Introduction
Globally, chronic conditions have become the most prevalent and costly of health problems, imposing a growing drain on healthcare delivery systems and healthcare financing1,2. Chronic conditions also deplete the physical and emotional resources of the affected individuals. Depressive symptoms and disorders are one of the most common complications of chronic illness. In fact, depression is increasingly being viewed as a chronic illness in its own right3 because depressed individuals experience high rates of symptom recurrence4 and sustained functional impairment5. Depression can intensify pain, fatigue, self-doubt and lead to self-isolation6,7.
Depression in rural women who are chronically ill
As a mood disorder characterized by chronic sadness and feelings of hopelessness8, depression has a major negative impact on one's perceived quality of life9. In recent years, depression has been recognized as a major health problem for women10. In the USA, 4.5% of all women aged 45-64 years experience serious psychological distress11; however, 5.0% of rural women (eg women living outside metropolitan and micropolitan areas as defined by the US Office of Management and Budget) experience serious psychological distress12. Contributing to this phenomenon may be the women's rural location, and their exposure to circumstances, conditions, and behaviors that may put them at greater risk for depression. These include poverty and its associated morbidity13,14, fair or poor health, physical inactivity, heavy alcohol consumption, fewer regular dental visits15 and higher incidences of chronic illness13,16,17 when compared with their urban counterparts. There are contributory stressors that are unique to the rural environment including: isolation; few social outlets; limited access to health services and healthcare providers due to distance, poor roads, and travel costs; lack of health insurance; the declining farm economy; an unpredictable, irregular income; financial and educational disadvantages; and traditional family/community caregiver responsibilities13.
Given these burdens, it is not surprising that depression is present in many of the women who seek help from rural primary care providers, particularly those women who are also chronically ill18,19. With 40% of all provider visits due to stress13, the latent depression may go undetected. In one study, only 24% of individuals with depression who were independently identified by a diagnostic inventory were diagnosed by the rural care provider20. To further compound the problem, the women typically do not disclose their depression on their visits. Instead, they tend to seek help for somatic problems such as headaches, backaches, sleep problems, and fatigue21. However, should their depression be diagnosed, obtaining specialist care for these women is often difficult because mental healthcare providers to whom they can be referred are limited17.
Positive social support has the potential for decreasing stress and depression22,23, as well as increasing self-esteem, personal empowerment, and a sense of wellbeing24. A case in point is described by this chronically ill, depressed rural woman ('Women to Women' study participant, online message, 2009. Unpubl. data of Clarann Weinert):
My depression has taken over again and I find myself under my quilt with my dog on my lap letting the world go away. Seems like all the news I get is bad and I can't do anything right. But had a couple of good conversations with a couple of special friends and am now working on climbing out of my hole. Have done some checking and I may be able to get some therapy long distance. Ahh, the rural life .
Combating depression in rural women with chronic conditions
In an effort to help rural women better self-manage their chronic illnesses, more successfully adapt to life's challenges, and improve the quality of their lives, the Women to Women Project (WTW) has been providing online social support and health education to isolated women in western USA for almost 15 years. The overarching conceptual framework for this research-based intervention was adaptation to chronic illness. Since psychosocial indicators have been found to be better predictors of adaptation than disease activity25, those selected and expected to be positively impacted by WTW were social support, self-esteem, empowerment, self-efficacy, depression, stress, and loneliness. Improvements were noted in all of these psychosocial indicators for the WTW intervention group and mean scores declined or remained stable among the controls26. It is important that depression in rural chronically ill women be better understood and recognized because depression can influence quality of life, levels of physical activity, skills of illness self-management, and ability to communicate productively with their healthcare providers27.
Purpose
The purpose of this article is to describe the experience of depression in a sample of chronically ill rural women who participated in an online social-support and health education research project. The descriptions are a result of an analysis of virtual forum conversations among the women in the online support intervention of the WTW project.
Methods
Criteria for participation
Women with chronic conditions (N= 233) were recruited from Montana, Idaho, North Dakota, South Dakota, and Wyoming through newspaper advertisements, the state agricultural extension offices, and assistance from health professionals and voluntary agencies28. Participants were required to have at least one chronic condition, be aged 35-65 years, and live on a farm, ranch, or in a community at least 40 km (25 miles) from a town of 12 500 or greater population. The study was approved by the Institutional Review Board at Montana State University.
