Introduction
Australia's rural and remote medical workforce shortages are well documented. Responses have included the growth of rurally oriented medical schools and rural placements, rural scholarships, rural incentives and other retention strategies, and the development of training pathways into rural medicine1-4. The Australian College of Rural and Remote Medicine (ACRRM) has developed a training pathway, standards, and a Fellowship examination in rural and remote medicine5. The Royal Australian College of General Practitioners (RACGP) has its own pathway and endpoint for a qualification in rural general practice6. Australian doctors can train towards either or both endpoints and be recognized as specialists in rural medicine through ACRRM's independent pathway, or via Australian General Practice Training or the Remote Vocational Training Scheme (RVTS)7,8.
Queensland Health's Rural Generalist Pathway (RGP) provides a supported career pathway for junior doctors to train in rural and remote medicine which joins rural medical educational strategies with rural medical workforce and practice strategies. This article describes how Queensland Health has developed the pathway to meet the needs of Queensland's rural and remote communities, and outlines experience in the pathway since its establishment in 2007.
Queensland Health's Rural Generalist Pathway
What is a Rural Generalist?
Rural Generalists are rural doctors providing a broad range of services including specialised skills such as emergency medicine, obstetrics, or anaesthesia, usually with a relevant fellowship qualification9. The Rural Doctors Association of Australia (RDAA) comments:
The term 'rural generalist' has been used to emphasise the expansive nature of the professional role required to meet community needs in rural and remote practice. This includes providing care in general practice or primary care AND secondary care such as rural hospitals or other extended settings.
Terms like 'extended general practice' are also used. The RDAA suggests10 the:
...philosophy that underpins this set of principles is that any advanced training program must include training in community based general practice and the professional role of the doctor completing the program must accommodate the provision of a continuum of comprehensive care across general practice.
A rural generalist is an extended medical generalist. ACRRM's president Richard Murray asserts11:
Generalism in clinical medicine has retreated in the face of the rise of medical sub-specialisation throughout the twentieth century... [arguing the] ...extended medical generalist role will be a key pillar for our health care future.... ACRRM is committed to building pathways for the naturally adventurous, generalist-inclined medical graduate to pursue diverse and interesting careers as an extended medical generalist - with an emphasis on the bush.
The RGP is one such pathway.
Within Queensland Health, a 'Rural Generalist' (RG) specifically refers to a rural doctor credentialed to serve in9:
- hospital-based and community-based primary medical practice, and
- hospital-based secondary medical practice:
- in at least one specialist medical discipline (eg obstetrics, anaesthetics, and surgery) AND
- without supervision of a specialist medical practitioner in the relevant disciplines
- and possibly hospital- and community-based public health practice - particularly in remote and Indigenous communities.
Background
In 2005 a seminal meeting in the Queensland town Roma of representatives of Queensland Health, ACRRM, and other stakeholders established 'The Roma Agreement', which committed to12:
...develop and sustain an integrated service and training program to form a career pathway supplying the Rural Generalist workforce that the bush needs.
This agreement fulfilled the State Government's promise of a specialist career pathway for RGs, a component of the Queensland Government's response to the Bundaberg Hospital Commission of Inquiry13. The Roma Agreement has a jurisdictional objective: supplying rural generalists to both the public and private sectors of the bush - and articulated nine key principles (Fig1).

Figure 1: The Roma Principles.
The agreement arose in response to the failure of supply of Queensland's rural and remote workforce which was evident early in the 21st century despite substantial strategy and initiatives by Commonwealth and state governments, colleges and education providers over the preceding 15 years. Queensland had enjoyed reasonable success in recruiting medical superintendents and medical officers with 'right to private practice' to service smaller towns using a blended payment system (retainer plus private practice), with rostered relief and locum support. However, the salaried Senior Medical Officer (SMO) workforce in larger rural centres was in decline, with such dependency on international medical graduates (IMGs) that by the early 2000s rural IMG workforce management dominated Queensland rural medical workforce planning and strategy. In all, 52% of Queensland rural and remote workforce in 2008 were IMGs, compared with the national average of 41%12.
Applications to Queensland's long-standing rural medical scholarship scheme were also declining with fewer applicants than scholarships. Contract breaching rates almost equalled the rate of return of rural service. Fears were expressed that this decline was terminal, that graduates from Australian medical schools would not aspire to rural careers, and that the obvious solution to rural and remote medical care in Queensland was enhancement of the retrieval and transport service to transfer patients to larger centres. Workforce data suggested a 'disappointing' 3.8% of the state's medical graduates from 1990 to 2007 were working in rural and remote Queensland12.
