Rural Health Clinics (RHCs) have served the primary healthcare needs of the medically underserved in US rural areas for more than 30 years. Today's approximately 4000 RHCs throughout the nation face multiple challenges. Not only do they serve populations with higher percentages of elderly and higher rates of chronic disease compared with urban populations, they also continue to struggle to attract and retain qualified professional staff.
Accountable Care Organizations (ACOs) pose potential opportunities for addressing the healthcare needs of rural populations (Fig1). Established through the Patient Protection and Affordable Care Act (PPACA or ACA), ACOs are provider-run (physicians, hospitals, and/or other healthcare organizations) groups that accept responsibility for the cost and quality of care of a defined population. Despite several rural constraints to ACO participation, opportunities exist for rural providers to improve care and share in the cost savings that will become available through the ACA1.

Figure 1: Definition of Accountable Care Organizations.
There are many variations of ACOs. One means of describing them is by sponsor - a healthcare provider, an insurance company, or Medicare. Medicare offers several ACO programs, including the Pioneer ACO, the Shared Savings Program ACO, and the Advance Payment Initiative ACO. RHCs may participate in the Medicare Shared Savings Program (SSP), either independently or as one of several healthcare organizations.
Despite their potential benefits, little is known about how the ACO model will accommodate the unique challenges of RHCs. Moreover, little is known about the extent to which RHCs will participate in ACOs, nor the characteristics of RHCs that choose to participate (or not participate) in ACOs.
This article reports on the results of a survey, focus groups, and phone interviews with RHC management personnel on the subject of benefits and barriers to RHC participation in ACOs. These research methods were among a variety of analytical approaches used in a multi-year study of the clinical and economic outcomes of RHCs in the Southern USA. How ACO participation influences RHC outcomes is a particular focus of this multi-year study. The survey, focus groups, and phone interview investigation was driven by the research question:
What are the benefits of and barriers to RHC participation in ACOs from the perspective of RHC management personnel?
Previous studies
Although some healthcare organizations exhibited ACO-like characteristics in the early 2000s and earlier, most ACO development has taken place since January 2012. Since that time, Medicare has certified three waves of ACOs through its Pioneer Program and SSP. In addition, numerous hospital systems, insurers, and provider groups have formed ACOs. The growth of ACOs may be more common in urban areas. One study found rural regions of the US to have little ACO growth before September 20112. Factors contributing to this slow rural growth and the actual penetration of ACOs in rural areas are not clear, and the extent to which ACOs will include rural areas remains to be seen.
The benefits of and barriers to rural provider participation in ACOs can be viewed from two perspectives: that of the ACO sponsoring or founding organizations, and that of the rural providers as they consider the strategic advantages of participation. A description of potential benefits and barriers, and recent related literature follows.
Benefits: There are several potential opportunities for rural primary-care practices that choose to join ACOs. These may be summarized as follows.
Improved population health One fundamental goal of ACOs is that they will improve the health and wellness of a defined population for which the ACO is accountable. This goal is promoted by increasing the emphasis on preventive care provided by primary care services, and coordinating services across levels of care.
Improved patient quality of care Healthcare organizations that participate in ACOs receive incentives for meeting quality standards of care while at the same time lowering growth in healthcare costs. Medicare's SSP has 33 quality performance standards that ACOs must meet, with the objective of achieving two broad aims: (i) better care for individuals; and (ii) better health for populations.
A focus on the patient ACOs are systems of healthcare organizations that, like Patient-Centered Medical Homes (PCMHs), are patient-focused. ACOs also emphasize the use of teams to care for the individual patient across care settings. These settings include the primary care provider, hospitals, and long-term facilities. Coordinating services is aimed at reducing fragmentation - an outcome that may prove not only advantageous to the ACO partners, but also for the insurers that contract with them, as well as employers3.
Physician leadership Whereas the managed care model was dominated by insurance companies, the ACO model allows its physicians to decide how to best care for their patients.
In their case study of the Advocate Physician Partners' ACO, Shields et al view physician governance in ACOs as contributing to physician acceptance of performance measurement and improvement4. In RHCs, physicians make up approximately half of the professional staff; nurse practitioners compose another approximately 40%. ACOs may be attractive to RHCs provided these professionals are able to take on active leadership roles.
