Introduction
Chronic and complex wounds often have prolonged healing times and require frequent assessment and treatment from a healthcare professional. Their management represents a significant burden on the healthcare system, with the annual cost of treating chronic wounds worldwide estimated at US$7 billion1.
In the rural Midwest region of Western Australia (WA), an audit of outpatient services found that the management of conditions involving wounds constituted 41% of all presentations. In the region wounds are managed in diverse care settings, such as an out-patient clinic, at the hospital, or by a GP or domiciliary nurse.
A regional scoping study found that optimal wound care was impeded by constraints related to multiple healthcare providers; poor confidence and limited training in the management of chronic wounds among nurses; limited access to expert review; incomplete and inconsistent wound history and management documentation; and no processes or tradition for secure sharing of medical records among providers.
Electronic healthcare systems can assist in addressing such problems. Remote expert review of digital wound images and patient care in the Kimberley region of WA has demonstrated significant patient care outcomes2. Continuity of care may also be improved with the sharing of timely, accurate and secure electronic information between the public and private sectors, and between the tertiary, secondary and primary care sectors3,4. In order to test the feasibility of a telehealth solution to the chronic wound care problems in the Midwest, a project called 'Wound Witch' was developed.
Wound Witch used a modified version of AMWISTM (http://www.medseed.com/page/our_products.html - the electronic software program used in the Kimberley region) to record wound history and treatment, store digital images of the wound and refer for expert review and consultation. Information exchange was to be achieved by storing patient data on a central server, ensuring its availability at point-of-care to all regional providers who managed wounds, and the urban-based wound care nurse consultant. The project team was aware that establishing successful rural telehealth initiatives can be challenging.
An Australian telehealth leader has proposed seven principles for the successful development and implementation of a telemedicine system5:
- Telemedicine applications and sites should be selected pragmatically, rather than philosophically.
- Clinical drivers and telemedicine users must own their own systems.
- Telemedicine management and support should follow best practice business principles.
- The technology should be as user friendly as possible.
- Telemedicine users must be well trained and supported, both technically and professionally.
- Telemedicine applications should be evaluated and sustained in a clinically appropriate and user-friendly manner.
- Information about the development of telemedicine must be shared.
Maldron surveyed healthcare providers regarding their perceived barriers to telehealth and identified deficits in user experience, technological and managerial support, and resourcing of equipment and staff time6. Yellowlees5 and Maldron6 also highlighted the need for telehealth applications to be simple and located on desktop computers that are part of clinicians' usual working environment. This view is supported by Nesbitt et al. who added that informed and willing staff are critical to successful implementation of telehealth7. These conclusions are similar to those reached in rural America8,9 and Canada10.
Methods
Description of intervention and evaluation methods
The barriers, recommendations and principles outlined by Yellowlees5 and others were considered in the design of the Wound Witch trial, which took place from May to December 2007. In particular, Wound Witch provided a telehealth application that had adequate IT and clinical support, used tried and tested software, provided sufficient funding, did not require real-time specialist consultation, confirmed managerial and organisational support, and was to be used in an identified area of need (Fig1).
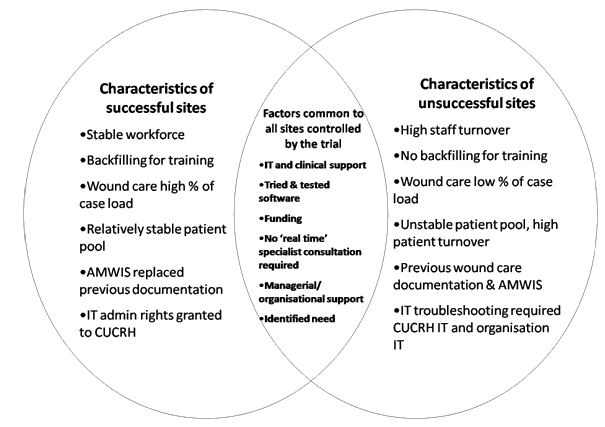
Figure 1: Factors affecting the implementation of the Wound Witch
Prior to designing the trial, meetings were held with managers and clinicians from regional and tertiary health organisations. This ensured the project met priority needs and was considered feasible. Ethical approval to conduct the trial was granted by the University of WA Human Research Ethics Committee.
An information session was held for all potential sites in the region. Local managers and clinicians had the opportunity to raise questions about IT support, wound care training and other practical issues. Twelve of the 14 sites represented at the session agreed to participate. The sites consisted of two private general practices, one private podiatry service, one private hospital, two residential aged care facilities, one not-for-profit domiciliary nursing service, a hospital in the home and four rural or remote WA health clinics.
