Introduction
The Sustainable Farm Families (SFF) and the Sustainable Dairy Farm Families (SDFF) projects have been developed through a process of intersectoral collaboration involving health services, universities, agricultural agencies, training organisations and farming communities. Together these bodies have combined through an evidence-based research approach to address the poor health status of the farm family.
Often in healthcare delivery what is needed is seen in terms of the imperative for healthcare providers to 'go forth and deliver' health information and knowledge to satisfy the requirements set by healthcare funding bodies. However, current evidence from health promotion and adult learning informs us that the approach used can either stifle or encourage the attainment of knowledge by population groups1. Research undertaken by Rydhom and Kirkhorn using county fairs as avenues of health education and change mechanisms revealed a positive effect on farm practices and health behaviours, evaluated by six-month telephone survey2. Studies examining farm-safety related knowledge assessed by McCallum et al. revealed significant retention in pre- to post-knowledge at a 3 month interval in 8-13 year-old age groups, and indicated that studies over longer periods and with adult populations would provide greater insight3. In this article we report on an approach to learning for farm families over a period of 3 years that includes physical assessment, referral, pre- and post-knowledge surveys and workshops that result in a change in behaviours for farm families.
Rural hospitals have traditionally focussed on the acute and aged-care aspects of health service delivery with rural communities concerned over the number of acute and aged care beds in their hospital, rather than the number of healthy people in their communities. Western District Health Service (WDHS) is a rural health service located in the Western District of Victoria providing health care for a direct population of 17 000 and surrounding population of approximately 37 000 people. The WDHS developed a community services division in 1998, which focuses on preventative health and early intervention including programs such as rural men's and women's health. Success within these structured five-week education and assessment programs and strong background in farming and agricultural networks led to the application for funding through the Joint Research Venture on Farm Health and Safety managed through the Rural Industries Research and Development Corporation (RIRDC). Understanding the need for intersectoral collaboration, an alliance was developed with Royal Melbourne Institute of Technology (RMIT) University, Farm Management 500 (FM500; a benchmarking farmer group), Land Connect Australia (a training organisation) and the Victorian Farmers Federation (VFF) to undertake a 3 year study of farm family health in broadacre farmers producing mainly beef, wool and grains in Victoria (Benalla, Horsham, Hamilton, and Swan Hill, including farmers from southern New South Wales) and South Australia (Clare). In addition to the initial success of this project, funding was secured from the Geoffrey Gardiner Foundation to undertake research into 210 dairy farmers across 11 sites within Victoria over an additional 3 years. The results of the broadacre project and initial dairy findings are reported in this article.
History
In understanding the attitudes of the Australian farm population to health and wellbeing, one needs to empathise with the underlying cultural characteristics of the farm family unit: a strong work ethic, lower socio-economic status, high level of injury and risk taking behaviours and, as a rural population, higher per capita levels of disease rates and morbidity4. Farmers are ageing, working harder and longer, and increasingly relying on family members to provide the extra labour needed to survive in today's environment of climatic change and agricultural strain5. As commented by Troeth, farmers experience higher death and morbidity rates than the Australian population, they are over-represented in injury statistics, and have varying levels of socio-economic disadvantage6. In addition, residents of rural areas have a below average life expectancy. This is confirmed by the Australian Institute of Health and Welfare, which notes that the general health of rural people is, by urban standards, very poor7. Rural populations also experience above average rates of premature mortality through heart disease, cancer and suicide. This is consistent with research conducted by Fragar and Franklin who noted that male farmers face a 40% increase in age-standardised deaths compared with the general male population8. Cancer, farm injury, cardiovascular disease, and suicide account for this increased mortality in the farmer population. International research also highlights hearing deficits9. Farm-work practices can also result in pesticides being taken into the home where children and spouses are exposed10. Suicide rates across most age groups for men are higher in rural and remote centres and for women in the 30-44 year-old age group11. While the cost of farmer illness, injury and accidents is not known, it has been noted that the full costs of farm injury and illness are probably not being borne by the industry8.
The SFF catch phrase: 'There's no point in having a healthy bottom line if you're not there to enjoy it' was reinforced throughout the project. As one farmer noted, they invest heavily in stock health, natural resource and financial management, yet pay little attention to the health of their own families. The SFF project approach relies on intersectoral collaboration to illustrate how good health, wellbeing and safety practices relate to farming productivity, profitability and healthy communities.
