Introduction
Approximately 19% of US children aged 6 to 11 years are classified as obese (ie sex-specific Body Mass Index [BMI] for age ≥95th percentile) and an additional 18% overweight (85th to <95th percentile)1. Children who are obese are at increased risk of numerous physical and psychosocial health consequences, including type 2 diabetes, risk factors for cardiovascular disease, social difficulties, and lower self-esteem, as well as additional health complications in adulthood2. Additionally, research shows associated economic burdens, with overweight accounting for approximately 9% of total annual medical expenditures in the US in 19983.
Similar to trends observed in ethnic minority groups1, the problem of overweight is more common in children residing in rural areas4. Both higher prevalence rates and greater health risk behaviors, including unhealthy diet and less physical activity, have been documented among individuals in rural areas5,6. The Appalachian Region Commission has described Appalachia as a particularly high-risk population with an excess of premature deaths due to overweight/obesity related causes (eg cardiovascular disease, diabetes, cancer)7. The Institute of Medicine recently concluded that more evidence from varied types of evaluations in diverse settings is needed to identify promising approaches to preventing childhood obesity8. This article describes results from focus groups conducted with teachers, parents, and students in one school community during the development of a school-based obesity prevention initiative in rural Appalachia, called Winning with Wellness.
Methods
Setting
The setting for this 2005 study was an elementary school with students in kindergarten through fourth grade, located in a rural northeast Tennessee (TN) county (timeline shown in Table 1). At the time of the study the county was one of 10 pilot sites for the Tennessee Coordinated School Health (CSH) Project. The state of TN Department of Education was appropriated funding for a pilot study of CSH after the legislature passed TCA 49-1-1002- the CSH Improvement Act of 2000. The CSH model, developed by Allensworth and Kolbe9, includes 8 components: (i) nutrition services; (ii) physical education; (iii) health services; (iv) health education; (v) counseling/psychological/social services; (vi) family/community involvement; (vii) health promotion for staff; and (viii) healthy school environment.
The US Centers for Disease Control and Prevention (CDC) has advocated use of the CSH Program model as a comprehensive approach to promoting child health via involvement of schools, families, healthcare organizations, media, and community groups10. In 2004, amid concern about the problem of child obesity in northeast TN, a partnership between TN CSH, a local department of education, a regional hospital system, and the Department of Pediatrics at East Tennessee State University facilitated the formation of a multidisciplinary coalition including health care providers, educators, researchers, parents, media, and business personnel who began discussing how to curb the epidemic of child obesity through a school-based initiative based on the CSH model. Employing a community based participatory research approach to program development and evaluation, the coalition sought input from school community stakeholders11.
Table 1: Timeline of Tennessee Coordinated School Health Project, focus group and Winning with Wellness activities
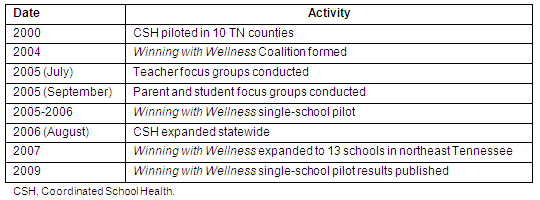
Population and sample
Based on 2000 census data, it was estimated that there were 107 198 persons residing in the study county, with 22 833 of these being under the age of 18 years. Approximately 4% of the population is African American and 1% Hispanic or Latino. Data from 2002 estimate that 13.7% of persons and 17.6% of children under the age of 18 years are living below the poverty level12.
The elementary school has a total of 491 students, 41 teachers, and 105 total staff. Approximately 52% of students are classified as economically disadvantaged13. Purposeful sampling ensured participation by members of 3 stakeholder groups in the school community: teachers, parents, and fourth-grade students14. All teachers and academic staff at the school were invited to participate; school administrators identified parents who had volunteered at the school to invite to participate in the study. One fourth-grade class was chosen to participate by the principal.
Procedure
Human subject approval and study oversight was provided by the East Tennessee State University Institutional Review Board.
Focus groups were conducted according to established methodology14-19. Data were collected during the summer-fall of 2005. Focus groups were conducted in settings familiar to the participants. Teachers participated in focus groups during 2 teacher in-service days in July 2005. During September 2005, parents participated during an open house meeting at the school and children participated during the school day.
