Introduction
General practitioners (GPs) are the cornerstone of primary care and are the first 'port of call' for most Australians seeking medical attention1-4. In particular, small rural towns throughout Australia are dependent on the GP and GP proceduralist workforce for procedural and after-hours medical services in their hospital emergency rooms5. General practitioner proceduralists, especially, are a highly trained cohort of GPs that have historically provided anaesthetic, obstetric, surgical and other routine and emergency procedural interventions for patients in local communities6-7.
However, the GP proceduralist landscape has changed substantially over time. Until the 1950s most GPs delivered babies and, until approximately 30 years ago, many performed a range of surgical procedures in hospitals throughout the country6. Equipment costs, indemnity issues and the lack of opportunity to maintain procedural skills8, together with new technologies, research in pharmaceuticals and an expanding knowledge-base has seen the growth of diverse medical specialist disciplines, which has displaced many GPs from procedural work in anaesthetics, obstetrics and surgery9-10.
In rural Australia, GP:population ratios are poor2 and a large percentage of the workforce is approaching retirement11, particularly in rural locations12. Overseas trained doctors comprise a considerable percentage of the rural GP workforce13-14 and women are entering the medical profession15 in ever increasing numbers16. Although the medical student intake will increase by over 80% between 2005 and 201217 it is unlikely to meet the demand for doctors due to changing population demographics and community expectations18, together with doctors' preference for part-time work and a reduction in the total number of hours worked per week11,19.
Many Victorian and New South Wales regional towns have identified sustainable business, environmental and cultural opportunities for social and economic development that continue to influence the composition and characteristics of their population centres20. Government policy initiatives direct the level, type and conditions of available funding for health services21. These factors, interalia, influence the demand for and supply of medical services, infrastructure and facilities. Importantly, they exert pressure on the extent and type of GP procedural practice in any given community.
Objective
It is against this background that the Bogong Regional Training Network commissioned a needs analysis of GP procedural medicine in the Bogong region of north-east Victoria. Bogong Regional Training Network is a Commonwealth funded training provider that offers a range of postgraduate training for GPs and registrars in, or entering, general practice in Australia. The region consists of three Divisions of General Practice (Border, NE Victoria and Goulburn Valley) and includes the major regional towns of Albury/Wodonga, Wangaratta and Shepparton. The purpose of the research was threefold, to:
- Take stock of the extent, type and frequency of procedural medicine undertaken in the region - particularly in anaesthetics, obstetrics and surgery.
- Estimate the likely demand for and supply of the GP proceduralist workforce in the future.
- Develop evidence about potential training opportunities in procedural medicine to enable procedurally trained doctors to remain in the Bogong region.
There is much demographic data about the composition of rural communities and extensive information about the number and composition of GP practices but little or no qualitative or quantitative data to build a comprehensive picture of the current and likely future of GP procedural practice. Consequently, a research framework was developed and three research questions posed:
- What procedures are currently being performed by proceduralist GPs in local rural hospitals and health services in the Bogong region?
- What procedures are no longer performed in the region and why?
- What is the likely future of GP procedural practice in the next 5-10 years?
Defining GP procedural medicine
The literature provides many useful, but competing definitions of general practice and procedural medicine22-24. Dunbabin's 2002 study of GP proceduralists distinguishes between GPs who perform minor procedures and those who perform more advanced procedural work in anaesthetics, obstetrics and surgery. Dunbabin's definition was used in this research25:
Procedural GPs were defined as GPs doing one or more of the following advanced skills: obstetrics (including normal deliveries, procedural intervention and operative obstetrics), anaesthetics (including general, neurolept, major regional, epidural and spinal anaesthetics) and surgery (defined as a surgical procedure requiring more than a basic infiltration of local anaesthetic).
Method
A qualitative case study research methodology was chosen as the most appropriate means to explore the world of the GP proceduralist and the factors that influence the future of GP proceduralist medicine. A research team consisting of the Bogong CEO and three members of the board oversaw the research process. An independent research officer was employed to manage the project and conduct a literature review of trends in procedural medicine.
Population data, based on Department of Human Services (DHS) drawn geographical boundaries were used to create a socioeconomic snapshot of communities in the catchment. Population demography, epidemiological and medical workforce projection data were analysed to identify trends in the composition and health needs of rural communities in the future.
