In recent decades there has been a call to action for the development of quality and safety indicators for pediatric emergency care1,2. The use of best practice knowledge (inclusive of research evidence, clinical judgment and patient information) is key in the delivery of quality care. In a busy pediatric emergency department (ED), the complexity of patient care, focus on patient flow, availability of resources, and the interruptive nature of the practice environment create less than ideal conditions for consistent use of best practice knowledge3. Further challenges exist in smaller rural EDs where workforce skill mix, limited patient volume and acuity (which minimize repetition of procedures such as resuscitation), and limited resources (eg access to continuing education because of clinical coverage or distance) can restrict exposure to best practice knowledge4-6. Recent studies report only 2.4% of Canadian specialist physicians are located in rural and small towns (communities with small populations and geographically distant from urban centers) where 21.1% of the population resides7. Rural EDs, where half of all emergency care in Canada is delivered, rely heavily on family physicians to staff departments8. Over 80% of children are seen in rural EDs5,8. Given rural Canadians have poorer outcomes from acute medical illness and injury, innovative strategies are needed to strengthen access to best practice knowledge in these complex practice environments5,8.
Knowledge exchange is understood to be a two-way flow of ideas, best practice knowledge, and experience between members in a community of practice9,10. In the healthcare literature, knowledge exchange generally focuses on the sharing of research knowledge between researchers and knowledge users (eg clinicians and policy makers)11. A feature common to all perspectives on knowledge exchange is the importance of a social process that involves knowledge sharing between individuals or groups12,13. To date, research focused on knowledge exchange between rural and urban emergency practice settings is limited.
Three key dimensions have been identified across a range of studies as important in knowledge exchange: characteristics of the individual; context of practice; and knowledge. Individual clinicians are the gatekeepers to the flow of knowledge in practice and play a central role in knowledge exchange. Knowledge, skills, attitudes, beliefs and behaviors of individual clinicians influence the extent to which they use and share knowledge14-17. The context in which knowledge is used and shared in health care can influence the development of an evidence-based practice environment18-20. The context of practice in this study is understood to mean the social, cultural, structural and material elements of the setting or environment where emergency practice occurs. Finally, the characteristics of the knowledge (relevance, complexity, availability and compatibility) have implications for its mobility and efficiency in practice21-25. Knowledge in this study is focused on best practice knowledge in pediatric emergency care arising from multiple ways of knowing.
To better understand how these dimensions influence knowledge exchange in rural and urban emergency practice settings, a follow-up survey of emergency clinicians who were invited to participate in a Web-based knowledge exchange intervention, the Pediatric Emergency Care Web Based Knowledge Exchange Project, was conducted. This knowledge exchange intervention was a password-protected website open to clinicians from nine rural and two urban EDs. The website contained 12 pediatric emergency practice learning modules with linked asynchronous discussion forums. The topics for the modules were determined through a needs assessment and module content was developed by known experts in the field. Additional details regarding the website and the primary outcomes of the project are presented elsewhere26,27. This article presents the results of a survey that sought to identify factors relevant to the decision made by rural and urban emergency clinicians to participate in a Web-based knowledge exchange intervention. In the context of this project, knowledge exchange refers to the seeking and sharing of all types of healthcare knowledge for the benefit of clinicians, researchers, administrators, patients and society at large.
Participants and sampling
Study participants (n=187) were clinicians from the 11 EDs who agreed to participate in the Pediatric Emergency Care Web Based Knowledge Exchange Project. This included 32 physicians, 146 nurses and nine pharmacists working in nine rural and two urban EDs in one province in Canada. In the context of this study, rural (regional and community) EDs served a catchment of fewer than 100 000 people. Ten of the 11 EDs had an affiliation with a provincial academic institution. All the departments, with the exception of one, operated 24 hours per day, seven days per week. Six of the 10 had single physician coverage for the evening and night hours and five of the EDs were staffed by family physicians. All study participants had Internet access in their ED.