Design
A detailed description of the WTW project methodology is provided elsewhere29-32, thus only an overview is presented here. The WTW consisted of a 22 week computer-based intervention in which consenting participants were randomized into three groups. The first group (n= 82) was assigned to an intense intervention that provided an interactive computer experience characterized by online health teaching units with internet access, expert-facilitated discussions and a virtual support group. These online activities were delivered by the Montana State University WebCT platform and were accessible to the women at any time of the day or night. The second group (n= 82) participated in a less intense intervention that consisted of online independent study health teaching units without access to expert input or discussion forums. The sole responsibility of the third (control) group (n= 69) was to complete the repeated measures questionnaires
Data generation and analysis
Data were collected from four cohorts of women between 2002 and 2005. The quantitative data were generated from paper/pencil repeated measures. Qualitative data were extracted from the online interactions of the women who participated in the computer interventions.
Quantitative data: Depressive symptomatology was measured by the Center for Epidemiologic Studies Depression Scale (CES-D). The CES-D is a 20 item, self-report measure of the individual's depressive symptoms experienced in the week preceding completion of the tool. Potential scores range from 0 to 6033 and reported reliability coefficients range from 0.84-0.90. A score equal to or greater than 16 is indicative of a clinically significant level of psychological distress. The quantitative data, CES-D scores and demographic information were analyzed using the Statistical Package for the Social Sciences v18 (SPSS Inc; Chicago, IL, USA). The depression data reported here were collected at the start of the study and the end of the computer intervention. Other psychosocial data collected via the repeated measure questionnaires were published elsewhere and will not be repeated here26,34.
Qualitative data: Identifying information was deleted from the online exchanges, and the de-identified messages were stored verbatim in the end-user database. They were then downloaded, into QSR NUD*IST (www.qrsinternational.com), a computer package designed to aid users in handling non-numerical and unstructured data in qualitative analysis.
A general, eclectic qualitative approach was used in the analysis of the online messages that involved blending deductive, inductive, and integrative analytical processes. In the deductive phase, messages were coded and sorted into categories according to the aims of the study, that is, depressive symptomatology. In the inductive phase, the messages were examined for themes, patterns, or recurring regularities that emerged. The strategy used for verification consisted of a second research team member recoding 10% of the coded segments. Discrepancies between analysts were examined and the codes/themes revised to reflect a mutually agreed upon definitions, a strategy used successfully in other qualitative studies32. In the final integrative phase of analysis, relationships were identified between and among themes.
For this report, exchanges among the women who participated in the supportive intervention were carefully examined for evidence of depressive symptomatology - feelings of sadness, loss of interest or pleasure, disturbed sleep or appetite, and low-self worth leading to the weakening of confidence and a loss of energy and poor concentration that deterred action - and coded 'depression'. Further, the women's perceptions of the relationship of depression to their chronic illnesses, and their strategies for coping with their depression were identified in order to better understand the experience of depression.
Results
Sample
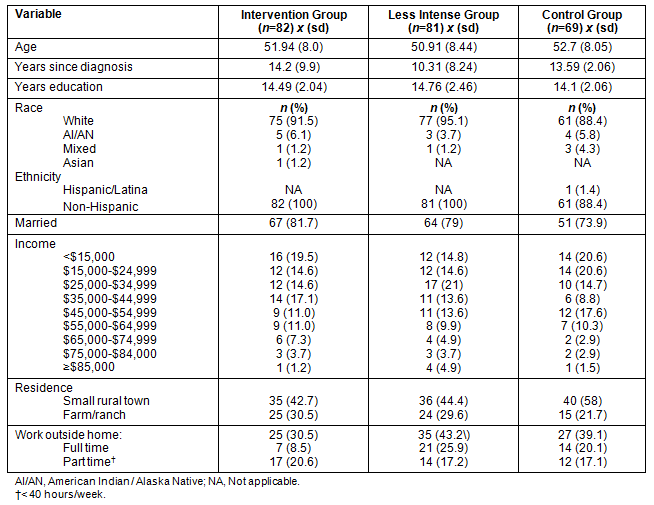
Eighty-two women participated in the supportive computer intervention. Their ages ranged from 36 to 65 years with a mean of 51.94 (sd=7.55). Of these women, 75 (91.5%) were Caucasian, 5 were American Indian, one was Asian, and one was of mixed race. The majority of women was married (81.7 %), most (42.7%) lived in a small rural town, while almost one-third (30.5%) lived on a farm or ranch. All of the women had at least a high school education (x=14 years; sd=2; range 12-19.5 years). The greatest number of women reported income of less than US$15,000 (n=16; 19.5%) with the next greatest number indicating incomes in the $35,000-$44,999 range (n=14; 17.1%). Twenty-five (30.5%) were working outside of the home on a full time (n=7; 8.5%) or part-time basis (n=17; 20.6%). The length of time since diagnosis with chronic illness ranged from 2 to 40 years (x=14.2; sd=9.99). No significant differences in demographics were found between the women in the computer intervention group and the women in the less intense computer and control groups with the exception of years since diagnosis. Women in the less intense group had a mean of 10.2 years since diagnosis compared with 14.2 and 13.6 years for the intervention and control groups respectively. The demographic information for all three groups of women is displayed (Table 1).
