full article:
Recruiting and retaining qualified nurses and other healthcare professionals to work in rural and remote areas is a continual struggle. Half of the world's population resides in rural areas yet only 38% of the nursing workforce are found in rural regions1. In Canada, 19% of the population resides in rural communities and only 10.8% of the registered nurse (RN) workforce and 17.5% of licensed practical nurses (LPNs) work in rural and remote areas2,3. Barriers to recruitment and retention of nurses in rural facilities include limited resources, professional development opportunities, and interpersonal ties to the area4. Strategies must be put in place to ensure these skilled professionals are retained so that rural communities have access to adequate healthcare resources.
Aligned with a call from WHO1, mentorship programs have been used to successfully recruit and retain rural nurses5-8. Mentorship is a mutually beneficial, non-evaluative relationship between a more experienced person (mentor) and a less experienced person (protégé), where the primary focus is professional development of the protégé. Indeed, novice nurses are better prepared to meet the challenges of rural healthcare environments when mentoring relationships are established and maintained6,9,10.
The literature abounds with examples purporting mentoring benefits, characteristics of effective mentors and protégés, roles and responsibilities of each member, and necessary elements for mentorship program creation and evaluation11-13. Even though mentorship is recognized as beneficial for easing transition of healthcare providers, there is sparse research examining rural healthcare professional perceptions of the required resources and supports to foster and sustain mentorships14. Furthermore, research identifying the facilitating and inhibiting factors to establishing and maintaining mentoring in rural environments and strategies to address these barriers is limited8,15. The shortage of rural healthcare professionals and the uniqueness of rural environments highlight the need to better understand the influence of mentorship in rural areas and identify the specific elements that facilitate and inhibit the development of these relationships16. The province of Saskatchewan has recognized the potential value of mentoring and has thus implemented a Provincial Mentorship Initiative17 to support all new healthcare employees as they transition into the workplace (see Appendix I).
The present study was conducted in one rural Saskatchewan health region with the aim to explore (i) employee perceptions of mentorship in rural healthcare organizations, (ii) the processes involved in creating mentoring relationships in rural healthcare organizations, and (iii) the organizational features supporting and inhibiting mentorship in rural healthcare organizations. The findings of this qualitative exploratory study increase understanding of rural RN and LPN perceptions of mentoring, highlight barriers and facilitators to establishing relationships, and identify effective strategies to create and sustain mentorships. They also inform the development of creative and supportive ways to establish mentorships and eliminate barriers to address the challenges specifically associated with integration of newly hired nurses into rural practice4.
Study information was distributed to managers and employees in one rural health region of Saskatchewan, Canada. One rural facility manager volunteered her facility to participate. The facility supports acute, respite, and long-term care client needs and employs more than 100 people. The local community population is less than 1500, but the facility serves an area of approximately 20 000. The nearest urban center is 200 km away. Eligible participants were any frontline health profession employees (ie physicians, RNs, LPNs, special care aides, continuing care assistants, physical therapists, occupational therapists) who were employed by the rural healthcare organization. Participation was voluntary and a consent form was completed by participants prior to data collection. A semi-structured interview guide was used to facilitate the interview process and all interviews were digitally audio-recorded. The interviews focused on exploring and gaining an understanding of participants' perceptions of mentorship in rural communities using open-ended interview questions that addressed the study objectives. Follow-up interviews were conducted when required to verify and confirm emerging concepts and relationships. During the interviews, research questions were altered to seek out alternative associations or exceptional circumstances18, and insights from the early interviews were incorporated into ongoing data collection.
Interviews were transcribed verbatim and reviewed for errors or omissions. Data were managed using NVivo v10 qualitative software (QSR International; http://www.qsrinternational.com) and analyzed using interpretive description methodology, considering what findings mean individually and how they relate to one another, identifying processes and structures in relation to relationships, and prioritizing or sequencing key conclusions19. Interpretive description places high value on participants' subjective perspective and knowledge of their experience. Initial coding was broad to categorize global themes and ideas. Constant comparative analysis was used to examine and compare data to consider relationships, similarities, and differences.
