In 2007 I helped, as a renal nurse, to initiate an Aboriginal Elder onto haemodialysis. He was clearly distressed and confused and his feelings of disempowerment and dislocation were palpable. Once he became clinically stable, I talked with him and we agreed that someone should do some research aimed at finding ways to improve service delivery for the large number of Aboriginal people requiring dialysis. He encouraged me to talk with him further and to take on this research myself. I became increasingly aware of the struggles of many Aboriginal people with chronic diseases in negotiating a public health system where they were often viewed as non-compliant 'others'1 who contributed to their own poor health outcomes. This was beyond my conventional nursing knowledge and not discussed within the clinical team except as problems of 'compliance' with treatment. As I wrote in my personal journal some years ago, a precursor to the research, I confronted the need to develop insight into my own influence on what was occurring and what I was seeing in my workplace. Reviewing this journal amplified my awareness of the impact of renal failure on Aboriginal people and their families.
These events began a research journey in partnership with an Aboriginal community in rural Australia. The research was aimed at understanding the experience of Aboriginal haemodialysis recipients through their stories. The objective was to use Aboriginal insights, based on their experience as patients, to assist clinicians and policy makers develop strategies for improving quality of care and health outcomes for Aboriginal people with renal failure requiring haemodialysis. My personal journals reflected on informal conversations with 11 Aboriginal patients about my desire to do this research; however, by the time the study began in 2010 as my doctoral study, five of these patients had died.
I am not only a nurse and researcher, I am also (coincidentally) the wife of a man with renal disease facing a future on dialysis. The overlapping of my three roles in this research demanded alignment of the lenses through which I viewed people requiring dialysis. The multiple positions from which I viewed this research and how I approached the participation of Aboriginal people posed ethical, cultural and methodological challenges. These challenges prompted me to develop a deeply reflexive approach as I balanced my relationship to the research and the participants and health services (with whom I am still employed as a clinician).
The writing of an Australian Indigenous nurse and scholar confirmed that I must be vigilant in exploring my motives and attitudes whilst engaging in a project aimed at improving the health and wellbeing of her people2. The seminal work of Maori woman L.T. Smith also provided valuable insight into the history of colonial research and the damaging effects of Western academic traditions in failing to view the world through the eyes of Indigenous people3.
Definitions
Guba and Lincoln view reflexivity as 'the process of reflecting critically on the self as researcher, the 'human instrument'' and define this as 'a conscious experiencing of the self as both inquirer and respondent, as teacher and learner, as the one coming to know the self within the process of research itself'4. According to Willig5, 'Personal reflexivity involves reflecting upon the ways in which our own values, experiences, interests, beliefs, political commitments, wider aims in life and social identities have shaped the research'. Additionally, reflexivity can extend to an analysis of the epistemological underpinnings of a study, exploring the evolution of research questions, design and methods. In essence, reflexivity challenges us to understand who we are and what we bring to the creation of new knowledge, and how as researchers we shape and influence research findings.
The value of practising multi-layered reflexivity is well recognised6-8. Nicholls has explored how non-Indigenous researchers can engage with and counter colonial thinking by way of critical reflection. She views reflexivity as an evaluation of all encounters when engaging in research with Indigenous people8. Reflexivity as defined by these researchers can be an effective instrument for mitigating power, class and cultural differences in research9-11.
In this paper I define 'reflexive practice' as a multilayered and sustained critical reflection on the conscious and unconscious beliefs, assumptions, attitudes, motivations and actions influencing myself as a researcher. 'Self' reflexivity explores my biases and identifies what I bring to the study from past experience. 'Interpersonal' reflexivity examines my interactions with participants, exploring power imbalances and the learning that occurs within relationships. 'System' reflexivity scrutinises and reflects on institutional policy and practice that negatively influences the experiences of Aboriginal participants in the study. This scrutiny in particular can inform strategies for change. The three layers are captured initially through journaling. Extracts from my journals illustrate how I have applied this reflexive practice. The goal of this article is to describe the methods I instituted to develop my reflexive skills. I report this using a pragmatic description informed by theory, of how I managed my closeness to the topic and the processes used to ensure my own subjectivity did not interfere with the quality of research.
