Canadian researchers have examined rural and urban residence in relation to mental health services utilization and have found few differences1-5. However, the 1994/1995 National Population Health Survey (NPHS) revealed that 3% of urban residents but only 1% of rural residents reported consulting a psychologist in the previous year6. In the 2005 Canadian Community Health Survey (CCHS) rural residents were less likely than urban residents to report seeing medical specialists including psychiatrists7. This and other evidence suggests that rural residents are less likely than urban residents to receive specialized mental health care8-10. Some evidence indicates that compared with urban residents, rural residents might experience somewhat lower rates of mental disorders11,12. Thus, rural residents might have less need for specialized mental health services than urban residents. However, factors other than rural and urban residence, such as age7,10, education10, sex13,14, social roles14, chronic medical conditions5, and type of mental condition2,4,5 are known to predict service utilization, including type of services used1,5. Thus, a wide range of demographic, social and health factors must be considered together when evaluating the role of rural versus urban residence in utilization of the various types of mental health services.
Objectives
In the present study, Canadian data collected in 2002 in the CCHS on Mental Health and Well Being Cycle 1.215 were analyzed to answer three specific questions:
- Among people who have a probable anxiety or mood disorder, is rural or urban residence associated with:
- any professional mental health service utilization
- use of specialized mental health services (ie psychiatry or psychology)?
- Among people who used professional mental health services in the previous year, what demographic and health status characteristics, including rural or urban location of residence, predicted use of a particular type of professional mental health service?
Data were from the CCHS on Mental Health and Well Being Cycle 1.215,16, conducted in 2002. The sample was selected using a multi-stage stratified cluster design based on the Canadian Labour Force Survey. One person aged 15 years or older was randomly selected from sampled households. Younger people (15-24 years) and older adults (≥65 years) were over-sampled to ensure adequate sample sizes. Most interviews were conducted in person (86%), with the remainder conducted by telephone. Further methodological details are available elsewhere16. Data analyses were conducted using SPSS (www.spss.com) at a Statistics Canada Research Data Centre. This study was approved by the University of Northern British Columbia Research Ethics Board.
Survey questions designed to detect the presence of specific symptoms were used to identify participants who were likely to have met diagnostic criteria for an anxiety or mood disorder17. This method permits estimates of the number of people who have a probable anxiety or mood disorder independent of access to professional diagnostic services, which may be lacking in some communities. The presence of some mental disorders of interest, such as schizophrenia and dementia, cannot be captured accurately using self-report methods, whereas other disorders of interest, such as eating disorders, were assessed via self-report in the CCHS Cycle 1.2 but were not considered in this study due to their low prevalence17,18.
Dichotomous outcome variables reflecting participants' use of each of four types of professional services for mental, emotional, and/or alcohol or drug problems were derived from responses to questions about mental health service use. The outcome variables reflect whether, in the year prior to the survey, the person had a session of counselling or therapy of 15 min or longer with a professional, either in person or by telephone. The categories of mental health professions examined were: (i) family doctor or GP; (ii) nurse, social worker, counsellor or psychotherapist; (iii) psychiatrist; and (iv) psychologist18. Nurses, social workers, counsellors, or psychotherapists were grouped together because their mental health services (ie counselling) are similar. They are referred to as 'counsellors' throughout the remainder of this article. Psychiatrists and psychologists were defined as specialists whereas GPs and counsellors were defined as non-specialists. A set of 17 predictor variables was selected for inclusion in regression analyses (Table 1). All 17 variables were significant predictors of mental health service use when considered individually.