Written informed consent was obtained from both teachers and parents. A letter that described the study was sent home with students asking parents to indicate if they did not want their child to participate. Verbal informed assent was obtained from child participants prior to their participation.
At the beginning of each focus group, the trained moderators (ie Caucasian medical doctor and Caucasian medical student) discussed the estimated length (ie 60-90 min for adults and 30-40 min for students) and the purpose of the discussion, as well as rules to assist the discussion to proceed smoothly. All focus groups were audio-recorded. As an incentive, teachers received refreshments and US$10 for their participation. The school received $10 for each parent and student who participated in the study.
Measures
Moderators used a written guide (available from the authors) developed specifically for the study and participant group, bearing in mind the CSH model, with input from the coalition to facilitate the discussion and provide consistency across the groups. Open-ended questions and queries were used to facilitate discussion. All groups were asked similar questions regarding perceptions of school nutrition (eg 'What do you think about the food served in the school cafeteria?') and physical education (eg 'How much physical activity and physical education do students get at school?'). Questions also assessed family and community involvement with children's eating and physical activity as well as views regarding the relationships among eating and physical activity, school behavior and academic performance. In addition, teachers and parents were asked about perceptions of child overweight and perceived barriers/reactions to a school-based obesity prevention program based on the CSH model. Students were asked about school rules and changes the school should make regarding nutrition and activity. Nothing was asked about 'weight' or discussed during the student focus groups.
Analysis
Data analysis included a systematic approach aimed at preserving the reliability and validity of the data20,21. Transcripts were made from focus group audio-recordings. Using an induction method and following a multistage interpretive thematic process, these transcripts were first reviewed and independently coded by the two focus group moderators to identify themes across variables of interest. These included perceptions about school nutrition and physical activity (including views regarding parental involvement and influence on school behavior and academic performance), as well as perceptions regarding child overweight and thoughts about barriers to improving nutrition and physical activity and proposed changes in the school. These broader conceptual categories were refined further via constant comparison within and across transcripts. Following independent coding, the team engaged in consensus coding by reviewing themes and reaching agreement on common themes as well as representative quotations. The CSH model was used as a framework for organizing themes and highlighting their relevance for the design of interventions.
Results
The participants were 23 teachers (96% female), 12 parents (92% female), and 19 fourth grade students (58% female) out of a total of 97 students. A repetition of themes was heard within and across participant groups16. Common themes are presented according to CSH model component in statements provided by teachers, parents, and students (Table 2).
Table 2: Focus group themes and statements according to Coordinated School Health (CSH) model components
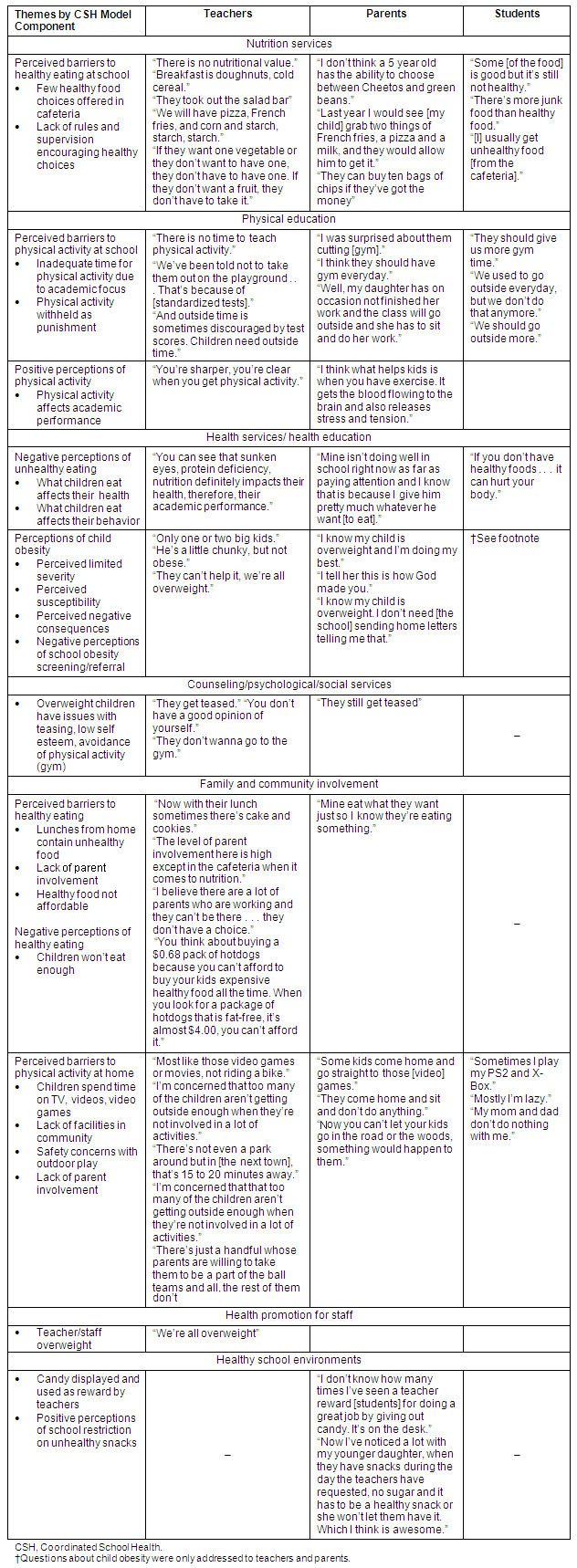
Nutrition services
Teachers, parents and students all agreed that there were not enough healthy food choices offered in the school cafeteria. Teachers reported that students were only expected to have three items on their cafeteria tray, and the school policies about selection of these items (ie students are not required to choose a fruit or vegetable) and purchase of a la carte items did not promote healthy eating. Parents perceived their children as unable to make healthy choices without guidance and suggested parent volunteers were needed to assist children in making healthy food choices. Students were aware of healthy options in the cafeteria, but many admitted to choosing less healthy foods. Lunches brought from home also included unhealthy options.