Lower costs Achieving cost savings is one of the two primary goals of ACOs (the other being providing high quality care to a defined population). The cost savings would be achieved by emphasizing preventive care, increasing operational efficiencies, and reducing hospital readmissions. Thus, ACOs may contribute to meeting America's challenge of providing cost-effective care to growing numbers of chronically ill3.
Shared savings From a practical standpoint, primary-care practices could achieve financial benefit through their participation in such programs as the Medicare Shared Savings ACO Program. ACOs that participate in the Medicare SSP will be rewarded for lowering their growth in healthcare costs while meeting quality standards. Centers for Medicare & Medicaid Services (CMS) will apply a sharing rate to the difference between a benchmark and actual expenditures for the performance year. (This benchmark is updated for growth in national per capita expenditures for Parts A & B Medicare services, and adjusted for changes in severity and case mix of the Medicare beneficiaries.)
Barriers: In addition to the possible benefits, researchers have posed several barriers or drawbacks to ACO participation for rural healthcare providers. These relate to the distinctive cultures of rural healthcare providers, their infrastructure needs, and meeting the requirements of ACOs as established by the Federal Government.
The unique mission of RHCs Rural Health Clinics are dedicated to providing cost effective health care to rural underserved areas. RHCs may perceive that partnering with other providers that serve geographic areas outside their vicinity would detract from their dedication to immediate communities.
Anticipation of losing autonomy Many rural providers, including RHCs, have operated independently for years or often decades. Over time, these providers have become accustomed to operating in relative autonomy and have developed distinct cultures reflecting their owners, administrators, and communities. The merging of cultures necessary for ACO development would require not only time, but a fundamental change in approach to conducting business for many RHCs.
Inadequate capital for information technology improvements Although RHCs qualify to participate in SSP ACOs, either independently or along with other providers, many do not have adequate financial resources to develop the information technology systems necessary for coordinating care - one of the primary goals of ACOs. Care coordination is a basic tenant of ACOs and requires teamwork and information infrastructure systems that support data sharing. Shortell and Casolino stress that ACOs that are comprised of small practices, as well as most Independent Practice Associations (IPAs) and many Physician Hospital Organizations (PHOs), would need technical assistance to restructure their practices in order to be successful5. Nationwide, the mean size of RHCs (as measured by physicians + nurse practitioners + physician assistants) was 2.956. Thus, many Rural Health Clinics exemplify the small practices that would need technical assistance in order to successfully participate in ACOs.
Payment structure/financing Rural providers that participate in Medicare ACOs have the opportunity to share in cost-savings. However, in that many rural providers are small, they may not feel they have adequate negotiating power to compete for an appropriate share in the savings of an ACO that is led by a large, integrated system.
Legal and regulatory barriers RHCs may perceive that there are regulatory barriers to their participation in ACOs. However, the final rule on the Medicare SSP does allow for RHCs to form ACOs independently or with other healthcare providers. An additional 'de-motivator' is that ACOs require contractual and/or legal agreements between hospitals and other providers that align incentives - a difficult goal particularly for rural providers that are less accustomed to collaborations between multiple providers1.
Population base is not large enough RHCs serve non-urbanized areas that are designated as Health Professional Shortage Areas or Medically Underserved Areas. One requirement of Medicare ACOs is that they serve at minimum 5000 Medicare beneficiaries. The population density of many RHCs' service areas is simply too low to meet this minimum threshold.
Other barriers MacKinney et al identified several additional constraints or 'de-motivators' to ACO participation for rural providers1. Among these are rural efficiency and rural leadership inexperience. Many rural providers, they explain, are already efficient in managing expenses because they are accustomed to 'doing more with less'. Thus, they are less likely to be improving on efficiency by participating in ACOs. In addition, providing healthcare in rural areas reinforces independence and autonomy and does not offer providers many opportunities to cultivate leadership skills in settings with multiple collaborators.
A combination of three research methods was used to gather and analyze RHC opinions about the benefits of or barriers to ACO participation: survey research, focus groups, and phone interviews. The survey also analyzed a variety of RHC characteristics, including organizational structure, clinical practices, data collection, and information infrastructure. Several of the survey questions were written from the perspective of the Medicare SSP because it is the model in which RHCs are more likely to participate.
The study population was composed of all RHCs existing in 2011 in Region 4 (as designated by the Department of Health and Human Services) and reported in the CMS Online Survey, Certification and Reporting (OSCAR) database. Region 4 encompasses the following states: Mississippi, Alabama, Florida, Georgia, North Carolina, South Carolina, Tennessee, and Kentucky. The total study population was 870 RHCs or approximately 23% of all RHCs in the USA.
