The last decade has seen the emergence of a political movement in Australia aimed at changing the way Australians think about the delivery of mental health services1. Underlying this is several decades of mental health research revealing that adolescence is the stage in which most mental health problems first manifest2. Research also suggests that delays in seeking help for mental health problems lead to poorer treatment outcomes3-5 . For these reasons it is essential that mental health problems are detected and treated early, and that the mental health system is strongest during the period of life when services are needed most1,2. While funding has been given to improve accessibility to youth-specific mental health services for rural youth in recent times6, there is still a long way to go to improve access for the majority of Australia's youth. Unfortunately, rural adolescents face additional barriers to obtaining professional psychological help due to poor availability and accessibility of services in rural areas. These issues need to be considered alongside the implementation of new youth mental health services in rural Australia7.
Summary of research on help-seeking for mental health problems by adolescents
The adolescent literature in general indicates that female adolescents are more likely to seek help for mental health problems than males8,9 and that help-seeking for mental health problems by adolescents increases with age9,10. In terms of mental health status, there is also evidence to suggest that help-seeking behaviour is lower in young people suffering from mental distress11. This is thought to be, in part, due to their negative expectations about the future.
Most of what is known about barriers to help-seeking for rural adolescents in Australia, however, has come from qualitative studies. For example, Quine et al12, in a focus group study, noted several differences between rural and urban adolescents in their health concerns and experiences in accessing services. They found that contrary to the concerns of adolescents from urban areas, rural adolescents were most concerned about youth suicide and teenage pregnancy. Rural adolescents also highlighted structural differences in service provision such as cost and lengthy waiting periods, the limited choice of health professionals, and poor public transport. They also identified limited educational and employment opportunities along with limited recreational opportunities as impacting on their health.
Francis et al13 also conducted a focus group study focused on the attitudes of rural adolescents towards seeking help for mental health problems. Each focus group in this study was presented with two hypothetical scenarios of an adolescent living in a rural area affected by a mental health problem. The participants in the study identified several barriers to help seeking that could be considered unique to rural contexts, including: (i) a lack of specialist local services and the consequent need to travel to gain access to professional help; (ii) the need to reveal mental health problems to another person in order to obtain transport in the absence of local public transport options; (iii) fear of social stigma and exclusion as the result of revealing a mental health problem and identified rural gossip networks as limiting anonymity; and (iv) that mental health problems were perceived as a sign of weakness in their communities. Although the young people in this study considered the range of professionals as potential providers of help for mental health problems, they did not view GPs positively.
Boyd et al14 conducted in depth interviews with a small number of first year university students at a regional university who in their adolescence had sought help for a mental health problem while residing in a rural town. These young people revealed a range of barriers which confirmed the findings of Francis et al13. Concerns about lack of anonymity due to gossip, a culture of self-reliance whereby the acknowledgement of mental health problems is perceived as weak, and lack of knowledge about available help sources were raised by each participant. Participants who had managed to receive help discussed experiences in which their helpers had noticed their distress and had approached them to offer assistance.
In addition to help-seeking barriers, Boyd et al13 also asked their participants to discuss their preferences regarding the source of help that they received. Participants expressed a preference for school-based help over medical help, due in part to the ability of school-based helpers to be readily available. Participants also identified the characteristics possessed by these helpers that had made them approachable; these included being caring, non-judgemental, genuine, young, and able to maintain confidentiality. This corresponded to previous research findings that although young people prefer informal sources of help, particularly peers, to formal sources15, when seeking professional help adolescents look for several characteristics in potential helpers; that they are 'nonjudgmental', able to 'relate to teens', and 'make themselves available'. Barriers to help seeking are created if a professional is perceived as 'psychologically inaccessible (acts superior)' or too busy16.