As is shown (Fig1), farmer health is a complex issue that has a ripple effect on the farm, the farm family unit and the local community. Poor farmer health outcomes may be improved with early intervention and ongoing health maintenance, with flow-on benefits to profitability and to family and rural community members in the long term.
The SFF and SDFF projects have also created interest amongst rural health professionals keen to learn and be a part of this education and research process.
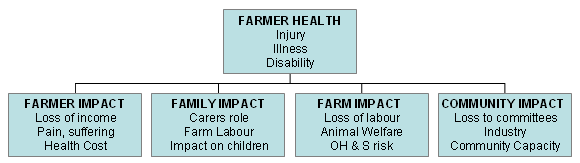
Figure 1: The flow-on effect of poor health for farmers, families, farms and communities12.
Methods
Methodological background to project
In developing the SFF and SDFF, theories and principles were used to inform and formulate a new approach. Development of education programs needed to be specific to farm men and women who may have differing levels of education and comprehension. Azjen and Fishbein's theory of 'reasoned action and planned behaviour' guides the learning experienced by participants in the SFF and SDFF projects13. Their theory suggests that behaviour changes in this program occur through:
- the sharing of values and beliefs about health of the farming peer group
- a common commitment to individual physical and knowledge assessment
- sharing with peers how best to influence health outcomes
- understanding the consequences of poor health and safety behaviour on farming families.
This process of learning is essential for farm families and allows particular focus on issues such as farm health and safety, the role of good farm practices, and the affects on the farm family unit. This process has allowed participants to use the experience and support of their peers to make informed choices and identify behaviours that effect farming family health.
The training and delivery model is based on Kolb's learning cycle, which allows participants to follow a systematic approach to identify and comprehend new information14. Kolb's model uses the principle that individuals reflect on their own experiences, acquire new concepts, actively experiment with new ways of working, which become part of their experience base. This learning is supported by videos, graphs, statistics and reflection on one's own practice. In summary, the Kolb learning model is based on his observations that people learn through a series of iterations in which they:
- Immerse themselves in the learning.
- Reflect on their own concrete experiences of an issue, or topic.
- Acquire new concepts, information, understanding, and/ or attitudes about the issue.
- Plan to use new knowledge and understand change in their own context.
The strength of the SFF project is one of continued support and trust in the delivery team (health professionals with expertise in women's, men's and rural health) enabling ongoing learning for all participants. Key collaborative partners assist in the recruitment, maintenance and coordination of participants.
The workshop is evaluated using Kirkpatrick's training evaluation framework15. This approach to evaluation includes four levels and is carried out over 3 years.
- positive experience - evaluate reaction of participants
- conceptual understanding - evaluate learning of participants
- can the learnings make a difference - evaluate behaviours of participants
- demonstrable outcomes - evaluate results of the workshop.
Rogers research on the diffusion of innovation helps us to understand how new ideas and practices are adopted in groups16. His work, which included adoption of innovation among farming communities, defines diffusion as 'the process by which innovation is communicated through certain channels over time by members of a social system'. The SFF projects involve a number of key groups to assist in the early adoption of the health and safety practices advocated in the program. Importantly, the most powerful group is the farmers who participate in this program and who meet regularly to discuss farming matters, which now include health, wellbeing and safety. The FM500 group was chosen for this research because they are known as innovators in farm management and can be considered 'innovators' and 'early adopters' in Rogers' typology. Our rationale in working with this group is to obtain evidence on the relationship between health, farm related accidents and farm business sustainability. We wanted to target early adopters to refine the workshop approach, identify issues and engage with them on a three-year health and wellbeing program.
The education process
Designing the education process meant considering the specific learning needs of participants and the timelines for the project. Previous learnings and feedback from rural men's and women's health projects, and further input from the registered training organisation and university enabled the process to be developed more fully. As a pilot, the project allowed for constant critical review, adjustment and evaluation throughout the timeframe.
A resource manual was developed and guided by Kolb's14 approach to aid in the learning process of participants. A registered training organisation was contracted to assist in the design and coordination of the resource manual; RMIT University assisted in the development of research-based frameworks and the selection of data gathering techniques for the project. Recruitment of participants was coordinated through FM500 and the VFF. Other collaborative partners included Australian Women in Agriculture, Department of Primary Industries and Meat and Livestock Australia. A steering committee was formed with quarterly meetings in both metropolitan and rural areas. Issues such as time of delivery, venue, resources, coordination and facilitation were reviewed by the steering committee and all points of view were considered in the development of the delivery process. This unique collaborative process allowed for all partners to be involved in the structure and logistics of the program rollout.
