Introduction
A disproportionate number of Aboriginal Canadians have been affected by chronic disease1-3. For instance, the age adjusted prevalence rates for type 2 diabetes (T2D) in Aboriginal adults are 3 to 5 times higher than those in the general population2. Concomitantly, chronic disease risk factors such as obesity are also more prevalent in the Aboriginal population (37.8%) compared with the general population (22.6%)4. More than half of the Canadian Aboriginal peoples reside in rural and remote areas5 where the prevalence of many health risk factors is higher, potentially exacerbating these health issues.
The health of Aboriginal children and youth is of even greater concern. The prevalence of childhood overweight and obesity is greater in Aboriginal Canadian children compared with non-Aboriginal children4,6. Canadian Aboriginal children are presenting with conditions formerly referred to as having adult onset. These include diabetes (impaired glucose tolerance, T2D and the components of metabolic syndrome)6,7. Further, susceptibility to T2D now extends to increasingly younger children8.
Health promotion strategies initiated early in life that target obesity and chronic disease prevention in Aboriginal children may be the best way to counter this disturbing trend. Schools are key settings for public health actions9 for a number of reasons: (i) children attend school for substantial portions of their day and year; (ii) access to programs is generally equitable; (iii) children from across cultures and socioeconomic strata are represented10; and (iv) schools have a formal role in the delivery of health and physical education11. Thus, although schools are primarily vehicles for learning and education, they may also present pathways and provide mechanisms for health behavior change12.
Comprehensive whole-school health models hold promise as one effective solution11,13-15. Traditionally, these models consist of multiple components; they incorporate integrated planning based on individual school needs and context with facilitation by a local planning team. A shift toward these broader comprehensive and environmental approaches is becoming more apparent, as is illustrated by interventions such as the Child and Adolescent Trial for Cardiovascular Health (CATCH)16, the Middle School Physical Activity and Nutrition trial (MSPAN)17, Jump-In18, Physical Activity Across the Curriculum (PAAC)19 and Action Schools! BC (AS! BC)20.
Recent chronic disease prevention initiatives in Aboriginal communities in North America including Pathways21, Sandy Lakes Diabetes Prevention Project (SLDPP)14,22 and Kahnawake School Diabetes Prevention Project (KSDPP)13,23-25, used a comprehensive school health approach. Positive outcomes from school-based trials such as these, although variable, have included decreased plasma insulin and improved glucose tolerance26, enhanced dietary intake27, enhanced food environments28, and increased knowledge and self-efficacy14. Positive changes in physical activity (PA) and body mass index (BMI) have been more elusive13,29 with sustainability of changes not demonstrated13. Important principles when intervening in Aboriginal communities identified in Canadian initiatives include: involving community, providing learning opportunities, balancing community preferences with proven strategies, intervening in multiple settings and allowing for tailoring to the local context25,30.
Wide-spread implementation of evidence-based interventions is necessary to improve overall health and prevent chronic diseases31,32, and to maximize cost-effectiveness. In British Columbia, for example, there were 203 First Nations communities33 and 124 First Nations schools registered with the First Nations Schools Association in 2008-0934. However, Ho et al highlighted a lack of knowledge about how to 'scale up' feasible and effective interventions, while still allowing for tailoring and community involvement30.
The 'Action Schools! BC' (AS! BC) model has been described in detail previously35. It is a flexible, comprehensive, health-oriented model that provides tools for schools and teachers to create individualized 'action plans' that take into account their local context and increase opportunities for PA and healthy eating (HE). Efficacy trials showed that AS! BC significantly increased school delivery of PA and HE opportunities35,36, and children's PA37, cardiovascular38 and bone health39 and knowledge and consumption of fruit and vegetables36. Based on these results, the Province of British Columbia funded the 'scaling up' of AS! BC provincially, providing support for implementation in the form of resources for planning and implementation, training and ongoing provincial and regional facilitation20,35.
A long-standing collaborative relationship between 3 communities within the Tsimshian cultural group and pediatric residents and researchers at the University of British Columbia on the Brighter Smiles Project identified an urgent need for diabetes prevention40. This provided the foundation for further study into the feasibility of a school-based healthy living intervention for Aboriginal children living in rural and remote communities. Concurrently, the AS! BC support team was actively consulting with Aboriginal stakeholders throughout the province about their needs and the suitability of the AS! BC model for their communities. A partnership between University of Victoria and University of BC researchers with the Brighter Smiles team was forged to leverage funding for community action and to test the suitability of the AS! BC model in the First Nations context.
