Public health efforts to promote mental health among older adults in rural communities through increased awareness and knowledge are impeded by stigma regarding psychiatric disorders and treatment1 as well as stigma about aging2. Further, treatment outcomes suffer when individuals' symptoms become more complex and severe due to delayed management3. Efforts to inform and empower rural and remote community residents about mental health/substance abuse (MH/SA) and aging are vital to the promotion of mental health and quality of life among older adults in such areas. Community-based efforts to promote mental health may help rural residents recognize the need for mental health treatment at the earliest sign of a problem and also obtain that treatment when necessary.
Addressing mental health in rural and remote communities can be extremely challenging for several reasons. As Lawrence and McCulloch4 noted, many individuals prefer not to discuss their mental health and would rather keep thoughts on their mental health private. Denial, fear of stigmatization, and avoidance are common responses to the prospect of discussing one's mental health status5. In rural areas in particular, there are limitations in formal and informal mental health care and treatment resources as a result of social, economic, psychological, demographic and physical barriers6,7. For instance, much of the difference between rural and urban residents' mental health status is explained by financial and educational disparities across these regions8. In addition, in rural and remote environments an emphasis on independence and self-reliance can make intervening in residents' lives difficult9. Also, in remote areas seeking out resources may be difficult because of geographic barriers (eg traveling on mountainous roads in Appalachian Kentucky) and lack of adequate transportation to services10. Further, the healthcare resources that are available in remote and rural areas may be inadequate or outdated11. Given these challenges, mental health research and interventions need to focus on empowering residents to identify and address their own MH/SA problems while simultaneously promoting high quality community living for individuals experiencing mental health issues in rural and remote areas12.
Addressing MH/SA is important for several reasons. Mental illness can be detrimental to older adults but often goes unrecognized13,14 and is frequently misrepresented as a normal part of aging15. Mental health disorders, such as depressive syndromes, lead to poor health trajectories in areas such as morbidity, functioning and mortality16,17, particularly among older adults18. Severe mental illness, such as depression, can reduce life expectancy by nearly 25 years; this reduction is attributable to poor health behaviors and the presence of preventable diseases19.
Depression is one of the most common mental health problems. Depression affects approximately 14.8 million United States adults (6.7%) in a given year20, with approximately 27% of community-residing adults over the age of 60 reporting depressive symptoms21. Further, up to 50% of older adults in rural areas meet criteria for depressive disorders22. According to the WHO, depression is one of the leading causes of disability23. Further, depression increases the risk for disability24, ischemic events25, cancer26, pain27 and mortality28,29.
The presence of substance dependence, another major MH/SA problem, leads to continued chemical use and risky driving behaviors30. Heavy alcohol consumption in particular has been associated with poor health behavior patterns31, multiple risk behaviors32 and low use of preventive health services33. Further, less than half of adults in treatment for alcohol disorders exercise regularly, partly due to low self-efficacy for physical exercise34. Compounding the negative effects of substance abuse in general, older adults are more vulnerable to risks associated with alcohol consumption35,36. Changes in physiology associated with aging contribute to this increased risk37 and the need to decrease levels of alcohol consumption38. Older adults are hospitalized for alcohol-related complications as much as for myocardial infarctions39 . In addition, the elevated use of medications can interact with alcohol, putting older adults at heightened risk for poor outcomes when consuming alcohol40. Prescription drug safety is a vital area for health promotion due to increases in fatal medication errors related to alcohol and illicit drug use occurring more so than deaths from medication or alcohol/illicit drug use alone41 . Older rural residents are among the highest risk for experiencing prescription drug misuse issues42 . Overall, substance abuse can lead to poorer health behavior patterns and ultimately poor health outcomes.
In addition to the poor health and behavioral outcomes associated with MH/SA disorders, the need for appropriate treatment is also necessary. Across the USA, only 48-62% of individuals with depression problems43 and 34-48% of individuals with substance abuse problems receive recommended care44, leaving approximately 38-66% of individuals without appropriate treatment. Even among individuals who have been properly diagnosed and provided with an opportunity to engage in MH/SA treatment, across age groups, only 50% attend scheduled appointments for treatment45. These results are likely to underestimate the numbers of people with untreated MH/SA problems, since individuals in need of MH/SA treatment are not always identified46.
With the prevalence of MH/SA disorders among older adults, the serious ramifications and the frequent lack of identification, MH/SA is a greatly needed area for intervention among older adults. Unfortunately, provision of MH/SA services for older adults is insufficient to meet the growing mental health needs47. Thus, there is a need for the development of improved MH/SA community management services to increase identification and subsequently treatment planning and treatment engagement to avoid negative mental and physical health outcomes. Special attention must be paid to older adults due to their higher levels of health burden48,49 and their lower rates of treatment compared to younger adults50. Attention is needed in rural areas, in particular, due to a greater limitation on mental health resources and trained professionals51.
