full article:
Effective team collaboration is critical to achieving patient-centered, safe, timely, effective, efficient and equitable care1 . In the context of health care, collaboration refers to 'an interprofessional process of communication and decision making that enables the separate and shared knowledge and skills of care providers to synergistically influence the client/patient care provided'2. Interprofessional collaboration is a complex process that has the potential to transform patient care for the better in urban, rural and remote healthcare settings1,3. Teaching teams to collaborate is complex because it involves a shift in professionals' behaviors and attitudes determined by factors beyond the scope of formal interprofessional education (IPE) curricula4. Research on IPE predominantly focused on assessing learner outcomes using pre- and post-intervention surveys; however, few studies have used qualitative research methods to explore the process that led to improvements in interprofessional competence. Hean and Dickinson argue, 'there is a case for looking outside the box and developing theory that has originated from IPE experience specifically'5. To better capture the breadth of factors that influence IPE learning, Freeth and Reeves developed a Presage-Process-Product (3P) model of IPE learning and teaching6. In keeping with this proposition, this study drew from the perspective of facilitators and actors regarding the interprofessional collaboration that took place at a wilderness medicine conference because they offer critical insight into the presage, process and product of interprofessional learning. The conference, an annual 3-day wilderness medicine conference (WildER Med) on Manitoulin Island in Northern Ontario, Canada, has been shown to improve participant collaboration without formal IPE curriculum7. This event uses workshops, didactic lectures and simulations to teach wilderness medicine knowledge and skills. In the first 2 days, participants camp together and learn wilderness medicine and orienteering in assigned teams. On the third day, the teams navigate through the woods to medical emergencies performed by patient-actors from a local Aboriginal theatre troupe, Debajehmujig Storytellers8. After completing the scenario, participants receive group feedback from the patient-actors and scenario facilitators.
Understanding how this learning occurred may enable the use of simulation in similar rural and remote settings to teach collaboration. Others have investigated the process of IPE such as Freeth and Reeves who found learning collaboration was influenced by factors beyond the formal curriculum. They suggest that understanding these factors would enable educators to develop more effective IPE opportunities6. When attempting to understand how interprofessionalism is learned at WildER Med, authors encountered several issues including the complexity of interprofessionalism acquisition, challenge of understanding why a wilderness medicine conference was effective IPE and the difficulty of drawing data on hidden and informal curriculum.
At WildER Med, Reade and colleagues used mixed methods to study participants' perceptions of their own interprofessional competencies. They found participants reported improvements in interprofessional competencies by participating in WildER Med7. This may be, in part, due to the wilderness simulated scenarios. Robertson and Bandali suggest that visually and kinaesthetically realistic simulation cases support the psychological and cognitive aspects of interprofessional learning9. As such, rural and wilderness medicine conferences may provide the stimulation and intimacy required for interprofessional interactions. There has been widespread acceptance and uptake of simulation in interprofessional education but the teaching and learning processes that underpin the learning are not well understood9,10.
To better understand how collaboration was taught and learned, the hidden and informal curriculum needs to be explored11. Freeth and Reeves describe interprofessionalism acquisition using a 3P model which includes elements of the hidden and informal curriculum that may not be adequately captured through participant surveys6. Facilitators and actors are critical players in the presage, process and product of interprofessional learning and may offer better insight into the mechanisms of interprofessional learning5. The authors used purposive sampling to include a range of facilitators, actors and faculty of the WildER Med conference. Of the 25 people approached, 11 agreed to participate. Six participants were male and five were female. Four were actors from Debajehmujig Storytellers. Seven were facilitators and included police officers, physicians, paramedics, nurses, nurse practitioners and health administrators. The authors used one-on-one semi-structured interviews to elicit WildER Med facilitators' and actors' perceptions of how the setting, scenarios, emergent group dynamics and other factors identified by Freeth and Reeves impacted group function. A grounded theory approach based in social constructivist theory was then used to study the phenomenon of the acquisition of interprofessional collaboration competencies in simulated wilderness medical emergencies.