Table 1: Group demographics
Evidence of depression
Of the 82 women who began the intensive computer intervention, 47 (57%) demonstrated clinically significant psychological distress at the time of enrollment into the WTW project by scoring 16 or above on the CES-D (range=0-48; x=19.27; sd=11.25). Twenty-two weeks later, at the end of the computer intervention, complete data were available on 57 women. Of these remaining 57 participants, 24 (42%) scored 16 or above on the CES-D (range=0-49; x=15.74; sd=11.55) indicating continuing psychological distress. Reasons for those who did not complete the intervention were: conflicts in priorities in their time, deterioration in health status, moving away to an urban area, technical problems, or death.
Messages posted to the online forums reflected the women's daily experiences and were not influenced by any prompting from the research team. In all, 59 messages were coded 'depression'. Consistent with our purpose to gain insights into the chronically ill women's experiences of depression, we guided our attempts to discern the themes embedded in the messages by looking for those related to depressive symptomatology, perceptions of the impact of their depression on living with chronic illnesses, and strategies for coping with their depression.
Themes identified
The themes identified related to symptoms of depression8 were feelings of worthlessness and guilt as well as helplessness and hopelessness; alterations in sleep patterns; and loss of energy. Other themes and subthemes associated with depressive symptoms that emerged were the interrelationship of depression and illness and pain; traditional and complementary healthcare treatments; relationships with healthcare providers; medication use; relationships with family and friends; and Seasonal Affective Disorder. In addition, the women described a variety of strategies they used in coping with their depression.
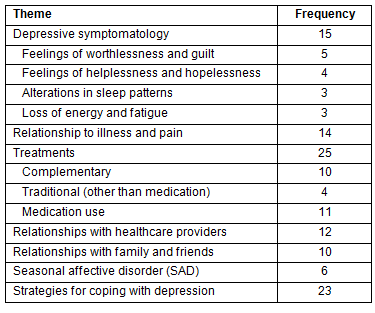
The themes related to the experience of depression are listed (Table 2). More than one theme was often expressed in a single message. The distribution of messages among the women was: 16 women posted 1 message, 12 women posted 2-3 messages, and one woman posted 17 times. Descriptions of depressive symptomatology were cited 15 times. The symptoms of depression expressed were feelings of worthlessness and guilt (n=5), feelings of helplessness and hopelessness (4), alterations in sleep patterns (3), and the loss of energy and fatigue (3).
The two most frequently discussed topics related to the experience of depression were the relationship of symptoms of depression to chronic illness and pain (n=14) and the healthcare treatments used (14), both complementary (10) and traditional (4). The women's relationships with healthcare providers (12) were often described as was their use of medications (11). The disruption in relationships with family and friends was also mentioned (10). Seasonal Affective Disorder was specified as a cause of depressive symptoms (6).
Table 2: Frequency of themes in 59 messages related to depression (in descending order)
Within the messages, there were 23 references to strategies the women used to deal with their depression, such as optimizing inner and spiritual resources and seeking reliable health information. Specific suggestions were: venting honestly within their group; trying to proactively conquer or at least control their disease; thinking positively and squashing negative thoughts; recognizing one's own self-worth; reprioritizing what is important in life; reducing stress and relaxing more; and rejuvenating by reading or listening to inspirational books and tapes.
