Introduction
The Australian medical workforce, like that of many developed nations, has a distinct urban bias1. Consequently, the rural medical workforce is both undersupplied2 and mal-distributed3,4. The Australian Medical Workforce Advisory Committee (AMWAC) has projected that by 2012 rural and remote areas could experience a shortfall of 1182 doctors5. Given that the Rural Doctors Association of Australia has reported that less than 5% of medical graduates have taken up rural practice in the last 15 years6, such shortfalls are not unexpected.
To redress this imbalance and inequity the Australian Commonwealth Government has established the Rural Clinical Schools (RCS) program7. Initially 9 medical schools were funded by the Commonwealth Department of Health and Ageing in 2000 to provide students with medical education and clinical training in a rural environment8. The establishment of the RCS program was based on research findings indicating that a strong relationship exists between rural educational exposure and an increased interest in pursuing a rural career or selecting a rural internship4,9,10. Currently the program involves 16 universities managing 17 RCSs throughout Australia, with each RCS consisting of multiple campus locations.
It is mandatory for all Australian medical students to undertake a minimum 4 week rural residential placement. However, short rotations are not as effective as longer term rotations in encouraging students to become part of the rural medical workforce11. Arguably this is because it takes time to appreciate the rural lifestyle, connect with the local community and its residents, and to feel an emotional attachment to rural living11,12. The RCSs are mandated to provide 25% of their parent medical schools' Commonwealth supported medical students with 1 year of their clinical medical education in a rural setting13. By 2006 there were 379 medical students enrolled across the 14 RCS programs8.
At times, in order to meet Commonwealth mandates, medical schools have conscripted students to RCS programs13. There are, however, reasons for caution in using this method of RCS recruitment. In one study, whether students planned to become part of the rural workforce was related to whether their attendance at rurally located training had been voluntary or compulsory; voluntary attendance was positively related while compulsory allocation was negatively related to students' decision to practice in a rural location14. Other studies have found that having a positive experience is of vital importance in determining future rural practice11,15,16. It is certainly arguable that unwelcome conscription may negatively taint rural training experiences.
While universities have various schemes to augment the numbers of students who attend their RCS, it is important to the development and sustainability of an adequate future rural medical workforce that medical schools are able to identify and foster the factors that encourage voluntary student recruitment to the RCSs. Finally, other countries are also building rural medical campuses and rural medical schools in order to address rural workforce shortages. The aim of this study is to determine which factors medical students consider in their decision to attend RCSs.
Method
In 2006, each of the 13 Australian universities managing RCSs were asked to participate in the survey and 6 agreed. These were the Universities of New South Wales, Melbourne, Tasmania, Adelaide, Sydney and the Australian National University. Students who had completed their RCS term were surveyed (n=166) and 125 responded, a response rate of 75%.
The FRAME Questionnaire 'Rural Clinical School Evaluation 2006' was developed as an evaluation tool to determine baseline data about students studying in an RCS17. Questions identified background characteristics including age, gender, marital status, dependents, ethnicity, admission and entry into medical school, rural background and education. Using a 6 point Likert scale, students were asked to indicate their level of agreement with 14 items concerning factors they considered in their decision to attend RCSs. These included family needs, academic reputation, patient access, transportation and accommodation. Students were also able to provide open-ended comments about their decision-making. Ethics approval for the study was obtained from each of the participating universities.
All data were pooled. The software SPSS v15 (SPSS Inc; Chicago, IL, USA; www.spss.com) was used to generate descriptive analyses and to identify factors used in the decision to attend the RCS. Qualitative analysis of responses to open-ended questions was performed where appropriate.
