full article:
Diabetes mellitus type II (diabetes) is a worldwide problem and was the seventh leading cause of death in the USA in 20071. This number is likely underrepresented due to deaths from secondary effects of diabetes. Being diagnosed with diabetes doubles the mortality risk when compared with the risk of patients without diabetes. Direct and indirect costs for diabetes are estimated to be US$174 billion annually. Diabetes is a debilitating disease which affects most major body systems, including circulatory, nervous, reproductive, urinary, and integumentary2. Major complications from diabetes include stroke, heart disease, hypertension, blindness and eye problems, kidney disease, amputations, nervous system disease, and dental disease1. Diabetes is a growing concern in the USA, with 6% of the population diagnosed with diabetes and another 5% having pre-diabetes2. The prevalence of diabetes is 17% higher in rural areas than in central cities2. Surveys of state and local rural health leaders showed diabetes is considered a priority area in rural health3. Diabetes, heart disease, and stroke are considered equally significant medical concerns in rural populations3.
Members of rural communities comprise an increasing number of diabetic patients with poorer outcomes than those living in urban communities. Rural patients make fewer visits to doctors and are less likely to receive adequate care after a hospital stay2. Studies in both the USA and Canada have shown that rural communities receive inadequate diabetic care compared to that described in the guidelines developed by the American Diabetes Association (ADA)4. In addition to inadequacy of care, individuals with diabetes who live in rural areas are less likely to report diabetes-associated morbidities5.
The ADA recommends routine physician visits, hemoglobin A1C (HbA1C) testing, professional foot exams and dilated eye exams for all persons diagnosed with diabetes5. Studies conducted on diabetic persons living in rural and underserved areas have demonstrated disparities in meeting ADA recommendations for diabetics5. Those with diabetes in rural communities are diagnosed later in the disease than urban communities, which leads to more complications from disease progression3.
In Rural Healthy People 2010, diabetes was the third-highest rural health concern after access to care, and stroke and heart disease3. In all four US Census Bureau designated regions in the USA, diabetes was ranked among the top five priorities. The south ranked diabetes a higher priority than the other three regions. The prevalence of diabetes in developed rural communities is higher than that of underdeveloped rural communities. US Census projections have predicted that by 2050 the prevalence of diabetes will double3.
There is an estimated 17% higher prevalence of diabetes in rural versus urban communities. Some of the disparities are rooted in farther distances to clinics, financial restrictions, mistrust, cultural barriers, language difficulties, and health illiteracy6. The challenge resides in providing the members of these underserved communities the access to care and diabetic education in a cost-effective manner. By doing these things, adequate glycemic control can be achieved to decrease the burden of diabetes and reduce morbidity and mortality6. Research was conducted to identify the best evidence-based strategies directed towards improving diabetic outcomes of rural populations by reducing HbA1C.
For the purpose of this review, rural is defined using the US Department of Health and Human Services guideline: all populations not residing in an urban area. Adult diabetics are those patients older than 18 years who have been diagnosed with diabetes by a healthcare provider.
Inclusion and exclusion criteria
For literature to be included in the review, studies must have been conducted in an outpatient setting, been published in the English language, have utilized a rural population, have a primary focus on adults, and have been published within the past 8 years.
Literature that used an inpatient setting, focused on children or adolescents, focused on pregnancy-related diabetes, published in a language other than English and literature that did not meet any inclusion criteria was excluded from the review.
Search strategy
The review focussed on diabetes care for older adults in rural populations, therefore the literature search was conducted using the following key terms: diabetes, adult, education, hemoglobin A1C and rural. Scholarly databases that were used include CINAHL, PubMed, Medline, and Sage Pub. Using these search engines, with the key terms and using the inclusion and exclusion criteria, returned 15 articles for review.
Search
The combined searches from Medline, CIHNAL, PubMed, and Sage Pub yielded 1819 articles that referenced the key terms. Titles of the articles were reviewed for relevance to the subject, which narrowed the list to 52 articles. Abstracts of the remaining articles were read, further narrowing the selection to 23. The remaining articles were read in full, and 15 of these were selected for the final review.
