Introduction
The Northern Territory has the highest rates of population turnover among GPs of any jurisdiction in Australia. Between 2001 and 2006, a volume of GPs equivalent to 60% of the total workforce moved in and out of the Territory. This is more than double the rates in other jurisdictions, and at least 50% higher than rates in other rural and remote parts of Australia.
A number of specific conditions in the Northern Territory contribute to high workforce turnover rates. These include the absence of a full medical school (although one has recently been funded by the Commonwealth Government), the very small number of 'home grown' practitioners, and the isolated nature of many communities. Migration theory would predict high turnover among the Northern Territory workforce (and population generally) because practitioners who arrive are likely to already be more mobile than their colleagues elsewhere1,2. The inevitability of high turnover in the Northern Territory is recognised in its system of providing short-term contracts for GPs.
The main challenge for new migrants is to establish 'place attachment', which is the sense that a particular location is a desirable residence, and is likely to remain a desirable residence into the future3. For migrants who intend to stay long periods, this requires a process of adaptation, where trade-offs are made between structural (work oriented), personal, social and environmental values. Theory suggests that shorter staying migrants adjust rather than adapt4, temporarily setting aside rather than more permanently recasting those values. Onward migration occurs when the adjustment becomes unsustainable and adaptation is ruled out as an option. The purpose of this research was to examine the place attachment experiences of GPs throughout the Northern Territory to develop a better understanding of how they address the adjustment/adaptation process. Such an understanding may inform recruitment and (particularly) retention programs and contribute to improved workforce planning.
Dimensions of place attachment
The idea that 'place attachment' the key driver of decisions by in-migrants to remain in a location has been prominent in the migration literature for some time3,5,6. Newly arrived migrants experience an initial 'arrival' phase characterised by both optimistic anticipation and regret, following which they need to establish a sense of place attachment or will move on or otherwise withdraw from the location (through depression, self harm etc)7. Much of the place attachment literature is concerned with migration episodes that involve an expectation of a long tenure of stay at the destination. In these cases, place attachment emerges from how well migrants adapt to the new conditions. Adaptation involves recasting personal ambitions and values to be consistent with what can be achieved, given the local circumstances. It has been argued that shorter term migrants adjust rather than adapt - they temporarily set aside ambitions and values in light of local conditions, rather than more permanently recasting them4.
Establishing place attachment in the first year or two of residence in a new location does not guarantee a 'successful' migration event because place attachment is a dynamic phenomenon. The characteristics of the migrant and the characteristics of the place change over time. Population modelling (with regard to the impact of migration) essentially tries to anticipate what these changes will be and the extent to which place attachment will be resilient to those changes8. In remote areas for example, it is often expected that GPs will migrate out when their family circumstances change (children reach school age, spouse wishes to enter or return to the workforce etc)9,10.
Where migration to remote areas is based on the search for employment, the nature of the work is clearly an essential factor in determining length of stay11. This does not just narrowly mean the conditions of work (duties, working hours, leave arrangements, work related infrastructure), but includes the structures in place to allow working life to integrate with total life12. This might include, for example, the extent to which the employer assists in the search for work for spouses, schooling for children, housing and recreation for the individual and family13,14. In more remote areas, 'the company' tends to assume (and is expected to assume) greater responsibility for the these 'filter factors'15 which represent the structural dimension of place attachment (Fig1).
In non-remote settings, people often select work because they prefer to be in the place. In those contexts, the social and personal factors that bind people to their communities are seen as stronger than the structural factors associated with work5,16-20. Eisenhauer and colleagues21 for example, found that family/friend related reasons were most important in establishing place attachment, and that the influence of the spouse was very strong14. Beyond the immediate circle of family and friends, participation in the broader community has been cited as an indicator of successful place attachment6. Goudy3 noted that the length of residence is an important factor in creating these social bonds and sentiments. Beckley22 agreed that 'length of residence is highly correlated with knowledge of local ecological and environmental processes and that knowledge of local ecological attributes or processes may lead to increased attachment to place'. Length of residence leads to what Riger and Lavrakas18 term 'behavioural rootedness'.