Ethics approval
Ethics approval was obtained from the University of Saskatchewan Research Ethics Board (#13-30).
Seven female participants volunteered to be interviewed. All were RNs or LPNs with experience ranging from less than 1 year to more than 35 years. Five participants were interviewed in a private room at the rural healthcare facility, one in the primary researcher's office, and one by phone. Two follow-up interviews were conducted. Five participants had been both a mentor and a protégé in the past and two only had experience as a protégé. Only some had participated in the formal mentorship program offered by the province of Saskatchewan and the participating health region; the remainder had been involved in informal mentorships.
The new nurse in a rural community
Nurses expressed the stress associated with being in charge of an entire rural facility - clients, staff, and building. Participants described the multiple 'hats' they wore, particularly after standard working hours:
Occupational therapy and physiotherapy is the nurse's job ... and we are very much the plumbers, the floor washers and the dietary people after hours. (Employee F)
These multiple responsibilities were extremely intimidating for new employees:
I've noticed you get thrown into things a lot quicker and there's a lot more responsibility than if you were working in the city. (Employee A)
These working conditions were seen as directly related to difficulties with recruitment and retention:
As a registered nurse, you are in charge of not only the nursing, the clients, but you're in charge of every other department on night shift. Yes you have a rural manager on call in the event that there is something, but you are responsible in your decision making. It's a huge responsibility. And you wonder why it's hard to get young nurses to come to rural [areas]? (Employee C)
The diversity and complexity of patients coming into the rural emergency department and the variety of patients being cared for were seen as both exciting and challenging. However, this range of patients and unpredictability added to feelings of being overwhelmed and intimidated:
Well it can be quite scary for a new nurse coming to a rural facility and in particular if you have an emergency room, it's scary because you don't know what's coming through the door. (Employee B)
The role of mentorship in rural healthcare environments
Mentorship was seen by participants as an integral component to new employee transition into rural healthcare facilities:
If there was a formal mentorship program, then it would be easier to transition. (Employee B)
All participants described mentorship as a supportive relationship between a more experienced person and a less experienced person for the purposes of smoothing the transition to the rural healthcare facility. Nurses believed the mentor role was about being available for questions, guidance, direction, and decision-making support. Staff did not talk about benefits for the mentor or the organization; their definition of mentorship focused solely on the development of new staff members:
Mentorship to me is when a seasoned nurse takes a person just entering their career under their wing and just tries to help them with the growing process. (Employee G)
Mentorship was seen as a strategy to support nurses in a variety of contexts due to the complexities and stressors of working in a rural area. Nurses believed mentorships assisted with alleviating feelings of isolation and provided someone with whom to discuss the mixed emotions of the transition experience:
Sometimes it can be hard to find your way into a small town, [and] tightly knit, staff group. And everybody has their ways, and when you don't know the ways or you want to try and change things, it can be tough. But with a mentorship, you got that friend there that you can talk to about tough days, and they'll help you through. (Employee E)
Rural mentorship was also seen as a tool to recruit new graduate nurses:
It's not just the shock of graduating, but if you're hoping to have some of those nurses move into the rural area, the mentorship program is definitely a way to facilitate that and to make it easier and to recruit people because there's so much already going on in the mind of a new grad, that to ask them to move to a community where they don't know anybody, where they're starting a completely new job, with a large amount of responsibility, that's a lot. (Employee B)
Transitioning to rural healthcare through mentorship
Participants believed mentorships facilitated the transition to rural healthcare environments and were vital to the personal and professional success of new employees in rural areas. This transition was influenced by three factors: rural community influences, organizational influences, and mentorship program influences (Fig1).