To prepare the sites, participating healthcare providers were offered 2 hours of education in basic wound care. They were also interviewed to determine their level of confidence in providing wound care and to ascertain their existing wound management practices. The number of patients currently receiving care for chronic wounds at each site was recorded as a baseline estimate of caseload.
Following this, AMWIS software was installed at all 12 healthcare sites on a computer located where patients were treated. The AMWIS system enables healthcare providers to describe and annotate a digital picture of a wound, and record patient information; it has been demonstrated to be user friendly in many different healthcare settings. Once mastered, it takes less than 5 min to enter a patient's data, the anticipated time for documenting in paper notes. The AMWIS system offers the facility to store an objective wound assessment, care plan interventions and track healing outcomes from a digital image.
Wound Witch used an adapted AMWIS program that stores patient records in a central MS SQL (Microsoft; http://www.microsoft.com/sqlserver/2008/en/us/product-information.aspx) wound database, in accordance with National E-Health Transition Authority guidelines. The central server database enabled all healthcare providers involved in treating a patient to have immediate updated information at their site. The clinical expert (who also had AMWIS loaded on a computer with internet access) reviewed recently posted or updated patient records and provided advice on the characteristics of the wound and management strategies.
Training was carried out at each site immediately following the installation of AMWIS. In groups of no more than three, participants were shown how to use AMWIS with a hypothetical patient. Training was offered repeatedly with no restriction on the number of training sessions for an individual participant. Each training session lasted for 1 hour and all individuals attended a minimum of two training sessions. All training was conducted by the project officer, an experienced rural and remote nurse. Funding was made available through the project to back-fill nurses while they attended training, ensuring the budget of the participating health organisation was unaffected.
A flow chart of the trial protocol was developed and distributed to trial sites to facilitate processes and understanding (Fig2). All patients who presented to the participating sites with wounds were assessed for eligibility. All wounds present for 3 weeks or longer, or assessed to have a healing time of more than 3 weeks were eligible for recruitment to the trial. If patient consent was obtained the relevant patient information, assessment and treatment plan were entered into AMWIS, along with a digital image of the wound. Each time the healthcare provider treated the wound, the file was updated with new information or wound image. Healthcare providers were instructed to email the expert reviewer fortnightly, if required, for advice. The expert reviewer then accessed the server and relevant patient information, viewed the most recent photograph and treatment regimen, and added advice to the record. Scheduling conflicts were minimised because it was not necessary for the rural healthcare provider and the urban specialist to be available at the same time.
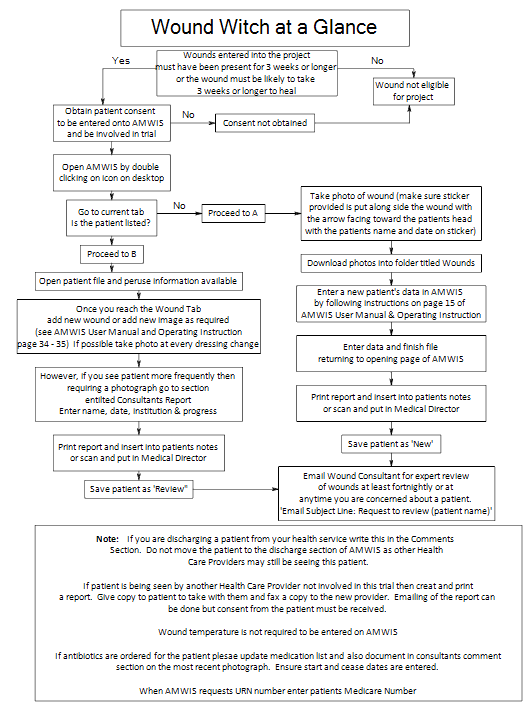
Figure 2: Trial protocols
The project officer stayed in regular telephone and email contact with all sites, trouble-shooting problems, offering additional education and documenting any problems and successes in the implementation of the system. A diary of all encounters was kept in order to analyse the implementation process. An IT officer was also available to deal with technical problems as they arose. Healthcare providers were not required to set up or maintain the software; all software interaction was directly related to their work.
At the end of the trial the project officer interviewed all trained healthcare providers remaining at participant sites about their experience of using Wound Witch.
Results
Table 1 summarises the implementation of Wound Witch across the 12 sites. Software was installed within the first week of the trial in 6 sites (two aged care facilities, hospital in the home, the podiatry practice, the domiciliary nursing service and one general practice). These sites had 15 weeks in which to use Wound Witch. At the remote site and the other general practice it took 6 weeks to install the software, 8 weeks in the three rural clinics, and 13 weeks in the private hospital. On average, sites had less than 11 weeks use of the system before the trial ended. Delays were largely due to the time expended obtaining approval from distant decision-makers for permission to alter firewalls and other security system features to permit access to an external central server.