This groundwork is now seen as essential to the success of the project with the formulation of a collaborative steering committee of health, university, agricultural and industry representatives working together to improve the health of farming populations. Teleconferencing into local FM500 meetings and explanation of the education and assessment process assisted recruitment of farming family members, involving both men and women and extending to multiple generations within farm families. Early findings were that recruitment was enhanced by the provision of a full 30 min physical assessment within the program. This was again reinforced when participants were asked why they came to the first session and the majority answered that the physical assessment was a major reason.
Ethics approval was sought from the South West Health Care Ethics committee and was granted on the undertaking of specific objectives. The committee made several recommendations including the need to refer participants with fasting cholesterol levels greater than or equal to 5.5 mmols to their GP and to use the Heart Foundation's minimal requirements for exercise17. The formation of a health record on each participant with the safe storage of these records was also recommended; these records are stored at the WDHS in Hamilton. All participants required a signed consent and this was recorded in their medical record.
To be eligible to participate in the SFF program all participants were required to be aged between 18 and 75 years and to speak English. Participants were required to be involved in active farming over the last 5 years. Both husband and wife were considered to be participants, and if other family members such as parents and children were employed or actively employed within the farming enterprise they too were eligible to participate.
Delivery and methodology
The SFF program consists of a structured two-day workshop in year 1 and a one-day workshop in years 2 and 3. Participants were recruited from the industry partners and collaborative partners for each of the programs. Contacts with each participant were made by phone and mail, and a plain-language statement and consent form was signed and returned to WDHS. Information regarding the timetable, venue and fasting requirements was also sent out 4 weeks prior to program delivery. Industry knowledge in relation to time of year and workshop locations was vitally important. On the day of the program and prior to the topic delivery, a facilitator (non-health professional) would undertake a focus group discussion with group participants. This allowed for exchanging ideas, the introduction of participants and a general understanding of the project content. During this stage a group of questions were asked regarding their farming business, reason for attendance and the current value of good health to their farm entity.
A pre-session questionnaire was undertaken by all participants exploring the current knowledge related to health, wellbeing and safety topics. This focussed on their current knowledge and understanding of core topics that would be covered in the workshop program. This same questionnaire was given to each participant at the end of the two-day workshop to assess changes in knowledge following the program. These data were analysed to determine participant level of knowledge pre- and post-workshop.
Topics covered were linked to relevant health issues predominant in farming and rural populations. A participant resource manual provided both a written and visual resource for participants. The first day was timetabled to enable assessment of fasting blood cholesterol and glucose measurements. A 07.00 h start assisted in the physical assessment process and all participants were provided with a healthy breakfast following a brief physical assessment and introduction. Participants were seated in table groups to facilitate discussion of learning needs, as identified in Azjen and Fishbein's theory of reasoned learning model10. Topics were structured to address health issues experienced by farming populations and included:
- the state of rural health
- cardiovascular disease
- cancer including bowel and skin
- farm health and safety
- stress and stress management
- diet and nutrition - supermarket tour
- gender related topics delivered in separate groups, for example prostate cancer, impotence, women's health and breast cancer.
Two health professionals with expertise in rural health, men's and women's health and farming experience facilitated sessions. Relevant focus group data were collected for later collation for reference and evaluation.
Education sessions were run to a set timeline and incorporated specific learning objectives that would be completed by all participants within their resource manual. Following each of the sessions, each participant was required to assess the delivery of the session and the relevance of this to their farming entity and current life situation. A four-point Likert scale was used for this assessment and the data used for process evaluation. During each session frequent table group discussions enabled reflection, conceptualization and planning as per Kolb's model of effective learning14. In addition, participants developed 'action plans' in which they identified personal goals and strategies to achieve these goals. This process was an important part of the delivery process in that participants were able not only to learn from the health professionals, but also from each other and the peer experiences within table group discussion. From the evaluation process all participants found this education process to be of great benefit and all participants would recommend the program to other farmers.
Physical assessment
One of the most successful facets of the project, and the most influential in gaining attendance, was the physical assessment process undertaken by all participants. Many participants stated that the provision of a free 30-min physical assessment was the main factor that influenced them to join the SFF project. Further exploration of this through focus group discussions found that a similar proportion of individuals felt that a full and detailed physical assessment was one thing that modern medicine failed to deliver them. The concept within the SFF education process is that knowing and understanding one's relevant risks empowers people to seek treatment, change behaviour and implement interventions. Many of the participants felt that they were not fully aware of their personal results and what they could do to reduce risk.
