Introduction
Attracting mental health professionals to work in Australian rural and regional areas is a major concern for service providers, policy-makers and rural/regional communities. In common with other rural and remote areas of Australia, mental health services in Gippsland struggle to attract and retain suitably qualified professionals. Located in the south-east of the state Victoria, Gippsland covers 41 524.2 km2 and consists of 6 local government areas with a combined population of 238 907, 1.3% of whom are Indigenous Australians1. Unlike other Victorian rural regions, Gippsland does not have a major provincial city; the population is dispersed in townships, the largest of which Traralgon with a population of approximately 22 0002. Although a central transport corridor provides good access to the state capital Melbourne, the size and geography of the region together with a poor public transport infrastructure means that some regional locations are comparatively isolated and difficult to access. Local industries include power production, agriculture, forestry, fishing, tourism, education, health and retail. Public mental health services are provided by a state funded regional clinical mental health service, 5 psychiatric disability and rehabilitation support services, 6 community health generalist counselling services, 4 alcohol and other drug services, a regional social and emotional wellbeing service for the Indigenous population and a regional school support service. Medicare funded services are provided by GPs, psychologists and a very small number of consultant psychiatrists.
A good deal of the rural and remote workforce literature has focused on the recruitment and retention of the health workforce, in particular doctors. Identified key attractions and barriers to working in rural and remote areas are summarised (Table 1).
Table 1: Summary of attractions and barriers to working in rural and remote settings, with references for each factor3-11
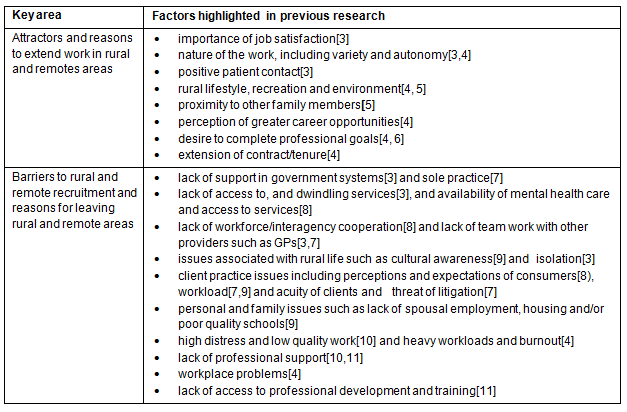
This information, which provides insight into issues of rural and remote workforce recruitment and retention, has been substantially qualified by two recent systematic literature reviews. One of these sought interventions to increase the number of health professions practicing in rural and remote areas12 but found no publications that met the Cochrane selection criteria. The subsequent review by Wilson et al13 used a less exacting inclusion criterion for research studies and the findings are summarised (Table 2), with weak evidence found for:
- education/training
- support
- coercion
- incentive strategies.
While the studies reviewed by Wilson et al13 suggested moderate evidence for 'incentives', this applied to short-term recruitment strategies and so is weak in the longer term. It is also important to note that when in students are in rural locations they value support and this is an important component in rural and remote placements, regardless of outcome14.
Table 2: Levels of evidence (graded convincing to strong, moderate, weak and absent) according to type of interventions to increase recruitment and retention of professionals in rural and remote areas13
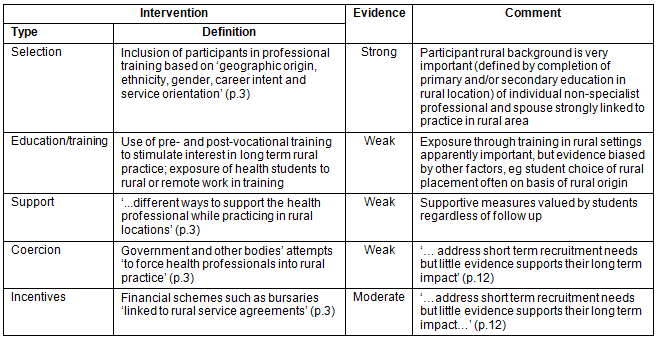
There is some evidence that pre- and/or post-vocational placements (eg clinical rotations) in rural areas impact on recruitment, although this evidence is biased by other factors such as student choice of placements13 and the confounder of participant rural origin has not been accounted for in some studies. Ranmuthugala et al15 raised similar concerns regarding the evidence for the effectiveness of rural medical and nursing workforce initiatives reported in Australia. However Rabinowitz et al16 concluded that in the USA, medical school rural programs have been highly successful, with an average of 53% to 64% of graduates working in rural settings.
