full article:
There is a shortage of family physicians in Canada. In 2011, 16.8% of Canadians over the age of 15 reported difficulties accessing routine or ongoing health care1. In Canada, such care is provided by family physicians and general practitioners with most specialists, including those in internal medicine, paediatrics and obstetrics/gynaecology working on a referral or consultation basis2.
In the context of an overall shortage of family physicians, there are communities that have chronic difficulties with recruitment and retention including those in the inner city, the north and rural parts of the country3-5. Canada is not alone. Within the past 10 years, both the United States General Accounting Office and Rural Health Workforce Australia have reported that, despite an increase in number of physicians per head of population, the disparity between metropolitan and non-metropolitan areas persisted6,7. The study to be reported here compares the eventual practice location of family physicians who undertook their postgraduate training in metropolitan and non-metropolitan communities.
In addition to financial incentives, regulatory and professional support strategies, a number of educational interventions have been suggested to increase recruitment and retention to medically underserved communities. Students who come from a rural background are more likely to select generalist specialties, including family medicine8, and plan rural practices8-11. Nevertheless, the majority of rural physicians continue to come from urban areas12. Rural practice location can be encouraged by providing clinical experiences in rural communities during both undergraduate13,14 and postgraduate training15-18. Trainees who have participated in a rural preceptorship or rural stream of training felt that rural exposure had an influence on their decision to enter rural practices17,19 and other studies have shown that graduates of rural programs enter rural practice more frequently than graduates in general15,16. While concluding that six or more months of rural postgraduate training was strongly associated with eventual rural practice, Rourke et al questioned a self-selection bias, with those planning a rural or small town practice seeking out longer rural rotations20. As many studies failed to control for other predictors of rural practice and few have examined long term retention, the effect of rural exposure on rural recruitment and retention has been inconclusive in comprehensive reviews21-23.
The University of British Columbia (UBC) is home to the only Faculty of Medicine in British Columbia (BC) Canada, a province of roughly 4.1 million people. The population of BC is concentrated in the south with metropolitan Vancouver constituting half the total provincial population (Fig1). Although definitions vary, roughly 60% of British Columbians live in large urban centers, 20% in small and medium communities, and 20% in rural areas24.
The UBC Department of Family Practice provides a 2-year postgraduate training program accredited by the College of Family Physicians of Canada (CFPC). The program is delivered at a number of sites, each with unique characteristics and particular learning opportunities. Six sites have been established for more than 15 years and are the subject of the current study: two in Metro Vancouver (St Paul's and Greater Vancouver), one each in three regional settings and a rural program that places residents with preceptors in over 30 small, rural and remote communities25. Of the regional sites, Victoria is a city of 300 000, capital of the province and located on Vancouver Island connected to Metro Vancouver by frequent ferry and air service. Chilliwack and Prince George are communities of approximately 70 000 each. While Chilliwack is located a 2-hour drive from the university, Prince George is in the less populous northern part of the province. The metropolitan sites offer core training in tertiary referral and university teaching hospitals whereas the distributed sites and rural program offer core training in regional hospitals. All trainees are required to spend at least 8 weeks in a rural family practice setting and trainees from the distributed sites can spend elective time in the university setting ('reverse distribution'). Curricular differences between sites reflect both the nature of medical practice in the different communities and the different needs of trainees preparing for rural versus urban practice. For example, trainees in distributed sites received more consistent exposure to procedural skills and minor surgeries undertaken by primary care preceptors whereas these were not always emphasized or available in urban training.
Prospective trainees select and rank individual UBC training sites through the Canadian Resident Matching Service (CaRMS) taking into account their specific preferences including location, scheduling, curriculum delivery, and site-specific opportunities. They are advised not to rank sites to which they do not wish to be matched. Applicants are then ranked by the program based on their scores on interviews and file reviews using standardized criteria. Finally, site and trainee rankings are matched by CaRMS using an algorithm that favors the preferences and goals of the trainee.
In 1996 Whiteside and Mathias reported that 51% of graduates of the rural program were practicing in rural areas and 20.5% in regional settings26. These results were descriptive, neither comparing outcomes with other programs nor taking into account other predictors or prior interest in rural practice. The current study uses survey data collected from 20 years of graduates to identify personal and educational factors in postgraduate family medicine training that predict or influence future practice location, specifically whether participation in a rural or regional training site increases recruitment to and retention in rural and regional practice. While this has been demonstrated in previous reports15-18, only the current study has been able to take into account other factors that might predispose residents to choosing a distributed stream of training, such as rural background or rural undergraduate training.