Survey development
The following questions guided the development of a self-administered survey: (i) What are the individual, context of practice or knowledge factors which impact a clinician's decision to participate in a Web-based knowledge exchange intervention?; (ii) What are clinicians' perceptions of organizational expectations regarding knowledge and information sources to be used in practice?; and (iii) What are the preferred knowledge sources of rural and urban emergency clinicians? The survey was designed to capture data related to the three dimensions of interest in this study (individual, context of practice and knowledge). A minimum of four items were developed for each dimension. Items in the individual dimension captured information about knowledge exchange beliefs, behaviors and activities. Items included under the context of practice dimension explored knowledge exchange structures and processes that were outside the control of the individual clinician. Items included in the knowledge dimension reflected activities and behaviors relevant to the use of Web-based technology for knowledge exchange. Responses were scored on a 4-point Likert scale (1 = strongly disagree, 2 = disagree, 3 = agree, 4 = strongly agree). A panel of five emergency practice content experts (two physicians, three nurses) reviewed the survey for face validity. Minor revisions were made to wording in four survey items based on this expert feedback. Demographic data regarding each participant's age, gender, discipline, years of emergency experience, additional education and certification achieved, computer literacy and practice location were also captured. The two-page survey took approximately 10 minutes to complete.
Survey administration
The Pediatric Emergency Care Web Based Knowledge Exchange Project occurred between February 2004 and December 2005. Data collection for this survey study occurred between January 2006 and March 2006. Surveys were mailed to the study site coordinators at each of the 11 sites for distribution to study participants via the internal health center mailing system. Site coordinators were instructed to send out one reminder email to all participants 2 weeks after the initial distribution. Each survey package included a letter of instruction directing the participant to return the completed survey to the site coordinator in the sealed envelope provided in the survey package. Each site coordinator was provided with a postage paid envelope to return completed surveys to the principal investigator.
Data analysis
Survey item responses were entered in Statistical Package for Social Sciences v15 (SPSS Inc; www.spss.com). Data were checked and cleaned through examination of frequency distributions and crosstabulations to highlight data entry errors, missing data and outliers. Missing data were replaced by item mode when less than 5% of item data was missing. Descriptive statistics (mean, mode, standard deviation and quartile range) and stem-leaf plots were generated for all items. Internal consistency (reliability) of the survey tool was checked using Cronbach's alpha. Chi-squared and Fisher's exact test were used to determine if there was a relationship between individual items in the three dimensions (individual, practice context and knowledge) and the participant's decision to take part in the knowledge sharing intervention. Mann-Whitney U-test was used to determine if there was a difference between rural and urban clinicians' perceptions of organizational expectations regarding knowledge use or preferred sources of knowledge.
Ethics approval
The Institutional Review Boards at all participating IWK Health Centre sites approved the protocol (approval ##3611). Written informed consent was obtained from all participants.
Demographic characteristics
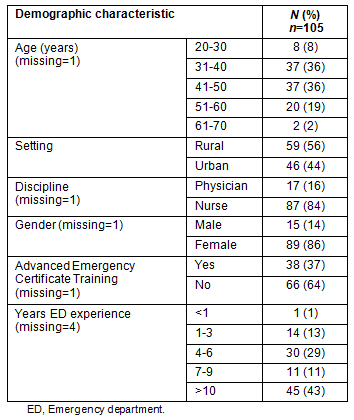
A total of 107 surveys were returned, although two surveys with only demographic sections completed were removed, resulting in a 56% (105/187) return rate. The majority of respondents were nurses (87/104, 84%, one missing) and slightly more than half were from rural settings (59/105, 56%) (Table 1). This distribution is similar to the demographic distribution of the sampling frame (n=187, 17% physicians, 42% urban). Seventy-four percent of respondents were between the ages of 31 and 50 years. The majority of respondents (63/104, 61%) did not have emergency certification in nursing or medicine and 43% of respondents had greater than 10 years of experience in emergency practice.
Table 1: Demographic characteristics of survey respondents
The reliability of the 23 item scale was strong (Cronbach's α= 0.841). The subscales, as planned during survey development, also demonstrated good or strong internal consistency (context of practice, α=0.755; individual, α=0.693; knowledge, α=0.786).
