levels of impact on professionals' eventual decision to stay working in a rural or northern community.
Although some participants identified past positive experiences in rural and northern communities and rural upbringing as influential in retention, the larger motivation appeared to staying close to family, such as children and grandchildren.
Well, number one is my family. My daughters are here and my grandchildren are here. And we are pretty close grandparents, my wife and I, so that is one of the main motivations to stay here now.
Of the most common retention factors were the need for professional services in northern communities, and the career opportunities for both the healthcare professional and their spouse. Many participants discussed the opportunity to become a sole practitioner and the chance to grow within their career. Several participants discussed the managerial support, training and continuing education opportunities provided by their employer that influenced their choosing to remain in a rural or northern community.
There were just a lot of opportunities for training. So, that was a big, big benefit for me; a reason for me to stay. Um... That I didn't feel like a lone ranger out here without a lot of support for learning the position. I was able to do lots of courses in Vancouver and in the United States. I did some mentorship stuff with one of the occupational therapists in [small community] and did a couple of courses in [regional centre]. In my first couple of years, I got a lot of support and a lot of training. That definitely gave me a strong foundation.
Almost half the participants mentioned the importance of peer support in their decision to stay. Job satisfaction and factors that influenced job satisfaction were the most important professional factors influencing retention.
A commitment to the community and community-based work were also highlighted. Community satisfaction, getting involved in the community, appreciating the activities the community has to offer, and the quality of life found in the north were all identified as factors influencing decisions to stay. One of the major themes was how the affordability of living in a rural or northern community allowed more time to spend with family. This differed from recruitment motivators, being more focused on family and less on vacations and recreational activities, suggesting a change in values.
Feelings of belonging to a community, familiarity, and knowledge of people in the community were identified as retention factors that developed over time. Many participants mentioned the friendliness of the people in their community as a major factor in their decision to stay. Participants suggested that northern people are friendly, welcoming, and 'make you feel comfortable'. Most participants did not have friends in the region when they arrived, but many developed close friendships over time, which influenced them to stay long term. The desire to know the people in their community was also highlighted as having a positive impact on retention.
When I walk down Main Street, I know everyone. People talk. It is a feeling of community that I would not get in a big city. That is a reason that I have stayed.
Similar to the reasons for coming to work in a rural or northern community, adventure, a love of the wilderness, and outdoor recreation were all named as factors influencing retention. More than a few participants discussed the appreciation of rural or northern lifestyle as key to their decision to continue working in the north. They explained the 'slow pace' and 'relaxed' lifestyle helped them to stay in their community. Others developed a 'Northerner' identity over time, which impacted on their decision to stay.
I am a Northern girl! I don't like the Lower Mainland. I love the people here. I like the weather. I enjoy the resourcefulness of people. I enjoy the activities that we can do in the winter and in the summer. And I like our location and the size of the community. I am a Northern girl!
These findings identify several factors involved in long-term retention, and also highlight personal characteristics and experiences shared by the long-term healthcare professionals in rural and northern communities. The following section explores this further.
Characteristics
The major goal of the current study was to identify the personal characteristics and experiences shared by long-term healthcare professionals in northern BC. This sample of healthcare professionals reported a number of personal characteristics germane to working long term in the north. Most participants identified some form of rural background or exposure as integral to their long term rural or northern work. Several participants identified their own professional characteristics which included independence, confidence, flexibility, resourcefulness, and being comfortable in dual relationships.
You always have to be mindful of the overlapping relationships here. Actually, that is the biggest aspect when you are working here. You are in a fishbowl with all sorts of contacts with people that overlap. Your clients and children of clients. You have to have a mindset that is tolerant and aware of the role you are in at the time. As a professional, you have to be able to change your role. You have to have that adjustment and I do not find that difficult.
Participants often described themselves as adventurous and sociable. The results also suggest long-term rural and northern healthcare professionals value the quality of life in the region and appreciate personal time with family and friends more than money, status, prestige or material things.
I didn't want to get caught up in ... or it is not really important to me, not to feel that I had to put in 40 hours of work a week, then traveling to and from. Just not having any time for myself and not having time to do anything. It is the quality of life that is huge for me. So, even though I was single and on my own, I didn't work full time because I felt that having the extra day off to pursue learning was really more important to me. Part of that is the affordability. You can live a simple, more affordable lifestyle that will allow you to do that.
