The shortage of physicians in rural and remote regions of Canada is expected to worsen over time due to many factors, including the retirement of a large number of doctors, the feminization of the profession and a narrowing of the family physician's scope of practice1,2. Understanding the contextual, professional and personal factors that affect the choice of practice location for physicians will contribute to a better understanding of how to develop the physician workforce and delineate more successful strategies to address geographical maldistribution of physicians3.
The choice of type and location of practice is a complex process that has been subject to numerous studies, particularly in Canada, USA and Australia, countries which share issues of physician maldistribution and regional shortages4-7. Bilodeau and Leduc5 proposed that the choice of the location of practice is composed of three distinct processes with different determinants and dynamics: attraction, establishment and retention in the practice location. The first process, attraction, is defined as a positive attitude towards medical practice in remote or isolated regions that does not necessarily lead to settling into practice there. The establishment process follows the attracting process and is the decision about practice location. Finally, retention or continuation of medical practice in a rural or remote location over time is a choice to persist practicing in that setting, based on personal experience.
A qualitative study of physicians in outlying regions of Quebec reported that different factors play a role in each of the three processes described by Bilodeau and Leduc5. Familiarity with the rural environment, family links, and presence of relatives (physician or spouses) were related to attracting and establishing physicians in outlying regions8. In another qualitative study, conducted in Alberta, the authors found that many residents training in the rural stream had no long-term plans to establish a rural practice9.
There is evidence that some personal and training factors predict a physician's location of practice10. Personal factors such as exposure to rural environments during childhood (rural background), rural background of spouse, sex, age, ethnicity, and father's educational status have been explored in several studies with different degrees of association to location of practice5-7,11. Brooks et al6 identified characteristics that are present prior to medical school as 'nature', and the aspects related to the medical training (curricula, faculty, rotations, medical school mission etc) that potentially foster the attraction of students toward some specific type of practice as 'nurture'.
Several studies explored 'nature' factors associated with rural or urban practice of family physicians (FPs) in Canada. Easterbrook et al12 conducted a cross-sectional survey of 159 FPs who graduated from a Canadian medical school and found that physicians raised in rural communities were 2.3 times more likely to practice in rural areas than those from non-rural communities. No other independent variable in this study was a significant predictor of rural practice12. Similarly, a later study13 reported that physicians with a rural background were 2.5 times more likely to be engaged in rural practice than their urban-raised peers. A cross-sectional study of 507 physicians practicing in Ontario14 found that rural physicians compared with urban physicians were more likely to have a rural background. Chan et al15 studied 382 FPs established in rural areas across Canada and found that physicians raised in rural areas were more likely than those raised in urban areas to have some interest in a rural practice at the start and the end of medical training, while physicians raised in urban areas were more likely to state that rural training was the most influential factor in the choice of a rural practice.
'Nurture', including characteristics of medical schools and training programs, have been studied mostly in the context of exposure to underserved areas during under and postgraduate medical education and curricula6,16-23. Medical training programs usually include clerkships and rotations in rural, remote or underserved areas. However, within the same program, these can be elective or can take place at different time, resulting in a large array of individual trajectories24. In the literature, nonetheless, there is a convergence towards the importance of duration (longer than 2 months) and type of exposure (long-term rotations, fixed base), suggesting a dose-response relationship25,26.
The purpose of this study was to compare two categories of predictors of establishing a rural family practice using undergraduate medical student's individual characteristics (nature) and participation in a rural program component of their training program (nurture) using institutional administrative data. Aims were to identify similarities and differences in factors that predict practice 2 years post-residency training and to determine the predictive value of combining nature and nurture variables using data from two undergraduate medical education programs in Canada.
Design
To address the questions of interest, a retrospective study was conducted using administrative data available from the Université de Sherbrooke (UdeS) and the University of British Columbia (UBC). Although the two medical schools are situated in different provinces, each within a unique cultural, institutional, and government context, both have a strong mandate to evaluate the impact of their programs on physician distribution and are collaborating to identify methodologies to achieve this goal.