Research methods/design
The research examined the experiences and perceptions of 18 Aboriginal people receiving haemodialysis in a regional centre of rural New South Wales (NSW), Australia. Ethical clearance for this project was gained from the local area health service, the Aboriginal Health and Medical Research Council of NSW and the University of Sydney. Participants provided an informed consent. The data drawn on in this article are predominantly from my own journals kept prior to and during the study rather from than data generated by the participants themselves, as I report the process of developing reflexive practice that underpinned my role within this research. These journals report my own responses, not participant data.
The project is embedded in an Indigenist research paradigm, with a decolonisation approach3,12. 'Indigenist research is research by [or for] Indigenous Australians whose primary informants are Indigenous Australians and whose goals are to serve and inform the Indigenous struggle for self-determination'13.
Principles of community-based participatory research (CBPR)14,15 also guided my work with Indigenous communities and leadership. Community-based participatory research repositions the 'researched' into 'co-researchers' or colleagues16. The fusion of Indigenist and CBPR methodologies creates a collaborative and participatory approach with relationships as central. So, in addition to formal ethical approval, this study has been conducted with and guided by local Aboriginal leaders within cultural norms and rules as determined by them. Scholars describe Aboriginal ways of knowing and being as based upon relationships, with people, animals, plants, objects, ideas and the entire cosmos17. The concept of gaining new knowledge is transformed from that which is gained and owned by individuals to relational ownership that is shared with all of creation18.
Relational accountability
According to Indigenous methodologies the rigour and validity of research are demonstrated through relational accountability18. Researchers have relational accountability to participants, co-investigators and the conduct of the study. For me, as a non-Aboriginal researcher, relational accountability is encapsulated by principles of respect, responsibility and reciprocity19. This is exemplified by this paper being written using my personal voice, despite being co-authored. In accordance with Indigenous methodologies where knowledge is developed through relationship and is shared and not owned by individuals, co-authors of this paper have been integral in the development of my reflexive practice. I cannot claim individual 'ownership' of this work and acknowledge this by sharing authorship with the co-constructors of this knowledge and the contributions of the Aboriginal advisory group within this paper. However, the use of my own voice has been retained as it better demonstrates my personal experience of the creation of this shared knowledge.
The process of developing reflexive practice
My multiple relationships with participants created complex layers of subjectivity. As a nurse, a researcher and the partner of a man facing dialysis, reflexive practice was essential. By incorporating Indigenist methods with my reflexive practice I was able to acknowledge that the research was shaped by who I am and my experiences to this point, whilst attempting to view the topic through the worldview of the Aboriginal people with whom I was working.
Where do I begin to find a methodology that will give participants an authentic voice and result in real, ongoing improvements in their day to day lives as dialysis patients living in an alien biomedical world? (Journal entry, 2 March 2010)
As a non-Indigenous clinician researching with Aboriginal people, I required another lens to view the world, informed by Aboriginal people and their culture20. I cannot negate or deny the influence of my background or culture. However, a reflexive and open-minded attitude to the community and participants can enable the perspectives and insights of Aboriginal people to be heard through the research21. I already knew intuitively that as a non-Indigenous researcher, I needed to describe my approach, making explicit my philosophy and values22. Examining the national ethical guidelines addressing research with Aboriginal people23,24 prompted further exploration of the writing of others who helped to shape my thinking. This confirmed that reflexive practice should play a major role in my work. The process that I used to undertake this practice is described below.
Tools for reflexive practice
Journaling: Much of my initial journaling explored how this research could be done using a collaborative approach, sharing power and control with the Aboriginal participants and Elders. Journaling helped me to reflect on my communication style, gauge community support for the project and examine my own philosophical beliefs.
Talking with an Elder today, I was struck by his ability to truly listen to my words. Then I noticed how he did not speak until he had thought about what I had said, giving me a thoughtful response. (Journal entry, 2 March 2010)
Journaling allows for the fusion of our personal and professional lives, providing insight into how our life experiences have shaped and influenced how we conduct research25. Regular journaling by researchers can 'enhance critical thinking about the research process in which they are engaged'25 and provides a meditative focus that helps the qualitative researcher to become a better research 'instrument'26.
Guidance and supervision: The formation of a community reference group (CRG) is in accord with the ethos behind both Indigenous and CBPR methods. This group includes Aboriginal dialysis patients, Elders and Aboriginal health workers. We meet three to four times a year and I provide reports on progress of the research. The CRG critiqued preliminary data analysis, and all documents produced by the research have been shared with this group.