Finally, Aisbett et al17 undertook a series of in depth interviews with rural adolescents who had received mental health services within their communities. These young people described how lack of transport to and from the mental health service was a barrier to young people accessing treatment. They also expressed frustration with long waiting lists and the remote after-hours service. Notably, they revealed that rural gossip networks and social visibility within rural communities compounded their experiences of stigma and social exclusion and explained how these experiences affected their on-going utilization of the mental health service.
Summary and rationale for the present study
Much knowledge about the barriers that face rural youth in accessing mental health services has been gained through qualitative study. The strength of focus group and interview methods is the ability to go 'straight to the source' in accessing the attitudes and experiences of young people directly. However, within the broader public health context where quantitative research findings are valued more than qualitative ones, the present researchers have felt an on-going need to verify these findings with a larger sample. In so doing, it is hoped that further insight will be gained into the extent of these issues across our State.
Therefore, the main objective of the present study was to conduct a piece of quantitative research, grounded in previous qualitative research findings, which would estimate the frequency of help-seeking intentions and preferences among a normative sample of rural youth. In addition to the frequency information, we aimed to conduct exploratory, multivariate analyses of the data in seeking to predict help-seeking intention. Finally, using open-ended questions in the survey, we aimed to understand the barriers to help-seeking perceived by the youth in our sample, in the attempt to verify the results of our previous qualitative research.
Method
Participants
The participants were 201 adolescents, of whom 74 were male (36.8%) and 127 were female (63.2%), recruited from 8 rural schools in Victoria, Australia. Participants ranged in age from 11 to 18 years with 92 participants (45.8%) in the younger age group of 11 to 14 years and 109 participants (54.2%) in the older age group of 15 to 18 years.
The remoteness of the participants' rural locations ranged from .21 to 5.29 according to the Accessibility/Remoteness Index of Australia (ARIA+). This index classifies rural locations on the basis of road distance from essential goods and services18. The range of ARIA+ scores for participants in this study fell into two broad ARIA categories: Inner and Outer Regional. On the basis of these categories, 149 participants (74.1%) were classified as living in an Inner Regional area and 52 participants (25.9%) were classified as Outer Regional.
Participating rural towns were located within the Loddon Campaspe, Grampians, Wimmera and Mallee regions of Victoria. The Inner Regional areas, the Loddon Campaspe and Grampians regions, are wine growing regions that offer relative prosperity compared with the Wimmera and Mallee. As Outer Regional areas, the Wimmera and Mallee regions of Victoria are wheat and livestock farming areas that have been severely impacted by drought conditions in recent years.
Measures
The Centre for Epidemiological Studies - Depression Scale: The CES-D is a 20 item self-report instrument that measures several components of depression including: depressed mood, feelings of helplessness and hopelessness, guilt and worthlessness, loss of appetite and sleep disturbance. Respondents rate the frequency with which they have experienced each of 20 symptoms of depression in the previous 2 weeks. These are rated on a four-point scale ranging from none of the time (= 0) to most of the time (= 3). The total severity score ranges from 0 to 60 and following the reversal of items 4, 8, 12 and 16 is obtained by simple summation of scores across all 20 items.
The CES-D has been previously administered to samples of junior high school students, young adults, depressed patients, and a representative community sample of adults19. It has been found to be a psychometrically sound instrument which has proved to be particularly well suited to high school and older adults with estimates of internal consistency ranging from .85 to .90.
The Zung Anxiety Scale: The Zung Anxiety Scale was developed as a 20 item self-report measure of the severity and frequency of current anxiety and associated symptoms. Each item is scored on a 4 point scale with none or a little of the time (= 0), to most or all of the time (= 4). Items 4, 5, 7 and 8 are reversed and the total score which ranges from 20 to 80 is obtained by a simple summation of scores across all 20 items. The Self-rating Anxiety Scale (SAS) has been found to have split half correlations of .7120. It has also been found to be a valid measure of anxiety, accurately predicting the severity of anxiety in a psychiatric sample.
