Error is often compounded by organisational risks which may be cultural or related to workload. In community pharmacy, it is perceived that pharmacists have onerous workloads, especially in inland Australia1. Trends in rural pharmacy are characterised by an ageing workforce and competition for retail sales, frequently addressed by extended shifts and working weeks for pharmacists. These may be in breach of the 5th principle of the Pharmaceutical Society of Australia Code of Professional Conduct2:
A pharmacist must neither agree to practise under conditions which compromise their professional independence, judgment or integrity, nor impose such conditions on other pharmacists.
The impact of these expectations on concentration due to fatigue may contribute to increased errors or 'near misses' (or 'captured' errors which get through some safety layers but are identified before they reach the patient and cause harm).
An annual drop-out rate of 3-7% of pharmacists3 compounds this trend for those remaining. Young pharmacists' attrition rates are attributable to limitations in advancement opportunities, or as Goodman suggests, 'burnout' due to excessive responsibility without sufficient mentoring3.
As Reason points out, if errors cannot be eliminated through design, the consequences must be mitigated4. The organic nature of human error complicates error reduction; however, organisational risk management, as applied in the aeronautical and nuclear power industries, has potential.
Errors may be classified as a5:
- mistake: choosing the wrong course of action
- slip: correct action chosen but executed incorrectly
- lapse: when incorrect execution involves a failure of memory
- violation: failure to use standard or mandatory procedures.
In pharmacy practice, a 'slip' is when the action was correctly intentioned, but physically flawed (eg a crooked label on a product, despite taking time to line it up squarely). A 'lapse' is a failure in memory often triggered by distractions.
You'll be halfway in dispensing something and then you'll be disrupted. For instance today... I was dispensing one thing in a basket for one set of customers and then I noticed... so I went over and started in their basket. And then I checked that, everything was fine, but somehow the other person's, one of their tablets, I'd put into the basket that I was checking. So I guess it's you just have to really finish or leave something before you go on to the next thing or you can muddle it up. (Pharmacist)
A 'mistake' is when the intended action is not appropriate for the circumstances, for example when a transcription error occurs, or if the dispensing assistant (DA) or pharmacist misreads the prescription. These errors are not malicious in intent, but the result of human fallibility, environmental distractions and/or frustrations.
A 'violation' is when mandatory procedures are not followed, such as forgetting to place 'cautionary label 1' on a box of diazepam in accordance with Appendix K of the 'Standard for the Uniform Scheduling of Medicines and Poisons' (SUSMP)6. Reasons for violations may not be malicious, and may include inadequate knowledge and training. A violation may also be a better action that is yet to be incorporated into regulations. For instance, there is currently a debate in pharmacy forums1 about emergency supply which suggests the time has come for legislation to bend to the common practice of supplying an entire month's supply rather than 'breaking the package' and giving enough for 3 days only in accordance with the SUSMP Subsection 2, Paragraph 39, Part 36.
A review of the literature on the control of errors in community pharmacy through design revealed that little investigation has been undertaken (M Madden, pers. data, 2008). Related research mostly pertained to medical errors (doctors and nurses). Recently interest has emerged in the pharmacist's role in capturing errors and near misses, with recommendations emerging to minimise errors7, research into medication errors in hospital pharmacy8 and preparation of dose administration aids9.
The aim of this pilot study was to explore the attitudes and actions of Australian pharmacists in rural and regional areas when responding to dispensing errors, in order to determine the decision-making processes behind organisational strategies implemented to detect and recover slips, lapses and mistakes. The rationale for this stems from the 'theory of planned behaviour' outlined by Ajzen (cited in10), where intention is perceived as the driving force towards behaviour. Three factors feed into intent:
- Attitude (positive or negative)
- Subjective norm (social pressure to perform or not)
- Perceived behavioural control (ease or difficulty of performing the behaviour).
The theory of planned behaviour encompasses intended actions which are appropriately executed; so in the case of errors, this would only encompass violations and mistakes. Environmental factors and internal variables influence the occurrence of slips and lapses. Hence, the reflection of pharmacists on strategies implemented to reduce those contributing organisational risks is also included.
