In some rural and remote locations in New South Wales (NSW), as well as in other Australian states, where the delivery of healthcare access is limited by the availability of various specialist and allied health services1,2, GPs and registered nurses (RNs) who have completed a short course in basic radiography may perform X-ray examinations when or where a radiographer is not available. They are referred to as 'remote X-ray operators', or simply 'remote operators' and are licensed under the NSW Radiation Control Act 1990 to perform limited general radiography, including chest and limb examinations3. Metropolitan-based practitioners are specifically excluded from holding a licence. Remote X-ray operators provide a valuable service that prevents rural and remote residents from having to travel to access minor radiographic examinations.
This is an example of 'skills transfer' or substitution4. Nancarrow and Borthwick recognised both vertical and horizontal substitution in the health workforce5. Vertical substitution involves 'the delegation or adoption of tasks across disciplinary boundaries where the levels of training and expertise (and generally power and autonomy) are not equivalent between workers'5. Willis referred to 'vertical specialisation' as being highly regulated, involving the phenomenon called 'pass-the-task'6, where more routine or mundane tasks are delegated to a subordinate occupational group. Horizontal substitution, however, involves the passage of tasks between providers with similar levels of training and expertise5. This form of skills transfer is less regulated. Remote X-ray operator radiography has characteristics of both forms of substitution.
It has been demonstrated elsewhere that different health professionals perceive and construct the task of performing radiography from different perspectives, which can affect the quality of the service4. It is argued that their experiences and perceptions are largely dictated by their core disciplinary role that is founded in their differing professional backgrounds, education and training. These affect how they construct both their primary role as GP or nurse and integrate it with their less familiar role as a remote X-ray operator7.
In radiography, the risks associated with a suboptimal examination are, foremost, unnecessary exposure to X-radiation due to poor radiographic technique, and resultant poor image quality, leading to repeated views and examinations8. Other significant risks include causing a patient unnecessary pain, discomfort or further injury because of poor positioning, and the possibility of a missed or mis-diagnosis as a result of either inferior image quality or inaccurate positioning, or both. These risks may be partly offset by the provision of high quality continuing education.
In some Australian states where limited X-ray licensing also exists, the competency of licensees is periodically reassessed as part of the process of licence renewal9. In addition, GPs who hold a remote area exemption to bill Medicare for the provision of diagnostic radiology services are required to participate in a quality assurance and continuing education program10. Under the NSW Radiation Control Act 1990, however, remote X-ray operators' licenses are renewed annually with no demonstration of competency or continuing education required3. The aim of this survey, therefore, was to investigate the self-reported radiographic competency of remote X-ray operators in NSW and their self-perceived need for continuing education in radiography and radiology. It was also an opportunity to gather background information about the NSW remote X-ray operator workforce.
Following approval from the University of Newcastle Human Research Ethics Committee, and with the cooperation of the NSW Department of Environment and Climate Change (DECC), questionnaires were mailed to all 131 remote X-ray operators in NSW. The mail-out took place in early June 2009, with reminder letters sent 6 weeks later.
The questionnaire consisted of 30 close-ended questions, requiring 'tick-the-box' responses, plus 3 open-ended questions, one asking their preferred mode of continuing education, another asking what kind of support they need to undertake continuing education, and the third inviting further comments. In one question, respondents were asked to rate their own competency in 12 examination types covered by their licence. A short clinical history was given and participants were asked to indicate whether they felt 'Not competent', 'Unsure' or 'Competent' in performing the examinations (Fig1). A similar style of question was used to ask 'how challenging' respondents found 10 specific aspects of general radiography, and to self-rate their 'level of understanding' of 9 other radiographic tasks. For these questions respondents were asked to score themselves on a scale of 1 to 5, where 1 was 'Very challenging' and 'Excellent understanding', respectively (Figs2,3).
Questionnaires were returned via pre-paid post and data were entered into a Microsoft Excel spreadsheet. Data analysis was performed using SPSS v17 (www.spps.com). Open-ended questions were analysed using qualitative research techniques to categorise responses.