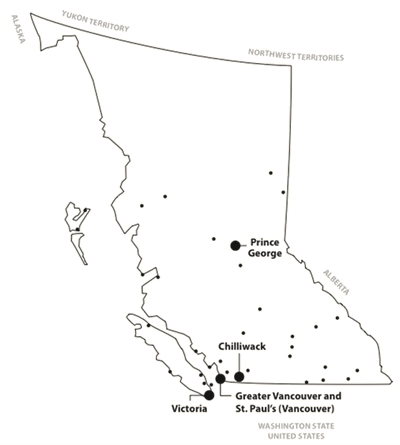
Figure 1: Map of British Columbia showing location of training sites.
Small communities used for the rural 'site' are indicated by small dots.
Beginning in 2000, the Department of Family Practice at UBC has conducted an annual survey of its residents at 2, 5, and 10 years after completion of training as part of ongoing program evaluation. A master file of all graduates, with unique identifiers, is maintained by the Department of Family Practice postgraduate program. This is updated using the Canadian Medical Directory and College of Physicians and Surgeons of BC Directory. The survey instrument (an eight-page questionnaire) and self-addressed stamped envelope are sent to graduates at 2, 5, and 10 years after completion of training by postgraduate program administration. There is a follow-up mailing at 6-8 weeks. Collection remains open for approximately 4-5 months, until a response rate of at least 40% has been achieved. The data is anonymized and entered into a database file. The current study made secondary use of this extensive dataset.
The survey instrument was based on previously validated questionnaires26-29 with some minor modifications over time. The survey at 2 years is most comprehensive, with background information including gender, age at graduation, status of student loans and prior experience in rural settings such as rural upbringing and rural undergraduate training. All surveys ask about current practice and recent professional activities, reasons for choosing practice location and both professional and personal satisfaction. Respondents were asked to rate their level of preparedness for practice in a number of areas on a four-point Likert scale and overall level of preparedness on a scale of 0-100.
Respondents were also asked to designate their location of practice both by size of community and by a description of the primary population served: inner city, urban, regional center (small city with high access to specialists) and rural/small town (population under 10 000 with primarily family physician care). These categories were chosen to be consistent with those used in a periodic national physician survey29. In post-hoc analysis, rural upbringing was defined as having spent at least 1 year in a rural or regional center as a child, teenager or young adult; the number of months in rural undergraduate training was classified as 0, 1-2, or 3+ months; and retention was defined as those who had been practicing in their current community for more than 1 year.
Ten years of cumulative data from the graduation cohorts of 1998 to 2007 (2-year), 1995-2004 (5-year) and 1990-1999 (10-year) inclusive was obtained and entered using the Statistical Package for the Social Sciences software v18,19 (SPSS; http://www.spss.com) for analysis. For each dataset, cross-tabulations were used to determine a relationship between site of training and location of practice. For the 2-year data, cross-tabulations were also used to identify relationships between site of training, location of practice, and other predictor variables for rural practice: age, gender, rural upbringing and rural undergraduate training. Binary logistic regression was then used to establish a stepwise prediction model for rural/regional practice. This was confirmed using classification tree analysis. Independent samples t-test compared overall preparedness for practice amongst those trained in distributed and metropolitan-based sites.
Ethics approval
The study received approval from the UBC Behavioural Ethics Review Board; ethics approval number H09-03281.
Response rate
Between 1990 and 2007, the Department of Family Practice graduated 851 residents, of which 477 were women and 374 men. A total of 649 responses were received from 480 individuals. Nineteen respondents completed the survey at all three time points and 131 provided responses for at least two time points. Although the 5- and 10-year surveys were not sent one year, the overall response rate was 45%, varying from 43% for the 5-year survey to 47% at 2 years. Respondents were excluded from analysis if they were not currently practicing as a family physician or were in the military.
There was no difference in response rate by site or year of graduation; however, in the 2-year group, women were more likely to respond (n=268, χ2=4.66, degrees of freedom (df)=1, p=0.031) and, following exclusions, were significantly more likely to be included in the analysis for recruitment (n=222, χ2=9.53, df=1, p=0.002) and retention (n=171, χ2=11.49, df=1, p=0.0007).