How do we ensure that this group is a true research collaboration? We need constant vigilance for it to be a real partnership that enacts the principles of reciprocity, respect, consultation, inclusion and sharing ... I must continue to follow advice of Elders and talk less, listen more. (Journal entry, 17 April 2011)
As this journal entry implies, reflexive practice was essential in developing my understanding of the centrality of this group for an effective collaborative and reciprocal relationship; also, the need to keep this group actively engaged throughout and beyond the research.
My PhD supervisory committee is led by a non-Indigenous clinician/academic with broad experience supervising Aboriginal health research projects. I have two Indigenous academic supervisors whose roles include mentoring me in working collaboratively with Aboriginal people. We meet fortnightly and they scrutinise my work, offering critique and debate.
Lester Rigney, an Australian Aboriginal researcher and creator of the term 'Indigenist research' writes that in order to ''privilege Indigenous voices in research', those seeking to study his people must keep their goal to 'serve and inform the Indigenous struggle for self-determination''13. Through reflexive practice I came to understand that by modifying his paradigm for use by a non-Indigenous researcher, I was acknowledging the power imbalances between service providers and Aboriginal people, and advocating Aboriginal peoples' need for self-determination and re-empowerment within health institutions.
Researcher positioning
I initially thought, following the subjective/objective tradition in much health and medical research, that I should separate my clinical role from the research. As I began to gather the stories of participants I, like other clinician/researchers before me, found my 'nurse' voice could not be excluded and was present during interviews27. I was constantly observing my behaviour, trying to find distinct boundaries between the way I worked with participants as a nurse in the clinical setting and as a researcher28. This attempt to separate my roles was complicated by the need to earn the trust of Aboriginal participants in order to gain access to their stories. This trust was based on participants knowing me as a renal nurse, and they preferred me in that role. Therefore, in accord with an Indigenist paradigm, my relationship to their world was connected to my nursing role and I should not try to separate the two.
How do I switch off my renal nurse voice when wearing my researcher hat? Or maybe I shouldn't, just be me and all that my relationality to this project brings (Journal entry, 3 March 2011).
The emotional influences on me as a woman facing a future with a partner on dialysis featured in my reflexive practice. Without an in-depth exploration of the emotional 'noise' coming from this, I was at risk of damaging and unhealthy influences, not only on my own relationship with my partner, but also on the entire research process. Reflexive practice however has enabled me to unpack my own anxieties about my partner's renal disease. It has helped me to gain a positive view of the future and made me thankful for the opportunity this project has given me to explore my feelings and attitudes.
I feel blessed to have my renal nursing to help us as a couple to come to terms with our future as his disease progresses. When we get anxious we talk about how jealous my patients are that he has his own personal renal nurse. (Journal entry, 22 August 2010)
The conflicts and tensions I had as nurse/wife/researcher required me to use reflexive practice to identify 'who and where am I' in the study. The seminal texts of Indigenous scholars guided me theoretically as I learned how they addressed their own tensions when researching with their people. Whilst reading the work of a Canadian Metis scholar, I realised that my positioning in the research is irrelevant if the study does not achieve real and positive change that can contribute to improving outcomes for participants.
If my work as an Indigenous scholar does not lead to action, it is useless to me or anyone. I cannot be involved in research and scholarly discourse unless I know that such work will lead to some change out there in that community, in my community.29
Then, I 'got it': I then understood that it is my relationship to the topic and the participants that has made me who and what I am in relation to this research30. Separating my roles and positioning myself was less important than what resulted from my involvement and interaction with the research and how effective I was as a research 'instrument'. I also understood that the overlapping of my research lenses needed a relational accountability 'filter'. This filter sits between my lenses and the participants' perspectives, reinforcing the principles of respect, responsibility and reciprocity. Despite this realisation I remained vigilant, using reflexive practice to examine how my multiple roles limited or altered access to and analysis of the data to answer the research questions.