The participants' physical assessment process was set up to undertake initial screening on arrival, following a minimum 10 hours' fasting to aid in accuracy of the testing procedures. Initial screening was a 5 min assessment including the following recorded tests:
- fasting total cholesterol and blood sugar
- weight and height measurement
- body mass index (BMI)
- body fat percentage
- blood pressure and pulse
- waist and hip measurement.
This initial assessment was a confidential process recorded in the health record and the participant's resource manual for later reference. Bookings for a full 30 min physical assessment were made prior to the commencement of breakfast; two of 338 members for the dairy or broadacre farmers refused this opportunity. These physical assessments were undertaken on the afternoon of the first day and in the morning of the second day of the program. Pre-existing health information documented by participants was used to enhance the assessment and evaluative process. A full health record was made and stored for each participant in accordance with relevant privacy and statutory laws. Specific topics and discussions undertaken in this assessment process included:
- evaluation and discussion of initial physical assessment results
- allergies and current medications
- familial history and incidence of disease
- neurological assessment
- skin spot assessment
- cardiovascular assessment
- respiratory assessment
- gastrointestinal assessment and risk for upper and lower gastrointestinal disorders
- urological assessment for relevant risk and disorders
- sexual history and assessment for disorders
- social history.
The 30 min assessment was undertaken in a private room and findings were recorded in the health record collated for each participant. Extensive discussions with each participant were made regarding the results and the need for referral to other health professionals, with a full referral made using relevant documented health information. In most instances a copy of this referral was also sent to the participant. A frustrating part of the project has been a lack of feedback from most health professionals to the project to advise on the action of the follow up. Follow up by SFF of referral outcome was therefore invariably limited to participants' verbal version of their GP's assessment. Some allied health professionals did provide feedback following receipt of the SFF referral and intervention.
Knowledge surveys
Knowledge surveys were given to participants before and following each annual program intervention. This involved a combination of true/false, recognition multiple choice and short answer questions23. Testing the change in knowledge was undertaken using a generalised linear model with binomial and logit link. All analyses were performed using GenStat v7.1 (VSN International Ltd; Oxford UK). This analysis was undertaken by an independent biometrician working for the Department of Primary Industries in Hamilton, Victoria.
Results
Referral rates for each of the programs and other health indicators are provided (Table 1).
Table 1: Statistical data from year 1 of Sustainable Farm Families and Sustainable Dairy Farm Families projects, illustrating demographics, health indicators and perceptions of health
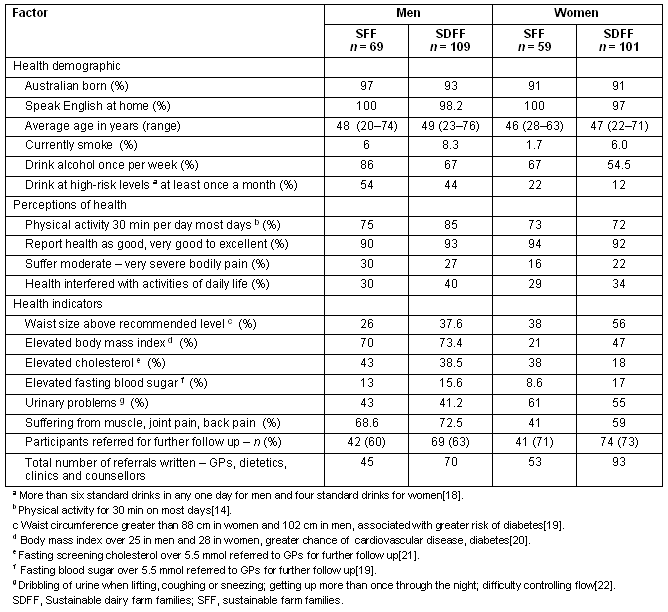
Quantitative findings
The results indicated a statistically significant change in knowledge which was retained over the 3 years of intervention in both broadacre and dairy groups24. The level of knowledge for women in year 1 from pre- to post-intervention with a p-value of <0.05 was evident in 88% of questions. Results for men for pre- and post-knowledge in year 1 revealed a p-value of <0.05 in 67% of questions. Retention of knowledge over the 3 year intervention in the broadacre program for women showed 86% of questions were answered correctly from information presented in year 1. For men this figure was recorded at a level of 85% retention of knowledge presented at year 1 and reassessed at year 323. The dairy program was not complete at the time of writing this article.
