People who live in rural communities face a range of challenges that may have an impact on their access to the healthcare system including longer travel distance and time to receive healthcare1, shortages of primary care providers2,3, hospitals undergoing financial stresses2, and greater risk of being uninsured4. These challenges are compounded by the strains resulting from higher poverty rates, lower rates of employment, and lower educational attainment for those who live in non-metropolitan (metro) areas compared to those who dwell in metro areas5. The geographic and demographic realities of rural life may also interact around health-related issues. Lower socioeconomic status is generally associated with poorer health, regardless of rurality of residence6, and greater distance to primary care has been associated with later diagnosis of serious health conditions in rural Maine, USA7. Even the types of employment available in rural areas (agriculture, mining, and fishing, for example) may come with health hazards2.
Considering these challenges, it is hardly surprising that rural residents are often thought to have poorer health compared to urban dwellers. In the area of chronic disease, unadjusted rates of type 2 diabetes, heart disease, hypertension, stroke, and cancer are all higher in rural compared to urban areas4. Some of these differences may be reduced or eliminated by adjusting for age, race, and income4. However, given the finding that life expectancy remains lower in rural compared to urban areas8, it seems clear that some health disparities between rural and urban dwellers are far more than statistical artifacts. Rural dwellers also face challenges in the area of maternal and child health. Teenage birthrates9, neonatal mortality10, and adverse birth outcomes (eg low birth weight and prematurity)11 have all been found to be higher in rural as compared to urban areas in some studies. However, as is the case for chronic disease, some of these disparities may reflect demographic differences in race and income4.
Because it has an impact on future generations, maternal and child health disparities along the rural-urban continuum are certainly a vital area of inquiry. The reasons for these differences are, to say the very least, multifactorial. Pre-pregnancy maternal demographics (age, race, marital status, and income), pre-pregnancy maternal behaviors (smoking, alcohol consumption, and body weight), and prenatal behaviors (smoking, alcohol consumption, weight gain, and seeking prenatal care) can all have an impact on the health of the pregnant women, the course of pregnancy (development of hypertension or gestational diabetes and the risk of Caesarean section birth), and the health of newborns. Postpartum maternal behaviors such as smoking and breastfeeding can also affect the newborn's health12. Further, many of these factors may differ in rural compared to urban communities, at least in some states4,13,14.
The objective in this study was to define differences in pre-pregnancy, prenatal, and postpartum health-related variables along the rural-urban continuum in the state of Maine. To accomplish this, data were analyzed for the state of Maine from the Pregnancy Risk Assessment Monitoring System (PRAMS) over the years 2000-201015. PRAMS is a public health surveillance project conducted by the US Center for Disease Control and Prevention in conjunction with state health departments. The PRAMS dataset contains demographic, behavioral, and health information about new mothers as well as health information about their newborn babies. These data were mapped in a geographic information system (GIS) with each birth spatially referenced to the town of residence of the mother. The rurality of each town was defined by rural-urban commuting area (RUCA) codes16. Maine is an important location to perform this analysis because Maine's communities are distributed broadly across the rural-urban continuum, rurality has already been shown to affect health in Maine17, and Maine is a state that is not successfully reducing its rates of important infant health indicators such as the rate of babies born with a low birth weight18. These results may be of interest to readers who are concerned about the impact of rurality on maternal and child health disparities in general, readers who are specifically concerned about these health issues in Maine, and readers who are interested in exploring maternal and child health indicators in their own area.
PRAMS data extraction
The PRAMS study population is all women who gave birth to a live infant in the previous 2-4 months, identified from birth certificates. The PRAMS study sample is a stratified representative sample of these women, with members of high-risk groups over-sampled. In Maine, women who gave birth to low birth weight infants are over-sampled. PRAMS methodology involves mailing questionnaires to women who have recently given birth, using telephonic follow-up to obtain information from non-responders, and linking questionnaire results to infant birth certificate data15. For this study, PRAMS data for Maine from 2000 to 2010 were obtained from the Maine Center for Disease Control and Prevention18.
The following PRAMS variables were used in this study: maternal age; maternal marital status; maternal town of residence; whether or not the mother had a previous live birth; household income; maternal education and race; maternal height; maternal pre-pregnancy weight and weight gain during pregnancy; gestational age of the infant when the woman was sure she was pregnant and at the earliest prenatal visit; whether or not the mother received prenatal care as early as she wished and whether or not smoking, drinking, and breast feeding were discussed during prenatal visits; maternal tobacco and alcohol use before, during, and after pregnancy; presence of hypertension during pregnancy or gestational diabetes; method of birth (Caesarean section vs vaginal birth); infant gestational age at birth, weight at birth, length of stay in hospital, and admission to an intensive care unit; and breastfeeding.
These variables were analyzed as follows:
- Maternal age, pre-pregnancy body mass index (BMI) calculated from weight and height, weight gain during pregnancy, gestational age at which the women were sure they were pregnant, gestational age at which the women began receiving prenatal care, and infant birth weight were analyzed as continuous variables.