Whilst I do try to explain to participants that I really need them to be honest to enable me to address real problems, I am wondering if they are partly blocked by my being a nurse, with participants not wishing to disclose to me. I do think I have a reasonable rapport with most, however I cannot know how much my insider role is impacting on how they disclose their issues with me around service delivery and communication with staff. (Journal entry, 10 July 2011)
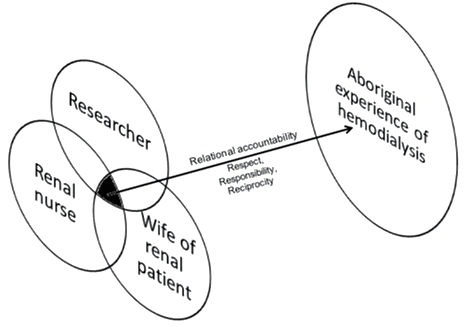
Figure 1: Aboriginal experience of haemodialysis is viewed through three
overlapping lenses of the researcher using the relational accountability filter.
Self reflexivity
The complexity of my relationship to this research initiated a lengthy period of journaling that helped unpack my worldviews, assumptions and attitudes.
As a child in Tasmania I always felt separate from and ashamed of the homogenous 'whites only' culture that I grew up in. The early colonists tried to commit genocide on the Aboriginal people and almost succeeded! Even at five or six I knew instinctively that I was not a 'rednecked' Tasmanian, felt that I never fitted in and hated the one-sided history I was taught at school. I often daydreamt about the natural life Aboriginal people must have had before the English came with their convicts, guns and disease. (Journal entry, 3 March 2010)
Early in the study, an intensive and at times distressing period of examining my position led me through difficult yet empowering discoveries about my feelings and attitudes. These were in relation to my career, my personal relationship to the topic through my partner and what I was bringing to the research as a white person from a privileged upbringing. I discovered some uncomfortable and distasteful truths about myself, which previously I had not addressed. This process helped discover my epistemological and ontological beliefs by 'unpacking' unconscious racist concepts and exploring the impact of living in a country where racism and the assumption of European white privilege are common31.
This process soon revealed long-held assumptions and Eurocentric attitudes and I became acutely aware of my own personal prejudices.
Although I know it is prejudiced and 'middle class' I find myself judging differences between Aboriginal people and 'us'. I'm witnessing my own feelings of superiority and whiteness, and feeling deeply ashamed. I thought I was above all that. But now I see that deep down I have also been like the nurses I call racist. (Journal entry, 13 April 2010)
This reflexive practice became the catalyst for choosing an Indigenist methodology. I realised that to be an effective research 'instrument' and agent of change for the people with whom I was working, I needed to attempt to see the world through 'their' eyes, using ways of discovering new knowledge that were congruent with their world view.
Interpersonal reflexivity
In keeping with the Indigenous tradition of oral history for passing on knowledge and information, I sought the perspectives and experiences of Aboriginal participants using 'yarning' and storytelling to generate information17,32. This was my attempt to create a relational space between myself and participants that was comfortable for them. Yarning is a word often used by some Aboriginal people, meaning 'let's have a chat'33. Use of minimal questions and prompts and acute listening skills have been the key to allowing the stories of participants to unfold.
Yarning helped me develop a more Aboriginal way of communicating; however, I constantly scrutinised my attitudes, behaviour and communication style.
Whilst I truly enjoy the company of Aboriginal people, am I silently patronizing in my approach? Can I truly say that I am aware of my own racially infused attitudes? Do these attitudes come through to Aboriginal people in both my spoken and unspoken communication style? (Journal entry, 5 June 2010)
Exploring interactions between researchers and participants can ensure that the emerging voices of participants are separated from the underlying social and cultural assumptions about those interactions brought by researchers' own values6. Although unpacking my privileged background and cultural assumptions helped to clarify my worldviews, there was still work to be done to address power issues within this research.
Power and unequal relationships: Issues of power and unequal relationships must be addressed by any researcher working with marginalised or vulnerable populations. Bishop describes how research with Maori people has perpetuated colonial power imbalances, belittling and undervaluing Maori knowledge21. Reflexivity can enable the voice of 'others' to be heard whilst tracking the 'reciprocal workings of power', including the 'changing position of the researcher within the research process'11. Educational researcher Heshusius has used the term 'participatory mode of consciousness' to describe a process of reordering the understanding of relationships between self and others in order to manage subjectivity within qualitative research. While it may not be possible to entirely overlook your 'self', this reordering takes focus away from self to an essential connectedness and relationship with others.