The Mental Healthiness Aging Initiative (MHAI) was developed to promote the mental health of rural older adults (aged 65+ years) by (i) developing community relationships in rural areas of Kentucky through partnerships with cooperative extension agents, (ii) creating discussion in the community regarding MH/SA and aging and (iii) implementing a community MH/SA educational intervention program using the information diffusion process52. In application, the program was designed to communicate key messages about MH/SA and aging, increase knowledge about MH/SA and aging, and ultimately decrease mental health related disadvantages experienced by older adults, particularly those residing in rural communities53,54. Specifically, the intervention component of MHAI was designed to empower community members to manage and promote mental health. Our earlier work on this topic identified community beliefs about the importance of mental health while aging, which served as the foundation for developing and implementing MHAI55 and the effectiveness of a train-the-trainer MHAI program56. Examining the macro-level effect of MHAI, it was found that target communities demonstrated greater knowledge and awareness of mental health and aging issues with MHAI programming exposure. However, the effect of the intervention component on individuals (micro-level effects) participating in the project, and the long-term effects, were left unclear57. The goal of the current study is to assess the immediate and sustained effect of the MHAI intervention component on individuals over time in an independent rural community sample. This information will support a tool that can be used to promote the mental health of older adults in rural communities through increased awareness, knowledge and social support for mental health problems.
The study sample (n=55) was recruited through two rural Kentucky counties through local cooperative extension service offices. The Kentucky Cooperative Extension Service serves as a link between the state's university and the communities to help individuals and communities improve quality of life through education, research and outreach. In the state of Kentucky, there is at least one cooperative extension office in each of the 120 counties. Two Kentucky cooperative extension agents were recruited through an email solicitation. Once recruited, the individual extension agents recruited participants within their jurisdictions. At the designated time, all interested participants came to attend the MHAI intervention at their local cooperative extension office. The intervention session lasted approximately 1 hour, which included a pre-assessment and a post-assessment. Thereafter, participants were contacted over the telephone 3 months and 6 months after the initial assessment to collect follow-up retention data.
The MHAI intervention program consisted of three key components: facts and information, application exercises, and community tools. These components were conceptualized through the information diffusion process to aid participants with the five stages of adoption: knowledge, persuasion, decision making, implementation and confirmation52. For instance, the knowledge stage was reached through the facts and information section, which included information and discussion about the signs and symptoms of MH/SA disorders. In the facts and information section, reaching the persuasion stage was done through the presentation of and discussion of MH/SA outcomes, suggestions for promoting good mental health and strategies for the management of MH/SA. The information for this section was acquired from current geriatric mental health scientific literature and focused on depression, alcohol use and prescription drug safety as the most prevalent and pertinent geriatric MH/SA issues13-15,37,38,47,58-69 . The facts and information component was expected to create an increase in MH/SA knowledge and greater acknowledgement of the MH/SA crisis to facilitate the adoption process.
The application exercise section was designed to promote the stages of decision making and implementation through a tutorial describing steps for implementing a community action plan entitled PALS - 'Pay attention, Ask questions, Listen actively, and Show support'. The PALS system was designed to empower participants to become mental health promotion agents in their communities by paying attention to their surroundings (in the context of mental health), talking to and listening to community members in possible need of mental health promotion and providing support in any requested way - whether the support be simply talking or even taking a friend to a doctor's visit to get mental health care. Participants were informed about how to use the PALS system when identifying possible MH/SA symptoms in community residents. The action plan was created in reaction to a need, expressed by cooperative extension agents, for a tool to practically disseminate and utilize MHAI information. Agents asked for an action plan/tool, in addition to facts and information, that would enable them to apply the knowledge learned in the MHAI program, and that they could use specifically when they suspected MH/SA problems in community residents. Having an action plan aids with a deeper level of adoption, empowers participants and can prevent the newly learned knowledge from lying dormant due to lack of application skills.
Finally, the confirmation phase was designed to be reached through the community tools section. The community tools sections provided complementary tools for distribution that represented and confirmed the key ideas presented in MHAI. The tools included bookmarks, pamphlets and note pads listing signs and symptoms of depression and alcohol abuse and strategies for promoting good mental health. The recommended strategies for promoting and managing mental health were within physical, mental, social and financial domains, such as engaging in exercise, practicing proper nutrition and focusing on mind-body wellness. As part of the toolbox, participants were also given a 'Talking to your doctor about mental health' handout to use as a communication tool when an MH/SA problem was suspected. Participants were instructed that contacting a primary care physician is a first response to suspected mental health problems. The community tools component is another method to aid participants with adoption, and provide participants with the means to actively disseminate and confirm knowledge retained from the MHAI program.