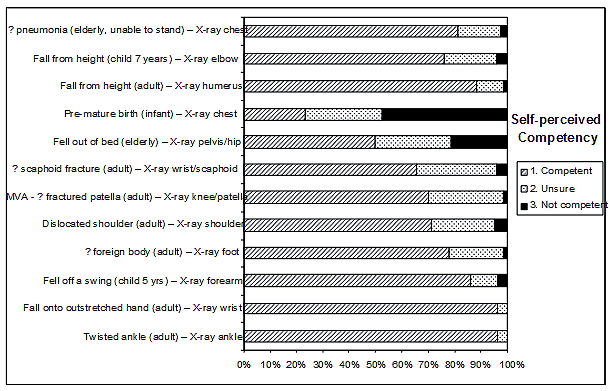
Figure 1: Responses regarding how competent respondents felt to perform particular examinations.
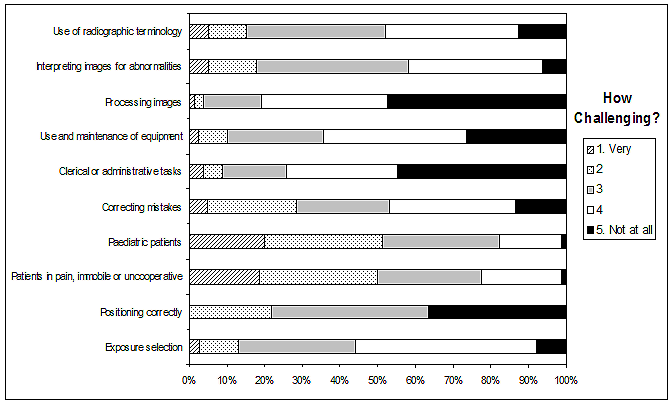
Figure 2: Responses for how challenging respondents found certain aspects of radiography.

Figure 3: Responses for how well respondents understood certain aspects of radiography.
Results
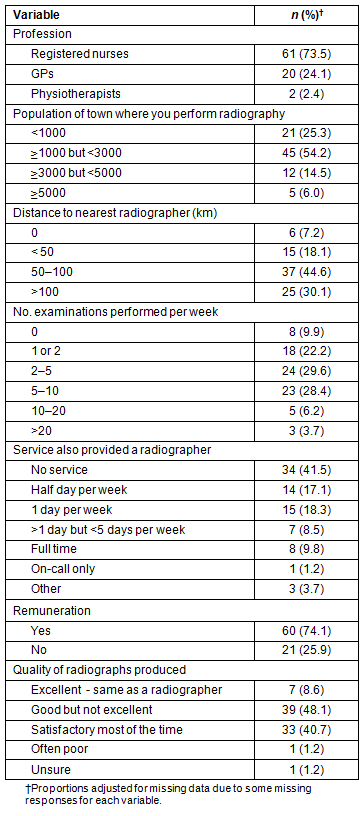
A total of 83 valid responses (63%) were received, of which 61 (74%) were from RNs and 20 (24%) from GPs; two physiotherapists also responded (Table 1). Approximately 80% of the respondents performed radiography in towns of 3000 people or less and three-quarters were located 50 km or more from the nearest radiographer-staffed service. Approximately 57% said that they and their remote operator colleagues at the same site performed an average of between 2 and 10 examinations a week. However, there were 8 respondents who said they did no radiography at all in an average week. Approximately 42% worked at a location where there was no radiographic service provided by a radiographer, while approximately 44% worked where a radiographer provided a fractional service on a regular basis, up to several days a week. Only 8 respondents were at a location where a radiographer was employed full time. Asked whether they were remunerated for their radiographic work, approximately three-quarters said 'Yes'. Only two of the 20 doctors said 'No', compared with almost one-third of the nurses/physiotherapists. Most of the GPs received Medicare payments, while others charged visiting medical officer rates. Approximately half of the non-medical remote operators said they received an 'allowance' ($AU6, according to one respondent).