The only 'strong' evidence found was in regard to student selection, indicating that 'rural applicants with a stated interest (or 'career intention') in general practice, and a service orientation, is the strategy with the greatest likelihood of reducing the rural-urban gap'12,13. Similarly, Stagg et al17 reported that some key influences on medical graduates' choice of a rural career pathway are:
- their own geographic location prior to entering medical school
- having a spouse/partner with a rural background
- having an extended rural based undergraduate learning experience.
Wilson et al also commented that the rural location of medical schools seems to lead to more rural doctors13, although this may be contingent upon the rural background of students, rather than the location of the medical school. While the quality of research is low, minimal evidence supports the successful relocation of urban professionals to rural and remote positions without consideration of additional intrinsic factors, such as having a partner from rural background.
Surprisingly, only three rural studies have gained the perspective of such senior rural informants. The single Australian study8 focused upon general issues for rural and remote health providers rather than specific issues of recruitment and retention in mental health. Two US studies examined the views of hospital CEOs from rural Illinois18, and then compared them with those of a similar rural Arkansas cohort19. The CEOs were surveyed for their perception of needs, barriers and strategies regarding recruitment and retention of rural health care professionals. They found that communities need to be 'attractive' to health professionals, where 'attractive' included such things as the community being collaborative, instilling hope and being supportive of families (eg being 'family friendly'). The most important recruitment and retention predictor was a positive perception of the public school system19. Unfortunately the survey design in this study was based on previous worker perceptions and not those of CEOs or managers. While the survey was rated by managers, the items were designed for workers. It is therefore unclear whether the findings represent the expansive and unfettered views of these key regional informants or are merely answers to a worker prescribed rubric. Consequently, the views of senior personnel are an important gap in the mental health recruitment and retention literature.
The present study sought to add to the literature by gaining the views of managers and leaders from mental health service providers throughout Gippsland. It was considered that their interface with workers and structural factors that influence regional employment together with their 'bigger picture' viewpoint would provide a region wide perspective on recruitment, retention and training. It was hypothesised that solutions determined from their perspective would enable the development of a well-founded regional mental health workforce strategy. In interviews, the participants were asked to consider key regional issues and current and potential solutions. This article explores these solutions.
Potential interviewees were selected on the basis of their expertise as either a manager of a mental health service, their role in policy development and/or implementation, or a direct involvement in the provision of mental healthcare services.
The Director of Mental Health, Latrobe Regional Hospital, facilitated the nomination of participants from the clinical mental health service. Those from all other sectors were recruited by an initial phone call. Each participant was sent a detailed background information sheet. Each participant was interviewed in his/her place of work during working hours, according to a semi-structured interview that explored issues and solutions relating to mental health workforce recruitment, retention and training in Gippsland generally and also their particular organisation. Interviews were recorded and transcribed. A record of interview validity check was undertaken with each participant20 by returning a brief summary of their interview for comment, correction and refinement. The research was approved by the Monash University human research ethics committee.
Data were analysed using intra- and cross-interview analyses. Initial analyses identified the central themes within each transcript. The first and third authors then analysed the data across transcripts, breaking each into units of meaning comprised of single or grouped phrases and sentences. This was undertaken independently with as little interpretation as possible in order to preserve the integrity of participants' meanings.
The analysis identified a number of recurring themes exhibiting internal consistency and distinction21. Comments that differed from the majority informed the researchers of issues otherwise not identified or differently interpreted. Interpretation was aided by reference to the research literature. The emergent themes were also examined by sector and sub-region to identify any variation in patterns within the region.
Results
Twenty-eight potential informants were identified and considered to be representative of management and clinical leadership of mental health service providers in the region. Two people declined to be interviewed as they did not consider they had sufficient background and understanding of the issues to contribute meaningfully. The remaining 26 informants (seven male and 19 female) were interviewed, included representatives from the clinical mental health service, Psychiatric Disability Rehabilitation And Support Services, community health, Divisions of General Practice, small rural health services, non-government agencies, professional groups (eg Australian Psychological Society, Australian Association of Social Workers) and private practitioners from the region. Informants included nurses, psychiatrists, medical practitioners, social workers, psychologists and administrators who had between 10 and 30 years experience in mental health and/or the Gippsland region.