There were several similar recruitment and retention factors, which were also reflected in the personal characteristics. Nonetheless, there were important differences noted, especially across the stages of a career. The varying influence of these factors, the relationship of these factors to stages of career, and how the findings fit with the literature are now described.
Discussion
A qualitative descriptive design was used to identify factors that influenced participants' decisions to choose rural or northern training, initiate practice in the north, and remain in the region. The findings regarding education suggest the decision to practice rurally is made before students choose rural or northern training; however, previous studies have suggested that rural training makes one more likely to choose rural practice4,8,14-20. These findings of the present study may have been influenced by retrospective recall; however, they may also suggest further investigation of factors other than rural training.
The major themes unveiled by the present study suggest personal characteristics and experiences, along with age and stage of life, rural background and location of family influence personal values about family, career, personal preferences, and community. Personal values determined the decision to come to or stay in a rural or northern community.
Conceptual model for understanding rural and northern suitability
The factors influencing both recruitment and retention are not static; rather, they are fluid and changing. Personal values related to family, career, personal preferences, and community influence the decision to come and stay in northern BC. Personal characteristics and experiences help to shape these personal values and, as such, impact on duration of practice. However, personal characteristics and experiences alone do not determine either recruitment or retention. Over time and depending on stage of life, personal values change. The influence of recreational activities earlier in life may decrease as the influence of family increases later in life. For example, one healthcare professional reported initiating a practice in a northern community based on personal preference for skiing but reported that family factors had more influence over the decision to stay long term.
Rural background and the amount of time spent in a rural or northern area were found to influence personal values. The longer a healthcare professional spent in northern BC, the more that experience influenced personal values. Therefore, rural background and experience indirectly influence both recruitment and retention. This is congruent with previous research which suggests rural background has a positive impact on the retention of healthcare professionals in rural areas1,14-20. The location of family members and spousal factors, along with family values, may also influence recruitment or duration of stay, which is also in agreement with previous research20,35, although previous literature has not emphasized the type of relationship with family and how it influences recruitment or retention.
The emergent themes in this study suggest personal characteristics and experiences help shape personal values related to family, career, personal preferences, and community. The current study also suggests values evolve over time and depend on the age and stage of life. Past experiences in rural and northern areas help shape personal values. The following model depicts how age and stage of life, rural background, location of family members and personal characteristics and experiences shape personal values, which in turn affect both the decision to come to and stay in a rural or northern community.
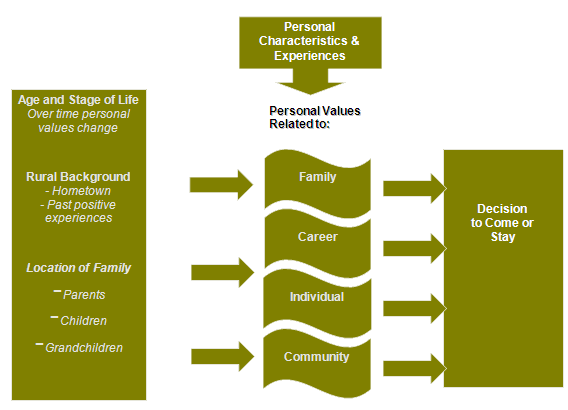
Figure 1: Conceptual model: understanding rural suitability.
This model of understanding rural and northern suitability has implications for education programs, and for employers interested in selecting, recruiting, and retaining healthcare professionals who will stay long term in rural and northern regions. The recommendation for health education programs that aim to train healthcare professionals who will practice in rural and northern areas is that such programs need to be offered in rural and northern areas so they are accessible to people who live in the region. Further, when health education programs aspire to select students who will remain in rural and northern areas, they need to consider a number of factors in relation to age and stage of life, background, location of family, as well as values.
Health education programs must address the way applicants' families and family commitments influence the environment in which they would like to work following graduation. Also important to identify are candidates' stage of career and preferred level of guidance, support, and professional autonomy. Education programs might explore applicants' preferences for variety, change, challenges and creativity. Finally, to understand the rural and northern suitability of applicants, education programs should attempt to determine personal preferences in relation to recreation, rural living, and quality of life. As in any assessment of suitability for training, such selection criteria must meet requirements for fairness and non-discrimination.