Themes as described by the women
The voices of depressed chronically ill women often go unheard, as is seen in how often they go undiagnosed. Our goal was to help them be heard. It is important that the women's thoughts, feelings, and moods be presented to get as close as possible to their experience of depression35. Exemplars of the subjective perspective of each of the themes follows as expressed in the women's own words. The symptoms of depression were detected in the women's messages as feelings of worthlessness or guilt, feelings of helplessness and hopelessness, changes in sleep patterns, and loss of energy and fatigue.
Feelings of worthlessness and guilt: One woman recognized her feelings of low self-worth and recounted her struggle to overcome them:
I guess I have a lot of work ahead of me. [I am] trying to understand my own self-worth. I feel good when I can give Praise or Comfort [to others] but I can't deal with hearing it about myself (WOW). It's so hard to do.... (3-814)
Others shared similar doubts and a sense of guilt, but an underlying spirit of trying to find a way out was also reflected in their messages, for example:
Yes I get depressed, fall down, cry like anyone else but just keep going and prove to others that I can... BUT I think about why me and did I do something to get this. (2-703)
Feelings of helplessness and hopelessness: Feelings of having limited choices or a loss of control by circumstances beyond their power were reflected in these comments:
I am getting a little better at not crying so much... Maybe I am all cried out? Is that possible? Seems strange but I think even crying gets to be old and terribly exhausting especially when you are sitting in a pool wondering why you are doing it in the first place.... (3-816)
The experience of hopelessness was put into words by this woman:
There are times when you want to be a mentor to all that have the same problems that you do..., but then good old depression rears its ugly head and you want to climb into the closet and tell the world to go away.... (2-717)
Changes in sleep patterns: Sleeping excessively was the change in sleep pattern described by most women: '[I] slept one night 10 PM to 9 AM, fed me and the cats and went back to sleep, waking up at 3 PM' (2-717). However, another woman did not consider her sleep pattern problematic: ' I'm battling depression also. I sleep good at night. I take two naps during the day. They are not long naps usually 30 min to one hr'. (3-817).
Loss of energy and fatigue:The relationship between depression and energy level was cited by the women and described in this way: 'I've found that when I get so tired then depression crawls in and I have two enemies to fight' (4-716). Another wrote '...I too get weepy and depressed when my energy is low' (2-716).
Relationship of depression with illness and pain: The belief that symptoms of depression frequently accompany their chronic illness and pain were common topics of their exchanges. One woman wrote:
I'm struggling with depression lately... It's hard enough being diagnosed with a disease, but then living with it every day is really hard on the spirit. (3-812)
Another shared:
I feel that Depression is a Big Factor in My Disease. I at times have a hard time to break them a part. Because if we hurt all the time as we do Depression sets in and because of the Depression, it goes back to the pain....I don't know if that is right or not or even if it makes sense?' (3-814)
In response to this inquiry, the woman received the following response:
...somebody asked the chicken-and-egg question about pain and depression. It's a circle. If I am stressed or depressed, the physical pain I feel is hugely magnified, and the more pain I am feeling, the unhappier and the more stressed I am. ...I have a theory about depression and pain - they are the same thing... (3-808)
Treatments utilized: The methods of treatments described and suggested were both traditional and complementary. A traditional approach for dealing with pain was described as:
...I have to go to my regular Dr. tomorrow to talk with her about my meds and the support group, and also talk with [counselor] who I am seeing about my Depression, she has been keeping me busy and doing an intake that I have to rate from 1 to 10, and also draw a picture of my pain and a face of how I look in pain... (3-814)
Another traditional approach that was discussed included the advantages and disadvantages of medication for treating depression. Some experienced successes and others had untoward responses. One woman was optimistic, 'There is so much now days to help us all out...' (3-814), while another echoed her opinion by saying, '...with so many drug choices out there, no one should have to suffer depression' (2-708). An untoward response was reported by a woman who said:
I took Zoloft for awhile and then several others but had some [bad] side effects... I'm not on anything now, but seriously considering trying something else. They all scare me though. (2-701)
The option of complementary therapies was introduced by several of the participants. One woman opined: 'I think the treatment we have gotten at the hands of the western medical world is what has led us to the nontraditional forms of healing...' (3-815). Another experienced positive results from combining traditional and complementary therapies:
I do take herbs, quite a few actually, am on an anti-depressant, try to do yoga and positive thinking...I am doing better at not crying so much and have actually been feeling better. (3-816)
Relationships with healthcare providers: The attitude of healthcare providers had profound impact, both positive and negative, upon the women's ability to deal with their depression. Two positive comments were:
I have to laugh when I remember one of the doctors telling me if he had diabetes, he would be depressed!! I appreciated his sharing that with me and helping with the depression. (2-708).