A population of 70 GPs located in 26 practices in 14 towns was initially identified as practising obstetric, surgical or anaesthetic procedures. Eleven individuals were excluded from the study because they were on leave (n = 3), unwilling to participate (n = 4) or did not fit Dunbabin's definition (n = 4). Of the remaining 59 GPs, structured interviews were conducted with 38 respondents in 13 towns in the region during March and April 2008.
Four focusing questions were asked at each interview. For each open-ended question, nested questions were included and prompts developed to guide the discussion and ensure that interviewers covered the same material. Interviewees completed a brief demographic profile about themselves. Each discussion lasted approximately 1 hour and was facilitated by a member of the research team and the research officer. All interviews were audiotaped and transcribed.
Of an additional 21 GP proceduralists who were not interviewed, 10 returned useable responses to a survey instrument. The questionnaire was developed by the research team and drew on two important earlier studies25-26 The survey added a quantitative dimension to the research methodology and provided a supplementary source of evidence that offered an opportunity to explore specific issues and test the consistency of the views expressed by interviewees. When interview and survey responses were combined, the response rate was 81%.
Table 1: Response to surveys according to characteristic
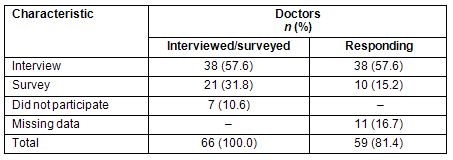
In May and June 2008, interviews were conducted with a senior DHS representative and five health service CEOs to gather data about directions in healthcare services and obtain their perspectives about the future of GP procedural practice.
Twenty-one hours of recorded data were transcribed into 20 documents, each signifying a discussion event. Content and thematic analysis identified key issues and explored elements of interest. Data sets were analysed to examine specific themes associated with trends in GP procedural practice over time.
Results
The research revealed five interrelated findings:
- GP proceduralists are attracted to rural general practice by a passion for and the challenges of procedural medicine, combined with a rural lifestyle and a desire for holistic patient care.
- Over several decades there has been a gradual decline in the volume and complexity of procedural work due in part to new technologies, centralisation of services, funding constraints, stringent credentialing requirements and shortages of ancillary medical and nursing staff.
- Nevertheless, there remains a substantial demand for GP procedural work in rural communities in the Bogong catchment.
- However, the GP proceduralist workforce is in decline as GPs age and cease procedural practice.
- Finally, GP proceduralists are essential to the primary healthcare system yet they are not recognised as a specific cohort of highly trained medical practitioners. They have become the 'hidden heart' of the health system in rural and regional Australia.
A passion for rural procedural practice
Lifestyle, cultural 'fit', spouse employment, secondary schooling options and a sense of belonging were important factors that attracted GPs to rural general practice. Positive early experiences of country practice and rural lifestyle were key elements that affected respondents' choice of location. Several GPs had grown up in or worked as registrars or junior doctors in rural environments and this influenced their decisions to locate in rural general practice.
However, it is the great diversity and challenge of general and procedural medicine that both attracts GP proceduralists to rural practice and keeps them there. Respondents reported that the variety of procedural work in a rural environment combined with the opportunity to interact with and learn from other medical practitioners in a hospital setting is both demanding and stimulating. Procedural medicine is not 'just a job'. They are passionate about their work and want to 'make a difference', even though they consider they are often overworked, sometimes undervalued and have pursued what some of their colleagues regard as one of the least attractive career options for medical professionals. The following comment was typical:
...the main reason I came to this town was because I could do obstetrics; ... it's why I came here; it's why I didn't do general practice in the city. I came to practise medicine. It's really enjoyable.
The changing landscape of procedural practice
In the last 20 years in the Bogong region there has been a gradual but sustained decline in procedural work. Respondents reported that they formerly provided a full range of obstetric and anaesthetic services and undertook various surgical procedures including tonsillectomies, appendicectomies, hysterectomies, removing gall bladders and repairing hernias. That work has narrowed considerably as the following results reveal.
Obstetrics: General practitioner obstetricians, the largest group of GP proceduralists in the Bogong catchment, are located in 10 of the 14 towns identified in the study. Most perform low risk deliveries and only four towns have GP proceduralists performing Caesarean sections.