Demographics
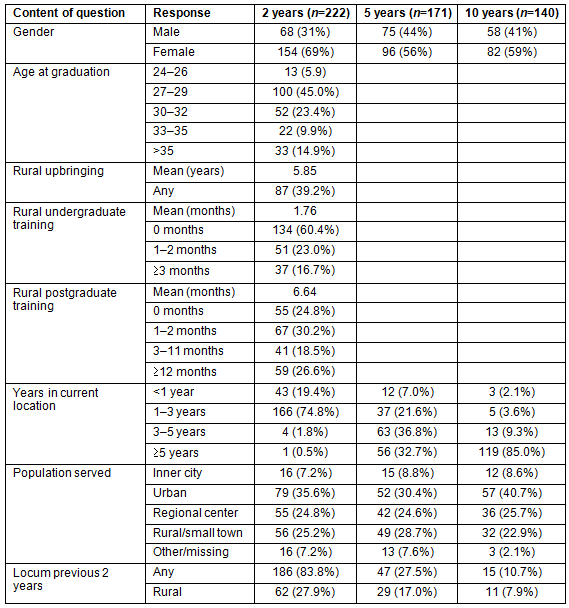
Other than gender, for which information is available for all respondents, additional background information was requested only from the respondents to the 2-year survey. The greatest number were 27-29 years of age at graduation, with 6% under 27 and 15% over 35. Only 40% had any rural upbringing (range 0-19 years, mean 5.8 years, standard deviation (SD) 8.1) or any rural undergraduate training (range 0-48 months, mean 1.8 months, SD 4.8). Three-quarters had some rural postgraduate training, even those in the metropolitan streams (range 0-24 months, mean 6.64, median 2, SD 8.4; Table 1).
Table 1: Demographics, background and professional practice location of all respondents
Professional activities and practice location
At 2, 5, and 10 years after completion of training, graduates were serving a variety of practice populations. In all three cohorts, the most common description for the primary practice population was 'urban'; however, more than half of all graduates described their practice setting as either 'rural/small town' or 'regional center'. The number serving an inner city population was consistent (7-9%) but small. For statistical analysis, this group was combined with the 'urban' practice population.
Most respondents have stayed in the same community for at least 1 year, doing locums, working in walk-in or other clinics or having established a permanent practice. At 2 years post-graduation, almost 84% had done some locums in the preceding 2 years, decreasing to 27.5% at the 5-year survey and 11% at 10 years. The percentage doing locum work in rural areas also decreased (28%, 17%, and 8% respectively); however, the proportion doing rural locum work as a percentage of all locums increased over time from 33% at 2 years to 62% at 5 years to 74% at 10 years.
Predictors of practice location
In bivariate analysis, site of training was correlated with practice location/population served, with those training in the Metro Vancouver based sites more likely to serve an urban or inner city population and those in the distributed sites more likely to serve a regional or rural population (Fig2). When regional and rural practice populations are combined, the relationship between training site and practice location is even more pronounced (Fig3). This relationship persists at 5 and 10 years after graduation (χ2=31 and 33 respectively, df=1, p<0.001). Using the 2-year cohort, the relationships between both practice location and choice of training site and other variables thought or previously shown to predict rural practice location - age, gender, rural upbringing and rural undergraduate training - were examined. Men were more likely to choose a rural practice site (χ2=8.26, df=1, p=0.004). People with at least 1 year of rural or regional upbringing were more likely to choose a distributed postgraduate training site (χ2=5.86, df=1, p=0.015) but this was only weakly associated with practice in a rural or regional setting (χ2=3.31, df=1, p=0.069).