The 10 themes that emerged from the data (Table 3), were aggregated at a higher level as factors external or internal to the organisation. The data indicated that while recruitment, retention and training are conceptually distinct, they are also intertwined (eg training is a significant factor in both recruitment and retention). The weight of commentary that led to the emergence of each theme is indicated by the number of 'units of meaning' that contributed to it, with the value suggestive of a crude hierarchy of importance and urgency (the authors acknowledge the philosophical tension in this position and use it with circumspection).
Table 3: External and internal themes according to recruitment, retention and training solutions
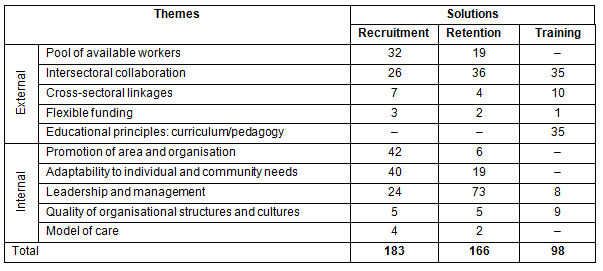
Themes external to the organisation
Pool of available workers: The 'pool of available workers' refers to the need for reform of the regulatory, industrial and training environment to increase the pool of available workers. Participants advocated reform to address shortages such as the development of nurse practitioners, enhancement of the role of Division 2 nurses and the restructuring of basic nurse training to better prepare them for mental health care and increase the pool of suitably trained potential workers. They also proposed the creation of links with potential recruits through the regional GP training program and development of traineeships for allied health assistants.
The second theme, that of inter-sectoral collaboration, links to the issue of the pool of available workers, with a number of participants suggesting that enabling 'secondment opportunities' and rotations across positions in the region would create career pathways within the region, while 'sister relationships' with metropolitan services would create new training and professional development opportunities.
Inter-sectoral collaboration: Cross-agency collaboration was highlighted as a core means to address training and professional development needs as well as issues of retention. Several participants identified the need to 'improve communication between agencies' by 'exchanging' and 'sharing' relevant information and resources. Organisations that had established 'joint positions with universities' and/or 'connections' with research agencies advocated the benefits of this approach. Other suggested mechanisms to improve retention include working together 'in a co-ordinated way' with 'a common language and complementary treatment programs', developing 'streamlined referral pathways that everyone is aware of' and 'co-location with other health services' to 'build networks and relationships and reduce isolation'.
A number of participants advocated for 'joint training, secondment opportunities or rotations with other services', 'trying to take a more strategic approach to training and professional development' and adopting an 'area based planning approach' based on 'identified local needs'. Some suggested that a regional structure, perhaps similar to the Gippsland Mental Health Alliance (a 2006 Victorian Department of Human Services initiative that aimed to provide a 'more cohesive recovery and rehabilitation mental health system' through formal partnership arrangements between state funded clinical mental health services and psychiatric disability rehabilitation support services in each area mental health service catchment) could co-ordinate such joint initiatives. The Dual Diagnosis Initiative was highlighted as an exemplar of the mix of organisational initiative and central seeding envisaged in the approach (this initiative was instituted to support the development of better treatment practices and collaborative relationships between drug treatment and mental health services; key activities include the development of local networks, the training, consultation and modelling of good practice through direct clinical intervention, and shared care arrangements).
Cross-sectoral linkages: The term 'cross-sectoral linkages' relates to establishing linkages with external organisations, bodies and sectors. Informants suggested that 'links to institutions who do basic training of mental health professionals' and 'links to research and academia' would increase the exposure and appeal of organisations. Others suggested that 'access to support networks' (eg the East Gippsland Counsellors Network and the Australian Psychological Society) was important. Also suggested was that 'strong networking and linkages with other sectors, for example Child Protection and Depart of Education and Early Childhood Development' could help in retaining geographically isolated workers. It was widely thought that social networks have a similarly beneficial effect on attracting new graduates to move into the region.
Flexible funding: A participant highlighted the benefit of flexible funding, 'we're also an MPS ...which means we have flexible money, which means we can respond' creatively to recruitment and retention issues. Another informant advocated that 'flexibility in relation to targets' would provide greater capacity to support staff gain access to training and professional development.