Following a brief presentation by the interviewer, participants were recruited at continuing professional education (CPE) days. The CPE days are video-conferenced to 4 venues in the Riverina, New South Wales, so information about the study spread and those interested contacted Charles Sturt University for more information. Hence, recruitment was opportunistic.
While there were more than 20 volunteers, the emergence of common themes and data saturation occurred at 12 interviews. The interviewees were practising pharmacists ranging in experience from newly registered to more than 40 years in both hospital and community settings. Practice locations and roles also varied and included community pharmacy owners, salaried community pharmacists (part-time and full-time), medication review pharmacists working on contract, and hospital pharmacists. At least four of the interviewed pharmacists regularly practised at more than one venue, or had recently changed their main venue of practice.
All interviewees worked in regional or rural areas (small towns in the Riverina-Wiradjuri country) at the time of the interviews. Ethics approval to conduct this research was provided by the School of Biomedical Science Ethics Committee at Charles Sturt University. Given the heightened privacy concerns of rural and regionally placed pharmacists, the interviews occurred at the pharmacists' practice site, and were audiotaped. The interviews were transcribed verbatim by a third party, and then analysed by the interviewer for emerging themes.
The design of the interview included a brief survey of 8 questions to which the pharmacist answered on a scale of 0 (completely disagree) to 5 (completely agree) to determine the attitudes of the interviewee to dispensing errors and error reporting. These questions were deliberately out of any obvious sequence, with themes recurring in a negatively-phrased manner to identify consistency in attitudes. This was followed by free discussion of personal experiences with dispensing errors and their repercussions. Prompts made by the interviewer were uniform as part of the structured interview, and open dialogue occurred to ensure a richer depth of discussion and complexity of themes11. The interview concluded with a brief description of demographic information. The time of the interview varied from 20 min to 50 min and many interesting themes emerged.
This interview was designed as an inductive tool to elicit themes and trends; hence, it lacks external validity. However, it is intended to shed light on specific issues related to the decision-making processes of pharmacists in rural and regional areas in order to prompt rigorous research. Further, this research relied on the recollection of the pharmacist, hence it lacks objectivity; for what the pharmacist recalls is influenced by their attitudes and bias.
Current attitudes to dispensing errors
Those interviewed ranged in age and experience, although these independent variables did not correlate with specific attitudes to errors. There were 3 male, and 9 female participants, but given the small number of participants, gender-dependant influence could not be determined and was not the focus of this research. Detail of their responses to the survey follow (Fig1).
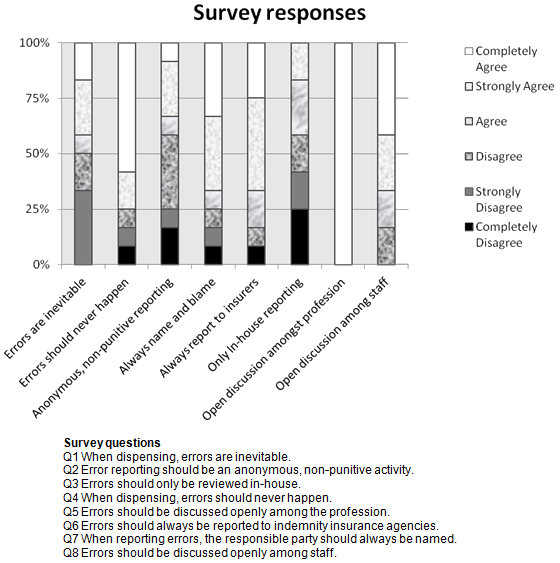
Figure 1: Survey questions and responses.
The first question 'When dispensing, errors are inevitable' produced a range of responses, with two interviewees answering '5', and four interviewees answering '1'. Despite the wide range of answers to this question, the fact that none of the pharmacists answered '0' is an indication that all acknowledged that total elimination of errors is currently unattainable. Errors have not been eliminated from dispensing, but that does not exclude the possibility occurring in the future.
The second question divided the interviewees further: 'Error reporting should be an anonymous, non-punitive activity'. Of the 12 interviewees, one completely agreed while two completely disagreed. However, those who tended towards the idea that 'Errors should only be reviewed in-house' did not correlate with those who strongly agreed with anonymity and no repercussions when reporting errors. Hence, those who tended to record errors in-house rather than report them to indemnity insurers had motivations other than to remain anonymous or avoid repercussions.