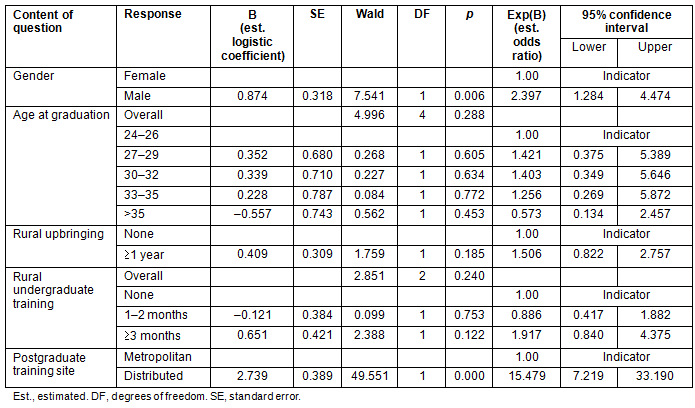
Binomial logistic regression was used to look at the interaction between variables and develop a predictive model for rural or regional practice. Variables were entered in a stepwise manner with a cut-off value of 0.5. Residents who participated in a distributed training site were 15 times more likely to enter regional or rural practice (Table 2). Among the retention subgroup who remained in a single practice location for more than 1 year prior to survey, those who trained in smaller sites were 36 times more likely to choose a rural or regional practice setting than those trained in metropolitan sites (95% confidence interval (CI) 12.2-108.5). Men were more likely to work in regional or rural locations although this effect was less pronounced for longer term retention.
Finally, decision tree analysis was used to distinguish between subgroups. Overall, the most important distinguishing characteristic or predictor variable is site of postgraduate training (χ2=66.86, df=1, p<0.001). Although the vast majority of those who trained in a metropolitan site had urban practice locations, a subgroup of those with some rural upbringing were more likely to practice in rural or regional settings. (χ2=7.98, df=1, p=0.005). For those who trained in distributed sites, gender is a more reliable predictor with men more likely to practice in rural/regional settings (χ2=5.23, df=1, p=0.022).
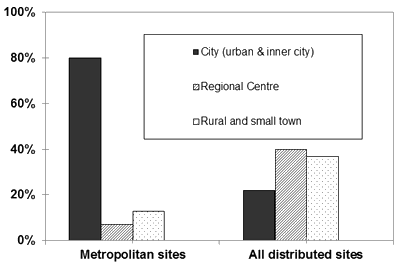
Figure 2: Practice location (percentage of graduates) at 2 years post-graduation
by site of training, metropolitan sites combined; distributed sites combined.
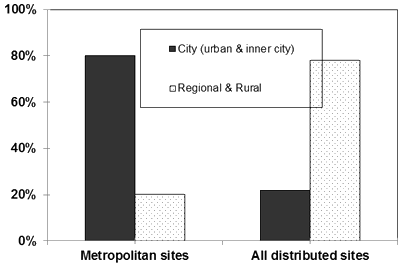
Figure 3: Practice location (percentage of graduates) at 2 years post-graduation by site of training.
Metropolitan sites combined; distributed sites combined. Those training in distributed sites were
significantly more likely to have rural or regional practice settings.
Table 2: Multiple logistic regression. Variables were introduces in a stepwise manner with a cut-off value of 0.5. Location of
postgraduate training is most predictive of professional practice location with those from distributed sites 15 times as likely to enter
rural or regional practice. Males are 2.4 times as likely to enter rural or regional practice. No other variables reach significance in this model.
Career decision-making and preparedness for practice
Using a Likert scale, with 1 being least important and 5 being most important, respondents were asked to rate reasons for their current practice location: interesting medicine, lifestyle for family, professional lifestyle, preparedness and residency experience, financial considerations, spousal work or education requirement and life experience in this setting. At 2, 5, and 10 years the most important of these seven reasons given were related to lifestyle, both professionally and for family, with residency experience consistently rated fifth most important. There were no significant differences between those choosing urban rather than regional or rural practice.
At each time point the survey also asked respondents to rate their overall preparedness for practice in their current setting on a scale of 0-100. Regardless of practice location, those who trained in distributed sites rated their overall preparedness higher at 2 years (80 vs 73, mean difference 6.5, 95% CI 3.01-9.92, p<0.001), 5 years (81 vs 72, mean difference 8.5, 95% CI 3.21-13.77, p=0.002) and 10 years (80 vs 72, mean difference 7.7, 95% CI 1.09-14.35, p=0.002) post-qualification.