- BMI was used to place pre-pregnancy weights into the standard categories (underweight, normal weight, overweight, and obese) and these categories were used to determine if the amount of maternal weight gain during pregnancy was less than the recommended range, within the recommended range, or greater than the recommended range according to current Institute of Medicine guidelines19. Pregnancy weight gain was also analyzed categorically (<6.8 kg (15 lb), 6.8-20.4 kg (15-45 lb), >20.4 kg (45 lb)). Other categorical variables analyzed for this study included maternal age (<20 years, 20-35 years, >35 years), length of the infant's hospital stay (1-2 days, 3-5 days, ≥6 days), infant birth weight (<2500 g, 2500-4000 g, ≥4000 g), and breastfeeding (never, <8 weeks, ≥8 weeks).
- Smoking and drinking were analyzed as dichotomous variables as were marital status; maternal educational attainment (≤12 years vs >12 years); household income (≤US$20 000/year vs >US$20 000/year); race (white vs all other races); whether or not the pregnant woman received prenatal care as early as she wished; and whether or not smoking, drinking, and breastfeeding were discussed during pregnancy.
Geographic information system construction
GIS analysis was conducted using ArcMap v10.1 (ESRI; http://www.esri.com/software/arcgis). Base maps of Maine's counties, towns, and census blocks were obtained from the Maine Office of GIS data catalog20. Census blocks were merged to create a statewide map of census tracts. Primary and secondary RUCA codes were obtained for all Maine census tracts from the US Department of Agriculture Economic Research Service21 and merged with the map of census tracts. Then each census tract was assigned to one of four rurality tiers (urban, suburban, large rural town, isolated rural) using the four-tier consolidation of the secondary RUCA codes22. There are 533 Maine towns and 358 Maine census tracts. In many instances in Maine census tracts and towns are defined by the same boundaries. In a very few of the largest cities there is more than one census tract in a city (although all of these census tracts fall into the same rurality tier), and in much of rural Maine a single census tract contains several towns. Rurality tiers were determined for each town by converting the census tract map to centroid points and determining which point was within the boundaries of or closest to each town. Finally, rurality tiers were assigned to each PRAMS questionnaire response based on the mother's town of residence.
Data analysis
Results for study subjects from the four rurality tiers were compared using the survey procedures in Statistical Analysis Software v9.3 (SAS Institute; http://www.sas.com) to adjust for the complex sampling strategy of the PRAMS dataset. Means (for continuous variables) and percentages (for categorical variables) were calculated for each rurality tier, along with 95% confidence intervals. Significant differences between rurality tiers were tested for using F-tests (for continuous variables) and χ2 tests (for dichotomous and categorical variables). Significance was accepted at p<0.05. If significant differences between rurality tiers existed, specific tiers were judged to be different from each other if their 95% confidence intervals did not overlap.
Ethics approval
This protocol was approved by the University of Southern Maine Institutional Review Board (IRB protocol #101912-01) and vetted before the Maine Center for Disease Control and Prevention.
Between 2000 and 2010 there were 12 600 Maine women who answered PRAMS questionnaires. This is a response rate of >70% for each year and overall. After excluding 29 births for which the infant's birth weight was unknown and another 10 for which the town of residence of the mother was unknown there were a maximum of 12 561 respondents to any question. Of these births, 3575 were to women who resided in urban areas, 2649 to women who resided in suburban areas, 2432 to women who resided in large rural towns, and 3905 to women living in isolated rural areas.
Pre-pregnancy results
There were significant differences along the rural-urban continuum for age, race, BMI, educational attainment, marital status, income, smoking risk, and drinking risk of women before pregnancy (p<0.0001 for each variable). There were also differences in the number of women who had a previous live birth (p=0.01; Tables 1, 2). The average ages of women from isolated rural areas (27.1 years) and large rural towns (27.7 years) were significantly less than the average ages of women from urban (29.0 years) or suburban (28.7 years) areas (Table 1). These differences result from the continuous increase in the number of women aged <20 years giving birth as rurality increased (from 6.2% of urban women to 10.5% of women from isolated rural areas) with a decrease in the number of women aged >35 years giving birth (from 17.5% in urban areas to 9.9% in isolated rural areas; Fig1). Mean BMI increased from 25.3 in urban areas to 26.1 in isolated rural areas (Table 2).
Women from isolated rural areas were significantly less likely to be married and more likely to have a household income ≤US$20 000/year than were women from any of the other rurality tiers. Among women from isolated rural areas, 57.8% were married (compared to 69.1% of women living in suburban areas) and 39.6% lived in households with income ≤US$20 000/year (compared to 23.6% of women from suburban areas and 28.8% of women from urban areas; Table 1). Women from rural towns and isolated rural areas were both more likely to have no education past 12th grade and to smoke cigarettes prior to pregnancy compared to women from urban or suburban areas, and less likely to drink alcohol prior to pregnancy than were women from urban areas. Among women from isolated rural areas 35.4% smoked cigarettes prior to pregnancy (compared to 27.8% of suburban women) and 51.8% had no education past high school (compared to 37.7% of women from urban areas; Tables 1, 2). The likelihood of having had a previous live birth was highest for women from rural towns and lowest for women from urban areas despite the fact that rural women were younger and more likely to be aged <20 years (Table 1, Fig1). Racial diversity (although very low overall in Maine by national standards) was highest for urban women, intermediate for women from isolated rural areas and rural towns, and lowest for suburban women (Table 1).