Table 1: Participant background information
Very few respondents felt that their radiography was of the same standard as that of a radiographer (Table 1), although approximately half thought it was 'Good but not excellent' and another 41% said it was 'Satisfactory most of the time'. Respondents rated their competency in performing 12 different radiographic examinations (Fig1). For only two examination types (ankle and wrist) did more than 90% of the respondents describe themselves as feeling competent. The infant chest X-ray had the lowest proportion of respondents in the competent category (23%, n=18). For 6 other examinations less than 80% of respondents felt competent.
The results for the questions 'How challenging do you find ...?' and 'How well do you understand ...?' (related to a range of knowledge and skill aspects of radiographic practice) are given (Figs2,3). The most challenging were performing examinations on paediatric patients and difficult patients, which generally require higher level radiographic and patient interactional skills11,12. The least challenging were image processing and administrative tasks. The highest self-reported level of understanding was in 'Radiation protection' and the lowest in the more cognitively complex tasks of evaluating radiographs for errors, image quality assessment, and identifying radiographic pathology13-15.
The responses to questions about continuing education and about feedback received about their radiography are shown (Table 2). Fifteen respondents answered that they 'Never' do any continuing education in radiography and radiology and another 28 'Rarely' did so. The proportion of nurses and physiotherapists who never or rarely did continuing education in this field was 61% (n=38), compared with the GP remote operators at 26% (n=5). Sixty-five respondents (80%), however, felt a need for continuing education. There were only 4 respondents who felt they did not need continuing education in radiography and radiology (3 doctors and one nurse).
Table 2: Continuing education and feedback
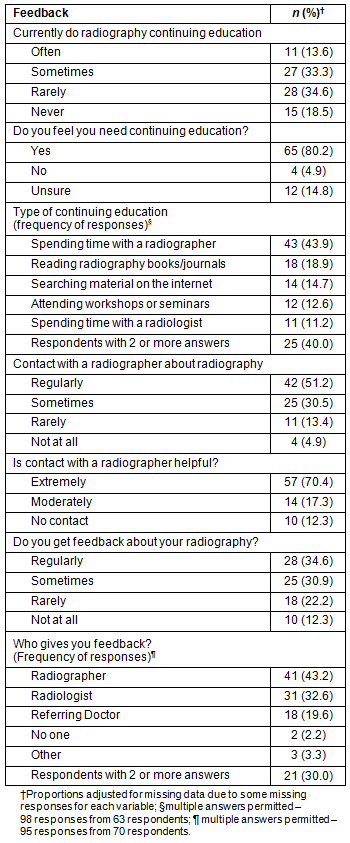
'Spending time with a radiographer' was the most common form of continuing education (44% of total responses; Table 2). Respondents could choose more than one answer to this question so there were 98 responses from 63 respondents. Asked whether they had contact with a local radiographer, approximately half said they 'Regularly' had contact, and a further 30% 'Sometimes' had contact with a radiographer. Approximately 70% said this was 'Extremely' helpful. Approximately two-thirds of respondents received feedback about their radiography either 'Regularly' or 'Sometimes'.
Again, with multiple answers allowed, the local radiographer was the most common person to give feedback , the next most common being the radiologist and then the referring doctor (Table 2); there were 92 responses from 70 respondents. Among the 16 GPs who received feedback, the local radiographer was nominated only 4 times in 20 responses, much less than among the non-medical remote operators, who nominated the radiographer 36 times in 72 responses from 54 respondents. Fourteen of the 16 GPs who received feedback nominated the radiologist as a source of that feedback.
Open-ended questions
Examples of the responses to the 3 open-ended questions (preferred methods of continuing education, support needed to undertake radiography continuing education, and other comments) are given according to theme, with the number of comments received on a specific theme provided in brackets after each quotation.
Preferred methods of continuing education: Responses relating to preferred methods of continuing radiography education were classified into the following 4 categories.
Face-to-face training This was the strongest preference, with respondents suggesting the need for regular in-service activities, incorporating a practical component. Suggestions included one or 2 days of intensive face-to-face training at intervals ranging from half-yearly to every 2-3 years. There were divided opinions about whether this was best undertaken locally or elsewhere. This was regarded by some as an opportunity for networking with other remote operators and with radiographers and as a means of earning continuing medical education (CME) points.