Teachers and parents agreed that students performed better academically if they made healthy food choices and participated in physical activity. Students also perceived diet to negatively impact behavior.
Physical education
Students at the school had 45 min of physical education once a week. Teachers, parents, and students expressed that this was not enough time. Teachers described pressures to meet expectations for standardized test performance as interfering with time for physical activity. Some parents believed that physical activity was inappropriately withheld by certain teachers as a form of punishment. According to teachers, sitting quietly all day and not having any physical activity makes children tired and unable to concentrate. Parents and student mentioned this relationship as well.
Health services/health education
Teachers believed that child overweight was not prevalent in their school, citing only 'one or two big kids'. Teachers seemed hesitant to label children as overweight/obese. One teacher said, 'He's a little chunky, but not obese', and that 'they can't help it, we're all overweight'. Parents were aware of child overweight with several admitting their child was overweight; however, some parents stated that they do not feel able to change their child's weight. BMI screening at school was not perceived favorably by several teachers or parents.
Counseling/psychological/services
Teachers perceived that overweight children have low self-esteem, get picked on, and do not participate in gym activities. Parents were also concerned that overweight children are teased, although one parent thought this was less of a problem since overweight has become more common.
Family and community involvement
Parents indicated concern that children would not eat enough if forced to eat healthy foods. They often reported that knowing their child was eating something at lunch everyday was important, whether what they ate was healthy or not. Financial constraints to parental provision of healthy foods and guidance on healthy eating were also noted by both teachers and parents.
Although some of the students stated that they were active, many reported playing video games or watching TV after school. Related to concerns about physical activity away from school, one teacher stated that the community does not have a safe place for children to play; others cited lack of parent involvement in promoting physical activity through sports participation.
Health promotion for staff
While teacher/staff health was not among the planned discussion topics for these focus groups, the high prevalence of overweight among teachers and staff was mentioned by a teacher who seemed to sympathize with overweight students: 'They can't help it we're all overweight'. In fact, 85% of teachers surveyed as part of the Winning with Wellness pilot project evaluation described themselves as overweight22.
Healthy school environments
Proposed changes and potential barriers to promoting healthy eating and physical activity were discussed. Teachers were worried that time, teacher enthusiasm, and administrative and parental support could be barriers to implementing an overweight prevention program. One teacher said, 'There's going to be parents who complain about [the program], they complain about anything'. Teachers recommended opening the gym after school, establishing a walking trail on school grounds and a daily fitness program with incentives for students. One teacher suggested that students 'exercise to music'. Many teachers were also in favor of students having pedometers to help them become more aware of their activity level. Parents suggested discontinuing the use of food as a reward and no longer withholding physical activity as a punishment. A student recommended putting 'healthy ice cream' in the cafeteria. Teachers also agreed that encouraging healthy snacks could be beneficial to students. Parents and students suggested students should have physical education daily.