Rural community influence: Participants recognized that the rural environment offered unique challenges and opportunities for the transition of new employees. New nurses often experience a lack of anonymity in the rural community:
... you don't know anyone, and everyone else knows you're the new nurse in town, that can get a bit intimidating too ... someone will walk up to you and say, 'Oh hi, I'm so and so. I heard you're the new nurse in town'. (Employee F)
Nurses felt that community members were cognizant of community healthcare professionals and sometimes could be skeptical of new members.
Nurses believed that the external rural community was integral in welcoming and integrating the new employee. If nurses were not welcomed into the community or did not integrate themselves into it, then they typically did not stay:
I have a friend who came to the community to work and she did not have either local friends or community connections and moved after a year because there was no life for her outside of work. (Employee D)
Participants recognized the importance of social connections beyond the workplace. Newly hired employees needed to be encouraged and supported to meet others in the community who had similar interests. Participants also acknowledged the importance of establishing external peer networks:
It was important ... that she met people that were her age and found someone who could actually help link [her] to the community because we don't have a lot of young staff here. (Employee F)
Nurses recognized it was sometimes difficult to build relationships with others within the community due to the very close-knit nature. Staff members also perceived more limited social opportunities in rural environments compared with urban centers, and recognized the importance of encouraging new staff members to become involved with local community events. Employees believed having a mentor could facilitate new staff integration and allow them to get to know the community better. Some participants suggested assisting with new employee integration into the community was not only the responsibility of the mentor, but also that of all staff in the facility:
It would be wonderful if perhaps that transition into the community wouldn't be just on the shoulders of the mentor but also the whole staff, saying you know, 'we're going to help you get to know the community. What are your interests? How can we do that?' (Employee B)
While most communities were welcoming of outsiders, some onus was on the new employee to build new relationships:
... it does take a bit of initiative on that individual to seek out social opportunities and take advantage of them. (Employee B)
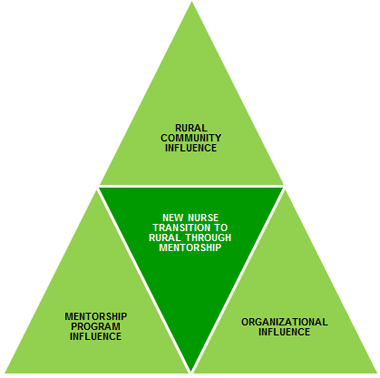
Figure 1: Model for transition to rural health care.
Organizational influence: Participants discussed numerous organizational limitations with respect to the transition of nurses to the rural environment. Limited staffing put new employees under considerable pressure to make sound decisions and to have good judgement:
... we're very limited in support systems, it is just you and I, two nurses, maybe three. We have to be the very best nurse because we don't have supports. (Employee C)
In particular, nurses described isolation and lack of support in their decision making at night when only one RN or LPN is on shift:
... it's a very different workplace than working in the city. And it can be very scary for them [new staff] because we have one RN, one LPN on a night shift. And we do get some very sick people. (Employee F)
Nurses saw the benefit of having a mentor to ease the stress of independent decision making and to serve as a sounding board to facilitate sound judgement.