In locations where lengths of stay are usually short (such as remote communities) and immediate kinship bonds are weak or absent (as in the case of new migrants), social and personal factors are insufficient in determining place attachment. Brehm and colleagues23 argued that, in such cases, work is still not necessarily the only place attachment factor. They noted that attributes of the physical environment (natural and built) are more immediately experienced than social and personal factors, and so are less dependent on length of stay. Brehm24 contends that new arrivals may have a lower level of social attachment, due to their shorter tenure in the community, but that they may possess place attachment via their valuing of the environmental attributes (often attained during visits for holidays or short-term work). The physical environment is not just valued aesthetically, but because it provides the setting for a particular way of life21. This can include recreation or work experiences that are heightened because of the setting in which they occur. Brehm24 suggested that the way of life advantages allow people to adjust to the absence of other amenities (such as shopping facilities), and to imperfect work environments.
The four dimensions of place attachment - the structural, personal, social, and environmental - are shown (Fig1). In most cases, the success of a migration event depends on how well the individual adapts to the complex interplay of these dimensions. While labour migration models, and particularly those applied to remote areas, continue to emphasise the precedence of the structural dimension, more evidence is emerging that the other dimensions can be facilitators of, rather than simply barriers to, retention11,25.
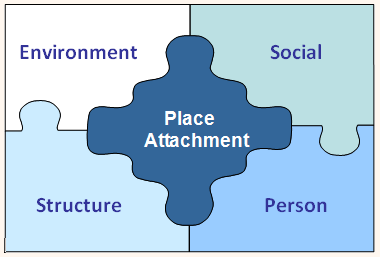
Figure 1: The dimensions of place attachment.
General practitioner place attachment challenges and responses in the Northern Territory
The primary health workforce recruitment (and retention) strategy targets GPs who value working in Indigenous health, having a greater variety of work and a higher degree of autonomy than might be found elsewhere26. General practitioner education and training are directed towards preparing practitioners for this work environment, and many recruitment and retention incentives involve increasing remuneration based on the complexity of the work environment. Initiatives that focus on broader quality of life issues (support for family, recreation opportunities etc) often temporarily remove the GP (and spouse and children) from the work environment and 'refresh' them off-site.
While there has been no research published specifically about mobility drivers for the Northern Territory GP workforce (although McDonnel Smets and Lowe26 considered some of these in their analysis of the impact of the Northern Territory Clinical School on recruitment and retention of the Northern Territory workforce), other labour force research in the Northern Territory27-29 has begun to suggest that the Northern Territory offers more than just a desirable temporary working environment. The Northern Territory may also, in particular places and for particular people at particular life stages, fulfil broader lifestyle ambitions. Adaptation rather than just adjustment should therefore be possible, resulting in longer lengths of stay.
The lack of a full medical school in the Northern Territory (a situation currently being addressed), and the lack of 'home grown' GPs means that the Northern Territory cannot effectively exploit the 'repatriation' approach which has found to be successful in addressing workforce issues in other states of Australia30. Territory GPs are likely to be more socialised to migration as a life stage response because virtually all of them (and their colleagues) have migrated to the Territory to begin with29. This factor in part explains the very high rates of in and out-migration of GPs recorded in a census and documented by various workforce and government agencies31.
Along with the social and personal challenges that emerge from having to move to the Northern Territory, and the well documented work challenges associated with remoteness, are the environmental challenges associated with the Northern Territory's harsh climate and isolation. These latter are widely cited as reasons for leaving the Northern Territory, whether it be because of the extremes of heat and cold experienced in the desert regions in the south or the relentless humidity of the 'build up' to the wet season in the north32.
The Northern Territory contains a wide variety of practice settings relative to the size of its GP population. Practice settings range from very remote and very small (and usually very economically disadvantaged) Indigenous communities with limited built infrastructure and poor transport and communications facilities, to the capital city of Darwin, which has a population of over 100 000 and is well served by health and community infrastructure. Between these extremes are what might be known elsewhere in Australia as small rural towns - between 2000 and 20 000 people - but distinguished here by the vast distances between them. For example, Alice Springs is the second largest centre in the Territory (approximately 25 000 population), but is over 1500 km from Darwin, and the intervening distance includes just two towns (Tennant Creek and Katherine) with more than 300 residents. While it is common in the Northern Territory to split management of health workforce between the urban areas (essentially Darwin and Alice Springs) and the remote areas, the overall size of the workforce is small (354 GPs in 2007)33, and management strategies (including those for recruitment and retention) usually have to deal with the diversity of locations.