When one forgets self and becomes embedded in what one wants to understand, there is an affirmative quality of kinship that no longer allows for privileged status. It renders the act of knowing an ethical act34.
When attempting to understand or address power imbalances within researcher/participant relationships, I agree with Heshusius that absolute objectivity is impossible when exploring the experiences and perceptions of 'others'. However, researcher subjectivity can be managed by a genuine attempt to immerse oneself in the words and reality of research participants and use a reflexive and 'participatory lens' to view their experience and perceptions. When this occurs, the researcher and participant can share a form of 'participatory consciousness' within their relationship that can be viewed as a more ethical way of knowing and understanding. According to Heshusius 'A participatory mode of consciousness, then, results from the ability to temporarily let go of all preoccupation with self and move into a state of complete attention'34.
Through my journal I examined the potential for exploiting my position of power over participants, not only as a researcher, but also as a nurse, with the privilege of knowledge and experience of their disease and treatment35. Reciprocity proved a highly effective tool to assist with sharing of power.
Reciprocity: Reciprocity as a core principle of Indigenist research is essential in any project aimed at improving the health of Aboriginal people19. Reciprocity within the context of interviews with participants36 and judgment used by researchers in the field can benefit greatly from reflexive practice. For example, during an interview a participant turned to me and asked, 'So, what's it like being a renal nurse?' As I attempted to answer this question honestly and clearly, a rich conversation ensued where we compared our perspectives. What I had intended to be an interview, where I listened to someone else's story, became a two-way dialogue and true 'yarning'. Journaling about this later, I realised that my concept of reciprocity was extended from reciprocal actions, for example providing transport and reimbursing costs, to a reciprocal exchange of ideas and experiences.
As my interactions with participants evolved from nurse-patient encounters in a hospital environment to relating as people in a more neutral space or in their own environment, I became acutely aware of shifts in relational dynamics. Participants came to know me as a woman, the partner of a man with 'their' disease and a researcher. These new relationships clearly influenced their stories and enhanced disclosure37.
We had a really good yarn. I gave her some background on where I have come from. We shared our experiences of visiting the outback and yarning with people from other areas. She wanted to hear about my life, renal nursing, and my man's illness. (Journal entry, 24 March 2011)
Health system reflexivity
Much of my reflexive practice was triggered by my observations in the clinical setting of behaviours I considered racist. The realisation that I was working within a predominantly racist system, where attitudes are entrenched, prompted me to examine my own level of cultural awareness and communication style as these are employed in my nurse role as part of the health system myself.
I don't fit in with the nursing/medical culture of judgment of Aboriginal patients. Blaming them as 'non-compliant others' instead of asking why their health status has not improved. If more of us would listen to Aboriginal people we might glimpse the world through other eyes. (Journal entry, 3 August 2010)
Whilst I realised I had much to learn in this area, my journal describes some of my colleagues labelling Aboriginal people as 'others'36,38 and deeming them as responsible for health problems resulting from their lifestyle choices and non-compliance with the Western model of health care.
I was horrified to hear [name withheld] telling a patient that she should 'get with the program and forget about her family's crap if she wanted to live'. He did not even bother to ask her why she had missed dialysis, just assumed it was her fault. (Journal entry, 26 September 2008)
This culture of judgment and blaming of Aboriginal patients persists39 despite increasing numbers of non-Aboriginal people suffering similar patterns of lifestyle-induced chronic illness. The Barker hypothesis suggests that stress, colonisation and other forces influence rates of illness in Aboriginal people40,41. This hypothesis proposes that intra-uterine malnutrition and other stressors result in low birth weight, common in Aboriginal infants, which in turn 'predisposes individuals to type 2 diabetes, hypertension, dyslipidaemia and cardiovascular disease'42.
Aboriginal people often experience racist attitudes in health institutions, where discriminatory policy and practice are 'embedded in organisational structures, often covertly'43. Unless there is critical reflection on the racist assumptions that underpin service provision, this covert form of racism within health institutions will continue. Durey's position is amply supported in my journal:
An Aboriginal woman on dialysis had extreme levels of physical, emotional and spiritual pain. Like so many people in constant pain, she dealt with this pain by substance abuse a lot of the time, using pot and high doses of prescription drugs to get through it all. There was judgment from staff around her drug use, with little empathy or respect. (Journal entry, 26 May 2010)
For Aboriginal people experiencing chronic disease, hospitals represent daunting and culturally alien organisations where many have seen their family members go to die39. The fear and confusion experienced by Aboriginal people when initiated into haemodialysis in hospital is well known44. The findings of this study, reported in detail elsewhere, revealed that family is the overall mediating factor for Aboriginal people on dialysis. Family enable and motivate them to endure and face challenging and often overwhelming circumstances.
