Introduction
General practitioners often have the uncomfortable role of gatekeeper concerning referrals to hospital1,2. They are assumed to ensure both equity and effectiveness in their daily practice through fair resource rationing of patients.
Low-grade continuity in the doctor-patient relationship is associated with lower confidence, the meeting with a new doctor potentially being a source of uncertainty and insecurity3. This can influence the communication and relationship between doctor and patient. It could also be assumed that the patient's threshold for seeing the doctor is affected4,5. A combination of these factors could impact on the proportion of patients referred on. Thus the type of doctor available to a population could influence the health situation of individuals. For example, prevention and follow up of cardiovascular disease has been shown to be inferior for patients who do not have a regular GP (RGP)6.
It is a traditional perception that the supply of specialists at a nearby hospital will increase referrals from primary care. However, community type, rather than specialist supply, has been found to be a factor influencing referral numbers, as has the gender and age of the physician7. Referrals to hospital and specialists may also be related to the patient case mix, for example the older the patients, the more patients with chronic diseases, and the more referrals. However, in some studies approximately two-thirds of the variation in referrals remained unexplained8. In a study of referrals from general practice to physiotherapy a large variation was found that could not be explained by measured characteristics such as practice location, or age and gender of the GP9. There are obviously other factors beside the need of the patient and the seriousness of the disease that determine referral to hospital.
Primary care and referral in Norway
Patients in rural Norway are listed with their 'assigned GP' (or the GP's PHC), who is responsible for providing primary care for both elective and more urgent matters. In situations where a list has no 'assigned GP', the PHC provides care using locum doctors (LDs) or regular colleagues.
The 'standard path' for hospital referral in rural Norway is for the 'assigned GP' to refer the patient to the local hospital for further assessment. If, for reasons of time or medicine, the local hospital cannot provide the required treatment, the patient is passed on to a regional hospital, which constitutes the next healthcare level.
Objective
The objective of this study was to analyse the referral patterns of two rural primary health care (PHC) centres to the same district hospital. In addition, this study sought to clarify whether the mainly LDs at one of the primary care centres had a different pattern of referral from the workforce of RGPs at its comparable neighbouring primary care centre.
Methods
The geographical sites
The study focused on two rural communities (Herøy and Dønna) on the Atlantic coast of northern Norway (Fig1). These two communities are equally sized neighbours in the archipelago of the Helgeland District. Both communities have their own PHC centre. A relatively short distance from both communities is a small town with a district hospital (Sandnessjøen Hospital). Due to the local geography, the structure of public transportation systems and Sandnessjøen Hospital's medical supply and capacity, this hospital receives almost all patients referred to hospital from primary care in the two nearby communities.
This study includes all patients referred to Sandnessjøen Hospital from the two primary care centres in the year 2003.
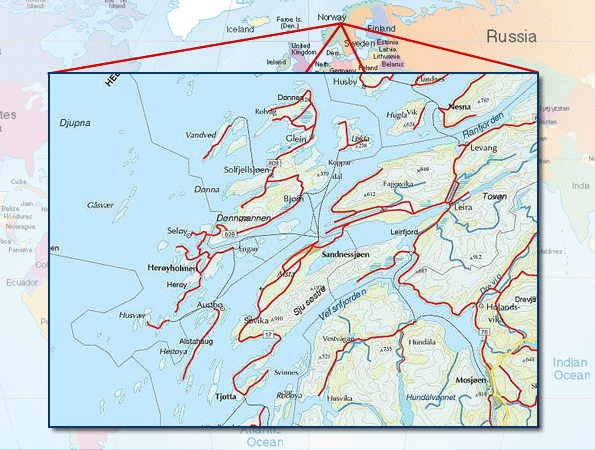
Figure 1: Map of the Atlantic coast of northern Norway, including roads and ferries, showing the two rural communities (Herøy and Dønna) in the archipelago of Helgeland District. ©Kystatlas and used with permission.
In Herøy approximately 99% of the population is listed with the local PHC, and the remainder mainly with Dønna PHC. In Dønna, nearly 100% of the population is listed with GPs at Dønna PHC. These figures have been stable for years. Demographically, the two communities are similar10. In 2003, the population sizes were 1793 for Herøy and 1541 for Dønna. The main industries in both communities were fisheries, agriculture, small industry and employment in the public sector. The age structure of the two communities was also similar (Fig2). It was assumed that the two communities' health situation, environmental factors, culture and genetics were all comparable.