Students' personal data and undergraduate MD program data were retrieved from the faculties of medicine and registrar's offices. Postgraduate program and practice location data were accessed from the Canadian Post-MD Education Registry (CAPER; www.caper.ca), and linked to individual data. This study was approved by the UBC and UdeS Behavioural Research Ethics Boards.
Study sites
The population studied included all physicians that were registered in the undergraduate medical programs (MD program) between 1995 and 2000 (N=780 UdeS; N=936 UBC), whose postgraduate training was in family medicine and took place between 2000 and 2006 (n=218 UdeS, n=237 UBC) and for which an address of practice in the CAPER registry was available 2 years after their postgraduate training (n=180 UdeS, n=194 UBC).
Dependent variable
The dependent variable was the location of practice 2 years after completing postgraduate training: a Canadian non-metropolitan area versus a Canadian metropolitan area or another country. Practicing in a non-metropolitan area was defined as having a practice address located in a municipality with less than 100 000 inhabitants27,28. All other practice addresses were identified as 'not practicing in non-metropolitan area'. In the context of the healthcare system where most specialized care is concentrated in metropolitan areas (>100 000 inhabitants), it is legitimate to use the definition of non-metropolitan area as a proxy of rural area.
Dissemination areas (DA; the smallest geographical unit of census data available) were used from the 2001 Canadian Population Census as a proxy for address29. The Postal Codes Conversion File30 allowed matching each DA with a category of the Statistical Area Classification that classifies postal code areas according to the population of the urban core27,28.
Independent variables
The independent variables represent physician individual characteristics and program components identified in the literature as potentially related to the choice of a location of practice, and available at the two institutions represented in the study. Because the aim was to explore the predictive power of equivalent variables in two different contexts, only variables that were similar across both universities were used. Variables that differed were not included in the analysis.
Individual characteristics in the analysis included sex; age at admission to the MD program; location of the high school (UBC) or the premedical college (UdeS); preadmission academic performance ('Cote de rendement global' for UdeS, overall undergraduate grade point average [GPA] for UBC); and the location of the student address in admission forms. The academic degree at admission to the MD Program was important to UdeS, given their provincial general and vocational education post-secondary educational program, a system exclusive to Quebec. Thus, degree at admission to the MD program was coded for UdeS (ie college/university). In BC, there is no comparable system, and this variable was not considered for the UBC analyses. Academic performance in each of the program years (ie years 1-4) was converted to a standardized score. High school/college and home addresses at admission were coded as: 1 = metropolitan area (municipality with 100 000 inhabitants or more), 2 = medium/small city (municipality with 10 000-99 999 inhabitants), 3 = rural/small town (municipality with <10 000 inhabitants) or 4 = country other than Canada27.
A programmatic variable (nurture) was included in the analysis to capture student exposure to non-metropolitan environments during year 3 clerkships. For UdeS this variable was the number of weeks spent in clerkships in non-metropolitan areas (ie municipalities under 100 000 inhabitants). At UdeS students chose the location of mandatory and elective clerkships among program-approved placements. For UBC, a comparable variable represented the location of a mandatory four-week community-based year 3 clerkship. Using a lottery system, students select a clerkship from underserved, widely dispersed geographical locations, including some inner city locations. The location of UBC clerkships was categorized according to the Statistical Area Classification: 1 = metropolitan areas (municipalities with ≥100 000 inhabitants), 2 = medium/small city (municipality with 10 000-99 999 inhabitants), 3 = rural/small town (Census Subdivision with <10 000 inhabitants), 4 = Territories (Yukon, Northwest and Nunavut Canadian territories).
Statistical analysis
Given the differences in variable definitions and data available at the two institutions in the study, separate analyses were conducted and results were conceptually interpreted to identify similarities and differences. Descriptive statistics were produced for each university and comparisons made between family practice physicians in non-metropolitan locations and in 'other' locations using χ2 analysis. Univariate logistic regressions were conducted to identify variables significantly associated with location of practice.