Resource use
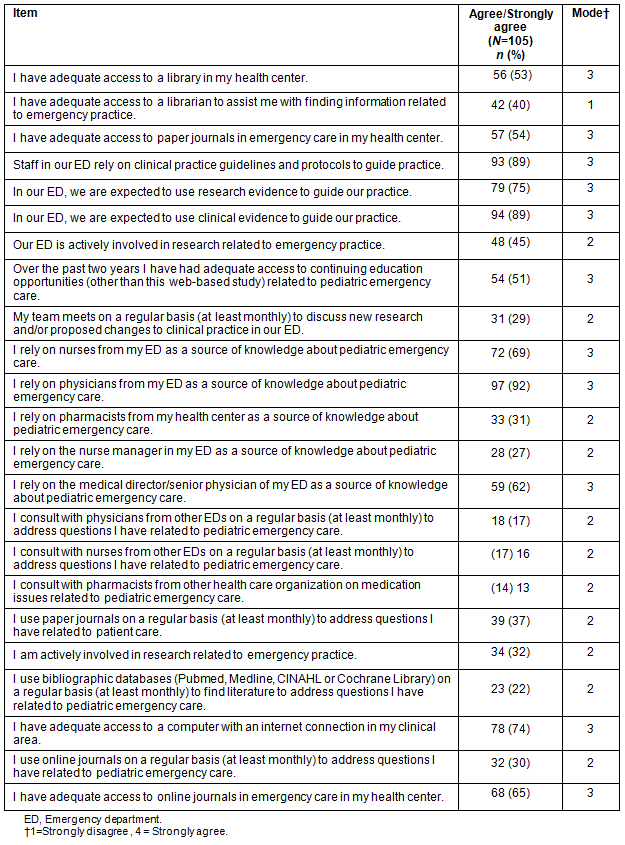
The majority of respondents reported adequate access to a number of explicit (text-based) knowledge sources but access to a librarian to assist with using these resources was limited (Table 2). More than 50% of respondents reported adequate access to paper journals (57/105 or 54%) and online journals (68/105 or 65%), but less than half reported using these resources to address questions arising in practice (paper journals, 37%; online journals, 30%). Participants reported relying on physicians (92%) and nurses (69%) from their own ED as primary sources of knowledge about pediatric emergency care. There was limited (nurses, 16%; physicians, 17%; pharmacists, 13%) consultation with clinical experts from other EDs as a source of knowledge to guide practice. In addition to personal sources of knowledge from their own department, participants also reported relying on clinical practice guidelines to guide practice (93/105 or 89%). Expectations regarding the use of knowledge from both research evidence (79/105 or 75%) and clinical experience (94/105 or 89%) to guide practice were also reported by the majority of respondents.
Table 2: Survey items' descriptive statistics
Individual survey item scores were then dichotomized and χ2 was used to explore the relationship between individual survey items and the outcome variable (participation). There was a relationship between participation in the knowledge exchange intervention and two items in the individual dimension (I consult with nurses outside of my ED, I am actively involved in research) and one item from the context dimension (In our ED we are expected to use research to guide practice) (Table 3).
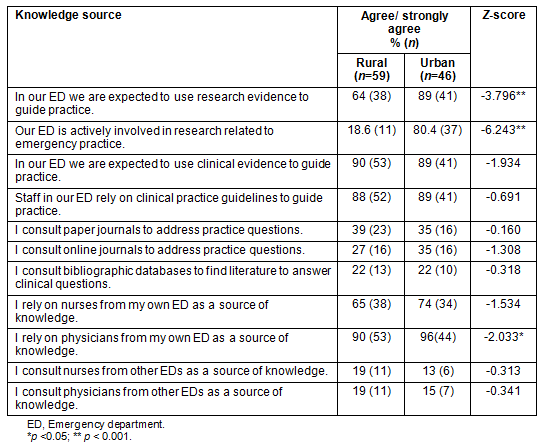
A comparison of rural and urban clinicians' preferred knowledge sources reveals that clinicians are generally similar with the exception of the use of research to guide practice and reliance on physicians as a source of clinical practice knowledge (Table 4). A significantly larger percentage of urban clinicians indicated that they use research evidence to guide practice and they rely on physicians in their own ED to guide practice.