It was postulated that the knowledge of and attitudes regarding ACOs among Region 4 RHCs would differ from those of other regions of the country, as would their willingness to join ACOs. RHCs in California were surveyed for comparison purposes. As of 2011, there were 274 RHCs in California comprising 7% of the US total.
Survey
The research team drafted approximately seven to ten questions for each theme. Next, the team reduced the number of questions and grouped the final questions into three sections to guide the respondent: (i) RHC organizational structure and culture; (ii) healthcare delivery models for RHCs; and (iii) data collection and infrastructure. An advisory committee composed of five RHC clinical and administrative management personnel contributed to the development of the survey as well as the interpretation of its results.
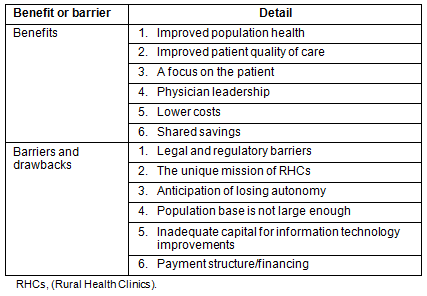
Several benefits of and barriers to RHC participation in ACOs were proposed in the survey. These were developed from the literature and are described as follows (Table 1).
Table 1: Benefits of and barriers to Accountable Care Organizations
The survey was pre-tested to examine its internal face validity. Draft surveys were mailed to a random sample of 20 RHCs drawn from the study population and stratified by state. Respondents were asked to complete the survey, and to comment on the length of the survey, as well as the clarity of the survey questions and responses. Based on the results of the pre-test, the survey tool was modified by re-wording the questions and responses, and by reducing the number of questions.
The final version of the survey was distributed to all 1144 RHCs (870 in Region 4 and 274 in California) during the Spring of 2012. The surveys were sent by postal service mail to 1015 RHCs and by email to 129 RHCs, accompanied by a cover letter and informed consent form. In an effort to increase the response rate, a second mailing was distributed. Two reminder emails and a second email distribution were conducted to increase number of the email responses.
Survey analysis: Data collected from the returned surveys were double-entered. The data were cleaned using a range checking method. The survey data were analyzed in two stages. First, descriptive statistics were used to summarize the characteristics of the clinics and their responses. Second, bivariate analyses were conducted of several relationships using a variety of statistics including analysis of variance, Pearson's χ² and likelihood χ². The relationships were examined between the RHCs' willingness to join ACOs and the respondent clinic's classification (as provider-based or independent). In addition, willingness to join ACOs were compared among Region 4 RHCs with those of California RHCs.
Focus groups and phone interviews
In order to gain a broader understanding of the results of the survey, focus groups and interviews by phone were conducted with RHC personnel. Ten questions were formulated for the focus group sessions. These explored the following themes: the organizational structure of the participant's RHC, the participant's knowledge of ACOs, and the participant's opinions about the benefits or and barriers to joining ACOs. Although several focus group sessions were scheduled, it proved to be difficult to coordinate the participants' schedules. It was found necessary to conduct phone interviews with individuals who were not able to attend one of the focus group sessions.
Sample: From all RHCs existing in Region 4 during 2011 that did not respond to the survey, a random sample of 40 RHCs was created using cluster sampling. The sample size from each state was in proportion to the percentage of RHCs in that state as compared with all Region 4 states. Management personnel from each of these RHCs were invited to participate in the focus groups to discuss their opinions about RHC participation in ACOs.
Data collection: Formal consent was obtained from each participant to the focus group session or interview. Each session was conducted by a moderator. Two researchers maintained notes during the sessions.
The discussion during each session was guided by 8 open-ended questions about the participants' knowledge of ACOs, and the benefits of or barriers to RHC participation in ACOs. Questions were formulated from the literature with input from the research team's advisory committee of RHC practitioners. Each session was limited to approximately 20 min.
Data analysis: The qualitative narratives were analyzed using content analysis procedures. For each question, responses were compiled and recurrent themes or patterns were identified as they emerged from the text. The themes or patterns were organized and frequencies for each theme were tabulated.
Ethics approval
Approval for the focus groups and phone interviews, and to conduct the research was obtained from the University of Central Florida's IRB (SBE-11-07815).