Due to the remote setting, many locations in the Northern Territory offer little in the way of flexible working patterns. Job sharing and part time work is difficult to arrange in smaller communities because of the difficulties in providing housing and transport. The lack of pre-existing social and family networks also means that any break from full-time work is likely to be accompanied by a move away. Most practices are very small, and it is difficult to divide work responsibilities functionally, meaning practitioners find it difficult to avoid work tasks that they find dissatisfying. Recruitment and retention strategies, therefore, tend to focus on why the standard model of working in remote areas is attractive and are obsessed with finding staff who 'fit the mould' of rural/remote workers34, more so than developing alternative ways of working for different types of practitioners.
The General Practice Network Northern Territory coordinates a range of projects and programs including GP recruitment and retention programs under the national Rural and Remote General Practice Program. It coordinates relocation, continuing education and other grant schemes. Remote Area Grants supplement GP salaries in communities where the financial viability of having GP is marginal. The Rural Retention Program provides financial incentives to retain long-serving GPs in rural and remote communities35. Northern Territory General Practice Education provides a range of continuing medical education programs and professional support networking.
The two main marketing ploys used to attract GPs (and many other professionals) to the Northern Territory are the nature of the work available, and the idea that the Northern Territory is an ideal location for a (working) 'adventure holiday'36. The adventure holiday focus promotes the idea of short-term stays and also presents the impression that 'real life' is on hold during tenure in the Northern Territory. For GPs, the expectation is that they will adjust their social and personal priorities for a short time in order to fulfil their ambition to work in Indigenous health or remote health. This research aims to explore whether this is what GPs actually do, and whether there is potential for longer term adaptation to locations in the Northern Territory that might help increase lengths of stay and improve workforce planning efforts.
Methods
The research employed face-to-face and telephone interviews with 19 GPs throughout the Northern Territory to investigate their experiences in forming place attachment to their current practice locations. Participants were recruited through an advertisement by Northern Territory General Practice Education (a self selected sample). The particular focus was on GPs who had been in the Northern Territory a relatively short time (less than 3 years) because they were still likely to be forming place attachment7 and therefore at high risk of onward migration. A sample of 14 newly arrived GPs was supplemented by five longer stayers to provide some further insights into differences between adjustment and adaptation strategies.
A diverse sample was recruited in terms of demographic and life stage characteristics and practice settings. There are, however, limitations to the extent of details provided about the sample due to the confidentiality requirements of the human research ethics approval (Charles Darwin University number H09035). However, in terms of practice location, there were several GPs from larger centres (Alice Springs and Katherine with populations of 25 000 and 10 000, respectively) and several from much smaller centres (including very remote communities with less than 500 residents). Several participants had worked in both contexts during their stay in the Northern Territory. One participant was operating on a 'fly in/ fly out' basis to remote communities from one of the larger centres.
The interviews were semi-structured, and participants were asked why they had moved to the particular location, how they had come to feel about the community (particularly in the first year or two) and what factors influenced decisions to stay or leave. Participants were asked how trade-offs were made between work and other lifestyle factors (personal, professional, environmental), and whether such trade-offs were seen as temporary or more long term.
The research used a phenomenological design in which the participants' perceptions of their own experiences were seen to constitute the raw data. The place attachment model (Fig1) was not used to direct the interviews but emerged as part of the process of dialogue between the researchers and the raw data.
Results
Demographic and life stage characteristics
There were 11 males and eight females, with four being overseas trained doctors. For one GP the Northern Territory was both birthplace and childhood locality. Fourteen of the participants were married or had a partner, and twelve of these had children aged less than 18 years. Length of stay in the Northern Territory ranged from a few months to 7 years. Intended length of stay (additional to time already spent in the Northern Territory) ranged from desiring to leave as soon as possible to remaining an additional 5 years. No respondent thought they would see out their entire remaining career in the Northern Territory, but most thought it possible that they would work multiple 'stints' in the Northern Territory throughout their careers.
Apart from the four overseas trained doctors, the majority of participants were from large urban centres in Australia (Sydney, Melbourne, Brisbane, Adelaide). In general, the background of the participant did not appear to influence responses. Rural origin participants did express their desire to continue a rural lifestyle. Urban origin respondents expressed 'boredom' with city life and a desire to be a more prominent member of the community (an ambition they thought could be better achieved in a small community).
Reasons for moving to Northern Territory
Half of the respondents had come to the Northern Territory purely for work related reasons, while the other half had a combination of work and lifestyle motivations. Work reasons included the challenge of remote work, the opportunity to work in a small hospital or practice, working in Indigenous health and the variety of work. The idea that work in the Northern Territory is different to work elsewhere (and the desire to experience this difference) was prominent. 'I wanted to be a procedural doctor - doing things with my hands' (male participant, 50 years).