Open-Ended Survey of the Help-Seeking Preferences and Intentions of Rural Youth: A survey of help-seeking preferences and intentions was specifically developed for use in this study to enable the main aims of the research to be addressed (Appendix I). Building on their previous qualitative work in the area of rural adolescent mental health, the researchers designed an instrument that would allow for further exploration help-seeking preferences and intention in a representative sample of rural youth while at the same time allowing flexibility to obtain some qualitative information from the participants. With these considerations in mind Boyd et al17 devised a scale that would provide:
- Frequency information regarding the intention to seek professional help should the participant experience a mental health problem.
- The potential help sources and preferences for type of professional that rural adolescents would seek help from.
- The barriers to seeking professional help in a rural town as perceived by rural youth.
- The reasons provided by rural adolescents who would not be prepared to seek professional help for a mental health problem.
The resulting survey was predominantly in open-ended response format (Appendix I).
Procedure
Ethical approval for the study was obtained from the University of Ballarat's Human Research Ethics Committee and the Department of Employment, Education, and Training's Ethics Committee. On approval from school principals, explanatory letters and consent form were sent home to the parents of school students. Only those students for whom parental consent was obtained participated in the study. Participation by the adolescents was voluntary and anonymous.
Surveys were administered on school premises during class time by either the first or third author. Students with consent were taken to a separate classroom for administration of the survey. The explanatory statement for the study was re-presented to students and any clarification regarding the nature of the study was openly discussed, including students' understandings of what was meant by 'help-seeking' and 'mental health problems'.
Data analysis
Qualitative data were content analysed by the fourth author who has expertise in qualitative research techniques. Content categories were separately checked by the first author for consistency. Frequency counts derived from the content analysis were subsequently entered into the Statistical Package for the Social Sciences v13 (SPSS; Chicago, IL, USA; www.spss.com) for further analysis, and quotations illustrating content categories were selected for inclusion in the paper by all members of the research team.
Quantitative data were analysed by the first and second authors using SPSS. Prior to analysis, several subgroups were created within the dataset. The first group of 11 to 14 year-olds was labelled 'Early Adolescence', and the second group of 15 to 18 year-olds was labelled 'Late Adolescence'. Rurality was also divided into 2 categories based on the ARIA14, such that ARIA+ scores ranging from .21 to 2.4 were designated as 'Inner Regional' and ARIA+ scores ranging from 2.4 to 5.29 were designated 'Outer Regional'. Chi-square analyses of cross-tabulated data were then conducted to determine whether observed frequencies differed on the basis of subgroup membership (ie sex, age, and rural location). A hierarchical logistic regression analysis was also conducted in order to test predictors of help-seeking intention. This analysis was achieved by conducting the regression analysis in two steps using the standard method of entry. In the first step, measures of distress (ie depression and anxiety scores) were entered as predictors. In the second step, demographic variables (ie sex, age, and rural location) were entered into the analysis. Sex was re-coded to create a dummy variable of 'femaleness', and age and ARIA were entered in their continuous forms (ie age in years and ARIA+ scores). The Hosmer and Lemeshow test was selected as the measure of goodness-of-fit.
Results
Frequency information on help-seeking preferences and intention
Seeking professional help: Regarding the intention to seek professional help for a mental health problem such as depression or anxiety, a total of 55.7% of participants (n = 112) indicated that they would. Further analysis (ie cross-tabulations) revealed no statistically significant differences on the basis of sex, age group, or rural location in this proportion.
The pattern of preferences for source of professional help for the overall sample with breakdowns according to age, sex, and rural location is shown (Table 1).
Table 1: Help-seeking preferences for participants who would seek professional help
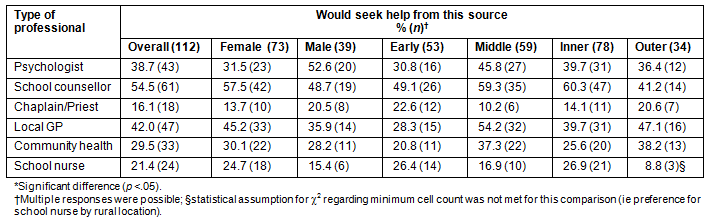
The majority of participants, regardless of subgroup, indicated that they would seek help for a mental health problem from a school counsellor (Table 1). The local GP and a psychologist were also endorsed as potential help sources by participants.