Discussion
Data from the Canadian Medical Association (CMA) and the Canadian Post-MD Education Registry, Office of Research and Information Services (CAPER-ORIS) shows that roughly three-quarters of physicians will stay in the province in which they completed their postgraduate education30. Less is known about the types of patient populations served. In a presentation to the 6th Annual Physician Workforce Research Conference, Steve Slade, Vice-President Research and Analysis CAPER-ORIS, suggested that as medical education is increasingly distributed across multiple training sites 'We need to look further at how training in a variety of clinical teaching facilities correlates with eventual practice location.'31 This research has done just that. The findings of the current study support the hypothesis that family physicians will enter permanent practice in a location similar to ones in which they trained and that location of postgraduate training is the most important predictor of eventual practice location.
This may reflect self-selection, as those with some rural upbringing were more likely to choose a distributed training site and may have chosen it based on an interest in this type of practice. In naturalistic studies, such as this, it is difficult to know to what degree the actual experience in a training location adds to (or subtracts from) that intention. Although respondents did not necessarily report that their residency was an important consideration in choosing a practice location, those from distributed sites were more prepared for practice overall, with those from metropolitan programs least prepared, particularly for work in a rural or regional setting.
A number of authors refer to a pipeline approach to rural physician resources in which rural students are encouraged to enter medicine and are provided with both rural undergraduate and postgraduate training opportunities32-35. The current data supports this pipeline approach, suggesting that these factors may be cumulative. Neither rural origin nor rural undergraduate training was independently associated with rural or regional practice. However, when combined with participation in a distributed postgraduate training site, these factors were significantly more likely to predict such a practice setting. Failing to provide postgraduate training in distributed sites could undo the important work of admissions and rural undergraduate learning experiences.
Both theoretical and practical explanations can be postulated for this. From a practical perspective, the trainees are exposed to particular clinical experiences relevant to that patient population and practice location. The rural site curriculum includes specific training in trauma care whereas the St Paul's site includes rotations in an inner city clinic. From a theoretical perspective, situated learning theory suggests that a training site provides the context within which the resident develops his or her professional identity36,37. The majority of clinical medical training for both undergraduates and postgraduates has been based on a rotation system, where trainees are based in university hospitals and rotate to rural or regional centers for specific educational experiences, usually 1-2 months in duration. Family medicine training provides longitudinal, community based clinical experience that allows the trainee to develop '... meaningful levels of continuity, or responsibility.'38 Family medicine residents in the distributed sites of the current study live and work in the rural and regional centers, returning to the university setting only for very specialized or elective experiences - so-called reverse distribution. This allows trainees, and their families, to develop roots in these communities - both professional and personal.
Postgraduate training programs in other specialties are beginning to base trainees in regional centers away from the traditional university teaching hospitals39. While requiring some exposure to high volume specialized rotations, regionally based specialty training provides an opportunity to develop the professional and personal roots in non-metropolitan communities that are hypothesized to increase recruitment and retention. Early results of these programs show promising association between postgraduate training in a distributed regional program and eventual practice in northern or smaller communities11.
While not the focus of the current study, it is interesting to note the group of physicians who continue to do locums as a career path, in addition to or instead of a permanent practice. In this study, three-quarters of those still doing locums 10 years after graduation were doing at least some of these in rural areas. Although not necessarily permanently situated in rural communities, this subgroup can contribute significantly to rural physician resources.
Using an existing data source has both advantages and limitations. Extensive longitudinal records could be accessed, and volunteer bias, if any, was not influenced by the research question. Practice location, a key outcome in the study, was based on self-report, which is open to individual interpretation. However, as the data was collected for another purpose and respondents were unaware of the research question, it is more likely that the inaccuracies would be of a random, rather than systematic, nature. The analysis was limited by the questions asked and by some lack of consistent administration and coding of the survey over the years. Demographic and personal background information was not collected for the 5- and 10-year cohorts, which prevented multivariable analysis of factors related to long term practice location. A response rate of 45% is reasonable but could be improved. There was a female response bias which, coupled with the finding that women in the study were more likely to work in cities, may have reduced the effect size. Finally, other non-educational factors such as regulatory and financial incentives will influence practice location and these have not been taken into consideration.
Participation in a distributed postgraduate family medicine training site is an important predictor of a non-urban practice location. This effect persists for 10 years after completion of training and is independent of other predictors of non-urban practice including gender, rural upbringing, and rural undergraduate training. It is hypothesized that this is due not only to a curriculum that supports preparedness for this type of practice but also to opportunities to develop personal and professional roots in these communities. While well established for family medicine, there is also a need for research to support the public policy direction of distributed postgraduate specialty education to improve geographic distribution of all physicians.
