The Northeastern Ontario Postgraduate Specialty (NOPS) program, initially offered by the Northeast Ontario Medical Education Corporation and now offered by the Northern Ontario School of Medicine (NOSM), provides 2-24 week rotations in northeastern Ontario in anesthesiology, internal medicine, psychiatry, surgery, and other specialties to residents with a view to encouraging eventual practice in northern cities or smaller sized cities.
Although the positive association between exposure to rural and remote practice during postgraduate training and eventual practice in rural areas has been well documented in the literature on family physicians/general practitioners1-11 few, if any, studies have examined this association for other specialties. Publications that deal with these specialties either advocate implementation of rural specialty training programs, recommend improvements or describe existing programs12-18 . These publications do not provide evidence linking rural or northern training and eventual practice location. This study addressed this gap in the literature and explored the association between practice location and northern education for specialties other than family medicine/general practice.
The NOSM administrative records provided the number, location and duration of residents' rotations in northeast Ontario from program inception in 2000 to 2006. Scott's Medical Database (SMDB) held by the Canadian Institute for Health Information (CIHI) provided the practice location at 31 December 2006 for 50 NOPS participants and matched specialists (described below). The SMDB practice location was checked against that of the College of Physicians and Surgeons of Ontario (CPSO) online directory (http://www.cpso.on.ca/docsearch/) for NOPS participants.
A comparison group of non-NOPS participants was selected by matching one for one on sex, year of birth, language, location of medical school, year of medical school graduation, age at graduation from medical school and specialty. If no exact matches were found, then criteria were relaxed to be ± 1 year for age or graduation year and medical versus surgical specialties. The study received research ethics approval from Laurentian University and CIHI.
Chi-square tests were used to analyze demographic characteristics as well as the relationship between the duration of northeastern Ontario rotations and practice location. Adjusted standardized residuals were used to identify cells with significant deviation from expected19. Paired t-tests were used to compare age in 2006 and age at graduation for NOPS and non-NOPS participants (Wilcoxon Signed Ranks tests gave similar results). Hierarchical log-linear models and χ2 tests were used to assess differences between NOPS and non-NOPS participants in geographic location and population size of practice community. Analyses were performed with PASW v17 (formerly SPSS; Predictive Analytic Software; Chicago, IL, USA; http://www.spss.com/).
All 50 NOPS participants were matched after six iterations. Exact matches were obtained for 12 participants, with 18 additional matches using specialty group. Allowing age and year of graduation to vary ± 1 added 11 and 9 matches for specialty and specialty group, respectively.
Paired t-tests indicated that NOPS and the matched non-NOPS program groups were not significantly different for age in 2006 (M=36.2, SD=5.6 vs M=36.3, SD=5.3, t=-0.09, df=43, p=0.93) and age at graduation from medical school (both groups with means of 27.2 years). Program groups matched exactly for sex, medical school location and specialty group.
Demographics of Northeastern Ontario Postgraduate Specialty program participants
Forty-six percent of NOPS participants were female and 80% came from Ontario residency programs. Seventy-two percent of participants were enrolled in medical specialties (the remainder were in surgical specialties) and this differed significantly by gender: 83% of females vs 63% of males (χ2=4.76, df=1, p=0.03). Fifty-eight percent completed residency training at 31-35 years of age. Fifty percent of NOPS participants obtained undergraduate medical degrees from Ontario universities, 34% from other Canadian universities and 16% from other universities.
Northeastern Ontario Postgraduate Specialty program participation and outcomes
A hierarchical log-linear model was developed for NOPS participation (yes or no), practice location (Northeastern Ontario, Southern Ontario or other location) and community population size (10 000-99 999, 100 000-499 999 or ≥500 000 people). A sample size of 100 provided expected frequencies in excess of 5 and no cell was an outlier after the model was fitted20. Backwards elimination of non-significant effects resulted in a model with all first order (main) effects and two of the three two-way associations. A likelihood ratio of 5.55, df=5, p=0.35 indicated a good fit of the model. Structural zeros were used to take into account that communities of ≥200 000 people do not exist in northern Ontario. The final model shows that NOPS participation was associated with practice location, but not with community size, whereas practice location was associated with community size. The lack of a significant three-way interaction suggests that the results of χ2 tests can be used to assess significance of two-way interactions.