The breakdown of responses by sex (male, female) and age group (early and late adolescence) revealed few differences in help-seeking preferences. Notable exceptions included the statistically significant difference in the preference for seeking help from a psychologist such that males were more likely to indicate this as a potential help source than females (Χ2 [1] = 4.70, p = .03). A significant difference in the preference to seek help from the local GP was found on the basis of age group such that participants in the late adolescence group were more likely to indicate this as a potential help source than those in the early adolescence group (Χ2 [1] = 7.71, p = .01).
A content analysis of the responses to the open-ended survey questions regarding reasons in the first choice of potential help source yielded interesting results. Regarding first choice of help, 29% indicated that the school counsellor would be their first choice, 27% indicated the local GP, 13% nominated the psychologist, and 11% the community health service. All other potential help sources were rated as first choice by less than 10% of respondents. In terms of the last choice, 49% of respondents indicated that the chaplain or priest would be their last choice; whereas, 23% indicated that the psychologist would be their last choice. All other potential help sources were nominated as last choice of potential helper in less than 10% of cases.
Analysis of the reasons given for first choice of potential help source revealed that 46.4% of the reasons given related to the young person having had prior positive experiences or an existing rapport with the nominated professional. For example, one participant wrote:
I would see a community health service person because I have been to see one before and that really helped.
In 27.8% of cases, the participant had nominated the professional as their first choice because of a belief that the professional was competent and appropriately qualified to help them. In illustration, one participant wrote:
[I would see] a psychologist/counsellor because they are trained and skilled to help with any problems you might have.
In 17.8% of cases, participants indicated that they had nominated their first choice of potential help source because of the convenience of the professional's location. The remaining responses (<10% per category) concerned the ability to trust the professional's ability to maintain confidentiality, the affordability of receiving help from the nominated source, as well as the ability of the professional to refer on to more appropriate help.
The three most common reasons given for nominating a potential help source as last choice included: (i) not being religious (in terms of not wanting to seek help from a chaplain or priest); (ii) perceiving that the type of professional was not competent to deal with their issues; and (iii) difficulties in trusting this type of professional to maintain confidentiality. Regarding the psychologist, several participants raised self-stigma as an issue, for example:
[My last choice would be] a psychologist because it would make me think I was crazy or there was something really wrong with me.
Other reasons given for participants nominating a professional as their last choice (<10% per category) included the limited availability of professional services, the cost of accessing help from the professional, a belief that their problem would not be serious enough for this type of professional and not feeling comfortable in talking to a stranger (in cases where the professional was not known to them).
Not seeking professional help: Of the 44.3% of participants who indicated that they would not seek help from a professional for a mental health problem such as depression or anxiety, 57.3% (n = 51) indicated that they would seek support from their friends and 43.8% (n = 39) would seek help from their family (multiple responses were possible). In contrast, 12.9% (n = 26) of participants who would not seek professional help for a mental health problem indicated that they would cope with the problem on their own. For those who indicated that they would prefer to cope on their own, several reasons were offered but most related to a need to be 'in control'. For example:
I don't like when people judge me, or I feel that I am being judged. I prefer it when others think I am confident and in control.
Analysis of differences in frequency of seeking help from family, friends or coping by self on the basis of the three subgroups (age, sex, and rural location) revealed that only one was statistically significant. This result revealed that participants were more likely to report that they would seek help from a family member if they were in early adolescence than late adolescence (Χ2 [1] = 4.47, p = .04).
When asked to provide reasons for the preference to not seek professional help, 30.6% of reasons related to not being comfortable discussing mental health problems with a stranger. A further 15.8% of reasons related to feeling closer to informal sources of support and 11.9% of reasons related to a fear of embarrassment or social stigma associated with seeing a professional. The following quotations illustrate these reasons.