Table 1: Pre-pregnancy demographics by rurality tier?
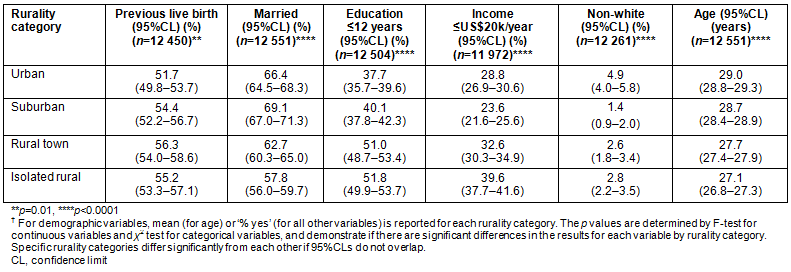
Table 2: Pre-pregnancy health behavioral variables by rurality tier?
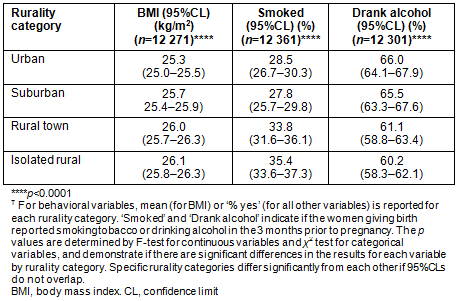
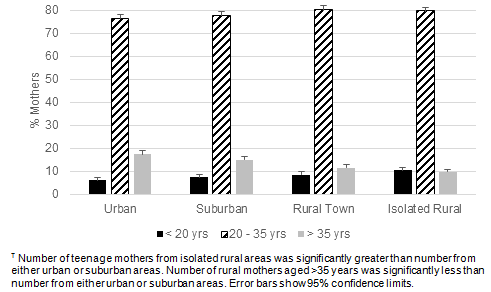
Figure 1: Distribution of maternal ages as a categorical variable varied
significantly by rurality tier, determined by χ2 test (n=12 251, p<0.0001).?
Pregnancy results
There were significant differences by rurality tier in smoking and drinking during pregnancy (p<0.0001) as well as in the number of women who reported that these topics (but not the topic of breastfeeding) were discussed during prenatal visits (p=0.004 for discussion of smoking and p=0.03 for discussion of drinking). There were significant differences in the prevalence of gestational diabetes (p=0.005) but not hypertension during pregnancy (Tables 3, 4). Analysis by rurality tier also revealed significant differences in the amount of weight gained during pregnancy, both when measured as a continuous variable (p<0.001) and when considered as a categorical variable (p=0.02 or p=0.04 depending on the categories used; Table 3, Figures 2, 3). There were significant differences by rurality tier in the gestational age at which women were sure they were pregnant (p<0.001) but not in the gestational age at which they initiated prenatal care (Table 4).
As was the case before pregnancy, women from isolated rural areas had higher rates of smoking (22.3%) and lower rates of drinking (5.1%) during pregnancy than did women from urban (14.7% smoked and 9.0% drank alcohol) or suburban areas. Women from isolated rural areas were the most likely to receive discussion of smoking and drinking during pregnancy; however, the number of women who received prenatal discussion on these subjects was >75% for all rurality tiers (Table 4). Women from rural towns had the lowest rate of gestational diabetes (8.4% compared to 11.7% for urban women; Table 3) and a significantly lower average weight gain during pregnancy (13.1 kg (28.8 lb)) than did women from urban or suburban areas (13.7 kg (30.1 lb) for each; Table 3). The low average weight gain for women from rural towns is a result of the fact that they were the least likely to gain >20.4 kg (45 lb; Fig2). The number of women whose pregnancy weight gain was within the recommended range (42.5% overall) was similar for all rurality tiers (Fig3). Women from isolated rural areas were sure they were pregnant at a later gestational age (5.8 weeks) than were women from urban or suburban areas (5.3 weeks for both; Table 4). However, this did not affect the gestational age at which they obtained prenatal care (8.6 weeks for all rurality tiers) or their ability to receive prenatal care as early as they wanted it. More than 85% of women in this study reported receiving prenatal care as early as they wanted (Table 4).
Table 3: Pregnancy risk factor variables by rurality tier?