The more notable results from the survey, focus groups, and phone interviews are described in this section. Survey results are also summarized (Table 2).
Survey respondents and focus group participants
A total of 90 RHCs responded. The characteristics of the survey respondents are illustrated (Table 2). After subtracting the number of surveys for the pre-test and those returned with invalid addresses, a total of 1105 surveys remained: 848 from Region 4 RHCs and 257 from California RHCs (Fig2). This yielded a response rate of 8.1% overall (7.5% for Region 4, and 10.1% for California). The focus groups and interview participants included eight management personnel of whom five were administrators/practice managers and two were clinical managers, and one had both clinical and non-clinical management responsibilities. Survey, focus group and interview participants represented both independent and provider-based RHCs.
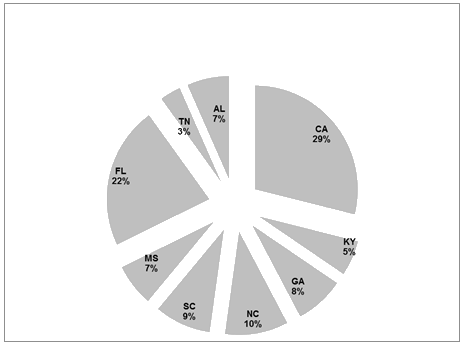
Figure 2: Survey respondent Rural Health Clinics by state; AL, Alabama;
CA, California; FL, Florida; GA, Georgia; KY, Kentucky;
MS, Mississippi; NC, North Carolina; SC, South Carolina; TN, Tennessee.
Knowledge
The survey respondents' degree of knowledge about ACOs is shown (Fig3). Almost half (48%) of the respondents reported having little knowledge of ACOs. Only 1% reported being very knowledgeable about ACOs. The focus group participants reported a similar lack of knowledge about ACOs.
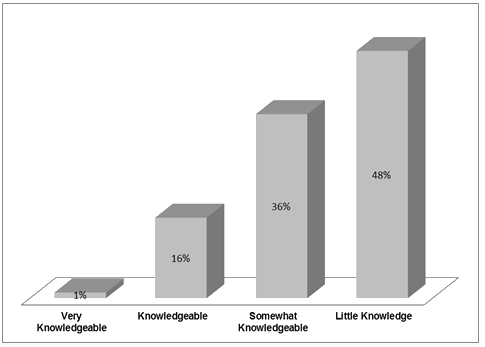
Figure 3: Survey findings - knowledge.
Benefits
The percentage of survey respondents who identified one or more of the benefits of ACOs as proposed in the survey is illustrated (Fig4). The most commonly cited benefits of ACOs related to patient-centered care and improving the quality of patient care. The most frequently citied benefit (58%) was that ACOs may provide improved patient quality of care, followed by a focus on the patient (54%). The potential to lower costs was the third most frequently cited benefit, reported by 46% of the respondents. Some survey respondents made written comments to this question. The majority of these reported that they did not have sufficient knowledge to comment on possible benefits of ACOs for RHCs. Two respondents commented that they saw no benefits of ACOs for their clinics.
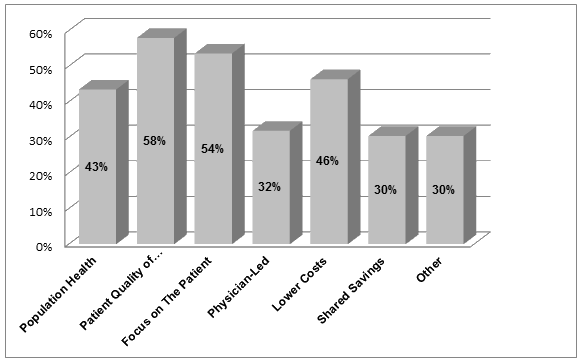
Figure 4: Survey findings - benefits.
The focus group participants echoed the interest in patient-related benefits of ACOs. One expressed that ACOs were the future for health care. Several commented on reduction in re-admissions, improved care coordination, and improved communication as potential benefits of ACOs.
Barriers
Respondent identified barriers to ACO participation are illustrated (Fig5). Of those that identified barriers, more than half (53%) cited financing as a deterrent to RHC participating in ACOs. Many (43%) reported that their clinic had inadequate capital to improve their information technology systems. Another 51% cited legal and regulatory barriers to ACO participation. Finally, 41% reported that their clinic's population base was not large enough to qualify for the Medicare SSP ACO participation.