Because the sample size was relatively small for both universities, multiple logistic regression models were performed using the independent variables statistically significant at p<0.10 from univariate analyses and the hypothesis that factors related to training program characteristics (ie nurture) are important predictors. Age and sex were included in all models. Individual student characteristics (nature) were included in the first model and the training program variable (nurture) was added to the second model to determine any change in the variance predicted. Chi-square was calculated to determine if there was a significant difference in R2 between the nature and nature plus nurture models.
Université de Sherbrooke
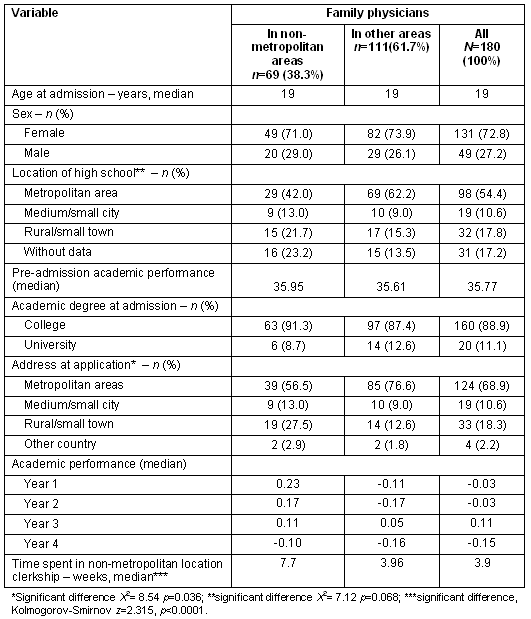
Descriptive data for the UdeS is provided (Table 1). Of the 180 FPs training between 1995 and 2006, 69 (38%) had established a practice in a non-metropolitan area 2 years after exiting residency. Family physicians established in non-metropolitan and in 'other' areas were similar for the majority of variables. A higher proportion of FPs practicing in non-metropolitan areas had a rural/small town address at the time of application to medical school (27.5%) compared with those practicing in other areas (12.6%; p=0.036). Similarly, a higher proportion of those practicing in non-metropolitan areas had attended a rural/small town high school as compared with those who were practicing in other areas (21.7% vs 15.3%, respectively; p=0.068). There was also a significant difference in the number of weeks FPs practicing in non-metropolitan areas had spent in non-metropolitan clerkships (p<0.0001, Kolmogorov Smirnov test). The median for those who had established a practice in a non-metropolitan location spent was 7.7 weeks in a non-metropolitan clerkship as compared with 3.9 weeks among those who were practicing in other areas.
Table 1: Description of Université de Sherbrooke population studied
Univariate logistic regressions found three variables with significant associations to location of practice (p<0.05). The academic performance for years 1 and 2 also showed some statistical significance (p<0.10) in the association to location of practice (Table 2). Age at admission and sex were included in the multiple logistic regressions, along with these five variables. The model developed with the individual variables explained 10% of the variability (R2= 0.101, n=176, Table 3) while the model developed adding the program variable, the nurture predictor, explained 21% of the variability (R2=0.211, n=176; Table 4). For the nature plus nurture model, the single nurture variable (length of clerkship in a non-metropolitan area) was the most important predictor (OR=1.14, 95% CI: 1.067-1.22), the odds of establishing a practice in a non-metropolitan location increasing by 14% for each week of clerkship spent in non-metropolitan areas. Just one nature predictor had a significant effect: having an address in a rural/small-town environment at the time of application to the medical school increases more than twice the chances of practicing in a non-metropolitan area (OR=2.61, 95% CI: 1.24-6.06). This predictor conserves an independent and significant effect when the nature predictor is taken into account.