When broadacre participants were asked to consider whether the SFF program prompted them to think differently about managing the work on the farm, 30% of participants focused directly on specific action to improve their health, with 24% of the responses concerning greater attention to improving farm safety practices; 15% stated they wanted to spend more time with their family. Overall, 54% of responses were concerned with improving farm safety and the consideration of improving their health. In addition to this a further 24% focused on improving health and wellbeing by taking holidays or spending more time with family24. These results are highlighted (Fig2).
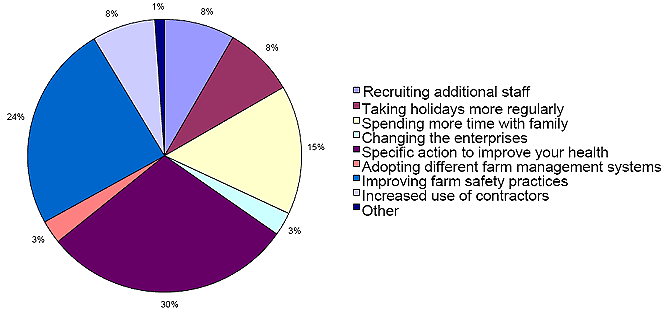
Figure 2: Has the Sustainable Farm Family program prompted you think differently about managing work on the farm?24.
Qualitative findings
Focus group discussions were an imperative part of the program design, with participants frequently asked to consider a part of each topic within their set table groups. During this time participants would use Kolb's Experiential Learning Model to consider the question and then present their response to the remainder of the larger group14.
Farm families, for example, participated in the workshop because it provided 'no fuss health assessment and information', with their farming support group peers. In the focus group discussions participants identified factors that inhibit good health and safety. They included:
- Safe work practices (chemicals, sunlight) - 'Lack of time', 'not a priority', 'cultural thing ... always done it this way', 'Children in the workplace is a problem'.
- Stress management - 'Don't know where to go', 'We are stressed', 'There aren't any mental health problems up here', 'We are pretty good here.'
- Balancing farm work and leisure - 'Women tend to get upset - we blokes just go out and work'.
- The health system - 'We don't have enough information to make a decision', 'If you don't know your way around it's hard to know what you can ask for'.
There were occasional references to gate-keeping by GPs, with some participants feeling that their GP did not always support them in their efforts to learn more about their personal health and to develop options for addressing issues. An example cited by participants was that when they wanted to see a dietician they were advised by medical group receptionists that they must first obtain a referral from a medical practitioner. Participants also commented that they usually waited until they had four or five things wrong with them because they did not want to waste their time or money. The lack of 'bulk billing' was also raised as a deterrent.
Discussion focusing on relevant disease processes, such as heart disease, cancer or diabetes, was considered from a farm family perspective and feedback supported conceptualisation and understanding within the farm family setting. Participants were able to learn from each other and assess the relevance of health within their own lives and that of their farming business.
Finally, the information collected in annual participant action plans also reveals something about what was thought useful and important to pursue. Several comments have been highlighted in the following categories:
- Physical activity - 'Increasing my physical activity for general health'; 'exercise riding, walking 30 minutes x 5'
- Diet - 'No idea how easy it was to understand basic label reading', 'altering shopping through reading labels', 'increase fibre', 'avoid high fat and high sugar'
- Improving farm safety/ prevent injury (one group undertook a workshop with Workcover) - 'Use ear muffs, bike helmets, protective clothing', 'complete first aid course', 'keep all machinery in safe working order', 'all covers and shield in place', 'work at a pace I can keep up with'
- BMI - 'Lose weight - get to normal BMI'
- Stress - 'Set aside time for rest and relaxation', 'recognise what stresses me', 'improve communication skills'
- Business - 'Health plan should be part of business plan', 'without health you've got nothing'.
Discussion
The results to date reveal health indicators that link to current health trends reported throughout Australia and the world. Farming sectors have significant health issues related to access to services and information that place their health, wellbeing and safety at risk. As revealed through the preliminary results, men and women are reluctant to report issues (such as body pain) that affect their work, and they are often content to continue with an ailment for long periods. Health screening reveals factors of concern and the need for referral to address serious issues for future disease and mortality rates.