Results
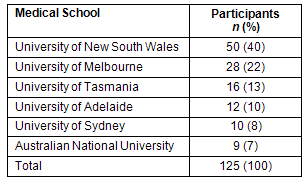
Respondents (Table 1) ranged in age from 21 to 43 years (M=24.5 years, SD=3.89), with 9 students aged 30 years or older. Approximately two-thirds of the sample was female (n=77, 62%). The majority of students were born in Australia (n=101, 83%), with 58 (47%) considering themselves to be from a rural background. There were 21 students (17%) born outside Australia who had lived in the country for an average of 19 years (M=18.63, SD=6.63). English was the second language of 15 (12%) students. The majority were single (n=109, 87%) with the remaining 16 (13%) married or in a de facto relationship. Of the 125 participants, only 6 students (5%) had children under 16 years. Sixty-nine (55%) students held at least one scholarship.
Table 1: Participants by medical school attended in 2006
Factors influencing the decision to attend an RCS were measured by 14 six-point Likert Scale questions. Students indicated their level of agreement (1=disagree strongly, 2=disagree moderately, 3=disagree slightly, 4=agree slightly, 5=agree moderately, 6=agree strongly) and responses were collapsed into 'disagree' (1-3) and 'agree' (4-6) for clarity. Whether each factor was a positive or negative consideration in choosing to attend an RCS was also recorded (Table 2).
Table 2: Factors influencing the decision to attend a Rural Clinical School
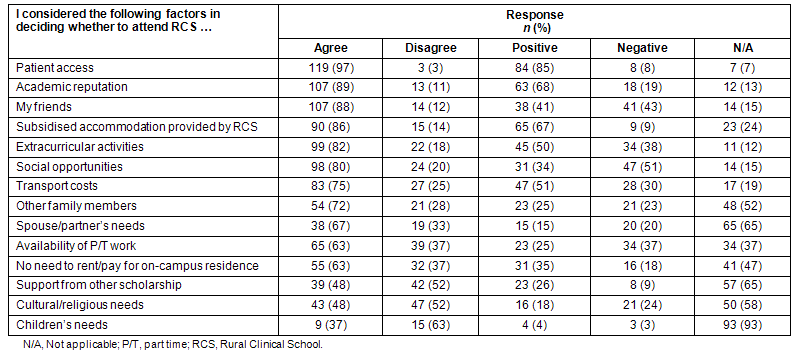
The key factor in choosing an RCS was 'patient access', with 97% (n=119) of students considering this important. In the decision-making process, 84% (n=81) indicated this factor had a positive influence on their selection. This suggests that students perceive RCSs as offering enhanced patient access. Another item featuring highly was 'academic reputation', with 89% (n=107) rating this as important and 68% (n=63) indicating this had a positive influence on their decision to choose an RCS.
Students were asked to provide comments on selecting the RCS option and 28 provided one or more comments. Of these, 10 (36%) said they believed the RCS would be a positive learning experience with comments about better student-doctor ratios, more 'hands on', smaller class sizes and better teaching. Comments included:
...the small numbers of students allow you to get more exposure to the doctors and more hands on experience as opposed to larger medical [clinical] schools.
[I] chose the RCS based on reputation for small class size and close contact with senior clinicians.
Interestingly, four of the students who provided written comments and were planning to work in a rural setting, wanted the RCS option to help establish ties and develop an understanding of rural practice; however two, who were also planning to work in a rural setting, reported that they would have preferred to complete their training in metropolitan medical schools. One student wrote:
I selected the RCS as an option due to my wanting to do rural medicine [general practice] in the future.
Another said:
Having come from a rural background I felt I was just getting my feet in the city when I was sent back to my hometown to study which I had just spent 18 years living in... and, I would have preferred to get some experience in the city, rather than going to the country where I know I am going to end up anyway.
Further, seven students commented on the availability of social opportunities in their decision to attend an RCS, with three indicating this was a positive factor, and four indicating this was a negative factor. Students wrote:
...excited to try something new, meet new people, see a new area in Australia.
...wanted a change/opportunity for new experiences and to challenge myself - having only ever lived in an urban environment.
Some students were concerned about distance and being away from their family:
I was isolated from my family as it would take me 4-5 hours to travel home.
However, another noted:
It was fantastic as I was able to return to the place where I grew up, and have family support.
Six students believed that accommodation would be more affordable or easier at the RCS:
I had no qualms in coming rural as it meant cheaper rent and a nicer lifestyle.