During the interviews, there was frequent acknowledgement that certain incidents discussed should have been reported to insurers. This failure to report resulted in no identified negative repercussions and resulted in the positive repercussion of saving time. Hence, this violation (intentional mistake) of procedure became established practice for the pharmacist. In fact, three interviewees reported that in-house recording only was the way errors had been managed since their internship - a time-period which varied widely among the interviewees.
Attitudes to reporting errors were controversial. Of the 5 interviewees who agreed that error reporting should be anonymous and non-punitive, two later agreed 'the responsible party should always be named'. This suggests that the non-punitive nature of reporting is agreed to, rather than the anonymity.
This subset of pharmacists displayed varying attitudes to rates of error reporting, with answers ranging from 'completely disagree' to 'completely agree' that 'Errors should always be reported to indemnity insurance agencies'. It is unclear whether this variety of responses would be narrowed if error reporting were non-punitive.
I don't know who he'd [the client] spoken to and I wasn't there [when the error was made] it was in my lunch hour as well, and he had brought in a video camera to film our response. (Pharmacist)
Given the availability of video-recording components in mobile phones and the litigious nature of Australian society; there is a high probability of litigation and loss of livelihood if an error occurs and is mishandled.
Further, the interviewer anticipated a correlation between attitudes to the inevitability of errors and the acceptability of errors, yet this was not evident. It appears those who see errors as avoidable (strongly disagree with question 1), are divided as to whether they 'should never' occur ('strongly agree' and 'completely disagree') that 'errors should never happen'. This suggests a difference in attitude towards the possibility of eliminating error through design. Some were of the opinion that humans are fallible so errors will always be possible, with the result of accumulating organisational risks.
You've got a set way to do your checking so you make sure you do it, like you're checking the drug against the name ... especially on weekends you get a lot of hospital doctors and antibiotics for children so I always make a point of thinking about the dose ...I'll have the little red paediatric book and I do check that...You just do your best but when you get busy I think mistakes are inevitable no matter how hard you try. (Pharmacist)
Others perceived the dispensing process as one that can be learned as an error-free sequence, hence any error is due to violation of procedures.
I think it [barcode scanning] is the best innovation that has been made in pharmacy in the last few years because it really means that if you get your first script [prescription] right, there shouldn't be too much reason for any subsequent scripts being wrong. (Pharmacist)
All 12 interviewees completely agreed that 'Errors should be discussed openly amongst the profession' which was anticipated from a group volunteering to participate in research about dispensing errors. However 2 interviewees disagreed to some extent that 'Errors should be discussed openly among staff'. There may be issues of pride, authority and seniority involved in this, prohibiting recriminations from more junior staff. It may be a lack of trust in staff's discretion, or perhaps the close-knit nature of the community from which staff is recruited producing privacy concerns that prevent open discussion. However, the benefit of open discussion is the 'wake-up call' example for instruction and training purposes that encourages vigilance, discretion and adherence to dispensing procedures.
Of the 12 interviewees, none answered the 8 questions in an identical fashion, even when responses were simplified to agreeing or disagreeing. This suggests a diverse mix of attitudes, with no correlation between worksite, sex, age or role identified. Aspects of personality such as self-monitoring and previous behaviours exert significant effect on attitudes in what has been described as the 'behaviour-attitude-behaviour sequence'12. Some pharmacists will be more reflective due to personality traits, creating a greater variety of responsiveness to forming current attitudes from previous behaviour.
As reflective people, subjective norms and perceived behavioural control may play a greater role in forming the intention to act than the individual attitudes of dispensing pharmacists. Hence, initiatives focussing on practical instruction, such as an internship period to improve pharmacists' error management skills, are likely to be more effective than initiatives that target theoretical instruction.
Reporting culture
The discussions with interviewees revealed details of the current safety culture in pharmacy in this region of inland Australia. Initially the data suggested that generational boundaries exist regarding readiness to acknowledge and report errors, but on closer analysis a vertical trend across the age brackets was suggested.