Just wanted to let you know how things went with the lady I see for depression; she is a wonderful, caring person, and it was a good meeting and she made me feel great, and she understands and listens to my issues... (3-814)
However this same woman described a less than desirable interaction with another of her care providers: '...then I had to go and see the so-called pain doctor. He made me feel like a person who was crazy and all the pain was in my head' (3-814). Strong advice for interacting with non-sensitive care providers was given by this woman: 'Don't give up. Just keep screaming until a Dr. listens!' (3-801).
Relationships with others: The stress of living with a chronic condition can carry over into women's relationships with family and friends. One woman put it this way:
I don't live alone - I have a husband and a grandson, but sometimes I feel like I'm all alone with my illnesses... The way some people relate to you and your illness isn't any help to your mind. I have more than one chronic illness and I have ups and downs you won't believe (2-720).
She added:
I get very frustrated with my illness and I know at times I make everyone round me miserable, but if people would learn to leave me alone to deal with things my way I do a lot better....(2-720)
Another woman offered a way to 'smooth the ruffled feathers' that can occur in a relationship stressed by chronic illness:
I lash out at my family and then apologize. I think the main step with any chronic illness is, instead of getting angry, to tell your loved ones that you are frustrated and mad at your life! (4-916)
Seasonal affective disorder: The shorter days and longer nights of autumn and winter were associated with a change in mood for some of the women. One asked:
Does anyone else have Seasonal Affective Disorder [SAD]? It is a depression from not getting enough light, and for me it starts the weekend that Daylight Savings Time ends... (3-808)
One woman responded:
I was just thinking something along the same line about depression. Maybe it's seasonal, or biorhythm, or weather, or something like that. I've been thinking about getting a full spectrum lamp for my reading chair. Depression seems to come and go with me as well, though I haven't journaled it. (3-805)
The need for brightness and sunshine was a common theme as can be seen in these remarks:
I bought a small pot of crocus (not blooming yet) to brighten the house... Mr. Depression does seem to smack [me] this time of year....NEED SUNSHINE. (3-801)
...have several problems to deal with and one is depression and it is going to get worse when the skies stay dark for so many days in a row. I need sunshine to be happy.... (2-717)
And lastly, ' I will be so glad when the sun shines again - I don't do as well when it's dismal outside. Snow is okay, but just give me sun!' (1-608).
Strategies for dealing with depression: Positive thinking was illustrated by a woman who said, ' Please hang in with us we all have good and bad days, try thinking about what you enjoy in your life...'. (3-814).
Taking proactive control of one's health was advocated by the woman who advised:
I am all about talking to your doctor and getting the proper medication that will not cure by certainly HELP the symptoms. (3-800)
Another proactive approach to seeking solutions was suggested in this message:
Ladies, there is a wonderful book I got from the lady who I see for depression it is called Managing PAIN Before it Manages You...it goes into great detail on our pain, depression, treatment for pain, doing a pain sheet every day, what we are stressed out about what we feel and how we deal with it, and ways to meet our GOALS.... My main goal is to take ownership for the pain, I can't wait for Dr's and family members to do it for me... (3-814)
Spirituality played a large part in helping some of the women adapt more successfully as was expressed by this woman:
[I] went to church... I am so glad I went today. I felt much better afterwards and realized that when I am depressed it helps me to be around other people... it felt comfortable sitting in the middle of my best friend and her daughter... so this morning I was in the right place. He works in mysterious ways.... (2-206)
Another wrote, 'God is good all the time. Even when my moods are not always so good'. (1-613).
Discussion
The purpose of this paper was to describe the experience of depression in a sample of chronically ill rural women who participated in an online social-support and health education research project. The women shared their symptoms of depression: the interrelationship of depression and chronic illness, pain and seasonal variations; relationships with healthcare providers, families and friends; and strategies used in coping with their depression.