There is no single model of obstetric care and each town operates at different levels of sustainability. In the last decade, at least 6 towns in the Bogong region have closed their birthing services5,27. As a result, GPs offer shared care in obstetrics but women travel to larger centres to deliver their babies. Respondents cited funding pressures, centralisation of services, insufficient volume of deliveries, shortages of nursing staff, fear of litigation and 'burn out' as causes of the loss of services.
As a consequence of obstetrics unit closures, a small number of GP obstetricians travel long distances in order to maintain their skills. It is commonplace, and of concern, that some doctors consult all day in their rooms, travel to another town to either deliver a baby or provide an on-call service and then return home at the end of a shift to work a further day in their rooms. One respondent commented:
I mean it's totally unsafe work practice. You're doing a 24 hour shift which might have you up half the night and then the next day you go to the clinic and do a normal day's work. I don't think anyone takes the day off after their shift.
Many towns with GP obstetricians experience onerous workloads because colleagues have relocated or ceased procedural practice. Discussions revealed that many respondents provide on-call emergency services in addition to their obstetrics workload. Several doctors, particularly those in towns with only two GP obstetricians, work a one-in-two day roster. They expressed concern about fatigue, loss of quality of life and family time. One respondent noted:
I'm finding it a bit difficult ... because we were doing a one in three on-call for obstetrics which just sort of merged into your other [emergency] on-call and you didn't really notice it. ... But now it's one in two it has become much more onerous ....
Typically, respondents in this predicament reported not taking more than 2 weeks holiday at one time because of insufficient back up for obstetrics services.
Anaesthetics: General practitioner anaesthetists, the second largest group of GP proceduralists, are located in 9 of the 14 towns identified in the study. They provide a range of general, regional and sedation anaesthetics to surgical and obstetrics patients. While some were clearly satisfied with the volume of work, others were not. Some GP anaesthetists, like their obstetrician colleagues, travel to other towns in order to gain sufficient procedural work to remain credentialed. In one town, respondents commented that the anaesthetic workload had steadily decreased in volume and complexity over the past 20 years. They reported that a weekly gynaecology list had become one list a month due to the retirement of a surgeon. Previously, they had a full complement of visiting specialists who provided general surgery, orthopaedic and endoscopy services. Currently, endoscopy is the only type of work that has increased and respondents were frustrated by the decline in elective surgery because it impacts on their ability to maintain skills.
Speaking as one of the anaesthetic doctors, it's a great source of frustration because we could be doing a lot more elective surgery than we are, and therefore anaesthetics. The struggle for us is to keep up our skills and the only way to do that is to do more elective lists.
Elsewhere, surgical lists were severely curtailed when a visiting surgeon left and neither the hospital nor the replacement surgeon had the appropriate equipment to continue offering the service. Respondents argued that if they had insufficient lists to retain the surgeon, a GP anaesthetist would consider relocating in order to maintain an anaesthetic workload. This would result in a negative flow-on effect as the remaining GP proceduralists' general consultation and after-hours emergency services workload increased. They were further concerned that such losses may affect their ability to maintain the current range of obstetric and emergency services, therefore impacting negatively on the extent to which trauma patients could be treated locally.
Surgery: General practitioner surgeons comprise the smallest group of GP proceduralists in the Bogong catchment. Indeed, the largest shift in procedural work has been the steady decline in GP surgeons and a substantial narrowing of the scope of surgery performed. Although 14 respondents performed surgical procedures, most reported doing only minor interventions compared with the types of surgical procedures they performed in the past. Only one GP surgeon appeared to have a substantial surgical workload, much of which was endoscopy.
Respondents commented that one regional hospital was known as a 'GP hospital' because GPs did most of the obstetrics, surgery, anaesthetics, paediatrics and emergency department work. Today, however, respondents noted that specialisation has forced them out of hospital practice and while they have admitting rights for palliative care patients, they are no longer accredited for paediatrics, surgery or general internal medicine. Although that town retained its GP obstetric workforce, this study found only one GP anaesthetist and no GP general surgeons were still practising.
This was not an isolated example of the demise of GP surgeons. Many smaller hospitals have lost locally available and experienced GP surgeons due to retirement, fear of litigation, 'burn out' or the withdrawal of GP privileging rights. In one town, GPs commented that 15 years previously they had thriving monthly orthopaedic and gynaecological surgery lists, with a waiting list for 'scopes' and 'lumps and bumps' (endoscopy and removal of lumps). Now they have one list every quarter of the year.