A state-wide survey of SMOs across 35 rural and remote hospitals in 2001 articulated the key issues of career choices and intentions, work roles and educational needs, leading to re-appraisal of the question, 'Can any more be done to recruit and retain an Australian medical graduate rural and remote workforce?'. This survey provided the evidence for a new supply-line strategy, based on three key advances.
First, it was acknowledgement that the uniqueness and value of a career in rural and remote medicine needed recognition in order to stimulate the interest of a new generation of Australian graduates. No formal mechanism existed in Queensland for the recognition of disciplines other than the Medical Board's Specialist Register. A State Credentials Committee was established to assess whether new disciplines in medicine should receive formal recognition based on key criteria of benefit in patient safety, improved healthcare outcomes and value for money, and the qualifications prescribed, scope of clinical practice and applicable salary range for each discipline. Rural Generalist Medicine was recognised by the State as a distinct discipline in its own right in 2008. The unique body of knowledge and skills defining rural practice was outlined in ACRRM's Primary Rural and Remote curriculum statements and the approved Advanced Specialised Training curricula5.
Second, negotiation of a critical first medical enterprise bargaining agreement in 2005 provided parallel capacity in industrial terms to recognise the value to Queensland of practice in Rural Generalist Medicine. The ensuring industrial agreement enabled salaried SMOs with credentials in Rural Generalist Medicine to access a new salary range (Medical Officer Advanced Credentialed Practice) with equivalent commencing salary levels to Staff Specialists.
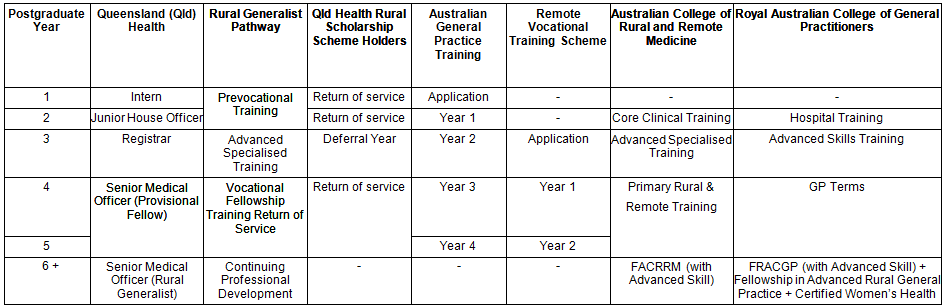
Finally, detailed exploration of existing vocational pathways to rural practice helped better understand the reasons for the undersupply. A new training pathway was devised building on existing training arrangements (Table 1). The intent was to enhance rather than duplicate existing pathways, blending a training program with a career pathway and industrial recognition in an attractive, incentive-based strategy to provide a sustainable medical workforce for rural Queensland. The pathway's design enabled state government scholarship holders to meet return-of-service requirements concurrently with their vocational training program9.
Table 1: Summary of Rural Generalist training and significant milestones
Operation of the Pathway
Medical students apply to the RGP in their final year of training through a formal merit-based selection process. They commence the pathway on starting internship, needing to have gained professional registration and a quarantined intern position at an RG training hospital.
Postgraduate years (PGY) 1 and 2 comprise the prevocational training component of the pathway. Rural Generalist trainees apply for formal general practice training during internship, commencing training in PGY2. After prevocational certification, trainees undertake Advanced Specialised Training (AST), usually in their third year, in one of a range of approved disciplines. They then undertake further vocational training in PGY 4 and 5 in a rural location, often their practice of destination (Table 1, Fig2).
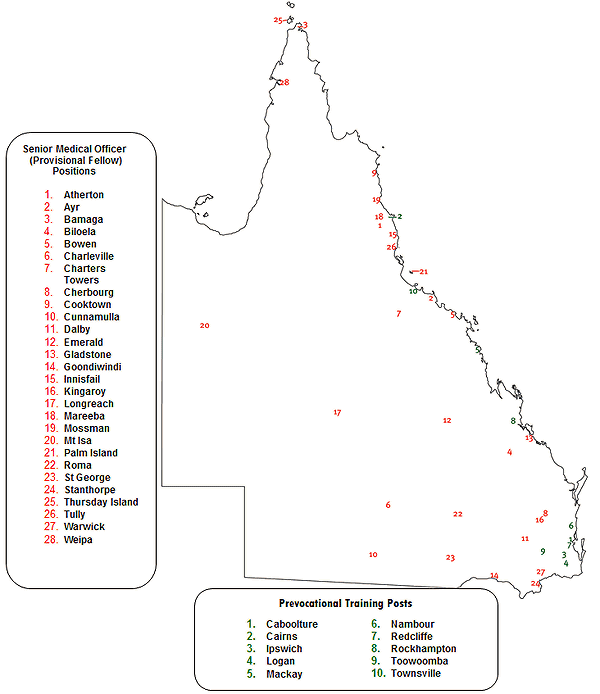
Figure 2: Rural Generalist training position locations.