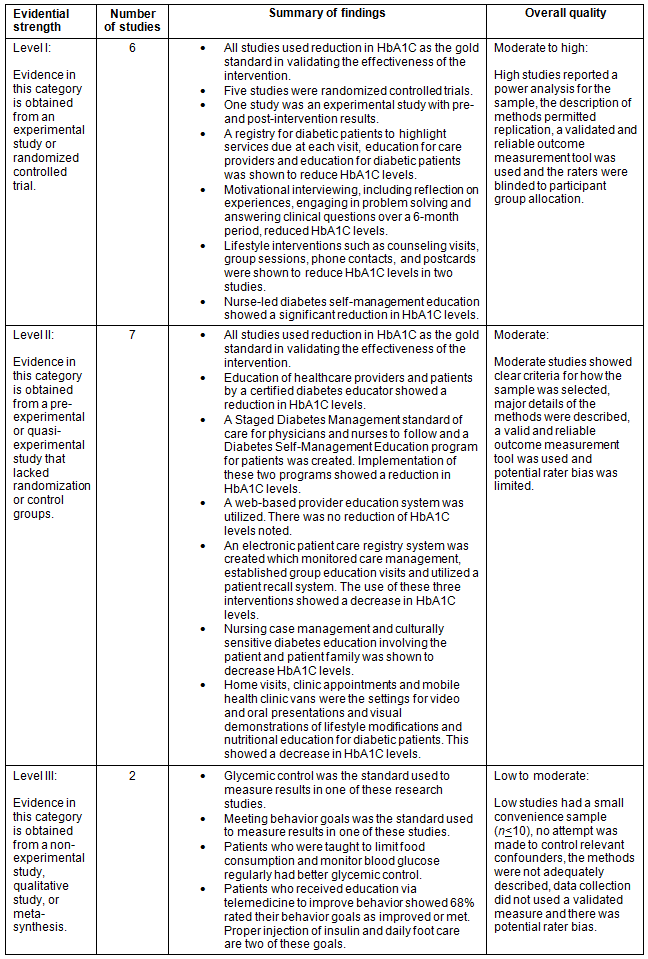
Table 1: Quality assessment levels of evidence according to the John Hopkins Nursing evidence-based practice model and guidelines7
 <
<
Interventional themes
Four interventional themes resonating throughout the literature are shown to lower HbA1C scores: lifestyle modifications, motivational counseling, nutritional education for patients, and education for providers. The literature presented is grouped by these themes of interventions. Some studies are discussed multiple times under the different groups.
Lifestyle modification: Lifestyle modifications are very important when trying to reduce one's HbA1C. In a study of rural Latino patients, education on lifestyle modification was provided through video presentations, verbal explanations, and written material. It is important to provide not only written material, but verbal material as well. This is even more pertinent in rural populations where illiteracy is highest. Lifestyle modifications that were discussed include smoking cessation and exercise for 30 minutes, three times per week. At the conclusion of the study, HbA1C scores of participants decreased by 0.5% or more in 71% at 6 months, 63% at 12 months, 57% at 18 months, and 64% at 24 months8.
Another study focused on lifestyle modification of moderate weight loss and a minimum of 150 minutes of physical activity per week to reduce HbA1C scores. The results showed HbA1C was reduced by up to 1.6 points for these participants9.
Motivational counseling: Studies by Hawkins10 and Samuel-Hodge et al11 have shown motivational counseling decreases HbA1C levels in diabetic patients in rural areas. Motivational counseling consists of counseling visits, group sessions, phone contacts, postcards reflecting on experiences, discussing problem solving, and encouraging participants. Consistent counseling and follow-up are the keys to success for lowering HbA1C. Motivational counseling is an intervention that reduces HbA1C levels, as long as the patient has access to the appropriate resources10,11.
Nutritional education for patients: Nutritional education is essential in HbA1C score reduction. Education including portion sizes and healthy alternative cooking methods was given to participants8,12. Other elements in these educational classes included how to choose low-fat foods using the diabetes food pyramid and practical strategies for reducing fats12. Brewer-Lowery et al13 found those who had a more structured approach to their diet, like limiting food consumption, had a better glycemic control than those who did not. Using these dietary strategies, HbA1C levels were reduced by 1.0%12.