Measurement variables
Each participant was evaluated prior to receiving the intervention (pre) and immediately after receiving the intervention (post) to determine whether MH/SA knowledge and beliefs had improved. Participants were also assessed over the telephone at 3 months and 6 months after participating in the intervention to examine whether changes were sustained. The evaluation survey consisted of the following sections: (i) demographics, (ii) MH/SA awareness (six questions) and (iii) MH/SA knowledge (13 questions). The demographic section contained standardized (census-based) questions about date of birth, gender (ie male/female), race (ie white, black, Asian, Native American, Pacific Islander, Hispanic, other), marital status (ie marred, single, divorced, widowed, cohabitating, separated), educational level (ie highest degree) and income level (ie annual household). The evaluation survey was designed specifically for this program to address MH/SA aging issues, ensuring face validity. The awareness section focused on perceptions of MH/SA and aging issues, as well as participants' own perceived ability to manage mental illness. Response options for the awareness questions were in a Likert scale format to assess the level of agreement. The knowledge questions focused on common myths about MH/SA and aging and were presented in true/false format; responses were aggregated to create a knowledge summation score. The evaluation survey was previously piloted in a state-wide MHAI implementation57.
Data analysis
Seven individual linear mixed models were analyzed using SAS v9.1 (www.sas.com), one for each of the awareness questions and one for the total percent correct knowledge questions. Convergence criteria were met for all linear mixed models analyzed, indicating fit. Mixed models offer the best fit for repeated measures to account for time effects (change/growth) on the dependent variable70 . The models included time (four levels: pre, post, 3 month follow-up and 6 month follow-up) as the main independent variable. MH/SA awareness (six items) and MH/SA knowledge (aggregate score) were the main dependent variables and were treated as continuous variables. In addition to means, modes and medians are provided to present normality.
Ethics approval
All study procedures were ethically approved by the University of Kentucky Institutional Review Board (IRB) (Number 09-0896-F4S). Accordingly, all participants signed an IRB approved consent form prior to participation.
Sample characteristics
A total of 55 individuals participated in the current study. The average age of the sample was 65.35 years (median=65, mode=68), with an average income of US$44,199 (median=US$44,000, mode=US$60,000). The majority of the sample was female (85%), white (100%), married (69%), living with a spouse/partner only (68%) and high school educated (57%); the mean education in years was 14 years (median=12, mode=12). There were no county differences across demographics; therefore, county was not considered in analyses. The return rate for the sample was 94% at post-test, 73% at the 3 month follow-up and 76% at the 6 month follow-up.
Awareness
There was significant improvement across the indicators for mental health awareness (p<0.05; Table 1). Specifically, mean trends indicate that over time there was an improvement in understanding that mental illness is not a normal part of aging. Over time there was also an improvement in agreement about: (i) older adults successfully being treated for mental illness; (ii) having the tools and knowledge to recognize mental illness; (iii) mental illness negatively affecting mental and physical health; and (iv) perceiving they can personally assist older adults that have mental illness. There were no awareness indicators that did not show improvement over time. Further, improvement was sustained at 6 month follow-ups.
Table 1: Sample survey responses pre-intervention and post-intervention, and at 3 month and 6 month follow up (n=55)
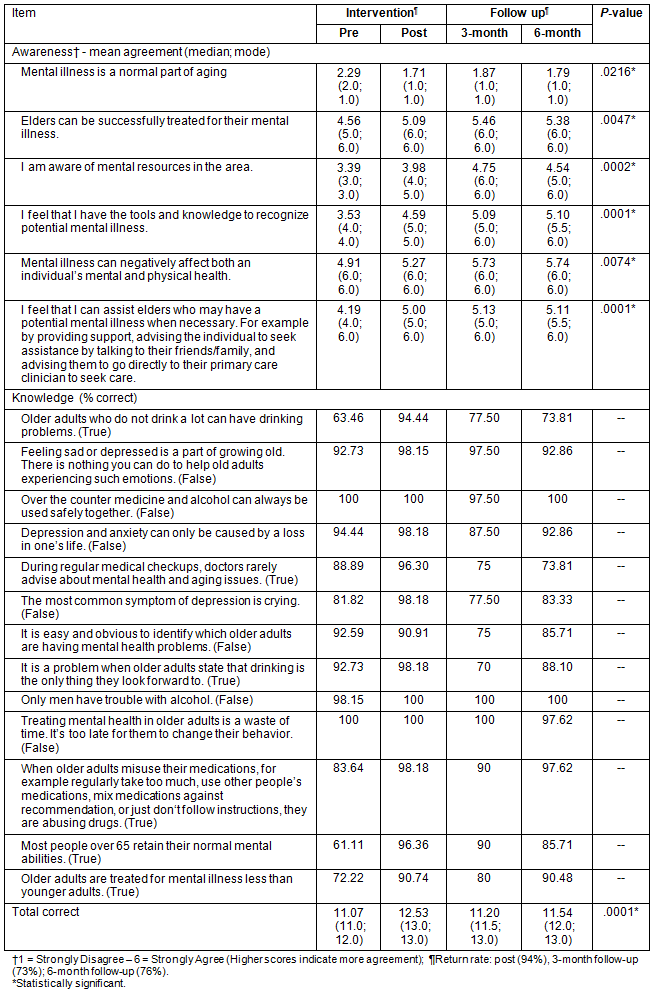
Knowledge
There was significant improvement across the indictors for mental health knowledge as indicated by the total correct score (p<0.05; Table 1). Improvement was sustained at the 6 month follow-up, with the peak of improvement being at the post-test administered immediately after the intervention session.