Table 1: Patients and staff detail according to participating sites
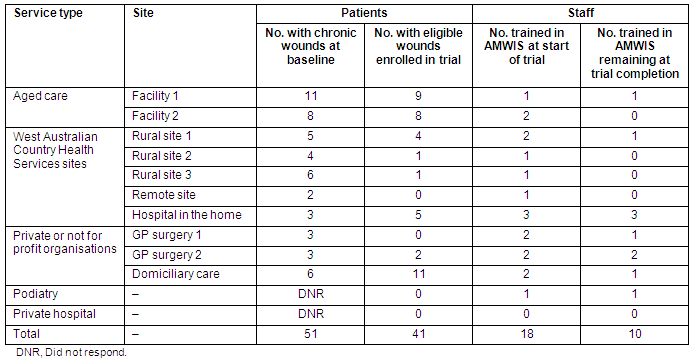
Although software was installed at all 12 sites, 4 sites did not participate in the initial wound care training or preliminary survey, and subsequently did not enroll patients. At the remaining 8 sites the total number of patients with chronic wounds captured during the trial period was similar to the number being managed before the trial started. Approximately 40% of recruited patients were being cared for in the aged care setting and another 25% by the domiciliary nursing service. The AMWIS users at these sites demonstrated more confident use of the system than those at the 4 sites that did not register any patients. The reasons given by the 4 sites for lack of participation included no eligible patients during the study period, delays experienced in installing the software, and general workforce shortages.
Only 45% of the 18 staff trained in use of the software at the beginning of the trial were still working at participating sites at the end of the trial. Prolonged periods of understaffing resulted in a workforce crisis in at least one remote clinic and an aged care facility. It was reported that this made it impossible for the remaining staff to allocate time for using the AMWIS system. Staff shortages also negatively impacted on some clinicians' willingness to invest time in gaining confidence in using the system. The offer to backfill staff positions was not taken up because other personnel were not available to fill these vacancies.
All sites shared the common elements of the trial displayed in the intersection area of Figure 1. Analysis of the end-of-project interviews identified other elements associated with successful or poor uptake. The successful sites were aged care facility 1, hospital in the home, and the domiciliary nursing service. These sites had a higher number of patients with wounds and a more stable workforce; software installation occurred promptly and paper records were replaced with the AMWIS system. In addition to the 4 sites where no patients were enrolled, the 3 rural sites, a general practice and an aged care facility were unable to adopt the system effectively. This was primarily due to workforce shortages, but delays in software installation and low numbers of patients with wounds were also factors.
The interviews also illuminated the challenges associated with the provision of modern dressings and devices in private practice settings where there is no reimbursement scheme, except for that available to war veterans. This was a disincentive to be involved in wound care management. For example, a general practice nurse said that patients who had complex wounds that would take a long time to heal were referred to either the not-for-profit domiciliary nursing service or hospital in the home, in order to reduce practice costs incurred in purchasing dressing materials.
Discussion
Considerable effort was put into designing a best practice tele-healthcare program. There was support from managers and clinicians at regional and local levels to address an area of health care considered a priority. Training was delivered as needed and at the point of care. The software was user friendly and IT support from the project was prompt.
The trial did have some limitations. Funding constraints meant the trial had to be completed in 6 months, and some sites had the system available for only a few weeks before the trial ended. Although arrangements were made to continue use of the Wound Witch system beyond the trial period with the same level of support, only the sites where it was already successful continued to incorporate the system in their regular wound care management. Time alone was not sufficient to overcome the other constraints. In addition, the project was unable to confirm the proportion of eligible patients enrolled; the baseline estimate was drawn from data up to several months old.
The Wound Witch project results highlight the relevance of service models, staff ratios and funding models to the adoption of telehealth innovations. The two most successful sites were an aged care facility and the domiciliary nursing service where chronic wound management was a feature of everyday practice. In addition, individual practitioners in these settings are likely to see the same patients over an extended period, and it could be assumed that they develop a greater commitment to the wound healing outcomes.
Residential, domiciliary and out-patient care services are funded according to the number of patients. Practices that enable patients to be treated more efficiently effectively 'buy' staff more time to care. Feedback from two of the high-use sites stressed that time-saving was a feature motivating continuing use of the Wound Witch. Nurses became more efficient at entering data and extended their wound care knowledge through consultation with the wound-care specialist. Cost efficiencies in wound management could therefore be anticipated with ongoing use.
The general practices in this trial did not have many patients with chronic wounds and rarely stocked the range of dressings and additional equipment recommended by the wound-care consultant. Because of the small case loads there were no financial or time-saving incentives to adopting new wound-care practices. Recent discussions on the scope of the Commonwealth Medical Benefits Scheme fees may result in a funding model more sustainable for multidisciplinary private practices. However, the inability to access reimbursement for dressing materials will remain a disincentive for general practices to become active in wound-care management.