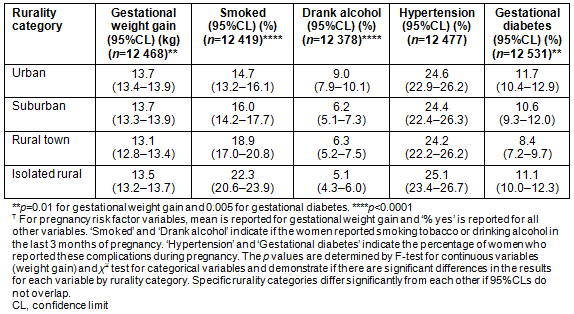
Table 4: Pregnancy care variables by rurality tier?
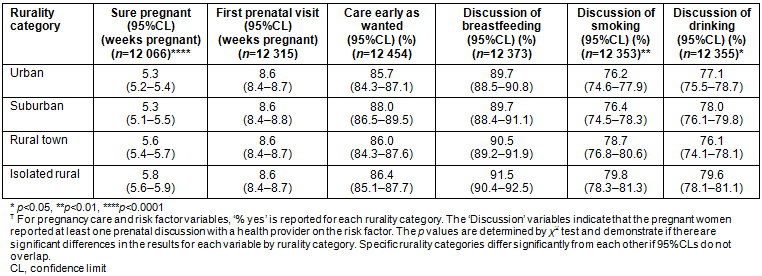

Figure 2: Distribution of maternal gestational weight gain as a categorical variable
varied significantly by rurality tier, determined by χ2 test (n=12 192, p=0.02).?
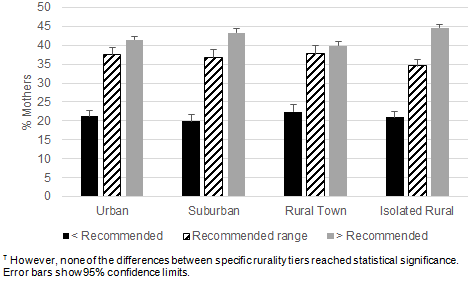
Figure 3: Distribution of maternal gestational weight gain relative to Institute of Medicine recommendations
varied significantly by rurality tier, determined by χ2 test (n=12 192, p=0.04).?
Postpartum results
There were significant differences by rurality tier in number of newborns admitted to an intensive care unit (p<0.0001; Table 5) and the length of time that newborns spent hospitalized (p=0.03; Fig4) but not in the number born by Caesarean section (overall, first time, or repeat; Fig5), their birth weight (Fig6), or the number born prematurely (<37 weeks gestational age; Table 5). Length of breastfeeding differed significantly by rurality tier (p<0.0001; Fig7) as did the number of women who smoked after giving birth (p<0.0001; Table 5).
During the study period, 10.9% of newborns with mothers from urban areas and 10.7% of newborns with mothers from suburban areas were admitted to intensive care units while only 8.4% of those born to mothers from isolated rural areas and 6.9% of those born to mothers from rural towns were (Table 5). There were also differences by rurality tier in the length of time newborns spent in the hospital. During the study period 8.5% of newborns of urban mothers and 8.8% of newborns of suburban mothers were hospitalized ≥6 days, compared to newborns to women from rural towns (8.0% hospitalized ≥6 days) and isolated rural areas (7.7% hospitalized ≥6 days; Fig4). Interestingly, these differences did not seem to reflect any of the pregnancy outcomes measured in this study. The number of births by Caesarean section across all rurality tiers was 28.2% (17.5% first-time Caesarean sections and 10.7% repeat operations with no differences by rurality tier; Fig5), 8.1% of newborns were born prematurely (with no differences by rurality tier; Table 5), and the number of newborns weighing <2500 g was 5.7% (again with no differences by rurality tier; Fig6). The number of women from isolated rural areas who did not breastfeed their infants at all was 24.7%, significantly higher than the number of urban women who did not breastfeed (19.3%). The number of women from isolated rural areas who breastfed for ≥8 weeks was 52.9%, significantly lower than the number of urban women who breastfed for this length of time (60.9%; Fig7).
Table 5: Postpartum outcome and risk factor variables by rurality tier?
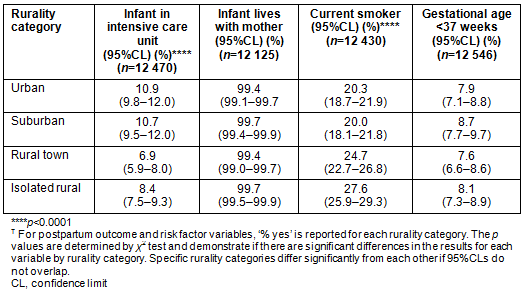
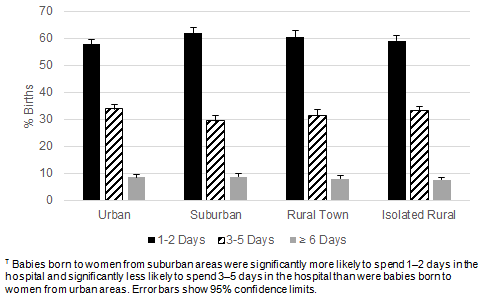
Figure 4: Distribution of hospital length of stay for newborns differs significantly
by rurality category, determined by χ2 test (n=12 341 and p=0.03).?