Family commitments are often prioritised ahead of treatment, with Aboriginal patients viewing this as relational accountability to their families. Service providers, however, consider this to be non-compliance with treatment. This conflict of thinking clearly demonstrates the lack of cultural safety for Aboriginal people within a health system that historically has overlooked 'the importance of family and the complexity of interrelationships between Aboriginal people and the places they occupy'45. Reflexive practice has led me to conclude and argue that this situation demonstrates endemic institutionalised racism.
Chronic health disparities for Aboriginal people are underpinned by complex historical, political and economic factors and it is necessary to acknowledge and address barriers to better health care and outcomes for Aboriginal people12,46. Despite evidence of strong links between colonisation and adverse health outcomes, institutionalised racism still exists within Australian health systems47 and until this is recognised and service delivery adjusted accordingly there can be no change.
If we nurses focused on showing respect, responsibility and reciprocity to all, our Aboriginal patients may find being under our care a more comfortable place to be. (Journal entry, 25 February 2012)
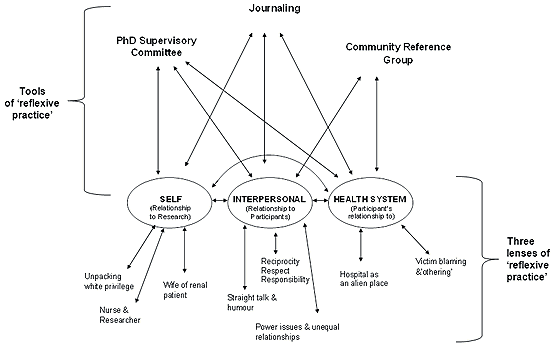
Figure 2: Multilayered reflexive practice as a method of research practice.
This article has outlined three layers of reflexive practice that I have labelled as 'self', 'interpersonal' and 'health system'. These layers assisted me as a non-Indigenous clinician/researcher to engage more effectively in research aimed at improving services and health outcomes for Aboriginal people. I have detailed influences on my thinking and how reflexive practice has evolved in the context of my research. The tools of reflexive practice include regular personal and professional journaling, as well as ongoing collaboration and discussion with Aboriginal people as research colleagues, and co-investigators/supervisors. These tools as elements of reflexive practice relate to a conceptual framework that describes the method of research practice underpinning the study, and maps how my roles influenced it.
I have described how self-reflexivity and the unpacking of my white privilege resulted in my embrace of an Indigenist paradigm to inform methods used to explore the research question through the eyes of participants. Interpersonal reflexive practice explores and clarifies how multiple roles and the self are managed in relationships with others. Critical examination of the health system that Aboriginal patients must negotiate to access treatment is the third layer of reflexive practice as I examined issues such as institutionalised racism, victim blaming, and hospitals as daunting and alien environments.
Insights and recommendations emerging from the stories of Aboriginal participants were based on analysis that was influenced by Aboriginal colleagues through the CRG. In this context, reflexive practice and Indigenist theory have helped me learn that I am merely the research 'instrument'. My role is to act rigorously and independently, but also as a conduit between the Aboriginal community and the health system to discover strategies that will return to Aboriginal patients some degree of self-determination and control that reliance on the health system has removed.
Through reflexive practice I discovered that positioning and separation of roles was of far less importance than how effective I am as a well-honed research 'instrument' that can contribute to improvements in treatment and health outcomes for the Aboriginal people with whom I am working. I realised that the key to being an effective 'instrument' was aligning the three lenses through which I viewed the study, incorporating respect, responsibility and reciprocity. Reflexive practice used in this manner can help manage complex relationships within Indigenous health research, aiming for clarity based on deep reflection and understanding that is validated by Aboriginal participants and colleagues.