Table 2: Univariate logistic models for MD graduates from Université de Sherbrooke
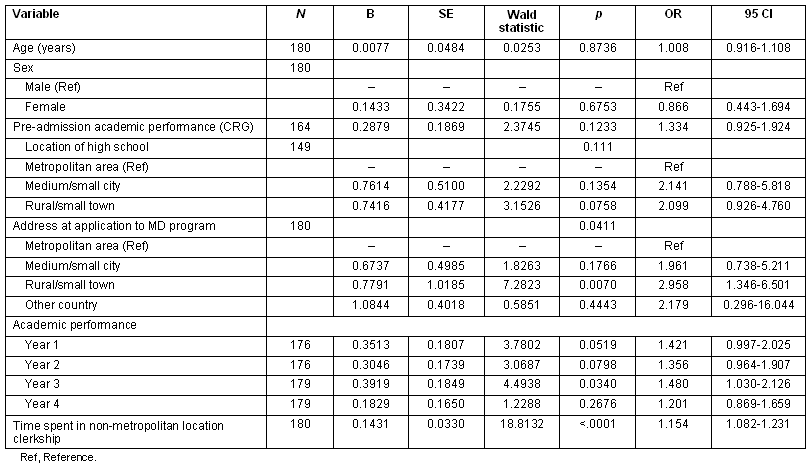
Table 3: Nature predictors of the location of practice in non-metropolitan areas for family physicians from Université de Sherbrooke (N=176), R2=0.101
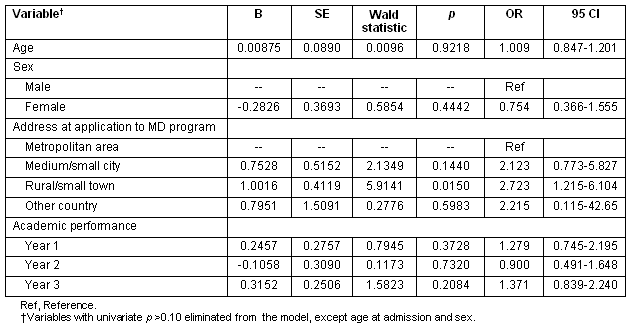
Table 4: Nature and nurture predictors of the location of practice in non-metropolitan areas for family physicians from Université de Sherbrooke (N=176), R2=0.211
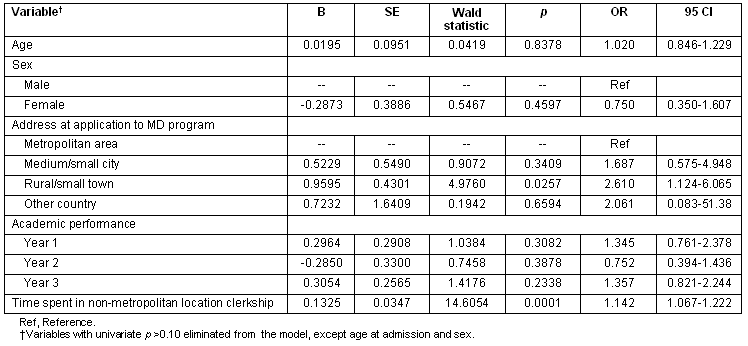
University of British Columbia
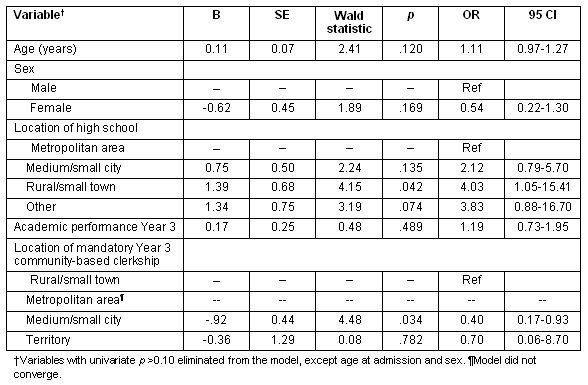
Descriptive data from the UBC program is provided (Table 5). Of the 194 FPs training between 1995 and 2006, 59 (30%) had established a practice in a non-metropolitan area 2 years after exiting residency. Family physicians established in non-metropolitan and 'other' areas were similar for the majority of variables examined. None of the students who completed the mandatory year 3 clerkship in a metropolitan area were likely to establish a practice in a non-metropolitan area (χ2 p=0.011, Cramer's V=0.011).