However, the limited staffing in the rural facility was also seen as a positive factor with respect to new employee transitions, because personnel were able to develop closer, cohesive working relationships. All participants described co-workers as 'family':
In rural [nursing], you really get to know somebody. I know when we're on call and it gets really busy and everybody's slammed, you're not just going to walk out and leave the night staff because you care about them and it's more of a family than just a working office. (Employee A)
Most participants described the close relationships that developed and that mentorships could be more easily fostered due to these positive relationships:
And they were just so just friendly and embracing of [me]. They just made me feel really appreciated that I was coming to work casual. One of the staff members gave me a hug my first day and she was just so happy that I was here. I think that just that positive environment makes you want to stay. And so that kind of begins the relationship off in a good way. (Employee B)
Participants indicated these close relationships enhanced work environments: they were more inclined to ask for colleague feedback and opinions and trust was easier to establish:
I think in rural, there's a lot more time for the personal aspect and so you can get to know your mentor better and become more comfortable in confiding in that person, and then as soon as you're comfortable with and feel safe with your mentor, I think then you have the ability to become more comfortable in your career. (Employee E)
Staff believed they took responsibility for facilitating and assisting mentorships by being an additional knowledge resource, allowing time for those relationships to develop, and providing for additional learning opportunities to the new employee even if they were not formally assigned:
I don't think the mentee should only ask their mentor questions for support. I think that in rural [nursing], it should just be a universal relationship with everybody where that new nurse can go and ask their opinion or a question and it's completely supported. (Employee A)
Benefits and barriers of rural mentorship: Formal rural mentorship programs were seen as an essential component to enhancing and supporting new staff development and success in the rural area:
It's important in rural to have a mentor so they can talk to someone, that they know it's a confidential relationship and they can tell them anything they want and they can talk about issues and things that they have when they work their shifts, because they can feel pretty alone and isolated. (Employee F)
Notably, however, not all staff were aware of or took advantage of the formal mentorship programs available with the health region.
Some participants indicated that a mentorship program was considered a recruitment tool:
... you know there's going to be support there when you move and you know that even if you commit to a year, it's less scary because you know there's going to be resources there to help you transition into the community ... I think it would be absolutely more appealing. (Employee B)
Participants who had been mentored and those who had mentored new employees into their rural positions expressed the profound significance of the relationship on the new employee's decision to remain in the position and community. When speaking of her mentor, one employee stated:
She really knows the community. She knows the people. She knows the dynamics. And without her, I don't know if I actually would have stayed in that position. (Employee B)
Participants expressed that a mentorship program would be invaluable to assist with decision-making support and the onus of having the responsibility of looking after the entire facility, staff, and building. Mentorship gave new employees the confidence and security to be able to do what was expected of them in their role. Participants believed that mentorships were also beneficial to the mentor:
Actually, I learned a lot about myself, I was fairly new nurse so I was feeling like, 'am I really doing a good job?' I learned where my strengths were in my nursing career and even in my interpersonal connections with my other work mates, I learned and grew just from teaching somebody else. (Employee D)
Employees also discussed the reciprocal learning that occurred between a mentor and protégé:
You learn so much from each other. We have even talked about different things that we learned from each other which was kind of cool, that I got to give her something back too. (Employee E)
New employees talked about becoming mentors to new staff because of their positive experiences with mentorship:
... everything that she did for me, I would love to do for somebody one day. (Employee E)
Many nurses felt one barrier to mentorship was the lack of staff working at one time. For example, one LPN and RN would be working together, resulting in limited opportunities for same-profession mentorship on a given shift. Moreover, same-profession staff would often not have time off together, making it hard for mentor/protégé dyads to meet outside of work. A related challenge was the limited selection of available and willing mentors in rural settings to best meet protégé needs. If a trusting mentorship was not developed, finding another mentor was difficult:
You don't have very many people to draw from for support, there are only so many of us that work. Just like if you can't establish a good friendship with the mentor or the person being mentored, and there's nowhere else for them to go to, it can be very difficult. (Employee D)
Participants felt mentor selection was essential to the success of the mentorship:
Ask people to be mentors who are truly interested in their job, who have a good work ethic and are a good example for the new nurses coming. People who are non-judgmental and the ones who will sit back and listen, not just be the bossy, chirpy ones who want to control everything, because you really have to let those new nurses develop their art of nursing. (Employee F)
Employees discussed the importance of a personality connection between the mentor and protégé in order for mentorships to be successful. They suggested completing personality questionnaires to aid in matching. Participants felt protégés should have input with respect to mentor selection. One newer nurse suggested getting to know staff first before establishing a formal mentorship with an individual:
I knew their personality, I got to know them a bit better. And I think with rural [nursing] you're going to be working with the same seven RNs all the time. It makes a big difference knowing who you get along with. If I was assigned to somebody who I didn't feel comfortable with, it would have made a complete difference. (Employee A)
One newer staff member highlighted the struggles to actively seek out mentorships when new to the area and suggested the onus should be on the manager or facility to assist with the establishment of such programs for new staff:
It's hard when you're new to walk in and seek out those mentorship programs. It's hard to go up and figure out who you can go to. I think you have to be a very assertive person to walk into a new work environment and say, 'Hey, do you want to be my mentor?' I mean not to say that it can't happen but I think those assertive people that reach out are the ones that are going to do just fine. It's the ones that are not as assertive that probably would really benefit from mentorship. (Employee B)
Regardless of how the mentorship was established, developing trusting relationships was a pervasive topic during interviews. Trust needed to be established before the relationship could be fostered:
An obstacle for mentorship would be if one person in the relationship doesn't trust the other person with their feelings and their thoughts. (Employee F)
After a trusting foundation was established, the protégé would feel more comfortable in sharing challenges or struggles and the mentor would feel more comfortable providing feedback. The mentor would act as a confidante:
To me that's what a mentor is, is that trusting relationship, that go to person for whatever you need. You want them to be that trusting friend as well. (Employee C)
Participants acknowledged that employees needed an awareness of mentorship. For example, they believed employees needed to know what the mentorship process entailed in order to establish and sustain such relationships. Participants were unaware of any specific resources about mentorships within their region or facility. They expressed a desire for more information about program objectives, roles and responsibilities of mentor/protégé, relationship development strategies, benefits/drawbacks/common challenges for mentorships, and methods for overcoming them. They appreciated hearing personal stories of mentorship and strategies for success. Overall, mentorship education was seen as an essential, yet lacking, component, and participants felt they were often thrown into formal mentorships with little or no training:
I really got nothing. It was like 'here's your mentor' and that was pretty much it. So it was kind of up to me and my mentor to figure out what our relationship was as opposed to having information. (Employee A)
Some participants knew introductory mentorship workshops were available in urban centers within the health region. However, most participants believed they must be offered in rural settings as it was difficult for them to get approval, funding, and time off to attend:
... it would be either not approved by management or you'd have to pay out of your own pocket to go and attend the workshop. So maybe if you offered [the mentorship workshop in] one central rural area once a year then people can travel to [a more urban rural town] where it's not far. (Employee A)
Staff suggested sessions would be more convenient if available to them electronically (eg online webinars, tele-health) or in the rural facility.
Discussion
These study findings indicate the rural community and its healthcare facilities present challenges for the transition and mentorship of nurses new to rural areas. Inhibiting factors to establishing and maintaining mentoring in rural environments have been identified and strategies to reduce or eliminate these barriers should be made by employers, employees, and new staff in order to ease transition and foster recruitment and retention. Overall, the study results support the need for rural-specific formal mentorship programs. Employers recognize formal mentorships as useful strategies to support new staff, reduce turnover, and enhance retention; however, considerable time, commitment and money are required for consistent delivery of programs9,20-23. The fact that some participants were unaware of the mentorship program in place in Saskatchewan is concerning. Mentorship education and awareness as well as program promotion should be of top priority within organizations in order to encourage uptake amongst healthcare providers. Thus, this process could benefit from some facilitation, perhaps through the creation of a rural-specific mentorship coordinator position. This individual could promote rural mentorships, provide general information about establishing mentorships in rural environments, assist with matching mentors and protégés, develop mentorship workshops, provide follow-up and consultation with the dyad, provide educational resources, and evaluate the formal program. All participants in this study noted the desire for more information related to formal mentorship program components.