Theory of sharing
A basic social process of sharing occurred as the central phenomenon throughout WildER Med that provided the basis for a substantive theory to explain the collaborative approach used to complete the wilderness medical simulations. As demonstrated in Figure 1, the term sharing refers to this process whereby group members (including the actors, facilitators and care providers) contributed knowledge, skills and ideas to achieve a common task. Through sharing, groups established common goals, mutual respect and shared leadership to collaboratively respond to the wilderness scenarios.
Research participants attributed sharing to the small team size, extensive time spent together, common vision, enthusiasm for wilderness medicine, and diversity of professional backgrounds. Three determinants found to be most deeply and frequently associated with collaborative interaction were 'wilderness and social environment', 'collaborative leaders' and 'basic urgent task'. This report will focus on the association with the wilderness and social environment. The data, analysis and reviewed literature are incorporated into the authors' analysis in accordance with Glaser's approach to presenting grounded theory12.
Facilitators, care providers and actors all engaged in sharing (Fig1). Care providers brainstormed together to assess and respond to the patients. Facilitators and actors worked together to set the scenario and give feedback to care providers afterwards. The term 'sharing' was used to describe these interactions and is often used by other researchers in describing collaboration such as sharing of power between partners, sharing of tasks, or being open to sharing information and learning from each other when entering into a collaborative process13,14.
Figure 1 depicts the patient as an equal contributor to sharing. This emphasizes the integral contribution of the patient, who is both the primary recipient of group's efforts and active collaborator. An actor's description of his experiences emphasizes this:
You learn on both ends, for us performance-wise it's something new and it gives us [the ability] to create real vulnerability and be believable ... and for them [the participants] it's like giving the real-life scenarios. (2, actor)
The actor found that he taught participants how to deal with real-life scenarios, and their responses taught him how to portray vulnerability, enabling them to enhance their roles and abilities to complete the scenarios together. Another actor expanded on this in her comment:
We learned that if we allow it to be more layered and complex it's a better experience for the medical practitioners. Not only more interesting for them, but there's more learning for them if we allow ourselves to be more human in the whole situation. (4, actor)
This demonstrates that sharing was a learning and teaching process similar to Oandasan and Reeves' definition of interprofessional learning: teaching each other and working in synergy15.
By sharing, group members also enhanced their skills for collaborative practice: shared leadership, common goal development, and mutual understanding and respect, as demonstrated in Figure 1. One facilitator commented upon his observation of the sharing of leadership:
There's no one person that takes the lead at every one of the scenarios, everybody takes their turn and gets the experience from being the lead person to being the deciding person, to being the navigating person. (11, facilitator)
Participants took turns leading the group in tasks such as orienteering, clinical assessment and evacuation planning. Interviewees also found that mutual understanding and respect developed not only between group members but also with facilitators over the weekend. For instance, one facilitator (10), a police officer, commented, 'It probably gives them [conference participants] a different look at the cop as opposed to someone who is just running the highway'. That facilitator felt that by learning orienteering from police officers and sharing time with them, participants gained a better appreciation for an officer's scope of practice. Respect for other professionals is foundational to collaboration and a skill that group members may be able to transfer to other interprofessional encounters.
The authors found their theory aligns with multiple researchers who also describe collaboration as a process4 . For instance, Gittell and colleagues propose the relational coordination (RC) theory to describe interprofessional collaborative practice14. They defined RC as the use of optimal communication and relationships with shared goals, shared knowledge and mutual respect to achieve higher levels of quality and efficiency. Both RC and sharing theory show collaboration as a process that leads to improved interactions and outcomes. This reinforces the suggestion that collaboration may be a result of a complex process of interaction between all team members that may exist in hidden and informal curriculum.
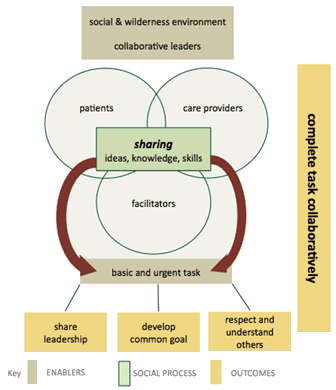
Figure 1: The theory of sharing.