I was a graduate and I, a customer brought it to my attention, it was the wrong strength and I went and spoke to the pharmacist... I guess it wasn't my error but I... had to manage it! ...the pharmacist had actually done it all. It was just I think their way of not dealing with it and seeing it as a learning experience of me having to deal with the customer. (Pharmacist)
Many young pharmacists reported that senior pharmacists display reluctance to report errors to indemnity insurers but some had been trained in a culture of regular reporting. Hence, the influence of advice about handling errors during internship and professional formation more strongly influenced whether the pharmacist would report frequently, than the information directly received from insurers.
Someone mature with some more experience... they've probably dealt with a lot of those situations before. So whether that's from dealing with PDL [the insurance agency Pharmacy Defence Ltd] or someone. I think a lot of the time as well; it is learn[ed] off working with older pharmacists who have more experience as well. I don't know that it's necessarily what you get from organizations but it's just... being taught with that culture in place that you then pick it up and run with it. (Pharmacist)
Interestingly, experiencing influence from both inclinations (regular reporters, and reluctant reporters) inclined the pharmacists to report more than not (given conflicting subjective norms). The crucial element appears to be early career exposure to the reporting procedure which may endorse the perception of behavioural control.
But in my graduate year she always said, 'Make sure if there is an error with somebody and they bring it in to you, that only you deal with it. So don't let the girls in the shop deal with it. Go out to the patient, find out exactly what's going on. Find out whether they had taken any of the medication, all the circumstances around it. You deal with it, you solve it, you ring the doctor. You do the whole bit.' Because obviously you don't want to make the patient feel like, the shop girl just tried to sort it all out and it's really not sorted and I don't feel like they're taking good care of me.... So I think that's really important. That means the pharmacist who deals with all of it and makes sure that the patient is okay with what's happened when they leave. (Pharmacist)
Reports were more likely to be made if the patient had consumed the erroneous product; however, they did not occur when an untouched pack of medication was returned, or if the error was identified before issue (a near miss).
Continuous quality improvement
In-house recording of errors included noting on the patient profile and recording the incident in the 'Quality Care Pharmacy Program Incident Report folder' (for recording errors or incidents in one accessible place). There were far more incidents recorded than reports made to the insurers, with four of the 12 interviewees (of diverse age, role and experience) never having made an insurance report. Discussion of these recorded errors and near misses were the majority of examples given by pharmacists, and included outlining the changes to procedure implemented to prevent the same error occurring.
We're always implementing new things here to try and minimise it that if something does happen, nearly happen, we try to put some system in place, but it is hard because the dispensary technicians, and I'm sure pharmacists don't always do what you ask them to do or they can make a mistake. (Pharmacist)
This revealed a culture of continuous quality improvement to readily identify procedural and structural obstacles to providing accurate medication management. Examples of procedural changes implemented are provided (Appendix I).
Where procedural issues were not identified as contributing, 'laziness', 'inexperience' and 'distractions' were identified as possible causes. Workload was not identified as a significant trigger of error; however, many interviewees reflected that errors were more likely to occur over lunch breaks or at closing time, which is consistent with research by Ashcroft et al13.
Many pharmacists pointed out that near misses and dispensing errors served as a 'wake up call' - a reminder of the seriousness of the repercussions if their daily tasks are not completed correctly. While these experiences were disheartening and alarming, they also served to initiate professional development and reflective practice, and discussion among the dispensing team.
Fitting the procedure to the worksite
Selection errors of 'sound-alike' and 'look-alike' packaging were the most frequently discussed errors and near misses.
I think it would be good to put something in place where two containers can't look so similar... you should have to have difference strengths, clearly different colourings. (Pharmacist)
At individual worksites, differing strategies were implemented to overcome similar hazards. Some staggered different strengths of medications (eg interspersed different strengths of a given medicine) with other medicines with brand names beginning with the same letter of the alphabet (Fig2). Others retained strict alphabetical order but altered the facing position or location of differing medication strengths in order to maximise packaging differences, for example different coloured package ends facing out, or one strength ending a row and another starting the next row.
Still others introduced a system where high velocity items dispensed most frequently (eg Amoxycillin 500mg capsules) were located in nearby bay, with remaining stock (eg Amoxycillin 250mg capsules) alphabetically ordered from a second bay. Finally, some changed the way the box or bottle faces the staff for each strength, for example strengths of Caduet are faced in a variety of ways to highlight the colour differences (Fig3).