Often the work motivation was supported by a lifestyle ambition to see 'the real Australia' (male participant, 50 years) or to 'get out of the city' (female participant, 35 years). In general, the work was seen as a temporary adventure into something 'different' in some place 'different'. The working environment was perceived as valuable because of some exposure to it during medical training (eg remote placements, courses in Indigenous health). Few participants mentioned other exposure to the Northern Territory (holidaying there, for example) as a factor in deciding to move, although one participant was encouraged to move by a colleague who had previously worked in the Northern Territory.
Structural dimension of place attachment
Work also featured prominently as a factor in helping form place attachment. All participants felt that the nature of the work was as they had expected and desired. They felt that they received good support from their work colleagues, employers, and workforce support agencies in the Northern Territory:
I attended [General Practice Network Northern Territory] Family Day and it was very useful to make friends and it was great for the kids ... such events help to make sacrifices [worthwhile]. (Female participant, 43 years)
They appreciated the efforts that were made by the work system to make life easier for themselves and their families by facilitating social and professional networking within the Northern Territory, travel away from the Northern Territory, and assisting in finding employment for spouses. Concerns were raised about employer- or community-provided housing, and the difficulties involved in travelling into and out of the practice location, particularly for those living in non-urban areas.
The quality of work life was, however, widely viewed as supporting temporary retention only. As one participant noted: 'You can put up with bad circumstances like housing or less lifestyle but not for long' (male participant, 38 years). And another: 'You can stay almost everywhere for one year' (female participant, 42 years). This idea of '1 year' or '2 years' as the length of time for which work considerations outweighed others was common.
Participants from all practice settings had concerns about accessing continuing education and securing career development if they stayed too long in the Northern Territory. While participants acknowledged the efforts made to provide continuing medical education and professional networking within the Northern Territory, they still felt distant from the systems in place elsewhere. Given their plans to (at some stage) move on, this perceived distance was a constant pressure when it came to migration decision-making.
Personal and social dimensions of place attachment
No participant had relatives or friends (apart from family who moved with them) in the community in which they worked. Participants recognised that this lack of personal links was a critical factor in their anticipated short length of stay. However, GPs found it easy to make friends and become part of social networks. Many felt that the transient nature of the Northern Territory population generally meant that people were used to making new friends and welcoming new arrivals. For longer staying GPs, however, this became a double-edged sword because the need to constantly make new friends was tiring and because of the expectation that they would welcome and 'socially integrate' new colleagues:
I don't want to be the entertainment monkey to drive everyone around and going out on Friday for a drink. ...I don't want to give up my spare time to become a social integrator. (male participant, 47 years)
The capacity to form social networks was perceived as lower by those working in Indigenous communities. In those settings, social networks were usually limited to other non-Indigenous professionals, who were also likely to have short stays. Friendships with Indigenous longer term residents were seen as difficult because of cultural differences and because GPs had the impression that Indigenous people were also tired of the constant process of welcoming new community members.
Most participants, irrespective of the strength of their social networks, did feel that they were accepted as part of the community. The feeling of acceptance came through experiences of being greeted by name by other community members, and participating in community organisations and clubs. It was acknowledged, however, that this process was one that takes time (3-5 years was the common perception) and initiative. Participants with children were more likely to feel part of the community simply because the (often school based) activities that their children engaged in gave the GP opportunities also to participate. While this was the case in urban and non-urban settings, participants were less likely to have their children living with them full-time in non-urban settings (children either away at boarding school or living with another family member in urban Northern Territory or another place). Non-urban based GPs acknowledged that they faced the paradox of needing longer time to become part of the community (because of the cultural differences and the 'turnover fatigue') while expecting to remain for less time than their urban counterparts.
On a more personal level, there was widespread concern about the opportunities that the Northern Territory provided for participants' children. The quality of education available in the Northern Territory was considered poor (even among urban dwellers - although concern there was mainly for secondary and tertiary education). Ambitions on behalf of children were the most cited reasons for considering a move away, irrespective of the satisfaction with work and the support provided by work related agencies.