Social wilderness environment
Interviewees gave rich descriptions of the environment of WildER Med and its importance to collaboration. One actor described the environment at WildER Med as pivotal to building awareness of self and others:
There's something about that natural environment when we get out to engage with each other that a lot of the mask and the roles that we might play with each other naturally and automatically disappear. And that's very important when you're trying to learn something new, that you get out of your own conceptual boxes to see a different thing that was never visible to you before. (4, actor)
The connection between collaboration and the social and environmental context is well established in literature on interprofessionalism15. An awareness of self and others, like the one described by this actor, is a core component of collaboration and elementary to developing mutual respect and understanding. Further, this quote demonstrates that at WildER Med the wilderness is not simply a geographic setting but a concept to which people attach value and invest in. Kitto also found that the conceptual aspects of an environment contributes to all three levels of curriculum: formal, informal and hidden16. This section will elaborate on the environment's influence in these three levels with regards to IPE.
As part of the formal curriculum, the wilderness environment was used to teach participants to assess the patient in their surroundings and improvise together. With limited time and resources, participants relied on one another's skills, ideas and experiences to develop creative solutions. One facilitator summarized this well in saying 'it does take a team in a harsh environment to succeed. No one person can do it all.' (9, facilitator). Another facilitator expanded on this idea of the wilderness encouraging awareness and a collaborative effort in saying 'because we were in such a close space, I think we were sort of forced to work together ... I think [it was] the actual physical geography ...' (10, facilitator). These quotes demonstrate that wilderness medicine required groups to interact and work together. Similarly, Mariano argues that space sharing and physical proximity reduce professional territoriality and help develop interpersonal relationships17. Therefore, the wilderness medicine curriculum seems to have promoted interprofessionalism even though IPE was not an explicit part of the formal curriculum.
The environment also facilitated interaction during shared meals and around the fire in the evening. One facilitator commented:
[The outdoor environment] brings the group together more because it's informal, they eat together, they're in a tent maybe twenty feet from their partner ... Even when our students are having their meal they are either talking with the instructors, asking them questions or they're working together. (6, facilitator)
People continued to share with one another in these informal social environments. This enhanced the cohesiveness of the group and their learning. Kitto describes this type of interaction as the informal curriculum occurring between health professionals in hospital hallways and cafeterias16. Kitto found that the 'unscripted, predominantly ad hoc and highly interpersonal form of teaching and learning' occurred in these environments. Similarly at WildER Med, the casual and intimate social environment enhanced this type of interaction and potentially contributed to learning collaboration.
The hidden curriculum encompasses the processes, pressures and constraints outside of or embedded within the formal curriculum11. Multiple interviewees alluded to such influences at WildER Med. For instance, one actor described how the culture of WildER Med motivated her to contribute:
This project [WildER Med] always has the culture of exploration with it, so it's not like you can fail at this (laughs), you can just get into it and do your best and see what happens. (4, actor)
This comment demonstrates that the environment promotes exploration and learning by allowing space for trial and error. Similarly, Oandasan and Reeves found that for adults to learn, they need an environment where they feel psychologically safe to express themselves openly15. Furthermore, this quote depicts the environment as dynamic and dependent on the people acting in it: the environment shapes people's actions and people shape the environment. This suggests an interactive component to the environment's influence on participants' behavior and contribution to the hidden curriculum.
Conclusions
In a wilderness medicine conference, without formal interprofessional education curriculum, collaboration emerged as a process of sharing. Furthermore, the informal and hidden curriculum of a social and wilderness environment that encouraged participants and leaders to interact and explore enhanced sharing and ultimately their collaboration. Applying this sharing theory to IPE may enable educators to design more effective learning experiences in similar rural and remote contexts such as emergency response teams, search and rescue, or rural health teams. Rural healthcare teams also experience small teams, limited resources, urgent tasks, and overlap of professional and social interactions, so may provide an environment where simulation may be used to teach interprofessional competencies. Further research into the role of sharing across different types of rural teams and evidence regarding the long-term effect on collaboration may enable educators to consistently use simulation and rural wilderness medicine to teach interprofessionalism.