In addition, the complexity of procedural work in smaller hospitals is limited by the type of available infrastructure. Services are constrained because hospitals are no longer funded to maintain operating theatres to the same level of operational efficiency as larger hospitals with a greater volume of regular work. As one CEO commented:
We don't allow, even specialists who do procedures in our theatres to undertake ... things like opening abdominal cavities for instance - because we have no air conditioning that would sustain those sorts of procedures.
Although hospital CEOs were supportive of their GP proceduralists and committed to retaining visiting specialists, the future of those services is not secure. Indeed, respondents in 3 towns did not consider the number of visiting specialists adequate for the current workload and believed that more could be done to maintain and increase elective surgery lists. They were keen for government to provide further funding for surgical services and, importantly, for the necessary equipment to support those services.
Centralisation of services has created economies of scale for larger hospitals but many small hospital facilities have been downgraded or closed. Between 1983 and 2005 in Victoria, 72% (n = 82) of small rural obstetrics units were disbanded28. According to respondents, and consistent with the literature, government funding priorities and limits on financial support for hospital facilities, infrastructure and elective work has negatively impacted on the range of services hospitals provide. Many hospitals in the region are struggling financially and have rationalised services by replacing acute beds with nursing home beds. Some hospitals have moved minor procedures from hospital theatres to GPs' rooms, and reduced the volume and frequency of elective work.
'Pashen et al29 suggested that the trend from generalism to specialisation arose when the specialty colleges emerged in the 1940s. They argued that new technologies and pressure from the colleges to move GPs out of the hospital setting and into community practices resulted in a decline in the scope of GP practice and correspondingly, a 'loss of status and morale'. They also observed that the decline in procedural practice was less pronounced in rural areas because of community needs and because of the expertise and interests of the GPs themselves. However, they noted that 'While the health sector landscape has changed both nationally and internationally, the needs of rural and remote communities for basic care have not'. The present research supports that contention.
Demand for general practitioner procedural services
Since the introduction of Australia's Medicare in 1984, there has been a continuing increase in the average number of medical services provided to individuals30 and sustained growth in the number, type and frequency of medical procedures being performed31. For example, GPs performed an average of 15 procedures per 100 patients in the period 2006-2007 compared with 12 procedures per 100 patients in 1998-19993. In addition, demand for healthcare services is driven interalia, by changes in population demographics, the cost of health care, and the socioeconomic and educational status and expectations of communities32.
Growth in general and procedural practice has particular implications for the workload of GP proceduralists in the Bogong region. Of the 1.4 million individuals who live in rural and regional Victoria33, approximately 22% reside in the Bogong catchment; between 2003 and 2007 the population of the region increased at an average of 2.5% per annum34-35. This is above the Victorian regional average of 0.8% per year33, although growth is uneven35.
Each town has different requirements for medical services depending on their unique circumstances and characteristics. Some towns with ageing populations are experiencing little growth. In these towns, respondents reported an increase in demand for endoscopy and diagnostic, and chronic health related procedures. In contrast, another town is enjoying a 4% growth per annum in permanent residents across all age groups36. The hospital CEO reported an increase in the need for both birthing and aged care services. Similarly, respondents and the CEO of another medium sized rural community anticipated 200 babies being delivered per year and believed that anaesthetic lists will expand as visiting surgeons continue to do 'interesting and varied work' in the hospital.
Other communities in the Bogong catchment have developed a strong visitor focus with eco and adventure tourism swelling local populations throughout the year. While the Alpine regions are popular ski resorts that rely on GPs and GP proceduralists for on-call emergency trauma in the winter months, one hospital CEO reported an 'exponential increase' in emergency trauma because the region promotes mountain, dirt bike and four wheel drive sports in the summer.
There is no doubt that town and community profiles will continue to change as a result of socioeconomic imperatives. The type, extent and volume of demand for procedural services will also vary over time. Nevertheless, the present research demonstrated a substantial and undeniable demand for GP procedural services throughout the Bogong region into the future.