When examining specific knowledge indicators, frequency distributions indicated that improvement was sustained over the 6 month follow-up for most knowledge indicators. However, certain items may require enhanced intervention efforts to produce sustained knowledge. Frequency trends indicated that participants did not sustain knowledge for the following concepts: (i) older adults who do not drink a lot can have drinking problems; (ii) during regular medical check-ups, doctors rarely advise about mental health and aging issues; (iii) the most common symptom of depression is crying; (iv) it is easy and obvious to identify which older adults are having mental health problems; (v) it is a problem when older adults state that drinking is the only thing they look forward to; and (iv) most people over 65 years retain their normal mental abilities. These indicators had below 90% accuracy at 6 months, despite having 90%+ accuracy at post-assessment immediately after the intervention administration.
Discussion
The goal of the current study was to assess the immediate and sustained effect of the MHAI intervention component on individuals over time in an independent sample of rural community members. Findings indicated sustained improvement across awareness and knowledge indicators. Results also indicated a need to improve sustained knowledge about clinical mental health communication, identifying/recognizing mental health problems, retention of mental abilities and alcohol consumption risk.
This research adds to a limited body of evidence investigating mental health and substance abuse education-based interventions. Based on recent literature, there is a clear need for mental health educational interventions71-74 . Most research in this area focuses on clinical and community gate keeper samples, not specifically community members as in the current study. Some research has focused on community workers to increase their knowledge about MH/SA75-77 . Much research exists on training clinicians about managing and treating MH/SA78,79 . Across the literature there is a limited focus on older adults. Accordingly, the current work expands the scientific literature as it includes a focus on older adults and community members in MH/SA educational interventions.
In relation to the study findings, there is a need for sustained improvement across specific awareness and knowledge indicators to improve MHAI effectiveness, specifically in the areas of clinical mental health communication, identifying/recognizing mental health problems, retention of mental abilities and alcohol consumption risk. Unfortunately, prior studies have indicated that mental health providers often do not communicate about mental health effectively and inadequate mental health provider communication can lead to treatment mismanagement80. More emphasis is needed in MHAI on MH/SA clinical communication. Also, identifying and recognizing mental health problems is very challenging and denial is one of the most common responses to mental illness81. Proper identification and recognition are initial important steps on the road to mental health recovery. Due to the difficulty in identifying mental health problems, the annual use of screening tools can be further reinforced in the MHAI intervention program. As such, more emphasis is needed in the MHAI intervention to convey how mental health appointments and screening tools are important for ensuring that mental health needs are addressed and clinical MH/SA communication can be reinforced.
As indicated through the study findings, there is a need to increase awareness that 90% of individuals do retain normal mental health capabilities into old age. It is well documented that older adults retain their mental abilities, with only a small portion of older adults (approximately 10%) experiencing mental or cognitive health issues61. With most late life mental abilities intact, the MHAI intervention needs to be adjusted to reinforce the need for continued planning and wellness in old age in order to live a fulfilled life. Further, individuals tend to underreport and underestimate the effects of alcohol82. Knowledge about alcohol risk, in particular, can be enhanced in the MHAI by placing greater emphasis in the intervention on the dangers of alcohol consumption and signs or symptoms of substance misuse.
Implementing the MHAI intervention program, as currently designed, is feasible in rural regions. Evidence from the current study indicates that rural community residents can be recruited to participate in a program about MH/SA and aging, and as an outcome have increased awareness and knowledge about MH/SA and aging. Future research will need to explore how to utilize MHAI-type intervention programs to a point where the mental health of rural adults can be improved. For instance, further investigation is needed to examine whether community mental health education interventions, such as the MHAI intervention program, can lead to earlier detection of MH/SA issues among older adults and increased treatment rates. If so, community mental health facilities and workers can experience MH/SA education interventions to increase local residents' awareness of their services and likelihood of utilizing mental health services.