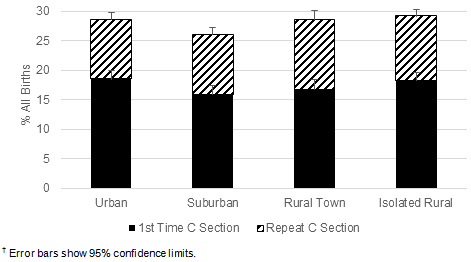
Figure 5: Distribution of first-time and repeat Caesarean (C) section birth rates did not differ
significantly by rurality tier, determined by χ2 test (n=12 551, p=0.07 for first-time C sections,
p=0.18 for repeat C sections, and p=0.10 for all C sections).?
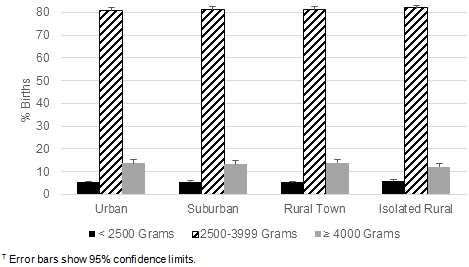
Figure 6: Infant birth weight as a categorical variable did not
vary significantly by rurality tier, determined by χ2 test (n=12 550, p=0.21).?
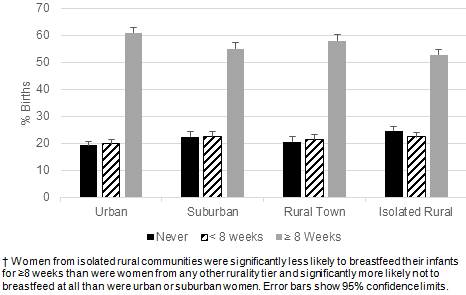
Figure 7: Breastfeeding behavior differed significantly by rurality tier, determined by χ2 test (n=12 028, p<0.0001).?
Discussion
Demographics
Differences in pre-pregnancy demographics along the rural-urban continuum similar to the results reported here have been reported in several other studies. A nationwide comparison of births in urban versus rural hospitals found that women who gave birth in rural hospitals were more likely to be younger, more likely to receive Medicaid (social health care for low income earners), and less racially diverse compared to those who gave birth in urban hospitals23. Similarly, in Oregon, rural women who gave birth were, on average, younger, less well educated, and less racially diverse than were urban women13. It should be noted that the results reported here for Maine and those from the Oregon study were spatially referenced by the rurality of the mother's residence, not by the rurality of the hospital where she gave birth as in the national study, and some women from rural areas with high-risk pregnancies may be sent to urban hospitals to give birth. However, all three studies show that rural women are younger, both the work reported here and the national study show that rural women had greater financial challenges (if receiving Medicaid is a marker for financial challenges), and both the Oregon study and the Maine results reported here show that rural women who gave birth were less well educated than their urban counterparts (Table 1, Fig1)13,23.
These findings have wide-ranging implications. Very young women who give birth (teenage pregnancies) are at risk for complications during pregnancy (hypertension, anemia, and premature labor) while women aged >35 years giving birth are at risk for complications of labor (prolonged labor, excess bleeding during labor, and increased rates of Caesarean section birth), particularly if they are giving birth for the first time24. Thus in Maine, where rural women giving birth are more likely to be aged <20 years and less likely to be aged >35 years compared to women from urban areas (Fig1), rural women giving birth may be at greater risk for some complications but at lower risk for others.
The financial challenges associated with rural residence may also present health challenges. This study reports that 39.6% of women from isolated rural areas of Maine had household incomes ≤US$20 000/year, representing 102% of the federal poverty limit for a family of three in 2013. Low income/poverty correlate with higher rates of both pre-pregnancy risks25 and pregnancy complications26. The lower level of educational attainment for rural women may also interact with lower income to produce even greater health challenges. Higher educational attainment is associated with better general health27 and some of this difference may result from the higher incomes associated with more education28.
Maine, however, does seem to have some unique characteristics. In Maine the number of women giving birth who were married decreased as their residences became more rural (Table 1), whereas in Oregon women from rural towns were least likely to be married and women from isolated rural areas were most likely to be married13. In the case of racial diversity, the Oregon study found that the number of women giving birth who were white increased along the continuum for urban to rural13 while in Maine there was a U-shaped relationship between rurality and racial diversity with the number of non-white women giving birth highest in urban and isolated rural areas (Table 1). These results suggest that rural areas in different parts of the country are not necessarily homogeneous and highlights the importance of performing analysis of the impact of rurality on health indicators in multiple locations.