Figure 2: Atacand 16mg starts this shelf, while lower strengths are found elsewhere.

Figure 3: Side of packaging with greatest visual colour difference displayed.
Each workplace had good reason for the different way in which they overcame this hazard, appropriate to the design and layout of the dispensary, and the training level of staff.
The solutions also reflected privacy concerns and increased discretion in regional centres, restricting the scope for engineering better solutions to identified hazards. Pharmacists working in regional areas appreciate the familiarity and rapport their customers share with the staff. However, this raises the risk of handing the wrong prescription to an individual, as staff members may be embarrassed to ask a regular client's name. Further, members of regional communities are thought to be less compliant with or/and welcoming of a tagging system or numbered dockets. Hence, strategies such as ensuring the customer sign every script at the time of handing out or a visual check for the name of the patient were implemented to minimise error. Point Of Sale (POS) linking to the dispensary, with display of the customer's name at the POS (not the names of their medicine) was also used as a visual cue which pharmacy assistants (PAs) were able to monitor, to assist in minimising this error.
Technological advances
At the time of the interviews, compulsory scanners were installed but not in regular use. There were many reasons for this, ranging from interrupted workflow of the pharmacist or DA, to high throughput of prescriptions, insufficient time to consult with staff about new procedures incorporating scanners, and technical issues relating to hardware and training.
We actually have scanners, we use them mostly for scanning the repeats. We have been discussing using them... if, for example, like we always have a technician working as well, if they aren't using the computer like if it's just the pharmacist like if it's a slow afternoon and there's not too many then we generally use the scanner for the product selection as well so if there's only one set of eyes involved we generally try and do that. However if they're there dispensing we can't use the scanner because it interrupts their process. So we have been talking about perhaps getting another screen and trying to hook up in some way to do that. (Pharmacist)
From discussion with interviewees, the most commonly identified error was incorrect strength selection. This correlates to research by Lynskey et al14, Ashcroft et al13 and Chua et al15 who found that the majority of errors during the dispensing process were incorrect strengths, while the most common near miss was incorrect drug selection. Many interviewees suggested that a barcode scanner would have prevented the error which, in some instances, had occurred decades before scanners were introduced.
Transcription errors were also common, especially when the patient had a history of sound-alike medicines and there was insufficient detail on a handwritten script. This type of error also included violations (intentional deviations from procedure) by DAs failing to flag new medicines.
We [pharmacists] would pick up more errors that the doctors have made writing the wrong script, because when they go through and select, they quite often select the wrong drug for example. So I found that there has probably been more errors since computer generated scripts than the old hand-written scripts. (Pharmacist)
None of those interviewed were familiar with automatic labelling machines or dispensing robots, despite six of the 12 interviewees being accustomed to completing in excess of 200 scripts per day with assistance from DAs. One mentioned over 400 scripts daily with three DAs. Discussion of these devices arose on two occasions, and they were considered to be a mechanical replacement of a DA, with error likely at the time of loading the machine, making the process of correcting the error much more time-consuming and labour intensive. This is in line with Reason's finding that computers can simplify the human end of the workload but compound the effects of human error16. In fact many dispensing robots exploit barcoding technology, so this type of error would be recognised as the machine is loaded. However, frequent changes to packaging and barcoding may encourage human operators to override this barcode check, rather than take the time required to manually input new barcodes.
Staff errors
This raised the issue of the difference between a pharmacist maintaining adherence to their own procedures (professional discretion) and staff being required to adhere to local procedures for which they may feel no ownership and have little appreciation. While this concern is addressed through the collaborative approach to the implementation of the Quality Care Pharmacy Program (QCPP; the Pharmacy Guild of Australia initiative to promote consistent standards of service throughout Australia), new staff joining the pharmacy after accreditation may not have this collaborative involvement in staff procedures unless it is promoted by the business owner/s. Further, program design and implementation are not always congruent, and there may be significant deviation from the design when introducing the program. There is a risk that staff may disregard QCPP because the standards and procedures quickly date after being established, for pharmacy is a profession in which new products and research are constantly emerging. Hence, the program requires frequent review and re-accreditation to maintain its link with current practice, and promote staff ownership of their procedures.