Environmental dimension of place attachment
The physical environment was a major factor in determining place attachment for virtually all participants. One expressed the view: 'lifestyle is about environment' (female participant, 35 years). The majority of participants engaged in outdoor activities such as bushwalking and camping. Several specifically noted that the environment and the opportunity to do these activities had encouraged them to stay in the Northern Territory longer than they originally planned. The environment was also seen as conducive to a 'laid back' way of life, and when combined with the advantages of small populations (less traffic, a less material culture) facilitated a lifestyle that was valued by GPs and their families. However, the disadvantages of small populations (limited choice for shopping and restaurants for example, along with access and housing issues previously discussed) were concerns particularly for non-urban practitioners.
Discussion
While reasons to come to the Northern Territory were consistent, the decision to stay or go (or really how long to stay, since all intended to go at some point) was far more specific to the person and their experience of place attachment. All newly arrived GPs appeared caught in an uncomfortable situation between their assurance that they could practice under any conditions for 'a year', and the recognition that developing place attachment which may increase the benefits they received from work in the Northern Territory would take 3 or 5 years.
What is interesting is that even these newly arrived GPs, and even those whose initial intention was a very short tenure, were actively seeking place attachment - trying to find a balance between the dimensions in the present place attachment model. This is consistent, then, with the view in the literature that the seeking of place attachment is a natural part of the process of migrating to a new location, even if only for a short time4. The present research revealed a transition from a focus purely on work/structural matters in the first few months or year, to a broader concern. The commonalities of that broader concern are reflected (Fig2), which identifies the two most prominent factors within each place attachment dimension. Where people differed was in the prominence given to each of these (and other, lesser) factors.

Figure 2: Most prominent factors within each place attachment dimension.
The study participants generally had been in the Northern Territory long enough to overcome the 'arrival' period optimism and regret. They represent a group of GPs who had been able to adjust to life in their new locations, and could potentially adapt for longer lengths of stay. Overwhelmingly, however, what was discovered was adjustment strategies - the temporary setting aside of a range of values and ambitions (including longer term career ambitions) to benefit from the experience of 'difference' in the Northern Territory. In general, adjustment strategies were about focusing on the work, but adjustment was also made through leveraging the social networks that their children formed (particularly through school), and engaging with the physical environment through outdoor activities. The workforce support system within the Northern Territory was also seen as facilitating adjustment, by providing professional networking, and offering opportunities for respite from the practice location.
The participants were generally satisfied with these adjustment strategies, largely because they retained the resources (financial wealth, ease of finding work elsewhere, established kinship ties elsewhere) to move on when the trade-offs became unsustainable. Participants were well able to identify when that would be, with most of the triggers associated with life stage progressions (children moving from primary to secondary school for example). There were surprisingly few major differences between urban and non-urban based GPs, although some urban based GPs could conceive of longer stays because of the better opportunities there for continuing education and career progression, and fewer issues with housing and transport. Overall, the diversity of the sample was not reflected in a diversity of strategies and responses to entering practice in the Northern Territory. It may be that any location in the Northern Territory is considered 'different' by practitioners coming from elsewhere (whoever they may be and from wherever they have come) and the degrees of 'difference' that may exist between the larger and smaller communities within the Northern Territory are insufficient to substantially affect place attachment strategies. This is an area warranting further investigation with a larger and more representative sample.
Participants who had been in the Northern Territory longer than 3 years still felt that their stay was temporary. In some respects, they were responding to the 'institutionalised temporariness' that they saw in the system. Incentive schemes appeared to be targeted at new arrivals and short stayers. Their social and professional networks were in constant flux. Contract arrangements were seen to normalise short stays, with longer stayers suspecting there might be something wrong with them because they had not already moved on.
The present findings are consistent with the literature on recruitment and retention of professionals in the Northern Territory27-29. A more prominent positive role for environmental factors may have been described than was previously considered, but it is clear that life stage events (eg children reaching school age, spouses entering or returning to the workforce) are crucial determinants of migration decisions, and that those decisions tend to involve movement out of (rather than around) the Northern Territory, despite the diversity of practice settings available there. In this regard, many respondents drew attention to the perception that opportunities particularly for children (through high standards of education) were not available anywhere in the Northern Territory, which limited the perceived value of moving from one Northern Territory location to another. First time Northern Territory residents associate the personal and social attributes that support life stage transitions with places outside of the Northern Territory. Those who do persevere within the Northern Territory are those who can compromise personal and social ambitions (by sending children to boarding school, or living separately from spouse and children, for example) and focus on environment and work attributes.