Mentoring education and training are considered a continuous part of organizational culture24. Education can be offered via tele-conferencing, video-conferencing, or web conferencing as a reasonable alternative to in-person mentoring education given financial constraints and remote locations. Education regarding mentoring programs is integral to implementation and sustainability5, but mentor volunteering and selection often became challenging in rural areas25. By providing mentoring education, a pool of mentors could be created to ease concerns regarding the low numbers available in rural areas. Connecting mentors and protégés who are in different locations via technology can enable long-distance relationships8 and also increase the potential number of participants.
Multiple mentorship opportunities can be an option for limited availability of mentors whereby one mentor is involved in simultaneous one-to-one mentoring relationships with more than one protégé11. Some consideration must also be given to the matching of mentor and protégé, be it by a third party, nurse managers, or self-selection26, as this is a crucial element to a successful mentorship6,27. As in other studies28, participants in the present study noted the desire to have some input into the matching process. Mentors and protégés perceived greater mentoring program effectiveness when they had input into the matching process as it allowed for a greater mutual connection and 'good fit' between the dyad29,30. Participants expressed the need for allowing time to develop the relationship and establishing trust between the dyad. Research has found that a trusting relationship between mentors and protégés resulted in the protégé feeling more comfortable asking questions, performing procedures, requesting and accepting feedback, and being socialized into the new role31. Thus, the dyad needs to prioritize time both within and outside of work to develop their relationship.
Lack of anonymity and dual relationships within the rural community were common elements discussed amongst participants; these reflect findings wherein nurses must learn to manage the competing perspectives of community member and nurse32 and accept that these roles are blurred33. Nurses are interconnected and highly visible members of the community, which can lead to lack of privacy and increased stress if pressured to divulge confidential information about clients20,34. Mentors can provide suggestions for how they maintain these dual relationships while also keeping confidentiality a priority.
Such aspects may seem at odds with the importance of establishing connections with the community35,36. The nurses in this study highlight the need for new staff to establish roots in the community outside of the work context37, as such interaction is an incentive to stay, live, and work in the rural community36,38. The results suggest roles for facility staff as a whole, the mentor, and the protégé in the transition process, with the onus on the mentor to introduce the new staff member to individuals outside of the healthcare facility and encourage and engage protégés in external social functions, and the staff providing additional support; the new nurse must also be motivated and proactive in seeking out these social community activities.
The RN participants in this study were often expected to make triaging and management decisions beyond their level of confidence and competence due to limited staff, and found themselves in leadership positions simply by being the only RN in the building. Notably, nurses new to rural healthcare facilities may gain a significant amount of clinical knowledge through social contexts and interpersonal relationships, often relying on and collaborating with colleagues to assist in decision making; mentorship of novice nurses in rural environments can be especially important in the development of the clinical reasoning and judgement needed to facilitate positive client outcomes39. Some individuals expressed that the reassurance of a mentor eased their anxiety with respect to the unpredictability of what was coming into the emergency room or being in charge of the entire facility. A mentor could be present within the building or be available on-call as needed when new staff members are on shift to allow for decision-making support.
Study limitations
There is limited generalizability with this study as it was conducted in one rural facility with nurses only. Seven nurse participants were included and their perceptions may not be representative of all healthcare professionals working in rural environments. Others' perspectives are missing and warrant further investigation. As the authors were reliant on study information being distributed by a third party to prevent coercion, all eligible facilities and healthcare employees may not have received the information.
Five participant interviews were conducted in person at the rural healthcare facility and their responses may have been influenced by the work setting. Participants who volunteered may have had positive experiences with mentorship only; those individuals whose relationships were not successful may have chosen not to participate.
Working in rural healthcare settings is multifaceted and complex and many newly hired nurses struggle with transition to these contexts. Mentorship was described as a vital component to personal and professional success of new employees in rural areas and special considerations for mentorship must be addressed. Results of this study will allow employees, healthcare organizations, and government agencies to better understand the specific mentoring needs of rural healthcare employees and facilities. While more research in this area is recommended, the findings will inform the development of future mentoring programs in rural facilities and health regions to enhance capacity development of healthcare professionals. Mentorship can serve as a means to recruit and retain nurses in rural areas, where having adequate, qualified, competent employees is crucial to ensuring the health of rural populations and communities.