Univariate logistic regressions found one variable, location of high school, to have a significant association with location of practice (p<0.05). Year 3 academic performance showed some statistical significance (p<0.10) in the association to the dependent variable (Table 6). Age at admission and sex were included in the multiple logistic regressions, along with these two variables. The model developed with only the individual variables (nature) explained 16% of data variability (R2=0.16, n=190; Table 7). Because the contribution of the year 3 mandatory clerkship (nurture) in predicting location of practice was to be examined, this variable was included in the second model. It was found that 27% of the variability in the location of practice was predicted (R2=0.27, n=125; Table 8) by adding this single nurture variable. An R2 difference test was performed to assess the R2 difference between the nature only and the nature plus nurture models indicated a statistically significant increase in R2 in the nature plus nurture model (F (3,180) = 9.49; p<0.001). For the nature plus nurture model, those who attended high school in a rural/small town were four times more likely to practice in a non-metropolitan area (OR= 4.03, 95% CI: 1.05-15.41). The odds of establishing a practice in a non-metropolitan location decreased by almost half for students placed in a medium/small city for their year 3 community-based clerkship as compared to those placed in a Rural/small town area (OR=0.40, 95% CI: 0.17-0.93). The model did not converge for the metropolitan area variable, likely due to missing data and small sample size.
Table 5: Description of the University of British Columbia population studied
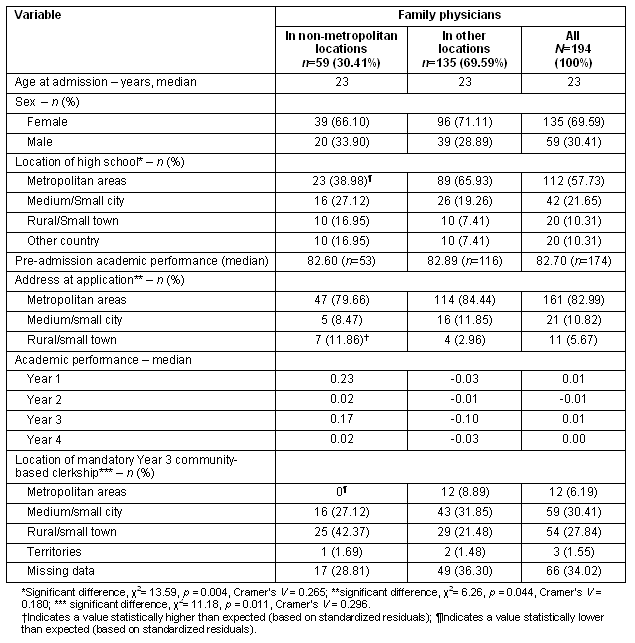
Table 6: Univariate logistic models for MD graduates from University of British Columbia
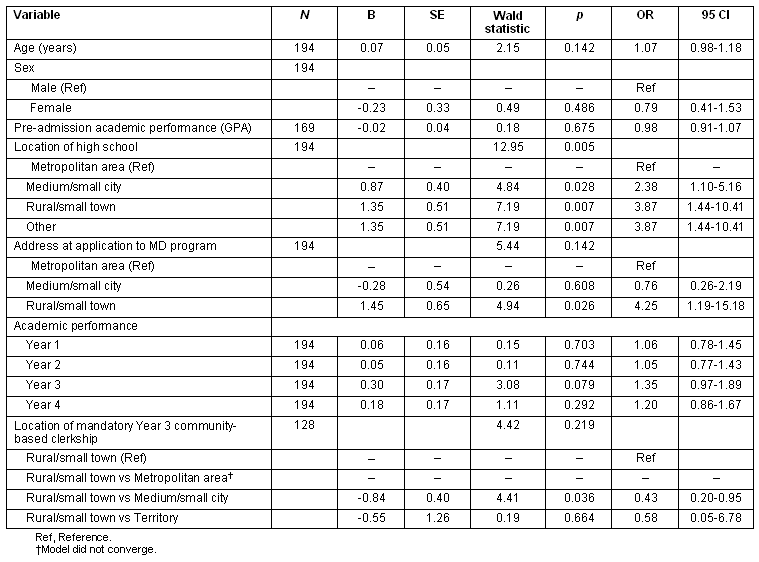
Table 7: Nature predictors of the location of practice in non-metropolitan areas for family physicians from University of British Columbia (N=190), R2=0.16
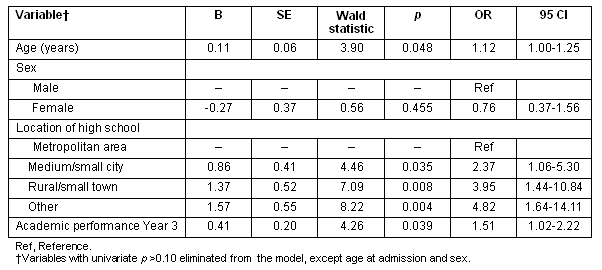
Table 8: Nature and nurture predictors of location of practice in non-metropolitan areas for family physicians from University of British Columbia (N=125), R2=0.27
Discussion
Adding a single nurture variable (ie component of training program) to the model using only nature variables (ie individual characteristics) significantly increased the amount of variation accounted for in predicting practice in non-metropolitan areas in the two medical schools. The finding that nature variables associated to rural or non-metropolitan backgrounds increases the chances of practicing in rural or non-metropolitan areas is consistent with previous research5,12-14. The length of clerkships in non-metropolitan areas (nurture) was the strongest predictor of the location of practice for UdeS independent of the other variables, reflecting the nurture effect highlighted by Brooks et al6. This was supported by the UBC