Discussion
The school setting continues to be recognized as important for promoting the development of healthy behaviors in children23. While demonstrating improvements in diet and increases in physical activity24, school-based obesity prevention programs have produced small changes in weight, indicating a need for more effective programs25. A recent review of existing programs recommended tailoring future programs to the needs of specific populations26. Research documenting effective school-based prevention programs, particularly among rural populations, is limited.
The three largest and most successful school-based programs emphasized the importance of involving stakeholders in planning, implementing, evaluating, and disseminating programs. These programs also included easy to use curricula, training, sound research methodology, and use of the CDC School Health Index for development and evaluation, as well as implementation27. Additional researchers have suggested more comprehensive approaches incorporating the involvement of stakeholders, programmatic and policy change, and sustainability24,26.
In the current study, teachers, parents, and students described cafeteria menus and practices as not promoting healthy eating and identified a need for additional physical activity during school hours. These reports are not uncommon. The recent Expert Committee Recommendations on the prevention of childhood obesity suggest improvements are needed in both diet and physical activity across school settings23. A recent review of school-based programs26 provides support for programs targeting these issues.
In the current study, students admitted to making less healthy food choices at school. Results revealed that lunches brought from home often contained unhealthy food items. Parents reported that the high prices of healthy food items affected their food choices at home. Some parents reported that simply knowing their children are eating anything is satisfactory. A lack of school policies encouraging healthy food choices in the cafeteria were concerns for both teachers and parents.
Physical education was offered only 45 min per week. This was far below the ≥30 min of physical activity per day at school recommended by the Institute of Medicine8. Data collected by CSH in Tennessee show student fitness compares poorly with national standards (20th-30th percentile on the President's Council on Physical Fitness)28. Teachers suggested having children exercise to music, wear pedometers, and receive incentives for physical activity. Parents recommended that withholding physical activity not be used as a punishment for misbehavior. In a prior study of perceptions of overweight factors, parents and students favored encouragement and reward for sustaining child involvement in nutrition and physical activity29.
Teachers also reported concerns that children were sedentary at home (eg television, video games) and attributed lack of parental involvement and areas to play safely as problems. Parents provide an important influence on the development of eating and activity behaviors in children30. Parents in rural areas may face additional barriers to providing healthy food options and opportunities for activity because of higher rates of poverty4 as well as fewer facilities and resources promoting healthy activity31. Teachers in the current study suggested developing a walking trail at the school.
The lack of involvement by some parents with the school was recognized by teachers as a significant barrier with speculation that increased working demands among parents contributed to this issue. On the other hand, some parents reported feeling that the school did not want them to be involved and suggested that parent involvement should be encouraged to promote healthier eating in the school cafeteria. Although research is limited, reviews of interventions for children who are overweight and/or obese clearly support parental involvement32,33. One of the most successful school-based prevention programs, Coordinated Approach to Child Health (CATCH), included a parental component34. Additionally, the Expert Committee recommendations for preventing obesity suggest parental involvement23, and a study on CSH in Massachusetts found parental and community involvement to be important factors for sustainability of the program35.
Teachers, parents, and students believed that nutrition and physical activity affect health and academic performance. Despite these beliefs, some teachers cited restrictions on physical activity resulting from demands for high performance on standardized tests. Research has shown a relationship between healthy lifestyle changes and improvement in school performance indicators36.
Teachers reported little awareness of overweight children within the school despite 47% of fourth-graders in the ten TN CSH pilot sites being classified as overweight or obese, based on BMI screening during 2004-200537. Contrary to a recent study demonstrating parents' lack of awareness of their child's overweight38, the parents in the current study recognized overweight in their own as well as other children. The feasibility and benefits of BMI screening have been previously demonstrated in schools in rural Appalachia39. However, neither teachers nor parents in the current school were receptive to BMI screening. Findings in this area appear to vary. Some studies show parental interest in receiving BMI information40, whereas others show less importance placed on BMI measurement41.
Both groups of adults in the current study reported little perceived control over children's weight, rather emphasizing the importance of acceptance. In terms of making school-based changes to promote healthier eating, more physical activity, and prevent obesity, teachers perceived barriers to include time, enthusiasm, and parental and administrative support.