Acknowledgments
The authors wish to thank Dr Jonathan Berkowitz for his statistical expertise, Dr Gordon Page for his advice on the draft manuscript, and Ms Shirley Tam (Program Administrator) for faithfully maintaining the survey in a research format for the past 12 years.
Dr Sivertz was instrumental in the conception and design of this study and actively participated in analysis of the results. Sadly Dr Sivertz passed away before the paper underwent final editing. The authors are grateful for her leadership and dedication to distributed medical education.
References
1. Statistics Canada. (Online). Table 105-3067, 'Difficulties accessing routine or on-going care, among those who required care at any time of day, household population aged 15 and over, Canada, provinces and territories'. CANSIM (database). Using E-STAT (distributor). http://www5.statcan.gc.ca/cansim/a26?lang=eng&retrLang=eng&id=1053067&tabMode=dataTable&srchLan=-1&p1=-1&p2=9 (Accessed 26 May 2013).
2. Goldsand G, Thurber AD. The overlapping roles of primary care physicians, general specialists and subspecialists - the Canadian perspective. Paper presented at 7th International Medical Workforce Conference, Oxford, United Kingdom, September 2003. Available: http://rcpsc.medical.org/publicpolicy/imwc/Can_overlapping_roles_George_Goldsand.pdf (Accessed 6 November 2013).
3. Pong RW, Pitblado JR. Geographic distribution of physicians in Canada: beyond how many and where. Ottowa: Canadian Institute for Health Information, 2005.
4. Task Force Two. Canada's physician workforce: occupational human resources data assessment and trends analysis. Final report. 2005 (Online). Available: http://www.effectifsmedicaux.ca/reports/OccHRReport-e.pdf (Accessed 6 November 2013).
5. Task Force Two. A physician human resource strategy for Canada. Final report, 2006 (Online). Available: http://www.effectifsmedicaux.ca/reports/TF2FinalStrategicReport-e.pdf (Accessed 6 November 2013).
6. Rural Health Workforce Australia. Will more medical places result in more rural GPs? Melbourne, VIC: Rural Health Workforce Australia, 2008.
7. United States General Accounting Office. Physician workforce: physician supply increased in metropolitan and nonmetropolitan areas but geographic disparities persisted. Report no. GAO-04-124. Washington: United States General Accounting Office, 2003.
8. Kassebaum DG, Szenas PL. Rural sources of medical students, and graduates' choice of rural practice. Academic Medicine 1993; 68(3): 232-236.
9. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11(6): 277-284.
10. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R et al. Rural background and clinical rural rotations during medical training: effect on practice location. Canadian Medical Association Journal 1999; 160(8): 1159-1163.
11. Hogenbirk JC, Mian O, Pong RW. Postgraduate specialty training in northeastern Ontario and subsequent practice location. Rural and Remote Health 11: 1603 (Online) 2011. Available:
www.rrh.org.au (Accessed 6 November 2013).
12. Chan BTB, Degani N, Crichton T, Pong RW, Rourke J, Goertzen J et al. Factors influencing family physicians to enter rural practice: does rural or urban background make a difference? Canadian Family Physician 2005; 51: 1247.
13. Zink T, Center B, Finstad D, Boulger JG, Repesh LA, Westra RDO et al. Efforts to graduate more primary care physicians and physicians who will practice in rural areas: examining outcomes from the University of Minnesota-Duluth and the Rural Physician Associate Program. Academic Medicine 2010; 85(4): 599-604.
14. Woloschuk W, Tarrant M. Does a rural educational experience influence students' likelihood of rural practice? Impact of student background and gender. Medical Education 2002; 36(3): 241-247.
15. Chen F, Fordyce M, Andes S, Hart LG. Which medical schools produce rural physicians? A 15-year update. Academic Medicine 2010; 85(4): 594-598.
16. Gray JD, Steeves LC, Blackburn JW. The Dalhousie University experience of training residents in many small communities. Academic Medicine 1994; 69(10): 847-851.
17. Norris TE, Norris SB. The effect of a rural preceptorship during residency on practice site selection and interest in rural practice. Journal of Family Practice 1988; 27(5): 541-544.