Couple of days of in-service where we can learn and discuss problems with other remote operators [#27]
Education with a group of other remote operators. Hands on plus revision of exposure settings and positioning [#24]
Working with a radiographer Spending time working alongside a radiographer was also a strong preference. Some respondents' linked this to face-to-face training and the opportunity to network. Again opinions varied about whether this should take place locally, on-site or at a larger centre or base hospital.
Day spent with radiographer to improve techniques and opportunity to ask questions [#10]
Time in a metropolitan centre for 5 days per year working in radiography [#66]
Review or audit of radiographs Some respondents already had their radiographs reviewed, while others saw a need for a formal process of critiquing and feedback. This was regarded as an opportunity for closer interaction with the local radiographers or the radiologists reporting on the images.
Currently on monthly basis 10 X-rays reviewed. It would be helpful to do this on a more formal basis [#3]
More feedback from reporting radiographer on quality of X-rays and areas required to improve. Perhaps returning a form designed for this purpose [#11]
Distance or online education Various means of self-directed learning were mentioned, including online education. However, these were generally considered less satisfactory than or supplementary to face-to-face training. It was thought that web-based continuing education may address some time-related issues; however, more practical training was generally preferred.
1. face-to-face followed up by 2. on-line [#42]
... but as time off or away to attend study sessions is infrequent, on-line would be a big bonus [#54]
Support needed to undertake radiography continuing education: The kind of support needed to undertake radiography continuing education fell into three themes, as follows.
Time off Time was the dominant consideration, although it overlapped with staffing issues. Comments were made about the difficulty of finding time for study leave, to arrange locums or to back-fill positions when staff members are away doing training. Some respondents suggested that they would have to undertake continuing education on weekends or in their own time.
... to perform and discuss X-rays without interruption from regular duties [#51]
Some roster support to spend time with local radiographer now and then...the only support that really works is being taken off the work roster for the required period [#54]
Financial support The issue of financial support was raised in the context of paid education time or receiving the appropriate amount of paid hours for continuing education. Others raised issues about being reimbursed for expenses such as course registration fees, travel and accommodation.
Appropriate amount of paid hours for continuing education [#44]
Payment of course/travel/lost income costs, as is done for emergency training [#48]
Managerial support Generally, respondents were confident that they would receive the necessary support and encouragement from their managers, although some were not as positive.
I think our manager would always be willing to give me time for a refresher [#50]
Many managers think that once you have the qualification that is it. It solves their problem about having someone to take X-rays, which is all they care about, not the future education [#47]
General comments: More than 30 respondents made general comments. Several made positive comments about the value of having a limited X-ray licence, such as:
I still enjoy using this skill and it has regularly been a huge advantage to local residents and doctors to know the same day/hour for sure and plan care accordingly. Hours and miles in pain are cut. Stress is minimised and people are usually better, more comfortable, supported locally. Also cheaper for patients and the health service. [#54]
Others raised issues about the restrictions on the use of the licence:
Would like to be able to do a lateral chest as find radiologist often reports needs to diagnose properly. Don't see the need for hip X-rays as problem can usually be diagnosed clinically the need to transfer to larger centre [#64]
However, three of the GPs agreed strongly that continuing education in radiography and radiology was not a high priority for them, for example:
With the other education priorities I have a rural GP, X-ray QA & CE is right down the list. [#20]
Another of the GPs commented:
[It is] very hard working this stuff for GP remote X-ray operators as more difficult to get time off work, costs to practice of loss of GP if on a working day, on call coverage etc. [#12]
Discussion
Remote X-ray operators only perform a small number of X-ray examinations. However, this in itself raises concerns about their level of competency in dealing with individual patients, especially in performing difficult, sometimes painful examinations, if they are not regularly practicing their radiographic skills. There are no competency requirements or minimum examination numbers to retain a NSW remote X-ray operator licence. As long as the annual fee is paid their licence is renewed, even if they perform no radiography at all, as was the case for 8 survey respondents. The lack of competency requirements for NSW remote X-ray operators called to the attention of the Garling Special Commission of Inquiry into Acute Care Services in NSW Public Hospitals, resulting in a recommendation that the licence conditions are amended to 'include the requirement for a quality audit of remote operators who hold licenses under the Act to perform X-ray radiology services' (p.863)16. No action has been taken by the NSW Government on this recommendation to date.