...no rent was a positive factor.
Another eight students viewed a rural lifestyle as having a positive influence on their decision to attend an RCS. Some students stated they preferred the country lifestyle with statements such as:
I can't breathe in the city, I love the country too much!
Nice area, close to national parks, something different.
Discussion
When students consider whether or not they will attend a RCS, it is apparent from this study that both clinical and non-clinical factors are taken into account. The primary factor considered in the present study was patient access. Other major factors, friends and academic reputation, appear equally considered. However, factors differed in the degree to which they were judged positive or negative.
Patient access was identified as a positive consideration by the majority of students in this study, and certainly numerous studies concur that better patient access is an RCS drawcard10,13,16,18. In this context, patient access refers to the ability to interact with the local patient population in a more direct manner than is possible for the urban student. The rural medical student is part of a small healthcare team, often involving only staff specialist and medical student. In contrast, the urban-based teaching team tends to be larger, composed of staff specialist, registrars of various levels and an increased number of medical students. Thus, the urban medical student tends to play a lesser role in patient-doctor interaction. Anecdotally, because rural areas are less saturated with medical practitioners and students, patients are reportedly more accepting of, and welcoming toward, the presence of medical students.
This particular RCS characteristic was not initially apparent to early students; a situation echoed in the UK where rural clinical placements are relatively new19. Reminiscent of the initial Australian experience13, UK students report they expect rural placements will provide a narrow range of patient contact19. Experience shows however that RCSs are able to provide 'excellent access to a willing population'20. As student numbers increase in Australia, RCSs should protect and maintain this critically valuable characteristic. Such 'access and enthusiasm'20 may be lost without careful planning20, particularly if student numbers are allowed to increase past saturation point21. Students remain in constant 'cyber-connection'22 and the impact of other students' experiences, recommendations and testimonials regarding RCS attendance should not be undervalued. These have been identified as having a substantial influence on students' decision to attend an RCS10. In short, if decreased patient access impinges on clinical learning, students will quickly take that into account.
The importance attributed to the academic reputation of RCSs by the participants of the present study is not surprising. Most students are achievement oriented22 and would not consider attending an RCS unless they could attain results at least equivalent to those achieved by metropolitan-based students22. Although the development of an academic record of excellence takes time20, it would appear that for many Australian RCSs, this time has passed23. In one study, over 80% of medical students reported they expected the RCS would provide 'broader and better clinical and academic learning opportunities'22 than those received by their city counterparts. The RCS students achieve equivalent, if not better, academic results than their city counterparts10,24. While academic reputation was a positive consideration for 68% of those who considered this in their decision to attend an RCS, 32% of students were not convinced about academic performance. While the achievement of high academic standards appears an imperative for RCSs, it is notable that these results have been achieved despite shortages of traditional academic teaching clinicians23.
While other studies have identified that family and partners play a significant role in the decision to attend an RCS25, the present study found these factors were considered eighth and ninth, respectively, in a hierarchy of 14 factors. This ranking may be a by-product of the respondents' relationship profiles (87% were single) and age profile (M=24.5 years, SD=3.89). However, as some medical schools offer both undergraduate and graduate degrees, RCSs should be aware of the influence that family and partner/spouse can have in the relocation decision-making process, particularly in relation to graduate students. Already more mature, these students may have strong family and financial ties to their metropolitan location20. Importantly, if medical students decide not to attend an RCS, their decision appears more often related to non-clinical/social factors rather than clinical or academic factors13; therefore, partner/spouse attitudes toward a rural location should not be underestimated. Further, a partner's rural background has been shown to have an odds ratio of 3.0 when predicting the likelihood of a medical graduate taking up practice in a rural and remote location4.
In the present study, 88% of students considered their friends when deciding whether to attend an RCS. Interestingly, even though for 43% of respondents 'friends' was a negative consideration, these students still decided to attend an RCS. This too may be indicative of the relationship and age profile of the respondents. Thus, the influence of family and partner/spouse (for those affected) appears quite formidable and much stronger than that of friends. Arguably, therefore, if medical schools were to provide their students with detailed information25 regarding rural relocation very early in their degree structure20, such relocation may be realistically considered by more students, particularly those with a family/spouse/partner.