Another tool implemented is the use of educational materials provided to patients. One of the materials, the 'ABCs of diabetes' (HbA1C, blood pressure, and low-density lipoprotein cholesterol values) was mailed to participants in a study conducted by Dettori et al14. By reviewing this material, participants achieved up to a 0.5% reduction in HbA1C14.
Provider-led discussions are another educational tool to lower HbA1C scores. From education workshops to nurse-led discussions, these interventions involved patients talking about their personal experiences to help others in the group14,15. Televisits (online discussions) were also implemented with nurse and dietician educators using goal-setting for behavior change to lower HbA1C16. All of these provider-led discussions had great success, with a reduction up to 0.7% in HbA1C scores14-16.
Education for providers: Literature has shown a reduction in HbA1C scores when the providers themselves are more educated in diabetes management. A rural study in Montana showed providers were not well educated on the guidelines for diabetes care and management. Because of this, a diabetes educational program was established for providers through the ADA, which reduced HbA1C by 0.5%14; however, this study may be unique. Estrada et al17 found no improvement in HbA1C scores when utilizing a web-based education system for primary care physicians using continuing education programs and performance feedback.
Research also found that establishing a diabetes registry or redesigning the healthcare delivery system has improved patients' HbA1C scores14,18,19. Dettori et al14 found that when setting up registries for diabetic patients to support ongoing patient care, with highlight services that were due at each visit (eg counseling and patient education), HbA1C scores dropped 0.5%. Siminerio et al19 also found when redesigning the delivery system of patient care that providers improved adherence to the ADA guidelines, and their patients showed an improvement in HbA1C scores. By adding these technological strategies, primary care providers can use their time and resources more appropriately to help manage their diabetic patients.
Discussion
This integrative review's purpose is to evaluate best evidence outcome strategies directed at improving diabetic outcomes of rural populations through HbA1C reductions. Reduction in HbA1C levels was used to quantitatively identify favorable results for diabetic patients. More than one method was found to produce these results; however, education was key in each method.
Education in many forms was found to improve outcomes for diabetic patients. With the rural population, it is necessary to provide education that is culturally sensitive and accessible for the patient. This education may be in group classes or one-on-one counseling. Education may be presented in a variety of formats such as online classes, brochures/pamphlets, hands-on demonstrations or videos depending on the abilities and/or limitations of individuals. Although online classes have the capability to bring education into the home for diabetic patients, some patients in rural areas may not have readily available internet access or may not be computer literate. Including family members in instructional classes and/or building meal plans around culturally significant foods is an additional method to increase dietary compliance in rural populations. Illiterate patients would benefit most from hands-on demonstrations and videos.
Education for the rural diabetic may focus on awareness of nutritional limitations or needs. It may also focus on lifestyle modifications to improve diabetic outcomes. The lifestyle modifications of a weekly exercise routine, weight loss and smoking cessation showed significant reductions in HbA1C levels. These modifications may also result in improved quality of life and fewer adverse effects.
No matter what educational format is used, the key to improved diabetic patient outcomes is consistency and follow-up. Motivational counseling should also be included to encourage and empower the diabetic patient to take control of his or her life and disease process. With proper education, the diabetic patient will be able to make informed choices, and this has been shown to alter the course of the disease process. Bringing education to diabetic patients in rural areas takes ingenuity and imagination, but the results emphatically demonstrate the effectiveness of education as an intervention to improve results for these diabetic patients.
Diabetes is a significant problem in the USA. Education for the patient is an important tool to improve outcomes for diabetic patients. The rural population has several disadvantages, including distance from healthcare providers, distance from educational classes, and possible cultural variances. In rural areas, education should be tailored to meet the needs of the specific population. Consistent follow-up after education also shows positive outcomes for the diabetic patient. Education for the primary care provider did not have a proven appreciable effect on diabetic outcomes. Awareness and need for change must be recognized in the diabetic rural population in order to delay progression of current disease and prevent future occurrences. Through lifestyle modification, motivational counseling, and nutritional education, these goals can be attained.
References
1. Centers for Disease Control and Prevention. 2011 National diabetes fact sheet. (Online). Available: http://www.cdc.gov/diabetes/pubs/factsheet11.htm (Accessed 1 October 2012).