When interpreting the results of this study, there are some limitations to consider. For instance, it is important to consider issues of clinical significance and practical significance83. Some of the statistically significant findings highlighted in this study require further research to ensure that better ratings of one's beliefs/knowledge about MH/SA issues and aging lead to improved mental health for rural older adults. Future research also needs to reduce sample attrition and place emphasis on expanding the sample size to provide sufficient power to compare results with a control group84. As indicated in the sample characteristics, the current sample is limited in diversity, with a higher distribution of white individuals living in a geographically limited region. With an increase in sample size, attempts need to be made to improve representation of non-white older adults with lower income and education levels and from diverse regions to ensure effectiveness across diverse demographics and cultural contexts. It is also important to note that the evaluation survey was designed, considering face validity, specifically for this program. Future studies need to examine the psychometric properties of the evaluation instrument to replicate study findings. Another factor to consider when reviewing study findings is that this study was completed in the state of Kentucky, a majority rural state with high levels of health impairment that can affect individual mental health85. Research conducted in Kentucky is generalizable to at least 16.6 million Americans across the USA who also reside in Appalachian rural environments86 , but future studies need to examine the effectiveness of community mental health interventions like the MHAI in other rural locales, and in larger and more diverse samples.
The MHAI program serves as a useful tool for improving community members' knowledge and awareness of MH/SA risks, symptoms and outcomes among older adults. The MHAI intervention program is one of the first evidence-based community MH/SA and aging education programs targeting older adults in rural communities. Special attention to older adults is needed due to their higher rates of morbidity and their lower rates of psychiatric treatment, especially among those residing in rural areas. The MHAI program is underscored by the exacerbated implications of MH/SA issues in older adults, who are more likely to also be faced with multiple morbidities, polypharmacy, stigmatization (related to both age and MH/SA) and physiological changes. Also, because mental health disorders, such as depression, may be viewed as normal aging, older adults are less likely to have mental health problems identified or addressed by healthcare workers. Promoting individual community members' awareness and knowledge of MH/SA can foster the proper management of such issues in older adults.
Results of the current study demonstrate that community interventions focusing on mental health and substance abuse can be implemented successfully within rural communities. Results indicate that some components of the MHAI intervention were effective, but more work is still needed to enhance effectiveness. Future research should examine whether increased community awareness and knowledge translates into higher rates of MH/SA detection, proper clinical management of MH/SA and, ultimately, improved physical and mental health among older adults in larger, more diverse samples.
Acknowledgements
This research was supported by grants from the USDA: CSREE (2007-46100-03962), the Research Trust Challenge Grant awarded to the Graduate Center for Gerontology at the University of Kentucky, and National Institutes of Health (NIDA 5K12DA014040 and 1K01DA031764).
References
1. Keyes KM, Hatzenbuehler ML, McLaughlin KA, Link B, Olfson M, Grant BF et al. Stigma and treatment for alcohol disorders in the United States. American Journal of Epidemiology 2010; 172(12): 1364-1372.
2. Calasanti T. Ageism, gravity, and gender: experiences of aging bodies. Generations 2007; 29(3): 5.
3. Steinman LE, Frederick JT, Prohaska T, Satariano WA, Dornberg-Lee S, Fisher R et al. Recommendations for treating depression in community-based older adults. American Journal of Preventive Medicine 2007; 33(3): 175-181.
4. Lawrence SA, McCulloch BJ. Rural mental health and elders: historical inequities. Journal of Applied Gerontology 2001; 20(2): 144-169.
5. Philo C, Parr H, Burns N. Rural madness: a geographical reading and critique of the rural mental health literature. Journal of Rural Studies 2003; 19: 259-281.
6. Conradson D. Geographies of care: spaces, practices, experiences. Social & Cultural Geography 2003; 4(4): 451-454.
7. Parr H, and Philo C, 2003. Rural mental health and social geographies of caring. Social & Cultural Geography 2003; 4(4): 471-488.
8. Jones AR, Cook TM, Wang J. Rural-urban differences in stigma against depression and agreement with health professionals about treatment. Journal of Affective Disorders 2001; 134: 145-150.
9. Fuller J, Edwards J, Procter N, Moss J. How definition of mental health problems can influence help seeking in rural and remote communities. Australian Journal of Rural Health 2000; 8: 148-153.
10. Hall HI, Uhler RJ, Coughlin SS, Miller DS. Breast and cervical cancer screening among Appalachian women. Cancer Epidemiology, Biomarkers & Prevention 2002; 11: 137-142.
11. Stensland J, Mueller C, Sutton J, Appalachian Regional Commission, Project Hope, Center for Health Affairs. An analysis of the financial conditions of health care institutions in the Appalachian region and their economic impacts. Bethesda, MD: Project HOPE, Center for Health Affairs, (Online) 2002. Available: http://www.arc.gov/index.do?nodeId=1647 (Accessed 1 June 2007).
12. Pinfold V. 'Building up safe havens ... all around the world': Users' experiences of living in the community with mental health problems. Health & Place 2000; 6: 201-212.
13. Pond CD, Mant A, Bridges-Webb C, Purcell C, Eyland EA, Hewitt H et al. Recognition of depression in the elderly: a comparison of general practitioner opinions and the Geriatric Depression Scale. Family Practice 1990; 7(3): 190-194.