Health-related behaviors
Rurality can also affect health-related behaviors around pregnancy. A South Carolina study divided women into two categories (urban and rural) and found that rural women were more likely to be overweight or obese prior to pregnancy compared to urban women14. This result is in general agreement with the increasing BMI by rurality tier reported here for Maine (Table 2). Higher pre-pregnancy BMI is important because even small increases in maternal BMI above 25 are associated with increased risk of infant death. In a large meta-analysis, the risk of death for infants born to mothers with a pre-pregnancy BMI of 27.5 was 8% higher than the risk for infants born to mothers with a BMI of 2529.
The reason for the differences in pregnancy BMI by rurality tier reported here and elsewhere requires further study, and does not seem to be related to differences in perceptions about the barriers to exercise30. The South Carolina study found that rural women were slightly more likely to have inadequate gestational weight gain (GWG) and slightly less likely to have excessive GWG compared to urban women. The results reported here show a similar result, but only for women from rural towns and not for women from isolated rural areas (Figs2, 3), demonstrating that the use of four rather than two rurality tiers can reveal subtle differences even among rural women.
Smoking before and during pregnancy is a risk to both the pregnant woman and the fetus12. The higher rates of smoking before, during, and after pregnancy among rural women reported here (Tables 2, 3, 5) are also in agreement with previous results from Oregon13 and from older women in British Columbia, Canada31 for smoking during pregnancy. The reason for these differences in unknown. However, poverty and lower educational attainment are associated with increased smoking risk among pregnant women in South Carolina32. Thus, the lower household incomes and educational attainment reported in this study for rural women (Table 1) may help explain the high smoking rates among rural women before, during, and after pregnancy in Maine. Regardless of the reason that so many pregnant rural women smoke, the higher number of rural women who report discussion of the dangers of smoking during pregnancy (Table 4) seems appropriate. However, it is also clear that more needs to be done to reduce tobacco-exposed pregnancies in Maine and elsewhere. Interestingly, a national study found lower rates of smoking during pregnancy in rural as compared to urban women33. However, rurality was defined as a dichotomous variable at the county level - a much different approach than the one taken in the study reported here.
The finding of this study that fewer Maine women from isolated rural areas consumed alcohol before and during pregnancy compared to the number of urban women who did so is also at odds with the higher rates of alcohol consumption found for older rural women in British Columbia, Canada31 and the higher rates of alcohol-related hospital admission for pregnant rural women in Australia34. This may reflect either site-specific variability in behaviors, the younger age of rural women in Maine, or differences in experimental approaches.
Access to care and pregnancy outcomes
Lack of access to health care is commonly cited as one of the most important challenges to rural health, if not the most important challenge4. There is little question that rural life produces barriers to obtaining health care. Rural dwellers travel further to obtain their health care and visit specialists less often1. There is also evidence that, in Maine, those who live further from hospitals receive somewhat different care when they do arrive in emergency rooms with acute complaints17. However, it remains an open question whether or not these barriers are sufficient to produce differences in maternal and child health outcomes.
In Alabama in the USA, a study that defined rurality in three categories by RUCA codes (urban, large town, and small town) found different temporal trends for women from small towns for 1990-2010 in the rates of pre-term and low-birth-weight births, until by the end of the study period risks for both of these outcomes were highest among women from small towns11. However, for women over the age of 35 years in British Columbia, women from rural area had a lower risk of small-for-gestational-age birth but a higher risk of perinatal mortality compared to urban women32. In Oregon, at least, any differences in pregnancy outcomes could not be easily explained by inability to obtain prenatal care. Rural women in that state were just as likely as urban women to receive prenatal care in the first trimester and just as likely to have received it as early as they wanted13. Other studies have failed to find that rurality constitutes a measurable barrier to positive maternal and child health outcomes. A four-state study failed to find that increased travel time to a clinic predicted increased risk of teenage pregnancy or unintended pregnancy35. Caesarean section rates have also been found to be lower in rural compared to urban hospitals23, and lower for older rural compared to older urban women in British Columbia31.
The results reported here also contain little evidence that rurality is negatively affecting either access to care or the type of care given during pregnancy and childbirth in Maine. In results similar to those obtained in Oregon13 rural women in Maine started prenatal care as early as urban women and were just as likely to receive prenatal care as early as they wished, even though they were not sure they were pregnant until a slightly later gestational age (Table 4). The high rate of discussions of smoking, drinking, and breastfeeding during prenatal visits reported by rural women (Table 4) suggests that they received quality prenatal care, as do the comparable rates of hypertension during pregnancy and lower rate of gestational diabetes for women living in rural towns (Table 3). The results reported here also found no differences by rurality tier in other outcomes that could suggest lack of access to high quality care including gestational age at birth, low birth weight (Fig6, Table 5), or Caesarean section rates (Fig5). However, this should not be taken as evidence that maternal health indicators that do differ by rurality tier (eg pre-pregnancy BMI, gestational weight gain, and smoking) have no impact on newborn health. A multi-variable analysis of factors predicting poor infant health would be needed to address this point. On the other hand, it does suggest that the differences found in this study in the care rural neonates received in the hospital (less likely to be admitted to an intensive care unit and less likely to spend 6 or more days in the hospital; Fig4, Table 5) may reflect the availability of services and medical practice norms in different areas rather than actual newborn health differences across rurality tiers.