The purpose of this formative research was to: (i) evaluate the suitability of the existing model, (ii) inform potential adaptations of the existing model, and (iii) lay the foundation for a larger scale efficacy trial within the First Nations community. Thus, the following research questions were addressed: (i) Is the existing model feasible and appropriate for schools and children in rural and remote Aboriginal communities? (ii) How was it implemented? (iii) What adaptations to the original model were necessary? and; (iv) What were the facilitators, barriers to its uptake? The project was reviewed and approved by the Children's and Women's Research Review Committee, the University of British Columbia Behavioural Research Ethics Board and the University of Victoria Human Research Ethics Board.
Methods
Setting
The Tsimshian are a First Nations people whose territory is near Prince Rupert on the north coast of British Columbia and the southernmost corner of Alaska. Currently, there are approximately 10 000 Tsimshian, with 8700 living in Canada. The Tsimshian cultural group consists of 14 bands; 3 participated in this study. Hartley Bay (Gitga'at) is a village located on the Inside Passage, 135 km southeast of Prince Rupert and 70 km southwest of Kitimat. It is a 3.5 hour passenger ferry trip or a 1 hour float plane trip from Prince Rupert. The village is built around a network of boardwalks. There are no stores in the village, although snack foods and pop can be purchased at several private homes. Groceries are purchased in bulk and transported to Hartley Bay but this depends on storage space and weather conditions. There is a fully equipped nursing station and two nurse practitioners reside, currently temporarily, in the village. In addition, the band has a community health representative and a patient transportation clerk. The population is approximately 180 (fluctuating up to 400).
Kitkatla (Gitkxaahla) is located 72 km (45 miles) southwest of Prince Rupert and has a population of approximately 500. It is accessible by passenger ferry once weekly (1 hour 45 min) or float plane (30 min). The economic base in the community is primarily fishing and logging. There are 3 general stores. There is an elementary/junior high school, a community hall, a recreation hall, church, fitness center and youth community center.
Port Simpson (Lax Kw'alaams) is on the Alaska border, 50 km north of Prince Rupert and accessible only by passenger ferry (1 hour 10 min) four times per week or float plane (15 min). The population is approximately 900 with 5% non-Aboriginal. There is a new aquatic /recreational center with a weight room and meeting rooms. There is a convenience store and 2 restaurants and the school is a private academy. Port Simpson was the most recent community to join the Brighter Smiles Project.
Participants
Participants were staff from schools in three rural remote Aboriginal communities that were participating in the Brighter Smiles Project6,7. In these small rural/remote communities, one school served all grade levels up to grade 10. Therefore, all teachers were involved in the implementation of the AS! BC intervention and invited to participate in the process evaluation. Nineteen (76%) of the teachers and administrators in the 3 schools consented to participate in the process evaluation.
Intervention
The AS! BC model has been described previously35,38 but a brief description is provided of the model. The AS! BC model is a 'whole-school model' that provides tools for schools and teachers to create individualized action plans that increase opportunities for PA and HE across 6 action zones. These include: (i) school environment; (ii) scheduled PE; (iii) classroom action; (iv) family and community; (v) extra-curricular; and (vi) school spirit.
The AS! BC model provided teachers (primarily generalists) with enhanced training and resources to implement their action plan for their class. Schools had 3 visits from the AS! BC support team. Teachers received two half-day training sessions: an overview of AS! BC and classroom action - PA (half-day Spring 2007) and classroom action - HE (Fall 2007). The support team also provided a further in-class refresher mid-year (both PA and HE), student leadership training for indoor and outdoor games, Sport Fit? training (Winter 2008) and telephone check-ins and consultation (on request). Each teacher received a 'planning guide', a copy of the action pages and a 'classroom action bin'. The classroom action bin was dedicated to the teacher's classroom and contained equipment and resources to facilitate classroom action (PA and HE) activities (for example enough skipping ropes, dyna-bands, grippers for the class as well as DVDs, posters and how-to manuals). The PA resources prioritized gender- and skill-level-inclusive activities.