The evidence from this survey is that a considerable proportion of NSW remote X-ray operators do not feel as competent as they should to perform the full range of examination types covered by their licence. Furthermore, most feel they need continuing education in radiography and radiology. Many already participated in a voluntary, self-regulated program of skills maintenance, most through their contact with a local radiographer. However, more than 40% of respondents worked at a site where there was no service provided by a radiographer and the majority worked at a location that was at 50 km away from a where a radiographer was employed, making it necessary for them to travel for this form of support.
Skills transfer should be part of the solution to the health workforce shortfall17, particularly in underserved areas; however, the risk of compromising service quality and patient safety must be recognised when renegotiating role boundaries and creating new, more flexible models of care. It should not be assumed that tasks or roles transferred across professional boundaries will be readily integrated with health professionals' existing (or other new) duties, responsibilities and expectations. A regimen of continuing education is necessary to assure optimum service quality and outcomes are maintained, no matter who performs the task or role. A Cochrane review found sound evidence that continuing education, particularly in the form of interactive workshops, the respondents preferred mode of delivery, has moderate to moderately large, positive effects on professional practice and healthcare outcomes18. This, together with the strong self-perceived need for continuing education19, is a strong indicator for change in the current licensing conditions for remote X-ray operators in NSW, as well as in other Australian states where the situation may be similar.
There were some notable differences in the self-perceived need of the GPs and that of the other remote operators for continuing education in radiography. Some GPs were strongly opposed to the idea, generally because their workload and other continuing education commitments were already burdensome. It has been noted elsewhere, however, that while GP remote operators generally have a stronger knowledge-base, their skills may still be lacking7. A much higher proportion of GPs compared with the non-medical remote operators took part in continuing education in this field, influenced by their continuing medical education requirements20. However, the GPs in this study were more inclined to refer to radiologists than radiographers for feedback about their radiography. It is suggested that this is because of issues related to the perceived higher professional status of doctors compared with other health professionals, which is known to inhibit effective communication and collaboration21,22. While contact with a radiologist will help their understanding of what views are required and why, contact with a radiographer will also address the challenges involved in getting the required views on patients who are in pain, have a limited range of movement or are unable to refrain from moving.
There is a need to put aside issues of professional status and hierarchy in the design of new models of care that include skills transfer. At times, as in the case of GP remote operators, the requisite knowledge and skills may be transferred from traditionally lower to higher status health professionals - in the reverse direction to Willis's 'vertical specialisation', cited earlier6. Wherever skills or competencies are shared across professional boundaries, it is beneficial to the health professionals involved, and to their patients, if the relationship is based on collaborative practice and teamwork, which include cooperation, communication, shared responsibility and, above all, trust23,24. It can be argued that sharing knowledge in a common, interactive learning environment will strengthen the sense of interprofessional teamwork and develop a better understanding of each others' core disciplinary role, no matter what the professional background of the participants.
At the same time, however, because of their foundation knowledge of anatomy, physiology and radiology, and their core role as diagnosticians, the GPs may have different learning needs and education requirements from the nurses and physiotherapists25. Rural doctors also have a great many demands on their time and, given the need travel to access most continuing education, they must be selective about how to use their time in meeting needs and requirements. Such differences should be catered for in designing continuing education resources in this or any other field where skills transfer is implemented. Educational packages and the mode of delivery must address the diverse learning needs of the various health professionals involved.