The decline in the GP proceduralist workforce
The shortages of GPs and GP proceduralists are well documented23,37-39, particularly in rural areas40,41. Despite the National Health Workforce Strategic Framework's measures to achieve a self-sufficient workforce supply42 and the establishment of decentralised training providers, the introduction of the rural pathway for GP registrar training, increases in training places and the creation of undergraduate rural clinical schools, there still remains a substantial shortfall in the supply of GPs in regional and remote Australia19,43.
Respondents noted that GP proceduralists have been displaced by a rise in specialisation, more stringent credentialing requirements, conflicts about remuneration arising from the visiting medical officer negotiation process, onerous on-call arrangements and workload stress. Indeed, GP proceduralist numbers are likely to continue to fall at an alarming rate as GPs cease procedural work, leave the district or retire. Disturbingly, over 50% of respondents reported that they intend ceasing procedural practice within 5 years but only 10% of all respondents had a succession plan. In addition, younger GP proceduralists, particularly females, are working substantially fewer hours than their older colleagues (Table 2).
Table 2: Hours worked per week according to age and sex
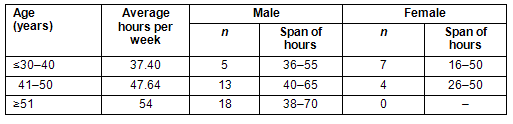
Analysis of discussion data revealed that the onerous nature of on-call and emergency work, and a lack of critical mass of available doctors is a significant disincentive to continuing procedural work in many small communities. Younger GP proceduralists want sufficient exposure to procedural work to maintain their skills. If procedural work ceased or substantially declined, several respondents indicated their intention to relocate. The following comment is typical: 'If I can't do obstetrics, I can't see any point being here'.
Recognising the general practitioner proceduralist
Notwithstanding the changes to procedural practice over the last 20 years and the gradual decline in the GP proceduralist workforce, most respondents believed they were appreciated and valued by their communities and colleagues. However, they expressed disquiet about the extent to which they were recognised by the wider health system. Indeed, little comprehensive research about the identity, location or work of GP proceduralists was found in the present research. The Australian Medical Workforce Advisory committee in its report on the anaesthetic workforce in Australia44 was unable to include GP anaesthetists in its research because of: 'A lack of adequate data on non-specialist anaesthetists and general practitioners'.
Furthermore, GP Divisions do not differentiate between GPs and GP proceduralists and so have little information specific to GP proceduralist demographics or practice. Moreover, the Rural Health Workforce National Minimum Data set 2009 report is unable to accurately document the number of GP proceduralists in rural and remote locations12. Without such recognition, the loss of GP proceduralists will continue unnoticed, and those who stay will remain under-rated, under-valued and under-resourced. Regrettably there is little awareness or acknowledgement of the far reaching health system consequences if the decline in rural GP proceduralists is not recognised and addressed.
Discussion
The ramifications of these trends are clear. The departure of a single GP proceduralist has a flow-on effect on the rest of the system. For example, the loss of a local GP obstetrician or surgeon, including specialists, may reduce the workload of the anaesthetist, leading to the loss of that person to the town. Conversely, the loss of an anaesthetist may narrow the availability of a full range of obstetrics services and cause the GP obstetrician to relocate. In either case, it is likely that the remaining GPs' workloads will increase, possibly to unsustainable levels. At best, this will threaten the continuation of procedural services in the town; at worst it will lead to adverse health outcomes for the remaining GPs or an exodus of GPs who are either unable or unwilling to take on the increased workload. Similarly, the loss of one service due to a lack of equipment, nursing, midwifery staff or hospital infrastructure may have serious unintended consequences for all procedural and GP services in a town.
The existence or not of a highly skilled procedural workforce impacts on the scope of treatment offered in hospital emergency departments. If GP proceduralists' skills decline due to a reduced volume and complexity of work, their confidence in successfully dealing with emergencies or complex situations is likely to wane, resulting in a withdrawal of their services from emergency departments. At best this may cause unnecessary hardship for patients who must travel to larger centres and, at worst, may result in patients' permanent incapacity or loss of life.