Limitations
The output of the PRAMS project is a national dataset with an extremely well respected sampling methodology, and the advantages of working with such a dataset are obvious. However, these data do come with some limitations. First, the data collected by questionnaire are self-reported. As such they may have systematic biases, particularly in biometrics (height and weight) and behaviors (smoking and drinking). However, there is no reason to believe that these biases have different impacts by rurality tier and direct confirmation of the reported data would be nearly impossible. Second, in some limited instances (eg birth weight) data from 100% of hospital births could be available from birth certificates. However, the robust nature of the PRAMS sampling method makes it very likely that this sample is representative of all Maine births and the advantages of having all study variables obtained from the same sample outweigh this limitation. Third, because the PRAMS dataset only contains information collected from women who had live births it cannot be used to assess such important health indicators as still-birth rate and perinatal mortality rate.
This study contains a report of changes in pre-pregnancy, pregnancy, and postpartum variables that may affect maternal and child health along the rural-urban continuum in Maine. This includes a range of demographic and behavioral factors that may negatively affect the health of rural dwellers and their newborns, most notably a high number of teenage pregnancies, high pre-pregnancy BMI, low educational attainment and household income, high smoking rates, and low rates of breastfeeding. However, rural women seem to have access to prenatal care similar to that of urban women, as measured by the age at which they receive their initial prenatal visit. The care rural women receive also seems similar to that given to urban women as measured variables ranging from risk factor discussions during prenatal visits to Caesarean section rates. Rates of premature and low-birth-weight births are similar for urban and rural women in Maine as well. These results highlight areas where focused pre-pregnancy and prenatal education may improve maternal and child health in rural Maine.
Acknowledgements
Many thanks to Tess F. Carley for her excellent work on the construction of the GIS used to assign rurality tiers to mothers' residence locations and to Erika Lichter for her insights into the complex world of the PRAMS dataset.
References
1. Chan L, Hart LG, Goodman DC. Geographic access to health care for rural Medicare beneficiaries. Journal of Rural Health 2006; 22(2): 140-146.
2. Ricketts TC. The changing nature of rural health care. Annual Review of Public Health 2000; 21: 639-657.
3. MacDowell M, Glasser M, Fitts M, Nielsen K, Hunsaker M. A national view of rural health workforce issues in the USA. Rural and Remote Health 10: 1531. (Online) 2010. Available: www.rrh.org.au (Accessed 14 August 2014).
4. Gamm LD, Hutchison LL, Dabney BJ, Dorsey AM (Eds). Rural healthy people 2010: a companion document of Healthy People 2010. Vol 1. (Online) 2013. Available: http://sph.tamhsc.edu/centers/rhp2010/publications.htm (Accessed 14 August 2014).
5. US Department of Agriculture. Rural America at a glance. Economic brief number 24. (Online) 2013. Available: http://www.ers.usda.gov/media/1216457/eb-24_single-pages.pdf (Accessed 14 August 2014).
6. Banks J, Marmot M, Oldfield Z, Smith JP. Disease and disadvantage in the United States and in England. JAMA 2006; 295: 2037-2045.
7. Parsons MA, Askland KD. Cancer of the colorectum in Maine, 1995-1998: determinants of stage at diagnosis in a rural state. Journal of Rural Health 2007; 23(1): 25-32.
8. Singh GK, Siahpush M. Widening rural-urban disparities in life expectancy, U.S., 1969-2009. American Journal of Preventive Medicine 2014; 46(2): e19-e29.
9. Ng AS, Kaye K. The National Campaign to Prevent Teen and Unplanned Pregnancy. Teen Childbearing in Rural America. No 47. (Online) 2013. Available: https://thenationalcampaign.org/sites/default/files/resource-primary-download/ss47_teenchildbearinginruralamerica.pdf (Accessed 14 August 2014).
10. Sparks PJ, McLaughlin DK, Stokes CS. Differential neonatal and postneonatal infant mortality rates across US counties: the role of socioeconomic conditions and rurality. Journal of Rural Health 2009; 25(4): 332-341.
11. Kent SK, McClure LA, Zaitchik BF, Gohlke JM. Area-level risk factors for adverse birth outcomes: trends in urban and rural settings. BMC Pregnancy and Childbirth 13: 129. (Online) 2013. Available: http://www.biomedcentral.com/1471-2393/13/129 (Accessed 14 August 2014).
12. Healthy People 2020. Maternal, infant, and child health. (Online) 2014. Available: http://www.healthypeople.gov/2020/topicsobjectives2020/overview.aspx?topicId=26 (Accessed 14 August 2014).
13. Epstein B, Grant T, Schiff M, Kasehagen L. Does rural residence affect access to prenatal care in Oregon? Journal of Rural Health 2009; 25(2): 150-157.
14. Gallagher A, Liu J, Probst JC, Martin AB, Hall JW. Maternal obesity and gestational weight gain in rural versus urban dwelling women in South Carolina. Journal of Rural Health 2013; 29: 1-11.