Teachers did recognize lower self-esteem and withdrawal from physical activities by children who are overweight. A recent study42 aimed at developing an integrated (ie targeting eating disorders and obesity) school-based intervention assessed student, parent, and school staff perceptions and found weight-related teasing and body image issues as prominent concerns. The CSH model prepares schools for addressing these co-morbidities by including a counseling or psychological services component.
The current study was qualitative and exploratory in nature. Limitations included the small sample size and collecting data in only one rural school setting. There was also potential for bias in those who were willing to participate. However, the current study provided important information that contributed to the development of a pilot intervention, Winning with Wellness, that was based on the CSH model, and aimed at improving nutrition and physical activity in the same rural elementary school22. This study, to our knowledge, represents the first attempt to understand multiple stakeholders' perceptions of school nutrition, physical activity, child overweight and the schools' role in obesity prevention in a rural school setting. This is important given the higher rates of overweight, poorer health outcomes, and limited health resources in rural populations. Further, individualized assessment regarding needs, barriers, and proposed changes are needed for prevention programs to be successful.
A pilot study in Florida demonstrated both feasibility and sustainability along with improved school performance using the CDC CSH approach36. Additionally, coordinated school health programs for healthy eating in Nova Scotia were associated with healthier diets, greater physical activity, and lower percentages of overweight among children, compared with schools only reporting policies and practices for offering healthy food alternatives43. Similar approaches may be especially important for rural areas where prevalence rates of obesity are higher4 and resources more limited44.
Conclusion
The existence of the TN CSH Project in the county school system provided both a model for developing interventions and an infrastructure for implementation and evaluation. This on-going study is utilizing a community based participatory research approach to ensure that the needs and perspectives of this population are considered in the design and implementation of school-based obesity prevention efforts, and that information-sharing and dissemination of evaluation findings are a priority. Additional information is also being gathered via multiple methods (self-report, anthropometric measures, cafeteria record review) and multi-informants (students, teachers, school staff) to further direct the development and sustainability of Winning with Wellness.
Acknowledgements
The authors recognize and thank all coalition members and community partners for their contributions in developing, supporting, and implementing the Winning with Wellness Pilot Program, including: Tennessee Coordinated School Health Project, Washington County Department of Education, Mountain States Health Alliance, East Tennessee State University, James H Quillen College of Medicine, America on the Move in Tennessee, University of Tennessee Extension Service, Sherry Franks Beavers, RN, and the pilot school students, parents, teachers, and staff/administrators. This study was supported by an East Tennessee State University Appalachian Center for Translational Research Disparities (ACTRID) grant through funding from NCMHD Project EXPORT grant number 5 R24 MD001106-02 awarded to Dr Joellen Edwards.
References
1. Ogden CL, Carroll MD, Curtin LR, McDowell MA, Tabak CJ, Flegal KM. Prevalence of overweight and obesity in the United States, 1999-2004. Journal of the American Medical Association 2006; 295: 1549-1555.
2. Jelalian E, Mehlenbeck R. Pediatric obesity. In: RC Michael (Ed.). Handbook of pediatric psychology. New York: The Guilford Press, 2003; 529-543.
3. Finkelstein EA, Fiebelkorn IC, Wang G. National medical spending attributable to overweight and obesity: how much, and who's paying? Health Affairs 2003: Jan-Jun(SupplW3): 219-226.
4. Lutfiyya MN, Lipsky MS, Wisdom-Behounek J, Inpanbutr-Martinkus M. Is rural residency a risk factor for overweight and obesity for US children? Obesity 2007; 15: : 2348-2356.
5. Crooks DL. Food consumption, activity, and overweight among elementary school children in an Appalachian Kentucky communit. American Journal of Physical Anthropology 2000; 112: 159-170.
6. Wu T, Wilson JL, Flowers JW, Tudiver F, Glen L, Dunn MS al. Assessment of health risk behaviors among teens in an Appalachian community. American Journal of Epidemiology 2004; 159: S019. (Abstract)
7. Halverson JA, Ma L, Harner EJ. Appalachian Regional Commission. An analysis of disparities in health status and access to health care in the Appalachian region. (Online) 2004. Available: http://www.arc.gov/index.do?nodeId=2467&print=yes%20*%20\ (Accessed 29 September 2008).