18. Rosenthal TC. Outcomes of rural training tracks: a review. Journal of Rural Health 2000; 16(3): 213-216.
19. Tolhurst HM, Adams J, Stewart SM. An exploration of when urban background medical students become interested in rural practice. Rural and Remote Health 6: 2 (Online) 2006. Available:
www.rrh.org.au (Accessed 6 November 2013).
20. Rourke J, Incitti F, Rourke LL, Kennard M. Relationship between practice location of Ontario family physicians and their rural background or amount of rural medical education experience. Canadian Journal of Rural Medicine 2005; 10(4): 231-239.
21. Grobler L, Marais BJ, Mabunda SA, Marindi PN, Reuter H, Volmink J. Interventions for increasing the proportion of health professionals practising in rural and other underserved areas. Cochrane Database of Systematic Reviews 2009, 21 Jan; (1): CD005314.
22. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 7(8): 790-798.
23. Ranmuthugala G, Humphreys J, Solarsh B, Walters L, Worley P, Wakerman J et al. Where is the evidence that rural exposure increases uptake of rural medical practice? Australian Journal of Rural Health 2007; 15(5): 285-288.
24. Statistics Canada. Health profile. (Online) 2013. Statistics Canada catalogue no. 82-228-XWE. Available: http://www12.statcan.gc.ca/health-sante/82-228/details/page.cfm?Lang=E&Tab=1&Geo1=PR&Code1=59&Geo2=PR&Code2=01&Data=Rate&SearchText=British%20Columbia&SearchType=Contains&SearchPR=01&B1=All&Custom=&GeoLevel=PR&GeoCode=59 (Accessed 6 November 2013).
25. Whiteside C, Longhurst MF. Establishment of a community-based residency training program. Canadian Family Physician 1987; 33(12): 2751-2754.
26. Whiteside C, Mathias R. Training for rural practice: are graduates of a UBC program well prepared? Canadian Family Physician 1996; 42(7): 1113-1121.
27. Whiteside C, Pope A, Mathias R. Identifying the need for curriculum change: when a rural training program needs reform. Canadian Family Physician 1997; 43(8): 1390-1394.
28. Bates J, Andrew R. What do they contribute? Family medicine residents who practise in cities. Canadian Family Physician 2003; 49(3): 337-341.
29. College of Family Physicians of Canada. The Janus project: National Family Physician Survey. (Online). Available: http://www.cfpc.ca/Janus (Accessed 5 February 2012).
30. Canadian Post-M.D. Education Registry. 2010-2011 Annual Census of Post-M.D. Trainees. Ottawa: Association of Faculties of Medicine of Canada, 2011.
31. Slade S. On the move: a retrospective, longitudinal view of physician migration patterns in Canada. Paper presented at the Sixth Annual Physician Workforce Research Conference, 6-7 May 2010, Alexandria, VA, USA.
32. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health 9(1): 1083. (Online) 2009. Available: www.rrh.org.au (Accessed 6 November 2013).
33. Norris TE. Education for rural practice: a saga of pipelines and plumbers. Journal of Rural Health 2000; 16(3): 208-212.
34. Rabinowitz HK, Paynter NP. The role of the medical school in rural graduate medical education: pipeline or control valve? Journal of Rural Health 2000; 16(3): 249-253.
35. Strasser R, Hogenbirk JC, Lewenberg M, Story M, Kevat A. Starting rural, staying rural: how can we strengthen the pathway from rural upbringing to rural practice? Australian Journal of Rural Health 2010; 18(6): 242-248.
36. Mann KV. Theoretical perspectives in medical education: past experience and future possibilities. Medical Education 2011; 45(1): 60-68.
37. Durning SJ, Artino AR. Situativity theory: a perspective on how participants and the environment can interact: AMEE Guide no. 52. Medical Teacher 2011; 33(3): 188-199.
38. College of Family Physicians of Canada. Standards for accreditation of residency training programs: family medicine; emergency medicine; enhanced skills; palliative medicine. Mississauga, Ontario: College of Family Physicians of Canada, 2006; 60.
39. Bates J, Frost H, Jamieson JL, Schrewe B, Ellaway R. Distributed education and distance learning in postgraduate medical education. Environmental Scan, Future of Medical Education in Canada Postgraduate Project (series). (Online) 2011. Available: http://www.afmc.ca/pdf/fmec/12_Bates_Distributed%20Education.pdf (Accessed 6 November 2013).