Because I wouldn't want strangers knowing things like that about me, even if they were going to help. I wouldn't feel comfortable.
I trust my family and friends, they know me personally, know my strengths and weakness and my personality in general. They would be more understanding and I'd feel more confident going to them.
[If I seek help from a professional] I feel as though I'm being and idiot and embarrassed and that people at school may find out, bag me for my illness if I have any.
A wide range of additional reasons for not seeking professional help were also provided by participants (<10% per category) including cost of professional services, bad experiences with professional services in the past, inability to trust professionals to keep information confidential, lack of professional services in the town, long waiting lists, not knowing where to find professional help, and not trusting the competence of this type of professional.
Multivariate analysis of help-seeking intention
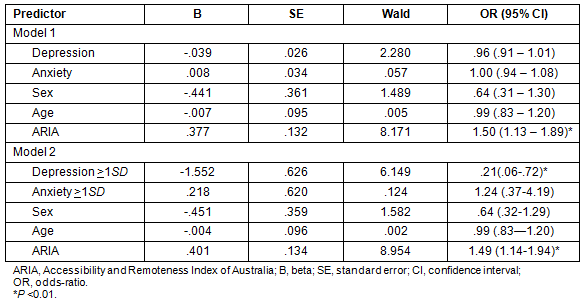
Overall help-seeking intention: A logistic regression was utilized to test overall intention of rural adolescents to seek help for mental health problems. The dependent variable was Question 1 of the open-ended survey: 'If you had something worrying you (eg depression or anxiety) would you seek professional help (eg counsellor, psychologist) for it?' and the independent variables were sex, age, ARIA score, depression score, and anxiety score. The correlations between these variables are shown (Table 2). The full model was significantly reliable - Χ2 (5) = 15.72, p = .008 (Hosmer and Lemenshow Χ2 [8] = 7.76, p = .46) - and accounted for between 9% and 12% of the variance in help-seeking; however, ARIA emerged as the only unique predictor. The model was more accurate at predicting help-seeking (69.1% correct), than not seeking help (44% correct). A summary of the results of this analysis is presented (Table 3), and reveals that young people in more rural areas were 50% (OR 1.50, p = .004, 95%CI 1.20, 1.89) more likely to report that they would seek help.
Help-seeking intention according to mental health status: Finally, to determine if young people with symptoms of depression or anxiety would seek help, the above mentioned logistic regression was conducted using depression and anxiety scores that were 1 standard deviation above the mean only. This analysis was conducted for theoretical reason given that past literature suggests that help-seeking intentions differ among young people who experience high levels of mental distress11. Again, the full model was significantly reliable - Χ2 (5) = 21.87, p = .001 (Hosmer and Lemenshow Χ2 [8] = 7.18, p = .52) - and accounted for between 11% and 16% of the variance in help-seeking. This time, however, ARIA and depression emerged significant predictors of help-seeking with the model correctly predicting this at a rate of 79.4% (Table 3). As expected, the model revealed that young people with higher levels of depression were 79% less likely to report help-seeking intention (OR .21, p = .013, 95%CI .06, .72).
Table 2: Correlation matrix
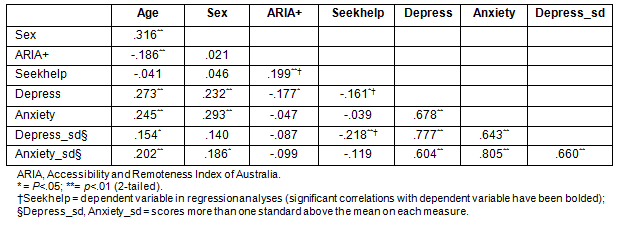
Table 3: Summary of the logistic regression analysis predicting intention of rural youth to seek professional help for a mental health problem
Barriers to seeking professional help for mental health problems in the context of a rural community
Participants' responses to an open-ended question asking them to identify the barriers to seeking professional help for mental health problems in the context of a rural community were content analysed and divided into categories. Results revealed that the perceived limited availability of professional services in the town was identified by participants with a frequency of 33.6% (n = 48), barriers associated with perceived social proximity and rural gossip were identified with a frequency of 32.1% (n = 44), and barriers associated with having to travel to obtain professional help occurred with a frequency of 17.5% (n = 24). Selected quotations illustrating these content categories follow.