Table 3: Relationship between survey items and participation in Web innovation
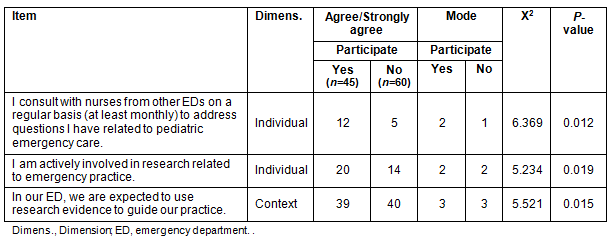
Table 4: Comparison of rural and urban clinicians' preferred knowledge sources
Discussion
Individual, context of practice and knowledge factors affecting participation
Less than half (43%) of the survey respondents participated in the Web-based knowledge exchange intervention, which was intended to link clinicians from rural and urban EDs to share knowledge related to pediatric emergency care. Review of the survey items would suggest that survey respondents rely heavily on peers (nurses 69% and physicians 92%) from their own ED for knowledge to guide their practice and are less inclined to use personal sources from other EDs or explicit sources such as paper journals or online journals. These results are similar to study findings from other practice settings28-30. The sharing of expert practice knowledge through discussion of exceptional or rare presentations by ED clinicians has the potential to become valued propositional knowledge through a process of debate, discussion and verification of the evidence by the community of practitioners who participate. However, the value of this type of knowledge exchange is limited in EDs where there are few clinicians with advanced emergency training and inadequate use of explicit knowledge sources.
Geographical boundaries have been shown to influence the social networks of nurses and physicians31. The Web-based knowledge exchange intervention was intended to minimize geographical boundaries and provide participants with an opportunity to engage in discussion with clinicians from outside of their own ED. In an earlier paper comparing emergency clinicians' online and offline knowledge exchange behaviors, a social network analysis revealed a significantly higher number of knowledge exchange opportunities in an online environment26. In the present study, the practice of consulting personal knowledge sources from other EDs (individual dimension) was found to be significantly related to decision to participate in the Web-based knowledge exchange intervention (χ2=6.369, p=0.012). Linkages between EDs are important for the exchange of new knowledge. Weak ties between groups (groups that have some connection but do not spend a lot of time together) have been identified as important for spreading new ideas and scientific information32. Although most weak ties serve no function, they can serve as a crucial bridge between different densely knit networks and allow novel ideas and new information to be introduced33. Emergency departments with few or no weak ties will be deprived of knowledge from other rural or urban centers. While the Web-based knowledge exchange intervention created the opportunity for clinicians to share information, additional strategies may have been needed to formally establish ties between EDs to start the flow of knowledge exchange.
Two other items that were found to be significantly related to participation in the Web-based knowledge exchange intervention were personal involvement in research activities (individual dimension) (χ2=5.234, p=0.019) and perception of organizational expectation to use research evidence to guide practice (context dimension) (χ2=5.521, p=0.015). Participation in research activities has been associated with research use in practice34,35. Less than half of survey respondents indicated they were personally involved in research or that their ED was involved in research. It is possible that a lack of exposure to or experience with research initiatives may have contributed to the moderate participation rate in this knowledge exchange intervention. The Web-based intervention provided clinicians with exposure to best practice knowledge through pediatric emergency specific learning modules and a discussion forum. Clinicians have demonstrated a willingness to use online evidence at the point of care to fill in gaps in their practice knowledge; however, adequate training and supportive leadership have been identified as important factors in optimizing the process36,37. Overt strategic initiatives and support from management are necessary to permeate the boundaries that inhibit the development of social relationships and consequently knowledge sharing between communities38. Organizational expectations regarding the use of research evidence to guide practice was related to participation in the knowledge exchange intervention in the current study. Engaging ED policymaker/administrative stakeholders in setting research priorities may assist with participation in future knowledge exchange interventions39.