The future of GP procedural practice in the Bogong catchment is not only dependent on the continuing demand for procedural services, but also on attracting sufficient numbers of interested new doctors to accommodate natural workforce attrition. It is difficult to attract doctors to towns where the on-call and after-hours workload is burdensome. Without a critical mass of GP proceduralists, emergency departments in many rural communities will struggle to provide adequate trauma management and patients will face transfer to larger regional or metropolitan hospitals. Indeed, if there are fewer GPs available or willing to practise emergency medicine, small hospitals may not have the capacity to offer an emergency department service. This would place greater stresses on larger regional and metropolitan health centres which may be struggling to cope with their own current case loads. This not only shifts the burden of financial costs to larger hospitals but also strains ambulance and transport services and increases the emotional, economic and personal stresses on patients, carers, families and support networks". At best this may cause unnecessary hardship for patients forced to travel to larger centres and at worst, may result in permanent incapacity or loss of patient lives. A decline in GP proceduralists would unquestionably increase the workload for the specialist workforce. This too may be unsustainable in a climate where evidence is emerging that there is a shortage of specialists across most medical disciplines45.
Although health services and local and state government departments may have comprehensive strategic plans for the provision of health services in general, there appears to be no cohesive and inclusive strategic focus on the likely demand and on-going need for GP procedural medicine throughout rural and remote towns. The present research has demonstrated that GP proceduralists are central to quality care and safety of patients in rural communities; however their existence is concealed and their location is somewhat serendipitous. While GPs may choose locations based on judgements about opportunity to practise procedural medicine, coupled with individual preferences for specific rural landscapes, their choices are not necessarily correlated with the current and future planned needs of communities. Thus, some communities struggle to achieve a critical mass of doctors to accommodate patient needs, while others are concerned that too many GP proceduralists will dilute an already shrinking workload.
Finally, if the consequences of the decline in GP proceduralists is of concern to health services and communities in this relatively affluent region where even the smallest towns are in relative proximity to larger regional centres, the implications for health services and patient outcomes in rural and remote areas throughout Australia is perilous. There is no substantive evidence to suggest that sufficient numbers of new graduates are likely to embrace rural general practice to replace exiting GPs, and even less evidence that they are likely to know about or wish to engage in GP procedural medicine in small rural towns. As one GP proceduralist noted, there needs to be a critical mass of GPs with procedural skills being trained and maintained in the wider system of rural general practice in order to have a labour force capable of working in more remote locations. If these downward demographic trends continue, and the demand for GP proceduralist services remains static or increases, then it will take a substantial recruitment drive and training effort in each of the procedural disciplines in order to maintain current supply levels.
Conclusion
Many factors have influenced the nature and direction of GP procedural practice in the Bogong region. It is clear, however, that there has been a gradual but sustained decline in the volume and complexity of procedural work available to GP proceduralists and that it is unlikely that they will ever return to the range of procedural medicine that was practised in the past. The findings of the present research show that the future of GP procedural medicine and the continuing existence of a viable and robust workforce of GP proceduralists in many towns in the Bogong catchment are at a 'breaking point'. Although the volume of procedural work and the numbers of GP proceduralists have declined, the demand for GP procedural services remains strong and there is potential for a robust and challenging workload for those who wish to enter or continue practising procedural medicine.
General practitioner proceduralists do not exist in isolation from the wider health system configuration. Each plays an integral and critical role in maintaining the efficient and effective operation of the whole health service. As the Australian Federal Government implements widespread reforms of the health system, there are opportunities to build on the strengths of GP procedural practice and work towards overcoming some of the barriers facing those who would remain in or wish to embark on a career in GP procedural medicine. As a first step, GP proceduralists must be counted and acknowledged if they are to remain at the heart of rural and regional health in Australia.
While this research paints a grim picture of the decline in GP procedural practice there is much that can be done to 'turn the tide'. However, tackling any single part of the system needs to be considered according to its relationship to other elements in the system. The future of GP procedural practice is dependent upon first acknowledging the importance of the GP proceduralist and then understanding the totality of the system in order to apply solutions in the context of the overall health service.
References
1. New South Wales Rural Doctors Network. NSW rural general practice workforce strategy: What can we do? Newcastle, NSW: New South Wales Rural Doctors Network, 2007; 2.
2. Australian Medical Workforce Advisory Committee. The general practice workforce in Australia: supply and requirements to 2013. Sydney, NSW. Australian Medical Workforce Advisory Committee, 2005; 5.
3. Australian Institute of Health and Welfare. Australia's health 2008. Cat. no. AUS99. Canberra, ACT: AIHW, 2008; 10.
4. Capolingua R, Preetham V, Rischbeith P, Pashen D. General practice solutions for enhancing primary health care. Canberra, ACT: Australian Medical Association, Royal Australian College of General Practitioners, Rural Doctors Association of Australia and Australian College of Rural and Remote Medicine, 2008.