Acknowledgements
We would like to thank the support of all the facilitators and actors who participated in this study and the Northern Ontario School of Medicine for providing the primary author with financial support.
References
1. Orchard C, Bainbridge L, Bassendowski S, Casimiro L, Stevenson K, Wagner S, et al. A national interprofessional competency framework. (Internet) 2010. Available: www.cihc.ca/files/CIHC_IPCompetencies_Feb1210.pdf (Accessed 12 May 2013).
2. Way D, Jones L, Baskerville NB. Improving the effectiveness of primary health care through nurse practitioner/family physician structured collaborative practice. Canadian Medical Association Journal 2001; 165(9): 1210-1214.
3. Reeves S, Perrier L, Goldman J, Freeth D, Zwarenstein M. Interprofessional education: effects on professional practice and healthcare outcomes (update). Cochrane Database of Systematic Reviews 2013; (3).
4. D'Amour D, Oandasan I. Interprofessionality as the field of interprofessional practice and interprofessional education: an emerging concept. Journal of Interprofessional Care 2005; 1: 8-20.
5. Hean S, Dickinson C. The Contact Hypothesis: an exploration of its further potential in interprofessional education. Journal of Interprofessional Care 2005; 19(5): 480-491. https://doi.org/10.1080/13561820500215202
6. Freeth D, Reeves S. Learning to work together: using the presage, process, product (3P) model to highlight decisions and possibilities. Journal of Interprofessional Care 2004; 18(1): 32-56. https://doi.org/10.1080/13561820310001608221
7. WildER Med. WildER Med: a wilderness medicine conference. (Internet). Available: http://www.wildermed.org (Accessed 30 June 2014).
8. Debajehmujig Storytellers. Debajehmujig Storytellers. (Internet). Available: http://www.debaj.ca (Accessed 30 June 2014).
9. Robertson J, Bandali K. Bridging the gap: enhancing interprofessional education using simulation. Journal of Interprofessional Care 2008; 22(5): 499-508. https://doi.org/10.1080/13561820802303656
10. van Soeren M, Devlin-Cop S, Macmillan K, Baker L, Egan-Lee E, Reeves S. Simulated interprofessional education: an analysis of teaching and learning processes. Journal of Interprofessional Care 2011; 25(6): 434-440. https://doi.org/10.3109/13561820.2011.592229
11. Hafferty FW. Beyond curriculum reform: confronting medicine's hidden curriculum. Academic Medicine 1998; 73(4): 403-407. https://doi.org/10.1097/00001888-199804000-00013
12. Glaser BG. Theoretical sensitivity: advances in the methodology of grounded theory. Mill Valley: Sociology Press, 1978; 93-134.
13. Mohaupt J, van Soeren M, Andrusyszyn M, MacMillan K, Devlin-Cop S, Reeves S. Understanding interprofessional relationships by the use of contact theory. Journal of Interprofessional Care 2012; 26(1): 370-375. https://doi.org/10.3109/13561820.2012.673512
14. Gittell JH, Godfrey M, Thistlethwaite J. Interprofessional collaborative practice and relational coordination: improving healthcare through relationships. Journal of Interprofessional Care 2013; 27(3): 210-213. https://doi.org/10.3109/13561820.2012.730564
15. Oandasan I, Reeves S. Elements of interprofessional education Part 1: the learner, the educator and the learning context. Journal of Interprofessional Care 2012; (Suppl.1): 21-38.
16. Kitto S, Nordquist J, Peller J, Grant R, Reeves S. The disconnections between space, place and learning in interprofessional education: an overview of key issues. Journal of Interprofessional Care 2013; 27(S2): 5-8. https://doi.org/10.3109/13561820.2013.801410
17. Mariano C. The case for interdisciplinary collaboration. Nursing Outlook 1998; 37(6): 285-288.