finding that location of UBC's mandatory year 3 community-based clerkship showed some relationship to location of practice, despite the small sample size. Although there is agreement that undergraduate rural experience can influence the choices made by students about practice location31, there is little evidence about the required length for this effect. At the postgraduate level, the threshold length of rural experience for impact on location choice was found to be 6 months in two separate family medicine studies14,32. A clerkship length of 6 weeks has been identified as a threshold to improve student educational and personal experiences in rural areas25, which may indeed lead students to choose longer rural experiences in their postgraduate training. As Ballance et al33 concluded in their review of the literature on factors that influence rural practice location, although 'nature' variables such as rural background are important factors, programs that encourage and reinforce rural practice are necessary to support students at both the undergraduate and postgraduate level.
The comparability of results from both universities is restricted by the differences in the provincial context and also because some of the variables result from different methods of collection and describe different program components. Despite this, it is interesting to note that both schools found similar results for nature variables. For UdeS, having an address in a rural/small-town environment at application to medical school and for UBC, location of high school in a rural/small town, increased the chances of practicing in a non-metropolitan area. For UdeS the nurture variable (ie length of clerkship in a non-metropolitan area) was the most significant predictor. This was not the case for UBC which is likely to be due to the small sample size; however, UBC results did indicate that the location of the mandatory year 3 community-based clerkship in a medium/small city, as compared to those placed in a Rural/small town area, decreased the chances of practicing in a non-metropolitan area. Further research is necessary to determine if this finding extends to clerkships in metropolitan areas.
The nature and nurture variables considered in the models explained only 21% to 27% of the variance in FPs' location of practice. This suggests that the study design could be improved by increasing the number of variables explored in this study that were not included in the models, because these data are not available through the universities' administrative databases (eg background, beliefs, intentions and internal models of the physicians). Another important reason for the poor fit of models is that contextual factors such as the structure of health systems in each province were not included in the models (because appropriate data was not available). Finally, a measure of postgraduate training was not included, which would most likely have improved the predictability of the model.