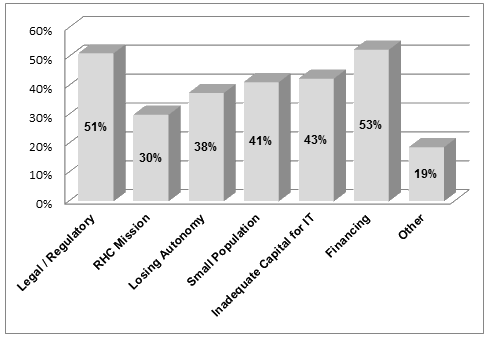
Figure 5: Survey findings - barriers to Accountable Care Organization
participation. RHC, Rural Health Clinic; IT, information technology.
Almost 20% of the respondents cited 'other' barriers. As with the responses for benefits, most of these respondents expressed not having enough knowledge about ACOs. Some respondents amplified on the issue of regulatory deterrents with their comments that they feared more bureaucracy and paperwork that could take time away from treating their patients.
The focus group participants' opinions ranged from apprehension about ACOs to whole-hearted acceptance. Some reiterated the importance that the patient comes first, and questioned whether the ACO model was focused on the patient or on financial opportunity for the clinic. Another participant expressed that providing patient access to care and maintaining quality care were the biggest concerns. Yet others felt that there were no barriers to RHC participation in ACOs, but that implementing the ACO model would undoubtedly take time, particularly for RHCs in larger corporate structures.
Comparison of willingness to join ACOs based on classification and region
One survey question assessed the extent of respondents' willingness to have their RHC join an ACO. Using a ten-point scale, responses were classified as low (0-3), moderate (4-7), or strong (8-10) willingness. A few relationships were examined between the respondent RHCs' characteristics and their willingness to join an ACO. A summary is listed of the possible factors related to RHCs' participation in ACOs (Table 2).
Table 2: Possible factors related to Rural Health Clinics' participation in Accountable Care Organizations
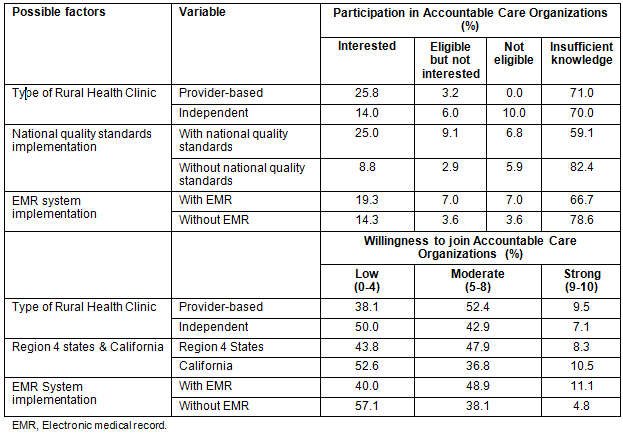
The respondent clinics were grouped and analyzed by classification as provider-based and independent. As illustrated (Fig6), of the two classifications, a higher percentage of provider-based RHCs reported a greater willingness to join ACOs than independent RHCs (19% vs 12%), although the difference in willingness was not statistically significant. Also compared were the responses from the Region 4 clinics with those from California. It was found that the percentages of Region 4 respondents reporting low (42%), moderate (42%), and strong (16%) willingness to join ACOs to be the same as for California, and that there was no statistically significant difference in 'willingness to join' between the two geographic areas.
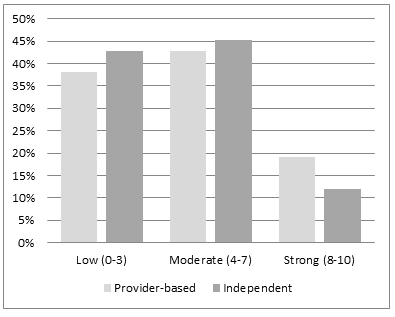
Figure 6: Survey findings - willingness to join Accountable
Care Organizations and Rural Health Clinic classification.
Discussion
One consistent and prominent finding of the survey, focus groups, and interviews was that the ACO model is generally unfamiliar to RHCs. Approximately 48% of the survey respondents reported having little knowledge of ACOs; the focus group participants and interviewees likewise reported a lack of knowledge. This is not a surprising finding, however, considering that the ACO is a new model of healthcare delivery. Another potential contributing factor is that RHC personnel are located in areas that make it difficult to attend meetings and conferences where such models might be discussed. The level of knowledge measured serves as a benchmark against which future assessments of knowledge might be compared.