8. Koplan JP, Liverman CT, Kraak VI. Preventing childhood obesity: health in the balance: executive summary. Journal of the American Dietetic Association 2005; 105: 131-138.
9. Allensworth DD, Kolbe LJ. The comprehensive school health program: exploring an expanded concept. Journal of School Health 1987; 57: 409-412.
10. National Center for Chronic Disease Prevention and health Promotion, Division of Adolescent and School Health. Healthy youth! Coordinated school health program. (Online) no date. Available: http://www.cdc.gov/HealthyYouth/CSHP/ (Accessed 30 April 2007).
11. Viswanathan M, Ammerman A, Eng E, Gartlehner G, Lohr KN, Griffith D et al. Community-based participatory research: assessing the evidence. Evidence report/technology assessment No. 99. AHRQ Publication 04-E022-2. Rockville, MD. Agency for Healthcare Research and Quality, 2004. Available: http://www.ncbi.nlm.nih.gov/books/bv.fcgi?rid=hstat1a.chapter.44133 (Accessed 15 June 2009).
12. US Census: US Bureau of the Census. Characteristics of Population, Vol. 1. Washington, DC: US Government Printing Office, 2002.
13. State of Tennessee. School report card 2003: Boones Creek Elementary School. Tennessee Department of Education. (Online) no date. Available: http://evaas.sas.com/tn_reportcard/welcome.jsp?Main=1&ID=900&School=25 (Accessed 9 September 2008).
14. Mays N, Pope C. Rigour and qualitative research. BMJ 1995; 311: 109-112.
15. Kitzinger J. Education and debate. BMJ 1995; 311: 299-302.
16. Sandelowski M. Sample size in qualitative research. Research In Nursing and Health 1995; 18(2): 179-183.
17. Patton MQ. Qualitative evaluation and research methods, 2nd edn. Newbury Park, CA: Sage, 1990.
18. Seidman I. Interviewing as qualitative research: a guide for researchers in education and social science. New York, NY: Teacher's College Press, 1998.
19. Adelman C. Uttering, muttering: collecting, using and reporting talk for social and educational research. London, England: Grant McIntyre, 1981.
20. Pope C, Ziebland S, Mays N. Qualitative research in health care: analyzing qualitative data. BMJ 2000; 320: 114-116.
21. Silverman D. Interpreting qualitative data: methods for analyzing talk, text, and interaction. London: Sage, 2001.
22. Schetzina KE, Dalton WT, Lowe EF, Azzazy N, VonWerssowetz K, Givens C et al. A coordinated school health approach to obesity prevention among Appalachian youth: the Winning with Wellness Pilot Project. Family and Community Health 2009; 32(3): 271-285.
23. Davis MM, Gance-Cleveland B, Hassink S, Johnson R, Paradis G, Resnicow K. Recommendations for prevention of childhood obesity. Pediatrics 2007; 120: S229-S253.
24. Budd G, Volpe S. School-based obesity prevention: research, challenges, and recommendations. Journal of School Health 2006; 76: 485-495.
25. Stice E, Shaw H, Marti CN. A meta-analytic review of obesity prevention programs for children and adolescents: the skinny on interventions that work. Psychological Bulletin 2006; 132: 667-691.
26. Summerbell CD, Waters E, Edmunds LD, Kelly S, Brown T, Campbell KJ. Interventions for preventing obesity in children. The Cochrane Library 2005; 4: 1-24.
27. Franks AL, Kelder SH, Dino GA, Horn KA, Gortmaker SL, Wiecha JL et al. School-based programs: lessons learned from CATCH, planet health, and not-on-tobacco. Preventing Chronic Disease 2007; 4: 1-9.
28. Goodrow B, Austin S, Wilder R. Tennessee coordinated school health report. Nashville, TN: Tennessee Department of Education, Office of School Health Programs, 2004.
29. Borra ST, Kelly L, Shirreffs MB, Neville K, Geiger CJ. Developing health messages: qualitative studies with children, parents, and teachers help identify communications opportunities for healthful lifestyles and the prevention of obesity. Journal of the American Dietetic Association 2003; 103: 721-728.
30. Davison KK, Birch LL Childhood overweight: a contextual model and recommendations for future research. Obesity Reviews 2001; 2: 159-171.