Even if the loss to follow up was less than 20% at both sites, the quality and availability of detailed administrative data on students and medical programs at each university was insufficient to respond to the need for tracking long-term outcomes in medical education. For example, at both universities it required months to locate, gather and 'clean' the data, and build a centralized database. Lack of consistency of variable definitions over the years available was challenging. At UBC the amount of missing data meant there was an inadequate sample size for the final model. It also resulted in wide confidence intervals which comprised the precision of data. As a consequence, different strategies are being implemented in each university to improve the quality of existing databases, as well as to collect relevant data about intent to practice, training characteristics, and attitudes, beliefs and backgrounds of students.
Based on the experience of conducting this work, the authors have begun to develop centralized databases that track students from admission to practice and are exploring the use of Scott's Medical Database34 to access information about location of practice to track long-term outcomes. At the same time the authors believe it is important to explore mechanisms for sharing and accessing data with other national and regional organizations working toward the same goal. There is increasing interest in addressing long-term outcomes in medical education. These questions cannot be answered by a single institution. New models of research should explore the development of longitudinal databases among collaborating schools35. Further work needs to be done to explore how institutional databases, such as the ones described in this article, can be merged.
Despite the limitations of this study, it contributes to the knowledge of factors associated with FPs choosing to locate in non-metropolitan areas in two provinces. Using complementary approaches from two provinces increases the credibility of findings.
Acknowledgements
The authors thank Dr Shayna Rusticus for statistical assistance, France Gagnon for contributing in the development of the database, and Joan Gray for editing. This project was funded by a grant from Frontline Health: an initiative of AstraZeneca Canada.
References
1. Canadian Labour and Business Centre. Canada's physician workforce. occupational human resources. data assessment and trends analysis. Executive Summary. Ottawa, ON: Task Force Two, 2005.
2. Pong R, Pitblado R. Répartition géographique des médecins au Canada: au-delà du nombre et du lieu. Ottawa, ON: Institut Canadien d'information sur la Santé, 2005.
3. Task Force Two. A Physician Human Resource Strategy for Canada. Final Report. Ottawa, ON: Task Force Two, 2006.
4. Vanasse A, Orzanco MG, Courteau J, Scott S. Attractiveness of family medicine for medical students: influence of research and debt. Canadian Family Physician 2011; 57(6): e216-27.
5. Bilodeau H, Leduc N. Recension des principaux facteurs d'attraction, d'installation et de maintien des médecins en régions éloignées. Cahiers de Sociologie et de Démographie Médicales 2003; 43(3): 485-504.
6. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77(8): 790-798.
7. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11: 277-284
8. Bilodeau H, Leduc N, Schendel NV. Analyse des facteurs d'attraction, d'installation et du maintien de la pratique médicale dans les régions éloignées du Québec. Montréal, QC: Groupe de recherche interdisciplinaire en santé, 2006.
9. Lu D, Hakes J, Bai M, Tolhurst H, Dickinson J. Rural intentions. Factors affecting the career choices of family medicine graduates. Canadian Family Physician 2008; 54: 1016-1017.
10. Rabinowitz H, Paynter N. The rural vs urban practice decision. JAMA 2002; 287(1): 113.
11. Fryer G, Stine C, Vojir C, Miller M. Predictors and profiles of rural versus urban family practice. Family Medicine Journal 1997; 29(2): 115-118.
12. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R et al. Rural background and clinical rural rotations during medical training: effect of practice location. Canadian Medical Association Journal 1999; 160(8): 1159-1163.
13. Woloschuk W, Tarrant M. Do students from rural backgrounds engage in rural family practice more than their urban-raised peers? Medical Education 2004; 38: 259-261.
14. Rourke J, Incitti F, Rourke L, Kennard MA. Relationship between practice location of Ontario family physicians and their background or amount of rural medical education experience. Canadian Journal of Rural Medicine 2005; 10(4): 231-239.
15. Chan B, Degani N, Crichton T, Pong R, Rourke J, Goertzen J et al. Factors influencing family physicians to enter rural practice. Does rural or urban background make a difference? Canadian Family Physician 2005; 51: 1246-1247.