15. Centers for Disease Control & Prevention. What is PRAMS? (Online) 2014. Available: http://www.cdc.gov/prams/ (Accessed 14 August 2014).
16. RUCA Rural Health Research Center. Rural-urban commuting area codes (RUCAs). (Online) 2014. Available: http://depts.washington.edu/uwruca/ (Accessed 14 August 2014).
17. Harris DE, Aboueissa A, Hartley D. Myocardial infarction and heart failure hospitalization rates in Maine, USA - variability along the urban-rural continuum. Rural and Remote Health 8: 980. (Online) 2008. Available: www.rrh.org.au (Accessed 14 August 2014).
18. Division of Public Health Systems, Maine Center for Disease Control & Prevention Data Research and Vital Statistics. Pregnancy Risk Assessment Monitoring System (PRAMS). (Online) 2014. Available: http://www.maine.gov/dhhs/mecdc/public-health-systems/data-research/prams/index.shtml (Accessed 14 August 2014).
19. Institute of Medicine. Weight gain during pregnancy: reexamining the guidelines. (Online) 2009. Available: http://iom.edu/~/media/Files/Report%20Files/2009/Weight-Gain-During-Pregnancy-Reexamining-the-Guidelines/Report%20Brief%20-%20Weight%20Gain%20During%20Pregnancy.pdf (Accessed 14 August 2014).
20. Office of Information Technology Maine Office of GIS. Maine Office of GIS Data Catalog. (Online) 2014. Available: http://www.maine.gov/megis/catalog/ (Accessed 14 August 2014).
21. United States Department of Agriculture Economic Research Service. Rural-urban commuting area codes. (Online) 2014. Available: http://www.ers.usda.gov/data-products/rural-urban-commuting-area-codes.aspx#.U-zBgBDgdYl (Accessed 14 August 2014).
22. Washington State Department of Health. Guidelines for using rural-urban classification systems for public health assessment. (Online) 2009. Available: http://www.doh.wa.gov/Portals/1/Documents/5500/RuralUrbGuide.pdf (Accessed 14 August 2014).
23. Kozhimannil KB, Hung P, Prasad S, Casey M, Moscovice I. Rural-urban differences in obstetric care, 2002-2010, and implications for the future. Medical Care 2014; 52: 4-9.
24. NIH Eunice Kennedy Shriver National Institute of Child Health and Human Development. What are the factors that put a pregnancy at risk? (Online) 2014. Available: http://www.nichd.nih.gov/health/topics/high-risk/conditioninfo/Pages/factors.aspx#age (Accessed 14 August 2014).
25. Bombard JM, Dietz PM, Galavotti G, et al. Chronic diseases and related risk factors among low-income mothers. Maternal Child Health Journal 2012: 16: 60-71.
26. Whitehead NS, Callaghan W, Johnson C, Williams L. Racial, ethnic, and economic disparities in the prevalence of pregnancy complications. Maternal Child Health Journal 2009; 13: 198-205.
27. Cutler DM, Lleras-Muney A. Education and health: evaluating theories and evidence. National Bureau of Economic Research, NBER Working Paper Series, working paper 12352. (Online) 2006. Available: http://www.nber.org/papers/w12352.pdf?new_window=1 (Accessed 14 August 2014).
28. Picker L. The effects of education on health. (Online) 2014. Available: http://www.nber.org/digest/mar07/w12352.html (Accessed 14 August 2014).
29. Aune D, Saugstad OD, Henriksen T, Tonstad S. Maternal body mass index and the risk of fetal death, stillbirth, and infant death: a systematic review and meta-analysis. JAMA 2014; 311(15): 1536-1546.
30. Marshall ES, Bland H, Melton B. Perceived barriers to physical activity among pregnant women living in a rural community. Public Health Nursing 2013; 30(4): 361-369.
31. Lisonkova S, Sheps SB, Janssen PA, Lee SK, Dahlgren L, MacNab YC. Birth outcomes among older mothers in rural versus urban areas: a residence-based approach. Journal of Rural Health 2011; 27: 211-219.
32. Nkansah-Amankra S. Neighborhood contextual factors, maternal smoking, and birth outcomes: multilevel analysis of the South Carolina PRAMS survey, 2000-2003. Journal of Women's Health 2010; 19(8): 1543-1552.
33. Shoff C, Yang T. Understanding maternal smoking during pregnancy: does residential context matter? Social Science & Medicine 2013; 78: 50-60.
34. Burns L, Black E, Powers JR, Loxton D, Elliott E, Shakeshaft A, Dunlop A. Geographic and maternal characteristics associated with alcohol use in pregnancy. Alcoholism: Clinical and Experimental Research 2011; 35(7): 1230-1237.
35. Goodman DC, Klerman LV, Johnson KA, Chang C, Marth N. Geographic access to family planning facilities and the risk of unintended and teenage pregnancy. Maternal Child Health Journal 2007; 11: 145-152.