Practitioners' perceptions of organizational expectations regarding use of knowledge
Organizational context has been identified as an important factor in knowledge exchange and best practice30,40. Overall, 75% of survey respondents reported that they were expected to use knowledge from a variety of sources (clinical practice guidelines, research evidence and clinical evidence) to guide their practice. Yet, only 37% reported using paper journals, 30% reported using online journals and 22% reported using bibliographic databases on a regular basis. In addition, only 43% chose to participate in a knowledge exchange intervention that presented best practice knowledge relevant to rural and urban emergency practice settings. Intraorganizational and interorganizational networks that have been established around a common practice are useful for spreading knowledge among practitioners41. Collaborative technologies such as electronic discussion boards have been shown to facilitate knowledge sharing among time-challenged and geographically dispersed rural and urban practitioners42. However, there is a pressing need for organizations to identify strategies and processes that support and encourage individuals to openly and freely share their practice knowledge43.
There was a significant difference (p<0.001; Z=-3.796) between rural and urban clinicians' perceptions of organizational expectations regarding use of research evidence to guide practice. This difference may have been due to the lower volume of research activities in rural settings. Recent initiatives demonstrate new opportunities for community EDs to participate in research activities44. For example, Translating Emergency Knowledge for Kids is a Canadian knowledge mobilization initiative that is building capacity through partnerships and exchange among 30 general emergency departments across Canada and members of Pediatric Emergency Research Canada (PERC), Pediatric Emergency Research Networks (PERN, an international collaborative) and Knowledge Translation Canada44. Practice contexts that embody characteristics of a learning organization have been identified as important in the literature on knowledge exchange in healthcare environments45. Activities such as journal clubs, regular team meetings or an active program of research create opportunities to discuss knowledge in the context of local practice and are reflective of a practice culture that values knowledge. Organizations need to demonstrate their value and commitment to knowledge exchange through formal structures and process. According to survey participants, structures to support seeking and sharing of explicit or external knowledge sources were limited. Only 29% of respondents indicated opportunities to participate in discussion about new research or proposed practice change in their ED and 60% felt that they did not have adequate access to a librarian to assist with finding new information related to their practice. Less than half (45%) of survey respondents indicated that their ED was actively involved in research. Clinicians recognize the importance of best evidence to guide practice; however, a lack of organizational infrastructure and resources to support knowledge sharing activities may influence clinicians' willingness to engage in a knowledge exchange intervention.
Preferred knowledge sources of rural and urban practitioners
Published studies exploring the information needs of health professionals suggest that rural health practitioners have the same patient-care information needs as their urban counterparts46. In general, rural and urban emergency clinicians in this study presented a similar preference pattern for knowledge resources: although external colleague sources were the least likely to be used, internal colleague sources, particularly physician sources, from their own ED were the most highly used resource. Tapping into organizational knowledge stored in social networks for decision making is well described in the organizational learning literature47. Explicit sources in the form of bibliographic databases and paper and online journals were used minimally in both rural and urban settings; however, clinical practice guidelines were identified as a valuable explicit source for both groups. This pattern is similar to that shown in other studies exploring knowledge sources of rural and urban clinicians48; that is, peers or colleagues are more highly valued knowledge sources than explicit, text-based sources49. However, the current study contributes new information regarding personal knowledge sources of rural and urban EDs. It is known that smaller rural centers have limited expert personal sources of knowledge50. In many smaller EDs family practice clinicians, with little or no formal emergency specialty training, provide medical coverage for emergency services and may not actually be onsite 24 hours per day. This may account for the significant difference (p<0.05; Z = -2.033) between the two groups in their reliance on physicians as a source of knowledge. In addition, results from the current study reveal that the use of personal sources of knowledge from other EDs to guide practice was limited. This suggests the flow of new knowledge between EDs may be limited and is an important knowledge exchange gap for under-resourced, smaller EDs. The Web-based knowledge sharing intervention in this study was intended to bridge geographically dispersed EDs and connect smaller communities of practice for knowledge exchange. There is a need to identify strategies to enhance the use of this resource.