There is nowhere you can go in a country town, they don't have special places for this kind of thing.
The fact that because the place is small it's quite likely that people will find out you have an issue. In a city you could seek help in a different suburb but here everybody knows everyone else.
Having to travel so far! It's not like there's a local GP next door to me.
Additional barriers identified with a frequency of less than 5% per category included the cost of professional services, not knowing where to find help, and a perceived lack of confidentiality from local providers. A total of 8.8% (n = 12) of respondents stated that there were no barriers to seeking professional help in the context of their rural town.
Discussion
Summary of the findings
Main findings of this study were that 55.7% of the sample indicated that they would seek help for a mental health problem. The majority of participants, regardless of subgroup, indicated that they would seek help for a mental health problem from a school counsellor. An observed gender difference was that male participants had a higher preference for seeking help from a psychologist than females. Furthermore, older adolescents were more likely to seek help from a GP than younger participants.
A multivariate analysis of help-seeking intentions revealed overall that ARIA was the only predictor of help-seeking intention; however, when extreme depression and anxiety scores were used as predictors they also became significant. A content analysis of the barriers to help-seeking nominated by participants revealed that perceived limited availability of professional services in the town, perceived social proximity and fear of rural gossip, and difficulties associated with travelling to obtain help were the most significant concerns for these youth.
Interpretation and implications of the findings
That the majority of rural adolescents in this study who indicated that they would seek help for a mental health problem is encouraging; however, there was still a sizeable proportion of the sample who reported that they would not seek help for a problem. This suggests further work is needed to improve help-seeking intention among rural adolescents. Ideally, all youth should report an intention to seek help for a mental health problem if they were to experience one, regardless of whom they would prefer to seek help from (ie formal and informal sources of support). For those who were not willing to seek help for a mental health problem in this study, concerns relating to the stigma of mental illness were the most frequently raised and this suggests the need for anti-stigma campaigns in rural areas.
In terms of help-seeking preferences, the first choice for the majority of participants regardless of sex, age, or location was the school counsellor. There are several possible reasons for this including trust, rapport, availability, accessibility, and no cost. One of the implications of this finding is the need to provide adequate training and support to school counsellors who are at the front line of youth mental health in rural areas. Distance and online models of education, training, and supervision must be further developed and made available to rural practitioners. Furthermore, the number of trained school counsellors should be systematically increased.
The finding that adolescents were more likely to seek help for a mental health problem if they lived in an outer regional area compared to an inner regional area was contrary to prediction. The researchers' expectation, based on previous research suggesting that social stigma of mental illness is amplified in small rural communities17,21, was that those in outer regional areas would be less likely to seek help. However, as Parr discusses, social proximity is a 'double-edged sword'21. While the experience of social stigma in small communities may be more pronounced, the sense of community may also be a protective factor. It is possible that adolescents in this study were more likely to seek help with increasing rurality due to the stronger sense of community and higher social capital in rural communities22-24 . It is interesting to speculate whether the recent hardships experienced by outer regional communities due to the drought may have strengthened sense of community in these areas. These hypotheses warrant further investigation.
The assumption that adolescents are less likely to seek professional help the more rural the location in which they reside was not supported. This suggests that help-seeking attitudes should not be the only target for intervention. In the rural context, it may be more important in terms of primary prevention of mental health problems to focus on community-wide strategies to reduce the barriers associated with help-seeking delays, rather than simply focusing on mental health literacy. The main barriers associated with obtaining professional help within a rural community were the perceived availability of services, concerns about confidentiality and anonymity in the context of high social proximity, and the need to travel long distances in order to gain access. Each of these factors should be specifically addressed in the design and development of rural primary prevention programs. This also involves the need to think outside the school to ways in which the whole community can be engaged in primary prevention efforts22.