Acknowledgments
We sincerely thank the Aboriginal participants in this study for contributing their stories. We also thank community reference group members who provided invaluable guidance throughout this study. We gratefully acknowledge the Bundjalung Nation, upon whose lands this research took place. ER is supported by The Clinical Excellence Commission, Ian O'Rourke Scholarship in Patient Safety.
References
1. Browne AJ, Varcoe C, Smye V, Reimer-Kirkham S, Lynam MJ, Wong S. Cultural safety and the challenges of translating critically oriented knowledge in practice. Nursing Philosophy. 2009; 10(3): 167-179.
2. Sherwood J. Do no harm: decolonising Aboriginal health research. PhD thesis. Sydney: University of NSW, 2010.
3. Smith LT. Decolonizing methodologies: research and indigenous peoples. Dunedin: University of Otago Press, 1999.
4. Guba EG, Lincoln YS. Paradigmatic controversies, contradictions, and emerging confluences. In: NK Denzin, YS Lincoln (eds). The Sage handbook of qualitative research. 3rd edn. Thousand Oaks: Sage Publications, 2005; 191-215.
5. Willig C. Introducing qualitative research in psychology. 1st edn. Maidenhead: McGraw Hill/Open University Press, 2001.
6. Chiu LF. Critical reflection. Action Research 2006; 4(2): 183-203.
7. Finlay L (ed.). The reflexive journey: mapping multiple routes. London: Blackwell Science, 2008.
8. Nicholls R. Research and Indigenous participation: critical reflexive methods. International Journal of Social Research Methodology 2009; 12(2): 117-126.
9. Bott E. Favourites and others: reflexivity and the shaping of subjectivities and data in qualitative research. Qualitative Research 2010; 10(2): 159-173.
10. Grbich CF. Qualitative research in health: an introduction. 1st edn. St. Leonards: Allen & Unwin, 1999.
11. Liamputtong P. Researching the vulnerable. Thousand Oaks: Sage Publications, 2007.
12. Edwards T, Sherwood J. Decolonisation: a critical step for improving Aboriginal health. Contemporary Nurse 2006; 22(2): 178-190.
13. Rigney LI. Internationalization of an Indigenous anticolonial cultural critique of research methodologies: a guide to Indigenist research methodology and its principles. Journal of Native American Studies 1999; 14(2): 109-121.
14. D'Alonzo KT. Getting started in CBPR: lessons in building community partnerships for new researchers. Nursing Inquiry 2010; 17(4): 282-288.
15. Rhodes SD, Hergenrather KC, Wilkin AM, Jolly C. Visions and voices: Indigent persons living with HIV in the southern United States use photovoice to create knowledge, develop partnerships, and take action. Health Promotion Practice 2008; 9(2): 159-169.
16. Mooney-Somers J, Maher L. The Indigenous Resiliency Project: a worked example of community-based participatory research. NSW Public Health Bulletin 2009; 20(7-8): 112-118.
17. Wilson S. Research as ceremony: Indigenous research methods. 1st edn. Winnipeg: Fernwood Publishing, 2008.
18. Wilson S. What is an Indigenous research methodology? Canadian Journal of Native Education 2001; 25: 175-179.
19. National Health and Medical Research Council. Ethical guidelines in Aboriginal and Torres Strait Islander research. (Online) 2003. Available: http://www.nhmrc.gov.au/publications/synopses/e52syn.htm (Accessed 30 May 2010).
20. Getty GA. The journey between Western and Indigenous research paradigms. Journal of Transcultural Nursing 2010; 21(1): 5-14.
21. Bishop R (ed.). Freeing ourselves from neocolonial domination in research. 3rd edn. Thousand Oaks: Sage Publications, 2005.
22. McGrath T, Butcher A, Koo Y, Pickering J, Smith H (eds). Engaging Asian communities in Aotearoa New Zealand: an exploration of what works in community research. 1st edn. Waitakere City: Muddy Creek Press, 2007.
23. National Health and Medical Research Council. Cultural competency in health: a guide for policy, partnerships and participation. Canberra: Commonwealth of Australia, 2006.
24. National Health and Medical Research Council (NHMRC). Keeping research on track: a guide for Aboriginal Islander peoples about health research ethics. (Online) 2005. Available: http://www.nhmrc.gov.au/_files_nhmrc/file/publications/synopses/e65.pdf (Accessed 30 May 2010).