Educational principles - curriculum/pedagogy: The two most commonly proposed training solutions were the need for inter-sectoral collaboration and use of innovative educational principles. Collaboration with other agencies was seen as a critical means of combining resources and bringing trainees together, thereby reducing the need for travelling long distances for training in Melbourne. The use of innovative educational curriculum and pedagogical techniques, including applied learning approaches such as scenarios and interactive 'second life' programs, were recommended as ways to make learning engaging and effective. 'Online learning and new technology' such as video-conferencing were suggested as ways of 'overcoming the tyranny of distance [and] ... the barrier of the generation gap'. However it was made clear that training had to be relevant to current practice, complement current models of service delivery, and be evidence-based.
Themes internal to the organisation
Promotion of the area and organisation: Informants stressed the importance of the promotion of region and organisation to improve recruitment. They reported that many organisations currently did this by providing support for short- and long-term accommodation and making use of available rural incentive programs. One participant indicated that their organisation had:
...developed a DVD that sells the area, you know, the beauty of it, sells the health facility, takes you through, shows you that it's a nice clean, well equipped, friendly facility and with the doctors we have our financial package that we can offer them.
Others suggested that recruitment can be enhanced by highlighting the organisations profile: '...we were able to offer staff this really exciting way of working' and 'we...talk about the models of service we deliver'. An informant emphasised the need for agencies to 'become learning organisations which [are] committed to career development'. The exposure of students to rural practice through placements was regarded as similarly important in organisations' recruitment and retention strategies. It was suggested that program areas such as child and adolescent mental health services would benefit from highlighting the career opportunities that these areas offer.
Adaptability to individual and community need: A core component of management practice found to be favourable to recruitment and retention has been the development of structures and processes that foster organisational adaptability to accommodate each (current and potential) employee's specific circumstances and characteristics. Such responsiveness has included flexible working arrangements in terms of 'hours of work, job share and part-time positions' and offering the '48/52' option (in some Australian industrial awards staff can exchange salary for an additional 4 weeks annual leave, while retaining their full rights and entitlements). Several managers spoke of the need to make appointments based upon a very clear idea of the 'profile of the person that would live in places like this', and of applicants' personal attributes - their 'interpersonal skills, attitude, motivation, communication skills and fit with where the organisation is heading' - rather than being tightly constrained by 'the right professional background'. They also spoke of their use of unorthodox recruitment methods such as 'head hunting', using the recruitment process to 'engage' the potential recruits, the use of recruitment agencies and, to reach younger workers, using the internet. A number suggested that exit interviews should be a key component of a planned approach, although this approach 'takes more effort... [it] is worthwhile because in the end you're not recruiting as often'.
Participants suggested the importance of a carefully structured approach to the support of particular cohorts of workers, in the form of targeted orientation and induction programs, social support (eg for young professionals) and essential training for those who lack qualifications or experience. This approach extends to the adaptation of routine practice to attract specific professional groups, as one organisation did by extending its model of care to attract more nurses. By modifying role expectations to suit the skills and experience of one cohort of workers, the organisation became the local employer of choice, while also retaining the services of older staff who found change difficult. Participants also said that organisations must adapt to meet the needs of the community in which they work. In one instance, a large sub-regional provider and a much smaller service in a remote hinterland community had developed and jointly funded an arrangement in which the larger service provides regular outreach psychological services to the smaller.
Leadership and management: Leadership and management were indicated as crucial in the implementation of the above strategies. It was suggested that high quality managers clearly outlined roles and expectations through orientation/induction programs and provided access to accredited training and/or professional development programs. One manager said:
...actually make people who come and work here feel as though they are getting something value-added...they're learning stuff, they're getting better, they feel supported, they feel...encouraged, empowered and able...to really progress in their professional development.
The importance of 'linking the aims and goals of personal professional development plans to core competencies and mental health workforce standards' was emphasised by another participant. One organisation has 'a strategic plan' with 'a whole section which is called supporting our people'. In this and other instances, managerial leadership was highlighted, with a key element being the ability to continue supporting change in the face of the difficulties. Consistent with this theme, one organisation has implemented a 'leadership training program' for managers.
The quality of organisational structures and cultures: Participants from the larger organisations highlighted the importance of mental health program representation on senior organisational administrative bodies. A respondent suggested that 'management structures can hinder or enable recruitment and retention'. Another participant suggested that regional program providers should 'ensure' that operational governance structures and administrative processes 'engender a sense of team' so 'that staff do not feel isolated' and thereby avoid problems of retaining staff. Several participants suggested that a 'centralised system' is a 'more efficient' way to coordinate recruitment, traineeships and training.