Finally, the finding that young people experiencing high levels of depression are less likely to express an intention to seek help supports previous research on help-seeking and mental health status. Unfortunately, the more depressed a young person feels, the less likely they are to seek help for their problems due to feelings of alienation and low expectations of the future11. The implications of this finding is clear and have been heralded nationwide in recent years - detect and intervene early1.
Research implications of the present study include the need for a reliable and valid measure of help-seeking barriers that is relevant to rural youth as well as a need for epidemiological data on the mental health of the rural population. In the absence of a measure of help-seeking barriers specific to rural environments, the hypothesis 'the more rural the location in which adolescents reside the more barriers to seeking professional help they face' cannot be tested, although there is accumulating evidence that this is the case. In addition, in the absence of good epidemiological data it cannot be concluded that the mental health of youth is poorer with increasing rurality. To advance the agenda of rural adolescent mental health, this research is sorely needed.
Methodological limitations
The present study represents an attempt to gain information on the preferences and intentions towards help-seeking for mental health problems from a normative sample of rural adolescents. However, as is often the case in adolescent and rural research, the research fell short of this aim. While the sample was sufficiently large for testing the hypotheses and for undertaking planned data analyses, its representativeness is questionable. Of the 42 rural schools approached, only 8 schools agreed to participate in the study. Of the adolescents who were asked to participate, less than 50% returned the consent form in time to take part.
Other limitations of the study relate to research design. The study is cross-sectional and quasi-experimental and, therefore, it is not possible to infer causality. Moreover, the study focused on the preferences and intentions of rural youth. As the link between attitudes and behaviour is not absolute, it should not be assumed that intentions necessarily result in help-seeking behaviour.
Conclusions
This study represents an attempt to better understand the help-seeking intentions and preferences of rural adolescents. While just over half of the participants indicated that they would seek help for mental health problems, almost half the sample indicated that they would not seek help of any kind. Furthermore, participants identified a series of barriers to help-seeking related to living in a rural environment. Much work is needed in the rural adolescent mental health area to improve access to services and reduce barriers to help-seeking in order to ultimately improve mental health outcomes for rural youth in Australia.
Acknowledgments
The first author expresses her gratitude to Dr Jack Harvey from the School of Human Movement at the University of Ballarat for his advice on the multivariate analysis of the data for this study, and to Dr Marieke Zwaanswijk from the Netherlands Institute for Health Services Research for her helpful comments during the drafting of this article. The thanks of all the authors is extended to Associate Professor John McDonald at the School of Behavioural and Social Sciences and Humanities, University of Ballarat for his on-going support of our research.
References
1. McGorry P, Purcell R, Hickie I, Jorm A. Investing in youth mental health is a best buy. Medical Journal of Australia 2007; 187(7Suppl): S5-S7.
2. Patel V, Flisher AJ, Hetrik S, McGorry P. Mental health of young people: a global public-health challenge. The Lancet 2007; 369: 1302-1313.
3. Conus P, McGorry PD. First-episode mania: A neglected priority for early intervention. Australian and New Zealand Journal of Psychiatry 2002; 36: 158-172.
4. Steinhausen HC, Rauss-Mason C, Serdel R. Follow up studies of anorexia nervosa: A review of four decades of outcome research. Psychological Medicine 1991; 21: 447-451.
5. Stephensen J. Delay in treating schizophrenia may narrow therapeutic window of opportunity. Journal of the American Medical Association 2000; 282: 2091-2092.
6. Hodges CA, O'Brien MS, McGorry PD. headspace: National Youth Mental Health Foundation: making headway with rural young people and their mental health. Australian Journal of Rural Health 2007; 15: 77-80.