Although the model emphasized choice using a whole-school framework, classroom action was a flagship component. Teachers were asked to provide students with a minimum of 15 additional minutes of PA each school day (with PE this adds up to 150 min per week) and at least one HE activity per month in the 'classroom action zone'. Teachers provided 'PA breaks' throughout the school day using a variety of activities and equipment outlined in the 'action pages' and/or with equipment provided in the action bin. These activities included hip hop dancing, skipping, 'bounce at the bell', chair aerobics, yoga and strength work with exercise bands. Most activities required minimal equipment and could be performed in the classroom, hallway or on the school playground (where one was available). DVDs that could be used to lead student sessions were also key resources (eg. Energy Blasts®, Classroom Workout® and Get Strong Video®).
The AS! BC model was initially designed for and evaluated with students in the upper elementary grades (grades 4-7). The school model was then adapted (a modified selection of resources and activities) for lower elementary (K-3) and middle school (grades 6-9). Depending on grade, teachers were provided with a choice of, and selected from, a variety of grade appropriate activities. Activities were also adapted by local teachers to enhance the relevance for the Aboriginal community (eg 'bounce at the drum' and introducing more fruit and vegetables into cultural feasts).
Design
Based on the history of the project, the relationship with communities and the purpose of the research (formative), a consumer-focused approach41 was adopted and process evaluation42 conducted using a case study design43. The implementation (what components and how much of the model as designed [fidelity] was delivered?) and feasibility of the model (challenges, facilitators, user satisfaction and recommendations to modify to better suit the context) were evaluated. The findings from the formative assessment are reported herein.
Measurement and analysis
Action plans: At baseline, all schools completed a school action plan with the AS! BC support team. Schools were asked to set goals in each 'action zone', describe activities and establish timelines for those activities. The action plans were entered into a MS Excel spreadsheet, and the planned activities were coded and categorized to determine the scope of use of the whole-school model.
Weekly activity logs: Teachers were asked to complete weekly 'activity logs'35. Teachers recorded type, frequency and duration (minutes) of PA and HE activities implemented in the classroom or in the other action zones using an established list (each log allowed for additional alternative activities to be added). Activity logs were submitted to the AS! BC support team in Vancouver by fax and entered into a MS Excel spreadsheet. Minutes of PA and HE delivery were calculated from the reported frequency and duration of activities. Additionally, activities were counted and categorized into action zones to assess implementation in each zone and of the whole-school approach overall.
Fidelity to the intervention was assessed by comparing actual PA and HE activities (as per weekly activity logs), to prescribed proposed PA and HE activities (from their action plans) across the 6 zones to evaluate adherence to the whole-school model.
Focus group interviews
To address feasibility of the model, evaluate implementation and identify facilitators and barriers to implementation, 3 semi-structured focus groups were conducted with participating teachers and administrators at each of the 3 schools (Spring 2008). The interview schedule addressed perceptions of the model, benefits of the model, challenges and supports for implementation and commitment to implement the model in the future. Focus groups were audio-recorded (digitally) and transcribed verbatim. Transcripts were then coded using NVIVO 2.0 Qualitative Software (www.qsrinternational.com). An iterative process of constant comparison, coding and recoding was performed with one member of the research team generating a set of preliminary themes and assigning text units and the other reviewing the themes and coded text units. The team engaged in dialogue about themes and data interpretation to reduce the themes. As a second phase of data analysis, the coded text by source (community and participant) was explored to understand if themes emerged from the experience across sites or reflected the view of one site or source.
A variety of techniques were employed to provide evidence of credibility44. To ensure credibility, the study used rich, thick description of the context, peer debriefing (two researchers dealt with themes and text coding), triangulation of data, prolonged engagement (the research team had spent time in the community previously and was in each community for 2-3 days on more than one occasion throughout the year) and reporting of discrepant or negative information.
Results
Implementation
Adherence to weekly PA logging was low at 34% for all weeks. This varied across communities from 53% of eligible weeks in one community to 27% and 29% in the other two. All schools logged PA for some portion of the year; only one school completed the detailed HE logs (these provide the whole list of HE activity options) but each school recorded the number and minutes of nutrition activity delivered on their PA logs.
Based on the PA weekly logs, schools delivered an average of 140.1 min of PA opportunities per week (SD 78.1, range 121.3-175.5). Scheduled PE was delivered on average 1.75 times per week (SD 1.2), with a mean of 76.4 min (SD 60.0). The remaining minutes of PA per week (65 min) were delivered through classroom action and other zones. The average number of nutrition activities delivered per week was 2.27 (SD 3.03) and the average duration of those activities was 15.6 min (SD 22.82). Based on the HE specific logs in one school, the average duration of time spent on HE activities per week in that school was 55 min (SD 21.3 minutes). On average, this school implemented 4.6 activities per week (range 2-8 activities/week).