References
1. World Health Organization. Increasing access to health workers in remote and rural areas through improved retention: global policy recommendations. Geneva, Switzerland: WHO, 2010.
2. Canadian Institute for Health Information. Regulated nurses: Canadian trends, 2007 to 2011. Ottawa, ON: Canadian Institute for Health Information, 2012.
3. Statistics Canada. Population, urban and rural, by province and territory (Canada). (Internet) 2011. Available: http://www.statcan.gc.ca/tables-tableaux/sum-som/l01/cst01/demo62a-eng.htm (Accessed 25 January 2016).
4. Aylward M, Gaudine A, Bennett L. Nurse recruitment and retention in rural Newfoundland and Labrador communities: the experiences of healthcare managers. Online Journal of Rural Nursing and Health Care 2011; 11(1): 54-69.
5. Block LM, Claffey C, Korow MK, McCaffrey R. The value of mentorship within nursing organizations. Nursing Forum 2005; 40(4): 134-140.
6. Scott ES, Smith SD. Group mentoring: a transition-to-work strategy. Journal for Nurses in Professional Development 2008; 24(5): 232-238.
7. Curran V, Hollett A, Hann S, Bradbury C. A qualitative study of the international medical graduate and the orientation process. Canadian Journal of Rural Medicine 2008; 13: 163-169.
8. Bourke L, Waite C, Wright J. Mentoring as a retention strategy to sustain the rural and remote health workforce. Australian Journal of Rural Health 2014; 22: 2-4.
9. Mills JE, Francis KL, Bonner A. Mentoring, clinical supervision and preceptoring: clarifying the conceptual definitions for Australian rural nurses. A review of the literature. Rural and Remote Health (Internet) 2005; 5: 410-450. Available: www.rrh.org.au (Accessed 25 January 2016).
10. MacPhee M, Scott J. The role of social support networks for rural hospital nurses: supporting and sustaining the rural nursing work force. Journal of Nursing Administration 2002; 32(5): 264-272.
11. Grossman SC. Mentoring in nursing: a dynamic and collaborative process. 2nd edn. New York, NY: Springer, 2014.
12. Johnson WB, Ridley CR. The elements of mentoring. 2nd edn. New York, NY: Palgrave Macmillan, 2008.
13. Fox K. Mentor program boosts new nurses' satisfaction and lowers turnover rate. The Journal of Continuing Education in Nursing 2010; 41(7): 311-316.
14. Mills J, Francis K, Bonner A. Getting to know a stranger - rural nurses' experiences of mentoring: a grounded theory. International Journal of Nursing Studies 2007; 45: 599-607.
15. Rohatinsky N, Ferguson L. Mentorship in rural healthcare organizations: challenges and opportunities. Online Journal of Rural Nursing and Healthcare 2013; 13(2): 149-172.
16. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health (Internet) 2009; 9(2): 1060. Available: www.rrh.org.au (Accessed 25 January 2016).
17. Government of Saskatchewan. Provincial Mentorship Initiative. (Internet) 2016. Available: http://www.saskatchewan.ca/government/health-care-administration-and-provider-resources/resources-for-health-care-businesses-and-career-development/provincial-mentorship-initiative (Accessed 25 January 2016).
18. Thorne S, Reimer-Kirkham S, O-Flynn-Magee K. The analytic challenge in interpretive description. International Journal of Qualitative Methods 2004; 3(1): 1-11.
19. Thorne S. Interpretive description. Walnut Creek, CA: Left Coast Press, 2008.
20. McCoy C. Professional development in rural nursing: challenges and opportunities. Journal of Continuing Education in Nursing 2009; 40(3): 128-131.