31. Janicke DM, Sallinen BJ, Perri MG, Lutes LD, Silverstein JH, Huerta MG et al. Sensible treatment of obesity in rural youth: Design and methods. Contemporary Clinical Trials 2008; 29: 270-280.
32. Jelalian E, Saelens BE. Empirically supported treatments in pediatric psychology: pediatric obesity. Journal of Pediatric Psychology 1999; 24: 223-248.
33. Kitzmann KM, Beech BM. Family-based interventions for pediatric obesity: methodological and conceptual challenges form family psychology. Journal of Family Psychology 2005; 20: 175-189.
34. Luepker RV, Perry CL, McKinlay SM, Nader PR, Parcel GS, Stone EJ et al. Outcomes of a field trial to improve children's dietary patterns and physical activity. The Child and Adolescent Trial for Cardiovascular Health. CATCH collaborative group. Journal of the American Medical Association 1996; 275: 768-776.
35. Cho H, Nadow MZ. Understanding barriers to implementing quality lunch and nutrition education. Journal of Community Health 2004; 29: 421-435.
36. Weiler RM, Pigg RM Jr, McDermott, RJ. Evaluation of the Florida coordinated school health program pilot schools project. Journal of School Health 2003; 73: 3-8.
37. Goodrow B, Austin S, Wilder R. Tennessee coordinated school health report. Nashville, TN: Tennessee Department of Education, Office of School Health Programs, 2005; 1-134.
38. Crawford C, Timperio A, Telford A, Salmon J. Parental concerns about childhood obesity and the strategies employed to prevent unhealthy weight gain in children. Public Health Nutrition 2006; 9: 889-895.
39. Demerath E, Muratova V, Spangler E, Li J, Minor VE, Neal WA. School-based obesity screening in rural Appalachia. Preventive Medicine 2003; 37: 553-560.
40. Murphy M, Polivka B. Parental perceptions of the schools' role in addressing childhood obesity. Journal of School Nursing 2007; 23: 40-46.
41. Murnan J, Price JH, Telljohann SK, Dake JA, Boardly D. Parents' perceptions of curricular issues affecting children's weight in elementary schools. Journal of School Health 2006; 76: 502-511.
42. Haines J, Neumark-Sztainer D, Thiel L. Addressing weight-related issues in an elementary school: what do students, parents, and school staff recommend? Eating Disorders 2007; 15: 5-21.
43. Veugelers PJ, Fitzgerald AL. Effectiveness of school programs in preventing childhood obesity: a multilevel comparison. American Journal of Public Health 2005; 95: 432-435.
44. Jackson JE, Doescher MP, Jerant AF, Hart LG. A national study of obesity prevalence and trends by type of rural county. Journal of Rural Health 2005; 21: 140-148.
Abstract
Introduction: High prevalence rates of obesity, particularly among those residing in US rural areas, and associated physical and psychosocial health consequences, direct attention to the need for effective prevention programs. The current study describes an initial step in developing a school-based obesity prevention program in rural Appalachia, USA. The program, modeled on the Centers for Disease Control and Prevention Coordinated School Health (CSH) Program, includes a community-based participatory research approach to addressing the health needs specific to this region.
Methods: Focus groups with teachers, parents, and 4th grade students were used to understand perceptions and school policy related to nutrition, physical activity, and the role of the school in obesity prevention.
Results: Results revealed that these community stakeholders were concerned about the problem of child obesity and supported the idea of their school doing more to improve the diet and physical activity of its students. Specifically, all groups thought that foods and drinks consumed by students at school should be healthier and that they should have more opportunities for physical activity. However, they cited limitations of the school environment, academic pressures, and lack of parental support as potential barriers to making such changes. Parents were most concerned that their children were not getting enough to eat and they and the teachers were not in favor of BMI screening at the school. Parents were in favor of increasing physical activity during school and thought that parent volunteers should help students select foods in the cafeteria. Students cited examples of how diet and physical activity affect their health and school performance, and thought that they should have more physical education time and recess.
Conclusions: The data collected in the current study contributed to the limited knowledge base regarding rural populations as well as identified strengths and potential barriers to assist with the development of a pilot program based on the CSH model, Winning with Wellness.
Key words: pediatric obesity, prevention, rural, school, USA.
You might also be interested in:
2009 - The mortality gap between urban and rural Canadians: a gendered analysis