A significantly greater (p<0.001; Z = -3.796) number of urban clinicians reported use of research evidence to guide practice compared to their rural counterparts. This is an interesting finding considering both groups have similar patterns in their use of explicit knowledge sources. However, the difference may be attributed to the significantly higher volume of research activities reported in the urban centers (p<0.001; Z = -6.243) versus the rural centers. This finding would support the notion that participation in research activities is associated with research use in practice35.
Limitations
There are several limitations of this work that require consideration. This study was based on self-report measures, which are subject to bias51. Responder bias could not be ascertained due to limitations of the demographic data collected. Although the survey was pilot tested for face and content validity, it requires further psychometric evaluation.
Multiple comparison adjustments were not made during data analysis. However, it has been argued that adjustments are not necessary when there is a strong basis for expecting a difference in groups52. Differences in the availability of resources in rural and urban settings are well documented in the emergency practice literature; therefore, there was a prior expectation for finding a difference in resource use. Although physician-double coverage in rural EDs is limited, particularly on evenings and weekends, this data was not collected. It is possible double-coverage could have affected physicians' consultation rate with outside ED clinicians. Finally, although the survey showed good reliability, it will benefit from further testing with a larger sample size and adjustment for multiple comparisons.
Regional support and additional educational resources are important for the recruitment and retention of rural clinicians53. Creating opportunities for knowledge exchange and enhancing research capacity is important for a number of reasons, including the potential for improving effectiveness and efficiencies in care towards optimizing patient outcomes. The study results revealed that participation in a knowledge exchange intervention was related to consultation with colleagues from other EDs, personal involvement in research activities and organizational expectation for the use of research evidence to guide clinical practice. Rural and urban clinicians in this study presented a similar preference pattern for particular knowledge resources, although they differed in their perceived organizational expectations for using research evidence to guide practice. External personal sources were the least likely to be used and personal sources from their own ED were the most highly used resource. Explicit sources in the form of bibliographic databases and paper and online journals were used minimally in both rural and urban settings. Overall, the majority of respondents identified organizational expectations to use multiple types of knowledge (clinical practice guidelines, research evidence and clinical evidence) to guide practice. The three dimensions (individual, context of practice and knowledge) provided a practical framework for the development of an evaluation survey for the Pediatric Emergency Care Web Based Knowledge Exchange Project. Results from this survey may provide useful information for emergency practice educators, researchers and administrators interested in facilitating Web-based knowledge exchange within and between rural and urban emergency practice settings.
References
1. Alessandrini E, Varadarajan K, Alpern ER, Gorelick MH, Shaw K, Ruddy RM et al. Emergency department quality: an analysis of existing pediatric measures. Academic Emergency Medicine 2011; 18(5): 519-526.
2. Institute of Medicine, Committee on the Future of Emergency Care in the United States Health System. Emergency care for children. Washington, DC: National Academic, 2007; 338.
3. American Academy of Pediatrics, Committee on Pediatric Emergency Medicine, American College of Emergency Physicians, Pediatric Committee. Care of children in the emergency department: guidelines for preparedness. Pediatrics 2001; 107(4): 777-781.
4. Wadman MC, Muelleman RL, Hall D, Tran TP, Walker RA. Qualification discrepancies between urban and rural emergency department physicians. Journal of Emergency Medicine 2005; 28(3): 273-276.
5. CAEP Working Group on the Future of Emergency Medicine in Canada. The future of emergency medicine in Canada: submission from CAEP to the Romanow Commission. Part 1. Canadian Journal of Emergency Medical Care 2002; 4(5): 359-368.
6. Simon HK, Sullivan F. Confidence in performance of pediatric emergency medicine procedures by community emergency practitioners. Pediatric Emergency Care 1996; 12(5): 336-339.
7. Pong R, Pitblado J. Geographic distribution of physicians in Canada: beyond how many and where. Ottawa, ON: Canadian Institute for Health Information, 2005.
8. CAEP Working Group on the Future of Emergency Medicine in Canada. The future of emergency medicine in Canada: submission from CAEP to the Romanow Commission. Part 2. Canadian Journal of Emergency Medical Care 2002; 4(6): 431-438.