Among respondents who were knowledgeable about ACOs, the most frequently cited benefits related to patient and population health. RHCs are strongly identified with their communities and devoted to serving their health needs. To RHC management, ongoing communication with the community and having the community's trust and respect are valuable in addressing disease systems and improving RHC effectiveness overall7.
Respondents expressed some wariness about whether RHCs could be treated as valued partners in ACOs. Although RHCs have been providing primary care since the mid-1970s, members of the healthcare provider community are still often unfamiliar with RHC services and operations. In addition, the small size of many RHCs may be disadvantageous from a negotiating position in an ACO, where other larger partners such as hospitals may dominate.
The participation of RHCs in ACOs may vary depending on their classification as provider-based or independent. Nationwide as of 2007, approximately 48% of RHCs were provider-based clinics (operated by hospitals, home health agencies, or nursing homes)8. Because they are structurally aligned with other healthcare organizations, provider-based RHCs may be more oriented toward partnering in ACOs than would independent RHCs.
The respondents' general lack of familiarity with the ACO concept, and their perception that legal and regulatory barriers preclude their clinics' participation in ACOs, has some implications for ACO development. At this early stage in ACO history, RHCs need greater access to information describing ACOs and the regulatory guidelines concerning RHC participation. Only then will they be able to make informed decisions about whether the ACO model will benefit their clinic's daily operations and quality of patient care.
Study limitations
The study was limited to 8 study states located in the Southeastern USA and included California as a comparison state. Another limitation was that the survey response rate was somewhat low (at 8.1%), and the focus group/interview-participant group was small. For these reasons, the study results cannot be generalized to the entire population of RHCs in the USA. However, the results provide some insight into the knowledge and opinions of RHC personnel about ACOs in the very early stage of their growth in the USA.
This article described the impressions of RHC management regarding the value of RHC participation in ACOs, as reported early in ACO history. While the ACO model was unfamiliar to many of the RHC participants, many suggested that ACOs may promote the quality of health care for RHC patients and their communities. If, however, RHCs are not provided the necessary technical assistance or are not valued as ACO partners, ACOs may not improve the services that RHCs provide.
To what extent the benefits of or barriers to ACO participation described reflect a lack of familiarity with the ACO model and regulations, is not clear. As the ACO model evolves it will be determined whether it will benefit most RHCs and their patients, or perhaps be more appropriate for provider-based RHCs specifically. How the ACO must be modified to accommodate the unique needs of RHCs is yet to be determined.
Acknowledgements
The authors thank Chiung-Ya Tang PhD for her contributions to the statistical analysis to this work. The analysis for this manuscript was supported by the National Institute on Minority Health and Health Disparities of the National Institutes of Health under award number U24MD006954. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
References
1. MacKinney AC, Mueller KJ, McBride TD. The march to Accountable Care Organizations-How will rural fare? Journal of rural health 2011; 27(1): 131-137.
2. Croshaw A. Growth and dispersion of Accountable Care Organizations. (Online) 2011. Available: http://leavittpartnersblog.com/2011/11 (Accessed 17 July 2012).
3. Shortell SM, Casalino LP, Fisher ES. How the Center for Medicare and Medicaid innovation should test accountable care organizations. Health Affairs 2010; 29 (7): 1293-1298.
4. Shields MC, Patel PH, Manning M, Sacks L. A model for integrating independent physicians into Accountable Care Organizations. Health Affairs 2011; 30(1): 161-172.
5. Shortell SM, Casalino LP. Implementing qualifications criteria and technical assistance for Accountable Care Organizations. JAMA 2010; 303(17): 1747-1748.
6. Ortiz J, Wan TTH, Meemon N, Paek SC, Agiro A. Contextual correlates of Rural Health Clinics' efficiency: Analysis of nurse practitioners' contributions. Nursing Economic$ 2010; 28(4): 237-244.
7. Ortiz J, Bushy A. A focus group study of Rural Health Clinic performance. Family & Community Health 2011; 34(2): 111-118.
8. Ortiz J, Meemon N, Zhou Y, Wan TTH. Trends in Rural Health Clinics and needs during US health reform. Primary Health Care Research & Development 2012; http://dx.doi.org/10.1017/S1463423612000503 (Accessed 30 May 2013).