An analysis of the action plans showed that activities were planned across all 6 zones in the whole-school model. There was interschool variability related to what was planned. The highest proportion of planned activities occurred in the classroom and the environment zones (Table 1).
Table 1: Number of actions planned by schools and action zones
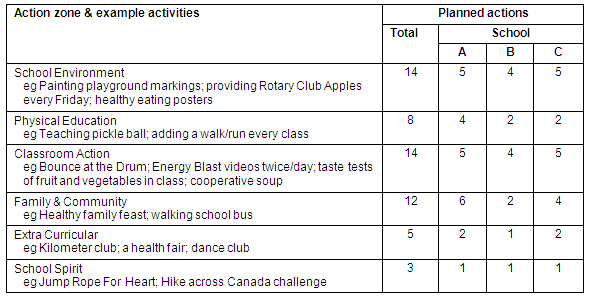
Feasibility
When asked what they thought about AS! BC, 28 of 35 coded text units were positive. Of the 7 that were negative, 2 were concerned about logging and the others reported: (i) difficulty finding time to deliver the activities (2 responses); (ii) insufficient school equipment (1 response) and; (iii) challenges with older students (2 responses). Thirteen positive responses highlighted the qualities of the program (quick and doable, choice-based, well supported, not just about sport), 8 highlighted how good, new, exciting, motivating or enjoyable it was, and 7 were about appreciating the level of provincial and school commitment. The most commonly cited benefits of AS! BC were 'healthy change' (10/19 comments related to changes in the children and 9/19 to changes in the school environment). Further benefits were the prospect of expanding and doing more activities over time (3 comments) and initiating other school activities (1 comment). A sample of comments related to the impact of AS! BC on students and the school are provided (Table 2).
Table 2: Quotes illustrating the perceived impact of the Actions Schools! BC model in participating schools

Facilitators
Support (training and resources) and ease of implementation were cited most often as key facilitators to implementation (Table 3). Focus group participants also felt that they would continue with AS! BC as long as there was enough support. For example, one participant said 'I think as long as there is AS! people coming up...I think it will keep going', and another commented:
I would like to see if we can't set up another time early...early in the Fall, maybe even in August for the trainers to come back...sort of showing how to implement all of this into the regular curriculum...that would really help us to keep going.
Anecdotally, the AS! BC support team was asked back to one of the communities to conduct more training in 2008.
Table 3: Implementation facilitators: number of text quotes by theme and school
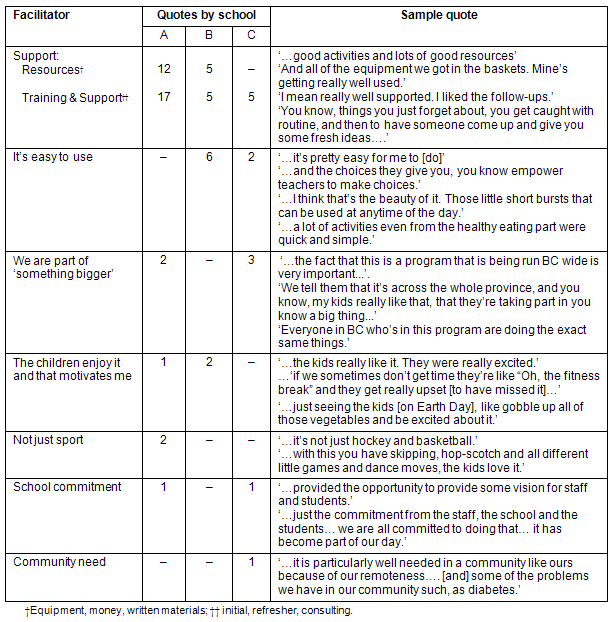
Barriers
Lack of time and school level resources, high staff turn-over, evaluation requirements, student behavior, low levels of staff knowledge about healthy living and lack of variety were key themes highlighted by the participants as barriers to implementation. A description of these themes, the frequency of quotes by community and an illustration using quotes from participants is provided (Table 4).
Table 4: Challenges associated with the implementation (number of quotes by theme and school)

Recommended modifications/adaptations
When asked how the program could be improved to better meet their needs, participants suggested a number of modifications that would enhance implementation and the relevance of the model and resources for Aboriginal communities. Participants suggested that enhanced community partnerships, parent education and a greater focus on the First Nations traditions would all improve the program. Moreover, they identified that if the model was part of the curriculum, they would have the additional support needed for successful implementation. Participant suggestions are shown (Table 5).