Alienation from a safety protocols can also be experienced with respect to Occupational Health and Safety (OHS) procedures. The revised New South Wales Occupational Health and Safety Act, Section 13, Division 2 states that any change to a workplace with OHS implications must be preceded by a consultative process with the employees17. An example of this can be as simple as talking to staff during morning tea and leaving a memo in the tea room about the introduction of a new POS system before it is purchased and implemented.
Frequently, QCPP implementation requires satisfying OHS regulations. Occasionally, duplication of paperwork occurs to satisfy the regulatory bodies (eg the recording of pseudoephedrine sales). Those pharmacies implementing Project STOP18 will record the sale of pseudoephedrine, recording the photo identification of the purchaser on a national database; and pharmacies following QCPP recommendations for 'frequently diverted medicines' also record the sale of these items against the patient's profile.
Management role of pharmacists
Management roles in rural and regional Australia comprise a greater proportion of the pharmacy employment opportunities than in metropolitan centres. This is due to the lower population density and smaller market place making employing more than one pharmacist in a given centre or department inefficient use of finances. Hence, pharmacists in rural and regional centres will be more affected by management issues than metropolitan pharmacists.
Three pharmacists bemoaned the increasing paperwork required to maintain the QCPP, adhere to residential care facility quality assurance, or simply to ensure all staff's superannuation is appropriately distributed.
We do a lot of Webster packing for a nursing home and retirement village and they are quite adept at giving out a report in triplicate if you make a mistake. (Pharmacist)
Two pharmacist managers acknowledged that their other roles removed them from the regular practice of dispensing. Consequently when they did dispense, their progress was slower, less automatic, and more error-prone.
You don't concentrate as well on what you are doing because you are conscious of everything else and also I guess in a bigger pharmacy environment, you've got to watch over everything else as well so you are continually dealing with staff issues and the phone might be right there. (Pharmacist)
Similarly, Reason points out that when tasks are automated, in the event of a failure, the human operators are less practised and more prone to errors16. Just as manual intervention is required in a mechanical breakdown, in an emergency (eg during a bush fire or flood) managers are called on to dispense during unprecedented high workload periods or when a technical failure (eg unreliable electricity supply) has slowed output. Hence, there is a twofold aggravation of risk: the failure of the technology increasing the workload, and the unpractised individual being confronted with the manual process of dispensing.
If I didn't think there was enough money in it when I was doing the job properly, then I'd rather not be involved in it, do you know what I mean? I was always just an employed pharmacist and I always thought it would be easier to be like that because you've got no, it doesn't matter, you're just doing your job properly. But I feel that since I've bought in, that nothing's changed. (Pharmacist)
The attitude of pharmacy owners and salaried pharmacists to high quality service was synonymous. In fact one owner pointed out that when dispensing errors occur, the negative impact of the associated drop in reputation and goodwill among the small community would be devastating from a business perspective.
While the attitudes of pharmacists of the Riverina or Wiradjuri region have been found to be diverse, the subjective norm or safety culture emphasised the importance of continuous quality improvement and in-house recording. The impact of the master-apprentice relationship of preceptor with intern empowered the intern to embrace safe policies and practices. That these practices do not conform precisely to professional practice standards is in response to upholding the duty of care to patients in understaffed conditions in rural and regional settings.
It appears that PAs and DAs have been more likely to violate store procedure than pharmacists to violate their own checking procedure. While the introduction of safety measures is vital to continuous quality improvement, perhaps there has been less consultation with PAs and DAs during this process than OHS legislation mandates.
Negative sentiment to the onerous nature of QCPP implementation and the amount of paperwork involved in maintaining appropriate records existed among pharmacists in management roles. While excessive workload was considered less significant in dispensing errors, there was a high incidence of recollection of errors occurring during lunchbreaks, on public holidays and toward the end of a work shift. Being removed from a regular dispensing role due to management responsibilities was reported to increase the risk of errors. As a greater percentage of pharmacists in rural and regional settings are required to participate in management roles, this issue is significant for pharmacists in inland Australia.
Technology to reduce human involvement in dispensing is available, but may increase the repercussions of errors when the technology fails. The higher throughput establishments in this study found other strategies to minimise errors through venue-specific training and design.
A smaller population base from which to draw staff contributed to privacy concerns about the discussion of errors among pharmacy staff. In regional areas there was an increased risk of handing medicine to the wrong customer due to the community expectation of being recognised by their local pharmacy staff.