In total, 100% of all participants would recommend the program to others and many have found the project to be a life-changing experience. Initial concerns were that we may be preaching to the 'worried well' and may not find significant health indicators due to the self-selecting sample within the program. Farmers would enrol in the project because they have an interest in their health, have a good concept of a healthy lifestyle and thus would not have significant health issues. Results from the initial project revealed a 60% need for referral to a medical practitioner or allied health specialist for men and 71% need for referral for women. Issues relating to mental health, alcohol consumption, body pain, poor work practices and sub-standard occupational health and safety practices were all discovered. Similar rates of referrals were required for the dairy industry; however, health indicators did reveal some differences between dairy and the broadacre farmers in the area of weight, cholesterol and blood glucose levels.
The results to date from the second and third year of the SFF broadacre program reveal a significant change in participants' state of health and a reduction in the need for referral to healthcare agencies. Improvements in BMI, total cholesterol, systolic blood pressure and waist measurements are all statistically significant24.
Reporting of pre- and post-knowledge revealed a high retention of knowledge obtained and retained after the SFF program intervention. A statistically significant increase of knowledge from the pre-program assessment to the end of third year for the broadacre sample reveals sustained retention and comprehension of health information delivered. This new knowledge and its link to farm family business and managing work on the farm differently is evident (Fig1), and the SFF intervention has influenced positively some participants' farm business decisions.
Initiatives including health awareness to behaviours addressing farm safety and family connectedness were made by participants as they linked farm family health into the farming business-unit decision making (Fig2).
The high rate of retention of participants in the SFF over several years is a function of the way the program is delivered and farmers are engaged in both learning and action about their state of health and its link to the family farming business. Effective health promotion balances the needs of the individual to engage and respond with the needs of the health service to deliver value-for-money services to the whole community served. We believe that the SFF process is an example of establishing an effective balance in these two competing sets of needs. It is a process that could be applied across a range of settings, possibly leading to similar health and wellbeing outcomes.
Conclusion
The SFF and SDFF projects are defining many of the health issues and needs of farming families in Victoria, southern New South Wales and South Australia. This project demonstrates through the qualitative and quantitative information collected that the health and wellbeing of both broadacre and dairy farming populations is not as good as it could be, and also reinforces the findings of previous studies undertaken for rural populations.
The key learnings that have emerged from the SFF project focus on the role of intersectoral collaboration and the need for evidence-based health education to be delivered to farming sectors throughout Australia. Many farming practices use the triple bottom line model that focuses on the financial (net production units), natural resource (pasture and environment management) and human resource (persons per production unit) aspects of the farming business. Together with research highlighting the significantly lower life expectancy, socio economic status and mortality rates associated with cancer, heart disease and suicide, farming families should be recognised as a population in need of social and political attention.
By providing education and assessment techniques focused on the needs of the farming population with broad intersectoral collaboration and ownership, the process of addressing the farming family health needs is possible. Farming families are an important part of Australian society because they provide valued commodities, while enduring economic, climatic, social and demographic challenges. We believe the key to the success of the SFF program/s is based on the ability to involve collaborative partnerships where all partners have a key role within the development and delivery of the project to their relevant representative groups. Joint ownership is imperative in any collaborative body and this process was adapted to aid in the recruitment, facilitation, analysis and delivery of the project. In-kind support was shared among all collaborative bodies and well exceeded the current funding received to undertake the research. The SFF and SDFF projects and their associated research activities are giving voice to the health, wellbeing and safety needs of farm families and the means by which their health can be improved.
Acknowledgements
This project depended on bringing together a team of primary producers, farm families, health professionals, industry representatives and university academics that were committed to making the health of farm families a priority. We would like to thank all members for their dedication, patience and assistance in making the research project the catalyst of new evidence-based practice that will assist in making the health of farm families a priority in Australia. Collaborative partners at the commencement included:
- Joint Research Venture Farm Health and Safety managed by RIRDC
- Farm Management 500
- LandConnect Australia
- Australian Women in Agriculture
- RMIT University, Victoria
- Department of Primary Industries, Victoria
- Victorian Farmers Federation
- Geoffrey Gardiner Foundation
- WestVic Dairy
- United Dairy Farmers Victoria
- Colac Area Health, Victoria
- La Trobe University, Victoria
Specific appreciation must be directed to the Joint Venture on Farm Health and Safety (managed by RIRDC) and Geoffrey Gardiner Dairy Foundation, WestVic Dairy and Department Primary Industries for their funding and support for the promotion of farm family health. Appreciation to the Western District Health Service Board and Chief Executive Officer Jim Fletcher for the organisational support and strategic vision in backing the Sustainable Farm Families - the human resource in the triple bottom line. Their encouragement and strong interest has been outstanding.