Table 1: Predictor variables17-20
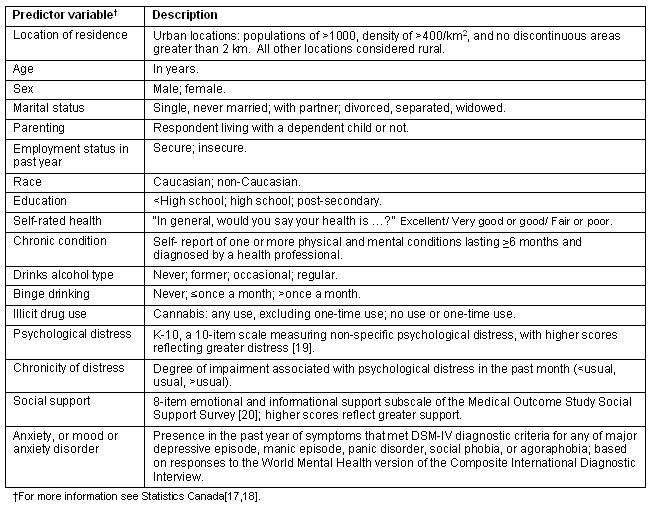
Cross-tabulated counts and 99% confidence intervals (CI) based on bootstrapped variance estimates were used to examine associations between presence/absence of an anxiety or mood disorder, rural/urban residence, and any service utilization, or use of specialist services, in the previous year. Multivariate logistic regressions were used to evaluate associations between use of professional services and the predictor variables. Four regression analyses were conducted, one for each of four types of professional (family doctor/GP, counsellor, psychiatrist, psychologist). Using the Bonferroni correction, α was set at p <0.01 (4 tests, α of .05/4 = .0125). Adjusted odds ratios (OR) with 99% CI based on bootstrapped variance estimates guided interpretation. The findings can be generalized to the population of Canadians aged 15 years or older living in private dwellings in the 10 provinces. The sample excluded people living in institutions, on Aboriginal reserves, and in some remote regions. The findings should be generalized only to urban and rural (but not remote) community-dwelling Canadians.
From among the total sample (n = 35140), 7.9% had sought professional mental health services in the past year. Among the people who sought help from professionals, the weighted percentage that had seen each type of professional was: family doctor/GP 66.4%; counsellor 30.7%; psychiatrist 24.2%; psychologist 24.7% (the values sum to >100% because participants may have seen multiple professional types in the past year).
Survey questions about anxiety and mood symptoms revealed that 8.3% of the overall sample were likely to have met the diagnostic criteria for one or more anxiety or mood disorder. Among rural residents with probable anxiety or mood disorders, 38.3% (99% CI: 29.8-46.9%) sought help from a professional in the past year. Urban residents with probable anxiety or mood disorders consulted professionals at a similar rate of 42.5% (99% CI: 38.8-46.2%). Among rural residents who had probable anxiety or mood disorders, 16.1% (99% CI: 9.9-22.3%) consulted mental health specialists (psychiatrists or psychologists). Urban residents with probable anxiety or mood disorders consulted specialists at a similar rate of 22.2% (99% CI: 19.4-25.0%). These analyses indicate that rural and urban people with probable anxiety or mood disorders were equally likely to use mental health services, whether these were specialized or not.
Multivariate logistic regression analyses focused on those people who used mental health services in the previous year. These analyses identified factors that significantly predict use of particular types of professional services, given any use. Rural versus urban residence was not a significant predictor for any type of professional mental health services when other demographic, social, and health status characteristics were taken into account (Table 2). People were more likely to see a family doctor/GP regarding mental, emotional, or alcohol/drug problems if they were older or had a probable anxiety or mood disorder in the previous year. People were more likely to see a counsellor if they were not Caucasian or had experienced an usual amount of chronicity of distress (compared with less than usual) in the previous month. Younger people were less likely to see a counsellor. People were more likely to see a psychiatrist if they had completed high school (compared with not completed). People were less likely to see a psychiatrist if they were younger, were not Caucasian, or used illicit drugs. People were more likely to see a psychologist if they had completed high school (compared with not completed), had a chronic health condition, had greater psychological distress, or had a probable anxiety or mood disorder in the previous year. People were less likely to see a psychologist if they were female or if they had usual (compared with less than usual) chronicity of distress in the previous month.