Model of care: A small number of participants indicated that implementing an evidence-based model of care influences recruitment and retention. One informant indicated that this involves 'delivering an intervention or interventions...based in evidence and validated by research'. Another suggested that 'implementing evidence based models of treatment and support' contributes to the retention of current staff and recruitment of new staff.
Discussion
The interviewed Gippsland mental health leaders made a clear distinction between workforce solutions that were internal and external to the service that they represented. This distinction focused on the difference between factors under their influence and others that were out of their control. This is an important distinction not found in the literature. It demonstrates the complexity of the issue that those in leadership positions face as they struggle to recruit and retain staff while also meeting service needs. It also highlights the important role leadership has in developing organisational attributes that promote the area and organisation to prospective employees, and also the critical need for leaders to be able to collaborate with other organisations and sectors.
The workforce literature rarely mentions the centrality of such management and organisational structures and cultures to rural and remote health organisations' ability to attract and retain employees. However, this study found them to be vitally important. Management flexibility is necessary so organisations can adapt to meet the personal and professional needs and aspirations of current and potential employees and their families. Rural mental health services have to aspire to become employers of choice, which includes providing information and incentives, individualising induction programs, and accommodating the practice preferences of different generational cohorts and needs in different localities22.
This organisational adaptability extends to building collaborative relationships with other organisations, establishing linkages with training, and research institutions, and forging links to local professional and social support networks. These approaches help enhance the support of trainee and student placements, tailor mentorship23 and preceptorship arrangements to meet individual needs24, and facilitate access to ongoing professional development. This approach to collaboration and intersectoral partnership is best represented in the implementation of the Victorian Dual Diagnosis Initiative in Gippsland.
The benefits of such a progressive and innovative management approach is demonstrated by organisations in Gippsland who successfully manage workforce recruitment and retention, and is a key to building and maintaining an effective and sustainable mental health workforce in the region. If well organised and well supported14, such human resource management has been found to enhance organisational stability and productivity by retaining interested and productive employees and building the organisation's capacity to meet the needs of clients and local communities3,4. The exposure of students and registrars to rural practice has been found to have similar outcomes25, and exposure to an intensive course on psychiatry has been found to influence students' decisions to undertake psychiatric residency programs26.
The findings of this study both support previous research and contribute to the existing knowledge base. Previous literature from the perspective of workers highlights that agencies must be flexible in recognising personal and family needs when recruiting personnel4,5,9. This finding also supports the studies by Glassen et al18 who found that US rural hospital CEOs believed communities need to be supportive of families (eg providing good schools, being 'family friendly'). The present study findings and previous literature illustrate the importance of considering the individual applicant and their family in recruitment strategies, thereby ensuring that the location is attractive to the prospective employee.
Conclusion
The solutions explored in this paper highlight the creative way in which managers of mental health organisations in Gippsland are responding to the workforce recruitment and retention challenges they face. These solutions also indicate possible future regional strategies that can be expected to address the ongoing shortage of mental health workforce in Gippsland. While this study adds a new perspective to the mental health workforce literature through the reflections of managers grounded in their day to day work, it also highlights the paucity of evidence regarding effective approaches to dealing with rural mental health workforce shortages. It is important therefore that further consideration be given to implementing and evaluating evidence-informed mental health workforce development strategies, and linking local regional strategies to State and National mental health workforce strategies.
References
1. Department of Human Services. Aboriginal statistical profiles: statistics collected by local government area on the Aboriginal population of Gippsland. (Online) 2008. Available: http://www.dhs.vic.gov.au/__data/assets/pdf_file/0006/383910/GS103.pdf (Accessed 11 October 2010).
2. Victorian Department of Planning and Community Development. Population trends and the Gippsland region. (Online) 2008. Available: http://www.dpcd.vic.gov.au/__data/assets/pdf_file/0016/32164/RegionalForums_Gippsland_Traralgon_1_47.pdf (Accessed 15 December 2010).
3. Eley D, Young L, Shrapnel M. Rural temperament and character: a new perspective on retention of rural doctors. Australian Journal of Rural Health 2008; 16(1): 12-22.