Table 5: Stakeholder suggestions on how to improve Action Schools! BC

Discussion
Action Schools! BC was feasible and well accepted by teachers and administrators in rural and remote Aboriginal communities in BC; some cultural adaptations were recommended. AS! BC is a flexible, whole-school model that provides planning tools, training, classroom resources and ongoing facilitation to support implementation. These resources and technical support and facilitation were identified as critical to ongoing implementation and sustainability.
Action Schools! BC represented several of the best practice principles for implementing community-based interventions in Aboriginal communities outlined by Potvin and Ho25,30. It was flexible, it engaged the community in planning and implementation, it connected the school to the broader community, and it provided learning opportunities for staff and students. At the school level, teachers and administrators chose activities most suitable for their own school. Some individual teachers made adaptations to make the activities more culturally relevant, while others did not. Some teachers also modified cultural events to make them more health relevant. The present data and both KSDPP and SLDPP clearly indicated the importance of these cultural adaptations25,14. In the classroom, AS! BC almost solely emphasized 'doing/experiencing' PA, which matched closely what Caballero et al.45 and Saksvig et al.14 described as accommodating traditional Aboriginal learning styles that favor experiential learning.
Schools delivered 93% of the target amount of PA and well over the goal of 1 activity per week of HE activities (double in fact). Teachers successfully implemented physical activities in the classroom, and this contributed to almost 50% of the recommended amount of PA during the week. Sandy Lake had planned this type of intervention, but implementation was unsuccessful due to lack of facilitation14. In the Pathways intervention, teachers selected and implemented one of 50 activity cards in the classroom. On average, they implemented 1.6 activities per day46. To the authors' knowledge, AS! BC provides the first example of successful implementation of this approach ('snacking on physical activity throughout the school day') to promote PA in the Aboriginal health literature, although this must be evaluated in light of the low adherence to logging.
Schools also planned and implemented activities across multiple zones within the whole-school framework. Implementation of the activities and evaluation procedures varied substantially across schools and teachers. High implementation variability was also found in KSDPP13. The KSDPP researchers reported that the integration of their evaluation and program created a synergy that enhanced implementation25.
Kahnawake relied on cognitive knowledge development in the classroom, PE, and school- and community-based events to increase PA. Pathways used the SPARK training for PE47 which was well received and resulted in high levels of implementation, but researchers reported that a number of PE specialists had to be added after the grade 3 process evaluation showed low levels of implementation initially46.
Action Schools! BC incorporates a family and community zone within the whole-school model. Although the model provided for it, and the action plans showed that schools planned family/community activities, the stakeholders felt that this component needed to be enhanced; this may reflect the fact that activities were planned but not necessarily implemented or feasible during the pilot. Ho et al.30, among others25,46 have previously emphasized the need for a multi-setting and multi-level approach, not only to shift the social culture within the overall community, but also to allow for integration of theoretical and cultural concepts and provide the space for active involvement of a variety of community members.
Barriers to implementation cited in this project were similar to those identified in previous research in Aboriginal schools. Lack of time, health attitudes of some teachers and staff turn-over were all barriers found in common with the Pathways intervention48 and other implementation literature35,49. In the classroom, the focus of AS! BC is on 'doing' enjoyable PA and food preparation and tasting activities rather than learning about PA and HE cognitively in a didactic teaching format. As a result, some of the teachers (from higher grade levels) identified the potential for disruptive student behavior (specifically related to the PA breaks) as a barrier and mentioned treating these activities as optional. Financial resources were cited as a potential barrier to the hands-on HE activities such as tasting sessions and smoothie-making. Ongoing financial support is currently available through an AS! BC food grant that schools can access annually. The teachers in this study, as in previous studies35, emphasized that tracking their classroom and school activities was a burden.
Our results identified further cultural adaptations and ongoing support as critically important to sustainability. Some participants adapted some of the activities. For example: 'bounce at the bell' became 'bounce at the drum'; some teachers incorporated Aboriginal stick and bone games into their activities; and fruit and vegetables were incorporated into cultural feasts. However, further adaptations related to local food and language were recommended. These adaptations are also challenges for the scaling up of AS! BC in rural and remote Aboriginal communities because of the variety of local food, language and cultures across First Nations communities. For instance there are 37 First Nations languages in BC, 10 language families33 and 14 biogeoclimate zones where vegetation and food supplies differ50.