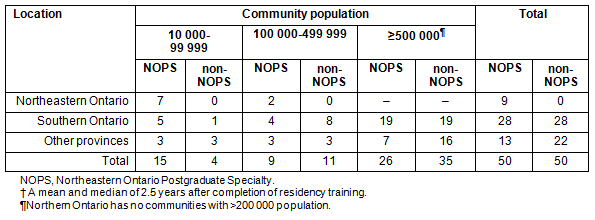
Significantly more NOPS participants than non-participants were practicing in northeastern Ontario (9 vs 0), identical numbers were practicing in southern Ontario (28 vs 28) and non-significantly fewer participants were in other provinces (13 vs 22) (χ2=11.3, df=2, p<0.01) (Table 1). Significantly more NOPS participants than non-participants were practicing in communities of 10 000-99 999 people (15 vs 4), roughly equal numbers in communities of 100 000-499 999 people (9 vs 11) and non-significantly fewer were practicing in communities of 500 000 people or more (26 vs 35) (χ2=7.90, df=2, p=0.02), though this interaction between program and community size was not significant in the hierarchical log-linear model.
There were no significant associations between specialty group (medical vs surgical) and practice location or community size or between gender and practice location (χ2 tests, p>0.34). However, proportionally more female surgeons (7/8) than males (8/20) practiced in metropolitan areas than in communities of other sizes (Fisher's Exact Test, 2-sided, p=0.04).
Excluding those participants who were out of Canada or were not registered for medical practice in 2006 left 29 NOPS participants and their matches - all of whom were assumed to be in active Canadian medical practice. Model and test results were very similar for the full or partial data sets and thus the findings seemed robust.
Table 1: Northeastern Ontario Postgraduate Specialty (NOPS) and non-NOPS participants according to location at 31 December 2006? and population size of community
Rotation details and association with outcomes
Most northeastern rotations were completed during the third (28%) or fourth (34%) residency year. Twenty percent of NOPS participants did more than one northeastern rotation. Fifty percent of the residents had a total northeastern rotation of 4 weeks or less, 30% had 6-12 weeks and 20% had 20-104 weeks. Overall, there was a mean of 15 (median=5) weeks per resident. Most participants did their rotations in the major northeastern Ontario cities of Sudbury (42%), North Bay (38%) or Sault Ste Marie (16%).
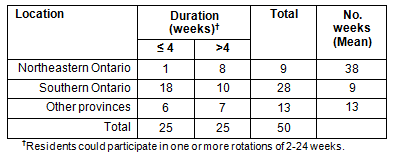
Eight of nine NOPS participants practicing in northeastern Ontario had longer rotations (>4 weeks) compared with 10 of 28 who were practicing in southern Ontario (χ2=7.81, df=2, p=0.02) (Table 2). However, a longer rotation was no guarantee of a northeastern practice location because approximately equal numbers of participants with longer rotations were spread throughout the 3 geographic locations. In contrast, a shorter rotation was strongly associated with a southern Ontario practice location (18/25). There was no association between duration and practice location in another province. The NOPS participants practicing in communities of 500 000 or more people were less likely to have longer rotations (17/26) than shorter rotations, but this difference was only marginally significant (χ2=5.13, df=2, p=0.08) and differences were less pronounced for communities of 10 000-99 999 or 100 000-499 999 people.
Table 2: Duration of Northeastern Ontario Postgraduate Specialty rotations and practice location at 31 December 2006
Discussion
This study provided evidence of a positive association between postgraduate specialty training in northeastern Ontario and eventual practice in northeastern Ontario communities or smaller communities (population <100 000). The study also found a strong association between longer duration of postgraduate specialty training in the northeast and northeastern practice and, to a lesser extent, between longer duration and practice in smaller communities.
The study could not rule out the influence of other factors. For instance, the study did not account for possible exposure to northern and rural medical practice through participation in other programs. The study also did not account for other factors that might be associated with northern practice (eg northern or rural background)8. For some specialists, NOPS participation might be a consequence of their earlier decision to practice in the north, while for others participation may have encouraged them to practice in the north.
There are some limitations associated with SMDB data. For instance, location in the SMDB is based on physician's mailing address (home, hospital or office) and may not reflect actual practice location. However, results are likely robust given that only 6% were home addresses. Excluding specialists who were located out of Canada or were not registered with the regulatory college did not substantially change the main findings, though sometimes statistical significance was reduced due to lower sample size.
The inability to match 54% of NOPS participants exactly on specialty is a limitation because some specialties may require a bigger population base to ensure a viable practice and this would preclude practice in smaller cities and possibly in the north altogether. While this may temper our NOPS versus non-NOPS comparisons, it does not affect our findings of a positive association between NOPS rotation duration and practice location.