This survey also raises issues related to the remuneration of remote X-ray operators for performing radiography that cannot be ignored. Self-referral and payment per examination poses a risk of unnecessary exposure of patients to ionising radiation, where the only justification maybe financial26. Concerns also exist about the variation in how remote operators are remunerated. For example, some nurses receive a small allowance yet others receive no payment for performing radiography. It is difficult to imagine that remote X-ray operators will take due responsibility for their extended role if they are given only a paltry allowance or are unpaid. Indeed, this trivialises the role and may be a further disincentive to undertaking continuing education in the field, particular when they are not provided paid study leave to do so. These issues should be examined further.
Limitations
There are inherent limitations in the use of self-assessment in the measurement of competency27. Davis et al. found both positive and inverse comparisons with external assessment and that the poorest accuracy in self-assessment was among those least skilled and those who were most confident. In this study, it is probable that individual participants have either overestimated or underestimated their competency but, because there is no comparable external measure of competency, it is not possible to know how this biases the results. The effect of this self-assessment bias will be exacerbated by the small number of respondents.
There is a need for more objective assessment of radiographic competency of remote operators. While image quality and positioning accuracy can be objectively measured from the resultant images, radiographic competency includes elements of patient interactional skills and decision-making abilities that require observational assessment at the time the examination is performed. In this sense, competency self-assessment using a three-point, Likert-type scale (competent, not competent or unsure) vastly oversimplifies the concept of radiographic competency. Further, the use of a three-point scale may magnify biases associated with the five-point Likert scale, such as a tendency for respondents to choose the equivocal midpoint rather than the extreme endpoints.
The purpose of continuing education is to improve outcomes for patients by improving clinical practice. It is apparent from this survey that there is a need for continuing education of remote X-ray operators in NSW. These health professionals work outside the traditional occupational boundaries of their profession, providing an essential service where and when no service is otherwise available. If they are to provide safe, high quality services they need to be supported in their atypical role by the provision of continuing education. Recognising the special circumstances and isolation under which they work, ongoing educational support, as well as the opportunity to benchmark their practice against more mainstream services, should be embedded in the licensing regimen, as recommended by the Garling Special Commission.
Recommended strategies are the implementation of a scheme of regular, local workshops, preferably conducted by the local radiographers. These would strengthen the sense of team work and increase opportunities for communication. However, this is time-consuming for all concerned and there is also a need for other forms of self-directed learning to supplement and complement the face-to-face workshops. These may include online, web-based methods of teaching and learning and recurrent quality audits of radiographic examinations, with feedback about ways to improve service quality and outcomes. It is also recommended that further analysis of the quality of remote X-ray operator radiography is carried out and correlated with the number of examinations performed and the frequency and type of continuing education. This information should used to establish benchmarks and standards in this field.
Limited licence, remote X-ray operator radiography is not unique to NSW. It exists in rural and remote parts of all Australian states, with several hundred practitioners nationwide, although the precise figure is unknown. While some states already have mandatory competency requirements, there is an opportunity to develop a best practice model for supporting and re-credentialing limited X-ray holders and to create a national benchmark. Doing so would not only have benefits in this field, but would also be relevant in other healthcare arenas where skills transfer is practised or may be practised in the future as the health workforce evolves.
References
1. Wakerman J. Defining remote health. Australian Journal of Rural Health 2004; 12(5): 210-214.
2. National Rural Health Alliance. Under pressure and undervalued: allied health professionals in rural and remote areas. (Online) 2004. Available: http://nrha.ruralhealth.org.au/cms/uploads/publications/allied%20health%20final%20november%202004.pdf (Accessed 30 March 2010).
3. Government of New South Wales. 1993, Radiation Control Act 1990 No.13. (Online) 2010. Available: http://www.legislation.nsw.gov.au/fullhtml/inforce/act+13+1990+first+0+N (Accessed 23 June 2010).
4. Smith T. 'Skill transfer' and interprofessional boundaries in rural and remote radiography. Australian Journal of Rural Health 2007; 15: 273-274.
5. Nancarrow SA, Borthwick AM. Dynamic professional boundaries in the health workforce. Sociology of Health and Illness 2005; 27(7): 897-919.