Table 2: Factors predicting whether people did or did not talk to a given type of professional
about mental, emotional, or drug and alcohol problems in the past year
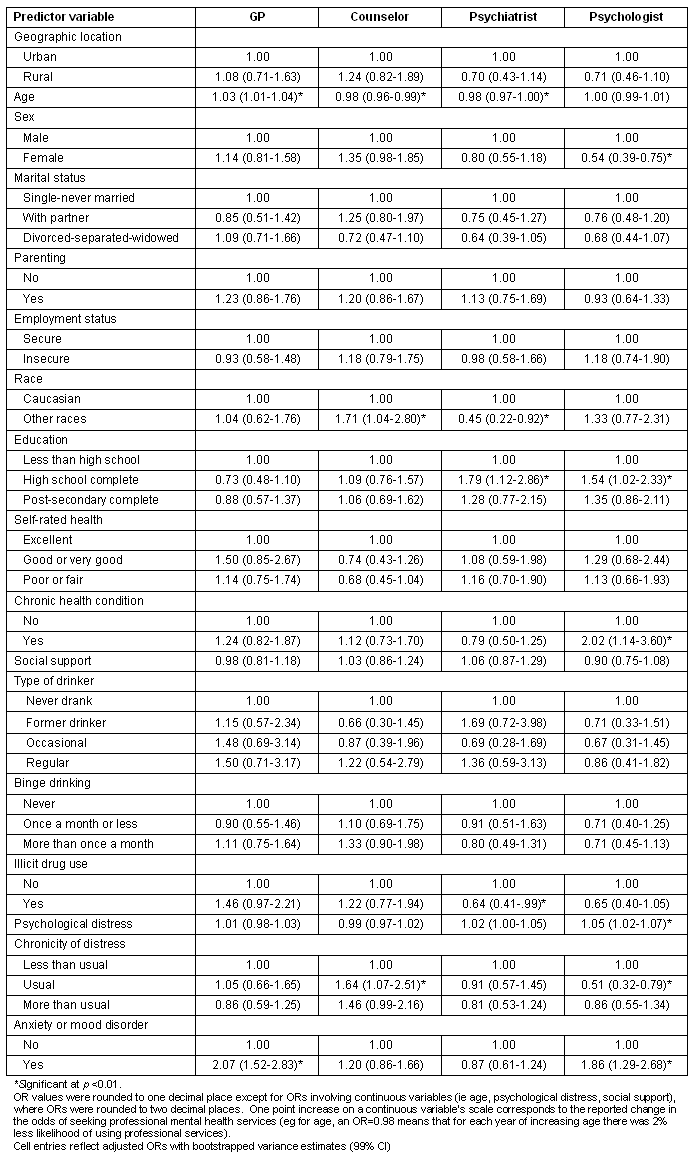
The objective of this population-based study was to evaluate the role of rural residence in relation to utilization of different types of professional mental health services. Place of residence was considered along with other demographic, social, and health status factors that predict use of professional services. When considering people with probable anxiety or mood disorders, rural residence was not an important factor in predicting any service use or use of specialized mental health services. Use of particular types of services varied as a function of age, sex, race, level of education, degree of psychological distress, chronicity of distress, and the presence of probable anxiety or mood disorders. These findings imply that if rural residents have a probable anxiety or mood disorder, they receive professional and specialized mental health care at similar rates to urban residents. The findings indicate that the mental health system in Canada must continue to provide a variety of professional services in order to meet the preferences of diverse groups. In view of these diverse preferences, mental health specialists must find and use strategies to provide appropriate supports to non-specialists who provide care to people with mental disorders21. Involvement of specialists in assessment of complex conditions, treatment planning, and when individuals do not respond to standard care, would reduce demands on specialized services while maximizing benefits.
Limitations
This study has limitations that affect generalization and interpretation of the results. The rural residents represented in this analysis did not live in Aboriginal reserve communities, remote communities, or Canada's northern territories, and the findings cannot be generalized to these communities, which are likely to have more restricted access to mental health professionals. The numbers of rural residents seeking professional help were relatively small, resulting in large confidence intervals. Some of the predictor variables were likely to be correlated with location of residence, but interactions among location of residence and other predictors could not be evaluated due to the relatively small number of rural residents who sought professional care. Residence location was measured at the time the survey was completed and might have changed in the previous year. The professionals identified as non-specialists are likely to have a wide variety of training and experience in mental health service provision, whereas the specialists might or might not have experience in treating anxiety and mood disorders. Finally, the quality and effectiveness of mental health services were not examined, and if examined, they might reveal important differences between rural and urban Canada.
Future research should focus on identifying elements required for treatment success for particular disorders and whether those elements vary across communities of different sizes. Small scale studies of service models specifically designed for rural communities would further our understanding of how to serve rural residents more effectively.
Acknowledgements
This research was funded and supported by the British Columbia Rural and Remote Health Research Institute. The research and analysis are based on data from Statistics Canada and the opinions expressed do not represent the views of Statistics Canada.