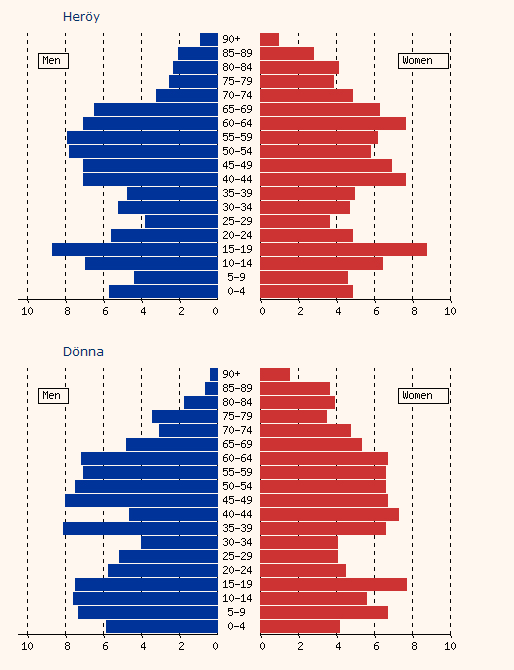
Figure 2: Age structure for male and female inhabitants in the two rural local communities (Herøy and Dønna); first graph is for Herøy, followed by Dønna10.
The majority of GPs in the hospital catchment area come from the Nordic countries, although information is not available about their country of education. An important difference between the two PHCs was that the Herøy primary care centre was served by a continuous supply of LDs, whereas the Dønna primary care centre had a more stable group of RGPs available throughout the year. Other PHC centres in the hospital catchment area also employed LDs during 2003 but as relievers rather than the regular source of care.
The community at Dønna was mainly served by RGPs who worked in their position for an average of 112 days (median 59 days) during 2003. The shortest serving time was 2 weeks, while the longest-serving doctor had been in his position continuously for 17 years. The median age for doctors in Dønna was 37.5 years. The community at Herøy was served by a succession of 17 LDs during the year 2003. Each doctor was employed for an average of 31.6 days (12-106 days, median 18 days). The LDs came from Sweden and their median age was 35.2 years.
Data collection
The data for this study were drawn from 5566 anonymized patient medical records from the district hospital for the year 2003. All patients were grouped according to the classification of their first, main diagnosis, as given by the hospital, in the chapters of ICD-10. Referral from the two studied PHC centres was identified as 307 from Herøy community (LD) and 240 from Dønna community (RGP).
Data analysis
Background data relating to demographic factors and the social and health situation of the two communities were collected from Norwegian official statistics and the Norwegian Directorate for Health and Social Affairs website10,11.
Because the gate-keeper function for primary care is unclear for ICD-10 chapter XXI 'Factors influencing health status and contact with health services', this diagnostic group was excluded from further analysis. The pattern of diagnoses for the remaining ICD-10 chapters were compared between the two PHC centres and also compared with the pattern for the district hospital's total patients in the same year (n = 4019). Based on percent-wise variations, chapters IV 'Endocrine, nutritional, metabolic', VI 'Nervous system', IX 'Circulatory system', X 'Respiratory system', XIV 'Genitourinary system' and XVIII 'Symptoms and signs' showed a differing pattern, which was analysed further using the two-tailed χ2 test.
Results
As is shown (Table 1), the number of primary care doctors was approximately the same in both communities. The Herøy inhabitants (LD) had slightly more visits to their doctor compared with those in Dønna (RGP), and the consumption of whole-day somatic care at the district hospital was also slightly higher for the Herøy population. However, the number of care days per hospital admission was lower for the Herøy (4.7 days) than the Dønna community (5.4 days).
During the period 2000-2006, the consumption of somatic hospital days was very similar between the two communities (Herøy [LD] 23.5 days vs Dønna [RGP] 23.4 days).
Table 1: Healthcare indicators for the communities of Herøy and Dønna, 2003. Data from the Norwegian Directorate for Health and Social Affairs11

The total number of referrals was approximately 200/1000 inhabitants/year (ICD-chapter XXI excluded) for the period 2000-2006 for both communities, differing insignificantly. For 2003, the total number of referrals to the district hospital was 240 from Dønna (RGP) and 307 from Herøy (LD), ICD-chapter XXI excluded. The number of patients referred in 2003 to the district hospital, excluding those from the studied two PHC centres, was 5019.