There is some potential to better exploit the adjustment strategies adopted by GPs to increase lengths of stay. One strategy would be to better reward longer stayers (the target of the Rural Retention Program, for example). Rewards might need to be more oriented towards social, personal and environmental values than structural ones.
Another avenue worth exploring is to increase the mobility of GPs within the Northern Territory. The respondents saw their options largely as remaining in their current practice location or leaving the Northern Territory (with the possibility of return at some unspecified future time). Exposing GPs to the diversity of practice (and social and environmental) settings within the Northern Territory might allow them to make a series of different adjustments (accept poor transport infrastructure in location A, and less Indigenous health work in location B, for example) and so stay longer in the Northern Territory in total (even though not staying longer in specific locations). That exposure may also increase the chances of repeat tenure in the future.
Conclusions
This research has provided some insights into the experiences of place attachment by GPs throughout the Northern Territory. A mutually reinforcing dynamic between systemic expectations of temporariness has been revealed, and GPs looking to adjust rather than adapt to their destinations. This dynamic may well be impossible to break until more 'home grown' GPs emerge and the Northern Territory becomes seen as a suitable location for more life stage transitions (particularly for children). Importantly, however, it has been shown that adjustment to the Northern Territory is not simply about foregoing 'lifestyle' ambitions to experience a valued work setting. There are personal, social, and environmental factors which facilitate successful adjustment, and these may be better exploited to increase lengths of stay and perhaps even broaden the potential pool of GPs (for whom the work setting alone is an insufficient reason to move to the Northern Territory). More research is needed into the differences between urban and non-urban settings, and to more quantitatively correlate the adjustment strategies of Northern Territory GPs with the factors known to increase rural practice propensity, such as rural background and rural training.
References
1. James D, Ferguson E, Powis D, Bore M, Munro D, Symonds I et al. Graduate entry to medicine: widening psychological diversity. BMC Medical Education 2009; 9: 67.
2. Chalkiti K, Carson D. Knowledge cultures, competitive advantage and staff turnover in hospitality in Australia's Northern Territory. In: D Harorimana (Ed.). Cultural implications of knowledge sharing, management and transfer: identifying competitive advantage. New York: IGI Global, 2009; 203-229.
3. Goudy W.J. Community attachment in a rural region. Rural Sociology 2009; 55(2): 178-198.
4. Bush KR, Bohon SA, Kim HK. Adaptation among immigrant families: resources and barriers. In: PC McKenry, SJ Price (Eds). Families and change: coping with stressful events and transitions, 3rd edition. Thousand Oaks, CA: Sage 2005; 307-332.
5. Burley D. Are the social and physical really so different? Elements in the development of an attachment to place. Conference Papers - American Sociological Association 2007; 1: 000.
6. Kasarda JD, Janowitz M. Community attachment in mass society. American Sociological Review 1974; 39(3): 328-339.
7. Pernice R, Brook J. The mental health pattern of migrants: Is there a euphoric period followed by a mental health crisis? International Journal of Social Psychiatry 1996; 42(1): 18-27.
8. Booth H. Demographic forecasting: 1980 to 2005 in review. International Journal of Forecasting 2006; 22(3): 547-581.
9. Gil-Soo H, Humphreys JS. Integration and retention of international medical graduates in rural communities: a typological analysis. Journal of Sociology 2006; 42(2): 189-207.
10. Lehmann U, Dieleman M, Martineau T. Staffing remote rural areas in middle- and low-income countries: a literature review of attraction and retention. BMC Health Services Research 2008; 8: 19.
11. Halseth G. 'We came for the work': situating employment migration in B.C.'s small resource-based communities. Canadian Geographer 1999; 43: 363-381.
12. Pretty G, Bramston P, Patrick J, Pannach W. The relevance of community sentiments to australian rural youths' intention to stay in their home communities. American Behavioral Scientist2006; 50(2): 226-240.
13. Shumaker S, Taylor R. Toward a clarification of people-place relationships: a model of attachment to place. Environmental psychology: directions and perspectives 1983; 219-251.
14. Kazanjian A, Pagliccia N. Key factors in physicians' choice of practice location: findings from a survey of practitioners and their spouses. Health and Place 1996; 2(1): 27-34.
15. Kulig JC, Stewart N, Penz K, Forbes D, Morgan D, Emerson P. Work setting, community attachment, and satisfaction among rural and remote nurses. Public Health Nursing 2009; 26(5): 430-439.