6. Willis E. Medical dominance. Sydney, NSW: Allen & Unwin, 1989.
7. Smith T, Jones P. Remote X-ray operator radiography: a case study in interprofessional rural clinical practice. Journal of Interprofessional Care 2007; 21(3): 289-302.
8. Smith T. Radiographic technique: justification and optimisation. In: H Warren-Forward (Ed.). Patient dose levels and risk in diagnostic radiology: Proceedings of the Newcastle Medical Radiation Symposium. Newcastle, NSW: The University of Newcastle, 2000.
9. Queensland Health Radiation Health Unit, Queensland Government. Information sheet: Licensing of X-ray operators. Available: http://www.health.qld.gov.au/radiationhealth/ (Accessed 23 June 2010).
10. Glazebrook R, Chater B, Graham P. Rural and remote Australian general practitioners' educational needs in radiology. Journal of Continuing Education for Health Professionals 2001; 21: 140-149.
11. Bowman S. The radiographer/patient relationship: a short term but vital interaction. Radiography Today 1993; 59(675): 17-18.
12. Culmer P. Models of radiographic practice. In: A Paterson, R Price (Eds). Current Topics in Radiography (Number 3). London: WB Saunders, 1997.
13. Bowman S. Technical evaluation of radiographs: a case study in radiographic judgment and decision-making. In: A Paterson, R Price (Eds). Current Topics in Radiography (Number 3). London: WB Saunders, 1997.
14. Nodine CF, Krupinski EA. Perceptual skill, radiology expertise, and visual test performance with NINA and WALDO. Academic Radiology 1998; 5(9): 603-612.
15. Donovan T, Manning DJ. The radiology task: Bayesian theory and perception. British Journal of Radiology 2007; 80(954): 389-391.
16. State of New South Wales. Final Report of the Special Commission of Inquiry: Acute Care in NSW Public Hospitals, 2008. Volume 2. (Online) 2010. Available: http://lawlink.nsw.gov.au/Lawlink/Corporate/ll_corporate.nsf/pages/attorney_generals_department_acsinquiry (Accessed 23 June 2010).
17. Duckett SJ. Health workforce design in the 21st century. Australian Health Review 2005; 29: 201-210.
18. Forsetlund L, Bjørndal A, Rashidian A, Jamtvedt G, O'Brien MA, Wolf F et al. Continuing education meetings and workshops: effects on professional practice and health care outcomes. Cochrane Database of Systematic Reviews 2009, Issue 2. Art. No.: CD003030. DOI: 10.1002/14651858.CD003030.pub2
19. Grant J. Learning needs assessment: assessing the need. BMJ 2002; 324(7330): 156-159.
20. Glazebrook R, Chater B, Graham P, Kokar G, Robinson M, Escott R et al. Evaluation of the ACRRM national radiology program for Australian rural and remote medical practitioners. Rural Remote Health 5(3): 349. (Online) 2005. Available: www.rrh.org.au (Accessed 16 March 2010).
21. Kenny A. Medical dominance and power: a rural perspective. Health Sociology Review 2004; 58(6): 158-165.
22. Kenny A, Duckett S. A question of place: medical power in rural Australia. Social Science in Medicine 2004; 58(6): 1059-1073.
23. Norsen L, Opalden J, Quinn J. Practice model: collaborative practice. Critical Care Nursing Clinics of North America 1995; 7(1): 43-52.
24. Hall P. Interprofessional teamwork: professional cultures as barriers. Journal of Interprofessional Care 2005; 19(Suppl1): 188-196.
25. Norman GR, Shannon SI, Marrin ML. The need for needs assessment in continuing medical education. BMJ 2004; 328: 999-1001.
26. International Commission on Radiological Protection. 1990 Recommendations of the ICRP. ICRP Publication 60. Bethesda: Pergamon, 1991.
27. Davis DA, Mazmanian PE, Fordis M, Van Harrison R, Thorpe KE, Perrier L. Accuracy of physician self-assessment compared with observed measures of competence. JAMA 2006; 296(9): 1094-1102.