25. Banks-Wallace J. Eureka! I finally get IT: Journaling as a tool for promoting praxis in research. ABNF Journal 2008; 19(1): 24-27.
26. Janesick VJ. 'Stretching' exercises for qualitative researchers. 2nd edn. Thousand Oaks: Sage Publications, 2004.
27. Carolan M. Reflexivity: a personal journey during data collection. Nurse Researcher 2003; 10(3): 7-14.
28. Arber A. Reflexivity: a challenge for the researcher as practitioner? Journal of Research in Nursing 2006; 11(2): 1-157.
29. Weber-Pillwax C. What is Indigenous research? Canadian Journal of Native Education 2001; 25(2): 166-174.
30. Martin KL. Please knock before you enter: Aboriginal regulation of outsiders and the implications for researchers. Teneriffe: Post Pressed, 2008.
31. MacIntosh C. The role of law in ameliorating global inequalities in Indigenous peoples' health. Journal of Law, Medicine & Ethics 2013; 41(1): 74-88.
32. Bird S, Wiles JL, Okalik L, Kilabuk J, Egeland GM. Methodological consideration of story telling in qualitative research involving Indigenous Peoples. Global Health Promotion 2009; 16(4): 16-26.
33. Bessarab D, Ng'andu B. Yarning about yarning as a legitimate method in Indigenous research. International Journal of Critical Indigenous Studies 2010; 3(1): 37-50.
34. Heshusius L. Freeing ourselves from objectivity: managing subjectivity or turning toward a participatory mode of consciousness? Educational Researcher 1994; 23(3): 15-22.
35. Walker R, Sonn C. Working as a culturally competent mental health practitioner. In: N Purdie, P Dudgeon, R Walker (eds). Working together: Aboriginal and Torres Strait Islander mental health and wellbeing principles and practice. Canberra: Department of Health and Ageing, ACER, Kulunga Research Network & Telethon Institute for Child Health Research, 2010; 157-180.
36. Liamputtong P. Performing qualitative cross-cultural research. Cambridge: Cambridge University Press, 2010.
37. Finlay L (ed.). Through the looking glass: intersubjectivity and hermeneutic reflection. London: Blackwell Science, 2008.
38. Bartlett JG, Iwasaki Y, Gottlieb B, Hall D, Mannell R. Framework for Aboriginal-guided decolonizing research involving Métis and First Nations persons with diabetes. Social Science & Medicine 2007; 65(11): 2371-2382.
39. Eckerman A, Dowd T, Chong E, Nixon L, Gray R, Johnson S. Binan Goonj: bridging cultures in Aboriginal health. 2nd edn. Marrickville: Elsevier Australia, 2006.
40. Barker DJ, Hales CN, Fall CH, Osmond C, Phipps K, Clark PM. Type 2 (non-insulin-dependent) diabetes mellitus, hypertension and hyperlipidaemia (syndrome X): relation to reduced fetal growth. Diabetologia 1993; 36(1): 62-67.
41. Cass A. Health outcomes in Aboriginal populations. Canadian Medical Association Journal 2004; 171(6): 597-598.
42. Hoy WE, Rees M, Kile E, Mathews JD, Wang Z. A new dimension to the Barker hypothesis: low birthweight and susceptibility to renal disease. Kidney International 1999; 56(3): 1072-1077.
43. Durey A. Reducing racism in Aboriginal health care in Australia: where does cultural education fit in? Australian & New Zealand Journal of Public Health 2010; 34(S1): S87-S92.
44. Anderson K, Devitt J, Cunningham J, Preece C, Cass A. 'All they said was my kidneys were dead': Indigenous Australian patients' understanding of their chronic kidney disease. Medical Journal of Australia 2008; 189(9): 499-503.
45. Fredericks B. What health services within rural communities tell us about Aboriginal people and Aboriginal health. Rural Society 2010; 20(1): 10-20.
46. Durey A, Wynaden D, Thompson SC, Davidson PM, Bessarab D, Katzenellenbogen JM. Owning solutions: a collaborative model to improve quality in hospital care for Aboriginal Australians. Nursing Inquiry 2011; 19(2): 1-9.
47. Sherwood J. Who is not coping with colonization? Laying out the map for decolonization. Australasian Psychiatry 2009; 17(s1): S24-S27.