14. Mackel CL, Sheehy CM, Badger TA. The challenge of detection and management of alcohol abuse among elders. Clinical Nurse Specialist 1994; 8(3): 128-135.
15. Substance Abuse and Mental Health Services Administration (SAMHSA). Get connected: linking older adults with medication, alcohol, and mental health resources. DHHS Pub. No, (SMA) 03-3824. Rockville, MD: Center for Substance Abuse Treatment, Substance Abuse and Mental Health Services Administration, 2003.
16. Benton T, Staab J, Evans DL. Medical co-morbidity in depressive disorders. Annals of Clinical Psychiatry 2007; 19(4): 289-303.
17. Evans DL, Staab JP, Petitto JM, Morrison MF, Szuba MP, Ward HE et al. Depression in the medical setting: biopsychological interactions and treatment considerations. Journal of Clinical Psychiatry 1999; 60(4Suppl): S40-S55.
18. Roberts RE, Kaplan GA, Shema SJ, Strawbridge WJ. Does growing old increase risk for depression? American Journal of Psychiatry 1997; 154: 1384-1390.
19. National Association of State Mental Health Program Directors (NASMHPD). Medical Directors Council. Morbidity and mortality in people with serious mental illness: 13th Technical Report. Alexandra, VA: Medical Directors Council, 2006.
20. Kessler RC, Chiu WT, Demler O, Walters EE. Prevalence, severity, and comorbidity of twelve-month DSM-IV disorders in the National Comorbidity Survey Replication (NCS-R). Archives of General Psychiatry 2005; 62(6): 617-627.
21. Blazer D, Hughes DC, George LK. The epidemiology of depression in an elderly community population. Gerontologist 1987; 27(3): 281-287.
22. Fisher KM, Copenhaver V. Assessing the mental health of rural older adults in public housing facilities: a comparison of screening tools. Journal of Gerontological Nursing 2006; 32(9): 26-33.
23. World Health Organization. Mental health: depression. (Online) 2012. Available: http://www.who.int/mental_health/management/depression/en/index.html (Accessed 31 October 2012).
24. Beekman ATF, Deeg DJH, Braam AW, Smit JH, Van Tilburg W. Consequences of major and minor depression in later life: a study of disability, well-being and service utilization. Psychological Medicine 1997; 27: 1397-1409.
25. Bremmer MA, Hoogendijk WJ, Deeg DJ, Schoevers RA, Schalk BW, Beekman AT. Depression in older age is a risk factor for first ischemic cardiac events. American Journal of Geriatric Psychiatry 2006; 14(6): 523-530.
26. Pennix BWJH, Guralnik JM, Pahor M, Ferrucci L, Cerhan JR, Wallace RB et al. Chronically depressed mood and cancer risk in older persons. Journal of the National Cancer Institute 1998; 90: 1888-1893.
27. Landi F, Onder G, Cesari M, Russo A, Barillaro C, Bernabei R et al. Pain and its relation to depressive symptoms in frail older people living in the community: an observational study. Journal of Pain Symptom Management 2005; 29(3): 255-262.
28. House A, Knapp P, Bamford J, Vail A. Mortality at 2 and 24 months after stroke may be associated with depressive symptoms at 1 month. Stroke 2001; 32: 696-701.
29. Frasure-Smith N, Lesperance F. Depression and other psychological risks following myocardial infarction. Archives of General Psychiatry 2006; 60: 627-636.
30. Begg DJ, Langley JD, Stephenson S. Identifying factors that predict persistent driving after drinking, unsafe driving after drinking, and driving after using cannabis among young adults. Accident Analysis and Prevention 2003; 35: 669-675.
31. Green C, Polen MR. The health and health behaviors of people who do not drink alcohol. American Journal of Preventive Medicine 2001; 21(4): 298-305.
32. Rosal MC, Ockene JK, Hurley TG, Reiff S. Prevalence and co-occurrence of health risk behaviors among high-risk drinkers in a primary care population. Preventive Medicine 2001; 31: 140-147.
33. Urbanoski KA. The use of preventive healthcare by Canadian women who drink alcohol. Preventive Medicine 2003; 37: 334-341.
34. Read JP, Brown RA, Marcus BH, Kahler CW, Ramsey SE, Dubreuil MA et al. Exercise attitudes and behaviors among persons in treatment for alcohol use disorders. Journal of Substance Abuse Treatment 2001; 21: 199-206.
35. Chiu E. Alcohol for the older person--friend or foe? Age and Ageing 2008; 37(5): 505-512.
36. Ferreira MP, Weems MKS. Alcohol consumption by aging adults in the United States: health benefits and detriments. Journal of the American Dietetic Association 2008; 108(10): 1668-1676.