Our study found a strong positive association between participation in the NOPS program and a northeastern Ontario practice location. It is not clear whether longer northern rotations encourage northern practice or whether this reflects an existing disposition towards northern practice. It is clear, however, that those specialists who had the longest northeastern rotations were more likely to set up practice in the northeast and, to some extent, in smaller cities.
Acknowledgements
The authors thank Dr Maureen Topps, Associate Dean of Postgraduate Education and Dr Henry Leung, former Program Director for Specialty Residency Training, Northern Ontario School of Medicine, for their support and advice and for funding in support of this study. They also thank Jeannette Salmi, Administrative Manager, NOSM Community Development Unit for compiling the administrative data and John David Stanway, Senior Analyst, Canadian Institute for Health Information, for matching cases and extracting data.
References
1. Seifer SD, Vranizan K, Grumbach K. Graduate medical education and physician practice location. Journal of American Medical Association 1995; 274: 685-691.
2. Watanabe M, Flick GH. Influence of undergraduate and postgraduate education on recruitment and retention of physicians in rural Alberta. Clinical and Investigative Medicine 1995; 18(3): 217-228.
3. Whiteside C, Mathias R. Training for rural practice: are graduates of a UBC program well prepared? Canadian Family Physician 1996; 42: 1113-1121.
4. Pathman DE, Steiner BD, Jones BD, Konrad TR. Preparing and retaining rural physicians through medical education. Academic Medicine 1999; 74(7): 810-820.
5. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of literature. Academic Medicine 2002; 77(8): 790-798.
6. Hutten-Czapski P, Thurber AD. Who makes Canada's rural doctors? Canadian Journal of Rural Medicine 2002; 7(2): 95-100.
7. McCready W, Jamieson J, Tran M, Berry S. The first 25 years of the Northwestern Ontario Medical Programme. Canadian Journal of Rural Medicine 2004; 9(2): 94-100.
8. Rourke JTB. Relationship between practice location of Ontario family physicians and their rural background or amount of rural medical education experience. Canadian Journal of Rural Medicine 2005; 10(4): 231-239.
9. Heng D, Pong RW, Chan BTB, Degani N, Crichton T, Goertzen J et al. Graduates of northern Ontario family medicine residency programs practise where they train. Canadian Journal of Rural Medicine 2007; 12(3): 146-152.
10. Thistlethwaite JE, Shaw T, Kidd M, Leeder S, Burke C, Corcoran K. Attracting health professionals into primary care: strategies for recruitment. Australian Primary Health Care Research Institute (APHCRI) research report, 07/11. Canberra, ACT: APHCRI. Available: http://www.anu.edu.au/aphcri/Domain/Workforce/Thistlethwaite_25_FINAL.pdf (Accessed 3 February 2009).
11. Mathews M, Rourke JTB, Park, A. The contribution of Memorial University's medical school to rural physician supply. Canadian Journal of Rural Medicine 2008; 13(1): 15-21.
12. Worley PS, Strasser RP, Prideaux DJ. Can medical students learn specialist disciplines based in rural practice: lessons from students' self reported experience and competence. Rural and Remote Health 4: 338. (Online) 2004. Available: www.rrh.org.au (Accessed 3 February 2009).
13. Tesson G, Curran V, Pong R, Strasser R. Advances in rural medical education in three countries: Canada, the United States and Australia. Education for Health 2005; 18(3): 405-415.
14. Field Jr RJ. Beyond the scalpel. American Surgeon 1995; 61(1): 1-6.
15. Kiroff G. Training, retraining and retaining rural general surgeons. Australia and New Zealand Journal of Surgery 1999; 69(6): 413-414.
16. Birks D, Green T. Training, retraining and retaining rural general surgeons: comment. Australia and New Zealand Journal of Surgery 1999; 69(12): 885-886.
17. DeWitt DE, Migeon M, LeBlond R, Carline JD, Francis L, Irby DM. Insights from outstanding rural internal medicine residency rotations at the University of Washington. Academic Medicine 2001; 76(3): 273-281.
18. Seal RF. Crisis in rural anesthesia. Canadian Journal of Rural Medicine 2001; 6(4): 241-243.
19. Agresti A. Categorical data analysis. New York: John Wiley, 2002.
20. Tabachnick BG, Fidell LS. Using multivariate statistics. Boston, MA: Allyn and Bacon, 2001.