References
1. Wass A. Promoting health: the primary health care approach, 2nd edn. Sydney, NSW: Bailliere Tindall, 2000.
2. Rydholm L, Kirkhorn S. A study of the impact and efficacy of health fairs for farmers. Journal of Agricultural Safety & Health 2005; 11(4): 441-448.
3. McCallum DM, Conaway MB, Drury S, Braune J, Reynolds SJ. Safety-related knowledge and behaviour changes in participants of farm safety day camps. Journal of Agricultural Safety and Health 2005; 11(1): 35-50.
4. Australian Institute of Health and Welfare. Health in rural and remote Australia. Canberra, ACT: AIHW, 1998.
5. Todd H. Social and family aspects of dairy farm expansion - findings from the "Sustainable dairy farm systems for profit" project. M5 Project information series. Brisbane, QLD: Department of Primary Industries and Fisheries, 2006.
6. Troeth J. Healthy farms need healthy farmers. Canberra, ACT: Department of Agriculture and Forestry, 2004.
7. Australian Institute of Health and Welfare. Australia's health 2008: the eleventh biennial health report of the Australian Institute of Health and Welfare. Canberra, ACT: AIHW, 2008.
8. Frager L, Franklin R. The health and safety of Australia's farming community. A report of the National Farm Injury Data Centre for the Farm Safety Joint Research Venture. Canberra, ACT: Rural Industries Research and Development Corporation, 2000.
9. McCullagh M, Lusk SL, Ronis DL. Factors influencing use of hearing protection among farmers: a test of the pender health promotion model. Nursing Research 2002; 51(1): 33-39.
10. Thompson B, Coronado G, Grossman J, Klaus P, Solomon C, Islas I et al. Pesticide take-home pathway among children of agricultural workers: study design, methods, and baseline findings. The Journal of Occupational and Environmental Medicine 2003; 45(1): 42-53.
11. Caldwell TM, Jorm AF, Dear KBG. Suicide and mental health in rural, remote and metropolitan areas. Medical Journal of Australia 2004; 181(7): s10-s14.
12. Brumby S. Rural directions for a better state of health. In: S Brumby, B Wilson, S Willder. Living longer on the land - sustainable farm families in broadacre agriculture. Canberra, ACT: Rural Industries Research Development Corporation, 2008; 6.
13. Ajzen I Fishbein M. Understanding attitudes and predicting social behaviour. Englewood Cliff, NJ: Prentice Hall, 1980.
14. Kolb DA. Experiential learning: experience as the source of learning and development. Englewood Cliff, NJ: Prentice Hall, 1984.
15. Kirkpatrick DL. Evaluating training programs: the four levels. New York: Berrett-Koehler, 1998.
16. Rogers EM. Diffusion of innovations, 3rd edition. New York: Free Press, 1983.
17. Heart Foundation. How to have a healthy heart. Melbourne, VIC: Heart Foundation, 2002.
18. National Health and Medical Research Council. Australian alcohol guidelines: health risks and benefits. Canberra, ACT: Commonwealth of Australia, 2001.
19. International Diabetes Institute. The Australian diabetes, obesity and lifestyle report. Melbourne, VIC: IDI, 2001.
20. Better Health Channel. Body mass index (BMI). (Online) 2009. Available: http://www.betterhealth.vic.gov.au/bhcv2/bhcarticles.nsf/pages/Body_Mass_Index_(BMI) Accessed: (29 February 2009).
21. Southwest Ethics Committee. Sustainable Farm Families Project. Warrnambool, VIC: South West Health Care, 2003.
22. Continence Foundation of Australia. The prostate and bladder problems. Melbourne, VIC: CFA, 2002
23. Kay D. Workplace Assessor Training. Melbourne, VIC: Workplace Assessment WINTRAIN, 2002.
24. Brumby S, Wilson B, Willder S. Living Longer on the Land. Sustainable Farm Families in Broadacre Agriculture. Publication no 08/048. Canberra, ACT; Rural Industries Research Development Corporation, 2008.