Within this group, depressive symptomatology, as measured by the CES-D, was present in more than half of the participants at the start of the project and persisted in nearly half of the women at the conclusion of the computer-based intervention, consistent with reports of the increased prevalence of depression in rural dwellers and those with chronic illness13,16,17. Likewise, their symptoms were consistent with those described in the literature8. In their conversations in an online asynchronous forum, they shared the real meaning of the symptomatology of depression - some of which has been reported here. Much can be learned from these insightful expressions of the reality of living with depression.
Implications
How can rural healthcare providers become more alert to the possibility that depression may be a factor in their rural women clients? The first step is recognizing that depression is a common accompaniment to chronic illness. Drawing from the words of the women themselves, a primary care provider should be alert to expressions such as those seen in (Fig1). Hearing similar phrases when in conversation with chronically ill women should prompt primary care providers to initiate a discussion of depression with their patients. The use of screening tools such as the CES-D (http://www.hepfi.org/nnac/pdf/sample_cesd.pdf) or Beck's Depression Inventory (http://www.ibogaine.desk.nl/graphics/3639b1c_23.pdf) to determine whether depression diagnosis and treatment are appropriate should be explored.

Figure 1: Expressions of depression in women with CES-D Scores ranging from 14 to 48 (borderline to severe depressive symptomatology).
If depressive symptomatology is identified by a screening tool, what options are available to rural dwellers? While there are barriers associated with getting treatment for depression in rural areas, the likelihood of rural persons receiving care for depression may be better than for other mental health problems36. Because there are few mental health specialists to whom they can refer patients, rural primary care practitioners may treat more cases of depression on their own than their urban counterparts37. Outcomes for treatment for depression by rural primary care providers (physicians, physician assistants, and advance practice nurses) can be improved by better basic preparation of rural healthcare providers and through outreach educational programs associated with area health education centers, volunteer agencies, and professional organizations. If, through such interventions, the primary care providers' knowledge and confidence in treating depression is improved, then the lack of mental health specialty providers in rural areas need not mean a lack of access to treatment for depression.
While rural primary care providers can and do treat women with depression, many rural and remote areas have no practitioners or a very limited number of healthcare providers serving vast and sparsely populated areas. Decreased access to healthcare services supports the need for self-care skills, including monitoring for depressive symptoms. Rural individuals living with chronic illness should be especially alert for signs of psychological distress. Making education materials available to those at risk for depression, suspected of being depressed or diagnosed with depression and experiencing symptoms of distress is an important step in illness self-management. Primary care providers should routinely instruct these individuals to monitor for symptoms of psychological distress, changes in existing symptomatology, and the circumstances under which to contact their healthcare provider. Voluntary healthcare organizations, healthcare providers serving rural residents and education-focused groups can provide education materials to persons living in medically-underserved areas in a variety of ways including online websites, community events, and through educational extension offices serving rural communities. In addition to education, alerting women patients to online programs similar to the WTW project that provide a venue for chronically ill patients to share experiences and give and receive support to one another should be considered by rural practitioners.
In addition to client education, discussion and support of coping strategies that work to ameliorate depressive symptomatology should be integrated into the plan of care for affected persons and those at risk for depression. Drawing upon the suggestions from the women in this study, such strategies include positive thinking, reading motivational literature, spending time in the sun, developing and maintaining positive relationships, focusing on spiritual beliefs, and talking with supportive others. Because of the synergistic relationship between pain and depression, working with individuals to keep pain under control should be a priority. Finding treatments for depression that work for a particular person can be a trial and error experience. Support for the women during this potentially stressful time is important while the appropriate treatment, whether it is allopathic or complementary, is found and adjusted for the woman's particular symptoms.
Empowerment, the ability of people to gain understanding and control over forces in their lives, is an accepted strategy for health promotion38 while lack of control, enhances the risk for illness. The descriptions of depression from the women in this study indicated a desire for increased understanding and control of their symptoms, treatments, and strategies used to prevent depression. Assisting the women to strengthen these self-care skills is not only appropriate but essential for healthcare providers working in rural and remote settings.