Providing ongoing support to rural and remote communities was challenging and will be an issue for scaling up health promotion initiatives and supporting implementation in these communities. Both the AS! BC support and research teams had to fly, boat or travel long distances in and out of some communities, and transportation was expensive and limited by weather. Creating a network of Aboriginal trainers and measurement teams (if further evaluation is to be conducted) that reside in First Nations communities is a potential solution and a key recommendation from KSDPP26.
Conclusions
Our evaluation demonstrated that AS! BC was appropriate and feasible for the First Nations schools in these rural and remote communities with some cultural adaptations and ongoing support. Rural and remote locations have very specific challenges that need to be considered in broader dissemination strategies.
Acknowledgments
The authors thank the communities of Hartley Bay, Kitkatla and Port Simpson for their collaborative partnership. They thank Mr David Benton for his critical review of this manuscript. This study was funded by the Canadian Council on Learning, Canadian Diabetes Association, British Columbia Medical Services Foundation and the Lawson Foundation. Dr Panagiotopoulos is the recipient of the Child & Family Research Institute Clinician Scientist Award and the Canadian Diabetes Association Clinician Scientist Award.
References
1. Liu J, Young TK, Zinman B, Harris SB, Connelly PW, Hanley AJ. Lifestyle variables, non-traditional cardiovascular risk factors, and the metabolic syndrome in an Aboriginal Canadian population. Obesity 2006; 14(3): 500-508.
2. Young TK, Reading J, Elias B, O'Neil JD. Type 2 diabetes mellitus in Canada's first nations: status of an epidemic in progress. Canadian Medical Association Journal 2000; 163(5): 561-566.
3. MacMillan HL, MacMillan AB, Offord DR, Dingle JL. Aboriginal health. Canadian Medical Association Journal 1996; 155(11): 1569-1578.
4. Katzmarzyk PT. Obesity and physical activity among Aboriginal Canadians. Obesity 2008; 16(1): 184-190.
5. Kirby MJ, LeBreton M. The health of Canadians- the federal role. Volume two: Current trends and future challenges. Ottawa: The Standing Senate Committee on Social Affairs, Science and Technology, Parliament of Canada, 2002.
6. Wahi G, Zorzi A, Macnab A, Panagiotopoulos C. Prevalence of type 2 diabetes, obesity and the metabolic syndrome among Canadian First Nations children in a remote Pacific coast community. Paediatrics & Child Health 2009; 14(2): 79-83.
7. Zorzi A, Wahi G, Macnab AJ, Panagiotopoulos C. Prevalence of impaired glucose tolerance and the components of metabolic syndrome in Canadian Tsimshian Nation youth. Canadian Journal of Rural Medicine 2009; 14(2): 61-67.
8. Health Canada Aboriginal Diabetes Initiative. Diabetes among Aboriginal (First Nations, Inuit and Métis) people in Canada: the evidence. Ottawa, ON: Health Canada, 2001.
9. St. Leger LH, Kolbe L, Lee A, McCall DS, Young IM. School health promotion: achievements, challenges and priorities. In: DV McQueen, CM Jones (Ed.). Global Perspectives on Health Promotion Effectiveness. New York: Springer Science, 2007; 107-123.
10. Fox KR, Cooper A, McKenna J. The school and promotion of children's health-enhancing physical activity: perspectives from the United Kingdom. The Journal of School Health 2004; 23: 338-358.
11. Naylor PJ, McKay HA. Prevention in the first place: schools as a setting for action on physical inactivity. British Journal of Sports Medicine 2009; 43(1): 10-13.
12. Mullen PD, Evans D, Forster J, Gottlieb NH, Kreuter M, Moon R et al. Settings as an important dimension in health education/promotion policy, programs, and research. Health Education Quarterly 1995; 22(3): 329-345.
13. Paradis G, Levesque L, Macaulay AC, Cargo M, McComber A, Kirby R et al. Impact of a diabetes prevention program on body size, physical activity, and diet among Kanien'keha:ka (Mohawk) children 6 to 11 years old: 8-year results from the Kahnawake Schools Diabetes Prevention Project. Pediatrics 2005 Feb 1; 115(2): 333-339.
14. Saksvig BI, Gittelsohn J, Harris SB, Hanley AJG, Valente TW, Zinman B. A Pilot School-based healthy eating and physical activity intervention improves diet, food knowledge, and self-efficacy for Native Canadian children. The Journal of Nutrition 2005; 135(10): 2392-2398.