5. Rural Doctors Association of Victoria. Victorian rural procedural GP workforce and ages statistics 04-09. (Online) 2009. Available: http://www.rdav.com.au/documents/Proceduralists%20Survey.pdf (Accessed 20 May 2010).
6. Wilson RE, Multispecialty surgical conditions in general practice. Medical Journal of Australia 2005; 182(7): 337.
7. Victorian Government Department of Human Services. Rural directions for a better state of health. Melbourne, VIC: Victorian Government Department of Human Services, 2005; 13.
8. Australian Health Workforce Advisory Committee. Health workforce planning and emergency care model of care. Sydney, NSW: Australian Health Workforce Advisory Committee, 2006.
9. Bollen M, Saltman D, A history of general practice in Australia. In: General Practice in Australia. Canberra, ACT: Department of Health and Aged Care, 2000; 4.
10. Power P, Aloizos J. The operating environment of general practice. In: General Practice in Australia. Canberra, ACT: Department of Health and Aged Care, 2000; 157.
11. Schofield DJ, Page SL, Lyle DM, Walker TJ. Ageing of the baby boomer generation: how demographic change will impact on city and rural GP and nursing workforce. Rural and Remote Health 6: 604. (Online) 2006. Available: http://www.rrh.org.au. (Accessed 16 January 2009).
12. Health Workforce Queensland and New South Wales Rural Doctors Network. Medical practice in rural and remote Australia: Combined Rural Workforce Agencies National Minimum Data Set report as at 30th November 2009. Brisbane, QLD: Health Workforce Queensland, 2010; 4.
13. Rural Workforce Agency, Victoria. 2007 GP Workforce Snapshot - Victoria. Divisions of General Practice. (Online) 2007. Available: http://www.rwav.com.au/filesUpload/PUBLICATION/FILE0000000738.pdf (Accessed 25 June 2010).
14. Australian Medical Association. AMA urges greater suppport for international medical graduates (IMGs). (Online) 2010. Available: www.ama.com.au/print/5281 (Accessed 29 July 2010).
15. Loy CS, Warton RB, Dunbar JA. Workforce trends in specialist and GP obstetric practice in Victoria. Medical Journal of Australia 2007: 186(1): 26-30.
16. Kilmartin MR, Newell CJ, Line MA. The balancing act: key issues in the lives of women general practitioners in Australia. Medical Journal of Australia 2002: 177: 87.
17. Joyce CM, Stoelwinder JU, McNeil JJ, Piterman L. Riding the wave: current and emerging trends in graduates from Australian university medical schools. Medical Journal of Australia 2007: 186(6): 309.
18. National Health Workforce Taskforce. Health workforce in Australia and factors for current shortages. Melbourne, VIC: National Health Workforce Taskforce, 2009.
19. Health Workforce Queensland and Australian Rural and Remote Workforce Agencies Group. Doing the sums; Will there be a future health workforce for rural and remote Australia? A concise overview of past and present rural and remote general practice workforce trends. Brisbane, QLD. Health Workforce Queensland and Australian Remote Workforce Agencies Group, 2006.
20. Australian Government. Regional Development Network Area Consultative Committees - NSW and Victoria. (Online) no date. Available: http://www.acc.gov.au/index.aspx (Accessed 25 January 2009).
21. The Commonwealth of Australia. Australian Health Care Agreement between the Commonwealth and the State of Victoria 200 -2008. (Online) no date. Available: www.health.vic.gov.au (Accessed 7 July 2008).
22. Royal Australian College of General Practitioners. What is general practice? Definition of general practice and general practitioner. Royal Australian College of General Practitioners. 2005. (Online) no date. Available: www.racgp.org.au (Accessed 23 July 2008).
23. Pegram R. Meeting the needs of rural and remote Australians for specialists medical care: issues and options. Edinburgh. Journal of the Royal College of Physicians 2005: 35: 298-308.
24. Glazebrook rM, Harrison SL, Obstacles and solutions to maintenance of advanced procedural skills for rural and remote medical practitioners in Australia. Rural and Remote Health 6: 502. (Online) 2006. Available: http://www.rrh.org.au (Accessed 28 July 2010).