Limitations
The small number of participants limits the ability to extrapolate the findings to other settings. However, as this study was meant to be an exploratory, in-depth assessment of the influences affecting selected healthcare professionals, the in-depth data allowed for a nuanced examination of characteristics and experiences.
Conclusion
Although the research aimed to outline a number of personal characteristics and experiences shared by long-term healthcare professionals, the findings suggest there is no one factor that dictates duration of practice in a rural or northern community. Rather, a combination of varying personal values impact the decision to come to or stay. Personal characteristics and experiences help to shape these personal values but over time these change. Age and stage of life, rural background, and location of family members also have bearing on personal values, which in turn impact recruitment and retention.
Acknowledgements
The authors extend their thanks to all the healthcare professionals who participated in this study and to Dr Karen Dyck at the University of Manitoba for the external audit of this project. The authors would also like to thank Dr Glen Schmidt for his critical review of the research proposal and final thesis. Thanks are given also to Dr Karen Harlos for her helpful comments and feedback on the final thesis, as well as Nikki Logan and Kelly Stickle for their editorial support. Thanks are extended to the Michael Smith Foundation for Health Research, the University of Northern British Columbia, and the Social Sciences and Humanities Research Council of Canada for financial support of this project.
References
1. Pong RW, Pitblado JR. Geographic distribution of physicians in Canada: beyond how many and where. Ottawa, ON: Canadian Institute for Health Information. (Online) 2005. Available: http://www.cihi.ca/cihiweb/dispPage.jsp?cw_page=PG_529_E&cw_topic=529&cw_rel=AR_1346_E (Accessed 5 Feb 2009).
2. Teplitsky F. Health human resources planning in Ontario: a status report. Willowdale, ON: Central Ontario Regional Planning Group, Health Human Resources Project, 2000.
3. Poz MRD, Kinfu Y, Dräger S, Kunjumen T. Counting health workers: definitions, data, methods and global results. Geneva : World Health Organization, Department of Human Resources for Health Evidence and Information for Policy, 2006.
4. Johnson A, Fyfe T, Snadden D. Rural and remote suitability score: a review. Prince George, BC: Northern Medical Program, University of Northern British Columbia, 2006.
5. Humphreys J, Jones J, Jones M, Hugo G, Bamford E, Taylor D. A critical review of rural medical workforce retention in Australia. Australian Health Review 2001; 24(4): 91-105.
6. Eley D, Young L, Shrapnel M, Wilkinson D, Baker P, Hegney D. Medical students and rural general practitioners: Congruent views on the reality of recruitment into rural medicine. Australian Journal of Rural Health 2007; 15(1): 12-20.
7. Hegney D, McCarthy A, Rogers-Clark C, Gorman D. Why nurses are attracted to rural and remote practice. Australian Journal of Rural Health 2002; 10(3): 178-186.
8. Bushy A, Leipert BD. Factors that influence students in choosing rural nursing practice: A pilot study. Rural and Remote Health 5: 387. (Online) 2005. Available: http://www.rrh.org.au (Accessed 27 July 2009).
9. Butler C, Sheppard L. The impact of undergraduate rural education on recently graduated physiotherapists. Australian Journal of Physiotherapy 1999; 45(1): 23-30.
10. Heaney SE, Tolhurst H, Baines SK. Choosing to practice in rural dietetics. What factors influence that decision? Australian Journal of Rural Health 2004; 12(5): 192-196.
11. Daniels ZM, VanLeit BJ, Skipper BJ, Sanders ML, Rhyne RL. Factors in recruiting and retaining health professionals for rural practice. Journal of Rural Health 2007; 23(1): 62-71.
12. Devine S. Perceptions of occupational therapists practicing in rural Australia: A graduate perspective. Australian Occupational Therapy Journal 2006; 53(3): 205-210.
13. Crump WJ, Barnett D, Fricker S. A sense of place: Rural training at a regional medical school campus. Journal of Rural Health 2004; 20(1): 80-84.
14. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77(8): 790-798.
15. Bates J, Frinton V, Voaklander D. A new evaluation tool for admissions. Medical Education 2005; 39(11): 1146.
16. Rourke J. Strategies to increase the enrolment of students of rural origin in medical school: Recommendations from the Society of Rural Physicians of Canada. Canadian Medical Association Journal 2005; 172(1): 62-65.
17. Barer ML, Stoddart GL. Improving access in needed medical services in rural and remote Canadian communities: Recruitment and retention revisited. Vancouver, BC: Centre for Health Services and Policy Research, University of British Columbia, 1999.
18. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R et al. Rural background and clinical rural rotations during medical training: Effect on practice location. Canadian Medical Association Journal 1999; 160(8): 1159-1163.
19. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11(6): 277-284.
20. Chan BTB, Degani N, Crichton T, Pong RW, Rourke J, Goertzen J et al. Factors influencing family physicians to enter rural practice: Does rural or urban background make a difference? Canadian Family Physician 2005; 51(9): 1246-1252.
21. Ranmuthugala G, Humphreys J, Solarsh B, Walters L, Worley P, Wakerman J et al. Where is the evidence that rural exposure increases uptake of rural medical practice? Australian Journal of Rural Health 2007; 15(5): 285-288.
22. University of Northern British Columbia Medical Program Community Action Group. Building for the future of health care in Northern BC. Prince George, BC: University of Northern British Columbia. (Online) 2003. Available: http://www.health.gov.bc.ca/pcb/pdf/nmp_report_final.pdf (Accessed 23 Jul 2009).
23. Northern Health. Northern Health's community consultation response. Prince George, BC: Northern Health. (Online) 2005. Available: http://www.northernhealth.ca/About/documents/1840-CommunityConsultationResponse.pdf (Accessed 11 July 2009).
24. Pong RW, Russell N. A review and synthesis of strategies and policy recommendations on the rural health workforce. Sudbury, ON: Centre for Rural and Northern Health Research, Laurentian University, (Online) 2003. Available: http://www.cranhr.ca/pdf/TORC_Ruralhealthworkforcesynthesis-finaldraft-May.pdf (Accessed 3 Feb 2007).
25. Hays R, Wynd S, Veitch C, Crossland L. Getting the balance right? GPs who chose to stay in rural practice. Australian Journal of Rural Health 2003; 11(4): 193-198.
26. Schofield D, Fuller J, Fletcher S, Birden H, Page S, Kostal K et al. Decision criteria in health professionals choosing a rural practice setting: Development of the Careers in Rural Health Tracking Survey (CIRHTS). Rural and Remote Health 7(3): 666. (Online) 2007. Available: http://www.rrh.org.au (Accessed 12 Jul 2009).
27. Hanlon N, Halseth G. The greying of resource communities in northern British Columbia: implications for health care delivery in already-underserviced communities. Canadian Geographer 2005; 49(1): 1-24.
28. du Plessis V, Beshiri R, Bollman R, Clemenson H. Definitions of rural. Rural Small Town Canada Analysis Bulletin 2001; 3(3): 1-17.
29. Schmidt GG. Remote, northern communities: Implications for social work practice. International Social Work 2000; 43(3): 337-349.
30. Kulig JC, Andrews ME, Stewart NL, Pitblado R, MacLeod ML, Bentham D et al. How do registered nurses define rurality? Australian Journal of Rural Health 2008; 16(1): 28-32.
31. Schmidt GG, Klein R. Geography and social worker retention. Rural Social Work 2004; 9: 235-243.
32. Krippendorff K. Content analysis: An introduction to its methodology. Newbury Park, CA: Sage, 1980.
33. Creswell JW. Educational research: Planning, conducting, and evaluating quantitative and qualitative research, 2nd edn. Upper Saddle River, NJ: Pearson Education, 2005.
34. Patton MQ. Qualitative research & evaluation methods, 3rd edn. Thousand Oaks, CA: Sage, 2002.
35. Mayo E, Mathews M. Spousal perspectives on factors influencing recruitment and retention of rural physicians. Canadian Journal of Rural Medicine 2006; 11(4): 271-276.