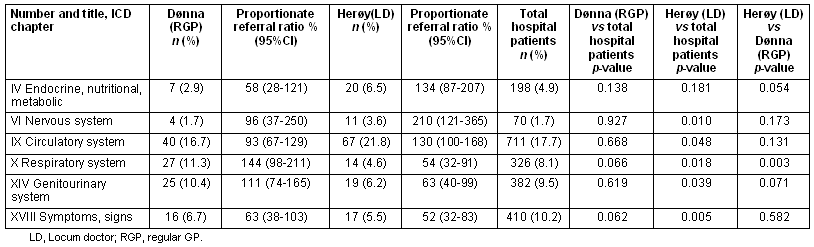
The diagnosis pattern as percentage distribution among diagnosis chapters is shown (Table 2) for the patients from Herøy and Dønna PHCs and for the rest of the patients at the district hospital. Table 2 also shows the proportionate referral ratio, calculated as the percentage of the expected number of patients, based on the total hospital material (n = 4019). Herøy community (LD) had significantly more referrals than was expected for chapter VI 'Diseases of the nervous system' (p = 0.010), and chapter IX 'Diseases of the circulatory system' (p = 0.048). However, Herøy (LD) had significantly fewer referrals for chapter X 'Diseases of the respiratory system' (p = 0.018), and chapter XIV 'Diseases of the genitourinary system' (p = 0.039). There were also significantly fewer Herøy referrals for chapter XVIII 'Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified' than the norm for the rest of the patients at the district hospital (p = 0.005). For 14 out of the 19 studied ICD chapters (chapter XXI excluded), Herøy did not differ significantly from expected values (data not shown). These 14 ICD-chapters represent 2360 out of 4019 patients, or 59% of the total material. Dønna did not differ significantly from the total material in any ICD chapter.
Table 2: The pattern of diagnoses, shown as distributed among selected ICD-chapters, for patients from the two rural primary health care centres (Herøy and Dønna) and for the remainder of patients at the district hospital, 2003.
Discussion
Main findings
This study compared all referrals in one year to a district hospital from primary care in two different but comparable rural communities in Norway, and relates them to the local norm. The major difference between the two PHCs was that one was exclusively run by short-term LDs and the other by RGPs during the year studied. Compared with the local norm, the locum-run PHC referred relatively more patients to the district hospital with diagnoses relating to the nervous and circulatory systems, and relatively fewer patients with respiratory or genitourinary disease.
When examining referrals from the Herøy PHC (LD) for chapter IX 'Diseases of the circulatory system', the most frequent diagnosis was I20.9 unspecified angina pectoris. Assuming that the sub-populations within the hospital's catchment area have equal health status, the angina incidence should be similar within random variations. If this is correct, angina may have been over-diagnosed by the LDs, or under-diagnosed by RGPs in the rest of the area. A previous study found that prevention and follow up was less effective when patients did not have an RGP6. The increased frequency of cardiovascular referrals from the LDs' PHC may have been in compensation for such an effect.
Both over- and under-diagnosing have potential consequences. Under-diagnosing of angina pectoris may increase suffering and lower quality of life and survival for individual patients. When time is of essence, the diagnosis will influence the type of transportation or ambulance unit used for transfer to hospital. Thus, the doctor's diagnosis impacts on transport costs, because different means of transport differ in terms of cost. Further discussion of patient consequences and healthcare expenditure implications are outside the scope of the present study.
Factors affecting referrals
Differences in referral rate could reflect that LDs in rural primary care have a lower 'threshold' than RGPs for referring a patient to hospital. In this study the referral frequency (number of referrals/1000 inhabitants/year) was similar in the two groups of doctors, suggesting that locum and regular doctors had a similar threshold for hospital referrals. The number of consultations divided by the number of referred patients also gives similar referral ratios between the sites.
It can be assumed that the level of continuity in a doctor-patient relationship can influence the doctor's choice to either refer the patient at once or to 'wait and see'. An LD who works on his own and will leave in the near future cannot easily follow up the patient personally or by asking colleagues. In this situation, the doctor may refer the patient 'for the sake of safety', in order to secure continuity and quality in follow up and treatment, or possibly hoping to leave follow up to the hospital. In addition, physicians in a single practice have been found to have a higher referral rate than physicians in a group practice, as have physicians with a high work load12. Both these factors may be applicable in this case.