This study, while inductive in design, elicited a depth of narrative about the response of individuals to the stressful experience of making (or recognising) a dispensing error. As a result, these findings are not externally valid, but descriptive. Themes emerging from this research are suggestive of rural and regional issues pertaining to dispensing errors.
The communities of inland Australia would benefit from further investigation into issues surrounding the safe supply of medicines by pharmacists with respect to privacy concerns, the unique design of each dispensing environment, increased use of technology, and staff interaction with the safety culture.
Acknowledgements
This project was partially supported by an unconditional grant to the Pharmacy Foundation, Charles Sturt University, from Pharmacy Defence Limited, to support research into error reduction. Also acknowledged for advice and contribution to study design is Gene Hodgins BA(Hons), DPsych(Clin), MAPS, Lecturer and Clinical Psychologist.
References
1. Auspharm. Auspharmenews. (Online) 0000. Available: http://www.auspharmacist.net.au/ (Accessed 12 February 2009).
2. Pharmaceutical Society of Australia. Australian Pharmaceutical Formulary and Handbook, 19th edn. Canberra, ACT: Pharmaceutical Society of Australia, 2004.
3. Goodman M. Mentoring future pharmacists. Australian Pharmacist 2007; 26(11): 892-894.
4. Reason J. Human Error. Cambridge: Cambridge University Press, 1990.
5. Pani J, Cariker J. The psychology of error in relation to medical practice. Journal of Surgical Oncology 2004; 88(3): 130-142.
6. Department of Health and Ageing. Standard for the Uniform Scheduling of Medicines and Poisons No. 1. Canberra, ACT: Commonwealth of Australia, 2010.
7. Semple S, Roughead E. Reducing medication error and harm: an important role for pharmacy in medication safety and safer systems. Australian Pharmacist 2005; 24: 840-845.
8. Runciman WB, Roughead EE, Semple S, Adams RJ. Adverse drug events and medication errors in Australia. International Journal for Quality in Health Care 2003; 15: 149-159.
9. Thong N. Enhanced Safety: Identification and analysis of dispensing errors associated with Community Pharmacy packing of sealed Dose Administration Ai. BPharm Honours Discertation. Charles Sturt University, 2008.
10. Norman P, Abraham C, Conner M. Understanding and changing health behaviour from health beliefs to self-regulation. London: Routledge, 2006.
11. Liamputtong P, Ezzy D. Qualitative Research Methods, 2nd edn. Melbourne, VIC: Oxford University Press, 2007.
12. Zanna MP, Olson JM, Fazio RH. Attitude-behavior consistency: an individual difference perspective. Journal of Personality and Social Psychology 1980; 38(3): 432-440.
13. Ashcroft D, Quinlan P, Blenkinsopp A. Prospective study of the incidence, nature and causes of dispensing errors in community pharmacies. Pharmacoepidemiology & Drug Safety 2005; 14: 327-332.
14. Lynskey D, Haigh S, Patel N, Macadam A. Medication errors in community pharmacy: an investigation into the types and potential causes. International Journal of Pharmacy Practice 2007; 15(2): 105-112.
15. Chua S, Wong I, Edmondson H, Allen C, Grantham JE. A feasibility study for recording of dispensing errors and 'near misses' in four UK primary care pharmacies. Drug Safety 2003; 26(11): 803-813.
16. Reason J. Managing the Risks of Organizational Accidents. Sydney, NSW: Ashgate, 1997.
17. New South Wales Government. Occupational Health and Safety Act. (Online) 2000. Available: http://www.legislation.nsw.gov.au/xref/inforce/?xref=Type%3Dsubordleg%20AND%20Year%3D2008%20AND%20No%3D39&nohits=y (Accessed 18 April 2011).
18. Pharmacy Guild of Australia. Project STOP. (Online) 2007. Available: www.projectstop.com.au (Accessed 11 April 2011).
19. New South Wales Government. Pharmacy Practice Regulation. (Online) 2008. Available: http://www.austlii.edu.au/au/legis/nsw/consol_reg/ppr2008256/ (Accessed 11 April 2011).
________________________
Appendix I: Procedural changes19