7. Boyd CP, Aisbett DL, Francis K, Kelly M, Newnham K, Newnham K. Issues in rural adolescent mental health in Australia. Rural and Remote Health 6:501. (Online) 2006. Available http://www.rrh.org.au (Accessed 22 December 2010).
8. Leong FTL, Zachar P. Gender and opinions about mental illness as predictors of attitudes toward seeking professional psychological help. British Journal of Guidance & Counselling 1999; 27: 123-133.
9. Ciarrochi J, Wilson C J, Deane FP, Rickwood D. Do difficulties with emotions inhibit help-seeking in adolescence? The role of age and emotional competence in predicting help-seeking intentions. Counselling Psychology Quarterly 2003; 16: 103-120.
10. Schonert-Reichl KA, Muller, JR. Correlates of help-seeking in adolescence. Journal of Youth and Adolescence 1996; 25: 705-727.
11. Deane FP, Wilson CJ, Ciarrochi J. Suicidal ideation and help-negation: not just hopelessness or prior help. Journal of Clinical Psychology 2001; 57: 901-914.
12. Quine S, Bernard D, Booth M, Kang M, Usherwood T, Alperstein G et al. Health and access issues among Australian adolescents: a rural-urban comparison. Rural and Remote Health 3:245. (Online) 2003. Available http://www.rrh.org.au (Accessed 22 December 2010).
13. Francis K, Boyd CP, Aisbett DL, Newnham K, Newnham K. Rural adolescents' perceptions of barriers to seeking help for mental health problems. Youth Studies Australia 2006; 25: 42-49.
14. Boyd CP, Francis K, Aisbett D, Newnham K, Sewell J, Dawes G et al. Australian rural adolescents' experiences of seeking psychological help for a mental health problem. Australian Journal of Rural Health 2007; 15: 196-200.
15. Sullivan K, Marhsall SK, Schonert-Reichl, KA. Do expectancies influence choice of help-giver? Adolescents' criteria for selecting an informal helper. Journal of Adolescent Research 2002; 17: 509-531.
16. Lindsey, CR, Kalafat, J. Adolescents' views of preferred helper characteristics and barriers to seeking help from school-based adults. Journal of Educational Psychology and Consultancy 1998; 9: 171-193.
17. Aisbett DL, Boyd CP, Francis K, Newnham K, Newnham K. Understanding barriers to mental health service utilization for adolescents in rural Australia. Rural and Remote Health 7:624. (Online) 2007. Available http://www.rrh.org.au (Accessed 22 December 2010).
18. GISCA. About ARIA+ (Accessibility/Remoteness Index of Australia). (Online) no date. Available: http://gisca.adelaide.edu.au/projects/category/about_aria.html (Accessed 3 August 2010).
19. Radloff LS. The use of the Centre for Epidemiological Studies Depression Scale in adolescents and young adults. Journal of Youth and Adolescence 1991; 20: 149-166.
20. Zung WWK. A rating instrument for anxiety disorders. Psychosomatics 1971; 11: 371-379.
21. Parr H, Philo C Rural mental health and social geographies of caring. Social and Cultural Geography 2003; 4: 471-488.
22. Boyd CP, Hayes L, Wilson RL, Bearsley-Smith C. Harnessing the social capital of rural communities for youth mental health: an asset-based community development framework. Australian Journal of Rural Health 2008; 16: 189-193.
23. Pretty GH, Chipuer H M, Bramston P. Sense of place amongst adolescents and adults in two rural Australian towns: The discriminating features of place attachment, sense of community and place dependence in relation to place identity. Journal of Environmental Psychology 2003; 23: 273-287.
24. Pretty G, Bramston P, Patrick J, Pannach W. The relevance of community sentiments to Australian rural youths' intention to stay in their home communities. American Behavioural Scientist 2006; 50: 226-240.
___________________________-
Appendix I: Survey on help seeking