2. Dabney B, Gosschalk A. Diabetes in rural America. (Online). Available: www.srph.tamhsc.edu/centers/rhp2010/05Volume1diabetes.pdf (Accessed 20 October 2012).
3. Gamm LD, Hutchinson LL, Dabney BJ, Dorsey AM. Rural healthy people 2010: a companion document to healthy people 2010. College Station, Texas: Texas A&M University System Health Science Center, School of Rural Public Health, Southwest Rural Health Research Center, 2003.
4. ECARE-DIABETES. Diabetes in rural and minority communities. (Online) 2009. Available: http://www.ecarediabetes.org/About/Communities.cfm (Accessed 1 October 2012).
5. Hale NL, Bennett KJ, Probst JC. Diabetes care and outcomes: disparities across rural America. Journal of Community Health 2010; 35(4): 365-374.
6. Appel C, Buchanan K, Cherrington A, Massey C. Improving diabetes care in rural communities: an overview of current initiatives and a call for renewed efforts. Clinical Diabetes 2010; 28(1): 20-27.
7. Newhouse RP, Dearholt SL, Poe SS. John Hopkins Nursing - evidence-based practice model and guidelines. Baltimore: Sigma Theta Tau International, 2007.
8. Outcomes and challenges of familias saludables: a rural Latino chronic disease screening and management project. Hispanic Health Care International 2011; 9(3): 137-143.
9. Mayer-Davis EJ, D'Antonio AM, Smith SM, Kirkner G, Martin SL, Parra-Medina D, et al. Pounds off with empowerment (POWER): a clinical trial of weight management strategies for black and white adults with diabetes who live in medically underserved rural communities. American Journal of Public Health 2004; 94(10): 1736-1742.
10. Hawkins SY. Improving glycemic control in older adults using a videophone motivational diabetes self-management intervention. Research & Theory for Nursing Practice 2012; 24(4): 217-232.
11. Samuel-Hodge CD, Keyserling TC, Park S, Johnston LF, Gizlice Z, Bangdiwala SI. A randomized trial of a church-based diabetes self-management program for African Americans with type 2 diabetes. The Diabetes Educator 2009; 35(3): 439-454.
12. Anderson-Loftin W, Barnett S, Bunn P, Sullivan P, Hussey J, Tavakoli A. Soul food light: culturally competent diabetes education. The Diabetes Educator 2005; 31(4): 555-563.
13. Brewer-Lowery AN, Arcury TA, Bell RA, Quandt SA. Differentiating approaches to diabetes self-management of multi-ethnic rural older adults at the extremes of glycemic control. The Gerontologist 2010; 50(5): 657-667.
14. Dettori N, Flook BN, Pessel E, Quesenberry K, Loh J, Harris C et al. Improvements in care and reduced self-management barriers among rural patients with diabetes. Journal of Rural Health 2005; 21(2): 172-177.
15. Tshiananga JKT, Kocher S, Weber C, Erny-Albrecht K, Berndt K, Neeser K. The effect of nurse-led diabetes self-management education on glycosylated hemoglobin and cardiovascular risks: a meta analysis. The Diabetes Educator 2012; 34(1): 108-123.
16. West SP, Lagua C, Trief PM, Izquierdo R, Weinstock RS. Goal setting using telemedicine in rural underserved older adults with diabetes: experiences from the informatics for diabetes education and telemedicine project. Telemedicine and e-Health 2010; 16(4): 405-416.
17. Estrada CA, Safford MM, Salanitro AH, Houston TK, Curry W, Williams JH et al. A web-based diabetes intervention for physician: a cluster-randomized effectiveness trial. International Journal for Quality in Health Care 2011; 23(6): 682-689.
18. Bray P, Thompson D, Wynn JD, Cummings DM, Whetstone L. Confronting disparities in diabetes care: the clinical effectiveness of redesigning care management for minority patients in rural primary care practices. The Journal of Rural Health. 2005; 21(4): 317-321.
19. Siminerio LM, Piatt G, Zgibor JC. Implementing the chronic care model for improvements in diabetes care and education in a rural primary care practice. The Diabetes Educator. 2005; 31(2): 225-234.