37. Dufour MC, Archer L, Gordis E. Alcohol and the elderly. Clinic in Geriatric Medicine 1992; 8(1): 127-141.
38. Blow FC. Substance abuse among older adults: treatment improvement protocol (TIP) series. Rockville, MD: US Department of Health and Human Services, 2004.
39. Adams W, Yuan Z, Barborial JJ, Rimm AA. Alcohol-related hospitalizations of elderly people. JAMA 1993; 270:1222-1225.
40. Qato DM, Alexander GC, Conti RM, Johnson M, Schumm P, Lindau ST. Use of prescription and over-the-counter medications and dietary supplements among older adults in the United States. JAMA 2008; 300: 2867-2878.
41. Phillips DP, Barker GE, Eguchi MM. A steep increase in domestic fatal medication errors with use of alcohol and/or street drugs. Archives of Internal Medicine 2008; 168(14): 1561-1566.
42. Shannon LM, Havens JR, Mateyoke-Scrivner A, Walker R. Contextual differences in substance use for rural Appalachian treatment-seeking women. American Journal of Drug and Alcohol Abuse 2009; 35(2): 59-62.
43. Dobscha SK, Delucchi K, Young ML. Adherence with referrals for outpatient follow-up from a VA psychiatric emergency room. Community Mental Health Journal 1999; 35(5): 451-458.
44. Kerr EA, McGlynn EA, Adams J, Keesey J, Asch SM. Profiling the quality of care in twelve communities: results from the CQI study. Health Affairs 2004; 23(3): 247-256.
45. Oslin DW, Ross J, Sayers S, Murphy J, Kane V, Katz IR. Screening, assessment, and management of depression in VA primary care clinics: the behavioral health laboratory. Journal of General Internal Medicine 2006; 21(1): 46-50.
46. Stockdale SE, Klap R, Belin TR, Zhang L, Wells KB. Longitudinal patterns of alcohol, drug, and mental health need and care in a national sample of U.S. adults. Psychiatric Services 2006; 57(1): 93-99.
47. Hooyman N, Unutzer J. A perilous arc of supply and demand: how can America meet the multiplying mental health care needs of an aging populace? Generations 2010; 34(4): 36-42.
48. Prochaska TR, Clark MA. Health behaviors and the human lifespan. In: DS Gochman (Ed). Handbook of health behavior research, Vol. 3: Demography, development, and diversity. New York: Plenum, 1997; 29-48.
49. Prohaska TR, Leventhal EA, Leventhal H, Keller ML. Health practices and illness cognition in young, middle aged and elderly adults. Journal of Gerontology 1985; 40(5): 569-578.
50. Ohayon MM. Epidemiology of depression and its treatment in the general population. Journal of Psychiatric Research 2007; 41(3-4): 207-213.
51. Hartley D, Korsen N, Bird D, Agger M. Management of patients with depression by rural primary care practitioners. Archives of Family Medicine 1998; 7(2): 139-145.
52. Rogers EM. Diffusion of innovation, 5th edn. New York: Free Press, 2003.
53. Glasglow N, Morton LW, Johnson NE. Critical issues in rural health. Ames, IO: Blackwell Publishing, 2004.
54. Mainous AG 3rd, Kohrs FP. A comparison of health status between rural and urban adults. Journal of Community Health 1995; 20(5): 423-431.
55. Kruger T, Murray D, Zanjani F. Rural community members' perspectives on mental health and aging: an ecological approach to interpreting and applying focus group results. Journal of Extension 2011; 49(2): 1-11.
56. Kruger T, Murray D, Zanjani F. Mental Healthiness and Aging Initiative: lessons from a social marketing-informed research campaign in Kentucky. Social Marketing Quarterly 2011; 48: 193-201.
57. Zanjani F, Kruger T, Murray D. Evaluation of the Mental Healthiness Aging Initiative: community program to improve awareness about mental health and aging issues. Community Mental Health Journal 2011; 17(3): 18-38.
58. Bartels SJ, Miles KM, Van Citters AD, Forester BP, Cohen MJ, Xie H. Improving mental health assessment and service planning practices for older adults: a controlled comparison study. Mental Health Services Research 2005; 7(4): 213-223.
59. Beyer JL. Managing depression in geriatric populations. Annals of Clinical Psychiatry 2007; 19(4): 221-238.
60. Blazer DG, Steffens DC, Busse EW. The American psychiatric publishing textbook of geriatric psychiatry. Washington, DC: American Psychiatric Publishing, 2004.
61. Blazer DG, Steffens DC. The American psychiatric publishing textbook of geriatric psychiatry, 4th edn. Washington, DC: American Psychiatric Publishing, 2009.
62. Cockerham WC, Kunz G, Lueschen G. Psychological distress, perceived health status, and physician utilization in America and West Germany. Social Science and Medicine 1988; 26(8): 829-838.