21. Gibb H, Anderson J, Forsyth K. Developing support for remote nursing education through workplace culture that values learning. Australian Journal of Rural Health 2004; 12: 201-205.
22. MacKinnon K. Learning maternity: the experiences of rural nurses. Canadian Journal of Nursing Research 2010; 42(1): 38-55.
23. Stewart S, Wootten R. A survey of e-mentoring among New Zealand midwives. Journal of Telemedicine and Telecare 2005; 11(2): 90-92.
24. Zachary LJ. Creating a mentoring culture: the organization's guide. San Francisco, CA: Jossey-Bass, 2005.
25. Lynds D, van der Walt SJ. Mentoring in rural emergency departments: challenges and opportunities. In: E Ralph, K Walker (Eds). Adapting mentorship across the professions: fresh insights and perspectives. Calgary, AB: Detselig Enterprises, 2011; 73-85.
26. Blake-Beard SD, O'Neill RM, McGowan EM. Blind dates?: The importance of matching in successful mentoring relationships. In BR Ragins, KE Kram (Eds). The handbook of mentoring at work. Los Angeles, CA: Sage, 2007; 617-632.
27. McKinley MG. Mentoring matters: creating, connecting, empowering. American Association of Critical-Care Nurses Clinical Issues 2004; 15(2): 205-214.
28. Eby LT, Lockwood A. Proteges' and mentors' reactions to participating in formal mentoring programs: a qualitative perspective. Journal of Vocational Behavior 2005; 67: 441-458.
29. Allen TD, Eby LT, Lentz E. Mentorship behaviors and mentorship quality associated with formal mentoring programs: closing the gap between research and practice. Journal of Applied Psychology 2006a; 91(3): 567-578.
30. Allen TD, Eby LT, Lentz E. The relationship between formal mentoring program characteristics and perceived program effectiveness. Personnel Psychology 2006b; 59(1): 125-153.
31. Beecroft, PC, Santner S, Lacy ML, Kunzuman, L, Dorey F. New graduate nurses' perception of mentoring: six-year programme evaluation. Journal of Advanced Nursing 2006; 55(6): 736-747.
32. Mills J, Lennon D, Francis K. Contributing to a culture of learning: a mentor development and support project for Australian rural nurses. International Journal of Nursing Practice 2007; 13: 393-396.
33. Lea J, Cruickshank MT. Factors that influence the recruitment and retention of graduate nurses in rural health care facilities. Collegian 2005; 12(2): 22-27.
34. Kenny A, Endacott R, Botti M, Watts R. Emotional toil: psychosocial care in rural settings for patients with cancer. Journal of Advanced Nursing 2007; 60(6): 663-672.
35. Buykx P, Humphreys J, Wakerman J, Pashen D. Systematic review of effective retention incentives for health workers in rural and remote areas: towards evidence-based policy. The Australian Journal of Rural Health 2010; 18: 102-109.
36. Cameron PJ, Este D, Worthington CA. Professional, personal and community: 3 domains of physician retention in rural communities. Canadian Journal of Rural Medicine 2012; 17(2): 47-55.
37. Bennett P, Brown J, Barlow V, Jones D. What do new graduate registered nurses say they want from jobs in remote communities? The Australian Journal of Rural Health 2010; 18: 212-213.
38. Penz K, Stewart N, D'Arcy C, Morgan D. Predictors of job satisfaction for rural acute care registered nurses in Canada. Western Journal of Nursing Research 2008; 30(7): 785-800.
39. Sedgwick M, Grigg L, Dersch S. Deepening the quality of clinical reasoning and decision-making in rural hospital nursing practice. Rural and Remote Health (Internet) 2014; 14: 2858. Available: www.rrh.org.au (Accessed 25 January 2016).
_________________________________
Appendix I: Current state of mentorship in Saskatchewan for regional health authorities