The RGP's design is flexible, with only one move of location required during training. Postgraduate years 1-3 can be completed in a single location, usually a regional or outer metropolitan hospital. Training from PGY 4 is in a rural location (Table 1)9.
The pathway is managed by a team of experienced rural medical advisors, clinicians, educators and administrators. The pathway Co-Directors are geographically dispersed throughout Queensland with fractional appointments in addition to their substantive roles in clinical practice, management, education and policy. This group has developed a management and governance framework which ensures high-level advocacy and representation, and supports trainees progressing through the pathway. The RG educators regularly meet with trainees, mapping their training through the Vocational Indicative Planning process, which matches educational, personal (including family) and workforce needs with available posts and other requirements including scholarship obligations. The RG team provide training advice, assist with negotiating posts, and liaise with supervisors, hospitals and Regional Training Providers. Workshops are arranged for trainees in PGY 1 and 2, which offer specific skills training, acculturation to life as an RG, additional time for vocational planning, and social and networking opportunities.
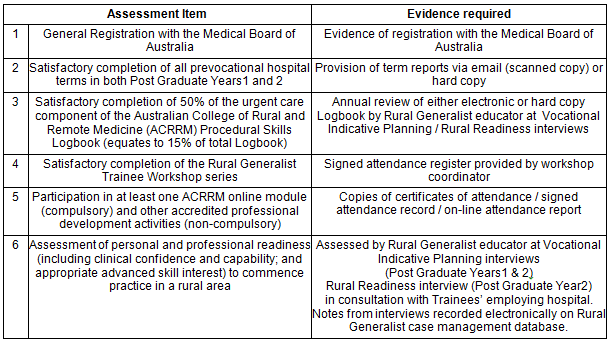
Trainees need to meet some important milestones to achieve prevocational certification (Table 2). Prevocational assessment, developed in partnership with ACRRM, evaluates an individual's capacity to practise safely in a supervised rural setting, and is required to progress to AST or rural practice. It enhances the educational pathway and is required for certain industrial remuneration benefits. Trainees must enrol with a regional training provider for their core vocational training and balance priorities of location and vocation in order to make decisions about AST choice, geographic area of practice, and vocational endpoint9. Seven trainees in remote locations have undertaken their vocational training via the RVTS8.
Table 2: Rural Generalist prevocational requirements
Rural Generalist trainees with prevocational certification undertake AST in PGY 3 or beyond. Training posts are usually for 12 months and are currently established in the following specialties:
- anaesthetics
- obstetrics and gynaecology
- emergency medicine
- surgery
- Indigenous health
- internal medicine
- paediatrics
- mental health.
The choice of AST relates to the skills needed in rural Queensland hospitals, and is based on an agreed curriculum and assessment which would enable recognition of that skill by a Queensland Health credentialing committee. For example, a trainee with advanced anaesthetic skills could be credentialed to provide an unsupervised anaesthetic service in a rural hospital. Appointment as a SMO or Medical Officer with right of private practice to a post specifying this skill in the position description, would ensure eligibility for industrial recognition at Staff Specialist salary levels as a 'Provisional Fellow'.
Rural Generalist trainees complete training, including Fellowship requirements (FACRRM and/or FRACGP) in an accredited rural hospital, often their location of final destination, and may also take up private practice options or have part-time hospital roles, perhaps with a hybrid public-private appointment.
The pathway enhances existing pathways to vocational recognition through Regional Training Providers or RVTS, aiming to add value through the Vocational Indicative Planning process, career advice, additional workshops and other targeted activities. The endpoint is dual: college fellowship but also sign-off by the RGP at prevocational and vocational levels, including certified and credentialed advanced skills. This combination has important industrial implications. The pathway matches choice of AST to clinical needs, job descriptions and industrial recognition.
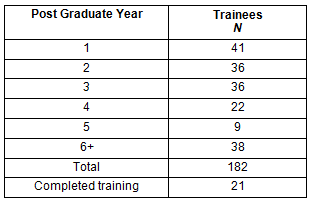
From an initial intake of 30 trainees in 2007, the pathway has grown to 21 trainees completing the program and a current enrolment of 182 (Table 3). Entry is competitive and over-subscribed, with a cohort of 41 commencing training in 2012 across 10 intern training hospitals. In late 2011, 78 trainees were undertaking accredited vocational training in rural practice - significantly, providing medical services as Provisional Fellows while completing training - with 24 of these (30%) concurrently or wholly in private general practice9. In all, 53 trainees have completed AST posts with a further 37 undertaking training in 2012.