Timely treatment of depression in rural women is complicated by their reluctance to disclose their depressive symptomatology and the paucity of mental healthcare providers practicing in rural areas17. The responsibility to recognize and treat the growing problem of depression in rural persons falls to physicians, physician assistants, and advance practice nurses providing primary care in rural and remote settings, and to the rural persons themselves.
Limitations and recommendations
The description of depression in this article is limited since the sample of participants was composed of middle-aged Caucasian women from the western USA. Additional research is needed to understand the experience of depression in underserved rural women with chronic illness and in women of differing cultural backgrounds, age groups, and locales. The knowledge generated from these explorations will increase the potential for providing acceptable and appropriate health care to rural women at risk for depression as well as women in other circumstances.
Conclusion
The findings add to the knowledge base of illness management by chronically ill women in a rural environment. Additional research is needed with women of differing rural locales, ages and cultural backgrounds. The knowledge generated will increase the potential for providing acceptable and appropriate health care to rural women at risk for depression. The data also provide significant information for healthcare providers. It can enhance their sensitivity to rural clients' needs and the everyday challenges of living with depression in the context of the rural environment.
Acknowledgements
The authors thank Dr Clarann Weinert and the WTW research team for their assistance with the development of this manuscript and the following organizations for their financial support of the WTW Project: NIH/National Institute of Nursing Research (1R01NR007908-01), Sigma Theta Tau International/Zeta Upsilon Chapter Research Award, SC Ministry Foundation, and National Arthritis Foundation.
References
1. Center for Disease Control and Prevention. Chronic disease and health promotion. (Online) 2009. Available: http://www.cdc.gov/chronicdisease/index.htm (Accessed 17 November 2010).
2. World Health Organization. Preventing chronic diseases: a vital investment. 2005. Available: http://www.who.int/chp/chronic_disease_report/en/ (Accessed 17 November 2010).
3. Andrews G. Should depression be managed as a chronic disease? BMJ 2001; 322(7283): 419-421.
4. Lin EH, Katon WJ, VonKorff M, Russo JE, Simon GE, Bush T et al. Relapse of depression in primary care. Rate and clinical predictors. Archives of Family Medicine 1998; 7(5): 443-449.
5. Hays RD, Wells KB, Sherbourne CD, Rogers W, Spritzer K. Functioning and well-being outcomes of patients with depression compared with chronic general medical illnesses. Archives of General Psychiatry 1995; 52(1): 11-19.
6. Cleveland Clinic. Chronic iIllness and depression. (Online) 2007. Available: http://www.cchs.net/health/health-info/docs/2200/2282.asp?index=9288 (Accessed 18 August 2009).
7. National Institute of Mental Health. Depression. (Online) 2008. Available: http://www.healthyplace.com/depression/nimh/about-major-depression-dysthymia-bipolar-disorder/menu-id-1419/ (Accessed 17 November 2010).
8. World Health Organization. The world health report 2003 - shaping the future. (Online) 2003. Available: http://www.who.int/whr/2003/en/ (Accessed 17 November 2010).
9. Mullins LC, Dugan, E. The influence of depression, and family and friendship relations, on residents' loneliness in congregate housing. Gerontologist 1990; 30(3): 377-384.
10. Franks F, Faux, SA. Depression, stress, mastery, and social resources in four ethnocultural women's groups. Research in Nursing & Health 1990; 13(5): 283-292.
11. U.S. Census Bureau. The 2010 Statistical Abstract. (Online) 2010. Available: http://www.census.gov/compendia/statab/past_years.html (Accessed 23 August 2010).
12. Centers for Disease Control and Prevention. National Center for Health Statistics. Health Data Interactive. (Online) no date. Available: www.cdc.gov/nchs/hdi.htm (Accessed 20 September 2010).
13. Mulder PL, Shellenberger S, Streiegel R, Jumper-Thurman P, Danda CE, Kenkel MB et al. The behavioral health care needs of rural women. (Online) 2000. Available: http://www.apa.org/pubs/info/reports/rural-women.pdf (Accessed 17 November 2010).
14. Auchincloss AH, Hadden W. The health effects of rural-urban residence and concentrated poverty. Journal of Rural Health 2002; 18(2): 319-336.
15. National Center for Health Statistics. Health, United States, 2009: with Special Feature on Medical Technology. (Online) 2009. Available: http://www.cdc.gov/nchs/data/hus/hus09.pdf (Accessed 17 November 2010).