Although rural origin is reportedly one of the most significant predictors of rural practice uptake4,15,16, the findings of the current study indicate that not all students from a rural background, even those with the intention of ultimately taking up a rural practice, wish to undertake rural clinical training. For one student in the present study this was because s/he believed s/he would 'end up' in a rural location 'anyway'; for another, urban living was a welcome change after 18 years in a rural area. These findings indicate that medical schools should remain mindful of such scenarios, particularly if student conscription becomes necessary. Indeed, given that those with a rural background are approximately twice as likely to work as rural doctors, compared with their urban counterparts4, perhaps it is open-minded urban students that medical schools should instead strive to recruit to their RCSs. After all, urban-background medical graduates in a Canadian study reported that, 'exposure to rural practice during medical school or residency was the most important factor in their decision to practice rural medicine'26.
Conclusion
Students consider both clinical and non-clinical factors in their decision to attend an RCS13,18,25. Having identified these factors, it is critical to the enlargement and sustainability of a future rural medical workforce that these factors be further developed, protected and improved upon by RCSs. Of note is that the deliberate rural streaming of rural-origin students may be counter-productive to the ultimate workforce mission of the RCS, if rural-origin students wish to train in a metropolitan environment. Moreover, assuming that there is enough 'experience' and capacity for rural-origin students, further research should focus on outcomes related to urban-origin students who might be recruited to an RCS experience. After all, having identified what attracts medical students to consider an RCS - if you build it they will come - the entire 25% of students trained at RCSs will not stay rural. Thus we must go further in order to solve the workforce crisis. Of arguably greater importance, is recruiting and encouraging urban-origin students to a future rural medical workforce, as indications are that, at least for some if they experience it, they will come back.
Acknowledgements
This study was funded by the Australian Government Department of Health and Ageing. It was authored on behalf of the FRAME Investigators and the authors acknowledge the support of the following FRAME members, and their staff at the RCSs, who agreed to allow, and facilitated, their students' involvement in this study: Professor Louis Pilotto (University of New South Wales), Professor Judi Walker (University of Tasmania), Associate Professor Joseph Canalese (University of Sydney), Associate Professor Jonathan Newbury (University of Adelaide), Professor Amanda Barnard (Australian National University).
References
1. Wilson NW, Couper ID, DeVries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health 9: 1060. (Online) 2009 Available: http://www.rrh.org.au (Accessed 7 September 2010).
2. Strong K, Tricket P, Titulaer I, Bhatia K. Health in rural and remote Australia. Canberra, ACT: Australian Institute of Health and Welfare, 1998.
3. Wilkinson D. Inequitable distribution of general practitioners in Australia: analysis by state and territory using census data. Australian Journal of Rural Health 2000; 8: 87-93.
4. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11(6): 277-284.
5. Health Workforce Queensland and New South Wales Rural Doctors Network. Medical practice in rural and remote Australia: combined rural workforce agencies national minimum data set report as at 30th November 2005. Brisbane, QLD: HWQ, 2006. Available: http://www.healthworkforce.com.au/downloads/Publications/1698_MDS%20Report%202005_final_nocov.pdf (Accessed 9 September 2010).
6. Rural Doctors Association of Australia. Response to the review of rural health programs: issues paper. Kingston ACT: Rural Doctors Association of Australia, 2009.
7. Australian Government Department of Health and Ageing. Workforce education and training - Rural Clinical Schools. (Online) 2010. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/work-st-rcs#list (Accessed 9 September 2010).
8. Australian Government Department of Health and Ageing. Report on the audit of health workforce in rural and regional Australia - rural based education. (Online) 2008. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/work-res-ruraud-toc~work-res-ruraud-3~work-res-ruraud-3-2~work-res-ruraud-3-2-1~work-res-ruraud-3-2-1-rur (Accessed 9 September 2010).
9. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37: 809-814.
10. Eley D, Young L, Baker P, Wilkinson D. Developing a rural workforce through medical education lessons from down under. Teaching and Learning in Medicine 2008; 20(1): 53-61.
11. Denz-Penhey H, Shannon S, Murdoch JC, Newberry JW. Do benefits accrue from longer rotations for students in Rural Clinical Schools? Rural and Remote Health 5: 414. (Online) 2005. Available: http://www.rrh.org.au (Accessed 7 September 2010).
12. Ranmuthugala G, Humphreys J, Solarsh B, Walters L, Worley P, Wakerman J et al. Where is the evidence that rural exposure increases uptake of rural medical practice? Australian Journal of Rural Health 2007; 15: 285-288.
13. Jones GI, DeWitt DE, Cross M. Medical students' perceptions of barriers to training at a rural clinical school. Rural and Remote Health 7: 685. (Online) 2007. Available: http://www.rrh.org.au (Accessed 7 September 2010).
14. Rolfe IE, Pearson SA, O'Connell DL, Dickinson JA. Finding solutions to the rural doctor shortage: the roles of selection versus undergraduate medical education at Newcastle. Australian New Zealand Journal of Medicine 1995; 25: 512-517.
15. Jensen CC, DeWitt DE. The reported value of rural internal medicine residency electives and factors that influence rural career choice. Journal of Rural Health 2002: 18: 25-30.
16. Spencer RJ, Cardin AJ, Ranmuthugala G, Sommers GT, Solarsh B. Influences on medical students' decisions to study at a rural clinical school. Australian Journal of Rural Health 2008; 16: 262-268.
17. DeWitt DE, McLean R, Newbury J, Shannon S, Critchley J. Development of a common national questionnaire to evaluate student perceptions about the Australian Rural Clinical Schools Program. Rural and Remote Health 5: 486. (Online) 2005. Available: http://www.rrh.org.au (Accessed 7 September 2010).
18. Eley DS, Baker PG. Will Australian rural clinical schools be an effective workforce strategy? Early indications of their positive effect on intern choice and rural career interest. eMJA The Medical Journal of Australia 2007; 187(3): 166-167.
19. Deaville JA, Wynn-Jones J, Hays RB, Coventry PJ, McKinley RK, Randall-Smith J. Perceptions of UK medical students on rural clinical placements. Rural and Remote Health 9: 1165. (Online) 2009. Available: http://www.rrh.org.au (Accessed 7 September 2010).
20. Jones GI, DeWitt DE, Elliot SL. Medical students' reported barriers to training at a rural clinical school. Australian Journal of Rural Health 2005; 13: 271-275.
21. Eley, DS, Young L, Wilkinson D, Chater AB, Baker PG. Coping with increasing numbers of medical students in rural clinical schools: options and opportunities. Medical Journal of Australia 2008; 188(11): 669-671.
22. Denz-Penhey H, Murdoch JC. Reported reasons of medical students for choosing a clinical longitudinal integrated clerkship in an Australian rural clinical school. Rural and Remote Health 9: 1093. (Online) 2009. Available: http://www.rrh.org.au (Accessed 7 September 2010).
23. McLean RG, Pallant J, Cunningham C, DeWitt DE. A multi-university evaluation of the rural clinical school experience of Australian medical students. Rural and Remote Health 10: 1492. (Online) 2010 Available: http://www.rrh.org.au (Accessed 7 September 2010).
24. Waters B, Hughes J, Forbes K, Wilkinson D. Comparative academic performance of medical students in rural and urban clinical settings. Medical Education 2006; 40: 117-120.
25. Mihalynuk T, Snadden D, Bates J, Scott I, Frinton V, Wilson G. Size matters: what influences medical students' choice of study site? Medical Teacher 2008; 30: e108-e114.
26. Chan BTB, Degani N, Crichton T, Pong R, Rourke J, Goertzen J et al. Factors influencing family physicians to enter rural practice. Canadian Family Physician 2005: 51: 1246-1247.