A number of the rural sites were part of a larger government or non-government organization, and local authority was not available to approve software installation and access a central server.
Previous research by Krupinski11 and May et al.4 identified staff turnover and shortages as having the potential to result in telehealth applications being used less often and by uninformed or inexperienced staff. In accordance with this, the most important barrier found to implementing Wound Witch in the present study was the chronic workforce shortage in rural and remote Australia. In such a setting the need for repeated staff training sessions becomes a high priority; however, it is difficult to backfill positions when only one or two nurses cover an entire service. This constraint does not augur well for the implementation of rural and remote quality-improvement or reform initiatives, such as the telehealth innovation described.
Conclusion
Wound care in rural areas is influenced by the experience of a range of health providers and the resources available. Patients who have a chronic wound may have it treated as part of routine care by their GP or the domiciliary care team, as an inpatient or in residential aged care. Coordination of wound care across a continuum of care providers has the potential to be enhanced by a shared electronic wound record. Moreover, access to remote expert consultation offers many advantages to patients and practitioners. However, until the fundamental issues of workforce shortages and reimbursement for the dressing materials, devices and consumables used in wound management are addressed, the widespread uptake of shared patient electronic patient records to enable collaborative care among providers is unlikely.
The following recommendations are made:
- Imaging and medical records software should permit web-based access and storage, in view of the technical and administrative difficulties inherent in creating new firewalls.
- Staff should be relieved from their usual duties to attend training in the use of new systems, and collaborative effort should be expended generally on adopting time-saving telehealth initiatives.
- Managers at participating sites should receive software training to ensure local and ongoing technical support.
- Private practices should only be targeted for this type of service delivery if associated funding is available for reimbursement for use of consumables, such as wound dressings and devices.
Acknowledgements
The authors are grateful to the managers and staff at the participating sites, who demonstrated a commitment to providing quality health care under sometimes trying circumstances. Also acknowledged is the advice and assistance provided by Martin Weatherston, CEO Midwest GP Network; Prof Nick Santamaria of Curtin University of Technology; Grace Ley of WA Country Health Service Midwest; Richard de Trafford of CUCRH; and Russell Beattie from Medseed. The Silver Chain Nursing Association permitted use of its wound education modules. The authors acknowledge the funding support to CUCRH of the Australian Government Department of Health and Ageing through a Managed Health Network Grants Seeding Grant, and through infrastructure support of the University Departments of Rural Health program.
References
1. Austin D, Santamaria N. Digital imaging and the chronic wound: clinical application, relevance and patient perception of the Alfred/Medseed Wound Imaging System. Journal of Stomal Therapy Australia 2002; 22(4): 24-29.
2. Santamaria N, Carville K, Ellis I, Prentice J. The effectiveness of digital imaging and remote expert wound consultation on healing rates in chronic lower leg ulcers in the Kimberly region of Western Australia. Primary Intention 2004; 12(2): 62-70.
3. Seldon H, Siemienowicz J, Hawson M, Steele P, Ibrahim M. Closing the communication gap between hospitals and primary health care providers. Australian Journal of Primary Health Interchange 2000; 6(3): 91-97.
4. May C, Harrison R, Finch T, MacFarlane A, Mair F, Wallace P. Understanding the normalisation of telemedicine services through qualitative evaluation. Journal of the American Medical Informatics Association 2003; 10: 596-604.
5. Yellowlees P. Successfully developing a telemedicine system. Journal of Telemedicine and Telecare 2005; 11(7): 331-335.
6. Mauldon E. The use and attitudes towards telehealth in rural communities. Australian Journal of Primary Health 2007; 13(3): 29-33.
7. Nesbitt TS, Cole SL, Pellegrino L, Keast P. Rural outreach in home telehealth: assessing challenges and reviewing successes. Telemedicine Journal and e-Health 2006; 12(2): 107-113.
8. Alverson DC, Shannon S, Sullivan E, Prill A, Effertz G, Helitzer D et al. Telehealth in the trenches:reporting back from the frontlines in rural America. Telemedicine Journal and e-Health 2004; 10(2): 95-105.
9. Whitten P, Adams I. Success and failure: a case study of two rural telemedicine projects. Journal of Telemedicine and Telecare 2003; 9: 125-129.
10. Jennett PA, Scott RE, Affleck Hall L, Hailey D, Ohinmaa A, Anderson C, Thomas R, Young B, Lorenzetti D. Policy implications associated with the socio-economic and health system impact of telehealth - a case study from Canada. Telemedicine Journal and e-Health 2004; 10(1): 77-83.
11. Krupinski EA. Telemedicine consultations: failed cases and floundering specialities. Journal of Telemedicine and Telecare 2004; 10(S1): 67-69.