15. van Sluijs EMF, McMinn AM, Griffin S. Effectiveness of interventions to promote physical activity in children and adolescents: systematic review of controlled trials. BMJ 2007; 335(7622): 703-707.
16. Luepker RS, Perry CL, Osganian V, Nader PR, Parcel GS, Stone EJ et al. The child and adolescent trial for cardiovascular health (CATCH). The Journal of Nutritional Biochemistry 1998; 9(9): 525-534.
17. Sallis JF, McKenzie TL, Conway TL, Elder JP, Prochaska JJ, Brown M et al. Environmental interventions for eating and physical activity: a randomized controlled trial in middle schools. American Journal of Preventive Medicine 2003; 24(3): 209-217.
18. Jurg ME, Kremers SPJ, Candel MJJM, Van der Wal MF, Meij JSBD. A controlled trial of a school-based environmental intervention to improve physical activity in Dutch children: JUMP-in, kids in motion. Health Promotion International 2006; 21(4): 320-330.
19. Gibson C, Smith B, DuBose K, Greene JL, Bailey B, Williams S et al. Physical activity across the curriculum: year one process evaluation results. International Journal of Behavioral Nutrition and Physical Activity 2008; 5(1): 36.
20. Naylor PJ, Macdonald HM, Reed KE, McKay HA. Action Schools! BC: a socio-ecological approach to modifying chronic disease risk factors in elementary school children. Prevalence of Chronic Disease 2006; 3(2). (Online) 2006). Available: http://www.bpcommunityexchange.net/toolbox/Lessons%20Learned%20Action%20Schools%20BC.pdf (Accessed 1 April 2006).
21. Davis SM, Going SB, Helitzer DL, Teufel NI, Snyder P, Gittelsohn J et al. Pathways: a culturally appropriate obesity-prevention program for American Indian schoolchildren. American Journal of Clinical Nutrition 1999; 69(Suppl4): 796S-802S.
22. Hanley AJG, Harris SB, Barnie A, Gittelsohn J, Wolever TMS, Logan A et al. The Sandy Lake Health and Diabetes Project: design, methods and lessons learned. Chronic Diseases in Canada 1995; 16(4). Available: http://www.phac-aspc.gc.ca/publicat/cdic-mcc/16-4/index.html (Accessed 23 February 2010).
23. Macaulay AC, Paradis G, Potvin L, Cross EJ, Saad-Haddad C, McComber A et al. The Kahnawake Schools Diabetes Prevention Project: intervention, evaluation, and baseline results of a diabetes primary prevention program with a Native community in Canada. Preventive Medicine 1997; 26(6): 779-790.
24. Macaulay AC, Paradis G, Potvin L, Cross EJ, Saad-Haddad C, McComber AM et al. Primary prevention of type 2 diabetes in First Nations: experiences of the Kahnawake schools diabetes prevention project. Canadian Journal of Diabetes Care 1997; 22(3): 44-49.
25. Potvin L, Cargo M, McComber AM, Delormier T, Macaulay AC. Implementing participatory intervention and research in communities: lessons from the Kahnawake Schools Diabetes Prevention Project in Canada. Social Science & Medicine 2003; 56(6): 1295-1305.
26. Ritenbaugh C, Teufel-Shone NI, Aickin MG, Joe JR, Poirier S, Dillingham DC et al. A lifestyle intervention improves plasma insulin levels among Native American high school youth. Preventive Medicine 2003; 36(3): 309-319.
27. Himes JH, Ring K, Gittelsohn J, Cunningham-Sabo L, Weber J, Thompson J et al. Impact of the Pathways intervention on dietary intakes of American Indian schoolchildren. Preventive Medicine 2003; 37(Suppl1): S55-S61.
28. Story M, Snyder MP, Anliker J, Weber JL, Cunningham-Sabo L, Stone EJ et al. Changes in the nutrient content of school lunches: results from the Pathways study. Preventive Medicine 2003; 37(Suppl1): S35.
29. Going S, Thompson J, Cano S, Stewart D, Stone E, Harnack L et al. The effects of the Pathways Obesity Prevention Program on physical activity in American Indian children. Preventive Medicine 2003; 37(Suppl1): S62-S69.
30. Ho LS, Gittelsohn J, Harris SB, Ford E. Development of an integrated diabetes prevention program with First Nations in Canada. Health Promotion International 2006; 21(2): 88-97.