4. Perkins D, Larsen K, Lyle D, Burns P. Securing and retaining a mental health workforce in Far Western New South Wales. Australian Journal of Rural Health 2007; 15(2): 94-98.
5. Lau T, Kumar S, Robinson E. New Zealand's psychiatrist workforce: profile, recruitment and retention. Australian and New Zealand Journal of Psychiatry 2004; 38(7): 547-553.
6. Meyer D. Technology, job satisfaction, and retention: rural mental health practitioners. Journal of Rural Health 2006; 22(2): 158-163.
7. Gibb H, Livesey L, Zyla W. At 3 am who the hell do you call? Case management issues in sole practice as a rural community mental health nurse. Australasian Psychiatry 2003; 11(Suppl1): S127-S30.
8. Eley RM, Baker PG. Rural and remote health research: key issues for health providers in southern Queensland. Australian Journal of Rural Health 2007; 15(6): 368-372.
9. Roger AR, Andrilla CHA, Thomas C, Hart LG. Shortages of medical personnel at community health centers: implications for planned expansion. JAMA 2006; 295(9): 1042.
10. Gardiner M, Sexton R, Durbridge M, Garrard K. The role of psychological well-being in retaining rural general practitioners. Australian Journal of Rural Health 2005; 13(3): 149-155.
11. Hodgins G, Murray G, Donoghue A, Judd F, Petts A, Hodgins G et al. Introducing a professional development programme to a rural area mental health service: the importance of context. Australasian Psychiatry 2004; 12(2): 153-160.
12. Grobler L, Marais BJ, Mabunda SA, Marindi PN, Reuter H, Volmink J et al. Interventions for increasing the proportion of health professionals practising in rural and other underserved areas. Cochrane Database of Systematic Reviews 2009; (1): CD005314.
13. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ et al. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural Remote Health 9(2): 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 11 October 2010).
14. Lea J, Cruickshank M, Paliadelis P, Parmenter G, Sanderson H, Thornberry P. The lure of the bush: do rural placements influence student nurses to seek employment in rural settings? Collegian 2008; 15(2): 77-82.
15. Ranmuthugala G, Humphreys J, Solarsh B, Walters L, Worley P, Wakerman J et al. Where is the evidence that rural exposure increases uptake of rural medical practice? Australian Journal of Rural Health 2007; 15(5): 285-288.
16. Rabinowitz HK, Diamond JJ, Markham FW, Wortman JR. Medical school programs to increase the rural physician supply: a systematic review and projected impact of widespread replication. Academic Medicine 2008; 83(3): 235-243.
17. Stagg P, Greenhill J, Worley PS. A new model to understand the career choice and practice location decisions of medical graduates. Rural and Remote Health 9(4): 1245. (Online) 2009. Available: www.rrh.org.au (Accessed 11 October 2010).
18. Glassen M, Peters K, MacDowell M. Rural Illinois hospital chief executive officers' perceptions of provider shortages and issues in rural recruitment and retention. Journal of Rural Health 2006; 22(1): 59-62.
19. MacDowell M, Glasser M, Fitts M, Fratzke M, Peters K. Perspectives on rural health workforce issues: Illinois-Arkansas comparison. Journal of Rural Health 2009; 25(2): 135-140.
20. Lincoln Y, Guba E. Naturalistic inquiry. London: Sage, 1985.
21. Marshall C, Rossman G. Designing qualitative research, 3rd edn. Thousand Oaks, CA: Sage, 1999.
22. Hart LG, Salsberg E, Phillips DM, Lishner DM. Rural health care providers in the United States. Journal of Rural Health 2002; 18(Suppl): 211-232.
23. Mills J, Francis K, Bonner A. Live my work: rural nurses and their multiple perspectives of self. Journal of Advanced Nursing 2007; 59(6): 583-590.
24. Cleary M, Happell B. Promoting a sustainable mental health nursing workforce: an evaluation of a transition mental health nursing programme. International Journal of Mental Health Nursing 2005; 14(2): 109-116.
25. Hodges B, Rubin A, Cooke RG, Parker S, Adlaf E, Hodges B et al. Factors predicting practice location and outreach consultation among University of Toronto psychiatry graduates. Canadian Journal of Psychiatry 2006; 51(4): 218-225.
26. Lofchy J, Brunet A, Silver I. The psychiatry institute for medical students: a novel recruitment strategy. Academic Psychiatry 1999; 23(3): 151-156.