16. Probst JC, Laditka S, Moore C. Depression in rural populations: Prevalence, effects on life quality, and treatment-seeking behavior. (Online) 2005. Available: http://rhr.sph.sc.edu/report/SCRHRC_Depression_Rural_Exec_Sum.pdf (Accessed 17 November 2010).
17. Probst JC, Laditka SB, Moore CG, Harun N, Powell M, Baxley E. Rural-urban differences in depression prevalence: implications for family medicine. Family Medicine 2006; 38(9): 653-660.
18. Katon W, Sullivan MD. Depression and chronic medical illness. Journal of Clinical Psychiatry 1990; 51(Suppl3-11): 12-14.
19. Rouchelle A, Pounds R, Tierney J. Depression. In: M Wise, J Rundell (Eds). Textbook of consultation-liaison psychiatry. Washington, DC: American Psychiatric Publishing; 2002: 307-338.
20. Rost K, Williams C, Wherry J, Smith GR Jr. The process and outcomes of care for major depression in rural family practice settings. Journal of Rural Health 1995; 1(2): 114-121.
21. Van Hook MP. Challenges to identifying and treating women with depression in rural primary care. Social Work in Health Care 1996; 23(3): 73-92.
22. Foote AW, Piazza D, Holcombe J, Paul P, Daffin P. Hope, self-esteem and social support in persons with multiple sclerosis. Journal of Neuroscience Nursing 1990; 22(3): 155-159.
23. Gray J. Mastery of stress and health in women living with HIV infection. Dissertation Abstracts International. Section B: The Sciences and Engineering 1998; 8(8B): 138.
24. Finfgeld-Connett D. Clarification of social support. Journal of Nursing Scholarship 2005; 37(1): 4-9.
25. McFarlane AC, Brooks PM. Determinants of disability in rheumatoid arthritis. British Journal of Rheumatology 1988; 27(1): 7-14.
26. Hill W, Weinert C, Cudney S. Influence of a computer intervention on the psychological status of chronically ill rural women: preliminary results. Nursing Research 2006; 55(1): 34-42.
27. Piette JD, Richardson C, Valenstein M. Addressing the needs of patients with multiple chronic illnesses: the case of diabetes and depression. American Journal of Managed Care 2004; 10(2pt2): 152-162.
28. Cudney S, Craig C, Nichols E, Weinert C. Barriers to recruiting an adequate sample in rural nursing research. Online Journal of Rural Nursing and Health Care. (Online) 2004. Available: http://www.rno.org/journal/index.php/online-journal/article/viewFile/140/138 (Accessed 17 November 2010).
29. Cudney S, Winters C, Weinert C, Anderson K. Social support in cyberspace: lessons learned. Rehabilitation Nursing 2005; 30(1): 25-28; discussion 29.
30. Weinert C. Social support in cyberspace for women with chronic illness. Rehabilitation Nursing 2000; 25(4): 129-135.
31. Weinert C, Hill W. Rural women with chronic illness: computer use and skill acquisition. Women's Health Issues 2005; 5: 230-236.
32. Winters CA, Cudney S, Sullivan T, Thuesen A. The rural context and women's self-management of chronic health conditions. Chronic Illness 2006; 2(4): 273-289.
33. Radlof LS. The CES-D scale: a self-report depression scale for research in the general population. Applied Psychological Measurement 1977; 1: 385-401.
34. Weinert C, Cudney S, Hill W. Retention in a computer-based outreach intervention for chronically ill rural women. Applied Nursing Research 2008; 21(1): 23-29.
35. Sandelowski M. The use of quotes in qualitative research. Research in Nursing & Health 1994; 17(6): 479-482.
36. Lambert D, Agger M, Hartley D. Service use of rural and urban Medicaid beneficiaries with depression. AHSR FHSR Annual Meeting Abstract Book 1996; 13: 31-32.
37. Hartley D, Korsen N, Bird D, Agger M. Management of patients with depression by rural primary care practitioners. Archives of Family Medicine 1998; 7(2): 139-145.
38. Wallerstein N. Empowerment to reduce health disparities. Scandanavian Journal of Public Health Suppl. 2002; 59: 72-77.