16. Rourke J. Increasing the number of rural physicians. Canadian Medical Association Journal 2008; 178(3): 322-325.
17. Dalton LM, Routley GK, Peek KJ. Rural placements in Tasmania: do experiential placements and background influence undergraduate health science student's attitudes toward rural practice? Rural and Remote Health 8: 962. (Online) 2008. Available: www.rrh.org.au (Accessed 8 September 2011).
18. Chen F, Fordyce M, Andes S, Hart LG. Which medical schools produce rural physicians? A 15-year update. Academic Medicine 2010; 85(4): 594-598.
19. Ferguson WJ, Cashman SB, Savageau JA, Lasser DH. Family medicine residency characteristics associated with practice in a health professions shortage area. Family Medicine 2009; 41(6): 405-410.
20. Page S, Birden H. Twelve tips on rural medical placements: what has worked to make them successful. Medical Teacher 2008; 30(6): 592-596.
21. Straume K, Shaw DMP. Internship at the ends of the earth - a way to recruit physicians? Rural & Remote Health. Rural Remote Health 10(2):1366. (Online) 2010. Available: www.rrh.org.au (Accessed 8 September 2011).
22. Wilson M, Cleland J. Evidence for the acceptability and academic success of an innovative remote and rural extended placement. Rural and Remote Health 8(3): 960. (Online) 2008. Available: www.rrh.org.au (Accessed 8 September 2011).
23. Veitch C, Underhill A, Hays RB. The career aspirations and location intentions of James Cook University's first cohort of medical students: a longitudinal study at course entry and graduation. Rural Remote Health. Rural and Remote Health 6(1):537. (Online) 2006. Available: www.rrh.org.au (Accessed 8 September 2011).
24. Dunbabin JS, McEwin K, Cameron I. Postgraduate medical placements in rural areas: their impact on the rural medical workforce. Rural and Remote Health 6(2):481. (Online) 2006. Available: www.rrh.org.au (Accessed 8 September 2011).
25. Denz-Penhey H, Shannon S, Murdoch JC, Newbury JW. Do benefits accrue from longer rotations for students in rural clinical schools? Rural and Remote Health 5: 414. (Online) 2005. Available: www.rrh.org.au (Accessed 8 September 2011).
26. Pathman DE, Konrad TR, Ricketts TC. Medical-education and the retention of rural physicians. Health Services Research 1994; 29(1): 39-58.
27. du Plessis V, Beshiri R, Bollman R, Clemenson H. Definitions of 'Rural'. Agricultural and Rural Working Paper series no. 61. Ottawa: Statistics Canada, 2002.
28. Rambeau S, Todd K. Zones d'influence des régions métropolitaines de recensement et des agglomérations de recensement (ZIM) accompagnées de données de recensement. Ottawa: Division de la géographie, Statistique Canada, 2000.
29. Statistics Canada. Dictionnaire du recensement 2001. Ottawa: Statistics Canada, 2003.
30. Statistics Canada. Fichier de conversion des codes postaux (FCCP), Septembre 2006. Ottawa: Statistics Canada, 2007.
31. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health 9: 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 8 September 2011).
32. Chan BTB, Degani N, Crichton T, Pong RW, Rourke JT, Goertzen J et al. Duration of rural training during residency. Canadian Family Physician 2006; 52: 210-211.
33. Ballance D, Korneygay D, Evans P. Factors that influence physicians to practice in rural locations: a review and commentary. Journal of Rural Health 2009; 25(3): 276-281.
34. Canadian Institute for Health Information. Scott's medical database. (Online) no date. Available: http://www.cihi.ca/CIHI-ext-portal/internet/en/document/spending+and+health+workforce/workforce/physicians/hhrdata_smdb (Accessed 23 June 2011).
35. Cook DA, Andriole DA, Durning SJ, Roberts NK, Triola M. Longitudinal research databases in medical education: facilitating the study of educational outcomes over time and across institutions. Academic Medicine 2010; 85(8): 1340-1346.