References
1. Patten SB, Beck CA. Major depression and mental health care utilization in Canada: 1994 to 2000. Canadian Journal of Psychiatry 2004; 49: 303-309.
2. Rhodes AE, Bethell J. Suicidal ideators without major depression - Whom are we not reaching? Canadian Journal of Psychiatry 2008; 53: 125-130.
3. Steele L, Dewa C, Lee K. Socioeconomic status and self-reported barriers to mental health service use. Canadian Journal of Psychiatry 2007; 52: 201-206.
4. Vasiliadis HM, Lesage A, Adair C, Boyer R. Service use for mental health reasons: cross-provincial differences in rates, determinants, and equity of access. Canadian Journal of Psychiatry 2005; 50: 614-619.
5. Wang J, Patten SB, Williams JVA, Currie S, Beck CA, Maxwell CJ et al. Help-seeking behaviours of individuals with mood disorders. Canadian Journal of Psychiatry 2005; 50: 652-659.
6. Hunsley J, Lee CM, Aubry T. Who uses psychological services in Canada? Canadian Psychology 1999; 40: 232-240.
7. Nabalamba A, Millar WJ. Going to the doctor. Health Reports 2007; 18: 23-35. Available: www.statcan.gc.ca (Accessed 12 January 2011).
8. Canadian Psychological Association. Geographic locations survey of Registered Psychologists in Canada. Ottawa, ON: CPA, 1999; 9. Available: http://www.cpa.ca/docs/file/Practice/Geographic_Locations_Survey.pdf (Accessed 16 February 2011).
9. Rost K, Zhang M, Fortney J, Fortney J, Smith J, Richard G Jr. (1998). Rural-urban differences in depression treatment and suicidality. Medical Care 1998; 36: 1098-1107.
10. Starkes JM, Poulin, CC, Kisely SR. Unmet need for the treatment of depression in Atlantic Canada. Canadian Journal of Psychiatry 2005; 50: 580-590.
11. Patten SB, Wang JL, Williams JVA, Currie S, Beck CA, Maxwell CJ et al. Descriptive epidemiology of major depression in Canada. Canadian Journal of Psychiatry 2006; 51: 84-90.
12. Wang JL. Rural-urban differences in the prevalence of major depression and associated impairment. Social Psychiatry and Psychiatric Epidemiology 2004; 39: 19-25.
13. Health Canada. A Report on Mental Illness in Canada. Ottawa, Ontario: Health Canada, 2002; 108. Available: http://www.phac-aspc.gc.ca/publicat/miic-mmac (Accessed 12 January 2011).
14. Drapeau A, Lesage A, Boyer, R. Is the statistical association between sex and the use of services for mental health reasons confounded or modified by social anchorage? Canadian Journal of Psychiatry 2005; 50: 599-604.
15. Gravel R, Béland Y. The Canadian Community Health Survey: mental health and well-being. Canadian Journal of Psychiatry 2005; 50: 573-579.
16. Béland Y. Canadian community health survey - Methodological overview. Health Reports 2002; 13: 9-14.
17. Statistics Canada. Canadian Community Health Survey, Cycle 1.2 mental health and well-being: Derived variable specifications. (Online) 2003. Available: http://www.statcan.gc.ca/imdb-bmdi/document/5015_D8_T9_V1-eng.pdf (Accessed 9 September 2011).
18. Statistics Canada. Canadian Community Health Survey, Cycle 1.2 mental health and well-being. (Online) 2003. Available: http://www.statcan.gc.ca/imdb-bmdi/instrument/5015_Q1_V1-eng.pdf (Accessed 9 September 2011).
19. Kessler RC, Barker PR, Colpe LJ, Epstein JF, Gfroerer JC, Hiripi E et al. Screening for serious mental illness in the general population. Archives of General Psychiatry 2003; 60: 184-189.
20. Sherbourne CD, Stewart AL. The MOS support survey. Social Sciences & Medicine 1991; 32: 705-714.
21. Brennan C, Dyck, K, Hardy, C, Mushquash, C. Rural mental health services in Canada: a model for research and practice. In: J Kulig, AM Williams (Eds). Health in Rural Canada. Vancouver: UBC Press, 2011; 239-257.