The doctor's number of years in the profession has been shown to influence treatment quality, although most often negatively13. Also, the guidance function from secondary to primary care obviously works best when the primary care doctor has been at his post for some time.
The referring doctor does not work in a vacuum but acts in intersection between the patient's expectations, his own knowledge, and the support of practice colleagues. The LDs in Herøy worked on their own approximately 50% of the time, thereby reducing the chance of such support. A regular doctor is also able to 'wait and see', making a new appointment for the patient and a quick referral if the patient's condition changes.
The patient's wishes will also be of importance. It has been shown that short duration and low grade of continuity in the doctor-patient relationship is associated with lower patient confidence4. The patient may request a referral, especially if he has a longer relationship with and loyalty to the local hospital clinic.
Practical factors such as a lack of diagnostic facilities and equipment, especially in an ambulant rural setting, could cause the doctor to 'err on the safe side'. As far as it could be established retrospectively, the doctors in the two communities had similar diagnostic equipment, both at their offices and available when making home calls.
Because all LDs came from the neighbouring country Sweden, lingual and cultural barriers may have affected the communication between doctor and patient, but neither of these are likely to have had a substantial influence on the doctor's assessment or other efforts. In the Nordic countries, medical education and training are similar, as are treatment protocols, with some local adaption. For this reason, any possible influence from the LD's training and 'national medical culture' should be considered minor.
One should also recognize similarities in the pattern of referral between the two healthcare centres. For 59% of the referred patients, constituting 14 out of the 19 studied ICD-chapters (chapter XXI excluded), no significant difference was found between the referral patterns of LDs and the norm for PHCs in the hospital's catchment area.
Limitations and methodological considerations
Limitations in this study should be considered. The analysed rural local communities are quite small, as is the district hospital, and the study only spans one year. However, this district is typical of rural Norway and the uncomplicated lines of communication and referral makes it suitable for studies of this kind.
The analysed data were based on the hospital's main diagnosis, and thus not on the referring doctor's (preliminary) diagnosis. The hospital's independent diagnosing is an important part of the referral process, providing a 'second opinion' and thereby further clarifying the diagnostic picture. Minor differences between the hospital's main diagnosis and the referring doctor's will not affect data validity, because our analysis is based on a division into whole ICD chapters, not single diagnoses. If the hospital's diagnosis were to belong in a different ICD chapter this would, of course, affect the validity of the basic data, and thereby the conclusions.
Another possible source of error is that the data only states the district in which the patient lived, not which individual GP made the referral. Patients are expected to see their 'assigned GP' for all primary care and the assumption was made that this was so and that they were referred from their own PHC. Because the two districts cooperate in having one doctor on call outside working hours, it can be assumed that there has been some degree of 'mixing', where a patient was referred by the opposite district's doctor. If this mixing was widespread, the real differences were larger than we were able to prove in the present study. Less than 1% of the Herøy inhabitants are listed with doctors at the Dønna PHC, their diluting impact on the elective consultations in Dønna thus being insignificant. Similarly, the impact on Herøy PHC would be insignificant even if these individuals consistently saw the local PHC for urgent care.
The referral pattern from primary care has been shown to fluctuate short term, especially weekly14. Because this material is based on a whole year, the effect of short-term variations could be considered eliminated.
Conclusion
The difference in referrals for LDs compared with larger area referral patterns from primary care shown in this study indicates that both over-referral and under-referral occurred, possibly in part based on over- and under-diagnosing, respectively. Both phenomena would imply costs and consequences. For society, over-referral generate expenses in the form of 'unnecessary' examinations, occupied hospital beds, or more expensive and risky transportation of patients. For patients, under-referral could increase suffering, decrease quality of life and even lower survival rates.
References
1. Carlsen B, Norheim OF. Introduction of the patient-list system in general practice. Changes in Norwegian physicians' perception of their gatekeeper role. Scandinavian Journal of Primary Health Care 2003; 21: 209-213.
2. Carlsen B, Norheim OF. 'Saying no is no easy matter' a qualitative study of competing concerns in rationing decisions in general practice. BMC Health Services Research 2005; 5: 70.
3. Steine S, Finset A, Lerum E. Hva er viktig for pasienten i møtet med allmennpraktikeren? Tidsskrift for den Norske Lægeforening 2000; 120: 349-353 (in Norwegian).