16. Giuliani MV. Theory of attachment and place attachment. In: M Bonnes, T Lee, M Bonaiuto (Eds). Psychological theories for environmental issues. London: Ashgate, 2003.
17. Hidalgo MC, Hernandez B. Place attachment: conceptual and empirical questions. Journal of Environmental Psychology 2001; 21(3): 273-281.
18. Riger S, Lavrakas PJ. Community ties: patterns of attachment and social interaction in urban neighbourhoods. American Journal of Community Psychology 1981; 9(1): 55-66.
19. Sampson RJ. Local friendship ties and community attachment in mass society: a multilevel systemic model. American Sociological Review 1988; 53(5): 766-779.
20. Stedman RC. Is it really just a social construction? The contribution of the physical environment to sense of place. Society and Natural Resources 2003; 16(8): 671-685.
21. Eisenhauer BW, Krannich RS, Blahna DJ. Attachments to special places on public lands: An analysis of activities, reason for attachments, and community connections. Society and Natural Resources 2000; 13(5): 421-441.
22. Beckley TM. The relative importance of sociocultural and ecological factors in attachment to a place. In: LE Kruger (Ed.). Understanding community-forest relations. Portland, OR: US Department of Agriculture Forest Science, Pacific Northwest Research Station, 2003.
23. Brehm JM, Eisenhauer BW, Krannich RS. Dimensions of community attachment and their relationship to well-being in the amenity-rich rural west. Rural Sociology 2004; 69(3): 405.
24. Brehm J. Community attachment: The complexity and consequence of the natural environment facet. Human Ecology 2007; 35(4): 477-488.
25. Hanlon N, Halseth G. The greying of resource communities in northern British Columbia: implications for health care delivery in already under-serviced communities. Canadian Geographer 2005; 49(1): 1-24.
26. McDonnel Smedts A, Lowe MP. Clinical training in the Top End: impact of the Northern Territory Clinical School, Australia, on the Territory's health workforce. Rural and Remote Health 7:723. (Online) 2007. Available: www.rrh.org.au (Accessed 25 October 2010).
27. Hall D, Garnet S, Barnes T, Stevens M. Drivers of professional mobility in the northern territory: Dental professionals. Rural and Remote Health 7:655. (Online) 2007. Available: www.rrh.org.au (Accessed 25 October 2010).
28. Garnett ST, Coe K, Golebiowska K, Walsh H, Zander K, Guthridge S et al. Attracting and Keeping Nursing Professionals in an Environment of Chronic Labour Shortage: A Study of Mobility among Nurses and Midwives in the Northern Territory of Australia. Darwin, NT: Charles Darwin University Press, 2008.
29. Carson D, Coe K, Zander K, Garnett ST. Does the type of job matter? Recruitment to Australia's Northern Territory. Employee Relations 2010; 32(2): 121-137.
30. Somers GT, Strasser RJB. What does it take? The influence of rural upbringing and sense of rural background on medical students' intention to work in a rural environment. Rural and Remote Health 7:706. (Online) 2007. Available: www.rrh.org.au (Accessed 25 October 2010).
31. General Practice and Primary Health Care Northern Territory. Productivity commission health workforce study. (Online) 2005. Available: http://www.pc.gov.au/__data/assets/pdf_file/0009/11142/sub132.pdf (Accessed 25 October 2010).
32. Carson D. Northern Territory Population Mobility Survey 2006: Summary of key findings. Darwin, NT: Charles Darwin University. 2008. Available: http://www.cdu.edu.au/sspr/documents/northern_territory_population_mobility_survey_2006.pdf (Accessed 25 October 2010).
33. Australian Government Department of Health and Ageing. HECS reimbursement scheme. (Online) 2008. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/work-pr-hecs-about (Accessed 25 October 2010).
34. Eley D, Young L, Przybeck TR. Exploring the temperament and character traits of rural and urban doctors. Journal of Rural Health 2009; 25(1): 43-49.
35. Australian Government Department of Health and Ageing. Report of the audit of health workforce in rural and regional Australia, April 2009. Canberra, ACT: Commonwealth of Australia, 2008.
36. Golebiowska K, Brown M, Carson D. What can potential interstate migrants find out about professional opportunities in the NT on the NTG web? Charles Darwin University Population and Tourism Studies Group Working paper series 2008109. (Online) 2008. Available: http://www.cdu.edu.au/sspr/documents/Brief2008019WhatcanprofessionalsfindonNTGweb.pdf (Accessed 25 October 2010).