25. Dunbabin J. Procedural medicine in rural and remote NSW: The general practice workforce. Newcastle, NSW: Rural Doctors Network, 2002; 12.
26. Australian College of Rural and Remote Medicine. Barriers to the maintenance of procedural skills in rural and remote medicine. Brisbane, QLD: Australian College of Rural and Remote Medicine Research Project, 2002.
27. Robinson M. General practitioner Proceduralists: The hidden heart of rural and regional health in Australia. Wodonga, VIC: Bogong Regional Training Network, 2009; 33.
28. Rural Workforce Agency Victoria. White Paper: The Viability of Rural and Regional Communities resolving Victoria's rural medical workforce crisis. Discussion paper, v.1 March 2007; 15. (Online) 2006. Available: http://www.rwav.com.au/filesUpload/PUBLICATION/FILE0000000916.pdf (Accessed 19 May 2010).
29. Pashen D, Murray R, Chater B, Sheedy V, White C, Eriksson L et al. The Expanding role of the rural generalist in Australia - a systematic review. Brisbane, QLD: Australian College of Rural and Remote Medicine, 2007; 45
30. Australian Bureau of Statistics. 41020.0 - Australian social trends. (Online) 2003. Available: www.abs.gov.au/ausstats (Accessed 16 January 2008).
31. Britt H, Miller GC, Charles J, Pan Y, Valenti L, Henderson J et al. General practice activity in Australia 2005-06. Bettering the evaluation and care of health (BEACH): A joint report by the University of Sydney and the Australian Institute of Health and Welfare. General Practice series no19, AIHW cat. no GEP 19. Canberra, ACT: AIHW, 2007; xiv.
32. Australian Health Workforce Advisory Committee, Australian Medical Workforce Committee and Australian Health Workforce Officials' Committee. Demand for health Services and the health workforce - Information paper. Health Workforce Information Paper 3. Sydney, NSW: AHWAC, 2005.
33. Victorian Government Department of Planning and Community Development. Census 2006 Information Sheet: Urban and regional population change. Melbourne, Vic: Victorian Government, 2007.
34. Primary Health Care Research and Information Service. Key Division of General Practice characteristics 2006-2007. (Online) 2008. Available: www.phcris.org.au (Accessed 1 August 2008).
35. Primary Health Care Research and Information Service. Key Division of General Practice characteristics 2002-2003. (Online) 2004. Available: www.phcris.org.au (Accessed 1 August 2008).
36. MacroPlan Australia. Yarrawonga/Mulwala household and population forecasts. (Online) 2005. Available: www.moira.vic.gov.au (Accessed 12 August 2008).
37. Australian Institute of Health and Welfare. Medical labour force 2005. National health labour force series no 40. Cat. no HWL 41. Canberra, ACT: AIHW, 2008; 32.
38. Productivity Commission. Australia's health workforce. Canberra, ACT: 2005; 12.
39. Kosmina S. Victorian rural general practice workforce, planning for 2002-12. Melbourne, VIC: Rural Workforce Agency Victoria, 2003; 13.
40. Thistlethwaite JE, Shaw T, Kidd M, Leeder S, Burke C, Corcoran K. Attracting health professionals into primary care: strategies for recruitment. Canberra, ACT: Australian Primary Health Care Research Institute, 2007; 42.
41. Australian Government Department of Health and Ageing. Report on the audit of health workforce in rural and regional Australia. Canberra, ACT: Commonwealth of Australia, 2008; 44-45.
42. National Health Workforce Taskforce. Self sufficiency and International medical graduates - Australia. Melbourne, VIC. National Health Workforce Taskforce, 2008.
43. Health Workforce Queensland. Sinking deeper into the abyss: a concise overview of current and future trends in the Australian urban, rural and remote general practice workforce. Brisbane, QLD: Health Workforce Queensland, 2006: 8.
44. Australian Medical Workforce Advisory Committee. The anaesthetic workforce in Australia: supply, requirements and projections 1995-2006. Sydney, NSW: Australian Medical Workforce Advisory Committee, 2006.
45. Victorian Government. Next steps in Australian health reform: The proposals of the Victorian Premier. Melbourne, VIC: Department of Premier and Cabinet of Victoria, 2008; 54.