Table 3: Rural Generalist trainees by year (as at 17 December 2012)
The Future
Rural generalism is an idea whose time has come. Key organizations are calling for the implementation of a National Advanced Rural Training Pathway to support and encourage practice in rural and remote communities10. Many jurisdictions are developing their own approaches to rural generalist training, based on the principles developed by the Queensland pathway, and responsive to local needs. As rural training expands nationally there is a need for transferability across all training posts including ASTs, and increased efforts to align training with future workforce needs. Challenges to be overcome include matching training pathways with professional and industrial recognition and career progression in each jurisdiction, and overcoming perceptions that the pathway focuses on hospital/procedural medicine at the expense of private general practice.
In Queensland, the pathway is evolving as trainee numbers grow. Work is ongoing to ensure smooth engagement of trainees with the pathway, and to increase capacity, particularly in AST posts, and to match pathway graduates with workforce requirements and community needs. New approaches are being developed to co-ordinate AST applications. Further evaluation is planned, which can inform development of additional training posts, establishment of ASTs in other disciplines, and cross-accreditation of training such as Generalists in Emergency Medicine.
Conclusion
The RGP offers a supported fast-tracked path to procedural rural medical practice, providing a career path for doctors in rural Queensland. The pathway is flexible, minimising moves of location for the trainee, interfacing with other training providers and Colleges, and offers engagement with Queensland Health throughout training. The pathway matches return-of-service with career progression, high quality training, a recognized portable qualification, and near-specialist remuneration. The pathway is part of the pipeline to rural practice, harmonising with other rural initiatives including incentives, increased focus on rural training and growing numbers of students and junior doctors. This approach could be adopted by other jurisdictions, and perhaps by other disciplines.
References
1. Murray RB, Wronski I. When the tide goes out: health workforce in rural, remote and Indigenous communities. Medical Journal of Australia 2006; 185: 37-38. Available: http://www.mja.com.au/public/issues/185_01_030706/mur10288_fm.html (Accessed 14 May 2013).
2. Eley D, Baker P. Does recruitment lead to retention? - Rural Clinical School training experiences and subsequent intern choices. Rural Remote Health 6: 511. (Online) 2006. Available: www.rrh.org.au (Accessed 14 May 2013).
3. Magnus JH, Tollan A. Rural doctor recruitment: does medical education in a rural district recruit doctors to rural areas? Medical Education 1993; 27: 250-253.
4. Sen Gupta TK, Murray RB, McDonell A, Murphy B, Underhill AD. Rural internships for final year students: clinical experience, education and workforce. Rural Remote Health 8: 827. (Online) 2008. Available: www.rrh.org.au (Accessed 14 February 2013).
5. ACRRM. ACRRM Vocational training. (Online) 2012. Available: https://www.acrrm.org.au/vocational-training (Accessed 1 March 2012).
6. RACGP. The RACGP National Rural Faculty. (Online) no date. Available: http://www.racgp.org.au/rural (Accessed 1 March 2012).
7. AGPT. Australian General Practice Training. (Online) no date. Available: http://www.agpt.com.au/ (Accessed 1 January 2012).
8. RVTS. The Remote Vocational Training Scheme. (Online) no date. Available: http://www.rvts.org.au/ (Accessed 1 May 2012).
9. Queensland Government. Rural Generalist Training. (Online) 2013. Available: http://www.health.qld.gov.au/ruralgeneralist/default.asp (Accessed January 2012).
10. RDAA. Meeting the health needs of rural and remote Australia through an integrated strategic framework - an Advanced Rural Training Program. (Online) 2012. Available: http://www.rdaa.com.au/Uploads/Documents/NARTP%20Key%20Principles%20-%20final%20-%20February%202012_20120305123719.pdf (Accessed 1 March 2012).
11. Murray RB. Focus on the job and the pathway will follow. Australian Doctor 2012; 2 March. Available: www.australiandoctor.com.au (Guest editorial).
12. Queensland Government. A brief history of the Rural Generalist Pathway. (Online) 2007. Available: http://www.health.qld.gov.au/ruralgeneralist/docs/brief_history.pdf (Accessed 21 May 2013).
13. Bundaberg Hospital Commission of Inquiry. Queensland Health Initial Submission. (Online) 16 May 2005. Available: http://www.health.qld.gov.au/inquiry/submissions/INQUIRY.pdf (Accessed 1 April 2012).