31. Haines A, Kuruvilla S, Borchert M. Bridging the implementation gap between knowledge and action for health. Bulletin of the World Health Organization 2004; 82: 724-732.
32. Sussman S, Valente TW, Rohrbach LA, Skara S, Ann Pentz M. Translation in the health professions: converting science into action. Evaluation & the Health Professions 2006; 29(1): 7-32.
33. First Peoples Heritage Language and Culture Council. First People's language heritage map. Brentwood Bay, BC: First Peoples Heritage Language and Culture Council, 2010.
34. First Nations School Association. Fifth Annual FNSA School Measures and Data Collection Project Final Report. West Vancouver, BC: First Nations School Association, 2009.
35. Naylor PJ, Macdonald HA, Zebedee J, Reed KE, McKay HM. Lessons learned from Action Schools! BC - an 'active school' model to promote physical activity in elementary schools. Journal of Science, Medicine and Sport 2006; 9(5): 413-423.
36. Day ME, Strange KS, McKay HA, Naylor PJ. Action Schools! BC - Healthy Eating - effects of a whole-school model to modifying eating behaviours of elementary school children. Canadian Journal of Public Health-Revue Canadienne De Sante Publique 2008; 99(4): 328-331.
37. Naylor PJ, Warburton DER, Reed KE, McKay HA. An 'active school' model to promote physical activity in elementary schools: Action Schools! BC. British Journal of Sports Medicine 2008; 42: 338-343.
38. Reed KE, Warburton DER, Macdonald HM, Naylor PJ, McKay HA. Action Schools! BC: a school-based physical activity intervention designed to decrease cardiovascular disease risk factors in children. Preventive Medicine 2008; 46(6): 525-531.
39. Macdonald H, Kontulainen S, Petit M, Beck T, Khan K, McKay H. Does a novel school-based physical activity model benefit femoral neck bone strength in pre- and early pubertal children? Osteoporosis International 2008; 19(10): 1445-1456.
40. Panagiotopoulos C, Rozmus J, Gagnon RE, Macnab AJ. Diabetes screening of children in a remote First Nations community on the west coast of Canada: challenges and solutions. Rural and Remote Health 7(3): 771. (Online) 2007. Available: www.rrh.org.au (Accessed 21 April 2010).
41. Spoth R, Molgaard, V. Consumer-focused data collection in prevention program evaluation: rationale and illustrations. Evaluation of Health Professionals 1993; 16(3): 278-294.
42. Linnan L, Steckler A. Process evaluation for public health interventions and research: an overview. In: A Steckler, L Linnan (Eds). Processs evaluation for public health interventions and research. San Francisco, CA: Jossey-Bass, 2002; 1-24.
43. Yin RK. Case study research: design and methods. Applied social research methods series, vol 5. Thousand Oaks, CA: Sage, 1984.
44. Thomas JR, Nelson JK, Silverman SJ. Research methods in physical activity, 5th edn. Champaign, IL: Human Kinetics, 2005; 357-360.
45. Caballero B, Davis, S, Davis CE, Ethelbah B, Evans M et al. Pathways: a school-based program for the primary prevention of obesity in American Indian children. Journal of Nutrition and Biochemistry 1998; 9: 535-543.
46. Steckler A, Ethelbah B, Martin CJ, Stewart D Pardilla M et al. Pathways process evaluation results: a school-based prevention trial to promote healthful diet and physical activity in American Indian third, fourth and fifth grade students. Preventative Medicine 2003; 37: S80-S90.
47. McKenzie TL, Sallis JF, Faucette N, Roby JJ, Kolody B. Effects of a curriculum and inservice program on the quantity and quality of elementary physical education classes. Research Quarterly for Exercise and Sport 1993; 64(2): 178-187.
48. Gittelsohn J, Merkle S, Story M, Stone EJ, Steckler A, Noel J et al. School climate and implementation of the Pathways study. Preventive Medicine 2003; 37(Suppl1): S97-S106.
49. Connell D, Turner R, Mason E. Summary of findings of the school health education evaluation: health promotion effectiveness, implementation and costs. The Journal of School Health 1985; 55(8): 316-321.
50. Evans M, Huynh V, Schwendener T, Wang MY. Biogeoclimatic zones of BC. (Online) 2009. Available: http://www.sfu.ca/geog/geog351fall07/Group06/BC%20All%20Zones.htm (Accessed 21 July 2009).