9. Thomas-Hunt MC, Ogden TY, Neale MA. Who's really sharing? Effects of social and expert status on knowledge exchange within groups. Management Science 2003; 49(4): 464-477.
10. Herschel R, Nemati H, Steiger D. Tacit to explicit knowledge conversion: knowledge exchange protocols. Journal of Knowledge Management 2001; 5(1): 107-116.
11. Mitton C, Adair CE, McKenzie E, Patten SB, Waye Perry B. Knowledge transfer and exchange: review and synthesis of the literature. Milbank Quarterly 2007; 85(4): 729-768.
12. Molm LD. Theories of social exchange and exchange networks. In: G Ritzer, B Smart (Eds). Handbook of social learning theory. London: Sage, 2001.
13. Rycroft-Malone J. The PARIHS framework - a framework for guiding the implementation of evidence-based practice. Journal of Nursing Care Quality 2004; 19(4): 297-304.
14. Barta KM. Information-seeking, research utilization, and barriers to research utilization of pediatric nurse educators. Journal of Professional Nursing 1995; 11(1): 49-57.
15. Nagy S, Lumby J, McKinley S, Macfarlane C. Nurses' beliefs about the conditions that hinder or support evidence-based nursing. International Journal of Nursing Practice 2001; 7(5): 314-321.
16. McCaughan D, Thompson C, Cullum N, Sheldon TA, Thompson DR. Acute care nurses' perceptions of barriers to using research information in clinical decision-making. Journal of Advanced Nursing 2002; 39(1): 46-60.
17. Koehn ML, Lehman K. Nurses' perceptions of evidence-based nursing practice. Journal of Advanced Nursing 2008; 62(2): 209-215.
18. McCormack B, Kitson A, Harvey G, Rycroft-Malone J, Titchen A, Seers K. Getting evidence into practice: the meaning of 'context'. Journal of Advanced Nursing 2002; 38(1): 94-104.
19. Titler MG. Translation science and context. Research and Theory for Nursing Practice 2010; 24(1): 35-55.
20. Cummings GG, Estabrooks CA, Midodzi WK, Wallin L, Hayduk L. Influence of organizational characteristics and context on research utilization. Nursing Research 2007; 56(4Suppl): S24-S39.
21. Royle J, Blythe J. Promoting research utilisation in nursing: the role of the individual, organisation, and environment. Evidence Based Nursing 1998; 1(3): 71-72.
22. Powell CV. How to implement change in clinical practice. Paediatric Respiratory Reviews 2003; 4(4): 340-346.
23. Sudsawad P. A conceptual framework to increase usability of outcome research for evidence-based practice. American Journal of Occupational Therapy 2005; 59(3): 351-355.
24. Mickan S, Askew D. What sort of evidence do we need in primary care? BMJ 2006; 332(7542): 619-620.
25. Rowe BH, Diner B, Camargo CA Jr, Worster A, Colacone A, Wyer PC et al. Effective synthesized/preappraised evidence formats in emergency medicine and the use of supplemental knowledge translation techniques. Academic Emergency Medicine 2007; 14(11): 1023-1029.
26. Curran JA, Abidi SS. Evaluation of an online discussion forum for emergency practitioners. Health Informatics Journal 2007; 13(4): 255-266.
27. Curran JA, Murphy AL, Sinclair D, Best S. Use of an online learning environment to support best practice in rural and urban emergency departments in Nova Scotia. Canadian Journal of Emergency Medicine 2006; 8(3): 387.
28. Gerrish K, Clayton J. Promoting evidence-based practice: an organizational approach. Journal of Nursing Management 2004; 12(2): 114-123.
29. Estabrooks CA, Chong H, Brigidear K, Profetto-McGrath J. Profiling Canadian nurses' preferred knowledge sources for clinical practice. Canadian Journal of Nursing Research 2005; 37(2): 118-140.
30. Bennett NL, Casebeer LL, Zheng S, Kristofco R. Information-seeking behaviors and reflective practice. Journal of Continuing Education in the Health Professions 2006; 26(2): 120-127.