4. Mainous 3rd AG, Baker R, Love MM, Gray DP, Gill JM. Continuity of Care and Trust in One's Physician: Evidence from Primary Care in the United States and the United Kingdom. Family Medicine 2001; 33: 22-27.
5. Norwegian Board of Health Supervision. Report no 13/2004: Allmennlegetjenesten - en risikoanalyse. Oslo: Norwegian Board of Health Supervision, 2004 (in Norwegian).
6. Devroey D, Coigniez P, Vandevoorde J, Kartounian J, Betz W. Prevention and follow-up of cardiovascular disease among patients without a personal GP. Family Practice 2003; 20: 420-424.
7. Chan BT, Austin PC. Patient, physician, and community factors affecting referrals to specialists in Ontario, Canada: a population-based, multi-level modelling approach. Medical Care 2003; 41: 500-511.
8. Sullivan CO, Omar RZ, Ambler G, Majeed A. Case-mix and variation in specialist referrals in general practice. British Journal of General Practice 2005; 55: 529-533.
9. Jörgensen CK, Olesen F. Predictors for referral to physiotherapy from general practice. Scandinavian Journal of Primary Health Care 2001; 19: 48-53.
10. Statistics Norway. KommuneFakta - Nordland. (Online) 2008. Available: http://www.ssb.no/kommuner/region.cgi?nr=18 (Accessed 8 January 2009).
11. Norwegian Directorate for Health and Social Affairs. Nyttig å vite før du begynner. (Online) 2008. Available: http://nesstar.shdir.no/khp/index.jsp (Accessed 8 January 2009).
12. Iverson GD, Coleridge ST, Fulda KG, Licciardone JC. What factors influence a family physician's decision to refer a patient to a specialist? Rural Remote Health 5: 413. (Online) 2005. Available: www.rrh.org.au (Accessed 8 January 2009).
13. Choudry NK, Fletcher RH, Soumerai SB. The relationship between clinical experience and quality of health care. Annuals of Internal Medicine 2005; 142: 260-273.
14. Vehviläinen AT, Kumpusalo EA, Takala JK. They call it stormy Monday - reasons for referral from primay to secondary care according to the days of the week. British Journal of General Practice 1999; 49: 909-911.
Abstract
Introduction: A patient's needs and the seriousness of the disease are not the only factors that determine referral to hospital. The objective of this study was to analyse whether locum doctors (LDs) have a different pattern of referral to hospital from regular GPs (RGPs).
Methods: All hospital referrals for one year (n = 5566 patients) from two Norwegian rural primary health care (PHC) centres to the nearby district hospital were analysed with regard to ICD-10 diagnosis groups. A major difference between the PHCs was that one had a continuous supply of LDs while the other had a stable group of RGPs. The equal-sized communities were demographically and socio-culturally similar.
Results: The PHC centre mainly operated by short-term LDs referred a relatively high number of patients to the district hospital within the diagnosis groups of chapter VI 'Diseases of the nervous system' (proportionate referral rate 210%; p = 0.010), and chapter IX 'Diseases of the circulatory system' (proportionate referral rate 130%; p = 0.048), and a comparatively low number of patients for the diagnostic groups in chapter X 'Diseases of the respiratory system' (p = 0.018), and chapter XIV 'Diseases of the genitourinary system' (p = 0.039), compared with the norm of the district hospital's total population. The number and proportion of the total number of referrals, adjusted for population size, did not differ between the two rural communities. The LD-run PHC centre differed significantly from the total norm in 5 out of 19 ICD chapters, equal to 41% of the patients.
Conclusions: Only one significant difference in hospital referrals related to ICD-diagnoses groups were found between the studied rural PHC centres, but the LD-run PHC differed from the total norm. These differences could neither be explained from the district's consumption of somatic hospital care nor the demographical differences, but were related to staffing at the PHC, that is LDs or RGPs. The analysis also revealed that possible under- and/or over-diagnosing of certain diseases occurred, both having potential medical consequences for the patient, as well as increasing healthcare expenditure.
Key words: hospital, locum doctors, primary care, referral, referral pattern, rural area.
You might also be interested in:
2014 - The right staffing mix for inpatient care in rural multi-purpose service health facilities
2014 - How accurate is the diagnosis of diabetic retinopathy on telescreening? The Indian scenario