63. Fillmore MT, Weafer J. Alcohol impairment of behavior in men and women. Addiction 2004; 99(10): 1237-1246.
64. Lemke S, Moos RH. Treatment and outcomes of older patients with alcohol use disorders in community residential programs. Journal of Studies on Alcohol 2003; 64(2): 219-226.
65. Liberto JG, Oslin DW, Ruskin PE. Alcoholism in older persons: a review of the literature. Hospital Community Psychiatry 1992; 43(10): 975-984.
66. Oslin DW. Late-life alcoholism: issues relevant to the geriatric psychiatrist. American Journal of Geriatric Psychiatry 2004; 12(6): 571-583.
67. Skultety KM, Zeiss A. The treatment of depression in older adults in the primary care setting: an evidence-based review. Health Psychology 2006; 25(6): 665-674.
68. US Preventive Services Task Force. Screening and behavioral counseling interventions in primary care to reduce alcohol misuse: recommendation statement. Annals of Internal Medicine 2004; 140: 554-556.
69. Zanjani F, Oslin D. Substance use and abuse assessment. In: J Gallo, G Paveza, T Fulmer, H. Bogner (Eds). Handbook of geriatric assessment. Frederick, MD: Aspen Publishers, 2006; 175-192.
70. Kachman SD. An introduction to generalized linear mixed models. In: Proceedings, Implementation Strategies For National Beef Cattle Evaluation; 20-21 October 2001; Athens; 59-73.
71. Eack SM, Greeno CG, Christian-Michaels S, Dennis A, Anderson CM. Case managers' perspectives on what they need to do their job. Psychiatric Rehabilitation Journal 2009; 32(4): 309-312.
72. Jelinek GA, Weiland TJ, Mackinlay C, Hill N, Gerdtz MF. Perceived differences in the management of mental health patients in remote and rural Australia and strategies for improvement: findings from a national qualitative study of emergency clinicians. Emergency Medicine International 2011: 965027. (Online) 2011. Available: http://www.hindawi.com/journals/emi/2011/965027/ (Accessed 27 October 2012).
73. Mwape L, Sikwese A, Kapungwe A, Mwanza J, Flisher A, Lund C et al. Integrating mental health into primary health care in Zambia: a care provider's perspective. International Journal of Mental Health Systems 2010; 4: 21.
74. Steele M, Zayed R, Davidson B, Stretch N, Nadeau L, Fleisher W et al. Referral patterns and training needs in psychiatry among primary care physicians in Canadian rural/remote areas. Journal of the Canadian Academy of Child and Adolescent Psychiatry 2012; 21(2): 111-123.
75. Armstrong G, Kermode M, Raja S, Suja S, Chandra P, Jorm AF. A mental health training program for community health workers in India: impact on knowledge and attitudes. International Journal of Mental Health Systems 2010; 5(1): 17.
76. Hossain D, Gorman D, Eley R, Coutts J. Value of mental health first aid training of advisory and extension agents in supporting farmers in rural Queensland. Rural and Remote Health 10: 1593. (Online) 2010. Available: www.rrh.org.au (Accessed 27 October 2012).
77. Pierce D, Liaw ST, Dobell J, Anderson R. Australian rural football club leaders as mental health advocates: an investigation of the impact of the Coach the Coach project. International Journal of Mental Health Systems 2010; 4:10.
78. Church EA, Heath OJ, Curran VR, Bethune C, Callanan TS, Cornish PA. Rural professionals' perceptions of interprofessional continuing education in mental health. Health and Social Care in the Community. 2010; 18(4): 433-443.
79. Ellis IK, Philip T. Improving the skills of rural and remote generalists to manage mental health emergencies. Rural and Remote Health 10: 1503. (Online) 2010. Available: www.rrh.org.au (Accessed 27 October 2012).
80. Unützer J. Diagnosis and treatment of older adults with depression in primary care. Biological Psychiatry 2002; 52(3): 285-292.
81. Goldman LS, Nielsen NH, Champion HC. Awareness, diagnosis, and treatment of depression. Journal of General Internal Medicine 1999; 14(9): 569-580.
82. Fink A, Beck JC, Wittrock MC. Informing older adults about non-hazardous, hazardous, and harmful alcohol use. Patient Education Counseling 2001; 45(2): 133-141.
83. Braitman LE. Statistical estimates and clinical trials. Journal of Biopharmaceutical Statistics 1993; 3(2): 249-256.
84. Cohen J. A power primer. Psychological Bulletin 1992; 112(1): 155-159.
85. Kaiser Family Foundation. Statehealthfacts.org. (Online) no date. Available: www.Statehealthfacts.org (Accessed October 2009.
86. Murray CJ, Kulkarni SC, Michaud C, Tomijima N, Bulzacchelli MT, Iandiorio TJ et al. Eight Americas: investigating mortality disparities across races, counties, and race-counties in the United States. PLoS Medicine 2006; 3(9): e260.