31. West E, Barron DN. Social and geographical boundaries around senior nurse and physician leaders: an application of social network analysis. Canadian Journal of Nursing Research 2005; 37(3): 132-148.
32. Granovetter M. The strength of weak ties: a network theory revisited. Sociological Theory 1983; 1: 201-233.
33. Nelson R. The strength of strong ties: social networks and intergroup conflict in orgnaizations. Academy of Management Journal 1989; 32(2): 377-401.
34. Bostrom J, Suter WM. Research utilization: making the link to practice. Journal of Nursing Staff Development 1993; 42: 364-372.
35. McCleary L, Brown GT. Barriers to paediatric nurses' research utilization. Journal of Advanced Nursing 2003; 42(4): 364-372.
36. Prendiville TW, Saunders J, Fitzsimons J. The information-seeking behaviour of paediatricians accessing web-based resources. Archives of Disease in Childhood 2009; 94(8): 633-635.
37. Gosling AS, Westbrook JI. Allied health professionals' use of online evidence: a survey of 790 staff working in the Australian public hospital system. International Journal of Medical Informatics 2004; 73(4): 391-401.
38. Cross R, Liedtka J, Weiss L. A practical guide to social networks. Harvard Business Review 2005; 83(3): 124-132.
39. Smith N, Mitton C, Peacock S, Cornelissen E, MacLeod S. Identifying research priorities for health care priority setting: a collaborative effort between managers and researchers. BMC Health Services Research 2009; 9: 165.
40. Kitson A, Harvey G, McCormack B. Enabling the implementation of evidence based practice: a conceptual framework. Quality in Health Care 1998; 7(3): 149-158.
41. Brown J, Duguid P. Knowledge and organization: a social-practice perspective. Organization Science 2001; 12: 198-213.
42. Curran JA, Murphy AL, Abidi SS, Sinclair D, McGrath PJ. Bridging the gap: knowledge seeking and sharing in a virtual community of emergency practice. Evaluation & the Health Professions 2009; 32(3): 312-325.
43. Hall H. Social exchange for knowledge exchange. In: Proceedings, Managing Knowledge: Conversations and Critiques; 10-11 April 2001. University of Leicester Management Centre, Leicester, UK; 2001.
44. TREKK: Translating Emergency Knowledge for Kids. Translating emergency knowledge for kids. (Online) 2012. Available: http://trekk.ca (Accessed 29 March 2012).
45. Chunharas S. An interactive integrative approach to translating knowledge and building a 'learning organization' in health services management. Bulletin of the World Health Organization 2006; 84(8): 652-657.
46. Dorsch JL. Information needs of rural health professionals: a review of the literature. Bulletin of the Medical Library Association 2000; 88(4): 346-354.
47. Olivera F. Memory systems in organizations: an empirical investigation of mechanisms for knowledge collection, storage and access. Journal of Management Studies 2000; 37: 811-832.
48. Gorman PN, Yao P, Seshadri V. Finding the answers in primary care: information seeking by rural and nonrural clinicians. Studies in Health Technology and Informatics 2004; 107(Part 2): 1133-1137.
49. Coleman J, Menzel H, Katz E. Social processes in physicians' adoption of a new drug. Journal of Chronic Diseases 1959; 9(1): 1-19.
50. Canadian Association of Emergency Physicians (CAEP) Working Group. Canadian Association of Emergency Physicians (CAEP) Working Group on the Future of Emergency Medicine in Canada. Emergency medicine: change and challenge. Ottawa, ON: CAEP, 2001.
51. Adams AS, Soumerai SB, Lomas J, Ross-Degnan D. Evidence of self-report bias in assessing adherence to guidelines. International Journal for Quality in Health Care 1999; 11(3): 187-192.
52. Rothman KJ. No adjustments are needed for multiple comparisons. Epidemiology 1990; 1(1): 43-46.
53. Rourke J. Increasing the number of rural physicians. Canadian Medical Association Journal 2008; 178(3): 322-325.



